Attached files
| file | filename |
|---|---|
| EX-32.1 - EX-32.1 - Voyager Therapeutics, Inc. | vygr-20171231ex321ad5904.htm |
| EX-31.2 - EX-31.2 - Voyager Therapeutics, Inc. | vygr-20171231ex3123b26df.htm |
| EX-31.1 - EX-31.1 - Voyager Therapeutics, Inc. | vygr-20171231ex311f85e86.htm |
| EX-23.1 - EX-23.1 - Voyager Therapeutics, Inc. | vygr-20171231ex231e9df05.htm |
| EX-21.1 - EX-21.1 - Voyager Therapeutics, Inc. | vygr-20171231ex211199c06.htm |
| EX-10.22 - EX-10.22 - Voyager Therapeutics, Inc. | vygr-20171231ex10229c9cb.htm |
| EX-10.21 - EX-10.21 - Voyager Therapeutics, Inc. | vygr-20171231ex1021617d8.htm |
| EX-4.1 - EX-4.1 - Voyager Therapeutics, Inc. | vygr-20171231ex4167a89f3.htm |
UNITED STATES
SECURITIES AND EXCHANGE COMMISSION
Washington, DC 20549
FORM 10-K
(Mark One)
|
☒ |
ANNUAL REPORT PURSUANT TO SECTION 13 OR 15(d) OF THE SECURITIES EXCHANGE ACT OF 1934 |
For the fiscal year ended December 31, 2017
OR
|
☐ |
TRANSITION REPORT PURSUANT TO SECTION 13 OR 15(d) OF THE SECURITIES EXCHANGE ACT OF 1934 |
For the transition period from to
Commission File Number: 001-37625
Voyager Therapeutics, Inc.
(Exact Name of Registrant as Specified in Its Charter)
|
Delaware |
|
46-3003182 |
|
(State or Other Jurisdiction of Incorporation or Organization) |
|
(IRS Employer Identification No.) |
|
75 Sidney Street, |
|
02139 |
|
(Address of Principal Executive Offices) |
|
(Zip Code) |
(857) 259-5340
(Registrant’s Telephone Number, Including Area Code)
Indicate by check mark if the registrant is a well-known seasoned issuer, as defined in Rule 405 of the Securities Act. Yes ☐ No ☒
Indicate by check mark if the registrant is not required to file reports pursuant to Section 13 or Section 15(d) of the Act. Yes ☐ No ☒
Indicate by check mark whether the registrant: (1) has filed all reports required to be filed by Section 13 or 15(d) of the Securities Exchange Act of 1934 during the preceding 12 months (or for such shorter period that the registrant was required to file such reports), and (2) has been subject to such filing requirements for the past 90 days. Yes ☒ No ☐
Indicate by check mark whether the registrant has submitted electronically and posted on its corporate Web site, if any, every Interactive Data File required to be submitted and posted pursuant to Rule 405 of Regulation S‑T (§ 232.405 of this chapter) during the preceding 12 months (or for such shorter period that the registrant was required to submit and post such files). Yes ☒ No ☐
Indicate by check mark if disclosure of delinquent filers pursuant to Item 405 of Regulation S-K (§ 229.405 of this chapter) is not contained herein, and will not be contained, to the best of registrant’s knowledge, in definitive proxy or information statements incorporated by reference in Part III of this Form 10-K or any amendment to this Form 10-K. ☐
Indicate by check mark whether the registrant is a large accelerated filer, an accelerated filer, a non-accelerated filer, a smaller reporting company, or an emerging growth company. See the definitions of “large accelerated filer,” “accelerated filer,” “smaller reporting company,” and “emerging growth company” in Rule 12b-2 of the Exchange Act.
|
Large accelerated filer |
☐ |
|
|
Accelerated filer |
☒ |
|
Non-accelerated filer |
☐ |
(Do not check if a smaller reporting company) |
|
Smaller reporting company |
☐ |
|
|
|
|
|
Emerging growth company |
☒ |
If an emerging growth company, indicate by check mark if the registrant has elected not to use the extended transition period for complying with any new or revised financial accounting standards provided pursuant to Section 13(a) of the Exchange Act. ☒
Indicate by check mark whether the registrant is a shell company (as defined in Rule 12b-2 of the Act). Yes ☐ No ☒
The aggregate market value of Common Stock held by non-affiliates of the registrant computed by reference to the price of the registrant’s Common Stock as of June 30, 2017, the last business day of the registrant’s most recently completed second fiscal quarter, was approximately $94.4 million (based on the last reported sale price on the Nasdaq Global Select Market as of such date).
As of March 9, 2018, there were 32,206,786 shares of the registrant’s common stock, par value $0.001 per share, outstanding.
DOCUMENTS INCORPORATED BY REFERENCE
Portions of the registrant’s definitive Proxy Statement relating to its 2018 Annual Meeting of Stockholders are incorporated by reference into Part III of this Annual Report on Form 10‑K where indicated. Such Proxy Statement is expected to be filed with the U.S. Securities and Exchange Commission not later than 120 days after the end of the fiscal year to which this report relates.
|
|
|
|
|
Page |
|
|
|
|
|
|
|
|
|
4 | ||
|
|
|
52 | ||
|
|
|
108 | ||
|
|
|
108 | ||
|
|
|
108 | ||
|
|
|
109 | ||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
109 | ||
|
|
|
110 | ||
|
|
Management’s Discussion and Analysis of Financial Condition and Results of Operations |
|
112 | |
|
|
|
129 | ||
|
|
|
130 | ||
|
|
Changes in and Disagreements with Accountants on Accounting and Financial Disclosure |
|
130 | |
|
|
|
130 | ||
|
|
|
131 | ||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
131 | ||
|
|
|
131 | ||
|
|
Security Ownership of Certain Beneficial Owners and Management and Related Stockholder Matters |
|
131 | |
|
|
Certain Relationships and Related Transactions, and Director Independence |
|
131 | |
|
|
|
131 | ||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
132 | ||
|
|
|
132 | ||
|
|
|
|
|
|
|
|
|
|
F-34 |
2
Forward-Looking Statements
This Annual Report on Form 10-K contains forward-looking statements that involve substantial risks and uncertainties. All statements other than statements of historical facts contained in this Annual Report on Form 10-K, including statements regarding our strategy, future operations, future financial position, future revenue, projected costs, prospects, plans, objectives of management and expected market growth, are forward-looking statements. These statements involve known and unknown risks, uncertainties and other important factors that may cause our actual results, performance or achievements to be materially different from any future results, performance or achievements expressed or implied by the forward-looking statements.
The words “anticipate,” “believe,” “estimate,” “expect,” “intend,” “may,” “might,” “plan,” “predict,” “project,” “target,” “potential,” “contemplate,” “anticipate,” “goals,” “will,” “would,” “could,” “should,” “continue,” and similar expressions are intended to identify forward-looking statements, although not all forward-looking statements contain these identifying words. These forward-looking statements include, among other things, statements about:
|
· |
our plans to develop and commercialize our product candidates based on adeno-associated virus, or AAV, gene therapy; |
|
· |
our ability to identify and optimize product candidates and novel AAV gene therapy capsids; |
|
· |
our ongoing and planned clinical trials and related timelines, including our ability to continue to advance VY-AADC through the current Phase 1b clinical trial and into a planned pivotal Phase 2-3 clinical program as a treatment for advanced Parkinson’s disease, and our preclinical development efforts and studies; |
|
· |
formulation changes to our product candidates may require us to conduct additional clinical studies to bridge our modified product candidates to earlier versions; |
|
· |
the timing of and our ability to submit applications for, and obtain and maintain regulatory approvals for our product candidates, including our ability to file Investigational New Drug applications, or INDs, for our programs for the treatment of a monogenic form of amyotrophic lateral sclerosis, VY-HTT01 for the treatment of Huntington’s disease, and VY-FXN01 for the treatment of Friedreich’s ataxia; |
|
· |
our estimates regarding expenses, future revenues, capital requirements, and needs for additional financing; |
|
· |
our ability to continue to develop our product engine; |
|
· |
our ability to develop a manufacturing capability compliant with current good manufacturing practices for our product candidates; |
|
· |
our ability to access, develop, and obtain regulatory clearance for devices to deliver our AAV gene therapies to critical targets of neurological disease; |
|
· |
our intellectual property position and our ability to obtain and maintain intellectual property protection for our proprietary assets; |
|
· |
our estimates regarding the size of the potential markets for our product candidates and our ability to serve those markets; |
|
· |
the rate and degree of market acceptance of our product candidates for any indication once approved; |
|
· |
our strategic collaborations with Sanofi Genzyme and AbbVie, including the possibility and timing of each exercising options to certain of our programs as specified in the applicable collaboration agreements; |
|
· |
our plans and ability to raise additional capital, including through equity offerings, debt financings, collaborations, strategic alliances, and licensing arrangements; |
3
|
· |
our competitive position and the success of competing products that are or become available for the indications that we are pursuing; |
|
· |
the impact of government laws and regulations including in the United States, the European Union, and other important geographies such as Japan; |
|
· |
our ability to sustain consistency with recently announced results from our ongoing Phase 1b clinical trial in future clinical trials; and |
|
· |
our ability to enter into future collaborations, strategic alliances, or licensing arrangements. |
These forward-looking statements are only predictions and we may not actually achieve the plans, intentions or expectations disclosed in our forward-looking statements. You should not place undue reliance on our forward-looking statements. Actual results or events could differ materially from the plans, intentions and expectations disclosed in the forward-looking statements we make. We have based these forward-looking statements largely on our current expectations and projections about future events and trends that we believe may affect our business, financial condition and operating results. We have included important factors in the cautionary statements included in this Annual Report on Form 10-K, particularly in “Part I, Item 1A - Risk Factors” that could cause actual future results or events to differ materially from the forward-looking statements that we make. Our forward-looking statements do not reflect the potential impact of any future acquisitions, mergers, dispositions, joint ventures or investments we may make.
You should read this Annual Report on Form 10-K and the documents that we have filed as exhibits to the Annual Report on Form 10-K with the understanding that our actual future results may be materially different from what we expect. We do not assume any obligation to update any forward-looking statements whether as a result of new information, future events or otherwise, except as required by applicable law.
We are a clinical-stage gene therapy company focused on developing life-changing treatments for patients suffering from severe neurological diseases. We focus on neurological diseases where we believe an adeno-associated virus, or AAV, gene therapy approach that either increases or decreases the production of a specific protein can slow or reduce the symptoms experienced by patients, and therefore have a clinically meaningful impact. We have built a product engine, that we believe positions us to be the leading company at the intersection of AAV gene therapy and severe neurological disease. Our product engine enables us to engineer, optimize, manufacture and deliver our AAV-based gene therapies that have the potential to provide durable efficacy following a single administration. Additionally, we are working to identify novel AAV capsids, which are the outer viral protein shells that enclose the genetic material of the virus payload. Our team of experts in the fields of AAV gene therapy and neuroscience first identifies and selects severe neurological diseases that are well-suited for treatment using AAV gene therapy. We then engineer and optimize AAV vectors for delivery of the virus payload to the targeted tissue or cells. Our manufacturing process employs an established system that we believe will enable production of high quality AAV vectors at commercial-scale. Finally, we leverage established routes of administration and advances in dosing techniques to optimize delivery of our AAV gene therapies to target cells that are critical to the disease of interest either directly to discrete regions of the brain, or, more broadly, to the spinal cord region.
4
Our pipeline of gene therapy programs is summarized in the table below:
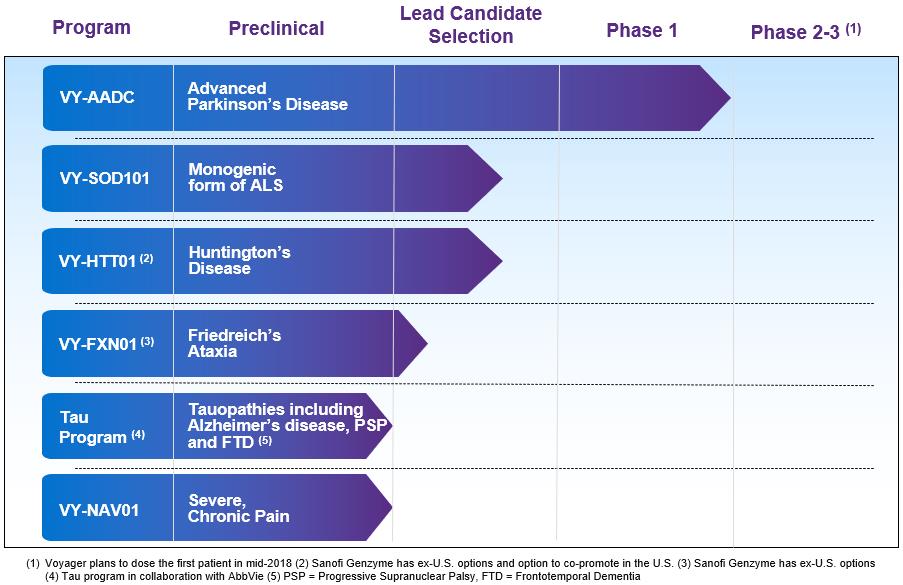
The company’s pipeline consists of six programs for severe neurological indications, including advanced Parkinson’s disease; a monogenic form of amyotrophic lateral sclerosis, or ALS; Huntington’s disease; Friedreich’s ataxia; tau-related diseases including Alzheimer’s disease, frontotemporal dementia, and progressive supranuclear palsy; and severe, chronic pain. Our product candidates may be eligible for orphan drug designation, breakthrough therapy designation, or other expedited review processes in the U.S., Europe, or Japan.
Our most advanced clinical candidate, VY-AADC for the treatment of advanced Parkinson’s disease, is being evaluated in an open-label, Phase 1b clinical trial. Preliminary data from Cohorts 1 through 3 from this trial were reported beginning in late 2016 and most recently in March 2018. In December 2017, we submitted an investigational new drug, or IND, application to the U.S. Food and Drug Administration, or FDA, for VY-AADC for the vector produced using our baculovirus/Sf9 system, as opposed to the vector manufactured using human embryonic kidney, or HEK293, cells which we have used in prior clinical trials including the ongoing Phase 1b clinical trial. This IND, which has subsequently become effective, allows us to initiate clinical trials and to begin screening and dosing patients in our planned pivotal Phase 2-3 clinical program. Clinical trial sites have been identified, and we plan to dose the first patient in this pivotal Phase 2-3 clinical program for advanced Parkinson’s disease in mid-2018. In 2018, the FDA granted fast track designation to VY-AADC.
During 2017, we dosed seven patients in a separate Phase 1 clinical trial designed to optimize the intracranial delivery of VY-AADC. This Phase 1 clinical trial explores a posterior, or back of the head, delivery approach into the putamen, compared to a transfrontal, or top of the head, delivery approach used in Cohorts 1 through 3 of the ongoing Phase 1b clinical trial. A posterior approach better aligns the infusion of VY-AADC with the anatomical structure of the putamen to potentially reduce the total procedure time and increase the total coverage of the putamen. Administration of VY-AADC with this posterior approach was well-tolerated with no reported serious adverse events, or SAEs, with most patients discharged from the hospital the day after surgery. This trial utilized the same dose concentration as Cohort 3 of
5
our Phase 1b clinical trial at a higher volume. The posterior approach was associated with greater average putaminal coverage (approximately 50%) and reduced average administration times compared with the transfrontal approach.
We are pursuing additional product candidates in the preclinical stages of development, including treatment programs for ALS, Huntington’s disease, Friedreich’s ataxia, tau-related neurodegenerative diseases and the treatment of severe, chronic pain. We plan to file two INDs from our ALS, Huntington’s disease and Friedreich’s ataxia programs during 2019. In late 2017, we initiated additional preclinical studies to further optimize our ALS program’s therapeutic approach, including exploration of additional routes of administration and novel AAV capsids in large animal models. Additionally, in 2017, we selected VY-HTT01 as our clinical candidate for the treatment of Huntington’s disease. Further optimization of routes of administration is underway to support filing of an IND application. We have begun additional preclinical studies to identify a lead clinical candidate for the treatment of Friedreich’s ataxia, with a goal of identifying a lead candidate during the second-half of 2018. In February 2018, we announced a global, strategic collaboration with AbbVie Biotechnology Ltd, or AbbVie, to develop potential new gene therapies consisting of vectors to deliver monoclonal antibodies to the brain directed against tau for Alzheimer’s disease and other tau-related neurodegenerative diseases, as described further below. We are conducting proof-of-concept studies on our VY-NAV01 program for the treatment of severe, chronic pain. Additionally, we continue to evaluate additional severe neurological diseases that could be treated using AAV gene therapy through application of either a gene replacement or a gene knockdown approach. Beyond these approaches, we are also actively exploring additional potential treatment methods that can utilize an AAV vector, including gene editing to correct or delete a gene in the cell genome.
Sanofi Genzyme Collaboration
In February 2015, we entered into a strategic collaboration with Sanofi Genzyme to leverage our combined expertise and assets to develop AAV gene therapies for certain severe neurological diseases. Under the agreement, we received $65.0 million in upfront cash, a $30.0 million upfront equity investment, and an in-kind commitment of $5.0 million, totaling $100.0 million. At the inception of the agreement, we were eligible to receive up to $745.0 million in option and milestone payments while retaining U.S. commercial rights to most programs. Under the terms of the collaboration, we granted Sanofi Genzyme an exclusive option (i) to license, develop and commercialize ex-U.S. rights to the VY-AADC program, VY-FXN01, VY-HTT01, and a future program to be designated by Sanofi Genzyme, which we refer to collectively as the Split Territory Programs; (ii) to license, develop and commercialize worldwide rights to VY-SMN101; and (iii) to co-commercialize VY-HTT01 in the United States. Each of Sanofi Genzyme’s options to a Split Territory Program is triggered following the completion of the first proof-of-principle human clinical study, or POP Study, on a program-by-program basis.
In October 2017, Sanofi Genzyme notified us that it had decided not to exercise its option for the ex-U.S. rights to VY-AADC for advanced Parkinson’s disease. As a result, we now possess global rights to VY-AADC and are no longer entitled to receive $45.0 million and $60.0 million of regulatory and commercial milestone payments, respectively, related to the Parkinson’s program. If we use certain Sanofi Genzyme technology in VY-AADC, Sanofi Genzyme is entitled to receive low-single digit royalty payments based on a percentage of net sales by us, and we may be obligated to make certain regulatory milestone payments to a third-party licensor.
AbbVie Collaboration
In February 2018, we entered into an exclusive collaboration and option agreement with AbbVie for the research, development, and commercialization of AAV and other virus-based gene therapy products for the treatment of diseases of the central nervous system and other neurodegenerative diseases related to defective or excess aggregation of tau protein in the human brain, including Alzheimer’s disease. Under the terms of the agreement, we received an upfront payment of $69.0 million and may receive future development and regulatory milestone payments and royalties. Under the terms of the agreement, we will perform specified research, preclinical, and Phase 1 development activities regarding vectorized antibodies directed against tau, after which AbbVie may select one or more vectorized antibodies to proceed into IND-enabling studies and clinical development. We will be responsible for the research, IND-enabling studies, and Phase 1 clinical trial activities and costs. Following the completion of Phase 1 clinical development, AbbVie has an option to license the vectorized tau antibody program and would then lead further clinical development and global commercialization for the product candidates pursuant to the agreement. We have an option to share in the costs of
6
clinical development for higher royalty rates. In addition to the upfront payment and the potential option exercise payments, we are eligible to receive up to $895.0 million in development and regulatory milestones for each vectorized tau antibody compound. We are also eligible to receive tiered, escalating royalties in a range, subject to certain specified exceptions, from a high-single digit to a mid-to-high teen percentage of the global net sales of the vectorized antibodies for tauopathies, including Alzheimer’s disease and other neurodegenerative diseases. Under the terms of the agreement, each party will own the entire right, title and interest in and to all know-how and patent rights first made or invented solely by it or its affiliates or its or their sublicensees in the course of the collaboration, with certain specified exceptions. We have also agreed to grant AbbVie a worldwide license to certain know-how and patent rights developed by us or jointly by the parties arising from the collaboration.
Mission and Strategy
Our mission is to become the world leader in AAV gene therapy focused on treating severe neurological diseases by developing transformative therapies. Our strategy to achieve this mission is to:
Cohorts 1 through 3 employed a transfrontal trajectory of VY-AADC into the putamen. To further optimize intracranial delivery, we enrolled seven patients in a separate Phase 1 trial exploring a posterior trajectory in 2017. A posterior trajectory better aligns the infusion of VY-AADC with the anatomical structure of the putamen to potentially reduce the total procedure time and increase total coverage of the putamen. This trial utilized the same dose concentration as Cohort 3 of our Phase 1b clinical trial at a higher volume, yielding a total dose of 4.5×1012 vg of VY-AADC. Preliminary results of this clinical trial suggest the posterior approach has resulted in greater average coverage (approximately 50%) and has reduced average administration times compared with the transfrontal approach of Cohorts 1 through 3 in the Phase 1b clinical trial. No serious adverse events have been reported, and most patients were discharged from the hospital the day after surgery. Despite the differences in dose concentration and volume, we expect data from these trials will help inform the design of the double-blind, placebo-controlled Phase 2 arm of the pivotal Phase 2-3 clinical program.
|
· |
Build and advance a pipeline of gene therapy programs focused on severe neurological diseases. Beyond our clinical-stage program for advanced Parkinson’s disease, we have a deep pipeline of AAV gene therapy programs in various stages of preclinical development. We plan to file two additional INDs for our preclinical programs in 2019. We believe that our leadership position in AAV gene therapy for severe neurological diseases and our product engine provide us with the necessary capabilities to evaluate and capitalize on external opportunities. As such, we plan to opportunistically expand our pipeline through acquisition, in-licensing or other strategic transactions. |
|
· |
Continually invest in our AAV product engine. We plan to continually invest in our product engine to maintain our leadership in AAV gene therapy for neurological diseases. Specifically, we intend to further |
7
develop and enhance our product engine by focusing on (i) vector engineering and optimization; (ii) manufacturing; and (iii) dosing and delivery techniques. We plan to continue generating novel AAV vectors by engineering and optimizing vectors best suited to a targeted disease. We have built an onsite, state-of-the-art process research and development facility to enable the manufacturing of high quality AAV gene therapy vectors at laboratory scale. We expect to utilize established and novel techniques for dosing and delivery of our AAV gene therapies to the central nervous system, or CNS. |
|
· |
Establish a leadership position in commercial-scale, high quality AAV manufacturing. We believe that manufacturing capacity and expertise are critical to successfully treating patients using gene therapy. Through one of our collaborations, with MassBiologics, an FDA-licensed manufacturer affiliated with the University of Massachusetts Medical School, we are establishing a commercial-scale current good manufacturing practice, or cGMP, compliant manufacturing capability. We initiated cGMP production activities at MassBiologics in late 2016. We have also established contract manufacturing relationships with third-party service providers that specialize in gene therapy and AAV vectors. We are using the baculovirus/Sf9 AAV production system, a technology for producing AAV vectors at scale in insect-derived cells, originally invented and developed by several current and former members of our production team while at the National Institutes of Health, or NIH, which we continue to improve upon. We believe that having oversight through these key relationships over our own commercial manufacturing process is critical to ensuring quality product with commercial yields. |
|
· |
Expand our intellectual property portfolio. We seek to have an industry leading intellectual property portfolio. To that end, we seek patent rights for various aspects of our programs, including vector engineering and construct design, our production process, and all features of our clinical products including compositions and methods of delivery. We expect to continue to expand our intellectual property portfolio by aggressively seeking patent rights for promising aspects of our product engine and product candidates. |
AAV Gene Therapy for Neurological Diseases
Gene therapy is an approach whereby gene expression is directly altered in patients to address the underlying cause or predominant manifestations of disease. We believe that the targeted nature of gene therapy may enable powerful treatment options, and provide these patients with meaningful and durable benefits.
While AAV gene therapy can potentially be harnessed for multiple treatment methods, we are currently focused on gene replacement and gene knockdown approaches. Gene replacement is intended to restore the expression of a protein that is not expressed, expressed at abnormally low levels or functionally mutated with loss of function. Gene knockdown, or gene silencing, is intended to reduce the expression of a pathologically mutated protein that has detrimental effects.
8
Our gene therapy approach uses AAV vectors which we believe are ideal vectors for gene therapy for several reasons:
Broad Applicability. AAV is able to transduce, or transfer a therapeutic gene, into numerous cell types including target cells in the CNS.
Safety. AAV is believed to be safe and is not known to cause any disease in humans. No vector-related SAEs have been reported in the more than 1,500 patients, including over 200 patients for neurological indications, treated with AAV gene therapy to date.
Does Not Readily Integrate. AAV does not readily integrate into the genome of the target cell, reducing the potential for oncogenesis, or the induction of cancer.
Scalability. AAV is able to be manufactured at commercial quality and scale.
We believe that neurological diseases are well-suited for treatment with AAV gene therapy for the following reasons:
Validated Targets. Many neurological diseases are caused by well-defined mutations in genes and these genes represent genetically validated drug targets for AAV gene therapy.
Targeted Delivery. Advances in delivery techniques allow for direct delivery of AAV vectors to discrete regions in the brain or broader delivery throughout the spinal cord via the cerebrospinal fluid, or CSF.
Durable Expression. Long-term gene expression may be achievable in the CNS following one-time dosing and transfer of the therapeutic gene with an AAV vector. Neurons in the CNS are terminally differentiated, or no longer divide, eliminating the potential for cell division to dilute expression of the therapeutic gene. Repeated or continual dosing with direct injection of drugs into the CNS is complex, therefore a one-time AAV gene therapy has significant advantages.
Immune Privileged Site. There is a reduced risk of harmful immune response or reduced efficacy due to localized delivery in a self-contained system.
While we are currently focused on gene replacement and gene knockdown approaches, we are also actively exploring additional potential treatment methods that can utilize an AAV vector, including the direct delivery of monoclonal antibodies to the CNS (such as in our collaboration with AbbVie on neurodegenerative diseases related to defective or excess aggregation of tau protein in the brain), as well as gene editing to correct or delete a gene in the cell genome.
The Voyager Product Engine
We have built a product engine that we believe positions us to be the leading company at the intersection of AAV gene therapy and severe neurological diseases. Our team of experts in the fields of AAV gene therapy and neuroscience first identifies and selects severe neurological diseases that are well-suited for treatment using AAV gene therapy. We then engineer and optimize AAV vectors for delivery of the virus payload to the targeted tissue or cells. Finally, we leverage established routes of administration and advances in dosing techniques to optimize delivery of our AAV gene therapies to target cells that are critical to the disease of interest either directly to discrete regions of the brain, or, more broadly, to the spinal cord region. We believe that optimizing each of these parameters is a key factor for overall program success. We expect that our current and future pipeline programs will make use of technological advances generated with our product engine.
9
Disease Selection
We assess potential product programs based upon the following criteria:
Unmet Need. There is a significant unmet medical need for the indication and substantial commercial potential.
Target Validation. There is strong evidence that expression of a specific gene, or lack thereof, is causing, or critical to, the disease state.
Delivery Using AAV. There is strong evidence supporting the ability to target the relevant tissue and cells using an AAV vector to achieve sufficient target gene expression.
Clinical Readouts. The clinical impact of an AAV gene therapy can be clearly measured, including through well-accepted clinical endpoints and the use of both existing and novel biomarkers.
Scalability of Manufacturing. Sufficient AAV vector to supply late-stage clinical development and commercialization can be manufactured.
In addition to the criteria above, we also look for groups of diseases where our knowledge can be transferred. For instance, we believe that some of the delivery parameters and imaging techniques that are employed in our VY-AADC program can be applied to AAV gene therapy delivery for Huntington’s disease or other diseases where direct, targeted delivery to the brain is warranted.
Vector Engineering and Optimization
We have advanced or intend to advance our multiple preclinical programs towards selection of lead clinical candidates using AAV vectors that we believe are best suited for each of our programs either through use of our existing capsids, through exercising a non-exclusive worldwide commercial license to capsid sequences covered by third parties, or by engineering or optimizing novel capsids. The key components of an AAV vector include: (i) the capsid, which includes the promoter and the therapeutic gene; (ii) the therapeutic gene, or transgene; and (iii) the promoter, or the DNA sequence that drives the expression of the transgene.
Members of our team have co-discovered many of the known naturally occurring AAV capsids and have also created promising genetically engineered AAV capsids. Genetically engineered capsids have yielded vectors with desirable properties, such as higher biological potency and enhanced tissue specificity. We believe that there is an opportunity to further optimize AAV capsids to confer desired characteristics relating to properties such as tissue specificity and immunogenicity. We have a significant effort dedicated to designing and screening for novel AAV capsids using a number of different scientific approaches. We believe that the information generated by this work will enhance our ability to rationally design AAV capsids with specific properties for particular therapeutic applications. In September 2016, we announced a co-exclusive worldwide license agreement with the California Institute of Technology, or Caltech, related to novel AAV capsids. The license agreement covers all fields of use and includes novel AAV capsids that have demonstrated enhanced blood-brain barrier penetration for the potential treatment of neurological diseases following systemic administration of an AAV gene therapy vector.
With respect to the target DNA delivered through AAV gene therapy, we are selecting promoters that we believe have the appropriate activity and tissue, selectively for our specific gene therapy programs. We are also designing transgenes to provide optimal expression once delivered to the targeted cells.
Manufacturing at Commercial Quality and Scale
The ability to produce high quality AAV vectors at commercial-scale is a critical success factor in AAV gene therapy. While at the NIH, current and former members of our production team invented and developed a
10
baculovirus/Sf9 AAV production system, which we use and have continued to improve. This system has a number of attributes that we believe will enable high quality commercial-scale manufacturing, including:
High Yield. A single manufacturing run at 500-liter scale can yield many thousands of doses of an AAV gene therapy.
High Purity. A relatively high percentage of AAV vectors contain the therapeutic DNA, reducing the number of empty capsids compared to alternative manufacturing approaches. In addition, the baculovirus/Sf9 system eliminates the risk of introducing mammalian cell derived impurities.
Scalability. This process has been reproduced at volumes ranging from 0.02 liters to 250 liters. We believe the existing process is scalable to substantially higher volumes.
We have built a state-of-the-art process research and development production facility for manufacturing research-grade AAV vectors onsite at our Cambridge, Massachusetts headquarters and a cGMP, commercial-scale AAV manufacturing capability through our collaboration with MassBiologics, in Fall River, Massachusetts, both of which employ our baculovirus/Sf9 production system. We have also established a contract manufacturing relationship with other companies specializing in the manufacture of gene therapy and AAV vectors.
Optimized Delivery and Route of Administration
Identifying the optimal route of administration and delivery parameters for AAV gene therapy, such as infusion volume, flow rate, vector concentration and dose and formulation for a specific disease, are critical to achieving safe and effective levels of transgene expression in the targeted location in the CNS. We aim to develop clinically feasible protocols that yield reproducible results across patients. For our advanced Parkinson’s disease and Huntington’s disease programs, we are pursuing direct injection into the brain, called intraparenchymal injection. For our ALS SOD1 and Friedreich’s ataxia programs, we are evaluating multiple routes of administration including injection into the CSF within the cerebrospinal space, called intrathecal injection, as well as intravenous injection and other delivery alternatives.
VTAGTM Intraparenchymal Injection to the Brain
The surgical approach that we are using for VY-AADC is similar, in some respects, to the stereotactic approach used for deep brain stimulation, or DBS, a marketed device-based treatment for advanced Parkinson’s disease. One primary difference with our approach is the ability to assist the physician in visualizing the delivery of VY-AADC to the putamen using real-time, intra-operative, magnetic resonance imaging, or MRI, to avoid specific blood vessels to reduce the risk of potential hemorrhages during the surgical procedure and to maximize the coverage of the putamen.
Investigators in the Phase 1b clinical trial of VY-AADC and the separate Phase 1 posterior trajectory trial use the real-time, intra-operative, MRI system called the ClearPoint System® from MRI Interventions, Inc. However, not all neuro-surgical units within the United States utilize this system and may employ other neuro-navigational systems that are not compatible with real-time MRI imaging.
Consequently, we are developing the Voyager Trajectory Array Guide, or V-TAG™, as our own device for use as a real-time, intra-operative, MRI-compatible device that can be used with other neuro-navigational systems for this and other surgical procedures. We plan to file an application for 510(k) clearance with the FDA in the first half of 2018. We believe that our experience gained from our VY-AADC program, including the use of V-TAG, can be applied to AAV gene therapy delivery for our Huntington’s disease program and possibly other projects as well.
11
Overview of Intraparenchymal Delivery
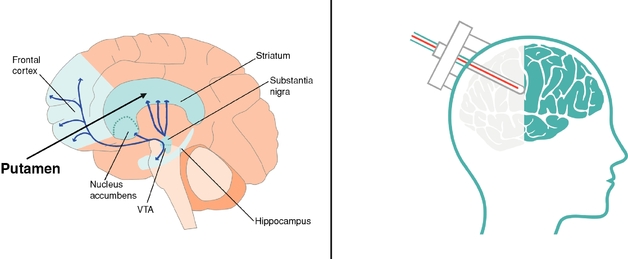
Courtesy of: Okinawa Institute of Science and Technology.
Overview of Our Pipeline
We have leveraged our product engine to assemble a pipeline of novel AAV gene therapies for the treatment of severe neurological diseases with high unmet medical need. Depending on the disease, our current AAV gene therapies will use either a gene replacement or gene knockdown approach. Our goal is to address the underlying cause or the predominant manifestations of a specific disease by significantly increasing or decreasing expression of the relevant proteins at targeted sites within the CNS.
Advanced Parkinson’s Disease Program: VY-AADC
Disease Overview
Parkinson’s disease is a chronic, progressive and debilitating neurodegenerative disease that affects approximately 1,000,000 people in the United States and seven to 10 million people worldwide. It is estimated that up to 15% of the prevalent population with Parkinson’s disease, or approximately 150,000 patients in the U.S., have motor fluctuations that are refractory, or not well-controlled, with levodopa, the current standard of care. While the underlying cause of Parkinson’s disease in most patients is unknown, the motor symptoms of the disease arise from a loss of neurons in the midbrain that produce the neurotransmitter dopamine. Declining levels of dopamine in this particular region of the brain leads to the motor symptoms associated with Parkinson’s disease including tremors, slow movement or loss of movement, rigidity, and postural instability. Motor symptoms during the advanced stages of the disease include falling, gait freezing, and difficulty with speech and swallowing, with patients often requiring the daily assistance of a caregiver.
While symptomatic treatments exist, there are currently no therapies that effectively slow or reverse the progression of Parkinson’s disease. Levodopa, also known as L-Dopa, remains the standard of care treatment, with its beneficial effects on symptom control having been discovered over 40 years ago. Patients are generally well-controlled with oral levodopa in the early stages of the disease but become less responsive to treatment as the disease progresses. Patients experience longer periods of reduced mobility and stiffness termed off-time, or the time when medication is no longer providing benefit, and shorter periods of on-time when their medication is effective.
12
The progressive motor symptoms of Parkinson’s disease are largely due to the death of dopamine neurons in the substantia nigra, a part of the midbrain that converts levodopa to dopamine, in a single step catalyzed by the enzyme AADC. Neurons in the substantia nigra release dopamine into the putamen where the receptors for dopamine reside. In advanced Parkinson’s disease, neurons in the substantia nigra degenerate and the enzyme AADC is markedly reduced in the putamen, which limits the brain’s ability to convert oral levodopa to dopamine. The intrinsic neurons in the putamen, however, do not degenerate in Parkinson’s disease. VY-AADC, comprised of the AAV2 capsid and a cytomegalovirus promoter to drive AADC transgene expression, is designed to deliver the AADC gene directly into neurons of the putamen where dopamine receptors are located, bypassing the substantia nigra neurons and enabling the neurons of the putamen to express the AADC enzyme to convert levodopa into dopamine. The approach with VY-AADC, therefore, has the potential to durably enhance the conversion of levodopa to dopamine and provide clinically meaningful improvements in motor symptoms following a single administration.
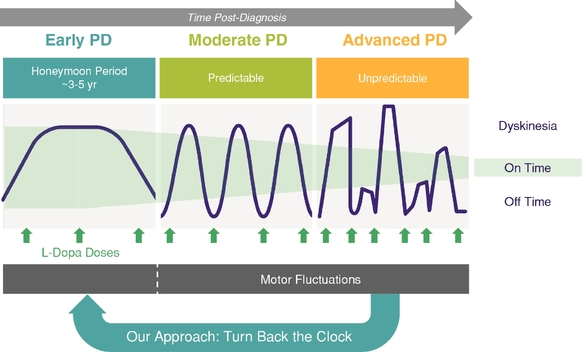
The Unified Parkinson’s Disease Rating Scale, or UPDRS, is a standard clinical rating scale for Parkinson’s disease. Part III of this scale measures motor function by physician examination. The UPDRS is conducted when patients are taking their Parkinson’s disease medications (referred to as “on” medication) and when patients are not taking their Parkinson’s disease medications (referred to as “off” medication). In addition, a patient-completed Hauser, diary records the patient’s motor response over the course of several days as on-time, or time when they have good mobility with or without non-troublesome dyskinesia, or uncontrolled, involuntary movement; off-time when they have poor mobility; and on-time with troublesome dyskinesia when they have uncontrolled movements. As shown in the figure below, diary on-time decreases, while off-time and dyskinesias increase as patients progress from the early honeymoon period into later stages of advanced Parkinson’s disease.
While L-Dopa and other pharmacological approaches to augmenting dopamine provide symptomatic benefit during the early stages of Parkinson’s disease, there are relatively limited treatment options for patients with advanced Parkinson’s disease. There are two FDA-approved therapies used to specifically treat advanced Parkinson’s disease patients with medically refractive motor fluctuations. The first, DBS, requires the implantation of an electrical stimulation device in the body, which is connected to electrodes that are placed into the brain during neurosurgery where the patient must stay awake during the procedure. The second, marketed as DUODOPA in Europe and DUOPA in the United States, requires the surgical placement of a tube into the intestine so that medication is delivered by a pump that resides outside the body, which patients must carry with them.
We believe that the need for indwelling hardware, being awake during surgery, and the maintenance associated with each of these approaches are significant deterrents for many potential patients. Given the size of the addressable patient population with advanced Parkinson’s disease and the limitations of the currently available treatment options for these patients, we believe that a significant unmet medical need exists for new treatment options.
Our Treatment Approach: “Turn Back the Clock”
We are developing VY-AADC, an AAV gene therapy product candidate, for the treatment of advanced Parkinson’s disease. VY-AADC is comprised of the AAV2 capsid, which has been used in multiple AAV gene therapy clinical trials for a number of different diseases, and the cytomegalovirus promoter that drives expression of the AADC transgene. VY-AADC is intended to deliver the AADC gene directly into the putamen. Our approach bypasses the dying neurons of the substantia nigra, allowing for the conversion of levodopa into dopamine within the putamen. We believe that our approach has the potential to provide patients with clinically meaningful improvements in motor symptoms following a single administration.
Our goal is to restore patients’ responsiveness to levodopa following treatment with VY-AADC to “turn back the clock” on their disease such that the patients’ motor symptoms are returned to a well-controlled state, consistent with the level of symptomatic benefit achieved from levodopa during the early honeymoon period. Following treatment with VY-AADC, patients with advanced Parkinson’s disease will continue to take levodopa, but we believe that the required dose will be reduced. The continued administration of levodopa will provide a means to titrate dopamine production to further optimize symptomatic control. We believe our approach will increase the conversion of dopamine from levodopa in the putamen, resulting in a clinically meaningful improvement in motor symptoms following a single administration.
13
Overview of Progression of Parkinson’s Disease (PD)
Preclinical Studies
Preclinical studies conducted by Krystof Bankiewicz, M.D., Ph.D., one of our co-founders, and his colleagues at the University of California San Francisco, or UCSF, evaluated the safety, efficacy and pharmacological activity of AAV2-AADC gene therapy, a gene therapy substantially similar to VY-AADC, delivered directly to the putamen in a non-human primate model of Parkinson’s disease. Overall, the procedure and vector were well-tolerated with no serious toxicity issues.
Positron emission tomography, or PET, imaging with tracers specific for AADC activity demonstrated a significant and sustained increase of activity in the brain region where the vector had been delivered. Increased responsiveness to levodopa was also evidenced by significant behavioral improvements observed post-treatment with the gene therapy compared to pre-treatment. In five animals, the mean improvement in behavior was determined at various doses of levodopa both one month before treatment, as a baseline measure for comparison purposes, and then again six months after treatment. A strong PET signal was observed in all five animals following treatment, confirming delivery of AADC into the putamen. Animals were significantly more sensitive to levodopa six months following treatment with the gene therapy when compared to baseline, as shown below.
14
Behavioral Response to Various Doses of levodopa Pre- and Post-Treatment with AAV2-AADC in Non-Human Primates(1)
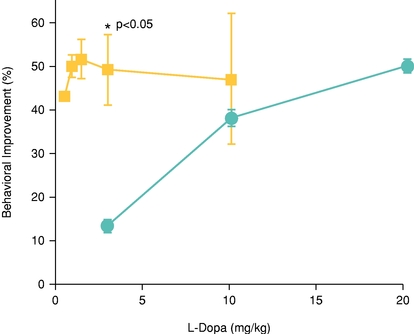
(1) Adapted by permission from Macmillan Publishers Ltd; Forsayeth et al, Molecular Therapy (2006), 14 (4); 571‑577, copyright 2006. Blue line represents base line measurements and yellow line represents six months post-treatment measurements.
* A result is considered to be statistically significant when the probability of the result occurring by random chance, rather than from the efficacy of the treatment, is sufficiently low. The conventional method for measuring the statistical significance of a result is known as the “p‑value,” which represents the probability that chance caused the result (e.g., a p-value = 0.001 means that there is a 0.1% or less probability that the difference between the control group and the treatment group is purely due to random chance).
We believe that these results provide evidence that AADC is active and being expressed at levels sufficient to measure a clinical benefit. Two animals from this cohort were followed for up to eight years following a single administration of the gene therapy and sustained PET imaging signals for AADC and behavioral signs of efficacy were observed in these animals.
The results of these preclinical studies provided support for the initiation of clinical trials.
Previous Phase 1 Clinical Trials
In a completed open-label Phase 1 clinical trial conducted at UCSF, VY-AADC was delivered directly to the putamen of Parkinson’s disease patients. The primary endpoints of this trial were safety and tolerability of VY-AADC. These endpoints were met as VY-AADC was well-tolerated and no treatment related SAEs were reported. Furthermore, pharmacologic activity of VY-AADC was observed. This trial was completed prior to our involvement in the program.
The Phase 1 clinical trial at UCSF was conducted in a total of 10 patients with advanced Parkinson’s disease. Two doses of VY-AADC were tested, 9×1010 vg and 3×1011 vg, with five patients per dose cohort. The infusion volume was 100µl per putamen, or 200µl per patient. Patients in both cohorts treated with VY-AADC showed modest improvements in motor fluctuations. At six months following treatment, diary off-time was observed to be reduced by an average of approximately three hours and a corresponding increase in diary on-time without dyskinesias was also observed. In addition, at six months following treatment, an approximately 30% improvement in on-medication and off-medication measures using the Total UPDRS score, a widely used rating scale that evaluates cognitive, functional, and motor deficits, as well as medication-related complications, was observed, as shown in the table below.
15
Summary of UPDRS Results from Phase 1 Trial(1)
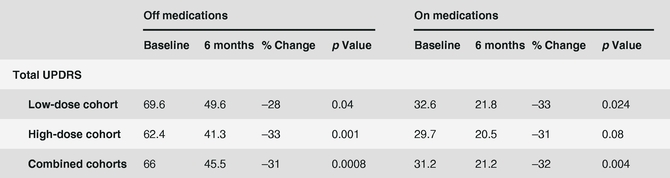
(1) Christine et al, Neurology (2009), 73: 1662-1669. The row titled “Low-dose cohort” represents data from the five patients treated with 9 X 1010 vg of VY-AADC01. The row titled “High-dose cohort” represents data from the five patients treated with 3 X 1011 vg of VY-AADC01. The row titled “Combined cohorts” represents data from all ten patients treated with VY-AADC01. The data in the columns under the header “Off medications” represents periods during which patients’ medications were not working as measured by a patient’s total UPDRS score at baseline, before treatment with VY-AADC01, and at six months following treatment with VY-AADC01, along with percent change from baseline to six months and the corresponding p-value. The data in the columns under the header “On medications” represents periods during which patients’ medications were working as measured by a patient’s total UPDRS score at baseline, before treatment with VY-AADC01 and at six months following treatment with VY-AADC01, along with percent change from baseline to six months and the corresponding p-value. A result is considered to be statistically significant when the probability of the result occurring by random chance, rather than from the efficacy of the treatment, is sufficiently low. The conventional method for measuring the statistical significance of a result is known as the “p‑value,” which represents the probability that chance caused the result (e.g., a p-value = 0.001 means that there is a 0.1% or less probability that the difference between the control group and the treatment group is purely due to random chance). Because of the small size of this trial, the p-values may not be reliable or repeatable, and may not be duplicated in future trials.
While no gene therapy related SAEs were reported, three patients experienced minor hemorrhages related to the surgical procedure. Two of the hemorrhages were asymptomatic, noticed only on imaging, and one was symptomatic with the patient making an almost complete recovery. Nevertheless, the stereotactic injection protocol used in the surgical procedure was modified to avoid specific blood vessels and no further hemorrhages were reported. The implementation of real-time, intra-operative MRI guidance in the ongoing Phase 1b clinical trial is a significant advancement in vector delivery.
The 10 patients were assessed clinically for up to four years after treatment and a durable, dose-dependent expression of AADC was observed. Patients treated with the low dose gene therapy were observed to have an increased PET signal, or uptake of the fluoro-meta-tyrosine tracer indicative of AADC expression and activity that persisted for up to four years. Patients treated with the high dose gene therapy were observed to have an increased PET signal that was greater on average when compared to the low dose cohort, which also persisted for up to four years.
16
Long-Term AADC Expression as Measured by PET Imaging in Patients Treated with High and Low Doses of AAV Gene Therapy in a Previous Phase 1 Clinical Trial (1)
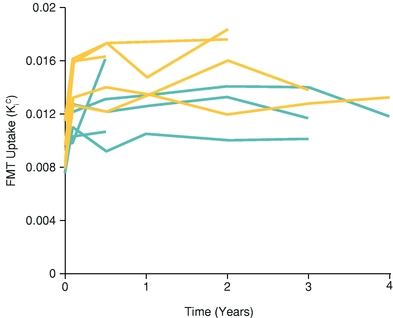
(1) Mittermeyer et al, Human Gene Therapy (2012), 23: 377-381. The publisher for this copyrighted material is Mary Ann Liebert, Inc. publishers. Blue lines represent patients treated with the low dose and yellow lines represent patients treated with the high dose.
A similar Phase 1 clinical trial was conducted at Jichi Medical University, or JMU, in Japan using the same vector that was used in the UCSF trial. The primary endpoints of this trial were safety and tolerability of the treatment. These endpoints were met as the treatment was well-tolerated and no treatment related SAEs were reported. Six patients were treated in this trial and an enhanced PET signal was observed in a subset of patients monitored 96 weeks following treatment. Patients remain in follow up in an open-label Phase 1/2 trial currently being conducted at JMU. The primary endpoints of this trial are safety and tolerability of the treatment. This trial is using lower infusion volumes and doses compared to the ongoing Phase 1b trial. Importantly, the JMU trial is not using real-time, intra-operative MRI guidance.
While the prior UCSF and JMU clinical results were encouraging and provided evidence of long-term AADC expression, the magnitude of the clinical benefits observed did not exceed placebo effects observed in previous surgical therapy trials in Parkinson’s disease patients, and the UCSF and JMU trials were not blinded. Further, based on post-operative imaging and our current work using real-time, intra-operative MRI monitoring, we estimate that less than 10% of the putamen volume was covered by the infusion in these trials, which reflects suboptimal distribution of VY-AADC in the putamen. We believe that there is an opportunity to further optimize the delivery, dose and infusion volume of VY-AADC to substantially increase the coverage of the putamen in order to achieve a more substantial clinical benefit.
Voyager VY-AADC Phase 1b Program Status
In 2014, UCSF initiated an open-label Phase 1b clinical trial to optimize the development of VY-AADC. The IND for the Phase 1b trial was filed by UCSF in July 2013 and was transferred to us in October 2015. The primary endpoints of this trial are safety and tolerability of the treatment. This trial incorporates three key design features:
|
· |
Use of real-time, intra-operative MRI system during surgery to assist the physician in visualizing the delivery of VY-AADC to the putamen and to avoid specific blood vessels during the surgical procedure, with the goal of reducing the risk of hemorrhages. |
17
|
· |
Larger infusion volumes designed to increase coverage of the putamen with VY-AADC. |
|
· |
Higher concentrations of VY-AADC vector compared to the previously completed UCSF Phase 1 trial. |
Secondary endpoints of this trial, which are being used to assess the potential pharmacologic activity of VY-AADC, include UPDRS, AADC PET imaging and a behavioral test using intravenous levodopa treatment to measure changes in a patients’ sensitivity to levodopa as well as endpoints to measure motor functions.
In March 2018, we updated interim results from the ongoing, open-label Phase 1b clinical trial of VY-AADC for the treatment of advanced Parkinson’s disease. The trial includes 15 patients with advanced Parkinson’s disease and disabling motor fluctuations, treated with a single administration of VY-AADC to assess the safety and distribution of ascending doses of VY-AADC administered under magnetic resonance imaging, or MRI, guidance to the putamen, a region of the brain associated with impaired motor function in Parkinson’s disease. Secondary objectives include assessment of aromatic L-amino acid decarboxylase, or AADC, expression and activity in the putamen measured by F-Dopa positron emission tomography, which we refer to as a F-Dopa PET scan, that reflects the capacity to convert levodopa to dopamine. Other secondary measures include assessments of motor function and activities of daily living, as measured by the Unified Parkinson’s Disease Rating Scale, which we refer to as UPDRS-III and UPDRS-II, respectively; quality of life; and a patient-completed Hauser diary.
The March 2018, interim results include data from all 15 patients treated in Cohorts 1, 2 and 3 (five patients in each Cohort) including data from patients in Cohort 1 at three years, Cohort 2 at 18 months and Cohort 3 at one year. Cohort 1 patients received a single administration of VY-AADC at a concentration of 8.3×1011 vgs per milliliter, or vg/ml, using an infusion volume of up to 450 µL per putamen, or up to 900 µL per patient, for a total dose of 7.5×1011 vg. Cohort 2 patients received a single administration of VY-AADC at a concentration of 8.3×1011 vg/ml, using an infusion volume of up to 900 µL per putamen, or up to 1,800 µL per patient, for a total dose of 1.5×1012 vg. Cohort 3 patients received similar infusion volumes (up to 900 µL per putamen) of VY-AADC to Cohort 2 but at three-fold higher vg concentrations for a total dose of up to 4.5×1012 vg.
Key findings from this trial to date include:
|
· |
The use of real-time, MRI-guided delivery and increasing infusion volumes resulted in progressively greater coverage of the putamen, from 21% mean coverage of the volume of the putamen with VY-AADC in Cohort 1, 34% mean coverage in Cohort 2, and 42% mean coverage in Cohort 3. |
|
· |
VY-AADC treatment resulted in a 13% increase, a 56% increase, and a 79% increase in mean putaminal AADC enzyme activity in Cohort 1, 2, and 3, respectively, at six months relative to baseline as measured by F-Dopa PET scan. Coverage of the putamen and AADC enzyme activity were highly correlated (r=0.84, p=0.0002). |
|
· |
VY-AADC treatment resulted in reduced daily doses of oral levodopa and related medications to achieve optimal motor control, suggesting a greater capacity for patients to make more dopamine but with less need for oral levodopa. Patients’ Parkinson’s medications were reduced by a mean of 208 mg (14%), 553 mg (34%) and 618 mg (42%) for Cohorts 1, 2 and 3, respectively, at six months compared with baseline. LED reductions were sustained for Cohorts 1 and 2 to eighteen months and for Cohort 3 to 12 months. |
Patients enrolled in Cohorts 1, 2 and 3 were:
|
· |
On average, 58 years of age with a Parkinson’s disease diagnosis for an average of 10 years. |
|
· |
Candidates for surgical intervention including deep-brain stimulation due to disabling motor complications despite treatment with optimal anti-Parkinsonian medication. |
|
· |
At baseline, the average patient diary on-time without troublesome dyskinesia was 10.5 hours, average UPDRS-III on medication score was 13.5, average diary off-time was 4.6 hours and average UPDRS-II activities of daily living off medication score was 16.5. Patients in Cohort 3 entered the trial with |
18
approximately 50% more severe dyskinesia at baseline than patients in Cohorts 1 and 2 based on the Unified Dyskinesia Rating Scale, with a mean score of 30.2 for Cohort 3 compared with a mean score of 19.2 and 17.4 for Cohorts 1 and 2, respectively. |
|
· |
At baseline, patients were treated with maximal levels of multiple dopaminergic medications including, in many cases, amantadine for the treatment of dyskinesia, or uncontrolled or involuntary movements. Patients’ average amount of Parkinson’s disease medications at baseline was 1,526 mg of oral levodopa equivalents per day. |
|
· |
During the trial, patients were instructed to reduce their daily doses of oral levodopa and related medications, or levodopa equivalent doses (LEDs), to achieve optimal motor control in response to severe dyskinesia observed post-treatment with VY-AADC. |
The results continue to demonstrate durable, dose-dependent and time-dependent improvements across multiple measures of patients’ motor function after a one-time administration of the gene therapy. These measures include patient-reported diaries, Parkinson’s disease rating scales, and quality of life, with diary on-time without troublesome dyskinesia at twelve months as the proposed primary endpoint of the planned pivotal program. The update of results from the ongoing Phase 1b trial of VY-AADC include a durable 2.1-hour improvement in patient-reported diary on-time without troublesome dyskinesia from baseline to three years for patients in Cohort 1, a durable and clinically meaningful 3.5-hour improvement from baseline to 18 months in Cohort 2, and an improvement from baseline to six months of 1.5 hours that plateaued from six to 12 months in Cohort 3. Cohort 3 patients had higher levels of severe dyskinesia at baseline than patients in Cohorts 1 and 2. This, coupled with treatment with a higher dose of VY-AADC, resulted in patients in Cohort 3 reducing their LEDs to a greater extent than patients in Cohorts 1 and 2 and may have resulted in less robust control of motor function as measured by on-time without troublesome dyskinesia compared to Cohort 2 by 12 months. We intend to apply these learnings to the protocols for the pivotal Phase 2-3 program.
VY-AADC also generated durable improvements in this trial in other measures of motor function including decreases in both diary off-time and diary on-time with troublesome dyskinesia and increases in both diary on-time without dyskinesia and diary on-time with non-troublesome dyskinesia. In Cohort 2 at 18 months, patients had a mean increase of 5.1 hours a day of on-time without any dyskinesia and experienced 65% less off-time.
In addition to motor function, VY-AADC improved patients’ quality of life as measured by the Unified Parkinson’s Disease Rating Scale (UPDRS) Part II activities of daily living section and the patient-reported 39-item Parkinson’s Disease Questionnaire (PDQ-39), demonstrating dose-dependent and clinically meaningful improvements in these scores. For PDQ-39, VY-AADC improved (reduced) patients’ score by a mean change from baseline to 12 months of -8.4 and -9.1 for Cohorts 2 and 3, respectively.
Infusions of VY-AADC have been well-tolerated in all fifteen patients treated in these Cohorts with no vector-related serious adverse events (SAEs). Fourteen of the 15 patients were discharged from the hospital within two days following surgery. As previously reported, one patient experienced two SAEs: a pulmonary embolism or blood clot in the lungs, and related heart arrhythmia or irregular heartbeat. The patient was treated with an anti-coagulant and symptoms associated with the SAEs have completely resolved. Investigators determined that this was most likely related to immobility during the administration and subsequent formation of a blood clot, or deep vein thrombosis (DVT), in the lower extremity. Consequently, DVT prophylaxis was added to the protocol and no subsequent events have been observed.
Voyager Phase 1 Posterior Trajectory Clinical Trial
During 2017, we dosed seven patients in a Phase 1 clinical trial designed to optimize the intracranial delivery of VY-AADC. This Phase 1 trial is exploring a posterior delivery approach of drug into the putamen, compared to a transfrontal delivery approach used in Cohorts 1 through 3 of the ongoing Phase 1b clinical trial. A posterior approach better aligns the infusion of VY-AADC with the anatomical structure of the putamen to potentially reduce the total procedure time and increase the total coverage of the putamen. Administration of VY-AADC with this posterior approach was well-tolerated with no reported serious adverse events, or SAEs, and most patients were discharged from
19
the hospital the day after surgery. This trial utilized the same dose concentration as Cohort 3 of our Phase 1b clinical trial at a higher volume, yielding a total dose of 4.5×1012 vg of VY-AADC compared with a total dose of up to 4.5×1012 vg in Cohort 3. The posterior approach was associated with greater average putaminal coverage (approximately 50%) and reduced average administration times compared with the transfrontal approach of Cohorts 1 through 3 in the Phase 1b clinical trial.
During the second half of 2018, we expect to provide longer-term safety, biomarker, motor function and quality of life data from Cohorts 1-3 and from patients in the posterior trajectory trial of VY-AADC for advanced Parkinson’s disease.
Voyager VY-AADC Pivotal Phase 2-3 Clinical Program Status
We plan to dose the first patient in our global pivotal Phase 2-3 clinical program for advanced Parkinson’s disease in mid-2018. In December 2017, we submitted an IND for VY-AADC which has become effective. As part of this IND, the chemistry, manufacturing, and controls section included data demonstrating comparability between VY-AADC produced under good manufacturing practice, or GMP, using our baculovirus/Sf9 manufacturing process and VY-AADC produced using a mammalian cell system consisting of triple-transfection of HEK293 cells, which was used in our Phase 1b clinical trial. Our baculovirus/Sf9 manufacturing process is designed for production of AAV vectors at clinical and commercial scale, with the potential for increased yields and efficient scalability compared with mammalian-based systems. We have demonstrated that this production platform change resulted in comparable vector quality and activity. We plan to use VY-AADC manufactured using our baculovirus/Sf9 process in our global pivotal Phase 2-3 clinical program.
We continue to follow patients from Cohorts 1 through 3 in the Phase 1b clinical trial of VY-AADC and patients in the Phase 1 posterior trajectory trial, and plan to report updated results from these trials from time to time. We plan to use VY-AADC manufactured in our baculovirus/Sf9 system in our pivotal Phase 2-3 clinical program. We plan to meet with the FDA as part of a Type C meeting to discuss the design of our pivotal Phase 2-3 clinical program during Q2 2018. Currently, our pivotal Phase 2-3 clinical program design provides for a single, placebo-controlled Phase 2 and a single, placebo-controlled Phase 3 clinical trial, conducted in staggered parallel and focused on key aspects of motor function measured over a sufficient period of time to potentially detect a meaningful and durable benefit versus placebo. We expect that the Phase 2 trial will inform us early on if we properly blinded the trial with placebo surgery and if we obtained sufficient coverage of the putamen. Achieving both of these objectives will allow us to begin enrolling the Phase 3 trial in staggered parallel while the Phase 2 trial continues blinded follow-up.
We expect that the Phase 2 trial will enroll at least 42 patients at approximately 16 trial sites, consisting of approximately eight surgical sites and eight corresponding patient-referral sites. The surgical sites will perform the infusions. The clinical patient-referral sites are the nearby hospitals and academic institutions from where eligible patients treated by movement disorder specialists will be identified, screened, and possibly referred to the surgical site for infusion of VY-AADC. We believe the primary endpoint of the Phase 2 clinical trial would be self-reported diary on-time without troublesome dyskinesia at twelve months, and secondary endpoints of the Phase 2 clinical trial would include diary off-time, UPDRS-III (physician-rated motor examination) scores and UPDRS-II (activities of daily living) scores. We expect the Phase 3 clinical trial to have the same primary and secondary endpoints but with a larger number of patients and more trial sites.
Based on our estimates of patient enrollment and a 12-month blinded treatment period, we expect top-line data from the Phase 2 portion of the pivotal Phase 2-3 clinical program in the second half of 2020. We currently anticipate that enrollment in the Phase 3 trial will begin during the first half of 2019. We expect that the Phase 3 trial will enroll approximately 100 to 120 patients and will include approximately 30 trial sites, consisting of approximately 10 surgical sites and 20 clinical referral sites. Based on our estimates of patient enrollment and a 12-month blinded treatment period, we anticipate top-line data from the Phase 3 trial during the first half of 2022. We believe that favorable results from both the Phase 2 and Phase 3 trials could support applications for marketing approval in the United States, Europe, and other regions beginning in mid-2022.
In 2018, the FDA granted fast track designation to VY-AADC.
20
Disease Overview
ALS is a fatal neurodegenerative disease that leads to muscle atrophy, spasticity and weakness as well as impaired speech, swallowing and breathing, with many patients requiring ventilator support as the disease progresses. The average age of onset of ALS is 55 years, and median survival is approximately three years after initial symptoms appear. It is estimated that there are approximately 20,000 patients in the United States who are living with the disease. Familial, or inherited, ALS accounts for approximately 10% of ALS cases, and an estimated 20% of familial ALS is caused by mutations in the superoxide dismutase 1, or SOD1, gene. Therefore, there are an estimated 400-800 patients in the United States with ALS caused by mutations in the SOD1 gene.
The normal function of the SOD1 protein is to catalyze the conversion of superoxide anion (O2-) to hydrogen peroxide (H2O2) and oxygen (O2). Mutations in SOD1 have been shown to lead to the formation of toxic aggregates of the SOD1 protein, resulting in the dysfunction and death of motor neurons. Patients with familial ALS caused by certain mutations in the SOD1 gene progress more rapidly than patients with other forms of ALS, although the reason for this more rapid progression is unknown.
There are currently only two FDA-approved treatments for ALS, Riluzole by Sanofi, which has been shown to have only modest efficacy, prolonging life by a few months, and Edaravone, which has been shown to slow decline of daily functioning.
Our Treatment Approach
We believe that AAV gene therapy is an attractive approach to treating monogenic ALS caused by SOD1 mutations. Since the SOD1 gene mutations that cause ALS are toxic gain-of-function mutations, we believe that we can employ an AAV gene therapy approach that targets the knockdown of SOD1 gene expression. In addition, the primary target cells - motor neurons - reside within the spinal cord, which we believe can be effectively transduced with AAV gene therapy through intrathecal injection as well as other routes of administration. The mechanism of action of VY-SOD101 is knockdown of SOD1 expression in motor neurons, thereby potentially reducing the level of toxicity associated with mutated protein, and slowing functional decline and prolonging ventilator-independent survival.
We believe that there is also the potential to leverage our approach for the treatment of other genetically defined forms of ALS.
Preclinical Studies Targeting SOD1 for Monogenic ALS
Results from published preclinical studies conducted at The Ohio State University support targeting mutant SOD1 for the treatment of monogenic ALS. In a non-human primate model, significant knockdown of SOD1 expression was observed following intrathecal injection of an AAV vector carrying a transgene designed to inhibit SOD1 expression. As shown in the figure below, SOD1 protein levels in lumbar spinal cord were knocked down by greater than 80%, on average, in three non-human primates. In addition, SOD1 expression in motor neurons was observed to be knocked down by 95%, on average, compared to a control group. No side effects from the treatment were reported.
21
Knockdown of SOD1 Using AAV-Mediated Delivery in Non-Human Primates(1)
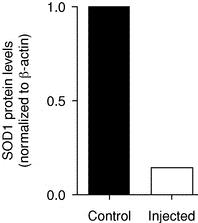
(1) Reprinted by permission from Macmillan Publishers Ltd: Foust et al, Molecular Therapy (2013), 21 (12); 2148-2159, copyright (2013).
The knockdown of SOD1 has also been reported to provide significant survival benefits in animal models of ALS. As shown in the example below, mice with a SOD1 mutation treated with an AAV vector to knock down expression of the SOD1 gene extended median survival by 87 days compared to mice treated with a control vector.
Improved Survival Post Knockdown of SOD1(1)
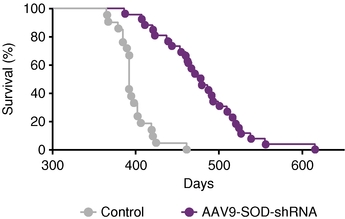
(1) Reprinted by permission from Macmillan Publishers Ltd: Foust et al, Molecular Therapy (2013), 21 (12); 2148-2159, copyright (2013). Purple line represents mice treated with AAV gene therapy, while gray line represents control mice.
These published studies as well as our own preclinical studies provide proof-of-principle for our approach to treating monogenic ALS due to SOD1 mutations with VY-SOD101.
Our Program Status
In late 2016, we identified VY-SOD101 as a lead clinical candidate after screening a series of capsids, microRNA expression cassettes, (a segment of DNA that contains the sequence that targets SOD1 gene expression selectively for knockdown), and encoded payloads. We screened more than 100 RNAi sequences, each represented by a bar in the graph below, and successfully identified multiple, highly-potent RNAi sequences targeting SOD1, as highlighted by the yellow bars in the figure below:
22
Overview of miRNA Target Sequences for Knockdown of SOD1
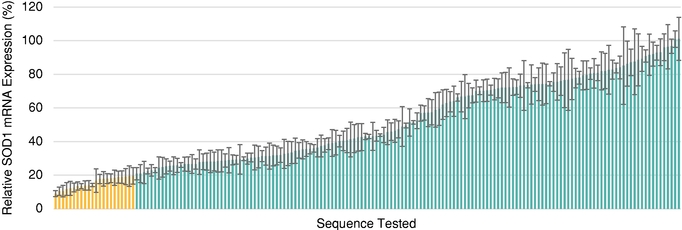
The most potent RNAi sequences targeting SOD1 gene expression were evaluated in multiple microRNA expression cassettes and with a number of vector genome configurations. We have completed the necessary experiments to evaluate these potential lead candidates based upon criteria that include safety, selectivity, potency, and efficiency and precision of microRNA processing.
In late 2017, we initiated additional preclinical studies to further optimize our therapeutic approach with this program, including exploration of additional routes of administration and novel AAV capsids in large animal models. We continue to further investigate and evaluate these additional routes of administration and novel capsids before progressing this program towards filing an IND application.
Friedreich’s Ataxia Program: VY-FXN01
Disease Overview
Friedreich’s ataxia is a debilitating neurodegenerative disease resulting in poor coordination of legs and arms, progressive loss of the ability to walk, generalized weakness, loss of sensation, scoliosis, diabetes and cardiomyopathy as well as impaired vision, hearing and speech. The typical age of onset is 10 to 12 years, and life expectancy is severely reduced with patients generally dying of neurological and cardiac complications between the ages of 35 and 45. According to the Friedreich’s Ataxia Research Alliance, there are approximately 6,400 patients living with the disease in the United States. There are currently no FDA-approved treatments for the disease.
Friedreich’s ataxia patients have mutations of the FXN gene that reduce production of the frataxin protein, resulting in the degeneration of sensory pathways and a variety of debilitating symptoms. Friedreich’s ataxia is an autosomal recessive disorder, meaning that a person must obtain a defective copy of the FXN gene from both parents in order to develop the condition. One healthy copy of the FXN gene, or 50% of normal frataxin protein levels, is sufficient to prevent the disease phenotype. We therefore believe that restoring FXN protein levels to at least 50% of normal levels by AAV gene therapy might lead to a successful therapy.
Our Treatment Approach
We are developing an AAV gene therapy approach that we believe will deliver a functional version of the FXN gene to the sensory pathways through intrathecal or intravenous injection. We think this approach has the potential to improve balance, ability to walk, sensory capability, coordination, strength and functional capacity of Friedreich’s ataxia patients. Most Friedreich’s ataxia patients produce low levels of the frataxin protein, which although insufficient to prevent the disease, exposes the patient’s immune system to frataxin. This reduces the likelihood that the FXN protein expressed by AAV gene therapy will trigger a harmful immune response.
23
Preclinical Studies
We conducted preclinical studies in non-human primates and achieved high FXN expression levels within the target sensory ganglia, or clusters of neurons, along the spinal region following intrathecal injection. As depicted in the figure below, FXN expression was normalized as a fold increase relative to FXN expression in a human brain reference sample. The levels of FXN expression observed using an AAV vector were, on average, greater than FXN levels present in normal human brain tissue. The increased levels of FXN were achieved in cervical, thoracic, lumbar and sacral levels. Relatively low, but measurable, levels of FXN expression were also observed in the cerebellar dentate nucleus, another area of the CNS that is often affected in Friedreich’s ataxia, and that is often considered difficult to target therapeutically.
FXN Expression in Sensory Ganglia Following Intrathecal Delivery in Non-Human Primates
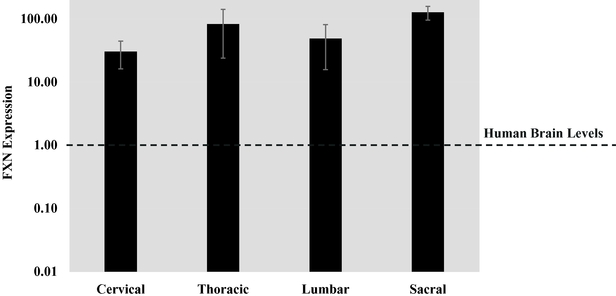
Our Program Status
VY-FXN01 is currently in preclinical development. We are in the process of identifying a lead candidate which will comprise an optimal capsid, promoter, and FXN transgene. We are completing several AAV capsid screening experiments to identify capsids that effectively distribute to disease target tissues in a desired manner. We are comparing capsids in non-human primates following intrathecal and intravenous injection, and evaluating these capsids based upon multiple criteria including safety, overall level of transgene expression achieved, distribution of transgene expression and the specific cell types transduced. In addition, we are optimizing the promoter and specific characteristics of the FXN transgene that we expect to use for VY-FXN01. To evaluate the therapeutic potential of our vectors, we have initiated testing in a new genetic mouse model of Friedreich’s ataxia. We also have a significant effort focused on better understanding the clinical course of Friedreich’s ataxia and identifying potential clinical endpoints for future clinical trials.
Once we identify a lead candidate for this program, we plan to complete preclinical studies to evaluate the safety and efficacy of our lead candidate, including studies in a relevant animal model of Friedreich’s ataxia and IND-enabling studies.
Huntington’s Disease Program: VY-HTT01
Disease Overview
Huntington’s disease is a fatal, inherited neurodegenerative disease that results in the progressive decline of motor and cognitive functions and a range of behavioral and psychiatric disturbances. The average age of onset is 39
24
years, with patients typically dying approximately 15 to 20 years following diagnosis. According to the Huntington’s Disease Society of America, Huntington’s disease affects approximately 30,000 patients in the United States. Huntington’s disease is caused by mutations in the huntingtin, or HTT, gene. Huntington’s disease is an autosomal dominant disorder, which means that an individual is at risk of inheriting the disease if only one parent is affected. More than 200,000 individuals in the United States are at risk for inheriting the mutant gene from an affected parent. While the exact function of the HTT gene in healthy individuals is unknown, it is essential for normal development before birth and mutations in the HTT gene ultimately lead to the production of abnormal intracellular huntingtin protein aggregates that cause neuronal cell death. Currently, there are no approved treatments targeting the underlying cause of the disease and only one drug, tetrabenazine, has been approved for the treatment of the specific motor symptoms of Huntington’s disease.
Our Treatment Approach
We believe that AAV gene therapy is an attractive approach to treating Huntington’s disease. Since HTT mutations that cause Huntington’s disease are toxic gain-of-function mutations, we believe that we can employ an AAV gene therapy approach designed to knock down expression of the HTT gene. In addition, the targeted cells for treatment primarily reside in discrete regions of the brain - the striatum and the cortex - that can be targeted with AAV gene therapy delivered directly into the brain. The mechanism of action of VY-HTT01 is knockdown of HTT expression in neurons in the striatum and cortex, thereby reducing the level of toxicity associated with mutated protein in these brain regions, and slowing the progression of cognitive and motor symptoms. We believe that we can use the same surgical approach for this program that has been used for VY-AADC delivery to the brain, allowing us to leverage prior clinical experience.
Preclinical Studies
Our collaborators at Sanofi Genzyme have completed significant preclinical work focused on AAV gene therapy for Huntington’s disease. Sanofi Genzyme’s preclinical studies in a mouse model of Huntington’s disease demonstrated the safety and efficacy of AAV gene therapy targeting the knockdown of the HTT gene in the CNS.
As shown in the figure below, using an AAV vector delivered directly to the CNS, HTT gene expression was observed to be reduced by over 50%, on average, in the treatment group as compared to the control group. No signs of toxicity were reported.
Knockdown of HTT Following AAV Delivery(1)
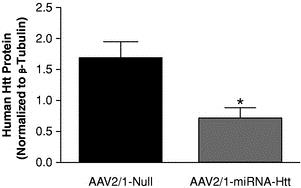
(1) Stanek et al, Human Gene Therapy (2014); 25; 461-474. The publisher for this copyrighted material is Mary Ann Liebert, Inc. publishers.
* p<0.05
In addition, significant functional benefit was observed in the treatment group, as measured by the rotarod test to assess motor function, and the Porsolt Swim Test to measure depressive behavior in mice. In the figure below, both normal or wild type mice, and mice with the HTT mutation, or YAC128, were evaluated following treatment with either
25
an AAV vector targeting the knockdown of the HTT gene, labeled as AAV2/1-miRNA-Htt below, or a negative control vector, labeled as AAV2/1-Null below. As expected, knocking down HTT in the control mice was observed to have no functional impact, whereas knocking down HTT in YAC128 mice was observed to have significant functional benefit.
Reduction of Behavioral Deficits in an Animal Model of Huntington’s Disease(2)
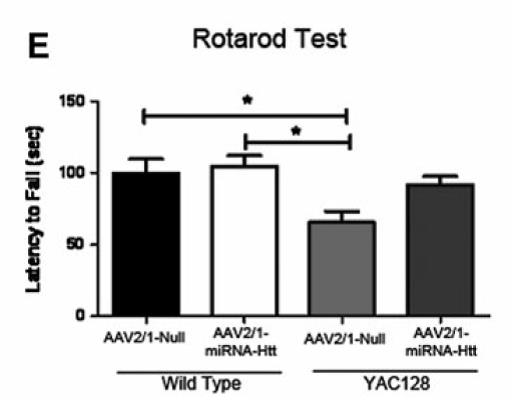
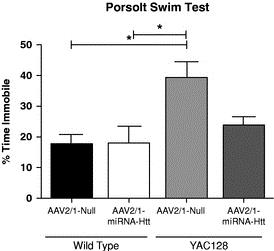
(2) Stanek et al, Human Gene Therapy (2014); 25; 461-474. The publisher for this copyrighted material is Mary Ann Liebert, Inc. publishers.
* p<0.05
Our Program Status
VY-HTT01 is in preclinical development. Sanofi Genzyme’s Huntington’s disease gene therapy program was combined with our efforts in connection with entering into our collaboration agreement in February 2015. Through our product engine, we also constructed and screened a series of microRNA expression cassettes and encoded payloads. Multiple rounds of optimization have resulted in potential candidates that are potent and selective for knocking down HTT. In addition, many construct configurations were evaluated toward the identification of one which would provide excellent yield and genome integrity for manufacturing scale-up in our baculovirus/Sf9 AAV manufacturing system in insect-derived cells.
We also conducted the necessary experiments to evaluate these potential lead candidates based upon criteria that include safety, selectivity, potency, and efficiency and precision of microRNA processing, leveraging the learnings from the VY-SOD101 program, including the miRNA cassettes and vector genome configurations that we have designed for the VY-SOD101 program. In June 2017, we reported that we had selected a lead clinical candidate.
In preclinical studies, a single administration of VY-HTT01 was well-tolerated and resulted in robust and widespread knockdown of HTT messenger RNA in disease-relevant regions of the non-human primate central nervous system. The extent of HTT mRNA suppression (greater than 50%) and high precision and efficiency of primary microRNA processing in our preclinical studies supported the selection of our lead clinical candidate. Additionally, preclinical data in large mammals have demonstrated that a single intraputaminal administration results in robust knockdown of HTT in the putamen.
Direct delivery of VY-HTT01 to the brain with a one-time administration could potentially slow or halt the progression of this uniformly fatal disease. Preclinical pharmacology and toxicology studies are now underway with VY-HTT01 to support filing of an IND application in 2019.
26
Tau Program
Disease Overview
In healthy individuals, tau is an abundant soluble cytoplasmic protein that binds to microtubules (key structural proteins in cells) to promote their stability and function. In Alzheimer’s disease, or AD, and other tauopathies, tau aggregates and forms insoluble tau-containing neurofibrillary tangles. The progressive spread of tau pathology along distinct anatomical pathways in the brain closely correlates with disease progression and severity in a number of tauopathies, including AD, FTD, and PSP. In addition, mutations in the tau gene have been shown to cause inherited forms of tauopathies, including FTD and PSP. Because the extent of tau pathology in AD and other tauopathies closely correlates with the severity of neurodegeneration, synapse loss, and cognitive deficits, attempts to prevent, reduce, or slow the development of tau pathology have become important therapeutic strategies for these diseases.
In previous preclinical studies, despite high weekly or biweekly systemic doses of anti-tau monoclonal antibodies administered over three to six months, only very low levels of antibody reached the brain, resulting in a modest reduction of tau pathology by ~40–50%. This incomplete and modest reduction in tau pathology following treatment with very high and frequent systemic doses of these antibodies may pose therapeutic challenges in humans with various tauopathies. To address these limitations, our collaboration with AbbVie attempts to develop AAV gene therapies to deliver monoclonal antibodies to the brain directed against tau as potential new treatments for Alzheimer’s disease and other tau-related neurodegenerative diseases.
Our Program Status
The Tau program is currently in the preclinical stage. We have agreed to collaborate with AbbVie on the research and development of specified vectorized antibody compounds comprised of an AAV or other viral capsid and a virus vector genome that encodes one or more antibodies that target and bind to a tau protein. During the research period of our collaboration, we and AbbVie agreed to each identify up to five potential antibodies for evaluation during the collaboration. Under the agreement, up to three research antibodies may be selected as candidates for creation of research compounds. AbbVie has the right to select two of the three research antibodies. During a specified portion of the research period, AbbVie may exercise one or more of its exclusive development options to select up to a total of three research compounds and their corresponding product candidates to proceed to the development period.
Severe, Chronic Pain Program: VY-NAV01
Disease Overview
Nav1.7 is a sodium ion channel that is required for transmission of pain signals to the CNS. We believe that an AAV gene therapy approach targeting the knockdown of Nav1.7 in sensory neurons could be an effective treatment for certain forms of severe, chronic pain. A major challenge for the successful development of small molecules and antibodies targeting Nav1.7 has been the selective inhibition of Nav1.7 over closely related sodium channels such as Nav1.5 which are important for cardiac function. MicroRNAs, which work by harnessing the RNA interference pathway, can achieve a high level of specificity for their messenger RNA targets, and can inhibit Nav1.7 selectively over other sodium channel subtypes. Such an approach could avoid the dose-limiting side effects associated with the non-selective profile of many current drugs used to treat severe, chronic pain, and also achieve a durable clinical benefit following a single administration of the therapy. VY-NAV01 leverages our extensive experience designing novel microRNA knockdown cassettes and delivering them using AAV, an approach that we are using for our ALS and Huntington’s disease programs.
Our Program Status
VY-NAV01 is currently in the research stage. We are in the process of conducting proof-of-concept studies to establish the level of Nav1.7 knockdown needed to relieve pain in animal models. We will then identify a lead candidate
27
which will comprise an optimal capsid, promoter, and microRNA targeting Nav1.7. We have also initiated proof-of-concept studies to evaluate knockdown of another sodium channel subtype implicated in chronic pain that may be combined with Nav1.7 knockdown. We are completing several AAV capsid screening experiments to identify capsids that effectively distribute to pain sensory neurons in a desired manner. We are comparing capsids in non-human primates following intrathecal and intravenous injection, and evaluating these capsids based upon multiple criteria including safety, overall level of transgene expression achieved, distribution of transgene expression and the specific cell types transduced.
Future Programs
We are evaluating additional severe neurological diseases that could be treated using AAV gene therapy through application of either a gene replacement or a gene knockdown approach. Beyond these approaches, we are also actively exploring additional potential treatment methods that can utilize an AAV vector, including gene editing to correct or delete a gene in the cell genome.
For information regarding amounts spent during each of the last three fiscal years on company-sponsored research and development activities, see Part II “Item 6 – Selected Financial Data” of this Annual Report on Form 10-K.
Collaborations and License Agreements
Sanofi Genzyme Collaboration
In February 2015, we entered into a strategic collaboration with Sanofi Genzyme to leverage our combined expertise and assets to develop AAV gene therapies for neurological diseases. Under the agreement, we retained U.S. rights to VY-AADC and VY-FXN01, as well as at least co-commercialization rights to VY-HTT01 in the United States. In October 2017, Sanofi Genzyme decided not to exercise its option for the ex-U.S. rights to VY-AADC. Therefore, we have maintained global rights to VY-AADC. VY-SOD101 is not included as part of the Sanofi Genzyme collaboration and we retain unencumbered worldwide rights to this program. Sanofi Genzyme maintains an exclusive option to license, develop and commercialize (i) ex-U.S. rights to the Split Territory Programs with an incremental option to co-commercialize VY-HTT01 in the United States, and (ii) worldwide rights to VY-SMN101. Sanofi Genzyme’s option for the Split Territory Programs and VY-SMN101 is triggered following the completion of the first POP Study on a program-by-program basis. In November 2016, we and Sanofi Genzyme elected to deprioritize the development of VY-SMN101 for spinal muscular atrophy due to, among other things, the significant progress we have made in our other preclinical programs and the evolving competitive landscape.
Prior to any option exercise by Sanofi Genzyme, we will collaborate with Sanofi Genzyme in the development of products under each Split Territory Program and VY-SMN101 pursuant to a written development plan and under the guidance of an alliance joint steering committee, comprised of an equal number of our employees and Sanofi Genzyme employees.
We are required to use commercially reasonable efforts to develop products under each Split Territory Program and VY-SMN101 through completion of the applicable POP Study. During the development of our joint programs, our and Sanofi Genzyme’s activities are guided by a Development Advisory Committee, which we refer to as the DAC. The DAC may elect to utilize certain Sanofi Genzyme technology relating to the VY-AADC program, the VY-HTT01 Program, or generally with the manufacture of Split Territory Program products. If we use certain Sanofi Genzyme technology in VY-AADC, Sanofi Genzyme is entitled to received low single digit royalty payments based on a percentage of net sales by us, and we may be obligated to make certain regulatory milestone payments to a third-party licensor.
We will be solely responsible for all costs incurred in connection with the development of Split Territory Programs and VY-SMN101 products prior to option exercise, subject to the following: (i) Sanofi Genzyme may agree to provide additional funds in return for agreed-upon payback or other agreed economic terms; (ii) we may request, and
28
upon mutual agreement, Sanofi Genzyme will provide in-kind services valued at up to $5.0 million; and (iii) expenses of certain activities under the VY-HTT01 development plan may be funded to the extent such activities are reimbursed through financial support that Sanofi Genzyme may receive from a disease foundation group.
Other than the VY-AADC program (for which a POP Study has been completed), if we do not initiate a POP Study for a given Split Territory Program by December 31, 2026 (or for the Future Program by the tenth anniversary of the date the Future Program is nominated by Sanofi Genzyme), and Sanofi Genzyme has not terminated this agreement with respect to such Collaboration program, then Sanofi Genzyme shall be entitled, at its sole and exclusive remedy, to a credit of $10.0 million for each such program against other amounts payable by Sanofi Genzyme under the Collaboration. However, if we do not initiate a POP Study by such date as a result of a regulatory delay or a force majeure event, such time period shall be extended for so long as such regulatory delay or force majeure event continues and we shall not be deemed to have failed to initiate a POP Study.
Post-Option Exercise
Upon Sanofi Genzyme’s exercise of its option to license a given product in a Split Territory Program, which we refer to as a Split Territory Licensed Product, we will have sole responsibility for the development of such Split Territory Licensed Product in the United States and Sanofi Genzyme shall have sole responsibility for development of such Split Territory Licensed Product in the rest of the world. We and Sanofi Genzyme will have shared responsibility for execution of ongoing development of such Split Territory Licensed Product that is not specific to either of our territories, including costs associated therewith.
A steering committee for each program will review and approve a written plan and budget for each relevant program. In addition, all development activities to be undertaken with respect to each Split Territory Licensed Product by or on behalf of either party will be set forth in a written development plan.
Sanofi Genzyme shall have the sole right to develop VY-SMN101 worldwide. Sanofi Genzyme shall be responsible for all of the development costs that occur after the option exercise date for VY-SMN101.
Commercialization
We shall be solely responsible, at our expense, for all commercialization activities relating to Split Territory Licensed Products in the United States. Sanofi Genzyme shall be solely responsible, at its expense, for all commercialization activities relating to Split Territory Licensed Products in the rest of the world. For VY-HTT01, if Sanofi Genzyme has exercised its option to co-commercialize VY-HTT01 in the United States, then Sanofi Genzyme will be the lead party responsible for all VY-HTT01 commercialization activities in the United States, and these activities will be set forth in reasonable detail in a written commercialization plan.
Sanofi Genzyme shall be solely responsible, at its expense, for all commercialization activities relating to VY-SMN101 worldwide. Sanofi Genzyme shall use commercially reasonable efforts to commercialize VY-SMN101 in each major market specified in the agreement where Sanofi Genzyme has obtained required governmental approvals.
Financial Terms
We received $65.0 million in upfront cash, a $30.0 million upfront equity investment and an in-kind commitment of $5.0 million, totaling $100.0 million. If Sanofi Genzyme exercises its option for a collaboration program, with the exception of VY-AADC, Sanofi Genzyme is required to make an option exercise payment of $20.0 million or $30.0 million for each program. We are no longer entitled to receive the regulatory and commercial milestone payments related to VY-AADC. Sanofi Genzyme shall pay us up to $540.0 million across the remaining product programs upon the achievement of specified regulatory and commercial milestones.
29
In addition, to the extent any Split Territory Licensed Product or the VY-SMN101 Product is commercialized, we are entitled to receive tiered royalty payments ranging from the mid-single digits to mid-teens based on a percentage of net sales. Sanofi Genzyme is entitled to receive royalty payments from us related to sales of the Split Territory Licensed Products ranging from the low-single digits to mid-single digits, depending on whether we use Sanofi Genzyme technology in a Split Territory Licensed Product or the VY-SMN101 Product. If Sanofi Genzyme exercises its option to co-commercialize VY-HTT01 in the United States, we will share any profits or losses from VY-HTT01 product sales.
Term and Termination; Remedies
Our collaboration agreement with Sanofi Genzyme will continue in effect until the later of (i) the expiration of the last to expire of the option rights and (ii) the expiration of all payment obligations unless sooner terminated by us or Sanofi Genzyme.
We and Sanofi Genzyme have customary termination rights including the right to terminate for an uncured material breach of the agreement committed by the other party and Sanofi Genzyme has the right to terminate for convenience.
AbbVie Collaboration
In February 2018, we entered into an exclusive collaboration and option agreement with AbbVie, or the AbbVie Collaboration Agreement, for the research, development, and commercialization of AAV and other virus-based gene therapy products for the treatment of neurodegenerative diseases related to defective or excess aggregation of tau protein in the human brain, including Alzheimer’s disease.
Under the AbbVie Collaboration Agreement, we have agreed to collaborate with AbbVie on the research and development of specified vectorized antibody compounds comprised of an AAV or other viral capsid and a virus vector genome that encodes one or more antibodies that target and bind to a tau protein. The collaboration is comprised of a research period, a development period, and an exclusive license option.
Research Period and AbbVie Development Option
During the research period, each party has agreed to identify up to five antibodies for inclusion in the collaboration. Subject to certain conditions and exceptions, the parties will then select up to three antibodies, or the Research Antibodies, as candidates for creation of research compounds, or the Research Compounds, with AbbVie having the right to select two of the three Research Antibodies. We are obligated to use diligent efforts to conduct antibody engineering and other research activities to create Research Compounds and to develop product candidates containing or comprised of such Research Compounds. We will be solely responsible for the costs and expenses during the Research Period. During a specified portion of the Research Period, or the Development Option Period, AbbVie may exercise one or more of its exclusive development options, each of which we refer to as a Development Option, to select up to a total of three Research Compounds, or the Selected Research Compounds, and their corresponding product candidates, or the Selected Product Candidates, to proceed to the development period.
Development Period and AbbVie License Option
During the development period, we are obligated to use diligent efforts to conduct development activities, including IND-enabling and Phase 1 clinical trial activities, for the Selected Research Compounds and corresponding Selected Product Candidates. We will be solely responsible for the costs and expenses during the development period. During a specified portion of the development period, or the License Option Period, AbbVie may exercise its exclusive license option, or the License Option, to further develop and commercialize all of the Research Compounds, or the Licensed Compounds, and corresponding product candidates, or the Licensed Products. Upon AbbVie’s exercise of its License Option, we have agreed to grant to AbbVie an exclusive, worldwide license, with the right to sublicense, under
30
certain of our intellectual property rights to develop and commercialize the Licensed Compounds and the Licensed Products for all human diagnostic, prophylactic and therapeutic uses. In addition, after AbbVie’s exercise of the License Option, we have certain obligations to complete any remaining research and development activities that have not been completed for any Research Compounds and Product Candidates.
Governance
Our research and development activities will be conducted pursuant to the plans agreed to by the parties and overseen by a joint governance committee, or JGC, comprised of an equal number of representatives from each party. Prior to AbbVie’s exercise of its License Option, we will have final decision-making authority within the JGC, subject to specified limitations; thereafter, AbbVie will have final decision-making authority, subject to specified limitations. Any material amendment to the research or development plans, however, must be mutually agreed to by the parties, which may be through the JGC.
Commercialization
Under the AbbVie Collaboration Agreement, AbbVie is required to use commercially reasonable efforts to develop and commercialize at least one Licensed Product in each of the United States, Japan, the United Kingdom, Germany, France, Italy and Spain. After exercise of the License Option, AbbVie is solely responsible for all development and commercialization activities relating to Licensed Compounds and Licensed Products at its sole cost and expense (subject to our obligation to complete any remaining research and development activities set forth in the agreed-upon plans), except that we may elect to share in AbbVie’s development costs relating to a Licensed Product on an indication-by-indication basis in exchange for a specified increase in royalties. If we exercise this cost-sharing option, we may either reimburse AbbVie for AbbVie’s applicable development costs or, in the case of certain budget overruns, AbbVie may instead deduct applicable development costs, up to a specified cap, from milestone and royalty payments owed by AbbVie to us.
Manufacturing
During both the research period and the development period, we will be solely responsible for the manufacture and supply of all pre-clinical and clinical requirements for the Research Compounds and Product Candidates. If AbbVie were to exercise its License Option, we would be required, at AbbVie’s request, to effect a full transfer of the manufacturing process for each Licensed Compound and corresponding Licensed Product to AbbVie. Following such transfer, we have agreed to disclose, on a continuing basis, all modifications, enhancements and improvements to manufacturing processes for the Licensed Products, and AbbVie has agreed to grant to us a non-exclusive, royalty-free license to modifications to the manufacturing process made by AbbVie, in each case subject to specified limitations.
Financial Terms
Under the terms of the AbbVie Collaboration Agreement, AbbVie has agreed to pay us an upfront payment of $69.0 million within 15 business days of entry into the agreement. AbbVie has also agreed to pay to us, within 30 days after the applicable exercise date: (1) upon AbbVie’s exercise of a Development Option, (a) $80.0 million for the first Selected Research Compound and its corresponding Selected Product Candidate and (b) $30.0 million each for up to two additional Selected Research Compounds and their corresponding Selected Product Candidates, and (2) upon AbbVie’s exercise of the License Option, a one-time payment of $75.0 million. We will be eligible to receive (1) specified development and first-sale milestone payments for each Licensed Compound of up to an aggregate of $550.0 million in the case of an Alzheimer’s disease indication, up to $230.0 million in the case of the first indication other than Alzheimer’s disease, and $115.0 million for subsequent non-Alzheimer’s disease indication; and (2) tiered, escalating royalties, in a range from a high-single digit to a mid-to-high teen (or, if we have exercised our cost-sharing option, low-twenties) percentage of aggregate net sales of Licensed Products on a Licensed Compound by Licensed Compound basis. The royalties are subject to potential reductions for biosimilar market penetration, patent claim expiration, and other provisions, subject to specified limits. For each Licensed Product, AbbVie may make a one-time request either to decrease its royalty payments to a specified low-single digit percentage or to terminate them altogether in exchange for a
31
one-time payment by AbbVie at a fair market value to be negotiated by the parties. If the parties are not able to agree to the terms of such buy-down, the parties may seek a fair market value determination for the buy-down pursuant to dispute resolution procedures specified in the agreement.
Intellectual Property
Under the terms of the AbbVie Collaboration Agreement, each party will own the entire right, title and interest in and to all know-how and patent rights first made or invented solely by it or its affiliates or its or their sublicensees in the course of the collaboration, with certain specified exceptions. Also subject to specified exceptions, the parties will jointly own all rights, title and interest in and to all know-how and patent rights first made or invented jointly by such party or its affiliates or its or their sublicensees in the course of the collaboration. Regardless of whether AbbVie has exercised a Development Option or the License Option, we have agreed to grant AbbVie perpetual, exclusive or non-exclusive (as the case may be), worldwide licenses to certain know-how and patent rights developed by us or jointly by the parties arising from the collaboration.
Exclusivity
During the term of the AbbVie Collaboration Agreement, (1) neither party nor any of its respective affiliates is permitted to directly or indirectly exploit any vectorized antibody compound targeting a tau protein, which we refer to as Vectorized Antibody Exclusivity, and (2) neither we nor any of our affiliates is permitted to directly exploit any Research Antibody targeting a tau protein, which we refer to as Research Antibody Exclusivity, in each case subject to specified exceptions, including our conduct of basic research.
Termination
Unless earlier terminated, the AbbVie Collaboration Agreement will expire on the earliest to occur of the expiration of (1) the Development Option Period, without AbbVie’s exercise of a Development Option; (2) the License Option Period, without AbbVie’s exercise of its License Option; and (3) the last-to-expire royalty term with respect to all Licensed Products in all countries. Subject to a cure period, either we or AbbVie may terminate the AbbVie Collaboration Agreement, in whole or, in the case of us, in part, subject to specified conditions, in the event of the other party’s uncured material breach. Either we or AbbVie may also terminate, subject to specified conditions, for insolvency of the other party, certain failures or delays to obtain certain regulatory clearances of the collaboration, or a joint determination of scientific infeasibility by the parties. AbbVie may terminate the AbbVie Collaboration Agreement (1) without cause, in its entirety or, after its exercise of the License Option, on a country-by-country basis, with 180 days’ prior written notice or (2) for our non-compliance with certain anti-bribery or anti-corruption covenants. We may terminate the AbbVie Collaboration Agreement, subject to specified conditions, if AbbVie or its affiliates challenge the validity or enforceability of certain of our, or jointly-held intellectual property rights.
Upon termination in certain cases, AbbVie has agreed to grant to us reversionary licenses to certain Licensed Compounds. In such case, we may be required to pay royalties to AbbVie in a range from a low to high single digit percentage of net sales of Licensed Products containing or comprised of such License Compound, subject to potential reduction in some cases. Additionally, upon termination in certain cases, the Vectorized Antibody Exclusivity and Research Antibody Exclusivity will survive until the third anniversary of the termination date. If the parties mutually agree to terminate for infeasibility or AbbVie terminates for our failure to deliver a final research or development report, neither us nor any of its affiliates may directly or indirectly exploit a vectorized antibody compound that targets or binds to a tau protein for 18 months after the termination date.
License Agreement with University of Massachusetts
On January 30, 2014, we entered into a license agreement with the University of Massachusetts, or UMass, pursuant to which UMass granted us an exclusive, worldwide, royalty-bearing license to certain of its licensed patents to make, have made, use, offer for sale, sell, have sold and import certain licensed products in the field of human diseases
32
that use gene therapy applications. Our license is subject to any rights that may be required to be granted to the government of the United States, and UMass reserves the right to use the licensed patents for education and research and, with our consent, for non-commercial patient care, without the payment of any compensation to us.
In consideration for rights granted to us under the agreement, we made an upfront payment of $0.2 million to UMass. We are obligated to pay UMass (i) low-single digit royalty payments based on net sales of the licensed products, (ii) annual maintenance payments of $30.0 thousand, which are creditable against royalties payable in such period, (iii) minimum aggregate annual royalty payments that are creditable against royalties payable in such period, with the minimum aggregate amount payable being in the low-six digits for each of the first four years of this agreement and a minimum aggregate amount payable being in the mid-six digits for each year, thereafter, (iv) milestone payments of up to $1.8 million, per licensed product for the first five licensed products, based on the achievement of development and regulatory milestones and (v) a percentage of sublicensing income that decreases over time from low double digit percentages to a mid-single digit percentage. We also agreed to reimburse UMass approximately $0.7 million for patent related expenses incurred by UMass as of the effective date of the agreement over a two-year period.
Under the agreement, we agreed to use commercially reasonable efforts to develop licensed products and to introduce such licensed products into the commercial market, and further agreed to certain development milestones.
The agreement will terminate on the date that is the later of (i) seven years after the first commercial sale of the last licensed product under the agreement or (ii) such time as there are no valid claims covering a licensed product. We have the right to terminate the agreement for any reason upon 90 days prior written notice, and we and UMass have the right to terminate the agreement if the other party fails to cure a written breach within 60 days of receiving written notice of such breach.
MassBiologics and UMass Collaboration Agreement
On October 20, 2014, we entered into a Collaboration Agreement with UMass and MassBiologics, pursuant to which we shall (i) fund certain projects that will be conducted by UMass or MassBiologics, (ii) fund certain educational programs of UMass, including post-doctoral research at our laboratories beginning in 2015 and an annual lecture series beginning in 2015 and (iii) collaborate with MassBiologics to establish scalable processes for manufacturing recombinant AAV vector products using cGMP.
In November 2014, we agreed to the first project under this agreement whereby we funded approximately $2.9 million over a 16-month period for certain research and development services performed by MassBiologics. The project commenced in January 2015 and completed during 2016. We and UMass and/or MassBiologics may agree to conduct other projects in the future, the terms of which will be agreed upon at such time.
This agreement will remain in effect for a period of five years and automatically renews for additional one-year periods. Either party has the right to terminate this agreement, once in each renewal period, for any reason upon providing the other party with 90 days written notice or in the event of a material breach of the agreement by the other party that is not cured within 60 days of written notice.
We will own all intellectual property rights generated under this agreement, either by our employees, UMass and/or MassBiologics employees, or jointly by our employees and UMass and/or MassBiologics employees, that cover AAV materials. We and UMass and/or MassBiologics, as applicable, will jointly own any intellectual property rights generated under this agreement jointly by our employees and the employees of UMass and/or MassBiologics, as applicable, that do not cover AAV materials.
License Agreement with REGENX
In May 2014, we entered into a license agreement with REGENXBIO Inc., formerly known as ReGenX Biosciences, LLC, or REGENX, for the development and commercialization of gene therapies to treat ALS, Friedreich’s
33
ataxia and Huntington’s disease. Under this license agreement, REGENX granted us a non-exclusive worldwide license to make, have made and use its technology solely for internal research and preclinical development for the identification of specific vectors that could be commercialized. Following identification, we have an option to obtain a non-exclusive worldwide license under the licensed intellectual property to a single specified AAV vector to make, have made, use, import, sell and offer for sale licensed products using the selected vector, which can be exercised for each of ALS, Friedreich’s ataxia, or Huntington’s disease.
Under the terms of this license agreement, we paid REGENX an upfront fee of $0.5 million, an extension fee of $0.1 million and are required to pay an annual maintenance fee. If we exercise any or all of the commercial options by a specified date, we will be required to make upfront payments to REGENX of up to $1.5 million and to pay to REGENX an annual maintenance fee payment ranging from five digits to six digits depending on the number of disease indication options exercised. In addition, we will be required to pay to REGENX up to $5.0 million in milestone fees per disease indication, mid- to high-single digit royalty percentages on net sales of licensed products, and low- to mid-single digit percentages of any sublicense fees that we receive from sublicensees for the licensed intellectual property rights.
Our license agreement with REGENX will expire upon the expiration, lapse, abandonment, or invalidation of the last claim of the licensed intellectual property to expire, lapse, or become abandoned or unenforceable in all the countries of the world. The license agreement will automatically terminate if we do not exercise any commercial options within a specified time period after entering into the license agreement, which may be extended. We may terminate the license agreement upon a specified number of days prior written notice. REGENX may terminate the license agreement if we, our affiliates, or sublicensees experience insolvency, if we are more than a specified number of days late in paying money due under the license agreement, or, effective immediately, if we or our affiliates commence any action against REGENX or its licensors to declare or render any claim of the licensed patent rights invalid or unenforceable. Either party may terminate the license agreement for material breach that is not cured within a specified number of days.
In November 2016, Voyager exercised commercial options for the use of REGENXBIO’s NAV® Technology Platform, or NAV, vectors for the development and commercialization of gene therapies for specific neurological diseases. Upon exercise of the options, REGENXBIO has granted Voyager a non-exclusive worldwide commercial license, with rights to sublicense, to three specific NAV vector sequences covered by REGENXBIO’s NAV Technology Platform, each for the treatment of a specific neurological disease. In return for these rights, REGENXBIO will receive undisclosed upfront payments, ongoing fees, milestone payments and royalties on net sales of products incorporating the licensed intellectual property.
Competition
The biopharmaceutical industry is characterized by intense and dynamic competition to develop new technologies and proprietary therapies. Any product candidates that we successfully develop into products and commercialize may compete with existing therapies and new therapies that may become available in the future. While we believe that our product engine, product programs, product candidates and scientific expertise in the fields of gene therapy and neuroscience provide us with competitive advantages, we face potential competition from various sources, including larger and better-funded pharmaceutical, specialty pharmaceutical and biotechnology companies, as well as from academic institutions, governmental agencies and public and private research institutions.
We are aware of several companies focused on developing gene therapies in various indications, including bluebird bio, Inc., Abeona Therapeutics, Inc., Adverum Biotechnologies, Inc., Aevitas Therapeutics, Inc., Agilis Biotherapeutics, LLC, Applied Genetic Technologies Corporation, Asklepios BioPharmaceutical, Inc., Audentes Therapeutics, Inc., AveXis, Inc., GenSight Biologics SA, LogicBio Therapeutics, Inc., Lysogene SA, MeiraGTx Ltd., NightstaRx Ltd, Prevail Therapeutics, Inc., REGENXBio Inc., Solid Biosciences, Inc., uniQure NV, or uniQure, Pfizer, Inc., or Pfizer, and Spark Therapeutics, Inc. or Spark, as well as several companies addressing other methods for modifying genes and regulating gene expression. Any advances in gene therapy technology made by a competitor may be used to develop therapies that could compete against any of our product candidates.
34
We expect that VY-AADC will compete with a variety of therapies currently marketed and in development for advanced Parkinson’s disease, including DBS marketed by Medtronic plc, Abbott Laboratories (acquired from St. Jude Medical in 2017), and other medical device companies, DUOPA/Duodopa marketed by AbbVie Inc., as well as other novel, non-oral forms of levodopa in development, including NeuroDerm’s ND0612 (acquired by Mitsubishi Tanabe Pharma in 2017), Acorda Therapeutics’ inhaled levodopa, CVT-301, and Sunovion Pharmaceuticals’ sublingual apomorphine, APL-130277 (acquired from Cynapsus Therapeutics). Gene therapy competition for advanced Parkinson’s disease previously included AMT-090 or AAV-GDNF, but this was deprioritized by uniQure in 2016. Oxford Biomedica plc is planning for a Phase 1/2 trial in 2018 for OXB-102, a second generation LentiVector gene therapy.
We expect that our preclinical programs will compete with a variety of therapies in development, including:
|
· |
VY-SOD101 for a monogenic form of ALS will potentially compete with IONIS-SOD1Rx being developed by Ionis Pharmaceuticals, Inc., or Ionis, in collaboration with Biogen Inc., or Biogen, and a gene therapy being developed by AveXis; |
|
· |
VY-FXN01 for Friedreich’s ataxia will potentially compete with AAV-FXN being developed by Adverum Biotechnologies, AAV-FXN being developed by Pfizer, and frataxin targeted gene therapy being developed by Agilis Biotherapeutics, LLC in collaboration with Intrexon Corporation, and BMN 290 being developed by BioMarin Pharmaceutical Inc.; |
|
· |
VY-HTT01 for Huntington’s disease will potentially compete with IONIS-HTTRx being developed by Ionis in collaboration with F. Hoffmann-La Roche Ltd., or Roche, WVE-120101 and WVE-120102 being developed by WAVE Life Sciences in collaboration with Takeda Pharmaceuticals, a Zinc Finger Protein (ZFP) therapy being developed by Sangamo Therapeutics, Inc. in collaboration with Shire plc, and gene therapies being developed by uniQure and Spark; |
|
· |
Our Tau program for tauopathies including Alzheimer’s disease, PSP, and FTD will potentially compete with tau antibodies being developed by Roche Genentech Inc. in collaboration with AC Immune SA, Eli Lilly & Co., AbbVie Inc., Biogen, and several other companies, as well as an antisense oligonucleotide program being developed by Ionis in collaboration with Biogen; and |
|
· |
VY-NAV01 for severe, chronic pain will potentially compete with Nav1.7 inhibitors being developed by Pfizer, Teva Pharmaceuticals, Biogen, Roche Genentech Inc. in collaboration with Xenon Pharmaceuticals, Inc., Amgen, Inc., and Astellas Pharma Inc, and Nav1.8 inhibitors being developed by Vertex Pharmaceuticals, or Vertex. |
In addition, companies that are currently engaged in gene therapy for non-neurological diseases could at any time decide to develop gene therapies for neurological diseases.
Many of our competitors, either alone or with their strategic partners, have substantially greater financial, technical and human resources than we do and significantly greater experience in the discovery and development of product candidates, obtaining FDA and other regulatory approvals of product candidates and commercializing those product candidates. Accordingly, our competitors may be more successful than us in obtaining approval for product candidates and achieving widespread market acceptance. Our competitors’ product candidates may be more effective, or more effectively marketed and sold, than any product candidate we may commercialize and may render our treatments obsolete or non-competitive before we can recover the expenses of developing and commercializing any of our product candidates.
Mergers and acquisitions in the biotechnology and pharmaceutical industries may result in even more resources being concentrated among a smaller number of our competitors. These competitors also compete with us in recruiting and retaining qualified scientific and management personnel and establishing clinical trial sites and subject registration for clinical trials, as well as in acquiring technologies complementary to, or necessary for, our programs. Smaller or
35
early-stage companies may also prove to be significant competitors, particularly through collaborative arrangements with large and established companies.
We anticipate that we will face intense and increasing competition as new product candidates enter the market and advanced technologies become available. We expect any product candidates that we develop and commercialize to compete on the basis of, among other things, efficacy, safety, convenience of administration and delivery, price, and the availability of reimbursement from government and other third-party payers.
Our commercial opportunity could be reduced or eliminated if our competitors develop and commercialize products that are safer, more effective, have fewer or less severe side effects, are more convenient or are less expensive than any products that we may develop. Our competitors also may obtain FDA or other regulatory approval for their product candidates more rapidly than we may obtain approval for ours, which could result in our competitors establishing a strong market position before we are able to enter the market.
Manufacturing
The manufacture of gene therapy products is technically complex, and necessitates substantial expertise and capital investment. Production difficulties caused by unforeseen events may delay the availability of material for our clinical studies. To meet the requirements of our current and planned future trials we have developed a proprietary manufacturing platform that provides a robust and scalable process for AAV production. We are using the baculovirus/Sf9 AAV production system, a technology for producing AAV vectors at scale in insect-derived cells. The process has been successfully transferred to our contract manufacturing organizations where it is used in manufacturing of clinical materials in accordance with the FDA’s current good manufacturing practices, or cGMP. We have also built an onsite, state-of-the-art process research and development facility to enable the manufacturing of high quality AAV gene therapy vectors at laboratory scale.
We presently contract with third parties for the manufacturing of our program materials. We currently have no plans to build our own clinical or commercial scale manufacturing capabilities. The use of contracted manufacturing and reliance on collaboration partners is relatively cost efficient and has eliminated the need for our direct investment in manufacturing facilities and additional staff early in development. Although we rely on contract manufacturers, we have personnel with manufacturing and quality experience to oversee our contract manufacturers.
Intellectual Property
Overview
We strive to protect the proprietary technology, inventions, and know-how to enhance improvements that are commercially important to the development of our business, including seeking, maintaining, and defending patent rights, whether developed internally or licensed from third parties. We also rely on trade secrets and know-how relating to our proprietary technology platform, on continuing technological innovation and on in-licensing opportunities to develop, strengthen and maintain the strength of our position in the field of gene therapy that may be important for the development of our business. We additionally may rely on regulatory protection afforded through data exclusivity, market exclusivity and patent term extensions where available.
Our commercial success may depend in part on our ability to: obtain and maintain patent and other protections for commercially important technology, inventions and know-how related to our business; defend and enforce our patents; preserve the confidentiality of our trade secrets; and operate without infringing the valid enforceable patents and intellectual property rights of third parties. Our ability to stop third parties from making, having made, using, selling, offering to sell or importing our products may depend on the extent to which we have rights under valid and enforceable licenses, patents or trade secrets that cover these activities. In some cases, these rights may need to be enforced by third-party licensors. With respect to both licensed and company-owned intellectual property, we cannot be sure that patents will be granted with respect to any of our pending patent applications or with respect to any patent applications filed by
36
us in the future, nor can we be sure that any of our existing patents or any patents that may be granted to us in the future will be commercially useful in protecting our commercial products and methods of manufacturing the same.
We have 89 patent applications pending in the United States and foreign jurisdictions. At least 24 patent applications have been filed and are pending in the United States and foreign jurisdictions by or on behalf of universities which have granted us exclusive license rights to the technology. To date, 55 patents have issued to our licensors which have granted us exclusive license rights to the technology. To date, 111 patents have issued to our licensors which have granted us non-exclusive license rights to the technology with 22 applications pending. Our policy is to file patent applications to protect technology, inventions and improvements to inventions that are commercially important to the development of our business. We seek United States and international patent protection for a variety of technologies, including: research tools and methods, methods for transferring genetic material into cells, AAV-based biological products, methods of designing novel AAV constructs, methods for treating diseases of interest and methods for manufacturing our AAV-based products. We also intend to seek patent protection or rely upon trade secret rights to protect other technologies that may be used to discover and validate targets and that may be used to identify and develop novel biological products. We seek protection, in part, through confidentiality and proprietary information agreements. We are a party to various other license agreements that give us rights to use specific technologies in our research and development.
Company-Owned Intellectual Property
Parkinson’s Disease
We own three pending patent families with a total of four patent applications directed to AAV constructs encoding the gene AADC for therapeutic uses. Patents that grant from this patent family are generally expected to start to expire in 2035, subject to possible patent term extensions.
ALS
We own three pending patent families with a total of 19 patent applications directed to targeting SOD1 for the treatment of ALS, and we have filed a fourth patent family with three patent applications directed to pharmaceutical compositions and methods for the treatment of ALS to protect our intellectual property arising from a funded grant from The Amyotrophic Lateral Sclerosis Association. Patents that grant from these patent families are generally expected to start to expire in 2035, subject to possible patent term extensions.
Friedreich’s Ataxia and Delivery
We own three pending patent families with two families having a total of six patent applications directed to delivery of AAV gene therapies to the CNS and AAVs encoding frataxin constructs for the treatment of Friedreich’s ataxia and the third family having one patent application directed to the delivery of AAV gene therapies to the CNS. Patents that grant from this patent family are generally expected to start to expire in 2036, subject to possible patent term extensions.
Huntington’s Disease
We own three pending patent families with five patent applications directed to pharmaceutical compositions and methods for targeting HTT for the treatment of Huntington’s disease. Patents from this family are generally expected to start to expire in 2037, subject to possible patent term extensions.
Tauopathies and Antibodies
We own five pending patent families directed to antibodies with a total of six patent applications. The first patent family has one patent application directed to assays for the detection of neutralizing antibodies. The other four
37
patent families have a total of five patent applications directed to vectorized antibodies and other therapies. Patents from these families are generally expected to start to expire in 2036, subject to possible patent term extensions.
Neuropathic Pain
We own one pending patent family with two patent applications directed to pharmaceutical compositions and methods for the treatment of neuropathic pain. Patents from this family are generally expected to start to expire in 2037, subject to possible patent term extensions.
Regulatable Expression
We own two pending patent families with a total of three patent applications directed to regulatable expression control of AAV transgenes. Patents that grant from this patent family are generally expected to start to expire in 2036, subject to possible patent term extensions.
Vector Engineering and Production
We own five pending patent families directed to AAV production and/or engineering. The first family has two patent applications directed to capsid engineering and domain swapping and AAV production. The second family has two patent applications directed to the production of self-complimentary AAV particles. The last three families have a total of 18 patent applications directed to the design of AAV drug delivery cassettes. Patents that grant from this patent family are generally expected to start to expire in 2035, subject to possible patent term extensions.
We own two additional pending patent families with a total of four patent applications directed to methods and compositions for CNS delivery. Patents that grant from this patent family are generally expected to start to expire in 2038, subject to possible patent term extensions.
Licensed Intellectual Property
We have obtained exclusive licenses and non-exclusive licenses to patents directed to both compositions of matter and methods of use.
We have licensed five families of patents and patent applications, in the exclusive field of gene therapy for human diseases, directed to RNAi constructs as vector payloads, their design and use in the treatment of neurological disorders from the University of Massachusetts. These families of patents and applications are pending and/or granted in the United States and other territories and comprises 65 granted patents and 8 applications. Patents have been granted in the United States, Canada, Europe, Israel, Japan, Korea and Australia. Nationalization for some members has taken place in Germany, Spain, France, Great Britain, Italy, and Netherlands. Patents that grant from these patent families are generally expected to expire between 2022 and 2025, subject to possible patent term extensions.
We have exclusively licensed three families of patents and patent applications directed to novel AAV capsids from the University of Massachusetts. These families of patents and applications, pending and/or granted in the United States and other territories, and comprises 17 granted patents and 15 applications. Patents have been granted in the United States, Europe and Japan. Nationalization for some members has taken place in Switzerland, Germany, Denmark, Spain, France, Great Britain, Ireland, Italy, Netherlands, and Sweden. Patents that grant from these patent families are generally expected to expire between 2030 and 2035, subject to possible patent term extensions.
We have non-exclusively licensed a patent family directed to production methods for AAV in insect cells from the NIH, U.S. Department of Health and Human Services. This family of patents is granted in the United States, Canada, Australia and Europe and further nationalized in Germany, France and Great Britain and comprises eight granted patents. Patents that grant from this patent family are generally expected to expire in 2022, subject to possible patent term extensions.
38
We have non-exclusively licensed two families of patents and patent applications directed to novel AAV capsids from the Board of Trustees of the Leland Stanford Junior University. These families of patents and applications, pending and/or granted in the United States, comprise 7 granted patents and 2 applications. Patents that grant from these patent families are generally expected to expire between 2027 and 2032, subject to possible patent term extensions.
We have non-exclusively licensed two families of patents and patent applications directed to AAV capsids from REGENXBIO Inc. These families of patents and patent applications are pending and/or granted in the United States and other territories and comprise 67 granted patents and 10 applications. Patents have been granted in Australia, Brazil, Canada, China, Europe, Hong Kong, Israel, India, Japan, Korea, Mexico, New Zealand, Philippines, Singapore, and the United States. Patents that grant from these patent families are generally expected to expire between 2022 and 2024, subject to possible patent term extensions.
We have non-exclusively licensed two families of patent applications directed to AAV capsids from the California Institute of Technology. These families are pending in the United States and have been filed internationally. Patents that grant from these patent families are generally expected to start to expire in 2034, subject to possible patent term extensions.
Trademark Protection
We own U.S. Reg. Nos. 4,545,283 for the service mark VOYAGER THERAPEUTICS and 4,621,083 for the service mark VOYAGER THERAPEUTICS Logo for “pharmaceutical research and development in the field of gene therapy.” These marks were granted registration on the Principal Register of the United States Patent and Trademark Office, or USPTO, on June 3, 2014 and October 14, 2014, respectively.
We also own pending trademark applications in the USPTO for the marks VOYAGER TRAJECTORY ARRAY GUIDE, V-TAG and the V-TAG Logo, for “medical system comprised of a surgical device for guiding, locating or placing a diagnostic device or therapeutic device, namely, stents, probes, needles, leads, grafts, pumps, syringes, catheters, and implants during a medical procedure and related software sold as a unit, for use in the field of neurology; MRI-compatible medical system comprised of an MRI-compatible surgical device for guiding, locating or placing a diagnostic device or therapeutic device, namely, stents, probes, needles, leads, grafts, pumps, syringes, catheters, and implants during a MRI-guided procedure and related software sold as a unit, for use in the field of neurology,” as well as European Community trademark applications for VOYAGER TRAJECTORY ARRAY GUIDE and V-TAG for these same goods.
We plan to register trademarks in connection with our biological products.
Trade Secret Protection
Finally, we may rely, in some circumstances, on trade secrets to protect our technology. We seek to protect our proprietary technology and processes, in part, by entering into confidentiality agreements with our employees, consultants, scientific advisors and contractors. We also seek to preserve the integrity and confidentiality of our data and trade secrets by maintaining physical security of our premises and physical and electronic security of our information technology systems. While we have confidence in these individuals, organizations and systems, agreements or security measures may be breached, and we may not have adequate remedies for any breach. In addition, our trade secrets may otherwise become known or be independently discovered by competitors. To the extent that our consultants, contractors or collaborators use intellectual property owned by others in their work for us, disputes may arise as to the rights in related or resulting know-how and inventions.
Government Regulation and Product Approval
In the United States, biological products, including gene therapy products, are licensed by FDA for marketing under the Public Health Service Act, or PHS Act, and regulated under the Federal Food, Drug, and Cosmetic Act, or
39
FDCA. Both the FDCA and the PHS Act and their corresponding regulations govern, among other things, the testing, manufacturing, safety, purity, potency, efficacy, labeling, packaging, storage, record keeping, distribution, import, export, reporting, advertising and other promotional practices involving biological products. FDA clearance must be obtained before clinical testing of biological products, and each clinical study protocol for a gene therapy product is reviewed by the FDA and, in some instances, the NIH, through its RAC. FDA licensure also must be obtained before marketing of biological products. The process of obtaining regulatory approvals and the subsequent compliance with appropriate federal, state, local and foreign statutes and regulations require the expenditure of substantial time and financial resources.
Within the FDA, the Center for Biologics Evaluation and Research, or CBER, regulates gene therapy products. Within CBER, the Office of Tissues and Advanced Therapies (OTAT) is responsible for gene therapy review and evaluation. CBER works closely with the NIH and its RAC, which makes recommendations to the NIH on gene therapy issues and engages in a public discussion of scientific, safety, ethical and societal issues related to proposed and ongoing gene therapy protocols. The FDA and the NIH have published guidance documents with respect to the development and submission of gene therapy protocols. The FDA also has published guidance documents related to, among other things, gene therapy products in general, their preclinical assessment, observing subjects involved in gene therapy studies for delayed adverse events, viral shedding, environmental assessments, potency testing, and chemistry, manufacturing and control information in gene therapy INDs. FDA guidance documents provide the agency’s current thinking about a particular subject but are not legally binding.
U.S. Biological Products Development Process
The process required by the FDA before a biological product may be marketed in the United States generally involves the following:
|
· |
completion of nonclinical laboratory tests and animal studies according to good laboratory practice, or GLPs, and applicable requirements for the humane use of laboratory animals or other applicable regulations; |
|
· |
submission to the FDA of an application for an IND, which must become effective before human clinical trials may begin; |
|
· |
approval by an institutional review board, or IRB, reviewing each clinical site before each clinical trial may be initiated; |
|
· |
approval by an institutional biosafety committee, or IBC, assessing the safety of the clinical research and identifying any potential risk to public health or the environment; |
|
· |
performance of adequate and well-controlled human clinical trials according to the FDA’s regulations commonly referred to as good clinical practice, or GCPs, and any additional requirements for the protection of human research subjects and their health information, to establish the safety, purity, potency, and efficacy, of the proposed biological product for its intended use; |
|
· |
submission to the FDA of a Biologics License Application, or BLA, for marketing approval that includes substantive evidence of safety, purity, potency, and efficacy from results of nonclinical testing and clinical trials; |
|
· |
satisfactory completion of an FDA inspection of the manufacturing facility or facilities where the biological product is produced to assess compliance with cGMP, to assure that the facilities, methods and controls are adequate to preserve the biological product’s identity, strength, quality and purity; |
|
· |
potential FDA audit of the nonclinical and clinical study sites that generated the data in support of the BLA; |
|
· |
potential FDA Advisory Committee meeting to elicit expert input on critical issues and including a vote by external Committee members; |
|
· |
FDA review and approval, or licensure, of the BLA, and payment of associated user fees; and |
40
Before testing any biological product candidate, including a gene therapy product, in humans, the product candidate enters the preclinical testing stage. Preclinical tests, also referred to as nonclinical tests, include laboratory evaluations of product chemistry, toxicity and formulation, as well as animal studies to assess the potential safety and activity of the product candidate. The conduct of the preclinical tests must comply with federal regulations and requirements including GLPs.
Where a gene therapy study is conducted at, or sponsored by, institutions receiving NIH funding for recombinant DNA research, prior to the submission of an IND to the FDA, a protocol and related documentation is submitted to and the study is registered with the NIH Office of Biotechnology Activities, or OBA, pursuant to the NIH Guidelines for Research Involving Recombinant DNA Molecules, or NIH Guidelines. Compliance with the NIH Guidelines is mandatory for investigators at institutions receiving NIH funds for research involving recombinant DNA, however many companies and other institutions not otherwise subject to the NIH Guidelines voluntarily follow them. The NIH is responsible for convening the NIH Office of Biotechnology Activities’ Recombinant DNA Advisory Committee, or the RAC, a federal advisory committee, that discusses protocols that raise novel or particularly important scientific, safety or ethical considerations at one of its quarterly public meetings. The OBA will notify the FDA of the RAC’s decision regarding the necessity for full public review of a gene therapy protocol. RAC proceedings and reports are posted to the OBA website and may be accessed by the public. Recent changes in the procedures for the RAC process issued by the NIH now include evaluation and assessment by independent IRBs and may result in some delay before initiation of a clinical trial. Annual reporting of clinical trial data including safety information also is required.
The clinical study sponsor must submit the results of the preclinical tests, together with manufacturing information, analytical data, any available clinical data or literature and a proposed clinical protocol, to the FDA as part of the IND. Some preclinical testing typically continues after the IND is submitted. An IND is an exemption from the FDCA that allows an unapproved product to be shipped in interstate commerce for use in an investigational clinical trial and a request for FDA authorization to administer an investigational product to humans. The IND automatically becomes effective 30 days after receipt by the FDA, unless the FDA requests certain changes to a protocol before the study can begin, or the FDA places the clinical study on a clinical hold within that 30-day time period. In such a case, the IND sponsor and the FDA must resolve any outstanding concerns before the clinical study can begin. With gene therapy protocols, if the FDA allows the IND to proceed, but the RAC decides that full public review of the protocol is warranted, the FDA will request at the completion of its IND review that sponsors delay initiation of the protocol until after completion of the RAC review process. The FDA may also impose clinical holds on a biological product candidate at any time before or during clinical trials due to safety concerns or non-compliance. If the FDA imposes a clinical hold, studies may not recommence without FDA authorization and then only under terms authorized by the FDA. Accordingly, we cannot be sure that submission of an IND will result in the FDA allowing clinical trials to begin, or that, once begun, issues will not arise that suspend or terminate such studies.
Clinical trials involve the administration of the biological product candidate to healthy volunteers or subjects under the supervision of qualified investigators, generally physicians not employed by or under the study sponsor’s control. Clinical trials are conducted under protocols detailing, among other things, the objectives of the clinical study, dosing procedures, subject selection and exclusion criteria, and the parameters to be used to monitor subject safety, including stopping rules that assure a clinical study will be stopped if certain adverse events should occur. Each protocol and any amendments to the protocol must be submitted to the FDA as part of the IND. Clinical trials must be conducted and monitored in accordance with the FDA’s regulations comprising the GCP requirements, including the requirement that all research subjects provide informed consent. Further, each clinical study must be reviewed and approved by an independent IRB, at or servicing each institution at which the clinical study will be conducted. An IRB is charged with protecting the welfare and rights of study participants and considers such items as whether the risks to individuals participating in the clinical trials are minimized and are reasonable in relation to anticipated benefits. The IRB also approves the form and content of the informed consent that must be signed by each clinical study subject or his or her
41
legal representative and must monitor the clinical study until completed. Additionally, some trials are overseen by an independent group of qualified experts organized by the trial sponsor, known as a data safety monitoring board or committee. Clinical trials involving recombinant or synthetic (or both) nucleic acid molecules performed at or sponsored by an institution that receives any NIH funding for such research also must be reviewed by an IBC, a local institutional committee that reviews and oversees basic and clinical research conducted at that institution. The IBC assesses the safety of the research and identifies any potential risk to public health or the environment.
Human clinical trials are typically conducted in three sequential phases that may overlap or be combined:
|
· |
Phase 1. The biological product is initially introduced into healthy human subjects and tested for safety. In the case of some products for severe or life-threatening diseases, especially when the product may be too inherently toxic to ethically administer to healthy volunteers, the initial human testing is often conducted in patients. Guidelines on clinical trials with gene therapy products issued by OTAT state that the FDA has determined that the benefit-risk ratio of these products does not warrant their evaluation in healthy human subjects. |
|
· |
Phase 2. The biological product is evaluated in a limited patient population to identify possible adverse effects and safety risks, to preliminarily evaluate the efficacy of the product for specific targeted diseases and to determine dosage tolerance, optimal dosage and dosing schedule. |
|
· |
Phase 3. Clinical trials are undertaken to further evaluate dosage, clinical efficacy, potency and safety in an expanded patient population at geographically dispersed clinical trial sites. These clinical trials are intended to establish the overall risk/benefit ratio of the product and provide an adequate basis for product labeling. |
Post-approval clinical trials, sometimes referred to as Phase 4 clinical trials, may be conducted after initial marketing approval. These clinical trials are used to gain additional experience from the treatment of patients in the intended therapeutic indication, particularly for long-term safety follow-up. The FDA recommends that sponsors observe subjects for potential gene therapy-related delayed adverse events for a 15-year period, including a minimum of five years of annual examinations followed by ten years of annual queries, either in person or by questionnaire, of trial subjects.
During all phases of clinical development, regulatory agencies require extensive monitoring and auditing of all clinical activities, clinical data, and clinical trial investigators. Annual progress reports detailing the results of the clinical trials must be submitted to the FDA. Written IND safety reports must be promptly submitted to the FDA, the NIH and the investigators for serious and unexpected adverse events, any findings from other studies, tests in laboratory animals or in vitro testing that suggest a significant risk for human subjects, or any clinically important increase in the rate of a serious suspected adverse reaction over that listed in the protocol or investigator brochure. The sponsor must submit an IND safety report within 15 calendar days after the sponsor determines that the information qualifies for reporting. The sponsor also must notify the FDA of any unexpected fatal or life-threatening suspected adverse reaction within seven calendar days after the sponsor’s initial receipt of the information. Phase 1, Phase 2 and Phase 3 clinical trials may not be completed successfully within any specified period, if at all. The FDA or the sponsor or its data safety monitoring board may suspend a clinical trial at any time on various grounds, including a finding that the research subjects or patients are being exposed to an unacceptable health risk. Similarly, an IRB can suspend or terminate approval of a clinical trial at its institution if the clinical trial is not being conducted in accordance with the IRB’s requirements or if the biological product has been associated with unexpected serious harm to patients.
Human gene therapy products are a new category of therapeutics. Because this is a relatively new and expanding area of novel therapeutic interventions, there can be no assurance as to the length of the study period, the number of patients the FDA will require to be enrolled in the studies in order to establish the safety, efficacy, purity and potency of human gene therapy products, or that the data generated in these studies will be acceptable to the FDA to support marketing approval. The NIH and the FDA have a publicly accessible database, the Genetic Modification Clinical Research Information System which includes information on gene transfer studies and serves as an electronic tool to facilitate the reporting and analysis of adverse events on these studies.
42
Concurrent with clinical trials, companies usually complete additional animal studies and must also develop additional information about the physical characteristics of the biological product as well as finalize a process for manufacturing the product in commercial quantities in accordance with cGMP requirements. To help reduce the risk of the introduction of adventitious agents with use of biological products, the PHS Act emphasizes the importance of manufacturing control for products whose attributes cannot be precisely defined. The manufacturing process must be capable of consistently producing quality batches of the product candidate and, among other things, the sponsor must develop methods for testing the identity, strength, quality, potency and purity of the final biological product. Additionally, appropriate packaging must be selected and tested and stability studies must be conducted to demonstrate that the biological product candidate does not undergo unacceptable deterioration over its shelf life.
Information about certain clinical trials must be submitted within specific timeframes to the NIH for public dissemination on its ClinicalTrials.gov website.
U.S. Review and Approval Processes
After the completion of clinical trials of a biological product, FDA approval of a BLA, must be obtained before commercial marketing of the biological product. The BLA must include results of product development, laboratory and animal studies, human studies, information on the manufacture and composition of the product, proposed labeling and other relevant information. In addition, under the Pediatric Research Equity Act, or PREA, a BLA or supplement to a BLA must contain data to assess the safety and effectiveness of the biological product for the claimed indications in all relevant pediatric subpopulations and to support dosing and administration for each pediatric subpopulation for which the product is safe and effective. The FDA may grant deferrals for submission of data or full or partial waivers. Unless otherwise required by regulation, PREA does not apply to any biological product for an indication for which orphan designation has been granted. The testing and approval processes require substantial time and effort and there can be no assurance that the FDA will accept the BLA for filing and, even if filed, that any approval will be granted on a timely basis, if at all.
Under the Prescription Drug User Fee Act, or PDUFA, as amended, each BLA must be accompanied by a significant user fee. According to the FDA’s fee schedule, effective from October 1, 2017 through September 30, 2018, the user fee for an application requiring clinical data is more than $2 million. The sponsor of an approved application is also subject to an annual program fee, which for fiscal year 2018 is more than $0.3 million. Fee waivers or reductions are available in certain circumstances, including a waiver of the application fee for the first application filed by a small business. Additionally, no user fees are assessed on BLAs for product candidates designated as orphan drugs, unless the product candidate also includes a non-orphan indication.
Within 60 days following submission of the application, the FDA reviews a BLA submitted to determine if it is substantially complete before the agency accepts it for filing. The FDA may refuse to file any BLA that it deems incomplete or not properly reviewable at the time of submission and may request additional information. In this event, the BLA must be resubmitted with the additional information. The resubmitted application also is subject to review before the FDA accepts it for filing. The application also needs to be published and submitted in an electronic format that can be processed through the FDA’s electronic systems. If the electronic submission is not compatible with FDA’s systems, the BLA can be refused to file. Once the submission is accepted for filing, the FDA begins an in-depth substantive review of the BLA. The FDA reviews the BLA to determine, among other things, whether the proposed product is safe, potent, and effective, for its intended use, and has an acceptable purity profile, and whether the product is being manufactured in accordance with cGMP to assure and preserve the product’s identity, safety, strength, quality, potency and purity. The FDA may refer applications for novel biological products or biological products that present difficult questions of safety or efficacy to an advisory committee, typically a panel that includes clinicians and other experts, for review, evaluation and a recommendation as to whether the application should be approved and under what conditions. The FDA is not bound by the recommendations of an advisory committee, but it considers such recommendations carefully when making decisions. During the biological product approval process, the FDA also will determine whether a Risk Evaluation and Mitigation Strategy, or REMS, is necessary to assure the safe use of the biological product. If the FDA concludes a REMS is needed, the sponsor of the BLA must submit a proposed REMS; the FDA will not approve the BLA without a REMS, if required.
43
Before approving a BLA, the FDA will inspect the facilities at which the product is manufactured. The FDA will not approve the product unless it determines that the manufacturing processes and facilities are in compliance with cGMP requirements and adequate to assure consistent production of the product within required specifications. Additionally, before approving a BLA, the FDA will typically inspect one or more clinical trial sites to assure that the clinical trials were conducted in compliance with IND study requirements and GCP requirements. To assure cGMP and GCP compliance, an applicant must incur significant expenditure of time, money and effort in the areas of training, record keeping, production, and quality control.
Notwithstanding the submission of relevant data and information, the FDA may ultimately decide that the BLA does not satisfy its regulatory criteria for approval and deny approval. Data obtained from clinical trials are not always conclusive and the FDA may interpret data differently than we interpret the same data. If the agency decides not to approve the BLA in its present form, the FDA will issue a complete response letter that usually describes all of the specific deficiencies in the BLA identified by the FDA. The deficiencies identified may be minor, for example, requiring labeling changes, or major, for example, requiring additional clinical trials. Additionally, the complete response letter may include recommended actions that the applicant might take to place the application in a condition for approval. If a complete response letter is issued, the applicant may either resubmit the BLA, addressing all of the deficiencies identified in the letter, or withdraw the application.
If a product receives regulatory approval, the approval may be significantly limited to specific diseases and dosages or the indications for use may otherwise be limited, which could restrict the commercial value of the product. Further, the FDA may require that certain contraindications, warnings or precautions be included in the product labeling. The FDA may impose restrictions and conditions on product distribution, prescribing, or dispensing in the form of a risk management plan, or otherwise limit the scope of any approval. In addition, the FDA may require post marketing clinical trials, sometimes referred to as Phase 4 clinical trials, designed to further assess a biological product’s safety and effectiveness, and testing and surveillance programs to monitor the safety of approved products that have been commercialized. As a condition for approval, the FDA may also require additional non-clinical testing as a Phase 4 commitment.
One of the performance goals agreed to by the FDA under the PDUFA is to review standard BLAs in 10 months from filing and priority BLAs in six months from filing, whereupon a review decision is to be made. The FDA does not always meet its PDUFA goal dates for standard and priority BLAs and its review goals are subject to change from time to time. The review process and the PDUFA goal date may be extended by three months if the FDA requests or the BLA sponsor otherwise provides additional information or clarification regarding information already provided in the submission within the last three months before the PDUFA goal date.
Post-Approval Requirements
Maintaining substantial compliance with applicable federal, state, and local statutes and regulations requires the expenditure of substantial time and financial resources. Rigorous and extensive FDA regulation of biological products continues after approval, particularly with respect to cGMP. We will rely, and expect to continue to rely, on third parties for the production of clinical and commercial quantities of any products that we may commercialize. Manufacturers of our products are required to comply with applicable requirements in the cGMP regulations, including quality control and quality assurance and maintenance of records and documentation. Following approval, the manufacturing facilities are subject to biennial inspections by the FDA’s biologics team and such inspections may result in an issuance of FDA Form 483 deficiency observations or a warning letter, which can lead to plant shutdown and other more serious penalties and fines. Prior to the institution of any manufacturing changes, a determination needs to be made whether FDA approval is required in advance. If not done in accordance with FDA expectations, the FDA may restrict supply and may take further action. Annual product reports are required to be submitted annually. Other post-approval requirements applicable to biological products, include reporting of cGMP deviations that may affect the identity, potency, purity and overall safety of a distributed product, record-keeping requirements, reporting of adverse effects, reporting updated safety and efficacy information, and complying with electronic record and signature requirements. After a BLA is approved, the product also may be subject to official lot release. As part of the manufacturing process, the manufacturer is required to perform certain tests on each lot of the product before it is released for distribution. If the product is subject to official release by
44
the FDA, the manufacturer submits samples of each lot of product to the FDA together with a release protocol showing a summary of the history of manufacture of the lot and the results of all of the manufacturer’s tests performed on the lot. The FDA also may perform certain confirmatory tests on lots of some products, such as viral vaccines, before releasing the lots for distribution by the manufacturer. In addition, the FDA conducts laboratory research related to the regulatory standards on the safety, purity, potency, and effectiveness of biological products. Systems need to be put in place to record and evaluate adverse events reported by health care providers and patients and to assess product complaints. An increase in severity or new adverse events can result in labeling changes or product recall. Defects in manufacturing of commercial products can result in product recalls.
We also must comply with the FDA’s advertising and promotion requirements, such as those related to direct-to-consumer advertising, the prohibition on promoting products for uses or in patient populations that are not described in the product’s approved labeling (known as “off-label use”), industry-sponsored scientific and educational activities, and promotional activities involving the internet. Discovery of previously unknown problems or the failure to comply with the applicable regulatory requirements may result in restrictions on the marketing of a product or withdrawal of the product from the market as well as possible civil or criminal sanctions. Failure to comply with the applicable U.S. requirements at any time during the product development process, approval process or after approval, may subject an applicant or manufacturer to administrative or judicial civil or criminal sanctions and adverse publicity. FDA sanctions could include refusal to approve pending applications, withdrawal of an approval or license revocation, clinical hold, warning or untitled letters, product recalls, product seizures, total or partial suspension of production or distribution, injunctions, fines, refusals of government contracts, mandated corrective advertising or communications with doctors, debarment, restitution, disgorgement of profits, or civil or criminal penalties. Any agency or judicial enforcement action could have a material adverse effect on us.
Biological product manufacturers and other entities involved in the manufacture and distribution of approved biological products are required to register their establishments with the FDA and certain state agencies, and are subject to periodic unannounced inspections by the FDA and certain state agencies for compliance with cGMPs and other laws. Accordingly, manufacturers must continue to expend time, money, and effort in the area of production and quality control to maintain cGMP compliance. Discovery of problems with a product after approval may result in restrictions on a product, manufacturer, or holder of an approved BLA, including withdrawal of the product from the market. In addition, changes to the manufacturing process or facility generally require prior FDA approval before being implemented and other types of changes to the approved product, such as adding new indications and additional labeling claims, are also subject to further FDA review and approval.
Orphan Drug Designation
Under the Orphan Drug Act, the FDA may grant Orphan Drug Designation, or ODD, to a drug or biological product intended to treat a rare disease or condition, which is generally a disease or condition that affects fewer than 200,000 individuals in the United States, or more than 200,000 individuals in the United States and for which there is no reasonable expectation that the cost of developing and making a drug or biological product available in the United States for this type of disease or condition will be recovered from sales of the product. ODD must be requested before submitting a BLA. After the FDA grants ODD, the identity of the therapeutic agent and its potential orphan use are disclosed publicly by the FDA. ODD does not convey any advantage in or shorten the duration of the regulatory review and approval process.
If a product that has ODD receives the first FDA approval for the disease or condition for which it has such designation, the product is entitled to orphan product exclusivity, which means that the FDA may not approve any other applications to market the same biological product for the same indication for seven years, except in limited circumstances, such as a showing of clinical superiority to the product with orphan exclusivity. This is the case despite an earlier court opinion holding that the Orphan Drug Act unambiguously required the FDA to recognize orphan exclusivity regardless of a showing of clinical superiority.
45
Competitors, however, may receive approval of different products for the indication for which the orphan product has exclusivity or obtain approval for the same product but for a different indication for which the orphan product has exclusivity. Orphan product exclusivity also could block the approval of one of our products for seven years if a competitor obtains approval of the same biological product as defined by the FDA or if our product candidate is determined to be contained within the competitor’s product for the same indication or disease. If a biological product designated as an orphan product receives marketing approval for an indication broader than what is designated, it may not be entitled to orphan product exclusivity.
Expedited Review and Approval Programs
The FDA has various programs, including fast track designation, priority review, accelerated approval, and breakthrough therapy designation, that are intended to expedite or simplify the process for the development and FDA review of biological products that are intended for the treatment of serious or life-threatening diseases or conditions and demonstrate the potential to address unmet medical needs. The purpose of these programs is to provide important new biological products to patients earlier than under standard FDA review procedures. To be eligible for a fast track designation, the FDA must determine, based on the request of a sponsor, that a biological product is intended to treat a serious or life-threatening disease or condition and demonstrates the potential to address an unmet medical need. The FDA will determine that a product will fill an unmet medical need if it will provide a therapy where none exists or provide a therapy that may be potentially superior to existing therapy based on efficacy or safety factors. In addition to other benefits, such as the ability to have greater interactions with the FDA, the FDA may initiate review of sections of a Fast Track BLA before the application is complete, a process known as rolling review.
The FDA may give a priority review designation to biological products that treats a serious condition and, if approved, would provide a significant improvement in safety or effectiveness. A priority review means that the goal for the FDA to review an application is six months, rather than the standard review of ten months under current PDUFA guidelines. Most products that are eligible for fast track designation may also be considered appropriate to receive a priority review.
In addition, biological products studied for their safety and effectiveness in treating serious or life-threatening illnesses and that provide meaningful therapeutic benefit over existing treatments may receive accelerated approval and may be approved on the basis of adequate and well-controlled clinical trials establishing that the biological product has an effect on a surrogate endpoint that is reasonably likely to predict clinical benefit, or on a clinical endpoint that can be measured earlier than irreversible morbidity or mortality, that is reasonably likely to predict an effect on irreversible morbidity or mortality or other clinical benefit, taking into account the severity, rarity or prevalence of the condition and the availability or lack of alternative treatments. As a condition of approval, the FDA may require a sponsor of a biological product receiving accelerated approval to perform post-marketing studies to verify and describe the predicted effect on irreversible morbidity or mortality or other clinical endpoint, and the biological product may be subject to accelerated withdrawal procedures.
Moreover, under the Food and Drug Administration Safety and Innovation Act enacted in 2012, a sponsor can request designation of a product candidate as a “breakthrough therapy.” A breakthrough therapy is defined as a biological product that is intended, alone or in combination with one or more other drugs, to treat a serious or life-threatening disease or condition, and preliminary clinical evidence indicates that the biological product may demonstrate substantial improvement over existing therapies on one or more clinically significant endpoints, such as substantial treatment effects observed early in clinical development. Biological products designated as breakthrough therapies are also eligible for accelerated approval. The FDA must take certain actions, such as holding timely meetings and providing advice, intended to expedite the development and review of an application for approval of a breakthrough therapy.
Even if a product qualifies for one or more of these programs, the FDA may later decide that the product no longer meets the conditions for qualification or decide that the time period for FDA review or approval will not be shortened. Furthermore, fast track designation, priority review, accelerated approval and breakthrough therapy designation, do not change the standards for approval and may not ultimately expedite the development or approval process.
46
Expedited programs for regenerative medicine therapies for serious conditions
As part of the 21st Century Cures Act, Congress amended the FDCA to create an expedited development and approval program for regenerative medicine advanced therapies, which include cell therapies, therapeutic tissue engineering products, human cell and tissue products, and combination products using any such therapies or products. As of November 2017, the FDA has interpreted this definition as follows: gene therapies, including genetically modified cells, that lead to a durable modification of cells or tissues may meet the definition of a regenerative medicine advanced therapy. At this time, it is not known if our in vitro gene therapies will qualify as a regenerative medicine advanced therapy based on this definition. Regenerative medicine advanced therapies do not include those human cells, tissues, and cellular and tissue-based products regulated solely under section 361 of the Public Health Service Act and 21 CFR Part 1271. The new program is intended to facilitate efficient development and expedite review of regenerative medicine advanced therapies, which are intended to treat, modify, reverse, or cure a serious or life-threatening disease or condition.
A drug sponsor may request that the FDA designate a drug as a regenerative medicine advanced therapy concurrently with or at any time after submission of an IND. The FDA has 60 calendar days to determine whether the drug meets the criteria, including whether there is preliminary clinical evidence indicating that the drug has the potential to address unmet medical needs for a serious or life-threatening disease or condition. A new drug application or BLA for a regenerative medicine advanced therapy may be eligible for priority review or accelerated approval through (1) surrogate or intermediate endpoints reasonably likely to predict long-term clinical benefit or (2) reliance upon data obtained from a meaningful number of sites. Benefits of such designation also include early interactions with the FDA to discuss any potential surrogate or intermediate endpoint to be used to support accelerated approval. A regenerative medicine advanced therapy that is granted accelerated approval and is subject to post-approval requirements may fulfill such requirements through the submission of clinical evidence, clinical studies, patient registries, or other sources of real world evidence, such as electronic health records; the collection of larger confirmatory data sets; or post-approval monitoring of all patients treated with such therapy prior to its approval.
U.S. Patent Term Restoration
Depending upon the timing, duration and specifics of the FDA approval of the use of our product candidates, some of our U.S. patents may be eligible for limited patent term extension under the Drug Price Competition and Patent Term Restoration Act of 1984, commonly referred to as the Hatch-Waxman Amendments. The Hatch-Waxman Amendments permit a patent restoration term of up to five years as compensation for patent term lost during product development and the FDA regulatory review process. However, patent term restoration cannot extend the remaining term of a patent beyond a total of 14 years from the product’s approval date. The patent term restoration period is generally one-half the time between the effective date of an IND and the submission date of a BLA plus the time between the submission date of a BLA and the approval of that application, less any time the applicant failed to act with due diligence. Only one patent applicable to an approved biological product is eligible for the extension and the application for the extension must be submitted prior to the expiration of the patent. The U.S. Patent and Trademark Office, in consultation with the FDA, reviews and approves the application for any patent term extension or restoration. In the future, we may intend to apply for restoration of patent term for one of our currently owned or licensed patents to add patent life beyond its current expiration date, depending on the expected length of the clinical trials and other factors involved in the filing of the relevant BLA.
Market and Data Exclusivity
The 2010 Patient Protection and Affordable Care Act, or the ACA, which was signed into law on March 23, 2010, included a subtitle called the Biologics Price Competition and Innovation Act of 2009 or BPCIA. The BPCIA established a regulatory scheme authorizing the FDA to approve biosimilars and interchangeable biosimilars. As of January 1, 2018, the FDA has approved nine biosimilar products for use in the United States. No interchangeable biosimilars have been approved. The FDA has issued several guidance documents outlining an approach to review and approval of biosimilars. Additional guidance is expected to be finalized by FDA in the near term.
47
Under the BPCIA, a manufacturer may submit an application for licensure of a biologic product that is “biosimilar to” or “interchangeable with” a previously approved biological product or “reference product.” In order for the FDA to approve a biosimilar product, it must find that there are no clinically meaningful differences between the reference product and proposed biosimilar product in terms of safety, purity and potency. For the FDA to approve a biosimilar product as interchangeable with a reference product, the FDA must find that the biosimilar product can be expected to produce the same clinical results as the reference product, and (for products administered multiple times) that the biologic and the reference biologic may be switched after one has been previously administered without increasing safety risks or risks of diminished efficacy relative to exclusive use of the reference biologic.
Under the BPCIA, an application for a biosimilar product may not be submitted to the FDA until four years following the date of approval of the reference product. The FDA may not approve a biosimilar product until 12 years from the date on which the reference product was approved. Even if a product is considered to be a reference product eligible for exclusivity, another company could market a competing version of that product if the FDA approves a full BLA for such product containing the sponsor’s own preclinical data and data from adequate and well-controlled clinical trials to demonstrate the safety, purity and potency of their product. The BPCIA also created certain exclusivity periods for biosimilars approved as interchangeable products. At this juncture, it is unclear whether products deemed “interchangeable” by the FDA will, in fact, be readily substituted by pharmacies, which are governed by state pharmacy law.
Pediatric exclusivity is another type of non-patent exclusivity in the United States and, if granted, provides for the attachment of an additional six months of marketing protection to the term of any existing regulatory exclusivity or patent protection, including the non‑patent and orphan exclusivity. This six‑month exclusivity may be granted if an application sponsor submits pediatric data that fairly respond to a written request from the FDA for such data. The data do not need to show the product to be effective in the pediatric population studied; rather, if the clinical trial is deemed to fairly respond to the FDA’s request, the additional protection is granted. If reports of requested pediatric studies are submitted to and accepted by the FDA within the statutory time limits, whatever statutory or regulatory periods of exclusivity or patent protection cover the product are extended by six months. Thus, pediatric exclusivity adds six months to existing exclusivity periods applicable to biological products under the BPCIA—namely, the four-year period during which the FDA will not consider an application for a biosimilar product, and the 12-year period during which the FDA will not approve a biosimilar application.
Other Healthcare Laws
Although we currently do not have any products on the market, we may be subject to additional healthcare regulation and enforcement by the federal government and by authorities in the states in which we conduct our business. Such laws include, without limitation, state and federal anti-kickback, fraud and abuse, false claims, privacy and security and physician sunshine laws and regulations, many of which may become more applicable to us if our product candidates are approved and we begin commercialization. If our operations are found to be in violation of any of such laws or any other governmental regulations that apply to us, we may be subject to penalties, including, without limitation, administrative, civil and criminal penalties, damages, fines, disgorgement, the curtailment or restructuring of our operations, exclusion from participation in federal and state healthcare programs and imprisonment, any of which could adversely affect our ability to operate our business and our financial results.
In addition, the Affordable Care Act is intended to broaden access to health insurance, reduce or constrain the growth of healthcare spending, enhance remedies against fraud and abuse, add transparency requirements for the healthcare and health insurance industries, impose taxes and fees on the health industry and impose additional health policy reforms. With regard to biopharmaceutical products, in addition to the Biologics Price Competition and Innovation Act of 2009 included in the Affordable Care Act, among other things, the Affordable Care Act expanded and increased industry rebates for drugs covered under Medicaid programs and made changes to the coverage requirements under the Medicare prescription drug benefit. Some of the provisions of the Affordable Care Act have yet to be fully implemented, while certain provisions have been subject to judicial and Congressional challenges. In January 2017,
48
Congress voted to adopt a budget resolution for fiscal year 2017, that while not a law, is widely viewed as the first step toward the passage of legislation that would repeal certain aspects of the Affordable Care Act.
Further, on January 20, 2017, President Trump signed an Executive Order directing federal agencies with authorities and responsibilities under the Affordable Care Act to waive, defer, grant exemptions from, or delay the implementation of any provision of the Affordable Care Act that would impose a fiscal burden on states or a cost, fee, tax, penalty or regulatory burden on individuals, healthcare providers, health insurers, or manufacturers of pharmaceuticals or medical devices. Congress also could consider subsequent legislation to replace elements of the Affordable Care Act that are repealed. In the coming years, additional legislative and regulatory changes could be made to governmental health programs that could significantly impact the biopharmaceutical industry and the success of our product candidates. The Affordable Care Act, as well as other federal, state and foreign healthcare reform measures that have been and may be adopted in the future, could harm our future revenues.
With enactment of the Tax Cuts and Jobs Act of 2017, which was signed by the President on December 22, 2017, Congress repealed the “individual mandate.” The repeal of this provision, which requires most Americans to carry a minimal level of health insurance, will become effective in 2019. According to the Congressional Budget Office, the repeal of the individual mandate will cause 13 million fewer Americans to be insured in 2027 and premiums in insurance markets may rise. Additionally, on January 22, 2018, President Trump signed a continuing resolution on appropriations for fiscal year 2018 that delayed the implementation of certain ACA-mandated fees, including the so-called “Cadillac” tax on certain high cost employer-sponsored insurance plans, the annual fee imposed on certain health insurance providers based on market share, and the medical device excise tax on non-exempt medical devices. The Congress will likely consider other legislation to replace elements of the ACA, during the next Congressional session.
There have also been several recent U.S. congressional inquiries and proposed federal and proposed and enacted state legislation designed to, among other things, bring more transparency to product pricing, review the relationship between pricing and manufacturer patient programs, reduce the costs of products under Medicare and reform government program reimbursement methodologies for products. At the federal level, Congress and the Trump administration have each indicated that it will continue to seek new legislative and/or administrative measures to control costs. At the state level, individual states are increasingly aggressive in passing legislation and implementing regulations designed to control pharmaceutical and biological product pricing, including price or patient reimbursement constraints, discounts, restrictions on certain product access and marketing cost disclosure and transparency measures, and, in some cases, designed to encourage importation from other countries and bulk purchasing. In addition, regional health care authorities and individual hospitals are increasingly using bidding procedures to determine what pharmaceutical products and which suppliers will be included in their prescription product and other health care programs. These measures could reduce the ultimate demand for our products, once approved, or put pressure on our product pricing.
Additional Regulation
In addition to the foregoing, state and federal laws regarding environmental protection and hazardous substances, including the Occupational Safety and Health Act, the Resource Conservancy and Recovery Act and the Toxic Substances Control Act, affect our business. These and other laws govern our use, handling and disposal of various biological, chemical and radioactive substances used in, and wastes generated by, our operations. If our operations result in contamination of the environment or expose individuals to hazardous substances, we could be liable for damages and governmental fines. We believe that we are in material compliance with applicable environmental laws and that continued compliance therewith will not have a material adverse effect on our business. We cannot predict, however, how changes in these laws may affect our future operations.
U.S. Foreign Corrupt Practices Act
The U.S. Foreign Corrupt Practices Act, to which we are subject, prohibits corporations and individuals from engaging in certain activities to obtain or retain business or to influence a person working in an official capacity. It is illegal to pay, offer to pay or authorize the payment of anything of value to any foreign government official, government
49
staff member, political party or political candidate in an attempt to obtain or retain business or to otherwise influence a person working in an official capacity.
Review and Clearance of Companion Diagnostics in the United States
If safe and effective use of a therapeutic depends on an in vitro diagnostic, then the FDA generally will require approval or clearance of that diagnostic, known as a companion diagnostic, at the same time that the FDA approves the therapeutic product. In August 2014, the FDA issued final guidance clarifying the requirements that will apply to approval of therapeutic products and in vitro companion diagnostics. According to the guidance, for novel drugs, a companion diagnostic device and its corresponding therapeutic should be approved or cleared contemporaneously by the FDA for the use indicated in the therapeutic product’s labeling. In July 2016, the FDA issued a draft guidance intended to assist sponsors of the drug therapeutic and in vitro companion diagnostic device on issues related to co-development of the products.
If FDA determines that a companion diagnostic device is essential to the safe and effective use of a novel therapeutic product or indication, FDA generally will not approve the therapeutic product or new therapeutic product indication if the companion diagnostic device is not approved or cleared for that indication. Approval or clearance of the companion diagnostic device will ensure that the device has been adequately evaluated and has adequate performance characteristics in the intended population. The review of in vitro companion diagnostics in conjunction with the review of our therapeutic treatments for cancer will, therefore, likely involve coordination of review by the FDA’s Center for Drug Evaluation and Research and the FDA’s Center for Devices and Radiological Health Office of In Vitro Diagnostics Device Evaluation and Safety.
Under the FDCA, in vitro diagnostics, including companion diagnostics, are regulated as medical devices. In the United States, the FDCA and its implementing regulations, and other federal and state statutes and regulations govern, among other things, medical device design and development, preclinical and clinical testing, premarket clearance or approval, registration and listing, manufacturing, labeling, storage, advertising and promotion, sales and distribution, export and import, and post-market surveillance. Unless an exemption applies, diagnostic tests require marketing clearance or approval from the FDA prior to commercial distribution. The two primary types of FDA marketing authorization applicable to a medical device are premarket notification, also called 510(k) clearance, and premarket approval, or PMA approval.
The PMA process, including the gathering of clinical and preclinical data and the submission to and review by the FDA, can take several years or longer. It involves a rigorous premarket review during which the applicant must prepare and provide the FDA with reasonable assurance of the device’s safety and effectiveness and information about the device and its components regarding, among other things, device design, manufacturing and labeling. PMA applications are subject to fees for medical device product review; for federal fiscal year 2018, the standard fee for review of a PMA is $310,764 and the small business fee is $77,691.
A 510(k) must demonstrate that the proposed device is substantially equivalent to another legally marketed device, or predicate device, that did not require premarket approval. In evaluating a 510(k), the FDA will determine whether the device has the same intended use as the predicate device, and (a) has the same technological characteristics as the predicate device, or (b) has different technological characteristics, and (i) the data supporting substantial equivalence contains information, including appropriate clinical or scientific data, if deemed necessary by the FDA, that demonstrates that the device is as safe and as effective as a legally marketed device, and (ii) does not raise different questions of safety and effectiveness than the predicate device. Most 510(k)s do not require clinical data for clearance, but the FDA may request such data. The FDA seeks to review and act on a 510(k) within 90 days of submission, but it may take longer if the agency finds that it requires more information to review the 510(k). If the FDA concludes that a new device is not substantially equivalent to a predicate device, the new device will be classified in Class III and the manufacturer will be required to submit a PMA to market the product.
50
Government Regulation Outside of the United States
In addition to regulations in the United States, we will be subject to a variety of regulations in other jurisdictions governing, among other things, clinical trials and any commercial sales and distribution of our products. Because biologically sourced raw materials are subject to unique contamination risks, their use may be restricted in some countries.
Whether or not we obtain FDA approval for a product, we must obtain the requisite approvals from regulatory authorities in foreign countries prior to the commencement of clinical trials or marketing of the product in those countries. Certain countries outside of the United States have a similar process that requires the submission of a clinical trial application much like the IND prior to the commencement of human clinical trials, e.g., a clinical trial application for each clinical trial for each EU country in which the trial is conducted; a clinical trial notification is required in Japan.
If we fail to comply with applicable foreign regulatory requirements, we may be subject to, among other things, fines, suspension or withdrawal of regulatory approvals, product recalls, seizure of products, operating restrictions and criminal prosecution.
Coverage, Pricing and Reimbursement for Biopharmaceutical Products
Sales of our products, when and if approved for marketing, will depend, in part, on the extent to which our products will be covered by third-party payors, such as federal, state, and foreign government health care programs, commercial insurance and managed healthcare organizations. These third-party payors are increasingly reducing reimbursements for medical products, drugs and services. In addition, the U.S. government, state legislatures and foreign governments have continued implementing cost containment programs, including price controls, restrictions on coverage and reimbursement and requirements for substitution of generic products. Adoption of price controls and cost containment measures, and adoption of more restrictive policies in jurisdictions with existing controls and measures, could further limit our net revenue and results. Decreases in third-party reimbursement for our product candidates or a decision by a third-party payor not to cover our product candidates could reduce physician usage of our products once approved and have a material adverse effect on our sales, results of operations and financial condition.
Incorporation and Public Offerings
We were incorporated under the laws of Delaware in June 2013. On November 16, 2015, we closed our Initial Public Offering, or IPO, whereby we sold 5,750,000 shares of common stock at a public offering price of $14.00 per share, including 750,000 shares of common stock issued upon the full exercise by the underwriters of their option to purchase additional shares, resulting in net proceeds to us of $72.9 million after deducting underwriting discounts, commissions, and offering expenses payable by us. On November 7, 2017, we sold 5,175,000 shares of common stock to the public at an offering price of $12.00 per share, including 675,000 shares of common stock issued upon the full exercise by the underwriters of their option to purchase additional shares, resulting in net proceeds to us of $58.0 million after deducting underwriting discounts, commissions, and offering expenses payable by us.
Employees
As of December 31, 2017, we employed 88 full-time employees in the United States, including 63 in research and development and 25 in general and administrative, and one part-time employee. Thirty-three of our employees have either an M.D. or a Ph.D. We have never had a work stoppage, and none of our employees is represented by a labor organization or under any collective-bargaining arrangements. We consider our employee relations to be positive.
Facilities
We lease our office and laboratory space, which consist of approximately 45,000 square feet located in two locations in Cambridge, Massachusetts. Our lease expires in 2024. In February 2018, we signed an amendment to an
51
existing lease for approximately 11,000 square feet of additional laboratory and office space in Cambridge, Massachusetts, to support our continued growth. The additional space will be ready for occupancy in the first half of 2018.
Legal Proceedings
As of the date of this Annual Report on Form 10-K, we were not party to any legal matters or claims. In the future, we may become party to legal matters and claims arising in the ordinary course of business, the resolution of which we do not anticipate would have a material adverse impact on our financial position, results of operations or cash flows.
Available Information
Our Internet address is http://www.voyagertherapeutics.com. We make available, free of charge, on or through our website our annual reports on Form 10-K, quarterly reports on Form 10-Q, current reports on Form 8-K, proxy statements and any amendments to those reports filed or furnished pursuant to Section 13(a) or 15(d) of the Securities and Exchange Act as soon as reasonably practicable after such material is electronically filed with or furnished to the Securities and Exchange Commission. The information on our website is not part of this Annual Report for the year ended December 31, 2017.
An investment in shares of our common stock involves a high degree of risk. You should carefully consider the following information about these risks, together with the other information appearing elsewhere in this Annual Report on Form 10-K, including our financial statements and related notes hereto, before deciding to invest in our common stock. The occurrence of any of the following risks could have a material adverse effect on our business, financial condition, results of operations and future growth prospects. In these circumstances, the market price of our common stock could decline, and you may lose all or part of your investment.
Risks Related to Our Financial Position and Need for Capital
We have incurred significant losses since inception and anticipate that we will continue to incur losses for the foreseeable future and may never achieve or maintain profitability.
We are a clinical‑stage gene therapy company with a limited operating history, and have not yet generated revenues from the sales of our product candidates. Investment in biotechnology companies is highly speculative because it entails substantial upfront capital expenditures and significant risk that the product candidate will fail to obtain regulatory approval or become commercially viable. We have not yet demonstrated the ability to complete any clinical trials of our product candidates, obtain marketing approvals, manufacture a commercial‑scale product or conduct sales and marketing activities necessary for successful commercialization. We continue to incur significant expenses related to research and development, and other operations in order to commercialize our product candidates. As a result, we are not and have never been profitable and have incurred losses since our inception. Our net losses were $70.7 million, $40.2 million, and $29.7 million for the years ended December 31, 2017, 2016, and 2015 respectively. As of December 31, 2017, we had an accumulated deficit of $160.7 million.
We historically have financed our operations primarily through private placements of our redeemable convertible preferred stock, public offerings of our common stock, and our collaboration agreement with Sanofi Genzyme. On November 16, 2015 we closed our initial public offering, or IPO, whereby we sold 5,750,000 shares of common stock at a public offering price of $14.00 per share, including 750,000 shares of common stock issued upon the full exercise by the underwriters of their option to purchase additional shares, resulting in net proceeds to us of $72.9 million after deducting underwriting discounts and commissions and offering expenses payable by us. On November 7, 2017, we sold 5,175,000 shares of common stock to the public at an offering price of $12.00 per share, including 675,000 shares of common stock issued upon the full exercise by the underwriters of their option to purchase additional
52
shares, resulting in net proceeds to us of $58.0 million after deducting underwriting discounts, commissions, and offering expenses payable by us. To date, we have devoted substantially all of our financial resources to building our product engine, selecting product programs, conducting research and development, including preclinical development of our product candidates, building our intellectual property portfolio, building our team, and establishing our collaborations with Sanofi Genzyme and AbbVie Biotechnology Ltd, or AbbVie. We expect that it could be several years, if ever, before we have a commercialized product candidate. We expect to continue to incur significant expenses and increasing operating losses for the foreseeable future. The net losses we incur may fluctuate significantly from quarter to quarter. We anticipate that our expenses will increase substantially if, and as, we:
|
· |
continue investing in our product engine to optimize vector engineering, manufacturing and dosing and delivery techniques; |
|
· |
continue to advance our clinical candidate, VY-AADC, through the current Phase 1b clinical trial and into a planned pivotal Phase 2-3 clinical program as a treatment for advanced Parkinson’s disease; |
|
· |
initiate additional preclinical studies and clinical trials for, and continue research and development of, our other programs; |
|
· |
conduct joint research and development under our strategic collaboration with AbbVie for the research, development, and commercialization of adeno-associated virus, or AAV, and other virus-based gene therapy products for the treatment of diseases of the central nervous system and other neurodegenerative diseases related to defective or excess aggregation of tau protein in the human brain, including Alzheimer’s disease; |
|
· |
continue our process research and development activities, as well as establish our research-grade and commercial manufacturing capabilities; |
|
· |
identify additional neurological diseases for treatment with our AAV gene therapies and develop additional programs or product candidates; |
|
· |
work to identify and optimize novel AAV capsids; |
|
· |
develop and obtain regulatory clearance for devices to deliver our AAV gene therapies; |
|
· |
seek marketing and regulatory approvals for VY-AADC or other product candidates or devices that arise from our programs that successfully complete clinical development; |
|
· |
maintain, expand and protect our intellectual property portfolio; |
|
· |
identify, acquire or in-license other product candidates and technologies; |
|
· |
develop a sales, marketing and distribution infrastructure to commercialize any product candidates for which we may obtain marketing approval; |
|
· |
expand our operational, financial and management systems and personnel, including personnel to support our clinical development, manufacturing and commercialization efforts and our operations as a public company; |
|
· |
increase our product liability and clinical trial insurance coverage as we expand our clinical trials and commercialization efforts; and |
53
|
· |
continue to operate as a public company. |
Because of the numerous risks and uncertainties associated with pharmaceutical product development, we are unable to accurately predict the timing or amount of increased expenses or when, or if, we will be able to achieve profitability. Our expenses will increase if:
|
· |
we are required by the U.S. Food and Drug Administration, or FDA, or the European Medicines Agency, or EMA, or other regulatory agencies to perform trials or studies in addition to those currently expected; |
|
· |
there are any delays in receipt of regulatory clearance to begin our planned clinical programs; or |
|
· |
there are any delays in enrollment of patients in or completing our clinical trials or the development of our product candidates. |
To become and remain profitable, we must develop and eventually commercialize product candidates with significant market potential, which will require us to be successful in a range of challenging activities. These activities can include completing preclinical studies and clinical trials of our product candidates; obtaining marketing approval for these product candidates; manufacturing at clinical and commercial scale; marketing and selling those products that are approved; satisfying any post-marketing requirements and achieving an adequate level of market acceptance of and obtaining and maintaining adequate coverage and reimbursement from third-party payors for such products; and protecting our rights to our intellectual property portfolio. We may never succeed in any or all of these activities and, even if we do, we may never generate revenues that are significant or large enough to achieve profitability. If we do achieve profitability, we may not be able to sustain or increase profitability on a quarterly or annual basis. Our failure to become and remain profitable would decrease the value of our company and could impair our ability to raise capital, maintain our research and development efforts, expand our business or continue our operations. A decline in the value of our company also could cause our stockholders to lose all or part of their investment.
We may not be able to generate sufficient revenue from the commercialization of our product candidates and may never be profitable.
Our ability to generate revenue and achieve profitability depends on our ability, alone or with our collaborative partners, to successfully complete the development of, and obtain the regulatory approvals necessary to commercialize, our current and future product candidates. Our lead product candidate VY‑AADC is being evaluated in a Phase 1b clinical trial and advancing into a pivotal Phase 2-3 clinical trial in 2018, and we do not anticipate generating revenues from product sales for the next several years, and we may never succeed in doing so. Our ability to generate future revenues from product sales depends heavily on our and our collaborators’ success in:
|
· |
completing preclinical and clinical development of our product candidates and identifying new product candidates; |
|
· |
seeking and obtaining regulatory and marketing approvals for product candidates for which we complete clinical trials; |
|
· |
launching and commercializing product candidates for which we obtain regulatory and marketing approval by establishing a sales force, marketing and distribution infrastructure or, alternatively, collaborating with a commercialization partner; |
|
· |
obtaining and maintaining adequate coverage and reimbursement by government and third‑party payors for our product candidates if and when approved; |
|
· |
maintaining and enhancing a sustainable, scalable, reproducible and transferable manufacturing process for our vectors and product candidates; |
54
|
· |
establishing and maintaining supply and manufacturing relationships with third parties that can provide adequate, in both amount and quality, products and services to support clinical development and the market demand for our product candidates, if and when approved; |
|
· |
obtaining an adequate level of market acceptance of our product candidates as a viable treatment option; |
|
· |
addressing any competing technological and market developments; |
|
· |
implementing additional internal systems and infrastructure, as needed; |
|
· |
negotiating favorable terms in any collaboration, licensing or other arrangements into which we may enter and performing our obligations in such collaborations; |
|
· |
maintaining, protecting and expanding our portfolio of intellectual property rights, including patents, trade secrets and know‑how; |
|
· |
avoiding and defending against third‑party interference or infringement claims; and |
|
· |
attracting, hiring and retaining qualified personnel. |
Even if one or more of the product candidates that we develop is approved for commercial sale, we anticipate incurring significant costs associated with commercializing any approved product candidate. Our expenses could increase beyond expectations if we are required by the FDA, EMA, or other regulatory authorities to perform preclinical studies and clinical trials in addition to those that we currently anticipate. Even if we are able to generate revenues from the sale of any approved products, we may not become profitable and may need to obtain additional funding to continue operations.
We will need to raise additional funding, which may not be available on acceptable terms, or at all. Failure to obtain this necessary capital when needed may force us to delay, limit or terminate certain of our product development efforts or other operations.
We expect our expenses to increase in connection with our ongoing and planned activities, particularly as we continue the research and development of, continue or initiate clinical trials of, and seek marketing approval for, our product candidates. In addition, if we obtain marketing approval for any of our product candidates, we expect to incur significant expenses related to product sales, medical affairs, marketing, manufacturing and distribution. Since the completion of our IPO on November 16, 2015, we have also incurred costs associated with operating as a public company. Accordingly, we will need to obtain substantial additional funding in connection with our continuing operations. If we are unable to raise capital or enter into business development transactions when needed or on acceptable terms, we could be forced to delay, reduce or eliminate certain of our research and development programs or any future commercialization efforts.
Our operations have consumed significant amounts of cash since inception. As of December 31, 2017, our cash, cash equivalents, and marketable debt securities were $169.1 million. Subsequent to December 31, 2017, we received $69.0 million in cash due to the execution of our collaboration agreement with AbbVie. Based upon our current operating plan, we expect that our existing cash, cash equivalents, and marketable debt securities, will enable us to fund our operating expenses and capital expenditure requirements into 2020.
Our future capital requirements will depend on many factors, including:
|
· |
the scope, progress, results, and costs of product discovery, preclinical studies and clinical trials for our product candidates; |
55
|
· |
the scope, progress, results, costs, prioritization, and number of our research and development programs; |
|
· |
the progress and status of our collaborations with Sanofi Genzyme and AbbVie, including any research and development costs for which we are responsible, the potential exercise by our collaboration partners of options to develop or license certain compounds, and our potential receipt of future milestone payments and royalties from our collaboration partners; |
|
· |
the extent to which we are obligated to reimburse, or entitled to reimbursement of, preclinical development and clinical trial costs, or the achievement of milestones or occurrence of other developments that trigger payments, under any other collaboration agreement to which we might become a party; |
|
· |
the costs, timing and outcome of regulatory review of our product candidates; |
|
· |
our ability to establish and maintain collaboration, distribution, or other marketing arrangements for our product candidates on favorable terms, if at all; |
|
· |
the costs and timing of preparing, filing and prosecuting patent applications, maintaining and enforcing our intellectual property rights and defending intellectual property‑related claims; |
|
· |
the extent to which we acquire or in‑license other product candidates and technologies or acquire or invest in other businesses, such as our investment in MRI Interventions, Inc.; |
|
· |
the costs related to evaluating possible alternative devices that may be useful in the delivery of our product candidates, including our ongoing development of our V-TAG device; |
|
· |
the costs of securing manufacturing arrangements for commercial production; |
|
· |
the level of product sales from any product candidates for which we obtain marketing approval in the future; and |
|
· |
the costs of establishing or contracting for sales, manufacturing, marketing, distribution, and other commercialization capabilities if we obtain regulatory approvals to market our product candidates. |
Identifying potential product candidates and conducting preclinical studies and clinical trials is a time-consuming, expensive, and uncertain process that takes years to complete. We may never generate the necessary data or results required to obtain marketing approval and achieve product sales. In addition, our product candidates, if approved, may not achieve commercial success. Our product revenues, if any, and any commercial milestones or royalty payments under our collaboration agreements, will be derived from sales of products that may not be commercially available for many years, if at all. Accordingly, we will need to continue to rely on additional financing and business development to achieve our business objectives. Adequate additional financing or business development transactions may not be available to us on acceptable terms, or at all. In addition, we may seek additional capital due to favorable market conditions or strategic considerations, even if we believe we have sufficient funds for our current or future operating plans.
Raising additional capital may cause dilution to our stockholders, restrict our operations or require us to relinquish rights to our technologies or product candidates.
Until such time, if ever, as we can generate product revenues sufficient to achieve profitability, we expect to finance our cash needs through a combination of equity offerings, debt financings, collaborations, strategic alliances, and licensing arrangements. We do not have any committed external source of funds other than the amounts we are entitled to receive from our collaboration partners for potential option exercises, the achievement of specified regulatory and commercial milestones, and royalty payments under our collaboration agreements. To the extent that we raise additional
56
capital through the sale of equity or equity-linked securities, including convertible debt, our stockholders’ ownership interests will be diluted, and the terms of these securities may include liquidation or other preferences that adversely affect our existing stockholders’ rights as holders of our common stock. Debt financing and preferred equity financing, if available, may involve agreements that include covenants limiting or restricting our ability to take specific actions, such as incurring additional debt, obtaining additional capital, acquiring or divesting businesses, making capital expenditures or declaring dividends. Our issuance of additional securities, whether equity or debt, or the possibility of such issuance, may cause the market price of our common stock to decline. Further, our existing stockholders may not agree with the terms of such financings.
If we raise additional funds through collaborations, strategic alliances, or licensing arrangements with third parties, we may have to relinquish valuable rights to our technologies, future revenue streams, research programs or product candidates or to grant licenses on terms that may not be favorable to us. If we are unable to raise additional funds through equity or debt financings when needed, we may be required to delay, limit, reduce or terminate our product development or future commercialization efforts or grant rights to develop and market products or product candidates that we would otherwise prefer to develop and market ourselves.
Our limited operating history may make it difficult for our stockholders to evaluate the success of our business to date and to assess our future viability.
We are an early-stage company. Our operations to date have been limited to building our team, business planning, raising capital, establishing our intellectual property portfolio, determining which neurological indications to pursue, advancing our product including delivery and manufacturing and conducting preclinical studies and clinical trials. Consequently, any predictions about our future success or viability may not be as accurate as they could be if we had a longer operating history.
In addition, as a new business, we may encounter unforeseen expenses, difficulties, complications, delays and other known and unknown factors. To achieve our current goals, we will need to transition in the future from a company with a research and development focus to a company capable of supporting commercial activities. We may not be successful in such a transition.
We expect our financial condition and operating results to continue to fluctuate significantly from quarter-to-quarter and year-to-year due to a variety of factors, many of which are beyond our control. Accordingly, our stockholders should not rely upon the results of any quarterly or annual periods as indications of future operating performance.
Risks Related to the Development and Regulatory Approval of Our Product Candidates
Our AAV gene therapy product candidates are based on a relatively novel technology, which makes it difficult to predict the time and cost of development and of subsequently obtaining regulatory approval, if at all. Only three gene therapy products have been approved in the United States and only two such products have been approved in the European Union.
We have concentrated our research and development efforts to date on our product engine, identifying our initial targeted disease indications, and our initial product candidates. Our future success depends on our successful development of viable AAV gene therapy product candidates. Currently, only one of our product candidates, VY-AADC, is in clinical development, and the remainder of our product candidates are in preclinical development. We cannot accurately predict when or if any of our product candidates will prove effective or safe in humans or whether these product candidates will receive marketing approval. There can be no assurance that we will not experience problems or delays in developing our product candidates and that such problems or delays will not cause unanticipated costs, or that any such development problems can be solved. We also may experience unanticipated problems or delays in expanding our manufacturing capacity.
The clinical trial requirements of the FDA, the EMA and other regulatory authorities and the criteria these regulators use to determine the safety and efficacy of a product candidate vary substantially according to the type,
57
complexity, novelty and intended use and market of the product candidate. The regulatory approval process for novel product candidates such as gene therapies can be more expensive and take longer than for other, better known or more extensively studied product candidates. Until August 2017, the FDA had never approved a gene therapy product. Since that time, it has approved Kymriah by Novartis International AG, for pediatric and young adult patients with a form of acute lymphoblastic leukemia, Yescarta by Kite Pharma, Inc., for adult patients with certain forms of non-Hodgkin lymphoma, and Luxturna by Spark Therapeutics, Inc., or Spark, for patients with an inherited form of vision loss. Similarly, only two gene therapy products, Glybera by uniQure N.V., or uniQure, which has since been withdrawn from the market by uniQure, and Strimvelis by GlaxoSmithKline PLC, have received marketing authorization from the European Commission.
It is difficult to determine how long it will take or how much it will cost to obtain regulatory approvals for our product candidates in either the United States or the European Union or how long it will take to commercialize our product candidates. The few regulatory approvals to date may not be indicative of what the FDA, European Commission, or other regulatory authorities may require for approval or of whether different or additional preclinical studies or clinical trials may be required to support regulatory approval in a particular jurisdiction. Delay or failure to obtain, or unexpected costs in obtaining, the regulatory approval necessary to bring a potential product candidate to market could decrease our ability to generate sufficient product revenue, and our business, financial condition, results of operations and prospects may be harmed.
Regulatory requirements governing gene and cell therapy products have changed frequently and may continue to change in the future. Such requirements may lengthen the regulatory requirements review process, require us to perform additional studies, and increase our development costs or may force us to delay, limit, or terminate certain of our programs.
The FDA has established the Office of Cellular, Tissue and Gene Therapies (now named the Office of Tissues and Advances Therapies, or OTAT) within CBER, to consolidate the review of gene therapy and related products, and has established the Cellular, Tissue and Gene Therapies Advisory Committee to advise CBER in its review. Gene therapy clinical trials conducted at institutions that receive funding for recombinant DNA research from the National Institute of Health, or NIH, are also potentially subject to review by the RAC. The ongoing Phase 1b clinical trial of VY-AADC and the separate Phase 1 trial exploring the delivery of VY-AADC using a posterior trajectory are being conducted at the University of California San Francisco, or UCSF, and University of Pittsburgh Medical Center, or UPMC, and two other sites and therefore are subject to oversight by these authorities. Even though the FDA decides whether individual gene therapy protocols may proceed, the NIH Office of Biotechnology Activities’ Recombinant DNA Advisory Committee, or the RAC, public review process, if undertaken, can delay the initiation of a clinical trial, even if the FDA has reviewed the trial design and details and permitted its initiation. Conversely, the FDA may place an Investigational New Drug application, or IND, on a clinical hold even if the RAC has provided a favorable review or an exemption from in depth, public review. In addition, NIH-funded institutions need to have their institutional biosafety committee, or IBC, as well as their institutional review board, or IRB, review proposed clinical trials to assess the safety of the trial. The ongoing Phase 1b clinical trial of VY-AADC has been reviewed by the IRBs of our four locations including UCSF and UPMC, and such trials will need to be re-reviewed by both institutional IRBs if the protocol for the trial is further amended. For any new protocol, the same processes and issues apply. In addition, adverse developments in clinical trials of gene therapy products conducted by us or others may cause the FDA or other oversight bodies to change the requirements for approval of any of our product candidates. Similarly, EMA and local health authorities of individual countries within the European Union may issue new guidelines concerning the clinical development and marketing authorization for gene therapy medicinal products and require that we comply with these new guidelines. The EMA and agencies at both the federal and state level in the United States have expressed an interest in further regulating new biotechnologies, including gene therapy. In addition, gene therapy products are considered genetically-modified organisms, or GMO, products and are regulated as such in each country. Designation of the type of GMO and subsequent handling and disposal requirements can vary across countries and is variable throughout the EU. Addressing each specific country requirement and obtaining approval to commence a clinical trial in these counties could result in delays in starting a clinical trial.
These regulatory review committees and advisory groups and the new guidelines they promulgate may lengthen the regulatory review process, require us to perform additional studies, increase our development costs, lead to changes
58
in regulatory positions and interpretations, delay or prevent approval and commercialization of these product candidates or lead to significant post‑approval limitations or restrictions. As we advance our product candidates, we will be required to consult with these regulatory and advisory groups, and comply with applicable guidelines. If we fail to do so, we may be required to delay or discontinue development of certain of our product candidates. These additional processes may result in a review and approval process that is longer than we otherwise would have expected. Delays as a result of increased or lengthier regulatory approval process and further restrictions on development of our product candidates can be costly and could negatively impact our or our collaborators’ ability to complete clinical trials and commercialize our current and future product candidates in a timely manner, if at all.
Results from preclinical studies and early‑stage clinical trials may not be indicative of efficacy in late‑stage clinical trials.
All of our product candidates are in early stages of development. Clinical testing is expensive, is difficult to design and implement, can take many years to complete and is uncertain as to outcome. A failure of one or more clinical trials can occur at any stage of testing. The outcome of preclinical testing and early clinical trials may not be predictive of the success of later stage clinical trials, interim results of a clinical trial do not necessarily predict final results and results from one completed clinical trial may not be replicated in a subsequent clinical trial with a similar study design. Some of our clinical trials, including our Phase 1 clinical trials and our Phase 1b clinical trial for VY-AADC, were conducted with small patient populations and were not blinded or placebo-controlled, making it difficult to predict whether the favorable results that we observed in such trials will be repeated in larger and more advanced clinical trials. Moreover, preclinical and clinical data are often susceptible to varying interpretations and analyses, and many companies that have believed their product candidates performed satisfactorily in preclinical studies and clinical trials have nonetheless failed to obtain marketing approval of their products.
A number of companies in the pharmaceutical and biotechnology industries have suffered significant setbacks in late‑stage clinical trials even after achieving promising results in early‑stage clinical trials. If a larger population of patients does not experience positive results, if these results are not reproducible, or if our products show diminishing activity over time, our products may not receive approval from the EMA or the FDA. Data obtained from preclinical and clinical activities are subject to varying interpretations, which may delay, limit or prevent regulatory approval. In addition, we may encounter regulatory delays or rejections as a result of many factors, including changes in regulatory policy during the period of product development. Failure to confirm favorable results from earlier trials by demonstrating the safety and effectiveness of our products in late‑stage clinical trials with larger patient populations could harm our business and we may never succeed in commercialization or generating product revenue.
The doses and coverage of the putamen being employed in the ongoing VY-AADC Phase 1b clinical trial are higher than those used in prior trials and may need to be further optimized or we may not generate sufficient clinical data in a placebo-controlled trial to achieve market authorization. Further, any favorable results which we obtain from our Phase 1b clinical trial might not be replicated in subsequent trials.
The clinical trial results of some of our collaborators have been negatively affected by factors that had not been fully anticipated prior to the examination of the trial results. For example, the magnitude of the clinical responses seen in the Phase 1 clinical trial of AAV2-AADC conducted by UCSF were similar to placebo effects observed in previous surgical therapies for Parkinson’s disease. As a result, we are unable to rely on the results of this Phase 1 trial for an indication of the efficacy of treatment with VY-AADC. We believe that there is a need to optimize the dose and volume of infusion of VY-AADC to substantially increase the coverage of the putamen, the region of the brain targeted by VY-AADC, to achieve a clinical benefit. However, we can provide no assurances that we will be able to optimize these parameters and thereby achieve sufficient coverage of the putamen to achieve a clinical benefit.
The ongoing Phase 1b clinical trial of VY-AADC incorporates several design features in an attempt to increase the area of the putamen, particularly the posterior putamen, which receives VY-AADC treatment. We are employing larger infusion volumes and higher doses of VY-AADC, and we are using the ClearPoint System to provide real time, intra operative MRI assistance to the physician surgically administering VY-AADC to the patient.
59
Based on the interim results from our Phase 1b clinical trial, we believe our Cohort 2 dose is likely to be the dose we will use in the planned Phase 2-3 clinical program. However, interim results of a clinical trial do not necessarily predict final results, and additional results from our Phase 1b clinical trial could change our proposed dose for our Phase 2-3 clinical program. Even if we do select the Cohort 2 dose, the results from Cohort 2 may not be replicated in our Phase 2-3 clinical program.
Additionally, we have initiated a separate Phase 1 clinical trial to explore a posterior, or back of the head, delivery approach of VY-AADC, compared with the transfrontal, or top of the head, delivery approach employed in our ongoing Phase 1b clinical trial. This trial utilized the same dose concentration as Cohort 3 of our Phase 1b clinical trial at a higher volume, yielding a higher total dose of VY-AADC than any of Cohort 1, 2 or 3 or than we currently believe we will select for our Phase 2-3 clinical program.
Due to the nature of the techniques being used in the Phase 1b clinical trial and the numerous variables that can be changed, it is possible that the data generated from this trial may not provide evidence of clinical benefit. For example, physicians may use cannulas, which are small tubes, of differing lengths in the infusion procedure, or may use differing infusion speeds or infusion angles. These differences could affect the dose of VY-AADC that ultimately reaches the putamen, leading to highly variable results. Similarly, we have limited experience to date with the posterior delivery approach we are testing in our Phase 1 clinical trial, and it may not generate sufficient data for us to determine whether a posterior approach would provide clinically superior outcomes to the transfrontal approach.
Furthermore, we plan to use a different manufacturing process for our vector in later stage Parkinson’s clinical trials. We manufacture VY-AADC using our baculovirus/Sf9 system for our later-stage clinical trials, as opposed to manufacturing in HEK 293 cells, which was used in our Phase 1 clinical trials. We have conducted studies to demonstrate comparability between the current version and the new version. It is possible, however, that the results of our pivotal Phase 2-3 clinical program in advanced Parkinson’s disease may differ from the results of our Phase 1b clinical trial.
We intend to conduct, and may in the future conduct, clinical trials for product candidates at sites outside the United States, and the FDA may not accept data from trials conducted in such locations.
To date, we have only conducted clinical trials in the United States. However, we may in the future choose to conduct, one or more of our clinical trials outside the United States. We generally plan to conduct our later stage and pivotal clinical trials of our product candidates globally.
Although the FDA may accept data from clinical trials conducted outside the United States, acceptance of these data is subject to conditions imposed by the FDA. For example, the clinical trial must be well designed and conducted and performed by qualified investigators in accordance with ethical principles. The trial population must also adequately represent the U.S. population, and the data must be applicable to the U.S. population and U.S. medical practice in ways that the FDA deems clinically meaningful. In addition, while these clinical trials are subject to the applicable local laws, FDA acceptance of the data will depend on its determination that the trials also complied with all applicable U.S. laws and regulations. If the FDA does not accept the data from any trial that we conduct outside the United States, it would likely result in the need for additional trials, which would be costly and time-consuming and would delay or permanently halt our development of the applicable product candidates.
60
Other risks inherent in conducting international clinical trials include:
|
· |
foreign regulatory requirements that could restrict or limit our ability to conduct our clinical trials; |
|
· |
administrative burden of complying with a variety of foreign laws, medical standards and regulatory requirements, including the regulation of pharmaceutical and biotechnology products and treatment; |
|
· |
failure of enrolled patients to adhere to clinical protocols or inadequate collection and assessment of clinical data as a result of differences in healthcare services or cultural customs; |
|
· |
foreign exchange fluctuations; |
|
· |
diminished protection of intellectual property in some countries; and |
|
· |
political and economic risks relevant to foreign countries. |
We may encounter substantial delays or difficulties in commencement, enrollment or completion of our clinical trials or we may fail to demonstrate safety and efficacy to the satisfaction of applicable regulatory authorities, which could prevent us from commercializing our current and future product candidates on a timely basis, if at all.
Before obtaining marketing approval from regulatory authorities for the sale of our current and future product candidates, we must conduct extensive clinical trials to demonstrate the safety and efficacy of the product candidates. Clinical trials are expensive, time‑consuming and their outcomes are uncertain.
We have very limited experience with clinical trials. The ongoing Phase 1b clinical trial of VY‑AADC and the separate Phase 1 trial exploring the delivery of VY-AADC using a posterior trajectory are being conducted at four locations including UCSF and UPMC. We cannot guarantee that any clinical trials will be conducted as planned or completed on schedule, if at all. A clinical trial failure can occur at any stage of testing.
Identifying and qualifying patients to participate in clinical trials of our product candidates is critical to our success. We may not be able to identify, recruit and enroll a sufficient number of patients, or those with required or desired characteristics, to complete our clinical trials in a timely manner or at all pursuant to the requirements of the FDA, EMA, or other regulatory authorities. Patient enrollment and trial completion are affected by many factors including:
|
· |
perceived risks and benefits of AAV gene therapy‑based approaches for the treatment of neurological diseases; |
|
· |
perceived risks of the delivery procedure, such as intracranial infusion for VY-AADC; |
|
· |
formulation changes to our product candidates may require us to conduct additional clinical studies to bridge our modified product candidates to earlier versions; |
|
· |
size of the patient population and process for identifying patients; |
|
· |
design of the trial protocol; |
|
· |
eligibility and exclusion criteria; |
|
· |
patients with preexisting antibodies to the vector that preclude their participation in the trial; |
61
|
· |
perceived risks and benefits of the product candidate under study; |
|
· |
availability of competing therapies and clinical trials; |
|
· |
severity of the disease under investigation; |
|
· |
availability of genetic testing for potential patients; |
|
· |
proximity and availability of clinical trial sites for prospective patients; |
|
· |
lack of adequate compensation of patients; |
|
· |
ability to obtain and maintain patient consent; |
|
· |
risk that enrolled patients will drop out before completion of the trial; |
|
· |
our inability to locate appropriately trained physicians to conduct such clinical trials, which may be particularly difficult for the VY‑AADC clinical trial, in which we are currently using the ClearPoint System, which is only available at a small number of academic medical centers in the United States; |
|
· |
willingness of patients to participate in a placebo-controlled trial; |
|
· |
patient referral practices of physicians; and |
|
· |
ability to monitor patients adequately during and after treatment. |
Further, we plan to seek marketing approvals in the United States, the European Union and other jurisdictions, which may require that we conduct clinical trials in foreign countries. Our ability to successfully initiate, enroll and complete a clinical trial in any foreign country is subject to numerous risks unique to conducting business in foreign countries, including:
|
· |
difficulty in establishing or managing relationships with clinical research organizations, or CROs, and physicians; |
|
· |
different standards for the conduct of clinical trials; |
|
· |
absence in some countries of established groups with sufficient regulatory expertise for review of AAV gene therapy protocols; |
|
· |
our inability to locate qualified local partners or collaborators for such clinical trials; and |
|
· |
the potential burden of complying with a variety of foreign laws, medical standards and regulatory requirements, including the regulation of pharmaceutical and biotechnology products and treatment. |
If we have difficulty enrolling a sufficient number of patients to conduct our clinical trials as planned, we may need to delay, limit or terminate ongoing or planned clinical trials, any of which would harm our business, financial condition, results of operations and prospects.
Other events that may prevent successful or timely completion of clinical development include:
|
· |
delays in reaching a consensus with regulatory authorities on trial design; |
62
|
· |
delays in initiating trials due to any additional review that is required by RAC; |
|
· |
delays in reaching agreement on acceptable terms with prospective CROs, and clinical trial sites; |
|
· |
delays in opening clinical trial sites or obtaining required IRB or independent ethics committee approval at each clinical trial site; |
|
· |
imposition of a clinical hold by regulatory authorities as a result of a serious adverse event or after an inspection of our clinical trial operations or trial sites; or our decision or the requirement of regulators or institutional review boards to suspend or terminate clinical research for various reasons, including noncompliance with regulatory requirements or a finding that the participants are being exposed to unacceptable health risks; |
|
· |
failure by us, any CROs we engage, or any other third parties to adhere to clinical trial requirements or regulatory requirements; |
|
· |
failure by us, the CROs we engage, or any other third parties to perform in accordance with the FDA’s good clinical practices, or GCP, or applicable regulatory guidelines in the European Union; |
|
· |
failure by physicians to adhere to delivery protocols leading to variable results; |
|
· |
delays in the testing, validation, manufacturing and delivery of our product candidates to the clinical sites, including delays by third parties with whom we have contracted to perform certain of those functions; |
|
· |
insufficient or inadequate supply or quality of our product candidates or other materials necessary to conduct clinical trials of our product candidates; |
|
· |
delays in having patients complete participation in a trial or return for post‑treatment follow‑up; |
|
· |
clinical trial sites or patients dropping out of a trial at a rate higher than we anticipate; |
|
· |
selection of clinical endpoints that require prolonged periods of clinical observation or analysis of the resulting data; |
|
· |
receipt of negative or inconclusive clinical trial results; |
|
· |
occurrence of serious adverse events associated with the product candidate that are viewed to outweigh its potential benefits; |
|
· |
occurrence of serious adverse events in trials of the same class of agents conducted by other sponsors; |
|
· |
changes in regulatory requirements and guidance that require amending or submitting new clinical protocols; or |
|
· |
the cost of clinical trials of our product candidates may be greater than we anticipate. |
Any inability to successfully complete preclinical studies and clinical trials could result in additional costs to us or impair our ability to generate revenues from product sales, regulatory and commercialization milestones and royalties. In addition, if we make manufacturing or formulation changes to our product candidates, we may need to conduct additional studies to bridge our modified product candidates to earlier versions. Clinical trial delays also could shorten any periods during which we may have the exclusive right to commercialize our product candidates or allow our
63
competitors to bring products to market before we do, which could impair our ability to successfully commercialize our product candidates and may harm our business, financial condition, results of operations and prospects.
Additionally, if the results of our clinical trials are inconclusive or if there are safety concerns or serious adverse events associated with our product candidates, we may:
|
· |
be delayed in obtaining marketing approval for our product candidates, if at all; |
|
· |
obtain approval for indications or patient populations that are not as broad as intended or desired; |
|
· |
obtain approval with labeling that includes significant use or distribution restrictions or safety warnings; |
|
· |
be subject to changes in the way the product is administered; |
|
· |
be required to perform additional clinical trials to support approval or be subject to additional post‑marketing testing requirements; |
|
· |
have regulatory authorities withdraw, or suspend, their approval of the product or impose restrictions on its distribution in the form of a Risk Evaluation and Mitigation Strategy, or REMS; |
|
· |
be subject to the addition of labeling statements, such as warnings or contraindications; |
|
· |
be sued; or |
|
· |
experience damage to our reputation. |
Our product candidates or the process for administering our product candidates may cause undesirable side effects or have other properties that could delay or prevent their regulatory approval, limit their commercial potential or result in significant negative consequences following any potential marketing approval.
In past clinical trials that were conducted by others with non‑AAV vectors, several significant side effects were caused by gene therapy treatments, including reported cases of leukemia and death. Other potential side effects could include an immunologic reaction and insertional oncogenesis, which is the process whereby the insertion of a functional gene near a gene that is important in cell growth or division results in uncontrolled cell division, which could potentially enhance the risk of malignant transformation. If our vectors demonstrate a similar adverse effect, or other adverse events, we may be required to halt or delay further clinical development of our product candidates. For example, in a recently published review of patients with hepatocellular carcinomas, it was shown that a small subset contained an integrated genome sequence of wild-type AAV2 and it was suggested that AAV2 may be associated with insertional oncogenesis.
In addition to side effects caused by the product candidate, the administration process or related procedures also can cause side effects. VY‑AADC and VY‑HTT01 will be administered directly to the targeted cells in the brain, requiring the patient to undergo brain surgery. In a previous Phase 1 clinical trial conducted by UCSF, three patients experienced hemorrhages caused by the surgical procedure for administering VY‑AADC. In the ongoing Phase 1b clinical trial of VY-AADC, we are using the ClearPoint System, which has only been used in limited gene therapy neurosurgeries to date to provide accurate placement of the cannula in the putamen, to allow for real‑time, intra‑operative MRI to assist the physician in visualizing the delivery of VY‑AADC to the putamen and to avoid specific blood vessels during the duration of the surgical procedure, with the goal of reducing the risk of hemorrhages. One patient in the ongoing Phase 1b trial at UCSF experienced two SAEs, a pulmonary embolism, or blood clot in the lungs, and related heart arrhythmia, or irregular heartbeat, which were determined to be related to the surgical procedure and prolonged immobility, not VY‑AADC. If other side effects were to occur in connection with the surgical procedure, our clinical trials could be suspended or terminated.
64
If in the future we are unable to demonstrate that such side effects were caused by the administration process or related procedures or are unable to modify the trial protocol adequately to address such side effects, the FDA, the European Commission, the EMA or other regulatory authorities could order us to cease further development of, or deny approval of, our product candidates for any or all targeted indications. For products that “knock down” or reduce the amount of an abnormal gene, their effects on other parts of the body, or “off target” effects, could result in unforeseen toxicity. Even if we are able to demonstrate that any future SAEs are not product‑related, and regulatory authorities do not order us to cease further development of our product candidates, such occurrences could affect patient recruitment or the ability of enrolled patients to complete the trial. Moreover, if we elect, or are required, to delay, suspend or terminate any clinical trial of any of our product candidates, the commercial prospects of such product candidates may be harmed and our ability to generate product revenues from any of these product candidates may be delayed or eliminated. Any of these occurrences may harm our ability to develop other product candidates, and may harm our business, financial condition and prospects significantly.
Additionally, if any of our product candidates receives marketing approval, the FDA could require us to adopt a REMS to ensure that the benefits outweigh its risks, which may include, among other things, a medication guide outlining the risks of the product for distribution to patients and a communication plan to health care practitioners. Furthermore, adverse events which were initially considered unrelated to the study treatment of the clinical trial may later be found to be caused by the study treatment. If we or others later identify undesirable side effects caused by our product candidate, several potentially significant negative consequences could result, including:
|
· |
regulatory authorities may suspend or withdraw approvals of such product candidate; |
|
· |
regulatory authorities may require additional warnings on the label; |
|
· |
we may be required to change the way a product candidate is administered or conduct additional clinical trials; |
|
· |
we could be sued and held liable for harm caused to patients; and |
|
· |
our reputation may suffer. |
Any of these events could prevent us from achieving or maintaining market acceptance of our product candidates and could significantly harm our business, prospects, financial condition and results of operations.
We may be unable to obtain orphan drug designation or exclusivity for any of our product candidates for which we seek such designation. If our competitors are able to obtain orphan drug exclusivity for products that constitute the same drug and treat the same indications as our product candidates, we may not be able to have competing products approved by the applicable regulatory authority for a significant period of time.
Regulatory authorities in some jurisdictions, including the United States and the European Union, may designate drugs for relatively small patient populations as orphan drugs. Under the Orphan Drug Act of 1983, the FDA may designate a product candidate as an orphan drug or biological product if it is intended to treat a rare disease or condition, which is generally defined as having a patient population of fewer than 200,000 individuals in the United States, or a patient population greater than 200,000 in the United States where there is no reasonable expectation that the cost of developing the drug or biological product will be recovered from sales in the United States. We have received feedback from the FDA that VY-AADC for the treatment of advanced Parkinson’s disease does not qualify for orphan disease designation because the potential for its use in earlier stages of Parkinson’s disease exceeds the 200,000 patient population criteria in the United States. In the European Union, EMA’s Committee for Orphan Medicinal Products grants orphan drug designation to promote the development of products that are intended for the diagnosis, prevention or treatment of a life‑threatening or chronically debilitating condition affecting not more than five in 10,000 persons in the European Union. Additionally, orphan designation is granted for products intended for the diagnosis, prevention or treatment of a life‑threatening, seriously debilitating or serious and chronic condition and when, without incentives, it is unlikely that sales of the drug in the European Union would be sufficient to justify the necessary investment in
65
developing the drug or biologic product. We have received feedback from the Committee for Orphan Medicinal Products that orphan designation likely would not be granted for VY-AADC in advanced Parkinson’s disease since they do not grant such status for more severe stages of a disease.
Generally, if a product candidate with an orphan drug designation receives the first marketing approval for the indication for which it has such designation, the product is entitled to a period of marketing exclusivity, which precludes the FDA or the European Commission from approving another marketing application for a product that constitutes the same drug treating the same indication for that marketing exclusivity period, except in limited circumstances. If another sponsor receives such approval before we do (regardless of our orphan drug designation), we may be precluded from receiving marketing approval for our product for the applicable exclusivity period. The applicable period is seven years in the United States and 10 years in the European Union. The exclusivity period in the United States can be extended by nine months if the BLA sponsor submits pediatric data that fairly respond to a written request from the FDA for such data. The exclusivity period in the European Union can be reduced to six years if a product no longer meets the criteria for orphan drug designation or if the product is sufficiently profitable so that market exclusivity is no longer justified. Orphan drug exclusivity may be revoked if any regulatory agency determines that the request for designation was materially defective or if the manufacturer is unable to assure sufficient quantity of the product to meet the needs of patients with the rare disease or condition.
We believe that all of our current programs may qualify for orphan drug designation except for VY-AADC for advanced Parkinson’s disease. Even if we obtain orphan drug exclusivity for a product candidate, that exclusivity may not effectively protect the product candidate from competition because different drugs or biological products can be approved for the same condition. In the United States, even after an orphan drug is approved, the FDA may subsequently approve another drug or biological product for the same condition if the FDA concludes that the latter drug or biological product is not the same drug or biological product or is clinically superior in that it is shown to be safer, more effective or makes a major contribution to patient care. In the European Union, marketing authorization may be granted to a similar medicinal product for the same orphan indication if:
|
· |
the second applicant can establish in its application that its medicinal product, although similar to the orphan medicinal product already authorized, is safer, more effective or otherwise clinically superior; |
|
· |
the holder of the marketing authorization for the original orphan medicinal product consents to a second orphan medicinal product application; or |
|
· |
the holder of the marketing authorization for the original orphan medicinal product cannot supply sufficient quantities of orphan medicinal product. |
Even if we seek orphan drug designation from the FDA, the European Commission or other regulatory agencies for a product candidate, there can be no assurances that the regulatory agency or agencies will grant such designation. Additionally, the designation of any of our product candidates as an orphan drug does not guarantee that any regulatory agency will ultimately approve that product candidate.
On August 3, 2017, the Congress passed the FDA Reauthorization Act of 2017, or FDARA. FDARA, among other things, codified the FDA’s pre-existing regulatory interpretation, to require that a drug sponsor demonstrate the clinical superiority of an orphan drug that is otherwise the same as a previously approved drug for the same rare disease in order to receive orphan drug exclusivity. The new legislation reverses prior precedent holding that the Orphan Drug Act unambiguously requires that the FDA recognize the orphan exclusivity period regardless of a showing of clinical superiority. The FDA may further reevaluate the Orphan Drug Act and its regulations and policies. We do not know if, when, or how the FDA may change the orphan drug regulations and policies in the future, and it is uncertain how any changes might affect our business. Depending on what changes the FDA may make to its orphan drug regulations and policies, our business could be adversely impacted.
66
A potential breakthrough therapy designation by the FDA for our product candidates may not lead to a faster development or regulatory review or approval process, and it does not increase the likelihood that our product candidates will receive marketing approval.
We may seek a breakthrough therapy designation for some of our product candidates. A breakthrough therapy is defined as a drug or biological product that is intended, alone or in combination with one or more other drugs, to treat a serious or life‑threatening disease or condition, and preliminary clinical evidence indicates that the drug or biological product may demonstrate substantial improvement over existing therapies on one or more clinically significant endpoints, such as substantial treatment effects observed early in clinical development. For drugs or biological products that have been designated as breakthrough therapies, interaction and communication between the FDA and the sponsor of the trial can help to identify the most efficient path for clinical development while minimizing the number of patients placed in ineffective control regimens. Drugs designated as breakthrough therapies by the FDA may also be eligible for accelerated approval.
Designation as a breakthrough therapy is within the discretion of the FDA. Accordingly, even if we believe one of our product candidates meets the criteria for designation as a breakthrough therapy, the FDA may disagree and instead determine not to make such designation. In any event, the receipt of a breakthrough therapy designation for a product candidate may not result in a faster development process, review or approval compared to drugs considered for approval under conventional FDA procedures and does not assure ultimate approval by the FDA. In addition, even if one or more of our product candidates qualify as breakthrough therapies, the FDA may later decide that the drugs or biological products no longer meet the conditions for qualification.
A potential regenerative medicine advanced therapy designation by the FDA for our product candidates may not lead to a faster development or regulatory review or approval process, and it does not increase the likelihood that our product candidates will receive marketing approval.
We may seek a regenerative medicine advanced therapy designation for some of our product candidates. A regenerative medicine advanced therapy is defined as cell therapies, therapeutic tissue engineering products, human cell and tissue products, and combination products using any such therapies or products. Gene therapies, including genetically modified cells, that lead to a durable modification of cells or tissues may meet the definition of a regenerative medicine therapy. The regenerative medicine advanced therapy program is intended to facilitate efficient development and expedite review of regenerative medicine advanced therapies, which are intended to treat, modify, reverse, or cure a serious or life-threatening disease or condition. A new drug application or a biologics license application, or BLA, for a regenerative medicine advanced therapy may be eligible for priority review or accelerated approval through (1) surrogate or intermediate endpoints reasonably likely to predict long-term clinical benefit or (2) reliance upon data obtained from a meaningful number of sites. Benefits of such designation also include early interactions with FDA to discuss any potential surrogate or intermediate endpoint to be used to support accelerated approval. A regenerative medicine therapy that is granted accelerated approval and is subject to post-approval requirements may fulfill such requirements through the submission of clinical evidence, clinical studies, patient registries, or other sources of real world evidence, such as electronic health records; the collection of larger confirmatory data sets; or post-approval monitoring of all patients treated with such therapy prior to its approval.
Designation as a regenerative medicine advanced therapy is within the discretion of the FDA. Accordingly, even if we believe one of our product candidates meets the criteria for designation as a regenerative medicine advanced therapy, the FDA may disagree and instead determine not to make such designation. In any event, the receipt of a regenerative medicine advanced therapy designation for a product candidate may not result in a faster development process, review or approval compared to drugs considered for approval under conventional FDA procedures and does not assure ultimate approval by the FDA. In addition, even if one or more of our product candidates qualify as regenerative medicine advanced therapies, the FDA may later decide that the biological products no longer meet the conditions for qualification.
67
Fast track designation by the FDA may not actually lead to a faster development or regulatory review or approval process and does not assure FDA approval of our product candidate.
If a drug is intended for the treatment of a serious or life-threatening condition and the drug demonstrates the potential to address unmet medical need for this condition, the drug sponsor may apply for FDA fast track designation. VY-AADC has been granted fast track designation by the FDA. We may seek such a designation for our other product candidates. A fast track designation does not ensure that the product candidate will receive marketing approval or that approval will be granted within any particular timeframe. Thus, fast track products may not experience a faster development process, review or approval compared to conventional FDA procedures. In addition, the FDA may withdraw fast track designation if it believes that the designation is no longer supported by data from our clinical development program. Fast track designation alone does not guarantee qualification for the FDA’s priority review procedures.
Priority review designation by the FDA may not lead to a faster regulatory review or approval process and, in any event, does not assure FDA approval of our product candidate.
If the FDA determines that a product candidate offers major advances in treatment or provides a treatment where no adequate therapy exists, the FDA may designate the product candidate for priority review. A priority review designation means that the FDA’s goal to review an application is six months, rather than the standard review period of ten months. We may request priority review for our product candidates. The FDA has broad discretion with respect to whether or not to grant priority review status to a product candidate, so even if we believe a particular product candidate is eligible for such designation or status, the FDA may decide not to grant it. Moreover, a priority review designation does not necessarily mean a faster regulatory review process or necessarily confer any advantage with respect to approval compared to conventional FDA procedures. Receiving priority review from the FDA does not guarantee approval within the six-month review cycle or thereafter.
Even if we complete the necessary preclinical studies and clinical trials, the marketing approval process is expensive, time-consuming and uncertain and may prevent us from obtaining approvals for the commercialization of some or all of our drug candidates. If we or any future collaborators are not able to obtain, or if there are delays in obtaining, required regulatory approvals, we or they will not be able to commercialize our drug candidates, and our ability to generate revenue will be materially impaired.
Our drug candidates and the activities associated with their development and commercialization, including their design, testing, manufacture, safety, efficacy, recordkeeping, labeling, storage, approval, advertising, promotion, sale and distribution, export and import, are subject to comprehensive regulation by the FDA and other regulatory agencies in the United States and by the EMA and comparable regulatory authorities in other countries. Failure to obtain marketing approval for a drug candidate will prevent us from commercializing the drug candidate. We have not received approval to market any of our drug candidates from regulatory authorities in any jurisdiction. We have only limited experience in filing and supporting the applications necessary to gain marketing approvals and expect to rely on third-party contract research organizations to assist us in this process.
Securing marketing approval requires the submission of extensive preclinical and clinical data and supporting information to the various regulatory authorities for each therapeutic indication to establish the drug candidate’s safety and efficacy. Securing regulatory approval also requires the submission of information about the product manufacturing process to, and inspection of manufacturing facilities by, the relevant regulatory authority. Our drug candidates may not be effective, may be only moderately effective or may prove to have undesirable or unintended side effects, toxicities or other characteristics that may preclude our obtaining marketing approval or prevent or limit commercial use.
The process of obtaining marketing approvals, both in the United States and abroad, is expensive (submission fee in the United States is more than $2.0 million and may be higher in the future), may take many years if additional clinical trials are required, if approval is obtained at all, and can vary substantially based upon a variety of factors, including the type, complexity and novelty of the drug candidates involved. Changes in marketing approval policies during the development period, changes in or the enactment of additional statutes or regulations, or changes in regulatory review for each submitted product application, may cause delays in the approval or rejection of an application. The FDA
68
and comparable authorities in other countries have substantial discretion in the approval process and may refuse to accept any application or may decide that our data are insufficient for approval and require additional preclinical, clinical or other studies. In addition, varying interpretations of the data obtained from preclinical and clinical testing could delay, limit or prevent marketing approval of a drug candidate. Any marketing approval we, or any future collaborators, ultimately obtain may be limited or subject to restrictions or post-approval commitments that render the approved product not commercially viable.
Accordingly, if we or any future collaborators experience delays in obtaining approval or if we or they fail to obtain approval of our drug candidates, the commercial prospects for our drug candidates may be harmed and our ability to generate revenues will be materially impaired.
Even if we obtain regulatory approval for a product candidate, our products will remain subject to regulatory oversight.
Even if we obtain any regulatory approval for our product candidates, they will be subject to ongoing regulatory requirements for manufacturing, labeling, packaging, storing, advertising, promoting, sampling, record‑keeping and submitting safety and other post‑market information. Any regulatory approvals that we receive for our product candidates also may be subject to a REMS, limitations on the approved indicated uses for which the product may be marketed or to the conditions of approval or contain requirements for potentially costly post‑marketing testing, including Phase 4 clinical trials, and surveillance to monitor the quality, safety and efficacy of the product. For example, the holder of an approved BLA, is obligated to monitor and report adverse events and any failure of a product to meet the specifications in the BLA. FDA guidance advises that patients treated with some types of gene therapy undergo follow‑up observations for potential adverse events for as long as 15 years. The holder of an approved BLA also must submit new or supplemental applications and obtain FDA approval for certain changes to the approved product, product labeling or manufacturing process. Advertising and promotional materials must comply with FDA rules and are subject to FDA review, in addition to other potentially applicable federal and state laws.
In addition, product manufacturers and their facilities are subject to payment of user fees and continual review and periodic inspections by the FDA and other regulatory authorities for compliance with cGMP, requirements and adherence to commitments made in the BLA or foreign marketing application. If we, or a regulatory authority, discover previously unknown problems with a product, such as adverse events of unanticipated severity or frequency, or problems with the facility where the product is manufactured or disagrees with the promotion, marketing or labeling of that product, a regulatory authority may impose restrictions relative to that product, the manufacturing facility or us, including requiring recall or withdrawal of the product from the market or suspension of manufacturing.
If we fail to comply with applicable regulatory requirements following approval of any of our product candidates, a regulatory authority may:
|
· |
issue a warning letter asserting that we are in violation of the law; |
|
· |
seek an injunction or impose administrative, civil or criminal penalties or monetary fines; |
|
· |
suspend or withdraw regulatory approval; |
|
· |
suspend any ongoing clinical trials; |
|
· |
refuse to approve a pending BLA or comparable foreign marketing application, or any supplements thereto, submitted by us or our strategic partners; |
|
· |
restrict the marketing or manufacturing of the product; |
|
· |
seize or detain the product or otherwise require the withdrawal of the product from the market; |
69
|
· |
refuse to permit the import or export of products; or |
|
· |
refuse to allow us to enter into supply contracts, including government contracts. |
Any government investigation of alleged violations of law could require us to expend significant time and resources in response and could generate negative publicity. The occurrence of any event or penalty described above may inhibit our ability to commercialize our product candidates and adversely affect our business, financial condition, results of operations and prospects.
In addition, FDA policies, and those of equivalent foreign regulatory agencies, may change and additional government regulations may be enacted that could prevent, limit or delay regulatory approval of our product candidates. We cannot predict the likelihood, nature or extent of government regulation that may arise from future legislation or administrative action, either in the United States or abroad. If we are slow or unable to adapt to changes in existing requirements or the adoption of new requirements or policies, or if we are not able to maintain regulatory compliance, we may lose any marketing approval that we may have obtained and we may not achieve or sustain profitability, which would harm our business, financial condition, results of operations and prospects.
We face significant competition in an environment of rapid technological change and the possibility that our competitors may achieve regulatory approval before us or develop therapies that are more advanced or effective than ours, which may harm our business and financial condition, and our ability to successfully market or commercialize our product candidates.
The biotechnology and pharmaceutical industries, including the gene therapy field, are characterized by rapidly changing technologies, intense and dynamic competition to develop new technologies and proprietary therapies, and a strong emphasis on intellectual property. We face substantial competition from many different sources, including large and specialty pharmaceutical and biotechnology companies, academic research institutions, government agencies and public and private research institutions.
We are aware of several companies focused on developing gene therapies in various indications, including bluebird bio, Inc., Abeona Therapeutics, Inc., Adverum Biotechnologies, Inc., Aevitas Therapeutics, Inc., Agilis Biotherapeutics, LLC, Applied Genetic Technologies Corporation, Asklepios BioPharmaceutical, Inc., Audentes Therapeutics, Inc., AveXis, Inc., GenSight Biologics SA, LogicBio Therapeutics, Inc., Lysogene SA, MeiraGTx Ltd., NightstaRx Ltd, Prevail Therapeutics, Inc., REGENXBio Inc., Solid Biosciences, Inc., uniQure NV, Pfizer, Inc., or Pfizer, and Spark, as well as several companies addressing other methods for modifying genes and regulating gene expression. Any advances in gene therapy technology made by a competitor may be used to develop therapies that could compete against any of our product candidates.
We expect that VY-AADC will compete with a variety of therapies currently marketed and in development for advanced Parkinson’s disease, including DBS marketed by Medtronic plc, Abbott Laboratories (acquired from St Jude Medical in 2017), and other medical device companies, DUOPA/Duodopa marketed by AbbVie Inc., as well as other novel, non-oral forms of levodopa in development, including NeuroDerm’s ND0612 (acquired by Mitsubishi Tanabe Pharma in 2017), Acorda Therapeutics’ inhaled levodopa, CVT-301, and Sunovion Pharmaceuticals’ sublingual apomorphine, APL-130277 (acquired from Cynapsus Therapeutics). Gene therapy competition for advanced Parkinson’s disease previously included AMT-090 or AAV-GDNF, but this was deprioritized by uniQure in 2016. Oxford Biomedica plc is planning for a Phase 1/2 trial in 2018 for OXB-102, a second generation LentiVector gene therapy.
We expect that our preclinical programs will compete with a variety of therapies in development, including:
•VY-SOD101 for a monogenic form of ALS will potentially compete with IONIS-SOD1Rx being developed by Ionis Pharmaceuticals, Inc., or Ionis, in collaboration with Biogen Inc., or Biogen, and a gene therapy being developed by AveXis;
70
•VY-FXN01 for Friedreich’s ataxia will potentially compete with AAV-FXN being developed by Adverum Biotechnologies, AAV-FXN being developed by Pfizer, and frataxin targeted gene therapy being developed by Agilis Biotherapeutics, LLC in collaboration with Intrexon Corporation, and BMN 290 being developed by BioMarin Pharmaceutical Inc.;
•VY-HTT01 for Huntington’s disease will potentially compete with IONIS-HTTRx being developed by Ionis in collaboration with F. Hoffmann-La Roche Ltd., or Roche, WVE-120101 and WVE-120102 being developed by WAVE Life Sciences in collaboration with Takeda Pharmaceuticals, a Zinc Finger Protein (ZFP) therapy being developed by Sangamo Therapeutics, Inc. in collaboration with Shire plc, and gene therapies being developed by uniQure and Spark;
•Our Tau program for tauopathies including Alzheimer’s disease, PSP, and FTD will potentially compete with tau antibodies being developed by Roche Genentech Inc. in collaboration with AC Immune SA, Eli Lilly & Co., AbbVie Inc., Biogen, and several other companies, as well as an antisense oligonucleotide program being developed by Ionis in collaboration with Biogen; and
•VY-NAV01 for severe, chronic pain will potentially compete with Nav1.7 inhibitors being developed by Pfizer, Teva Pharmaceuticals, Biogen, Roche Genentech Inc. in collaboration with Xenon Pharmaceuticals, Inc., Amgen, Inc., and Astellas Pharma Inc, and Nav1.8 inhibitors being developed by Vertex.
Many of our potential competitors, alone or with their strategic partners, have substantially greater financial, technical and other resources, such as larger research and development, clinical, marketing and manufacturing organizations. Mergers and acquisitions in the biotechnology and pharmaceutical industries may result in even more resources being concentrated among a smaller number of competitors. Smaller and other early stage companies may also prove to be significant competitors, particularly through collaborative agreements with large and established companies. Our commercial opportunity could be reduced or eliminated if competitors develop and commercialize products that are safer, more effective, have fewer or less severe side effects, are more convenient or are less expensive than any products that we may develop. Competitors also may obtain FDA or other regulatory approval for their products more rapidly or earlier than us, which could result in our competitors establishing a strong market position before we are able to enter the market. Additionally, technologies developed or acquired by our competitors may render our potential product candidates uneconomical or obsolete, and we may not be successful in marketing our product candidates against competitors. These third parties also compete with us in recruiting and retaining qualified scientific and management personnel, establishing clinical trial sites, and registering patients for clinical trials.
In addition, as a result of the expiration or successful challenge of our patent rights, we could face more litigation with respect to the validity and scope of patents relating to our competitors’ products. The availability of our competitors’ products could limit the demand, and the price we are able to charge, for any products that we may develop and commercialize. If we are not able to compete effectively against potential competitors, our business will not grow and our financial condition and operations will be harmed.
Even if we obtain and maintain approval for our product candidates from the FDA, we may never obtain approval for our product candidates outside of the United States, which would limit our market opportunities and adversely affect our business.
Approval of a product candidate in the United States by the FDA does not ensure approval of such product candidate by regulatory authorities in other countries or jurisdictions, and approval by one foreign regulatory authority does not ensure approval by regulatory authorities in other foreign countries or by the FDA. Sales of our product candidates outside of the United States will be subject to foreign regulatory requirements governing clinical trials and marketing approval. Even if the FDA grants marketing approval for a product candidate, comparable regulatory authorities of foreign countries also must approve the manufacturing and marketing of the product candidates in those countries. Approval procedures vary among jurisdictions and can involve requirements and administrative review periods different from, and more onerous than, those in the United States, including additional preclinical studies or clinical trials. In many countries outside the United States, a product candidate must be approved for reimbursement before it can be approved for sale in that country. In some cases, the price that we intend to charge for our products, if
71
approved, is also subject to approval. We intend to submit a marketing authorization application to EMA for approval of our product candidates in the European Union but obtaining such approval from the European Commission following the opinion of EMA is a lengthy and expensive process. Even if a product candidate is approved, the FDA or the European Commission may limit the indications for which the product may be marketed, require extensive warnings on the product labeling or require expensive and time‑consuming additional clinical trials or reporting as conditions of approval. Regulatory authorities in countries outside of the United States and the European Union also have requirements for approval of product candidates with which we must comply prior to marketing in those countries. Obtaining foreign regulatory approvals and compliance with foreign regulatory requirements could result in significant delays, difficulties and costs for us and could delay or prevent the introduction of our product candidates in certain countries.
Further, clinical trials conducted in one country may not be accepted by regulatory authorities in other countries. Also, regulatory approval for any of our product candidates may be withdrawn. If we fail to comply with the regulatory requirements, our target market will be reduced and our ability to realize the full market potential of our product candidates will be harmed and our business, financial condition, results of operations and prospects will be harmed.
Additionally, on June 23, 2016, the electorate in the United Kingdom voted in favor of leaving the European Union, commonly referred to as Brexit. On March 29, 2017, the country formally notified the European Union of its intention to withdraw pursuant to Article 50 of the Lisbon Treaty. Since a significant proportion of the regulatory framework in the United Kingdom is derived from European Union directives and regulations, the referendum could materially impact the regulatory regime with respect to the approval of our product candidates in the United Kingdom or the European Union. Any delay in obtaining, or an inability to obtain, any marketing approvals, as a result of Brexit or otherwise, would prevent us from commercializing our product candidates in the United Kingdom and/or the European Union and restrict our ability to generate revenue and achieve and sustain profitability. If any of these outcomes occur, we may be forced to restrict or delay efforts to seek regulatory approval in the United Kingdom and/or European Union for our product candidates, which could significantly and materially harm our business.
Risks Related to Third Parties
To date, all of our revenue has been derived from our collaborations with Sanofi Genzyme and AbbVie, and if either of these collaboration agreements were to be terminated, our business financial condition, results of operations and prospects would be harmed.
In February 2015, we entered into a collaboration agreement with Sanofi Genzyme to leverage our combined expertise and assets in gene therapy for neurological diseases. Under the agreement, we received an upfront commitment of approximately $100.0 million. Pursuant to the agreement, we granted Sanofi Genzyme an exclusive option to license, develop and commercialize (i) ex-U.S. rights to our advanced Parkinson’s disease, Friedreich’s ataxia and Huntington’s disease programs and a future program, or the Split Territory Programs, with an incremental option to co-commercialize the product candidate from our Huntington’s disease program in the United States and (ii) worldwide rights to our spinal muscular atrophy program. If Sanofi Genzyme exercises an option for a Split Territory Program, except for our advanced Parkinson’s disease program, it is required to make an option exercise payment to us. Furthermore, at the inception of the agreement, we were eligible to receive up to $745.0 million in the aggregate upon the achievement of specified regulatory and commercial milestones, including tiered royalty payments based on a percentage of net sales of product candidates from the programs for which Sanofi Genzyme exercised its option, or the Optioned Programs. Our research and development activities in connection with the collaboration might not be successful. We cannot accurately predict when or if any of our product candidates will prove effective or safe in humans or whether these product candidates will receive marketing approval. There can be no assurance that we will not experience problems or delays in developing our product candidates and that such problems or delays will not cause unanticipated costs, or that any such development problems can be solved. If Sanofi Genzyme were to elect not to exercise an option, we would have incurred significant development expenses but not receive the option exercise payment or be eligible to receive future milestone or royalty payments related to such program. For example, in October 2017, Sanofi Genzyme notified us that it had decided not to exercise its option for the ex-U.S. rights to VY-AADC and terminated the portion of its collaboration with us concerning Parkinson’s disease. As a result of Sanofi Genzyme’s decision, the Company is no longer entitled to receive up to $105.0 million of milestone payments related to the Parkinson’s program.
72
If Sanofi Genzyme exercised one or more options, following such exercise, Sanofi Genzyme will have sole responsibility for the development and commercialization of the product candidates from such program in the applicable territory. Sanofi Genzyme will have the sole discretion to determine and direct its efforts and resources, including the ability to discontinue all efforts and resources it applies to the development and, if approval is obtained, commercialization and marketing of the product candidates covered by the Optioned Programs in the applicable territories. Sanofi Genzyme may not be effective in obtaining approvals for the product candidates developed from the Optioned Programs or in marketing, or arranging for necessary supply, manufacturing or distribution relationships for, any approved products. Furthermore, Sanofi Genzyme may change its strategic focus or pursue alternative technologies in a manner that results in reduced, delayed or no revenue to us. Sanofi Genzyme has a variety of marketed products and product candidates under collaboration with other companies, including some of our competitors, and its own corporate objectives may not be consistent with our best interests. If Sanofi Genzyme fails to develop, obtain regulatory approval for or ultimately commercialize any product candidate from the Optioned Programs in the applicable territories, or if Sanofi Genzyme terminates our collaboration, our business, financial condition, results of operations and prospects would be harmed.
In addition, any dispute or litigation proceedings we may have with Sanofi Genzyme in the future could delay development programs, create uncertainty as to ownership of or access to intellectual property rights, distract management from other business activities and generate substantial expense. Finally, we also may not be able to seek and obtain a viable, alternative collaborator to partner with for the development and commercialization of the Split Territory Programs or the Optioned Programs.
In February 2018, we entered into an exclusive collaboration and option agreement with AbbVie for the research, development, and commercialization of AAV gene therapy products for the treatment of diseases of the central nervous system and other neurodegenerative diseases related to defective or excess aggregation of tau protein in the human brain, including Alzheimer’s disease. Under the terms of the agreement, we received an upfront payment of $69.0 million and may receive option exercise payments, future development and regulatory milestone payments and royalties.
Under the agreement, we are obligated to use diligent efforts to conduct research and development activities, including IND-enabling and Phase 1 clinical trial activities, for we are solely financially responsible. As described above, our research and development activities in connection with a collaboration might not be successful. Our collaboration and license agreement with AbbVie shall automatically terminate if AbbVie decides not to exercise one or more of its options prior to the expiration of the specified periods of the collaboration. If AbbVie did not exercise one or more of its options, we would have incurred significant research and development expenses but would not receive any future option exercise, milestone payments, or royalty payments under the collaboration.
Such research and development activities shall be pursuant to plans agreed to by the parties and overseen by a joint governance committee, or JGC. Initially, we will have final decision-making authority within the JGC, subject to specified limitations. If AbbVie exercises its license option, however, AbbVie will assume final decision-making authority within the JGC. If AbbVie exercises its license option, it will also be solely responsible for all development and commercialization activities relating to compounds and products licensed pursuant to the agreement, and, at AbbVie’s request, we could be required to effect a full transfer of the manufacturing process for such compound and products. Even if AbbVie does not exercise any of its options under the agreement, we have agreed to grant AbbVie perpetual, exclusive or non-exclusive (as the case may be), worldwide licenses to certain know-how and patent rights developed by us or jointly by us and AbbVie arising from the collaboration.
AbbVie might not be effective in administering the JGC, obtaining approvals for the product candidates arising from our collaboration, or commercializing or manufacturing the resulting products. Further, AbbVie’s objectives in connection with the collaboration may not be consistent with our best interests. AbbVie could use its leadership of the JGC or intellectual property it has licensed under the agreement in a manner adverse to us, or it could halt, slow, or deprioritize its development and commercialization efforts under the collaboration. In any such instances, our business, financial condition, results of operations and prospects could be materially harmed.
73
We have only used the ClearPoint System to deliver our product. While other devices for delivery may be used in the future, any issues with the ClearPoint System or the manufacturer of the ClearPoint System, may result in delays in the development and commercialization of certain of our product candidates, which could have an adverse impact on our business.
The surgical approach that we are using for VY-AADC is similar, in some respects, to the stereotactic approach used for deep brain stimulation, or DBS, a marketed device-based treatment for advanced Parkinson’s disease. One primary difference with our approach is the ability to assist the physician in visualizing the delivery of VY-AADC to the putamen using real-time, intra-operative, magnetic resonance imaging, or MRI, to avoid specific blood vessels to potentially reduce the risk of hemorrhages during the surgical procedure and to maximize the coverage of the putamen.
Investigators in the Phase 1b clinical trial of VY-AADC and the separate Phase 1 posterior trajectory trial use the real-time, intra-operative, MRI system called the ClearPoint System from MRI Interventions, Inc. However, not all neuro-surgical units within the United States utilize this system and may employ other neuro-navigational systems that are not compatible with real-time MRI imaging. We may continue to use the ClearPoint System in future clinical trials of VY-AADC and any other of our product candidates that are injected directly into the brain. Therefore, any issues with the ClearPoint System, such as a finding that use of the ClearPoint System causes adverse events or a product recall, or the manufacturer of the ClearPoint System, such as bankruptcy or a decision to stop production of the system due to lack of profitability, could delay the development or commercialization of certain of our product candidates as there currently is no other manufacturer of the ClearPoint System and we are not aware of any other medical device that would be deemed substantially equivalent to the ClearPoint System.
We are developing the Voyager Trajectory Array Guide, or V-TAG, as our own device for use as a real-time, intra-operative, MRI-compatible device that can be used with other neuro-navigational systems for this and other surgical procedures. We plan to file an application for 510(k) clearance with the FDA in the first half of 2018. We believe that our experience gained from the delivery in our VY-AADC program, including the use of V-TAG can be applied to AAV gene therapy delivery for our Huntington’s disease program and possibly other projects as well.
As of September 30, 2017, MRI Interventions, the manufacturer of the ClearPoint System, reported cash and cash equivalents of $11.0 million on its balance sheet, secured debt (senior and junior) totaling approximately $4.8 million, and a net loss for $5.1 million for the nine months ended September 30, 2017. In addition, in its past several Quarterly Reports on Form 10-Q, MRI Interventions has indicated that there is substantial doubt as to its ability to continue as a going concern, unless it raises the additional capital needed to run the business.
We may seek to enter into collaborations in the future with other third parties. If we are unable to enter into such collaborations, or if these collaborations are not successful, our business could be adversely affected.
We will seek to enter into additional collaborations in the future, including sales, marketing, distribution, development, licensing, and/or broader collaboration agreements. Our likely collaborators include large and mid-size pharmaceutical companies, regional and national pharmaceutical companies, biotechnology companies, and medical device manufacturers. However, we may not be able to enter into additional collaborations on favorable terms or at all. Our ability to generate revenues from our collaborations will depend on our and our collaborators’ abilities to successfully perform the functions assigned to each of us in these arrangements. In addition, our collaborators have the ability to abandon research or development projects and terminate applicable agreements. Moreover, an unsuccessful outcome in any clinical trial for which our collaborator is responsible could be harmful to the public perception and prospects of our gene therapy platform.
Our relationship with any future collaborations may pose several risks, including the following:
|
· |
collaborators have significant discretion in determining the amount and timing of the efforts and resources that they will apply to these collaborations; |
|
· |
collaborators may not perform their obligations as expected; |
74
|
· |
the preclinical studies and clinical trials conducted as part of these collaborations may not be successful; |
|
· |
collaborators may not pursue development and commercialization of any product candidates that achieve regulatory approval or may elect not to continue or renew development or commercialization programs based on preclinical study or clinical trial results, changes in the collaborators’ strategic focus or available funding or external factors, such as an acquisition, that divert resources or create competing priorities; |
|
· |
collaborators may delay preclinical studies and clinical trials, provide insufficient funding for preclinical studies and clinical trials, stop a preclinical study or clinical trial or abandon a product candidate, repeat or conduct new preclinical studies or clinical trials or require a new formulation of a product candidate for preclinical studies or clinical trials; |
|
· |
we may not have access to, or may be restricted from disclosing, certain information regarding product candidates being developed or commercialized under a collaboration and, consequently, may have limited ability to inform our stockholders about the status of such product candidates; |
|
· |
collaborators could independently develop, or develop with third parties, products that compete directly or indirectly with our product candidates if the collaborators believe that competitive products are more likely to be successfully developed or can be commercialized under terms that are more economically attractive than ours; |
|
· |
product candidates developed in collaboration with us may be viewed by our collaborators as competitive with their own product candidates or products, which may cause collaborators to cease to devote resources to the commercialization of our product candidates; |
|
· |
a collaborator with marketing and distribution rights to one or more of our product candidates that achieve regulatory approval may not commit sufficient resources to the marketing and distribution of any such product candidate; |
|
· |
disagreements with collaborators, including disagreements over proprietary rights, contract interpretation or the preferred course of development of any product candidates, may cause delays or termination of the research, development or commercialization of such product candidates, may lead to additional responsibilities for us with respect to such product candidates or may result in litigation or arbitration, any of which would be time‑consuming and expensive; |
|
· |
collaborators may not properly maintain or defend our intellectual property rights or may use our proprietary information in such a way as to invite litigation that could jeopardize or invalidate our intellectual property or proprietary information or expose us to potential litigation; |
|
· |
disputes may arise with respect to the ownership or inventorship of intellectual property developed pursuant to our collaborations; |
|
· |
collaborators may infringe the intellectual property rights of third parties, which may expose us to litigation and potential liability; |
|
· |
the terms of our collaboration agreement may restrict us from entering into certain relationships with other third parties, thereby limiting our options; and |
|
· |
collaborations may be terminated for the convenience of the collaborator and, if terminated, we could be required to raise additional capital to pursue further development or commercialization of the applicable product candidates. |
75
Collaboration agreements may not lead to the development or commercialization or product candidates in the most efficient manner, or at all. If our collaborations do not result in the successful development and commercialization of products, or if one of our collaborators terminates its agreement with us, we may not receive any future research funding or milestone or royalty payments under the collaboration. If we do not receive the funding we expect under these agreements, our development of our product candidates could be delayed, and we may need additional resources to develop our product candidates. Additionally, subject to its contractual obligations to us, if a collaborator of ours were to be involved in a business combination, it might deemphasize or terminate the development or commercialization of any product candidate licensed to it by us. If one of our collaborators terminates its agreement with us, we may find it more difficult to attract new collaborators, and the perception of us in the business and financial communities could be adversely affected. All of the risks relating to product development, regulatory approval and commercialization described in this Annual Report apply to the activities of our collaborators.
We will face significant competition in seeking appropriate collaborators, and the negotiation process is time-consuming and complex. Our ability to reach a definitive collaboration agreement with any future collaborators will depend, among other things, upon our assessment of the collaborator’s resources and expertise, the terms and conditions of the proposed collaboration and the proposed collaborator’s evaluation of several factors. Those factors may include the design or results of clinical trials, the likelihood of approval by the FDA or similar regulatory authorities outside the United States, the potential market for the subject product candidate, the costs and complexities of manufacturing and delivering such product candidate to patients, the potential of competing products, the existence of uncertainty with respect to our ownership of technology, which can exist if there is a challenge to such ownership without regard to the merits of the challenge, and industry and market conditions generally. The collaborator may also consider alternative product candidates or technologies for similar indications that may be available to collaborate on and whether such a collaboration could be more attractive than the one with us for our product candidate. We may also be restricted under future license agreements from entering into agreements on certain terms with potential collaborators. In addition, there have been a significant number of recent business combinations among large pharmaceutical companies that have resulted in a reduced number of potential future collaborators.
If we are unable to reach agreements with suitable collaborators on a timely basis, on acceptable terms, or at all, we may have to curtail the development of a product candidate, reduce or delay its development program or one or more of our other development programs, delay its potential commercialization or reduce the scope of any sales or marketing activities, or increase our expenditures and undertake development or commercialization activities at our own expense. If we elect to fund and undertake development or commercialization activities on our own, we may need to obtain additional expertise and additional capital, which may not be available to us on acceptable terms or at all. If we fail to enter into collaborations and do not have sufficient funds or expertise to undertake the necessary development and commercialization activities, we may not be able to further develop our product candidates or bring them to market or continue to develop our product engine. If we license rights to product candidates, we may not be able to realize the benefit of such transactions if we are unable to successfully integrate them with our existing operations and company culture.
We have relied, and we expect to continue to rely on third parties to conduct, supervise and monitor our clinical trials, and if these third parties perform in an unsatisfactory manner, our business could be harmed.
We expect to rely on CROs and clinical trial sites to ensure our clinical trials are conducted properly and on time. We may also engage third parties such as clinical data management organizations, medical institutions and clinical investigators to conduct or assist in our clinical trials or other clinical development work. While we will have agreements governing their activities, we will have limited influence over their actual performance. We will control only certain aspects of our third-party service providers’ activities. Nevertheless, we will be responsible for ensuring that each of our clinical studies is conducted in accordance with the applicable protocol, legal, regulatory and scientific standards. Our reliance on these third-parties does not relieve us of our regulatory responsibilities. For example, our ongoing Phase 1b clinical trial of VY-AADC and our separate Phase 1 trial exploring the delivery of VY-AADC using a posterior trajectory are being conducted by four locations, including UCSF and UPMC. If any locations terminated the clinical trial, we would be required to find another party to conduct any new trials. We may be unable to find a new party to conduct new trials of our product candidates or obtain clinical supply of our product candidates or AAV vectors for such trials.
76
We and our third-party service providers are required to comply with the FDA’s GCPs for conducting, recording and reporting the results of IND‑enabling studies and clinical studies to assure that the data and reported results are credible and accurate and that the rights, integrity and confidentiality of clinical trial participants are protected. We are also required to register ongoing clinical trials and post the results of completed clinical trials on a government-sponsored database, ClinicalTrials.gov, within specified timeframes. The FDA enforces these GCPs through periodic inspections of trial sponsors, principal investigators and clinical trial sites at which the FDA may determine that our clinical trials did not comply with GCPs. If we or our third-party service providers fail to comply with applicable GCPs, the clinical data generated in our future clinical trials may be deemed unreliable and the FDA may require us to perform additional clinical trials before approving any marketing applications. In addition, our future clinical trials will require a sufficient number of patients to evaluate the safety and effectiveness of our product candidates. Accordingly, if we or our third-party service providers fail to comply with these regulations or fail to recruit a sufficient number of patients, we may be required to repeat such clinical trials, which would delay the regulatory approval process. Failure to comply can also result in fines, adverse publicity, and civil and criminal sanctions.
Our third-party service providers are not our employees, and we are therefore unable to directly monitor whether or not they devote sufficient time and resources to our clinical and nonclinical programs. These third-party service providers may also have relationships with other commercial entities, including our competitors, for whom they may also be conducting clinical trials or other drug development activities that could harm our competitive position. If our third-party service providers do not successfully carry out their contractual duties or obligations, fail to meet expected deadlines, or if the quality or accuracy of the clinical data they obtain is compromised due to the failure to adhere to our clinical protocols or regulatory requirements, or for any other reasons, our clinical trials may be extended, delayed or terminated, and we may not be able to obtain regulatory approval for, or successfully commercialize our product candidates. As a result, our financial results and the commercial prospects for our product candidates would be harmed, our costs could increase, and our ability to generate revenues could be delayed.
Risks Related to Manufacturing
Gene therapies are novel, complex and difficult to manufacture. We could experience manufacturing problems that result in delays in the development or commercialization of our product candidates or otherwise harm our business.
The manufacture of gene therapy products is technically complex, and necessitates substantial expertise and capital investment. Production difficulties caused by unforeseen events may delay the availability of material for our clinical studies. To meet the requirements of our current and planned future trials we have developed a proprietary manufacturing platform that provides a robust and scalable process for AAV production. We are using the baculovirus/Sf9 AAV production system, a technology for producing AAV vectors at scale in insect-derived cells. The process has been successfully transferred to our contract manufacturing organizations where it is used in manufacturing clinical materials in accordance with the FDA’s current good manufacturing practices (cGMPs). We have also built an onsite, state-of-the-art process research and development facility to enable the manufacturing of high quality AAV gene therapy vectors at laboratory scale.
We presently contract with third parties for the manufacturing of our program materials. We currently have no plans to build our own clinical or commercial scale manufacturing capabilities. The use of contracted manufacturing and reliance on collaboration partners is relatively cost efficient and has eliminated the need for our direct investment in manufacturing facilities and additional staff early in development. Although we rely on contract manufacturers, we have personnel with manufacturing and quality experience to oversee our contract manufacturers.
To date, our third-party manufacturers have met our manufacturing requirements. We expect third-party manufacturers to be capable of providing sufficient quantities of our program materials to meet anticipated clinical trial scale demands. To meet our projected needs for commercial manufacturing, third parties with whom we currently work might need to increase their scale of production or we will need to secure alternate suppliers. We believe that there are alternate sources of supply that can satisfy our clinical and commercial requirements, although we cannot be certain that identifying and establishing relationships with such sources, if necessary, would not result in significant delay or material additional costs.
77
To date, our third-party manufacturers have met our quality standards. The manufacturers of pharmaceutical products must comply with strictly enforced cGMP requirements, state and federal regulations, as well as foreign requirements when applicable. Any failure of us or our contract manufacturing organizations to adhere to or document compliance to such regulatory requirements could lead to a delay or interruption in the availability of our program materials for clinical study. If we or our manufacturers were to fail to comply with the FDA, EMA, or other regulatory authority, it could result in sanctions being imposed on us, including clinical holds, fines, injunctions, civil penalties, delays, suspension or withdrawal of approvals, license revocation, seizures or recalls of product candidates or products, operating restrictions and criminal prosecutions, any of which could significantly and adversely affect supplies of our product candidates. Our potential future dependence upon others for the manufacture of our product candidates may also adversely affect our future profit margins and our ability to commercialize any product candidates that receive regulatory approval on a timely and competitive basis.
Biological products are inherently difficult to manufacture. Our program materials are manufactured using technically complex processes requiring specialized equipment and facilities, highly specific raw materials, and other production constraints. Our production process requires a number of highly specific raw materials with limited suppliers. Even though we aim to have backup supplies of raw materials whenever possible, we cannot be certain they will be sufficient if our primary sources are unavailable. A shortage of a critical raw material or a technical issue during manufacturing may lead to delays in clinical development or commercialization plans.
Delays in obtaining regulatory approval of our or our collaborators’ manufacturing process and facility or disruptions in our manufacturing process may delay or disrupt our commercialization efforts. Until recently, no cGMP gene therapy manufacturing facility in the United States had received approval from the FDA for the manufacture of an approved gene therapy product.
Before we can begin to commercially manufacture our product candidates in our own facility, or the facility of a collaborator, we must obtain regulatory approval from the FDA for our manufacturing process and our collaborator’s facility. A manufacturing authorization must also be obtained from the appropriate European Union regulatory authorities. Until recently, no cGMP gene therapy manufacturing facility in the United States had received approval from the FDA for the manufacture of an approved gene therapy product and, therefore, the timeframe required for us to obtain such approval is uncertain. In addition, we must pass a pre‑approval inspection of our or our collaborator’s manufacturing facility by the FDA and other relevant regulatory authorities before any of our product candidates can obtain marketing approval. In order to obtain approval, we will need to ensure that all of our processes, methods and equipment are compliant with cGMP, and perform extensive audits of vendors, contract laboratories and suppliers. If any of our vendors, contract laboratories or suppliers is found to be out of compliance with cGMP, we may experience delays or disruptions in manufacturing while we work with these third parties to remedy the violation or while we work to identify suitable replacement vendors. The cGMP requirements govern quality control of the manufacturing process and documentation policies and procedures. In complying with cGMP, we will be obligated to expend time, money and effort in production, record keeping and quality control to assure that the product meets applicable specifications and other requirements. If we fail to comply with these requirements, we would be subject to possible regulatory action and may not be permitted to sell any products that we may develop.
Failure to comply with ongoing regulatory requirements could cause us to suspend production or put in place costly or time‑consuming remedial measures.
The regulatory authorities may, at any time following approval of a product for sale, audit the manufacturing facilities for such product. If any such inspection or audit identifies a failure to comply with applicable regulations, or if a violation of product specifications or applicable regulations occurs independent of such an inspection or audit, the relevant regulatory authority may require remedial measures that may be costly or time‑consuming to implement and that may include the temporary or permanent suspension of a clinical trial or commercial sales or the temporary or permanent closure of a manufacturing facility. Any such remedial measures imposed upon our third‑party manufacturers or us could harm our business, financial condition, results of operations and prospects.
If our third‑party manufacturers or we fail to comply with applicable cGMP regulations, FDA and foreign regulatory authorities can impose regulatory sanctions including, among other things, refusal to approve a pending
78
application for a new product candidate or suspension or revocation of a pre‑existing approval. Such an occurrence may cause our business, financial condition, results of operations and prospects to be harmed.
Additionally, if supply from any third-party manufacturers is delayed or interrupted, there could be a significant disruption in the supply of our clinical or commercial material. We have agreements in place with our contract manufacturers pursuant to which we are collaborating on cGMP manufacturing processes and analytical methods for the manufacture of our AAV product candidates. Therefore, if we are unable to enter into an agreement with our contract manufacturers to manufacture clinical or commercial material for our product programs beyond VY-AADC, or if our agreement with our contract manufacturers were terminated, we would have to find suitable alternative manufacturers. This could delay our or our collaborators’ ability to conduct clinical trials or commercialize our current and future product candidates. The regulatory authorities also may require additional trials if a new manufacturer is relied upon for commercial production. Switching manufacturers may involve substantial costs and could result in a delay in our desired clinical and commercial timelines.
Any contamination in the manufacturing process for our products, shortages of raw materials or failure of any of our key suppliers to deliver necessary components could result in delays in our clinical development or marketing schedules.
Given the nature of biologics manufacturing, there is a risk of contamination. Any contamination could adversely affect our ability to produce product candidates on schedule and could, therefore, harm our results of operations and cause reputational damage.
Some of the raw materials required in our manufacturing process are derived from biologic sources. Such raw materials are difficult to procure and may be subject to contamination or recall. A material shortage, contamination, recall or restriction on the use of biologically derived substances in the manufacture of our product candidates could adversely impact or disrupt the commercial manufacturing or the production of clinical material, which could adversely affect our development timelines and our business, financial condition, results of operations and prospects.
Interruptions in the supply of product candidates or inventory loss may harm our operating results and financial condition.
Our product candidates are manufactured using technically complex processes requiring specialized facilities, highly specific raw materials and other production constraints. The complexity of these processes, as well as strict government standards for the manufacture and storage of our product candidates, subjects us to manufacturing risks. While product candidate batches released for use in clinical trials or for commercialization undergo sample testing, some defects may only be identified following product release. In addition, process deviations or unanticipated effects of approved process changes may result in these intermediate products not complying with stability requirements or specifications. Our product candidates must be stored and transported at temperatures within a certain range. If these environmental conditions deviate, our product candidates’ remaining shelf‑lives could be impaired or their efficacy and safety could be negatively impacted, making them no longer suitable for use.
The occurrence, or suspected occurrence, of manufacturing and distribution difficulties can lead to lost inventories and, in some cases, product recalls, with consequential reputational damage and the risk of product liability. The investigation and remediation of any identified problems can cause production delays, substantial expense, lost sales and delays of new product launches. Any interruption in the supply of finished products or the loss thereof could hinder our ability to timely distribute our products and satisfy customer demand. Any unforeseen failure in the storage of the product or loss in supply could delay our clinical trials and, if our product candidates are approved, result in a loss of our market share and negatively affect our business, financial condition, results of operations and prospects.
79
Risks Related to Our Business Operations
We may not be successful in our efforts to identify or discover additional product candidates and may fail to capitalize on programs or product candidates that may be a greater commercial opportunity, or for which there is a greater likelihood of success.
The success of our business depends upon our ability to identify, develop and commercialize product candidates generated through our product engine. Research programs to identify new product candidates require substantial technical, financial and human resources. Although VY‑AADC is currently in clinical development and our other product candidates are in preclinical development, we may fail to identify other potential product candidates for clinical development for several reasons. For example, our research may be unsuccessful in identifying potential product candidates or our potential product candidates may be shown to have harmful side effects, may be commercially impracticable to manufacture or may have other characteristics that may make the products unmarketable or unlikely to receive marketing approval.
Additionally, because we have limited resources, we may forego or delay pursuit of opportunities with certain programs or product candidates or for indications that later prove to have greater commercial potential. Our spending on current and future research and development programs may not yield any commercially viable products. If we do not accurately evaluate the commercial potential for a particular product candidate, we may relinquish valuable rights to that product candidate through strategic collaboration, licensing or other arrangements in cases in which it would have been more advantageous for us to retain sole development and commercialization rights to such product candidate. Alternatively, we may allocate internal resources to a product candidate in a therapeutic area in which it would have been more advantageous to enter into a partnering arrangement.
If any of these events occur, we may be forced to abandon our development efforts with respect to a particular product candidate or fail to develop a potentially successful product candidate, which could harm our business, financial condition, results of operations and prospects.
Our future success depends on our ability to retain key members of our management team, and to attract, retain and motivate qualified personnel.
We have been highly dependent on Steven M. Paul, M.D., our President and Chief Executive Officer as well as certain other members of our management team, the loss of whose services may adversely impact the achievement of our objectives. In early 2018, we announced Dr. Paul’s plans to transition from President and Chief Executive Officer to Executive Science Advisor. In addition to transitioning to an Executive Science Advisor role, in which he will focus on preclinical discovery research and portfolio development, Dr. Paul is expected to continue to serve on our Board of Directors, and as a member of our Science and Technology Committee.
While we have entered into employment agreements or offer letters with each of our executive officers, any of them could leave our employment at any time, as all of our employees are “at will” employees. We currently do not have “key person” insurance on any of our employees. The loss of the services of one or more of our current employees might impede the achievement of our research, development and commercialization objectives.
Recruiting and retaining other qualified employees, consultants and advisors for our business, including scientific and technical personnel, also will be critical to our success. There currently is a shortage of skilled individuals with substantial gene therapy experience, which is likely to continue. As a result, competition for skilled personnel, including in gene therapy research and vector manufacturing, is intense and the turnover rate can be high. We may not be able to attract and retain personnel on acceptable terms, if at all, given the competition among numerous pharmaceutical and biotechnology companies and academic institutions for individuals with similar skill sets. Our consultants and advisors may be employed by employers other than us and may have commitments under consulting or advisory contracts with other entities that may limit their availability to us. In addition, failure to succeed in preclinical or clinical trials or applications for marketing approval may make it more challenging to recruit and retain qualified personnel. The inability to recruit, or loss of services of certain executives, key employees, consultants or advisors, may impede the
80
progress of our research, development and commercialization objectives and could harm our business, financial condition, results of operations and prospects.
If we are unable to manage expected growth in the scale and complexity of our operations, our performance may suffer.
If we are successful in executing our business strategy, we will need to expand our managerial, operational, financial and other systems and resources to manage our operations, continue our research and development activities and, in the longer term, build a commercial infrastructure to support commercialization of any of our product candidates that are approved for sale. We can provide no assurances that we will have sufficient resources in the future to manage all of our planned programs. Future growth would impose significant added responsibilities on members of management, may lead to significant added costs, and may divert our management and business development resources. It is likely that our management, finance, development personnel, systems and facilities currently in place may not be adequate to support this future growth. Our need to effectively manage our operations, growth and product candidates requires that we continue to develop more robust business processes and improve our systems and procedures in each of these areas and to attract and retain sufficient numbers of talented employees. We may be unable to successfully implement these tasks on a larger scale and, accordingly, may not achieve our research, development and growth goals.
Our employees, principal investigators, consultants and commercial partners may engage in misconduct or other improper activities, including non‑compliance with regulatory standards and requirements and insider trading.
We are exposed to the risk of fraud or other misconduct by our employees, principal investigators, consultants and commercial partners. Misconduct by these parties could include intentional failures to comply with FDA regulations or the regulations applicable in the European Union and other jurisdictions, provide accurate information to the FDA, the European Commission and other regulatory authorities, comply with healthcare fraud and abuse laws and regulations in the United States and abroad, report financial information or data accurately or disclose unauthorized activities to us. In particular, sales, marketing and business arrangements in the healthcare industry are subject to extensive laws and regulations intended to prevent fraud, misconduct, kickbacks, self‑dealing and other abusive practices. These laws and regulations restrict or prohibit a wide range of pricing, discounting, marketing and promotion, sales commission, customer incentive programs and other business arrangements. Such misconduct also could involve the improper use of information obtained in the course of clinical trials or interactions with the FDA or other regulatory authorities, which could result in regulatory sanctions and cause serious harm to our reputation. We have adopted a code of conduct applicable to all of our employees, but it is not always possible to identify and deter employee misconduct, and the precautions we take to detect and prevent this activity may not be effective in controlling unknown or unmanaged risks or losses or in protecting us from government investigations or other actions or lawsuits stemming from a failure to comply with these laws or regulations. If any such actions are instituted against us, and we are not successful in defending ourselves or asserting our rights, those actions could have a significant impact on our business, financial condition, results of operations and prospects, including the imposition of significant fines or other sanctions.
81
Current and future legislation may increase the difficulty and cost for us and any future collaborators to obtain marketing approval of and commercialize our product candidates and affect the prices we, or they, may obtain.
In the United States and some foreign jurisdictions, there have been and continue to be a number of legislative and regulatory changes and proposed changes regarding the healthcare system that could, among other things, prevent or delay marketing approval of our product candidates, restrict or regulate post-approval activities and affect our ability, or the ability of any future collaborators, to profitably sell any products for which we, or they, obtain marketing approval. We expect that current laws, as well as other healthcare reform measures that may be adopted in the future, may result in more rigorous coverage criteria and in additional downward pressure on the price that we, or any future collaborators, may receive for any approved products.
In March 2010, President Obama signed into law the Patient Protection and Affordable Care Act, as amended by the Health Care and Education Reconciliation Act, or collectively the ACA. Among the provisions of the ACA of potential importance to our business and our product candidates are the following:
|
· |
an annual, non-deductible fee on any entity that manufactures or imports specified branded prescription drugs and biologic agents; |
|
· |
an increase in the statutory minimum rebates a manufacturer must pay under the Medicaid Drug Rebate Program; |
|
· |
a new Medicare Part D coverage gap discount program, in which manufacturers must agree to offer 50% point-of-sale discounts off negotiated prices; |
|
· |
expansion of the entities eligible for discounts under the Public Health Service pharmaceutical pricing program; |
|
· |
a new requirement to annually report drug samples that manufacturers and distributors provide to physicians; and |
|
· |
a new Patient-Centered Outcomes Research Institute to oversee, identify priorities in, and conduct comparative clinical effectiveness research, along with funding for such research. |
In addition, other legislative changes have been proposed and adopted since the ACA was enacted. These changes include the Budget Control Act of 2011, which, among other things, led to aggregate reductions to Medicare payments to providers of up to 2% per fiscal year that started in 2013 and, due to subsequent legislative amendments to the statute, will stay in effect through 2025 unless additional congressional action is taken, and the American Taxpayer Relief Act of 2012, which, among other things, reduced Medicare payments to several types of providers and increased the statute of limitations period for the government to recover overpayments to providers from three to five years. These new laws may result in additional reductions in Medicare and other healthcare funding and otherwise affect the prices we may obtain for any of our product candidates for which we may obtain regulatory approval or the frequency with which any such product candidate is prescribed or used. Further, there have been several recent U.S. congressional inquiries and proposed state and federal legislation designed to, among other things, bring more transparency to drug pricing,
82
review the relationship between pricing and manufacturer patient programs, reduce the costs of drugs under Medicare and reform government program reimbursement methodologies for drug products.
We expect that these healthcare reforms, as well as other healthcare reform measures that may be adopted in the future, may result in additional reductions in Medicare and other healthcare funding, more rigorous coverage criteria, new payment methodologies and additional downward pressure on the price that we receive for any approved product and/or the level of reimbursement physicians receive for administering any approved product we might bring to market. Reductions in reimbursement levels may negatively impact the prices we receive or the frequency with which our products are prescribed or administered. Any reduction in reimbursement from Medicare or other government programs may result in a similar reduction in payments from private payors.
Since enactment of the ACA, there have been numerous legal challenges and Congressional actions to repeal and replace provisions of the law. In May 2017, the U.S. House of Representatives passed legislation known as the American Health Care Act of 2017. Thereafter, the Senate Republicans introduced and then updated a bill to replace the ACA known as the Better Care Reconciliation Act of 2017. The Senate Republicans also introduced legislation to repeal the ACA without companion legislation to replace it, and a “skinny” version of the Better Care Reconciliation Act of 2017. In addition, the Senate considered proposed healthcare reform legislation known as the Graham-Cassidy bill. None of these measures was passed by the U.S. Senate.
With enactment of the Tax Cuts and Jobs Act of 2017, which was signed by the President on December 22, 2017, Congress repealed the “individual mandate.” The repeal of this provision, which requires most Americans to carry a minimal level of health insurance, will become effective in 2019. According to the Congressional Budget Office, the repeal of the individual mandate will cause 13 million fewer Americans to be insured in 2027 and premiums in insurance markets may rise. Further, each chamber of the Congress has put forth multiple bills designed to repeal or repeal and replace portions of the ACA. Although none of these measures has been enacted by Congress to date, Congress may consider other legislation to repeal and replace elements of the ACA. The Congress will likely consider other legislation to replace elements of the ACA, during the next Congressional session.
The Trump Administration has also taken executive actions to undermine or delay implementation of the ACA. In January 2017, President Trump signed an Executive Order directing federal agencies with authorities and responsibilities under the ACA to waive, defer, grant exemptions from, or delay the implementation of any provision of the ACA that would impose a fiscal or regulatory burden on states, individuals, healthcare providers, health insurers, or manufacturers of pharmaceuticals or medical devices. In October 2017, the President signed a second Executive Order allowing for the use of association health plans and short-term health insurance, which may provide fewer health benefits than the plans sold through the ACA exchanges. At the same time, the Trump Administration announced that it will discontinue the payment of cost-sharing reduction, or CSR, payments to insurance companies until Congress approves the appropriation of funds for such CSR payments. The loss of the CSR payments is expected to increase premiums on certain policies issued by qualified health plans under the ACA. A bipartisan bill to appropriate funds for CSR payments was introduced in the Senate, but the future of that bill is uncertain.
The costs of prescription pharmaceuticals in the United States has also been the subject of considerable discussion in the United States, and members of Congress and the Trump Administration have stated that they will address such costs through new legislative and administrative measures. To date, there have been several recent U.S. congressional inquiries and proposed state and federal legislation designed to, among other things, bring more transparency to drug pricing, review the relationship between pricing and manufacturer patient programs, reduce the costs of drugs under Medicare and reform government program reimbursement methodologies for drug products. The pricing of prescription pharmaceuticals is also subject to governmental control outside the United States. In these countries, pricing negotiations with governmental authorities can take considerable time after the receipt of marketing approval for a product. To obtain reimbursement or pricing approval in some countries, we may be required to conduct a clinical trial that compares the cost effectiveness of our product candidates to other available therapies. If reimbursement of our products is unavailable or limited in scope or amount, or if pricing is set at unsatisfactory levels, our ability to generate revenues and become profitable could be impaired.
83
Finally, legislative and regulatory proposals have also been made to expand post-approval requirements and restrict sales and promotional activities for pharmaceutical products. We cannot be sure whether additional legislative changes will be enacted, or whether the FDA regulations, guidance or interpretations will be changed, or what the impact of such changes on the marketing approvals of our product candidates, if any, may be. In addition, increased scrutiny by the U.S. Congress of the FDA’s approval process may significantly delay or prevent marketing approval, as well as subject us and any future collaborators to more stringent product labeling and post-marketing testing and other requirements.
Under the CURES Act and the Trump Administration’s regulatory reform initiatives, the FDA’s policies, regulations and guidance may be revised or revoked and that could prevent, limit or delay regulatory approval of our product candidates, which would impact our ability to generate revenue.
In December 2016, the 21st Century Cures Act, or Cures Act, was signed into law. The Cures Act, among other things, is intended to modernize the regulation of drugs and spur innovation, but its ultimate implementation is unclear. If we are slow or unable to adapt to changes in existing requirements or the adoption of new requirements or policies, or if we are not able to maintain regulatory compliance, we may lose any marketing approval that we may have obtained and we may not achieve or sustain profitability, which would adversely affect our business, prospects, financial condition and results of operations.
We also cannot predict the likelihood, nature or extent of government regulation that may arise from future legislation or administrative or executive action, either in the United States or abroad. For example, certain policies of the Trump administration may impact our business and industry. Namely, the Trump administration has taken several executive actions, including the issuance of a number of Executive Orders, that could impose significant burdens on, or otherwise materially delay, the FDA’s ability to engage in routine regulatory and oversight activities such as implementing statutes through rulemaking, issuance of guidance, and review and approval of marketing applications. An under-staffed FDA could result in delays in the FDA’s responsiveness or in its ability to review submissions or applications, issue regulations or guidance, or implement or enforce regulatory requirements in a timely fashion or at all. Moreover, on January 30, 2017, President Trump issued an Executive Order, applicable to all executive agencies, including the FDA, which requires that for each notice of proposed rulemaking or final regulation to be issued in fiscal year 2017, the agency shall identify at least two existing regulations to be repealed, unless prohibited by law. These requirements are referred to as the “two-for-one” provisions. This Executive Order includes a budget neutrality provision that requires the total incremental cost of all new regulations in the 2017 fiscal year, including repealed regulations, to be no greater than zero, except in limited circumstances. For fiscal years 2018 and beyond, the Executive Order requires agencies to identify regulations to offset any incremental cost of a new regulation and approximate the total costs or savings associated with each new regulation or repealed regulation. In interim guidance issued by the Office of Information and Regulatory Affairs within OMB on February 2, 2017, the administration indicates that the “two-for-one” provisions may apply not only to agency regulations, but also to significant agency guidance documents. In addition, on February 24, 2017, President Trump issued an executive order directing each affected agency to designate an agency official as a “Regulatory Reform Officer” and establish a “Regulatory Reform Task Force” to implement the two-for-one provisions and other previously issued executive orders relating to the review of federal regulations, however it is difficult to predict how these requirements will be implemented, and the extent to which they will impact the FDA’s ability to exercise its regulatory authority. If these executive actions impose constraints on the FDA’s ability to engage in oversight and implementation activities in the normal course, our business may be negatively impacted.
We may be subject, directly or indirectly, to federal, state, and foreign healthcare laws and regulations, including fraud and abuse laws, false claims laws and health information privacy and security laws. If we are unable to comply, or have not fully complied, with such laws, we could face substantial penalties.
If we obtain FDA approval for any of our product candidates and begin commercializing those products in the United States, our operations will be directly, or indirectly through our prescribers, customers and purchasers, subject to various federal and state laws and regulations, including, without limitation, the federal Anti‑Kickback Statute, the federal civil and criminal false claims act, and the Physician Payments Sunshine Act and regulations. These laws will impact, among other things, our proposed sales, marketing and educational programs. In addition, we may be subject to data privacy laws by both the federal government and the states in which we conduct our business. Such laws that may
84
constrain the business or financial arrangements and relationships through which we conduct our operations include, but are not limited to:
|
· |
the federal Anti‑Kickback Statute, which prohibits, among other things, persons and entities from knowingly and willfully soliciting, receiving, offering or paying any remuneration (including any kickback, bribe or rebate), directly or indirectly, overtly or covertly, in cash or in kind, to induce or in return for either the referral of an individual for, or the purchase, recommendation, leasing or furnishing of, an item or service reimbursable under a federal healthcare program, such as the Medicare and Medicaid programs. This statute has been interpreted to apply to arrangements between pharmaceutical manufacturers on the one hand, and prescribers, purchasers and formulary managers on the other. Further, the Affordable Care Act amended the intent requirement of the federal Anti‑Kickback Statute. A person or entity no longer needs to have actual knowledge of this statute or specific intent to violate it; |
|
· |
the federal civil and criminal false claims laws and civil monetary penalty laws, including the civil False Claims Act, which prohibit, among other things, individuals or entities from knowingly presenting, or causing to be presented, claims for payment or approval from Medicare, Medicaid or other government payors that are false or fraudulent, or making a false statement to avoid, decrease, or conceal an obligation to pay money to the federal government. The Affordable Care Act provided and recent government cases against pharmaceutical and medical device manufacturers support the view that federal Anti‑Kickback Statute violations and certain marketing practices, including off‑label promotion, may implicate the civil False Claims Act; |
|
· |
the federal Health Insurance Portability and Accountability Act of 1996, or HIPAA, which created additional federal criminal statutes that prohibit a person from knowingly and willfully executing or attempting to execute a scheme or from making false or fraudulent statements to defraud any healthcare benefit program, regardless of the payor (e.g., public or private); |
|
· |
HIPAA, as amended by the Health Information Technology for Economic and Clinical Health Act, or HITECH, and its implementing regulations, and as amended again by the final HIPAA omnibus rule, Modifications to the HIPAA Privacy, Security, Enforcement, and Breach Notification Rules Under HITECH and the Genetic Information Nondiscrimination Act; Other Modifications to HIPAA, published in January 2013, which imposes certain requirements relating to the privacy, security and transmission of individually identifiable health information without appropriate authorization by entities subject to the rule, such as health plans, health care clearinghouses and health care providers; |
|
· |
federal transparency laws, including the federal Physician Payments Sunshine Act, which is part of the Affordable Care Act, that requires certain manufacturers of drugs, devices, biologics and medical supplies for which payment is available under Medicare, Medicaid, or the Children’s Health Insurance Program, with specific exceptions, to report annually to Center for Medicare & Medicaid Services, or CMS, information related to payments and other transfers of value provided to physicians and teaching hospitals, and ownership and investment interests held by physicians and their immediate family members, by the 90th day of each subsequent calendar year, and disclosure of such information is made by CMS on a publicly available website; and |
|
· |
state and/or foreign law equivalents of each of the above federal laws, such as state anti‑kickback and false claims laws that may apply to arrangements and claims involving health care items or services reimbursed by non‑governmental third-party payors; state laws that require drug manufacturers to report information related to payments and other transfers of value to physicians and other healthcare providers or marketing expenditures; state laws that require pharmaceutical companies to comply with the pharmaceutical industry’s voluntary compliance guidelines and the relevant compliance guidance promulgated by the federal government; and state and foreign laws governing the privacy and security of health information in certain circumstances, many of which differ from each other in significant ways and may not have the same effect, thus complicating compliance efforts in certain circumstances, such as specific disease states. |
85
Because of the breadth of these laws and the narrowness of the statutory exceptions and safe harbors available, it is possible that some of our business activities could be subject to challenge under one or more of such laws. If our operations are found to be in violation of any of the laws described above or any other government regulations that apply to us, we may be subject to penalties, including civil and criminal penalties, damages, fines, exclusion from participation in government health care programs, such as Medicare and Medicaid, disgorgement, contractual damages, reputational harm, diminished profits and future earnings, imprisonment and the curtailment or restructuring of our operations, any of which could adversely affect our ability to operate our business and our results of operations.
The provision of benefits or advantages to physicians to induce or encourage the prescription, recommendation, endorsement, purchase, supply, order or use of medicinal products is prohibited in the European Union. The provision of benefits or advantages to physicians is also governed by the national anti‑bribery laws of European Union Member States, such as the UK Bribery Act 2010. Infringement of these laws could result in substantial fines and imprisonment.
Payments made to physicians in certain European Union Member States must be publicly disclosed. Moreover, agreements with physicians often must be the subject of prior notification and approval by the physician’s employer, his or her competent professional organization and/or the regulatory authorities of the individual European Union Member States. These requirements are provided in the national laws, industry codes or professional codes of conduct, applicable in the European Union Member States. Failure to comply with these requirements could result in reputational risk, public reprimands, administrative penalties, fines or imprisonment.
The collection and use of personal health data in the European Union is governed by the provisions of the Data Protection Directive. This directive imposes several requirements relating to the consent of the individuals to whom the personal data relates, the information provided to the individuals, notification of data processing obligations to the competent national data protection authorities and the security and confidentiality of the personal data. The Data Protection Directive also imposes strict rules on the transfer of personal data out of the European Union to the United States. Failure to comply with the requirements of the Data Protection Directive and the related national data protection laws of the European Union Member States may result in fines and other administrative penalties. The draft Data Protection Regulation currently going through the adoption process is expected to introduce new data protection requirements in the European Union and substantial fines for breaches of the data protection rules. If the draft Data Protection Regulation is adopted in its current form it may increase our responsibility and liability in relation to personal data that we process and we may be required to put in place additional mechanisms ensuring compliance with the new data protection rules. This may be onerous and adversely affect our business, financial condition, results of operations and prospects.
Product liability lawsuits against us could cause us to incur substantial liabilities and could limit commercialization of any product candidates that we may develop.
We face an inherent risk of product liability exposure related to the testing of our product candidates in clinical trials and may face an even greater risk if we commercialize any products that we may develop. If we cannot successfully defend ourselves against claims that our product candidates caused injuries, we could incur substantial liabilities. Regardless of merit or eventual outcome, liability claims may result in:
|
· |
decreased demand for any product candidates that we may develop; |
|
· |
loss of revenue; |
|
· |
substantial monetary awards to trial participants or patients; |
|
· |
significant time and costs to defend the related litigation; |
|
· |
withdrawal of clinical trial participants; |
|
· |
the inability to commercialize any product candidates that we may develop; and |
86
|
· |
injury to our reputation and significant negative media attention. |
Although we maintain product liability insurance coverage in the amount of $5.0 million per occurrence and $50.0 million in the aggregate, this insurance may not be adequate to cover all liabilities that we may incur. We anticipate that we will need to increase our insurance coverage each time we commence a clinical trial and if we successfully commercialize any product candidate. Insurance coverage is increasingly expensive. We may not be able to maintain insurance coverage at a reasonable cost or in an amount adequate to satisfy any liability that may arise.
If we, our collaborators, or any third-party manufacturers we engage fail to comply with environmental, health and safety laws and regulations, we could become subject to fines or penalties or incur costs that could harm our business.
We, our collaborators, and any third-party manufacturers we engage are subject to numerous environmental, health and safety laws and regulations, including those governing laboratory procedures and the generation, handling, use, storage, treatment, manufacture, transportation and disposal of, and exposure to, hazardous materials and wastes, as well as laws and regulations relating to occupational health and safety. Our operations involve the use of hazardous and flammable materials, including chemicals and biologic and radioactive materials. Our operations also produce hazardous waste products. We generally contract with third parties for the disposal of these materials and wastes. We cannot eliminate the risk of contamination or injury from these materials. In the event of contamination or injury resulting from our use of hazardous materials, we could be held liable for any resulting damages, and any liability could exceed our resources. We also could incur significant costs associated with civil or criminal fines and penalties.
Although we maintain general liability insurance and workers’ compensation insurance for certain costs and expenses we may incur due to injuries to our employees resulting from the use of hazardous materials or other work-related injuries, this insurance may not provide adequate coverage against potential liabilities. We do not maintain insurance for environmental liability or toxic tort claims that may be asserted against us in connection with our storage or disposal of biologic, hazardous or radioactive materials.
In addition, we may incur substantial costs in order to comply with current or future environmental, health and safety laws and regulations, which have tended to become more stringent over time. These current or future laws and regulations may impair our research, development or production efforts. Failure to comply with these laws and regulations also may result in substantial fines, penalties or other sanctions or liabilities, which could harm our business, financial condition, results of operations and prospects.
Further, with respect to the operations of any current or future collaborators or third-party contract manufacturers, it is possible that if they fail to operate in compliance with applicable environmental, health and safety laws and regulations or properly dispose of wastes associated with our products, we could be held liable for any resulting damages, suffer reputational harm or experience a disruption in the manufacture and supply of our product candidates or products.
Unfavorable global economic conditions could adversely affect our business, financial condition or results of operations.
Our results of operations could be adversely affected by general conditions in the global economy and in the global financial markets. The most recent global financial crisis caused extreme volatility and disruptions in the capital and credit markets. A severe or prolonged economic downturn, such as the most recent global financial crisis, could result in a variety of risks to our business, including weakened demand for our product candidates and our ability to raise additional capital when needed on acceptable terms, if at all. This is particularly true in the European Union, which is recovering from a severe economic crisis. A weak or declining economy could strain our suppliers, possibly resulting in supply disruption, or cause delays in payments for our services by third‑party payors or our collaborators. Any of the foregoing could harm our business and we cannot anticipate all of the ways in which the current economic climate and financial market conditions could adversely impact our business.
87
Our internal computer systems, or those of our collaborators or other contractors or consultants, may fail or suffer security breaches, which could result in a material disruption of our product development programs.
Our internal computer systems and those of our current and any future collaborators and other contractors or consultants are vulnerable to damage from computer viruses, unauthorized access, natural disasters, terrorism, war and telecommunication and electrical failures. While we have not experienced any such material system failure, accident or security breach to date, if such an event were to occur and cause interruptions in our operations, it could result in a disruption of our development programs and our business operations, whether due to a loss of our trade secrets or other proprietary information or other similar disruptions. For example, the loss of clinical trial data from completed or future clinical trials could result in delays in our regulatory approval efforts and significantly increase our costs to recover or reproduce the data. Although we maintain cyber risk insurance for certain costs we may incur due to a cyber related event, this insurance may not provide adequate coverage against potential liabilities. Additionally, to the extent that any disruption or security breach were to result in a loss of, or damage to, our data or applications, or inappropriate disclosure of confidential or proprietary information, we could incur liability, our competitive position could be harmed, and the further development and commercialization of our product candidates could be delayed.
Risks Related to the Commercialization of Our Product Candidates
The affected populations for our product candidates may be smaller than we or third parties currently project, which may affect the addressable markets for our product candidates.
Our projections of the number of people who have the diseases we are seeking to treat, as well as the subset of people with these diseases who have the potential to benefit from treatment with our product candidates, are estimates based on our knowledge and understanding of these diseases. The total addressable market opportunity for our product candidates will ultimately depend upon a number of factors including the diagnosis and treatment criteria included in the final label, if approved for sale in specified indications, acceptance by the medical community, patient access and product pricing and reimbursement. Prevalence estimates are frequently based on information and assumptions that are not exact and may not be appropriate, and the methodology is forward‑looking and speculative. The process we have used in developing an estimated prevalence range for the indications we are targeting has involved collating limited data from multiple sources. While we believe these sources are reliable, we have not independently verified the data. Accordingly, the prevalence estimates included in our periodic reports and other reports filed with or furnished to the SEC should be viewed with caution. Further, the data and statistical information used in such reports, including estimates derived from them, may differ from information and estimates made by our competitors or from current or future studies conducted by independent sources.
The use of such data involves risks and uncertainties and is subject to change based on various factors. Our estimates may prove to be incorrect and new studies may change the estimated incidence or prevalence of the diseases we seek to address. The number of patients with the diseases we are targeting in the United States, the European Union and elsewhere may turn out to be lower than expected or may not be otherwise amenable to treatment with our products, or new patients may become increasingly difficult to identify or access, all of which would harm our results of operations and our business.
If we are unable to establish sales, medical affairs and marketing capabilities or enter into agreements with third parties to market and sell our product candidates, we may be unable to generate any product revenue.
We have recently begun to build our sales and marketing organization. To successfully commercialize any products that may result from our clinical development programs, we will need to further develop these capabilities, either on our own or with others. The establishment and development of our own commercial team or the establishment of a contract sales force to market any products we may develop will be expensive and time‑consuming and could delay any product launch. Moreover, we cannot be certain that we will be able to successfully develop this capability.
Under our collaboration agreement with Sanofi Genzyme, Sanofi Genzyme has an exclusive option to license, develop and commercialize ex‑U.S. rights to our Friedreich’s ataxia program, a future program to be designated by Sanofi Genzyme and our Huntington’s disease program. Additionally, we have granted Sanofi Genzyme an incremental
88
option to co‑commercialize our Huntington’s disease program in the United States and to acquire worldwide rights to our spinal muscular atrophy program. If Sanofi Genzyme exercises any of these options, we would be eligible to receive specified option fees. In addition, we would be eligible to receive specified milestone payments and royalties for any product developed in such programs.
Under our collaboration and option agreement with AbbVie, AbbVie has options to advance certain compounds into further development and to obtain an exclusive, worldwide license, with the right to sublicense, under certain of our intellectual property rights to develop and commercialize such compounds and corresponding products for all human diagnostic, prophylactic and therapeutic uses. If AbbVie exercises any of these options, we would be eligible to receive specified option fees. In addition, we would be eligible to receive specified development and regulatory milestone payments and tiered royalties on the global commercial net sales products developed under our collaboration.
In the future, we may enter into collaborations regarding other of our product candidates with other entities to utilize their established marketing and distribution capabilities, but we may be unable to enter into such agreements on favorable terms, if at all. If any current or future collaborators do not commit sufficient resources to commercialize our products, or we are unable to develop the necessary capabilities on our own, we will be unable to generate sufficient product revenue to sustain our business. We compete with many companies that currently have extensive, experienced and well‑funded medical affairs, marketing and sales operations to recruit, hire, train and retain marketing and sales personnel. We also face competition in our search for third parties to assist us with the sales and marketing efforts of our product candidates. We might face unforeseen costs and expenses associated with creating an independent sales and marketing organization. Our sales personnel might also face difficulties obtaining access to physicians or being able to persuade adequate numbers of physicians to use or prescribe our products or selling our products if we lack complementary products, which could disadvantage us compared to companies with more extensive product lines. Without an internal team or the support of a third‑party to perform marketing and sales functions, we may be unable to compete successfully against these more established companies.
Our efforts to educate the medical community and third‑party payors on the benefits of our product candidates may require significant resources and may never be successful. Such efforts may require more resources than are typically required due to the complexity and uniqueness of our potential products. If any of our product candidates is approved but fails to achieve market acceptance among physicians, patients, or third‑party payors, we will not be able to generate significant revenues from such product, which could harm our business, financial condition, results of operations and prospects.
The insurance coverage and reimbursement status of newly‑approved products is uncertain. Failure to obtain or maintain adequate coverage and reimbursement for our product candidates, if approved, could limit our ability to market those products and decrease our ability to generate product revenue.
We expect the cost of a single administration of gene therapy products, such as those we are developing, to be substantial, when and if they achieve regulatory approval. We expect that coverage and reimbursement by government and private payors will be essential for most patients to be able to afford these treatments. Accordingly, sales of our product candidates will depend substantially, both domestically and abroad, on the extent to which the costs of our product candidates will be paid by health maintenance, managed care, pharmacy benefit and similar healthcare management organizations, or will be reimbursed by government authorities, private health coverage insurers and other third‑party payors. Coverage and reimbursement by a third‑party payor may depend upon several factors, including the third‑party payor’s determination that use of a product is:
|
· |
a covered benefit under its health plan; |
|
· |
safe, effective and medically necessary; |
|
· |
appropriate for the specific patient and the indication; |
|
· |
convenient and easy-to-administer compared to alternative treatments; |
|
· |
cost‑effective compared to alternative treatments; and |
89
|
· |
neither experimental nor investigational. |
No uniform policy requirement for coverage and reimbursement for drug products exists among third‑party payors. Therefore, coverage and reimbursement for drug products can differ significantly from payor to payor. As a result, obtaining coverage and reimbursement for a product from third‑party payors is a time‑consuming and costly process that could require us to provide to each different payor supporting scientific, clinical and cost‑effectiveness data. We may not be able to provide data sufficient to gain acceptance with respect to coverage and reimbursement. If coverage and reimbursement are not available, or are available only at limited levels, we may not be able to successfully commercialize our product candidates. Even if coverage is provided, the approved reimbursement amount may not be adequate to realize a sufficient return on our investment including our research, development, manufacture, sales, and distribution expenses. Interim reimbursement levels for new drugs, if applicable, may also not be sufficient to cover our costs and may not be made permanent. Reimbursement rates may vary according to the use of the drug and the clinical setting in which it is used, may be based on reimbursement levels already set for lower cost drugs and may be incorporated into existing payments for other services. Assuming we obtain coverage for a given product by a third‑party payor, the resulting reimbursement payment rates may not be adequate or may require co‑payments that patients find unacceptably high. Patients who are prescribed medications for the treatment of their conditions, and their prescribing physicians, generally rely on third‑party payors to reimburse all or part of the costs associated with their prescription drugs. Patients are unlikely to use our products unless coverage is provided and reimbursement is adequate to cover all or a significant portion of the cost of our products. Therefore, coverage and adequate reimbursement is critical to new product acceptance. Additionally, there may be significant delays in obtaining coverage and reimbursement for newly approved drugs and biologics, and coverage may be more limited than the purposes for which the drug is approved by the FDA or comparable foreign regulatory authorities.
There is significant uncertainty related to third‑party coverage and reimbursement of newly approved products. In the United States, third‑party payors, including government payors such as the Medicare and Medicaid programs, play an important role in determining the extent to which new drugs and biologics will be covered and reimbursed. The Medicare and Medicaid programs increasingly are used as models for how private payors and government payors develop their coverage and reimbursement policies. A primary trend in the U.S. healthcare industry and elsewhere is cost containment. Government authorities and third-party payors have attempted to control costs by limiting coverage and the amount of reimbursement for particular medications. Increasingly, third-party payors are requiring that drug companies provide them with predetermined discounts from list prices and are challenging the prices charged for medical products.
The CMS is responsible for determining whether a product should be approved for coverage and reimbursement under the Medicare program. It is difficult to predict what CMS will decide with respect to coverage and reimbursement for novel products such as ours, as there is no body of established practices and precedents for these types of products. Currently, no gene therapy product has been approved for coverage and reimbursement by the CMS. Moreover, reimbursement agencies in the European Union may be more conservative than CMS. For example, several cancer drugs have been approved for reimbursement in the United States and have not been approved for reimbursement in certain European Union Member States. It is difficult to predict what third‑party payors will decide with respect to the coverage and reimbursement for our product candidates, especially given that the cost of our product candidates is likely to be very high and pricing of such products is highly uncertain.
Outside the United States, international operations generally are subject to extensive government price controls and other market regulations, and increasing emphasis on cost‑containment initiatives in the European Union, Canada and other countries may put pricing pressure on us. For example, one gene therapy product was approved in the European Union in 2012 but is yet to be widely available commercially. In many countries, the prices of medical products are subject to varying price control mechanisms as part of national health systems. In general, the prices of medicines under such systems are substantially lower than in the United States. Other countries allow companies to fix their own prices for medical products, but monitor and control company profits. Additional foreign price controls or other changes in pricing regulation could restrict the amount that we are able to charge for our product candidates. Accordingly, in markets outside the United States, the reimbursement for our products may be reduced compared with the United States and may be insufficient to generate commercially reasonable product revenues.
90
Moreover, increasing efforts by government and third‑party payors in the United States and abroad to cap or reduce healthcare costs may cause such organizations to limit both coverage and the level of reimbursement for new products approved and, as a result, they may not cover or provide adequate payment for our product candidates. Payors increasingly are considering new metrics as the basis for reimbursement rates, such as average sales price, or ASP, average manufacturer price, or AMP, and Actual Acquisition Cost. The existing data for reimbursement based on some of these metrics is relatively limited, although certain states have begun to survey acquisition cost data for the purpose of setting Medicaid reimbursement rates, and CMS has begun making pharmacy National Average Drug Acquisition Cost and National Average Retail Price data publicly available on at least a monthly basis. The regulations that govern marketing approvals, pricing, coverage and reimbursement for new drug and device products vary widely from country to country. Current and future legislation may significantly change the approval requirements in ways that could involve additional costs and cause delays in obtaining approvals. Some countries require approval of the sale price of a drug before it can be marketed. In many countries, the pricing review period begins after marketing or product licensing approval is granted. In some foreign markets, prescription pharmaceutical pricing remains subject to continuing governmental control even after initial approval is granted. As a result, we might obtain marketing approval for a product in a particular country, but then be subject to price regulations that delay our commercial launch of the product, possibly for lengthy time periods, and negatively impact the revenues we are able to generate from the sale of the product in that country. To obtain reimbursement or pricing approval in some countries, we may be required to conduct a clinical trial that compares the cost-effectiveness of our product candidate to other available therapies. Adverse pricing limitations may hinder our ability to recoup our investment in one or more product candidates, even if our product candidates obtain marketing approval.
Therefore, it is difficult to project the impact of these evolving reimbursement metrics on the willingness of payors to cover candidate products that we or our partners are able to commercialize. We expect to experience pricing pressures in connection with the sale of any of our product candidates due to the trend toward managed healthcare, the increasing influence of health maintenance organizations and additional legislative changes. The downward pressure on healthcare costs in general, particularly prescription drugs and surgical procedures and other treatments, has become intense. As a result, increasingly high barriers are being erected to the entry of new products such as ours.
The commercial success of any of our product candidates will depend upon its degree of market acceptance by physicians, patients, third‑party payors and others in the medical community.
Ethical, social and legal concerns about gene therapy could result in additional regulations restricting or prohibiting our products. Even with the requisite approvals from the FDA in the United States, EMA in the European Union and other regulatory authorities internationally, the commercial success of our product candidates will depend, in part, on the acceptance of physicians, patients and health care payors of gene therapy products in general, and our product candidates in particular, as medically necessary, cost‑effective and safe. Any product that we commercialize may not gain acceptance by physicians, patients, health care payors and others in the medical community. If these products do not achieve an adequate level of acceptance, we may not generate significant product revenue and may not become profitable. The degree of market acceptance of gene therapy products and, in particular, our product candidates, if approved for commercial sale, will depend on several factors, including:
|
· |
the efficacy and safety of such product candidates as demonstrated in clinical trials; |
|
· |
the potential and perceived advantages of product candidates over alternative treatments; |
|
· |
the cost of treatment relative to alternative treatments; |
|
· |
the clinical indications for which the product candidate is approved by the FDA or the European Commission, or other regulatory authorities; |
|
· |
patient awareness of, and willingness to seek, genotyping; |
|
· |
the willingness of physicians to prescribe new therapies; |
91
|
· |
the willingness of physicians to undergo specialized training with respect to administration of our product candidates; |
|
· |
the willingness of the target patient population to try new therapies; |
|
· |
the prevalence and severity of any side effects; |
|
· |
product labeling or product insert requirements of the FDA, EMA or other regulatory authorities, including any limitations or warnings contained in a product’s approved labeling or restrictions on the use of our products together with other medications; |
|
· |
relative convenience and ease of administration; |
|
· |
the strength of marketing and distribution support; |
|
· |
the timing of market introduction of competitive products; |
|
· |
publicity concerning our products or competing products and treatments; and |
|
· |
sufficient third‑party payor coverage and reimbursement. |
Even if a potential product displays a favorable efficacy and safety profile in preclinical studies and clinical trials, market acceptance of the product will not be fully known until after it is launched.
Our gene therapy approach utilizes vectors derived from viruses, which may be perceived as unsafe or may result in unforeseen adverse events. Negative public opinion and increased regulatory scrutiny of gene therapy may damage public perception of the safety of our product candidates and adversely affect our ability to conduct our business or obtain regulatory approvals for our product candidates.
Gene therapy remains a novel technology, with three gene therapy products approved to date in the United States and only two gene therapy products approved to date in the European Union, of which one is no longer approved. Public perception may be influenced by claims that gene therapy is unsafe, and gene therapy may not gain the acceptance of the public or the medical community. In particular, our success will depend upon physicians who specialize in the treatment of genetic diseases targeted by our product candidates, prescribing treatments that involve the use of our product candidates in lieu of, or in addition to, existing treatments with which they are familiar and for which greater clinical data may be available. More restrictive government regulations or negative public opinion would have an adverse effect on our business, financial condition, results of operations and prospects and may delay or impair the development and commercialization of our product candidates or demand for any products we may develop. For example, earlier gene therapy trials led to several well‑publicized adverse events, including cases of leukemia and death seen in other trials using non-AAV vectors. Serious adverse events in our clinical trials, or other clinical trials involving gene therapy products or our competitors’ products, even if not ultimately attributable to the relevant product candidates, and the resulting publicity, could result in increased government regulation, unfavorable public perception, potential regulatory delays in the testing or approval of our product candidates, stricter labeling requirements for those product candidates that are approved and a decrease in demand for any such product candidates.
If we obtain approval to commercialize our product candidates outside of the United States, in particular in the European Union, a variety of risks associated with international operations could harm our business.
We expect that we will be subject to additional risks in commercializing our product candidates outside the United States, including:
|
· |
different regulatory requirements for approval of drugs and biologics in foreign countries; |
92
|
· |
reduced protection for intellectual property rights; |
|
· |
unexpected changes in tariffs, trade barriers and regulatory requirements; |
|
· |
economic weakness, including inflation, or political instability in particular foreign economies and markets; |
|
· |
compliance with tax, employment, immigration and labor laws for employees living or traveling abroad; |
|
· |
foreign currency fluctuations, which could result in increased operating expenses and reduced revenues, and other obligations incident to doing business in another country; |
|
· |
workforce uncertainty in countries where labor unrest is more common than in the United States; |
|
· |
shortages resulting from any events affecting raw material supply or manufacturing capabilities abroad; |
|
· |
business interruptions resulting from geopolitical actions, including war and terrorism or natural disasters including earthquakes, typhoons, floods and fires, or from economic or political instability; and |
|
· |
greater difficulty with enforcing our contracts in jurisdictions outside of the United States. |
We must dedicate additional resources to comply with numerous laws and regulations in each jurisdiction in which we plan to operate. The Foreign Corrupt Practices Act, or FCPA, prohibits any U.S. individual or business from paying, offering, authorizing payment or offering of anything of value, directly or indirectly, to any foreign official, political party or candidate for the purpose of influencing any act or decision of the foreign entity in order to assist the individual or business in obtaining or retaining business. The FCPA also obligates companies whose securities are listed in the United States to comply with certain accounting provisions requiring the company to maintain books and records that accurately and fairly reflect all transactions of the corporation, including international subsidiaries, and to devise and maintain an adequate system of internal accounting controls for international operations.
Compliance with the FCPA is expensive and difficult, particularly in countries in which corruption is a recognized problem. In many foreign countries, it is common for others to engage in business practices that are prohibited by U.S. laws and regulations applicable to us, including the FCPA. In addition, the FCPA presents particular challenges in the pharmaceutical industry, because, in many countries, hospitals are operated by the government, and doctors and other hospital employees are considered foreign officials. Certain payments to hospitals in connection with clinical trials and other work have been deemed to be improper payments to government officials and have led to FCPA enforcement actions.
Various laws, regulations and executive orders also restrict the use and dissemination outside of the United States, or the sharing with certain non-U.S. nationals, of information classified for national security purposes, as well as certain products and technical data relating to those products. If we expand our presence outside of the United States, it will require us to dedicate additional resources to comply with these laws, and these laws may preclude us from developing, manufacturing, or selling certain products and product candidates outside of the United States, which could limit our growth potential and increase our development costs.
The failure to comply with laws governing international business practices may result in substantial civil and criminal penalties and suspension or debarment from government contracting. The Securities and Exchange Commission also may suspend or bar issuers from trading securities on U.S. exchanges for violations of the FCPA’s accounting provisions. Although we expect to implement policies and procedures designed to comply with these laws and policies, there can be no assurance that our employees, contractors and agents will comply with these laws and policies. If we are unable to successfully manage the challenges of international expansion and operations, our business and operating results could be harmed.
93
Risks Related to Our Intellectual Property
Our rights to develop and commercialize our product candidates are subject to, in part, the terms and conditions of licenses granted to us by others.
We are reliant upon licenses to certain patent rights and proprietary technology from third parties that are important or necessary to the development of our technology and products, including technology related to our manufacturing process and our product candidates. These and other licenses may not provide exclusive rights to use such intellectual property and technology in all relevant fields of use and in all territories in which we may wish to develop or commercialize our technology and products in the future. As a result, we may not be able to prevent competitors from developing and commercializing competitive products in territories included in all of our licenses. These licenses may also require us to grant back certain rights to licensors and to pay certain amounts relating to sublicensing patent and other rights under the agreement.
In some circumstances, particularly in-licenses with academic institutions, we may not have the right to control the preparation, filing and prosecution of patent applications, or to maintain the patents, covering technology that we license from third parties. Therefore, we cannot be certain that these patents and applications will be prosecuted, maintained and enforced in a manner consistent with the best interests of our business. If our licensors fail to maintain such patents, or lose rights to those patents or patent applications, the rights we have licensed may be reduced or eliminated and our right to develop and commercialize any of our products that are the subject of such licensed rights could be adversely affected. In certain circumstances, we have or may license technology from third parties on a non-exclusive basis. In such instances, other licensees may have the right to enforce our licensed patents in their respective fields, without our oversight or control. Those other licensees may choose to enforce our licensed patents in a way that harms our interest, for example, by advocating for claim interpretations or agreeing on invalidity positions that conflict with our positions or our interest. In addition to the foregoing, the risks associated with patent rights that we license from third parties will also apply to patent rights we may own in the future.
Further, in many of our license agreements we are responsible for bringing any actions against any third party for infringing on the patents we have licensed. Certain of our license agreements also require us to meet development thresholds to maintain the license, including establishing a set timeline for developing and commercializing products and minimum yearly diligence obligations in developing and commercializing the product. Disputes may arise regarding intellectual property subject to a licensing agreement, including:
|
· |
the scope of rights granted under the license agreement and other interpretation‑related issues; |
|
· |
the extent to which our technology and processes infringe on intellectual property of the licensor that is not subject to the licensing agreement; |
|
· |
the sublicensing of patent and other rights under our collaborative development relationships; |
|
· |
our diligence obligations under the license agreement and what activities satisfy those diligence obligations; |
|
· |
the inventorship or ownership of inventions and know‑how resulting from the joint creation or use of intellectual property by our licensors and us and our partners; and |
|
· |
the priority of invention of patented technology. |
If disputes over intellectual property that we have licensed prevent or impair our ability to maintain our current licensing arrangements on acceptable terms, we may be unable to successfully develop and commercialize the affected product candidates.
94
If we fail to comply with our obligations under these license agreements, or we are subject to a bankruptcy, the licensor may have the right to terminate the license, in which event we would not be able to develop, manufacture, or market products covered by the license or may face other penalties under the agreements. Termination of these agreements or reduction or elimination of our rights under these agreements may result in our having to negotiate new or reinstated agreements with less favorable terms, or cause us to lose our rights under these agreements, including our rights to important intellectual property or technology.
Furthermore, the research resulting in certain of our licensed patent rights and technology was funded by the U.S. government. As a result, the government may have certain rights, or march‑in rights, to such patent rights and technology. When new technologies are developed with U.S. government funding, the U.S. government generally obtains certain rights in any resulting patents, including a non‑exclusive, royalty-free license authorizing the U.S. government, or a third party on its behalf, to use the invention for non‑commercial purposes. These rights may permit the government to disclose our confidential information to third parties and to exercise march‑in rights to use or allow third parties to use our licensed technology. The U.S. government can exercise its march‑in rights if it determines that action is necessary because we fail to achieve practical application of the government‑funded technology, because action is necessary to alleviate health or safety needs, to meet requirements of federal regulations or to give preference to U.S. industry. In addition, our rights in such inventions may be subject to certain requirements to manufacture products embodying such inventions in the United States. Any exercise by the government, or a third party on its behalf, of such rights could harm our competitive position, business, financial condition, results of operations and prospects.
If we are unable to obtain and maintain patent protection for our products and technology, or if the scope of the patent protection obtained is not sufficiently broad, our competitors could develop and commercialize products and technology similar or identical to ours, and our ability to successfully commercialize our products and technology may be adversely affected.
Our success depends, in large part, on our and our licensors’ ability to obtain and maintain patent protection in the United States and other countries with respect to our proprietary product candidates and manufacturing technology. We and our licensors have sought and we intend to seek in the future, to protect our proprietary position by filing patent applications in the United States and abroad related to many of our novel technologies and product candidates that are important to our business.
The patent prosecution process is expensive, time‑consuming and complex, and we may not have and may not in the future be able to file, prosecute, maintain, enforce or license all necessary or desirable patent applications at a reasonable cost or in a timely manner. For example, in some cases, the work of certain academic researchers in the gene therapy field has entered the public domain, which may compromise our ability to obtain patent protection for certain inventions related to or building upon such prior work. Consequently, we will not be able to obtain any such patents to prevent others from using our technology for, and developing and marketing competing products to treat, these indications. It is also possible that we will fail to identify patentable aspects of our research and development output before it is too late to obtain patent protection.
The patent position of biotechnology and pharmaceutical companies generally is highly uncertain, involves complex legal and factual questions and has, in recent years, been the subject of much litigation. As a result, the issuance, scope, validity, enforceability and commercial value of our and our licensors’ patent rights are highly uncertain. Our pending and future patent applications may not result in patents being issued which protect our technology or product candidates or which effectively prevent others from commercializing competitive technologies and product candidates. In particular, during prosecution of any patent application, the issuance of any patents based on the application may depend upon our ability to generate additional preclinical or clinical data that support the patentability of our proposed claims. We may not be able to generate sufficient additional data on a timely basis, or at all. Changes in either the patent laws or interpretation of the patent laws in the United States and other countries may diminish the value of our patents or narrow the scope of our and our licensors’ patent protection.
We may not be aware of all third‑party intellectual property rights potentially relating to our product candidates. Publications of discoveries in the scientific literature often lag the actual discoveries, and patent applications in the United States and other jurisdictions are typically not published until 18 months after filing or, in some cases, not at all.
95
Therefore, we cannot be certain that we were the first to make the inventions claimed in any owned or any licensed patents or pending patent applications, or that we were the first to file for patent protection of such inventions. Databases for patents and publications, and methods for searching them, are inherently limited, so it is not practical to review and know the full scope of all issued and pending patent applications. As a result, the issuance, scope, validity, enforceability, and commercial value of our and our licensed patent rights are uncertain.
Even if the patent applications we license or may own in the future do issue as patents, they may not issue in a form that will provide us with any meaningful protection, prevent competitors or other third parties from competing with us or otherwise provide us with any competitive advantage. Our competitors or other third parties may be able to circumvent our patents by developing similar or alternative technologies or products in a non‑infringing manner.
The issuance of a patent is not conclusive as to its inventorship, scope, validity or enforceability, and our patents may be challenged in the courts or patent offices in the United States and abroad. Such challenges may result in loss of exclusivity or in patent claims being narrowed, invalidated or held unenforceable, which could limit our ability to stop others from using or commercializing similar or identical technology and products, or limit the duration of the patent protection of our technology and product candidates. Given the amount of time required for the development, testing and regulatory review of new product candidates, patents protecting such candidates might expire before or shortly after such candidates are commercialized. As a result, our intellectual property may not provide us with sufficient rights to exclude others from commercializing products similar or identical to ours.
Our intellectual property licenses with third parties may be subject to disagreements over contract interpretation, which could narrow the scope of our rights to the relevant intellectual property or technology or increase our financial or other obligations to our licensors.
The agreements under which we currently license intellectual property or technology from third parties are complex, and certain provisions in such agreements may be susceptible to multiple interpretations. The resolution of any contract interpretation disagreement that may arise could narrow what we believe to be the scope of our rights to the relevant intellectual property or technology, or increase what we believe to be our financial or other obligations under the relevant agreement, either of which could harm our business, financial condition, results of operations and prospects.
We may not be successful in obtaining necessary rights to our product candidates through acquisitions and in‑licenses.
We currently have rights to certain intellectual property, through licenses from third parties, to develop our product candidates. Because our programs may require the use of proprietary rights held by third parties, the growth of our business likely will depend, in part, on our ability to acquire, in‑license or use these proprietary rights. We may be unable to acquire or in‑license any compositions, methods of use, processes or other intellectual property rights from third parties that we identify as necessary for our product candidates. The licensing or acquisition of third‑party intellectual property rights is a competitive area, and several more established companies may pursue strategies to license or acquire third‑party intellectual property rights that we may consider attractive. These established companies may have a competitive advantage over us due to their size, capital resources and greater clinical development and commercialization capabilities. In addition, companies that perceive us to be a competitor may be unwilling to assign or license rights to us. We also may be unable to license or acquire third‑party intellectual property rights on terms that would allow us to make an appropriate return on our investment.
We sometimes collaborate with non‑profit and academic institutions to accelerate our preclinical research or development under written agreements with these institutions. Typically, these institutions provide us with an option to negotiate a license to any of the institution’s rights in technology resulting from the collaboration. Regardless of such option, we may be unable to negotiate a license within the specified timeframe or under terms that are acceptable to us. If we are unable to do so, the institution may offer the intellectual property rights to other parties, potentially blocking our ability to develop our program.
If we are unable to successfully obtain rights to required third‑party intellectual property rights or maintain the existing intellectual property rights we have, we may be required to expend significant time and resources to redesign
96
our product candidates or the methods for manufacturing them or to develop or license replacement technology, all of which may not be feasible on a technical or commercial basis. If we are unable to do so, we may be unable to develop or commercialize the affected product candidates, which could harm our business significantly.
Obtaining and maintaining our patent protection depends on compliance with various procedural, document submission, fee payment and other requirements imposed by government patent agencies, and our patent protection could be reduced or eliminated for non‑compliance with these requirements.
Periodic maintenance fees, renewal fees, annuity fees and various other government fees on patents and/or applications will be due to be paid to the United States Patent and Trademark Office, or USPTO, and various government patent agencies outside of the United States over the lifetime of our licensed patents and/or applications and any patent rights we may own in the future. We rely on our outside counsel or our licensing partners to pay these fees due to non‑U.S. patent agencies. The USPTO and various non‑U.S. government patent agencies require compliance with several procedural, documentary, fee payment and other similar provisions during the patent application process. We employ reputable law firms and other professionals to help us comply and we are also dependent on our licensors to take the necessary action to comply with these requirements with respect to our licensed intellectual property. In many cases, an inadvertent lapse can be cured by payment of a late fee or by other means in accordance with the applicable rules. There are situations, however, in which non‑compliance can result in abandonment or lapse of the patent or patent application, resulting in partial or complete loss of patent rights in the relevant jurisdiction. In such an event, potential competitors might be able to enter the market and this circumstance could harm our business.
We may not be able to protect our intellectual property rights throughout the world.
Filing, prosecuting and defending patents on product candidates in all countries throughout the world would be prohibitively expensive, and our intellectual property rights in some countries outside the United States could be less extensive than those in the United States. In addition, the laws of some foreign countries do not protect intellectual property rights to the same extent as federal and state laws in the United States. Consequently, we may not be able to prevent third parties from practicing our inventions in all countries outside the United States, or from selling or importing products made using our inventions in and into the United States or other jurisdictions. Competitors may use our technologies in jurisdictions where we have not obtained patent protection to develop their own products and, further, may export otherwise infringing products to territories where we have patent protection, but enforcement is not as strong as that in the United States. These products may compete with our products and our patents or other intellectual property rights may not be effective or sufficient to prevent them from competing.
Many companies have encountered significant problems in protecting and defending intellectual property rights in foreign jurisdictions. The legal systems of certain countries, particularly certain developing countries, do not favor the enforcement of patents, trade secrets and other intellectual property protection, particularly those relating to biotechnology products, which could make it difficult for us to stop the infringement of our patents or marketing of competing products in violation of our proprietary rights generally. For example, an April 2014 report from the Office of the United States Trade Representative identified a number of countries, including India and China, where challenges to the procurement and enforcement of patent rights have been reported. Several countries, including India and China, have been listed in the report every year since 1989. Proceedings to enforce our patent rights in foreign jurisdictions could result in substantial costs and divert our efforts and attention from other aspects of our business, could put our patents at risk of being invalidated or interpreted narrowly and our patent applications at risk of not issuing and could provoke third parties to assert claims against us. We may not prevail in any lawsuits that we initiate and the damages or other remedies awarded, if any, may not be commercially meaningful. Accordingly, our efforts to enforce our intellectual property rights around the world may be inadequate to obtain a significant commercial advantage from the intellectual property that we develop or license.
Issued patents covering our product candidates could be found invalid or unenforceable if challenged in court. We may not be able to protect our trade secrets in court.
If one of our licensing partners or we initiate legal proceedings against a third party to enforce a patent covering one of our product candidates, the defendant could counterclaim that the patent covering our product candidate is invalid
97
or unenforceable. In patent litigation in the United States, defendant counterclaims alleging invalidity or unenforceability are commonplace. Grounds for a validity challenge could be an alleged failure to meet any of several statutory requirements, including lack of novelty, obviousness, lack of written description or non‑enablement. Grounds for an unenforceability assertion could be an allegation that someone connected with prosecution of the patent withheld information material to patentability from the USPTO, or made a misleading statement, during prosecution. Third parties also may raise similar claims before administrative bodies in the United States or abroad, even outside the context of litigation. Such mechanisms include re‑examination, post grant review, inter partes review and equivalent proceedings in foreign jurisdictions. Such proceedings could result in the revocation or cancellation of or amendment to our patents in such a way that they no longer cover our product candidates. The outcome following legal assertions of invalidity and unenforceability is unpredictable. With respect to the validity question, for example, we cannot be certain that there is no invalidating prior art, of which the patent examiner and we or our licensing partners were unaware during prosecution. If a defendant were to prevail on a legal assertion of invalidity or unenforceability, we could lose at least part, and perhaps all, of the patent protection on one or more of our product candidates. Such a loss of patent protection could harm our business.
In addition to the protection afforded by patents, we rely on trade secret protection and confidentiality agreements to protect proprietary know‑how that is not patentable or that we elect not to patent, processes for which patents are difficult to enforce and any other elements of our product candidate discovery and development processes that involve proprietary know‑how, information or technology that is not covered by patents. However, trade secrets can be difficult to protect. Some courts inside and outside the United States are less willing or unwilling to protect trade secrets. We seek to protect our proprietary technology and processes, in part, by entering into confidentiality agreements with our employees, consultants, scientific advisors, collaborators, contractors, and other third-parties. We cannot guarantee that we have entered into such agreements with each party that may have or have had access to our trade secrets or proprietary technology and processes. We also seek to preserve the integrity and confidentiality of our data and trade secrets by maintaining physical security of our premises and physical and electronic security of our information technology systems. While we have confidence in these individuals, organizations and systems, agreements or security measures may be breached, and we may not have adequate remedies for any breach. In addition, our trade secrets may otherwise become known or be independently discovered by competitors.
Third parties may initiate legal proceedings alleging that we are infringing their intellectual property rights, the outcome of which would be uncertain and could harm our business.
Our commercial success depends upon our ability and the ability of our collaborators to develop, manufacture, market and sell our product candidates and use our proprietary technologies without infringing the proprietary rights and intellectual property of third parties. The biotechnology and pharmaceutical industries are characterized by extensive and complex litigation regarding patents and other intellectual property rights. We may become party to, or threatened with, infringement litigation claims regarding our products and technology, including claims from competitors or from non-practicing entities that have no relevant product revenue and against whom our own patent portfolio may have no deterrent effect. Moreover, we may become party to, or be threatened with, adversarial proceedings or litigation regarding intellectual property rights with respect to our product candidates and technology, including interference proceedings, post grant review and inter partes review before the USPTO or foreign patent offices. Third parties may assert infringement claims against us based on existing patents or patents that may be granted in the future, regardless of their merit. There is a risk that third parties may choose to engage in litigation with us to enforce or to otherwise assert their patent rights against us. Even if we believe such claims are without merit, a court of competent jurisdiction could hold that these third‑party patents are valid, enforceable and infringed, which could adversely affect our ability to commercialize our product candidates or any other of our product candidates or technologies covered by the asserted third‑party patents. In order to successfully challenge the validity of any such U.S. patent in federal court, we would need to overcome a presumption of validity. As this burden is a high one requiring us to present clear and convincing evidence as to the invalidity of any such U.S. patent claim, there is no assurance that a court of competent jurisdiction would invalidate the claims of any such U.S. patent. Similar challenges exist in other jurisdictions. If we are found to infringe a third-party’s valid and enforceable intellectual property rights, we could be required to obtain a license from such third-party to continue developing, manufacturing and marketing our product candidates and technology. However, we may not be able to obtain any required license on commercially reasonable terms or at all. Even if we were able to obtain a license, it could be non‑exclusive, thereby giving our competitors and other third parties access to the same technologies
98
licensed to us, and it could require us to make substantial licensing and royalty payments. We could be forced, including by court order, to cease developing, manufacturing and commercializing the infringing technology or product candidates. In addition, we could be found liable for monetary damages, including treble damages and attorneys’ fees, if we are found to have willfully infringed a patent or other intellectual property right. A finding of infringement could prevent us from manufacturing and commercializing our product candidates or force us to cease some of our business operations, which could harm our business. In addition, we may be forced to redesign our product candidates, seek new regulatory approvals, and indemnify third parties pursuant to contractual agreements. Claims that we have misappropriated the confidential information or trade secrets of third parties could have a similar negative impact on our business, reputation, financial condition, results of operations and prospects.
Intellectual property litigation could cause us to spend substantial resources and distract our personnel from their normal responsibilities.
Competitors may infringe our intellectual property rights or the intellectual property rights of our licensing partners, or we may be required to defend against claims of infringement. To counter infringement or unauthorized use claims or to defend against claims of infringement can be expensive and time consuming. Even if resolved in our favor, litigation or other legal proceedings relating to intellectual property claims may cause us to incur significant expenses, and could distract our technical and management personnel from their normal responsibilities. In addition, there could be public announcements of the results of hearings, motions or other interim proceedings or developments and if securities analysts or investors perceive these results to be negative, it could have a substantial adverse effect on the price of our common stock. Such litigation or proceedings could substantially increase our operating losses and reduce the resources available for development activities or any future sales, marketing or distribution activities. We may not have sufficient financial or other resources to conduct such litigation or proceedings adequately. Some of our competitors may be able to sustain the costs of such litigation or proceedings more effectively than we can because of their greater financial resources and more mature and developed intellectual property portfolios. Uncertainties resulting from the initiation and continuation of patent litigation or other proceedings could adversely affect our ability to compete in the marketplace.
We may be subject to claims asserting that our employees, consultants or advisors have wrongfully used or disclosed alleged trade secrets of their current or former employers or claims asserting ownership of what we regard as our own intellectual property.
Many of our employees, consultants or advisors are currently, or were previously, employed at universities or other biotechnology or pharmaceutical companies, including our competitors or potential competitors. Although we try to ensure that our employees, consultants and advisors do not use the proprietary information or know‑how of others in their work for us, we may be subject to claims that these individuals or we have used or disclosed intellectual property, including trade secrets or other proprietary information, of any such individual’s current or former employer. Litigation may be necessary to defend against these claims. If we fail in defending any such claims, in addition to paying monetary damages, we may lose valuable intellectual property rights or personnel. Even if we are successful in defending against such claims, litigation could result in substantial costs and be a distraction to management.
In addition, while it is our policy to require our employees and contractors who may be involved in the conception or development of intellectual property to execute agreements assigning such intellectual property to us, we may be unsuccessful in executing such an agreement with each party who, in fact, conceives or develops intellectual property that we regard as our own. The assignment of intellectual property rights may not be self‑executing or the assignment agreements may be breached, and we may be forced to bring claims against third parties, or defend claims that they may bring against us, to determine the ownership of what we regard as our intellectual property.
If we fail in prosecuting or defending any such claims, in addition to paying monetary damages, we may lose valuable intellectual property rights or personnel. Even if we are successful in prosecuting or defending against such claims, litigation could result in substantial costs and be a distraction to management.
99
Changes in U.S. patent law could diminish the value of patents in general, thereby impairing our ability to protect our products.
Recent patent reform legislation could increase the uncertainties and costs surrounding the prosecution of patent applications and the enforcement or defense of issued patents. On September 16, 2011, the Leahy‑Smith America Invents Act, or the Leahy‑Smith Act, was signed into law. The Leahy‑Smith Act includes several significant changes to U.S. patent law. These include provisions that affect the way patent applications are prosecuted and also may affect patent litigation. These also include provisions that switched the United States from a “first‑to‑invent” system to a “first‑to‑file” system, allow third‑party submission of prior art to the USPTO during patent prosecution and set forth additional procedures to attack the validity of a patent by the USPTO administered post grant proceedings. Under a first‑to‑file system, assuming the other requirements for patentability are met, the first inventor to file a patent application generally will be entitled to the patent on an invention regardless of whether another inventor had made the invention earlier. The USPTO recently developed new regulations and procedures to govern administration of the Leahy‑Smith Act, and many of the substantive changes to patent law associated with the Leahy‑Smith Act, and in particular, the first to file provisions, only became effective on March 16, 2013. Accordingly, it is not clear what, if any, impact the Leahy‑Smith Act will have on the operation of our business. However, the Leahy‑Smith Act and its implementation could increase the uncertainties and costs surrounding the prosecution of our patent applications and the enforcement or defense of our issued patents, all of which could harm our business, financial condition, results of operations and prospects.
For example, the Leahy-Smith Act provides a new administrative tribunal known as the Patent Trial and Appeals Board, or PTAB, that provides a venue for companies to challenge the validity of competitor patents at a cost that is much lower than district court litigation and on timelines that are much faster. Although it is not clear what, if any, long-term impacts the PTAB proceedings will have on the operation of our business, the initial results of patent challenge proceedings before the PTAB since its inception in 2013 have resulted in the invalidation of many U.S. patent claims. The availability of the PTAB as a lower-cost, faster and potentially more potent tribunal for challenging patents could therefore increase the likelihood that our own licensed patents will be challenged, thereby increasing the uncertainties and costs of maintaining and enforcing them. Moreover, if such challenges occur, we may not have the right to control the defense. In certain situations, we may be required to rely on our licensor to consider our suggestions and to defend such challenges, with the possibility that it may not do so in a way that best protects our interests.
We also may be subject to a third-party preissuance submission of prior art to the USPTO, or become involved in other contested proceedings such as opposition, derivation, reexamination, inter partes review, post-grant review or interference proceedings challenging our patent rights or the patent rights of others. An adverse determination in any such submission, proceeding or litigation could reduce the scope of, or invalidate, our patent rights, allow third parties to commercialize our technology or products and compete directly with us, without payment to us, or result in our inability to manufacture or commercialize products without infringing third-party patent rights. In addition, if the breadth or strength of protection provided by our patents and patent applications is threatened, it could dissuade companies from collaborating with us to license, develop or commercialize current or future products.
The patent positions of companies engaged in the development and commercialization of biologics and pharmaceuticals are particularly uncertain. Two cases involving diagnostic method claims and “gene patents” have recently been decided by the Supreme Court of the United States, or Supreme Court. On March 20, 2012, the Supreme Court issued a decision in Mayo Collaborative Services v. Prometheus Laboratories, Inc., or Prometheus, a case involving patent claims directed to a process of measuring a metabolic product in a patient to optimize a drug dosage for the patient. According to the Supreme Court, the addition of well‑understood, routine or conventional activity such as “administering” or “determining” steps was not enough to transform an otherwise patent‑ineligible natural phenomenon into patent‑eligible subject matter. On July 3, 2012, the USPTO issued a guidance memo to patent examiners indicating that process claims directed to a law of nature, a natural phenomenon or a naturally occurring relation or correlation that do not include additional elements or steps that integrate the natural principle into the claimed invention such that the natural principle is practically applied and the claim amounts to significantly more than the natural principle itself should be rejected as directed to not patent‑eligible subject matter. On June 13, 2013, the Supreme Court issued its decision in Association for Molecular Pathology v. Myriad Genetics, Inc., or Myriad, a case involving patent claims held by Myriad Genetics, Inc. relating to the breast cancer susceptibility genes BRCA1 and BRCA2. In Myriad, the Supreme Court held
100
that an isolated segment of naturally occurring DNA, such as the DNA constituting the BRCA1 and BRCA2 genes, is not patent eligible subject matter, but that complementary DNA, which is an artificial construct that may be created from RNA transcripts of genes, may be patent eligible.
On March 4, 2014, the USPTO issued a guidance memorandum to patent examiners titled 2014 Procedure for Subject Matter Eligibility Analysis of Claims Reciting or Involving Laws of Nature/Natural Principles, Natural Phenomena, and/or Natural Products. These guidelines and more recent guidelines superseding them instruct USPTO examiners on the ramifications of the Prometheus and Myriad rulings and apply the Myriad ruling to natural products and principles including all naturally occurring nucleic acids. Patents for certain of our product candidates contain claims related to specific DNA sequences that are naturally occurring and, therefore, could be the subject of future challenges made by third parties. In addition, the recent USPTO guidance could make it impossible for us to pursue similar patent claims in patent applications we may prosecute in the future.
We cannot assure you that our efforts to seek patent protection for our technology and products will not be negatively impacted by the decisions described above, rulings in other cases or changes in guidance or procedures issued by the USPTO. We cannot fully predict what impact the Supreme Court’s decisions in Prometheus and Myriad may have on the ability of life science companies to obtain or enforce patents relating to their products and technologies in the future. These decisions, the guidance issued by the USPTO and rulings in other cases or changes in USPTO guidance or procedures could have an adverse effect on our existing patent portfolio and our ability to protect and enforce our intellectual property in the future.
Moreover, although the Supreme Court has held in Myriad that isolated segments of naturally occurring DNA are not patent‑eligible subject matter, certain third parties could allege that activities that we may undertake infringe other gene‑related patent claims, and we may deem it necessary to defend ourselves against these claims by asserting non‑infringement and/or invalidity positions, or paying to obtain a license to these claims. In any of the foregoing or in other situations involving third‑party intellectual property rights, if we are unsuccessful in defending against claims of patent infringement, we could be forced to pay damages or be subjected to an injunction that would prevent us from utilizing the patented subject matter. Such outcomes could harm our business, financial condition, results of operations or prospects.
Outside the United States, other courts have also begun to address the patenting of genetic material. In August 2015, the Australian High Court ruled that isolated genes cannot be patented in Australia. The decision did not address methods of using genetic material. Any ruling of a similar scope in other countries could affect the scope of our intellectual property rights.
If we do not obtain patent term extension and data exclusivity for our product candidates, our business may be harmed.
Depending upon the timing, duration and specifics of any FDA marketing approval of our product candidates, one or more of our U.S. patents may be eligible for limited patent term extension under the Drug Price Competition and Patent Term Restoration Act of 1984, or Hatch‑Waxman Amendments. The Hatch‑Waxman Amendments permit a patent extension term of up to five years as compensation for patent term lost during the FDA regulatory review process. A patent term extension cannot extend the remaining term of a patent beyond a total of 14 years from the date of product approval, only one patent may be extended per FDA-approved product, and only those claims covering the approved drug, a method for using it or a method for manufacturing it may be extended. Further, certain of our licenses currently or in the future may not provide us with the right to control decisions the licensor or its other licensees on Orange Book listings or patent term extension decisions under the Hatch-Waxman Act. Thus, if one of our important licensed patents is eligible for a patent term extension under the Hatch-Waxman Act, and it covers a product of another licensee in addition to our own product candidate, we may not be able to obtain that extension if the other licensee seeks and obtains that extension first. However, we may not be granted an extension because of, for example, failing to exercise due diligence during the testing phase or regulatory review process, failing to apply within applicable deadlines, failing to apply prior to expiration of relevant patents or otherwise failing to satisfy applicable requirements. Moreover, the applicable time-period or the scope of patent protection afforded during any such extension could be less than we request. If we are unable to obtain patent term extension or the scope of term of any such extension is less than we
101
request, the period during which we will have the right to exclusively market our product may be shortened and our competitors may obtain approval of competing products following our patent expiration, and our revenue could be materially reduced.
If our trademarks and trade name are not adequately protected, then we may not be able to build name recognition in our markets of interest and our business may be adversely affected.
We own service mark registrations in the USPTO for the marks “VOYAGER THERAPEUTICS” and “VOYAGER THERAPEUTICS Logo” and pending trademark applications in the USPTO for the marks “VOYAGER TRAJECTORY ARRAY GUIDE”, “V-TAG” and the “V-TAG Logo” as well as pending trademarks applications in the European Community for “VOYAGER TRAJECTORY ARRAY GUIDE” and “V-TAG”. Our trademarks or our trade name may be challenged, infringed, circumvented or declared generic or found to infringe prior third-party marks. We may not be able to protect our rights in our trademarks or in our trade name, which we need in order to build name recognition among potential partners or customers in our markets of interest. It is possible that competitors may adopt trade names or trademarks similar to ours, thereby impeding our ability to build brand identity and possibly leading to market confusion. In addition, there could be potential trade name or trademark infringement claims brought by owners of prior registered trademarks or trademarks that incorporate variations of our registered or unregistered trademarks or trade name. Over the long term, if we are unable to establish name recognition based on our trademarks and trade name, then we may not be able to compete effectively, and our business may be adversely affected. Our efforts to enforce and protect our proprietary rights related to trademarks, trade secrets, domain names, copyrights and other intellectual property may be ineffective and could result in substantial costs and diversion of resources and could adversely impact our financial condition or results of operations.
Intellectual property rights do not necessarily address all potential threats.
The degree of future protection afforded by our intellectual property rights is uncertain because intellectual property rights have limitations, and such rights may not adequately protect our business or permit us to maintain our competitive advantage. For example:
|
· |
others may be able to make gene therapy products that are similar to our product candidates but that are not covered by the claims of the patents that we license or may own in the future; |
|
· |
we, or our license partners or current or future collaborators, might not have been the first to make the inventions covered by the issued patent or pending patent application that we license or may own in the future; |
|
· |
we, or our license partners or current or future collaborators, might not have been the first to file patent applications covering certain of our or their inventions; |
|
· |
others may independently develop similar or alternative technologies or duplicate any of our technologies without infringing our owned or licensed intellectual property rights; |
|
· |
it is possible that our pending patent applications or those that we may own in the future will not lead to issued patents; |
|
· |
issued patents that we hold rights to may be held invalid or unenforceable, including as a result of legal challenges by our competitors; |
|
· |
our competitors might conduct research and development activities in countries where we do not have patent rights and then use the information learned from such activities to develop competitive products for sale in our major commercial markets; |
|
· |
we may not develop additional proprietary technologies that are patentable; |
102
|
· |
the patents of others may have an adverse effect on our business; and |
|
· |
we may choose not to file a patent for certain trade secrets or know‑how, and a third party may subsequently file a patent covering such intellectual property. |
Should any of these events occur, they could significantly harm our business, financial condition, results of operations and prospects.
Our reliance on third parties requires us to share our trade secrets, which increases the possibility that a competitor will discover them or that our trade secrets will be misappropriated or disclosed.
Because we currently rely on certain third parties to manufacture all or part of our product candidates and to perform quality testing, and because we collaborate with various organizations and academic institutions for the advancement of our product engine and pipeline, we must, at times, share our proprietary technology and confidential information, including trade secrets, with them. We seek to protect our proprietary technology, in part, by entering into confidentiality agreements and, if applicable, material transfer agreements, collaborative research agreements, consulting agreements or other similar agreements with our collaborators, advisors, employees and consultants prior to beginning research or disclosing proprietary information. These agreements typically limit the rights of the third parties to use or disclose our confidential information. Despite the contractual provisions employed when working with third parties, the need to share trade secrets and other confidential information increases the risk that such trade secrets become known by our competitors, are inadvertently incorporated into the technology of others or are disclosed or used in violation of these agreements. Given that our proprietary position is based, in part, on our know‑how and trade secrets, a competitor’s discovery of our proprietary technology and confidential information or other unauthorized use or disclosure would impair our competitive position and may harm our business, financial condition, results of operations and prospects.
Despite our efforts to protect our trade secrets, our competitors may discover our trade secrets, either through breach of these agreements, independent development or publication of information including our trade secrets by third parties. A competitor’s discovery of our trade secrets would impair our competitive position and have an adverse impact on our business, financial condition, results of operations and prospects.
Risks Related to Ownership of Our Common Stock
Our executive officers, directors, principal stockholders and their affiliates exercise significant influence over our company.
The holdings of our executive officers, directors, principal stockholders and their affiliates, including investment funds affiliated with Third Rock Ventures and Funds affiliated with Fidelity Management Research Company, or Fidelity, represent beneficial ownership, in the aggregate, of approximately 49% of our outstanding common stock as of December 31, 2017. As a result, these stockholders, if they act together, will be able to influence our management and affairs and the outcome of matters submitted to our stockholders for approval, including the election of directors and any sale, merger, consolidation, or sale of all or substantially all of our assets. In addition, this concentration of ownership might adversely affect the market price of our common stock by:
|
· |
delaying, deferring or preventing a change of control of us; |
|
· |
impeding a merger, consolidation, takeover or other business combination involving us; or |
|
· |
discouraging a potential acquirer from making a tender offer or otherwise attempting to obtain control of us. |
An active trading market for our common stock may not be sustained.
Our shares of common stock began trading on the NASDAQ Global Select Market on November 11, 2015. Given the limited trading history of our common stock, there is a risk that an active trading market for our shares will not be sustained, which could put downward pressure on the market price of our common stock and thereby affect the ability of our stockholders to sell their shares.
103
If securities analysts do not publish research or reports about our business or if they publish negative evaluations of our stock, the price of our stock could decline.
The trading market for our common stock will rely in part on the research and reports that industry or financial analysts publish about us or our business. If no or few analysts maintain coverage of us, the trading price of our stock would likely decrease. If one or more of the analysts covering our business downgrade their evaluations of our stock, the price of our stock could decline. If one or more of these analysts cease to cover our stock, we could lose visibility in the market for our stock, which in turn could cause our stock price to decline.
Sales of a substantial number of shares of our common stock in the public market could cause our stock price to fall.
Persons who were our stockholders prior to our initial public offering continue to hold a substantial number of shares of our common stock. If such persons sell, or indicate an intention to sell, substantial amounts of our common stock in the public market, the trading price of our common stock could decline.
In addition, shares of common stock that are either subject to outstanding options or reserved for future issuance under our stock incentive plans will become eligible for sale in the public market to the extent permitted by the provisions of various vesting schedules and Rule 144 and Rule 701 under the Securities Act of 1933, as amended, and, in any event, we have filed a registration statement permitting shares of common stock issued on exercise of options to be freely sold in the public market. If these additional shares of common stock are sold, or if it is perceived that they will be sold, in the public market, the trading price of our common stock could decline. In addition, we have registered on a registration statement on Form S-3 that has been declared effective, the sale of up to $250.0 million in aggregate of an indeterminate number of shares of common stock and preferred stock, an indeterminate principal amount of debt securities, and an indeterminate number of warrants. In November 2017, under such shelf registration statement, we issued and sold 5,175,000 shares of common stock to the public at an offering price of $12.00 per share, including 675,000 shares of common stock issued upon the full exercise by the underwriter of their option to purchase additional shares, resulting in net proceeds of $58.0 million after deducting underwriting discounts, commissions, and offering expenses payable by us. The registration statement also registers the offering, issuance, and sale of common stock having up to a maximum aggregate offering price of $75.0 million that we may issue and sell in an at-the-market offering under a sales agreement we entered into with Cowen and Company, LLC on December 1, 2016 pursuant to a sales agreement prospectus that forms a part of the registration statement. As of December 31, 2017, approximately $75.0 million in shares of common stock remain eligible for sale under the sales agreement.
Certain holders of our common stock have rights, subject to specified conditions, to require us to file registration statements covering their shares or to include their shares in registration statements that we may file for ourselves or other stockholders. Any sales of securities by these stockholders could have a material adverse effect on the trading price of our common stock.
The price of our common stock may be volatile and fluctuate substantially, which could result in substantial losses for holders of our common stock.
Our stock price may be volatile. The stock market in general and the market for smaller biopharmaceutical companies in particular have experienced extreme volatility that has often been unrelated to the operating performance of particular companies. As a result of this volatility, our stockholders may not be able to sell their common stock at or above the price at which they purchased it. The market price for our common stock may be influenced by many factors, including:
|
· |
our success in commercializing any product candidates for which we obtain marketing approval; |
|
· |
regulatory action and results of clinical trials of our product candidates or those of our competitors; |
|
· |
the success of competitive products or technologies; |
|
· |
the results of clinical trials of our product candidates; |
104
|
· |
the results of clinical trials of product candidates of our competitors; |
|
· |
the commencement, termination, and success of our collaborations; |
|
· |
regulatory or legal developments in the United States and other countries; |
|
· |
developments or disputes concerning patent applications, issued patents or other proprietary rights; |
|
· |
the recruitment or departure of key personnel; |
|
· |
the level of expenses related to any of our product candidates or clinical development programs; |
|
· |
the results of our efforts to discover, develop, acquire or in-license additional product candidates or technologies, the cost of commercializing such product candidates, and the cost of development of any such product candidates or technologies; |
|
· |
actual or anticipated changes in estimates as to financial results, development timelines or recommendations by securities analysts; |
|
· |
variations in our financial results or those of companies that are perceived to be similar to us; |
|
· |
the ability to secure third-party reimbursement for our product candidates; |
|
· |
changes in the structure of healthcare payment systems; |
|
· |
market conditions in the pharmaceutical and biotechnology sectors; |
|
· |
general economic, industry and market conditions; and |
|
· |
the other factors described in this “Risk Factors” section and in those “Risk Factors” sections in documents incorporated herein by reference. |
If our operating results fall below the expectations of investors or securities analysts for a given period, the price of our common stock could decline substantially. Furthermore, any fluctuations in our operating results from period to period may, in turn, cause the price of our stock to fluctuate substantially. We believe that such comparisons of our financial results are not necessarily meaningful and should not be relied upon as an indication of our future performance.
In the past, following periods of volatility in the market price of a company’s securities, securities class-action litigation often has been instituted against that company. We also may face securities class-action litigation if we cannot obtain regulatory approvals for or if we otherwise fail to commercialize our product candidates. Such litigation, if instituted against us, could cause us to incur substantial costs to defend such claims and divert management’s attention and resources, which could seriously harm our business, financial condition, results of operations and prospects.
We have broad discretion in how we use the proceeds from our IPO and other public offerings, and we may not use these proceeds effectively, which could affect our results of operations and cause our stock price to decline.
Our management will have broad discretion in the application of our existing cash, cash equivalents and marketable securities and the net proceeds from this offering and could spend these funds in ways that do not improve our results of operations or enhance the value of our common stock. The failure by our management to apply these funds effectively could result in financial losses that could cause the price of our common stock to decline and delay the development of our product candidates and preclinical programs. Pending their use, we may invest the net proceeds from this offering in a manner that does not produce income or that loses value.
105
We are an “emerging growth company,” and the reduced disclosure requirements applicable to emerging growth companies may make our common stock less attractive to investors.
For so long as we remain an “emerging growth company,” or EGC, as defined in the JOBS Act, we are permitted and intend to rely on exemptions from certain disclosure requirements that are applicable to other public companies that are not EGCs. These exemptions include:
|
· |
not being required to comply with the auditor attestation requirements in the assessment of our internal control over financial reporting pursuant to Section 404 of the Sarbanes‑Oxley Act of 2002; |
|
· |
not being required to comply with any requirement that may be adopted by the Public Company Accounting Oversight Board regarding mandatory audit firm rotation or a supplement to the auditor’s report providing additional information about the audit and the financial statements; |
|
· |
reduced disclosure obligations regarding executive compensation; and |
|
· |
exemptions from the requirements of holding a nonbinding advisory vote on executive compensation and stockholder approval of any golden parachute payments not previously approved. |
We may take advantage of these exemptions until we are no longer an EGC. We would cease to be an EGC upon the earlier of: (i) the last day of the fiscal year in which we have total annual gross revenue of $1.07 billion or more; (ii) the last day of the fiscal year following the fifth anniversary of the date of the completion of our IPO, which is December 31, 2020; (iii) the date on which we have issued more than $1.0 billion in nonconvertible debt during the previous three years; or (iv) the date on which we are deemed to be a large accelerated filer under the rules of the Securities and Exchange Commission or SEC, which means the first day of the year following the first year in which the market value of our common stock that is held by non‑affiliates exceeds $700.0 million as of June 30th.
We expect to continue to take advantage of some, but not all, of the available exemptions. In particular, we have not included all of the executive compensation information that would be required if we were not an EGC. We cannot predict whether investors will find our common stock less attractive if we rely on certain or all of these exemptions.
In addition, the JOBS Act provides that an EGC may take advantage of an extended transition period for complying with new or revised accounting standards. This allows an EGC to delay the adoption of certain accounting standards until those standards would otherwise apply to private companies. We have irrevocably elected not to avail ourselves of this exemption from new or revised accounting standards and, therefore, we will be subject to the same new or revised accounting standards as other public companies that are not emerging growth companies. If some investors find our common stock less attractive as a result, there may be a less active trading market for our common stock and our stock price may be more volatile and may decline.
We will incur increased costs as a result of operating as a public company, and our management will be required to devote substantial time to new compliance initiatives.
As a public company, and particularly after we are no longer an EGC, we will incur significant legal, accounting and other expenses that we did not incur as a private company. In addition, the Sarbanes‑Oxley Act of 2002, the Dodd-Frank Wall Street Form and Consumer Protection Act, and rules subsequently implemented by the SEC and The NASDAQ Stock Market have imposed various requirements on public companies, including establishment and maintenance of effective disclosure and financial controls and corporate governance practices. Our management and other personnel devote a substantial amount of time to these compliance initiatives. Moreover, these rules and regulations have increased our legal and financial compliance costs and have made some activities more time‑consuming and costly. For example, these rules and regulations have made it more difficult and more expensive for us to obtain director and officer liability insurance, and we have been required to accept reduced policy limits and coverage or incur substantially higher costs to obtain the same or similar coverage. As a result, it may be more difficult for us to attract and retain qualified people to serve on our board of directors, our board committees or as executive officers.
106
Pursuant to Section 404 of the Sarbanes‑Oxley Act of 2002, or Section 404, we will be required to furnish a report by our management on our internal control over financial reporting. However, while we remain an EGC, we will not be required to include an attestation report on internal control over financial reporting issued by our independent registered public accounting firm. To achieve compliance with Section 404 within the prescribed period, we will be engaged in a process to document and evaluate our internal control over financial reporting, which is both costly and challenging. In this regard, we will need to continue to dedicate internal resources, potentially engage outside consultants and adopt a detailed work plan to assess and document the adequacy of internal control over financial reporting, continue steps to improve control processes as appropriate, validate through testing that controls are functioning as documented and implement a continuous reporting and improvement process for internal control over financial reporting. Despite our efforts, there is a risk that neither we nor our independent registered public accounting firm will be able to conclude within the prescribed timeframe that our internal control over financial reporting is effective as required by Section 404. If we identify one or more material weaknesses in our internal control over financial reporting, it could result in an adverse reaction in the financial markets due to a loss of confidence in the reliability of our financial statements.
Provisions in our amended and restated certificate of incorporation and bylaws and Delaware law could make an acquisition of us, which may be beneficial to our stockholders, more difficult and may prevent attempts by our stockholders to replace or remove our current management.
Provisions in our amended and restated certificate of incorporation and bylaws may discourage, delay or prevent a merger, acquisition or other change in control of us that stockholders may consider favorable, including transactions in which our stockholders might otherwise receive a premium for their shares. These provisions also could limit the price that investors might be willing to pay in the future for shares of our common stock, thereby depressing the market price of our common stock. In addition, because our board of directors is responsible for appointing the members of our management team, these provisions may frustrate or prevent any attempts by our stockholders to replace or remove our current management by making it more difficult for stockholders to replace members of our board of directors. Among other things, these provisions:
|
· |
establish a classified board of directors such that only one of three classes of members of the board is elected each year; |
|
· |
allow the authorized number of our directors to be changed only by resolution of our board of directors; |
|
· |
limit the manner in which stockholders can remove directors from the board; |
|
· |
establish advance notice requirements for stockholder proposals that can be acted on at stockholder meetings and nominations to our board of directors; |
|
· |
require that stockholder actions must be effected at a duly called stockholder meeting and prohibit actions by our stockholders by written consent; |
|
· |
limit who may call stockholder meetings; |
|
· |
authorize our board of directors to issue preferred stock without stockholder approval, which could be used to institute a stockholder rights plan, or so‑called “poison pill,” that would work to dilute the stock ownership of a potential hostile acquirer, effectively preventing acquisitions that have not been approved by our board of directors; and |
|
· |
require the approval of the holders of at least 75% of the votes that all our stockholders would be entitled to cast to amend or repeal certain provisions of our amended and restated certificate of incorporation or bylaws. |
Moreover, because we are incorporated in Delaware, we are governed by the provisions of Section 203 of the Delaware General Corporation Law, which prohibits a person who owns in excess of 15% of our outstanding voting stock from merging or combining with us for a period of three years after the date of the transaction in which the person
107
acquired in excess of 15% of our outstanding voting stock, unless the merger or combination is approved in a prescribed manner.
Our amended and restated certificate of incorporation designates the Court of Chancery of the State of Delaware as the sole and exclusive forum for certain types of actions and proceedings that may be initiated by our stockholders, which could limit our stockholders’ ability to obtain a favorable judicial forum for disputes with us or our directors, officers or employees.
Our amended and restated certificate of incorporation, provides that, unless we consent in writing to an alternative forum, the Court of Chancery of the State of Delaware will be the sole and exclusive forum for (i) any derivative action or proceeding brought on our behalf, (ii) any action asserting a claim of breach of a fiduciary duty owed by any of our directors, officers and employees to us or our stockholders, (iii) any action asserting a claim arising pursuant to any provision of the Delaware General Corporation Law, our certificate of incorporation or our bylaws or (iv) any action asserting a claim that is governed by the internal affairs doctrine, in each case subject to the Court of Chancery having personal jurisdiction over the indispensable parties named as defendants therein. Any person purchasing or otherwise acquiring any interest in any shares of our capital stock shall be deemed to have notice of and to have consented to this provision of our amended and restated certificate of incorporation. This choice of forum provision may limit a stockholder’s ability to bring a claim in a judicial forum that he, she or it finds favorable for disputes with us or our directors, officers or employees, which may discourage such lawsuits against us and our directors, officers and employees even though an action, if successful, might benefit our stockholders. Stockholders who do bring a claim in the Court of Chancery could face additional litigation costs in pursuing any such claim, particularly if they do not reside in or near the State of Delaware. The Court of Chancery may also reach different judgments or results than would other courts, including courts where a stockholder considering an action may be located or would otherwise choose to bring the action, and such judgments or results may be more favorable to us than to our stockholders. Alternatively, if a court were to find this provision of our amended and restated certificate of incorporation inapplicable to, or unenforceable in respect of, one or more of the specified types of actions or proceedings, we may incur additional costs which could have a material adverse effect on our business, financial condition or results of operations.
Because we do not anticipate paying any cash dividends on our capital stock in the foreseeable future, capital appreciation, if any, will be our stockholders’ sole source of gain.
We have never declared or paid cash dividends on our capital stock. We currently intend to retain all of our future earnings, if any, to finance the growth and development of our business. In addition, the terms of any future debt agreements may preclude us from paying dividends. As a result, capital appreciation, if any, of our common stock will be the sole source of gain for our stockholders for the foreseeable future.
ITEM 1B. UNRESOLVED STAFF COMMENTS
Not applicable.
Our corporate headquarters are located in Cambridge, Massachusetts. Our current leased facilities encompass approximately 45,000 square feet of office and laboratory space, located at 75 Sidney Street and 64 Sidney Street, Cambridge, Massachusetts. In February 2018, we signed an amendment to lease an additional approximately 11,000 square feet in Cambridge, Massachusetts that is intended to support our continued growth. The additional facility includes laboratory and office space, and will be ready for occupancy in the first half of 2018.
In the ordinary course of business, we are from time to time involved in lawsuits, claims, investigations, proceedings, and threats of litigation relating to intellectual property, commercial arrangements and other matters. While the outcome of these proceedings and claims cannot be predicted with certainty, as of December 31, 2017, we were not party to any legal or arbitration proceedings that may have, or have had in the recent past, significant effects on our
108
financial position or profitability. No governmental proceedings are pending or, to our knowledge, contemplated against us. We are not a party to any material proceedings in which any director, member of senior management or affiliate of ours is either a party adverse to us or our subsidiaries or has a material interest adverse to us or our subsidiaries.
ITEM 4. MINE SAFETY DISCLOSURES
Not applicable.
ITEM 5. MARKET FOR REGISTRANT’S COMMON EQUITY, RELATED STOCKHOLDER MATTERS AND ISSUER PURCHASES OF EQUITY SECURITIES.
Our common stock has been traded on the Nasdaq Global Select Market under the symbol “VYGR” since November 11, 2015. Prior to this time, there was no public market for our common stock. The following table shows the high and low sale prices per share of our common stock as reported on the Nasdaq Global Select Market for the periods indicated:
|
|
|
High |
|
Low |
|
||
|
2016 |
|
|
|
|
|
|
|
|
First Quarter |
|
$ |
21.15 |
|
$ |
8.56 |
|
|
Second Quarter |
|
$ |
15.19 |
|
$ |
8.77 |
|
|
Third Quarter |
|
$ |
16.26 |
|
$ |
10.94 |
|
|
Fourth Quarter |
|
$ |
15.02 |
|
$ |
11.01 |
|
|
2017 |
|
|
|
|
|
|
|
|
First Quarter |
|
$ |
14.44 |
|
$ |
10.34 |
|
|
Second Quarter |
|
$ |
13.78 |
|
$ |
8.36 |
|
|
Third Quarter |
|
$ |
22.28 |
|
$ |
8.10 |
|
|
Fourth Quarter |
|
$ |
25.99 |
|
$ |
11.54 |
|
On March 9, 2018, the last reported sale price for our common stock on the Nasdaq Global Select Market was $26.89 per share.
Stock Performance Graph
The graph set forth below compares the cumulative total stockholder return on our common stock between November 11, 2015 and December 31, 2017, with the cumulative total return of (a) the Nasdaq Composite Index and (b) the Nasdaq Biotechnology Index, over the same period. This graph assumes the investment of $100 on November 11, 2015 in our common stock, the Nasdaq Composite Index, and the Nasdaq Biotechnology Index and assumes the reinvestment of dividends, if any. The graph assumes our closing sales price on November 11, 2015 of $17.75 per share as the initial value of our common stock and not the initial offering price to the public of $14.00 per share.
The comparisons shown in the graph below are based upon historical data. We caution that the stock price performance shown in the graph below is not necessarily indicative of, nor is it intended to forecast, the potential future performance of our common stock. Information used in the graph was obtained from the Nasdaq Stock Market LLC, a financial data provider and a source believed to be reliable. The Nasdaq Stock Market LLC is not responsible for any errors or omissions in such information.
109
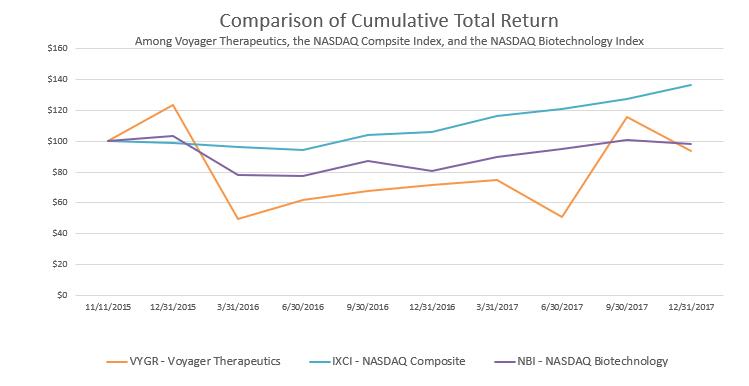
Stockholders
As of March 9, 2018, there were approximately 23 holders of record of our common stock. The actual number of stockholders is greater than this number of record holders, and includes stockholders who are beneficial owners, but whose shares are held in street name by brokers and other nominees. This number of holders of record also does not include stockholders whose shares may be held in trust by other entities.
Dividends
We have not paid any cash dividends on our common stock since inception and do not anticipate paying cash dividends in the foreseeable future.
Securities authorized for issuance under equity compensation plans
Information about our equity compensation plans is incorporated herein by reference to Item 12 of Part III of this Annual Report on Form 10-K.
Unregistered Sales of Equity Securities
We had no unregistered sales of securities for the year ended December 31, 2017.
Purchases of Equity Securities by the Issuer or Affiliated Purchasers
There were no repurchases of shares of common stock made during the year ended December 31, 2017.
ITEM 6. SELECTED FINANCIAL DATA
The following financial data should be read in conjunction with “Management’s Discussion and Analysis of Financial Condition and Results of Operations”, the financial statements and related notes, and other financial information included in this Annual Report on Form 10-K.
110
We have derived the statements of operations data for the years ended December 31, 2017, 2016, and 2015, and the balance sheet data as of December 31, 2017 and 2016, from our audited financial statements included elsewhere in this Annual Report on Form 10-K. We have derived the statements of operations data for the year ended December 31, 2014 and the period ended December 31, 2013, and the balance sheet data as of December 31, 2015, 2014, and 2013, from our audited consolidated financial statements not included in this Annual Report on Form 10-K. Historical results are not necessarily indicative of the results to be expected in future periods.
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Period from |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
June 19, 2013 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
(Inception) to |
|
|
|
|
|
Year ended December 31, |
|
December 31, |
|
|||||||||||
|
|
|
2017 |
|
2016 |
|
2015 |
|
2014 |
|
2013 |
|
|||||
|
|
|
(amounts in thousands, except share and per share data) |
|
|||||||||||||
|
Consolidated statements of operations data: |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Collaboration revenue |
|
$ |
10,135 |
|
$ |
14,220 |
|
$ |
17,334 |
|
$ |
— |
|
$ |
— |
|
|
Operating expenses: |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Research and development |
|
|
62,260 |
|
|
42,249 |
|
|
27,679 |
|
|
8,898 |
|
|
2,316 |
|
|
General and administrative |
|
|
19,738 |
|
|
13,270 |
|
|
9,909 |
|
|
5,469 |
|
|
1,450 |
|
|
Total operating expenses |
|
|
81,998 |
|
|
55,519 |
|
|
37,588 |
|
|
14,367 |
|
|
3,766 |
|
|
Loss from operations |
|
|
(71,863) |
|
|
(41,299) |
|
|
(20,254) |
|
|
(14,367) |
|
|
(3,766) |
|
|
Interest income (expense), net |
|
|
1,227 |
|
|
976 |
|
|
332 |
|
|
(1) |
|
|
(67) |
|
|
Other (expense) income, net |
|
|
(62) |
|
|
182 |
|
|
(9,750) |
|
|
(1,949) |
|
|
— |
|
|
Loss before income taxes |
|
|
(70,698) |
|
|
(40,141) |
|
|
(29,672) |
|
|
(16,317) |
|
|
(3,833) |
|
|
Income tax provision |
|
|
— |
|
|
52 |
|
|
— |
|
|
— |
|
|
— |
|
|
Net loss |
|
$ |
(70,698) |
|
$ |
(40,193) |
|
$ |
(29,672) |
|
$ |
(16,317) |
|
$ |
(3,833) |
|
|
Other comprehensive loss |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Net unrealized (loss) gain on available-for-sale-securities, net |
|
|
(235) |
|
|
199 |
|
|
(251) |
|
|
— |
|
|
— |
|
|
Comprehensive loss |
|
$ |
(70,933) |
|
$ |
(39,994) |
|
$ |
(29,923) |
|
$ |
(16,317) |
|
$ |
(3,833) |
|
|
Reconciliation of net loss to net loss attributable to common stockholders: |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Net loss |
|
$ |
(70,698) |
|
$ |
(40,193) |
|
$ |
(29,672) |
|
$ |
(16,317) |
|
$ |
(3,833) |
|
|
Accretion of preferred stock to redemption value |
|
|
— |
|
|
— |
|
|
(7,373) |
|
|
(1,366) |
|
|
— |
|
|
Accrued dividends on series A preferred stock |
|
|
— |
|
|
— |
|
|
(1,245) |
|
|
— |
|
|
— |
|
|
Net loss attributable to common stockholders |
|
$ |
(70,698) |
|
$ |
(40,193) |
|
$ |
(38,290) |
|
$ |
(17,683) |
|
$ |
(3,833) |
|
|
Net loss per share attributable to common stockholders—basic and diluted(1) |
|
$ |
(2.64) |
|
$ |
(1.59) |
|
$ |
(9.14) |
|
$ |
(27.83) |
|
$ |
(1,629.68) |
|
|
Weighted average number of common shares used in net loss per share attributable to common stockholders—basic and diluted(1) |
|
|
26,803,711 |
|
|
25,302,414 |
|
|
4,191,210 |
|
|
635,448 |
|
|
2,352 |
|
111
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
As of December 31, |
|
|||||||||||||
|
|
|
2017 |
|
2016 |
|
2015 |
|
2014 |
|
2013 |
|
|||||
|
|
|
(in thousands) |
|
|||||||||||||
|
Consolidated balance sheet data: |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Cash, cash equivalents, and marketable debt securities |
|
$ |
169,052 |
|
$ |
174,418 |
|
$ |
224,345 |
|
$ |
7,035 |
|
$ |
135 |
|
|
Working capital(2) |
|
|
155,893 |
|
|
164,984 |
|
|
171,963 |
|
|
5,884 |
|
|
(3,847) |
|
|
Total assets |
|
|
184,477 |
|
|
189,566 |
|
|
229,457 |
|
|
11,497 |
|
|
149 |
|
|
Redeemable convertible preferred stock |
|
|
— |
|
|
— |
|
|
— |
|
|
21,979 |
|
|
— |
|
|
Common stock and additional paid-in capital |
|
|
295,051 |
|
|
225,989 |
|
|
219,147 |
|
|
1 |
|
|
— |
|
|
Total stockholders’ equity (deficit) |
|
|
134,051 |
|
|
135,922 |
|
|
169,074 |
|
|
(20,830) |
|
|
(3,833) |
|
(1) See Statements of Operations Data and Note 2 to our financial statements for further details on the calculation of net loss per share, basic and diluted, attributable to common stockholders and the weighted-average number of shares used in the computation of the per share amounts.
(2) We define working capital as current assets less current liabilities. See our financial statements for further details regarding our current assets and current liabilities.
ITEM 7. MANAGEMENT’S DISCUSSION AND ANALYSIS OF FINANCIAL CONDITION AND RESULTS OF OPERATIONS
You should read the following discussion and analysis of our financial condition and results of operations together with our consolidated financial statements and related notes appearing elsewhere in this Annual Report on Form 10-K. In addition to historical information, this discussion and analysis contains forward-looking statements that involve risks, uncertainties and assumptions. Our actual results may differ materially from those anticipated in these forward-looking statements as a result of certain factors. We discuss factors that we believe could cause or contribute to these differences below and elsewhere in this report, including those set forth under Item 1A. “Risk Factors” and under “Forward-Looking Statements” in this Annual Report on Form 10-K.
We are a clinical-stage gene therapy company focused on developing life-changing treatments for patients suffering from severe neurological diseases. We focus on neurological diseases where we believe an adeno-associated virus, or AAV, gene therapy approach that either increases or decreases the production of a specific protein can slow or reduce the symptoms experienced by patients, and therefore have a clinically meaningful impact. We have built a product engine, that we believe positions us to be the leading company at the intersection of AAV gene therapy and severe neurological disease. Our product engine enables us to engineer, optimize, manufacture and deliver our AAV-based gene therapies that have the potential to provide durable efficacy following a single administration. Additionally, we are working to identify novel AAV capsids, which are the outer viral protein shells that enclose the genetic material of the virus payload. Our team of experts in the fields of AAV gene therapy and neuroscience first identifies and selects severe neurological diseases that are well-suited for treatment using AAV gene therapy. We then engineer and optimize AAV vectors for delivery of the virus payload to the targeted tissue or cells. Our manufacturing process employs an established system that we believe will enable production of high quality AAV vectors at commercial-scale. Finally, we leverage established routes of administration and advances in dosing techniques to optimize delivery of our AAV gene therapies to target cells that are critical to the disease of interest either directly to discrete regions of the brain, or, more broadly, to the spinal cord region.
Since our inception on June 19, 2013, our operations have focused on organizing and staffing our company, business planning, raising capital, establishing our intellectual property portfolio, determining which neurological indications to pursue, advancing our product including delivery and manufacturing, and conducting preclinical studies and clinical trials. We do not have any product candidates approved for sale and have not generated any revenue from product sales. We have funded our operations primarily through private placements of redeemable convertible preferred stock, public offerings of our common stock, and our collaboration with Sanofi Genzyme, or the Sanofi Genzyme Collaboration, which commenced in February 2015.
On October 29, 2015, in preparation for the IPO, our Board of Directors and stockholders approved a 1-for-4.25 reverse split of our common stock, which became effective on October 29, 2015. All share and per share amounts in our
112
consolidated financial statements and notes have been retroactively adjusted for all periods presented to give effect to this reverse split, including reclassifying an amount equal to the reduction in par value of common stock to additional paid-in capital.
On November 16, 2015, we completed the sale of 5,750,000 shares of common stock in our initial public offering, or IPO, at a price to the public of $14.00 per share, resulting in net proceeds of $72.9 million after deducting underwriting discounts and commissions and offering expenses payable by us. Upon the closing of the IPO, all of the outstanding redeemable convertible preferred stock automatically converted into shares of common stock resulting in our issuance of an additional 17,647,054 shares of common stock on that date.
On November 7, 2017, we completed the sale of 5,175,000 shares of common stock to the public at an offering price of $12.00 per share, including 675,000 shares of common stock issued upon the full exercise by the underwriters of their option to purchase additional shares, resulting in net proceeds of $58.0 million after deducting underwriting discounts, commissions, and offering expenses payable by us.
On February 16, 2018, we entered into an exclusive collaboration and option agreement with AbbVie Biotechnology Ltd, or AbbVie, for the research, development, and commercialization of adeno-associated virus and other virus-based gene therapy products for the treatment of diseases of the central nervous system and other neurodegenerative diseases related to defective or excess aggregation of tau protein in the human brain, including Alzheimer’s disease. Under the terms of the agreement, we received an upfront payment of $69.0 million and may receive future development and regulatory milestone payments and royalties. Under the terms of the collaboration and option agreement, we will perform specified research, preclinical, and Phase 1 development activities regarding vectorized antibodies directed against tau, after which AbbVie may select one or more vectorized antibodies to proceed into IND-enabling studies and clinical development. We will be responsible for the research, IND-enabling, and Phase 1 clinical trial activities and costs. Following the completion of Phase 1 clinical development, AbbVie has an option to license the vectorized tau antibody program and would then lead further clinical development and global commercialization for the product candidates pursuant to the agreement. We have an option to share in the costs of clinical development for higher royalty rates. In addition to the upfront and potential option exercise payments, we are eligible to receive up to $895.0 million in development and regulatory milestones for each vectorized tau antibody compound. We are also eligible to receive tiered, escalating royalties in a range, subject to certain specified exceptions, from a high-single digit to a mid-to-high teen percentage of the global net sales of the vectorized antibodies for tauopathies, including Alzheimer's disease and other neurodegenerative diseases. Under the terms of the agreement, each party will own the entire right, title, and interest in and to all know-how and patent rights first made or invented solely by it or its affiliates or its or their sublicensees in the course of the collaboration, with certain specified exceptions. We have also agreed to grant AbbVie a worldwide license to certain know-how and patent rights developed by us or jointly by the parties arising from the collaboration.
Since inception, we have incurred significant operating losses. Our net losses were $70.7 million, $40.2 million, and $29.7 million for the years ended December 31, 2017, 2016, and 2015, respectively. As of December 31, 2017, we had an accumulated deficit of $160.7 million. We expect to continue to incur significant expenses and operating losses for the foreseeable future. We anticipate that our expenses will increase significantly in connection with our ongoing activities, as we:
|
· |
continue investing in our product engine to optimize vector engineering, manufacturing and dosing and delivery techniques; |
|
· |
continue to advance our clinical candidate, VY-AADC, through the current Phase 1b clinical trial and into a planned pivotal Phase 2-3 clinical program as a treatment for advanced Parkinson’s disease; |
|
· |
initiate additional preclinical studies and clinical trials for, and continue research and development of, our other programs; |
113
|
· |
conduct joint research and development under our strategic collaboration with AbbVie for the research, development, and commercialization of adeno-associated virus, or AAV, and other virus-based gene therapy products for the treatment of diseases of the central nervous system and other neurodegenerative diseases related to defective or excess aggregation of tau protein in the human brain, including Alzheimer’s disease; |
|
· |
continue our process research and development activities, as well as establish our research-grade and commercial manufacturing capabilities; |
|
· |
identify additional neurological diseases for treatment with our AAV gene therapies and develop additional programs or product candidates; |
|
· |
work to identify and optimize novel AAV capsids; |
|
· |
develop and obtain regulatory clearance for devices to deliver our AAV gene therapies; |
|
· |
seek marketing and regulatory approvals for VY-AADC or other product candidates or devices that arise from our programs that successfully complete clinical development; |
|
· |
maintain, expand and protect our intellectual property portfolio; |
|
· |
identify, acquire or in-license other product candidates and technologies; |
|
· |
develop a sales, marketing and distribution infrastructure to commercialize any product candidates for which we may obtain marketing approval; |
|
· |
expand our operational, financial and management systems and personnel, including personnel to support our clinical development, manufacturing and commercialization efforts and our operations as a public company; |
|
· |
increase our product liability and clinical trial insurance coverage as we expand our clinical trials and commercialization efforts; and |
|
· |
continue to operate as a public company. |
Financial Operations Overview
Revenue
To date, we have not generated any revenue from product sales and do not expect to generate any revenue from product sales for the foreseeable future. For the year ended December 31, 2017, we recognized $10.1 million of collaboration revenue from the Sanofi Genzyme Collaboration. For additional information about our revenue recognition policy related to the Sanofi Genzyme Collaboration, see the section titled “—Critical Accounting Policies and Estimates—Revenue.”
For the foreseeable future, we expect substantially all of our revenue will be generated from our collaboration agreements with Sanofi Genzyme and AbbVie, and any other strategic relationships we may enter into. If our development efforts are successful, we may also generate revenue from product sales.
114
Expenses
Research and Development Expenses
Research and development expenses consist primarily of costs incurred for our research activities, including our program discovery efforts, and the development of our programs and product engine, which include:
|
· |
employee‑related expenses including salaries, benefits, and stock‑based compensation expense; |
|
· |
costs of funding research performed by third parties that conduct research and development, preclinical activities, manufacturing and production design on our behalf; |
|
· |
the cost of purchasing lab supplies and non‑capital equipment used in designing, developing and manufacturing preclinical study materials; |
|
· |
consultant fees; |
|
· |
facility costs including rent, depreciation and maintenance expenses; and |
|
· |
fees for maintaining licenses under our third‑party licensing agreements. |
Research and development costs are expensed as incurred. Costs for certain activities, such as manufacturing, preclinical studies, and clinical trials, are generally recognized based on an evaluation of the progress to completion of specific tasks using information and data provided to us by our vendors and collaborators.
At this time, we cannot reasonably estimate or know the nature, timing and estimated costs of the efforts that will be necessary to complete the development of our product candidates. We are also unable to predict when, if ever, material net cash inflows will commence from sales of our product candidates. This is due to the numerous risks and uncertainties associated with developing such product candidates, including the uncertainty of:
|
· |
successful enrollment in and completion of clinical trials; |
|
· |
establishing an appropriate safety profile; |
|
· |
establishing commercial manufacturing capabilities or making arrangements with third‑party manufacturers; |
|
· |
receipt of marketing approvals from applicable regulatory authorities; |
|
· |
commercializing the product candidates, if and when approved, whether alone or in collaboration with others; |
|
· |
obtaining and maintaining patent and trade secret protection and regulatory exclusivity for our product candidates; |
|
· |
continued acceptable safety profiles of the products following approval; and |
|
· |
retention of key research and development personnel. |
A change in the outcome of any of these variables with respect to the development of any of our product candidates would significantly change the costs, timing and viability associated with the development of that product candidate.
115
Research and development activities are central to our business model. We expect research and development costs to increase significantly for the foreseeable future as our development programs progress, including as we continue to support the Phase 1b clinical trial and initiate the pivotal Phase 2-3 clinical trial of VY‑AADC as a treatment for advanced Parkinson’s disease, and move such product candidates into additional clinical trials. There are numerous factors associated with the successful commercialization of any of our product candidates, including future trial design and various regulatory requirements, many of which cannot be determined with accuracy at this time based on our stage of development. Additionally, future commercial and regulatory factors beyond our control will impact our clinical development programs and plans.
General and Administrative Expenses
General and administrative expenses consist primarily of salaries and other related costs, including stock‑based compensation, for personnel in executive, finance, accounting, business development, legal and human resource functions. Other significant costs include corporate facility costs not otherwise included in research and development expenses, legal fees related to patent and corporate matters and fees for accounting and consulting services.
We anticipate that our general and administrative expenses will increase in the future to support continued research and development activities, including the continuation of the Phase 1b clinical trial and pivotal Phase 2-3 clinical trial of VY‑AADC and the initiation of clinical trials for our other product candidates. These increases will likely include increased costs related to the hiring of additional personnel and fees to outside consultants. We also anticipate increased expenses associated with being a public company, including costs for audit, legal, regulatory and tax‑related services, director and officer insurance premiums and investor relations costs.
Other Income (Expense)
Other income (expense) consists primarily of the gain (loss) on the equity securities investment in MRI Interventions.
Other expense during 2015 consists primarily of the re‑measurement losses associated with the change in the fair value of the tranche rights for the Series A Preferred Stock. During the year ended December 31, 2015, $9.8 million of expense was recorded related to the change in fair value of these rights. In February 2015, upon the issuance of the final tranche of Series A Preferred Stock, the tranche right liability was reclassified to Series A Preferred Stock and no further re‑measurement gains or losses was recognized related to these tranche rights.
Critical Accounting Policies and Estimates
Our management’s discussion and analysis of our consolidated financial condition and results of operations are based on our consolidated financial statements, which have been prepared in accordance with U.S. generally accepted accounting principles. The preparation of these consolidated financial statements requires us to make judgments and estimates that affect the reported amounts of assets, liabilities, revenues and expenses and the disclosure of contingent assets and liabilities in our consolidated financial statements. We base our estimates on historical experience, known trends and events, and various other factors that are believed to be reasonable under the circumstances. Actual results may differ from these estimates under different assumptions or conditions. On an ongoing basis, we evaluate our judgments and estimates in light of changes in circumstances, facts and experience. The effects of material revisions in estimates, if any, will be reflected in the financial statements prospectively from the date of change in estimates.
While our significant accounting policies are described in more detail in the notes to our consolidated financial statements appearing elsewhere in this Annual Report on Form 10-K, we believe the following accounting policies used in the preparation of our financial statements require the most significant judgments and estimates.
116
Revenue Recognition – ASC605
As of December 31, 2017, all of our revenue was generated exclusively from the Sanofi Genzyme Collaboration. We recognize revenue in accordance with Financial Accounting Standards Board, or FASB, Accounting Standards Codification, or ASC, Topic 605 Revenue Recognition, or ASC 605. Accordingly, revenue is recognized for each unit of accounting when all of the following criteria are met:
|
· |
persuasive evidence of an arrangement exists; |
|
· |
delivery has occurred or services have been rendered; |
|
· |
the seller’s price to the buyer is fixed or determinable; and |
|
· |
collectability is reasonably assured. |
Amounts received prior to satisfying the revenue recognition criteria are recorded as deferred revenue in our balance sheets. Amounts expected to be recognized as revenue within the 12 months following the balance sheet date are classified as deferred revenue, current portion. Amounts not expected to be recognized as revenue within the 12 months following the balance sheet date are classified as deferred revenue, net of current portion.
Multiple Elements Arrangements
Determination of Accounting Units
We analyze multiple element arrangements based on the guidance in FASB ASC Topic 605-25, Revenue Recognition—Multiple Element Arrangements, or ASC 605-25. Pursuant to the guidance in ASC 605-25, we evaluate multiple element arrangements to determine (1) the deliverables included in the arrangement and (2) whether the individual deliverables represent separate units of accounting or whether they must be accounted for as a combined unit of accounting. This evaluation involves subjective determinations and requires management to make judgments about the individual deliverables and whether such deliverables are separate from other aspects of the contractual relationship. Deliverables are considered separate units of accounting provided that: (i) the delivered item(s) has value to the customer on a standalone basis and (ii) if the arrangement includes a general right of return relative to the delivered item(s), delivery or performance of the undelivered item(s) is considered probable and substantially within our control. In assessing whether an item has standalone value, we consider factors such as the research, manufacturing and commercialization capabilities of the collaboration partner and the availability of the associated expertise in the general marketplace. We also consider whether our collaboration partner can use the other deliverable(s) for their intended purpose without the receipt of the remaining element(s), whether the value of the deliverable is dependent on the undelivered item(s) and whether there are other vendors that can provide the undelivered element(s). The Sanofi Genzyme Collaboration does not provide for a general right of return relative to any delivered items.
Options are considered substantive if, at the inception of the arrangement, we are at risk as to whether the collaboration partner will choose to exercise the option. Factors that we consider in evaluating whether an option is substantive include the cost to exercise the option, the overall objective of the arrangement, the benefit the collaborator might obtain from the arrangement without exercising the option and the likelihood the option will be exercised. When an option is considered substantive, we do not consider the option or item underlying the option to be a deliverable at the inception of the arrangement and the associated option fees are not included in allocable consideration, assuming the option is not priced at a significant and incremental discount. Conversely, when an option is not considered substantive, we would consider the option, including other deliverables contingent upon the exercise of the option, to be a deliverable at the inception of the arrangement and a corresponding amount would be included in allocable arrangement consideration. In addition, if the price of the option includes a significant incremental discount, the option would be included as a deliverable at the inception of the arrangement.
117
Allocation of Arrangement Consideration
Arrangement consideration that is fixed or determinable is allocated among the separate units of accounting using the relative selling price method. The applicable revenue recognition criteria in ASC 605 are applied to each of the separate units of accounting in determining the appropriate period and pattern of recognition. We determine the selling price of a unit of accounting following the hierarchy of evidence prescribed by ASC 605-25. Accordingly, we determine the estimated selling price for units of accounting within each arrangement using vendor specific objective evidence, or VSOE, of selling price, if available, third-party evidence, or TPE, of selling price if VSOE is not available, or best estimate of selling price, or BESP, if neither VSOE or TPE is available. We have only used BESP to estimate the selling price, since we have not had VSOE or TPE of selling price for any units of accounting to date. Determining BESP for a unit of accounting requires significant judgment. In developing the BESP for a unit of accounting, we consider applicable market conditions and relevant entity specific factors, including factors that were contemplated in negotiating the agreement with the customer and estimated costs. We validate BESP for units of accounting by evaluating whether changes in the key assumptions used by us to determine the BESP will have a significant effect on the allocation of arrangement consideration between multiple units of accounting.
Pattern of Recognition
We recognize the arrangement’s consideration allocated to each unit of accounting when all of the revenue recognition criteria in ASC 605 are satisfied for that particular unit of accounting. We will recognize revenue associated with license options upon exercise of the option, if the underlying license has standalone value from the other deliverables to be provided after delivering that license. If the license does not have standalone value, the amounts allocated to the license option will be combined with the related undelivered items as a single unit of accounting. The amounts allocated to the license option in the Sanofi Genzyme Collaboration will be deferred until the option is exercised. The revenue recognition upon option exercise will be determined based on whether the license has standalone value from the remaining deliverables under the arrangement at the time of exercise.
We recognize the amounts associated with research and development services, alliance joint steering committees and development advisory committees ratably over the associated period of performance. If there is no discernible pattern of performance or objectively measurable performance measures do not exist, then we recognize revenue under the arrangement on a straight-line basis over the period that we are expected to complete our performance obligations. Conversely, if the pattern of performance in which the service is provided to the customer can be determined and objectively measurable performance exists, then we recognize revenue under the arrangement using the proportional performance method. Revenue recognized is limited to the lesser of the cumulative amount of payments received or the cumulative revenue earned determined using the straight-line method or proportional performance, as applicable, as of the period end date.
Recognition of Milestones and Royalties
At the inception of an arrangement that includes milestone payments, we evaluate whether each milestone is substantive and at risk to both parties on the basis of the contingent nature of the milestone. This evaluation includes an assessment of whether: (i) the consideration is commensurate with either our performance to achieve the milestone or the enhancement of the value of the delivered item(s) as a result of a specific outcome resulting from our performance to achieve the milestone, (ii) the consideration relates solely to past performance and (iii) the consideration is reasonable relative to all of the deliverables and payment terms within the arrangement. We evaluate factors such as clinical, regulatory, commercial and other risks that must be overcome to achieve the respective milestone and the level of effort and investment required to achieve the respective milestone in making this assessment. There is considerable judgment involved in determining whether a milestone satisfies all of the criteria required to conclude that a milestone is substantive. In accordance with FASB ASC Topic 605-28, Revenue Recognition—Milestone Method, or ASC 605-28, clinical and regulatory milestones that are considered substantive, will be recognized as revenue in their entirety upon successful accomplishment of the milestone, assuming all other revenue recognition criteria are met. Milestones that are not considered substantive would be recognized as revenue over the remaining period of performance, assuming all other
118
revenue recognition criteria are met. Revenue from commercial milestone payments will be accounted for as royalties and recorded as revenue upon achievement of the milestone, assuming all other revenue recognition criteria are met.
We will recognize royalty revenue in the period of sale of the related product(s), based on the underlying contract terms, provided that the reported sales are reliably measurable, we have no remaining performance obligations, and assuming all other revenue recognition criteria are met.
Classifications of Payments to Customers
We also consider the impact of potential future payments we make in our role as a vendor to our customers or collaboration partners and evaluate if these potential future payments could be reductions of revenue from that customer. If the potential future payments to the customer are (i) a separately identifiable benefit and (ii) the fair value of the identifiable benefit can be reasonably estimated, then the payments are accounted for separately from the revenue received from the customer. If however, both of these criteria are not satisfied, then the payments are treated as a reduction of revenue.
Accrued Research and Development Expenses
As part of the process of preparing our financial statements, we are required to estimate our accrued expenses as of each balance sheet date. This process involves reviewing open contracts and purchase orders, communicating with our personnel to identify services that have been performed on our behalf and estimating the level of service performed and the associated cost incurred for the service when we have not yet been invoiced or otherwise notified of the actual cost. The majority of our service providers invoice us monthly in arrears for services performed or when contractual milestones are met. We make estimates of our accrued expenses as of each balance sheet date based on facts and circumstances known to us at that time. We periodically confirm the accuracy of our estimates with the service providers and make adjustments if necessary. The significant estimates in our accrued research and development expenses include the costs incurred for services performed by our vendors in connection with research and development activities for which we have not yet been invoiced.
We record our expenses related to research and development activities on our estimates of the services received and efforts expended pursuant to quotes and contracts with vendors that conduct research and development on our behalf. The financial terms of these agreements are subject to negotiation, vary from contract to contract and may result in uneven payment flows. There may be instances in which payments made to our vendors will exceed the level of services provided and result in a prepayment of the research and development expense. In accruing service fees, we estimate the time period over which services will be performed and the level of effort to be expended in each period. If the actual timing of the performance of services or the level of effort varies from our estimate, we adjust the accrual or prepaid accordingly. Non-refundable advance payments for goods and services that will be used in future research and development activities are expensed when the activity has been performed or when the goods have been received rather than when the payment is made.
Although we do not expect our estimates to be materially different from amounts actually incurred, if our estimates of the status and timing of services performed differ from the actual status and timing of services performed, it could result in us reporting amounts that are too high or too low in any particular period. To date, there have been no material differences between our estimates of such expenses and the amounts actually incurred.
Stock-based Compensation
We account for our stock-based compensation awards in accordance with ASC Topic 718, Compensation—Stock Compensation, or ASC 718. ASC 718 requires all stock-based payments to employees and directors, including grants of restricted stock and stock options, to be recognized as expense in the statements of operations based on their grant date fair values. Grants of restricted stock and stock options to other service providers, referred to as non-employees, are required to be recognized as expense in the statements of operations based on their vesting date fair
119
values. We estimate the fair value of options granted using the Black-Scholes option pricing model. We use the fair value of our common stock to determine the fair value of restricted stock awards.
The Black-Scholes option pricing model requires inputs based on certain subjective assumptions, including (a) the expected stock price volatility, (b) the calculation of expected term of the award, (c) the risk-free interest rate and (d) expected dividends. Due to a lack of company-specific historical and implied volatility data, we have based the estimate of expected volatility on the historical volatility of a group of similar companies that are publicly traded, blended with the most recent period of historic volatility of our common stock. The historical volatility is calculated based on a period of time commensurate with the expected term assumption. The computation of expected volatility is based on the historical volatility of a representative group of companies with similar characteristics to us, including stage of product development and life science industry focus. We use the simplified method as prescribed by the SEC Staff Accounting Bulletin No. 107, Share-Based Payment, to calculate the expected term for options granted to employees and directors as we do not have sufficient historical exercise data to provide a reasonable basis upon which to estimate the expected term. For options granted to non-employees, we utilize the contractual term of the arrangement as the basis for the expected term assumption. The risk-free interest rate is based on a treasury instrument whose term is consistent with the expected term of the stock options. The expected dividend yield is assumed to be zero as we have never paid dividends and do not have current plans to pay any dividends on common stock.
The fair value of each option issued to employees and directors was estimated at the date of grant using the Black‑Scholes option pricing model with the following weighted‑average assumptions:
|
|
|
Year ended December 31, |
|
|||||||
|
|
|
2017 |
|
2016 |
|
2015 |
|
|||
|
Risk-free interest rate |
|
2.0 |
% |
|
1.5 |
% |
|
1.6 |
% |
|
|
Expected dividend yield |
|
— |
% |
|
— |
% |
|
— |
% |
|
|
Expected term (in years) |
|
6.0 |
|
|
6.0 |
|
|
6.0 |
|
|
|
Expected volatility |
|
73.7 |
% |
|
73.1 |
% |
|
78.6 |
% |
|
The fair value of each option issued to non‑employees was estimated at each vesting and reporting date using the Black‑Scholes option pricing model. The reporting date fair value was determined using the following weighted‑average assumptions:
|
|
|
As of December 31, |
|
|||||||
|
|
|
2017 |
|
2016 |
|
2015 |
|
|||
|
Risk-free interest rate |
|
2.4 |
% |
|
2.1 |
% |
|
2.0 |
% |
|
|
Expected dividend yield |
|
— |
% |
|
— |
% |
|
— |
% |
|
|
Expected term (in years) |
|
8.5 |
|
|
9.1 |
|
|
10.0 |
|
|
|
Expected volatility |
|
76.2 |
% |
|
83.3 |
% |
|
84.0 |
% |
|
We expense the fair value of our stock-based compensation awards to employees and directors on a straight-line basis over the associated service period, which is generally the period in which the related services are received. Stock-based compensation awards to non-employees are adjusted through stock-based compensation expense at each reporting period end to reflect the current fair value of such awards and are expensed on a straight-line basis.
We record the expense for stock-based compensation awards subject to performance-based milestone vesting over the remaining service period when management determines that achievement of the milestone is probable. Management evaluates when the achievement of a performance-based milestone is probable based on the expected satisfaction of the performance conditions as of the reporting date. Management concluded that the achievement of the performance milestone for one of the three performance-based awards had been met during 2016. Accordingly, stock-based compensation expense in the amount of $1.4 million and $1.1 million was recorded in the years ended
120
December 31, 2017 and 2016, respectively. No stock-based compensation expense was recorded related to the performance-based awards in the year ended December 31, 2015.
Stock-based compensation totaled approximately $9.1 million, $6.3 million, and $4.0 million the years ended December 31, 2017, 2016, and 2015 respectively. As of December 31, 2017, we had $4.5 million and $16.1 million of unrecognized compensation expense related to restricted stock awards and stock option awards, respectively, which are expected to be recognized over weighted-average remaining vesting periods of approximately 0.38 and 2.66 years, respectively. We expect the impact of our stock-based compensation expense for restricted stock and stock options granted to employees, directors and other service providers to grow in future periods due to the potential increases in the value of our common stock and headcount.
Results of Operations
Comparison of the years ended December 31, 2017 and 2016:
The following table summarizes our results of operations for the years ended December 31, 2017 and 2016, respectively, together with the changes in those items in dollars:
|
|
|
Year ended |
|
|
|
|||||
|
|
|
December 31, |
|
|
|
|||||
|
|
|
2017 |
|
2016 |
|
Change |
|
|||
|
|
|
(in thousands) |
|
|||||||
|
Collaboration revenue |
|
$ |
10,135 |
|
$ |
14,220 |
|
$ |
(4,085) |
|
|
Operating expenses: |
|
|
|
|
|
|
|
|
|
|
|
Research and development |
|
|
62,260 |
|
|
42,249 |
|
|
20,011 |
|
|
General and administrative |
|
|
19,738 |
|
|
13,270 |
|
|
6,468 |
|
|
Total operating expenses |
|
|
81,998 |
|
|
55,519 |
|
|
26,479 |
|
|
Other income: |
|
|
|
|
|
|
|
|
|
|
|
Interest income |
|
|
1,227 |
|
|
976 |
|
|
251 |
|
|
Other (expense) income, net |
|
|
(62) |
|
|
182 |
|
|
(244) |
|
|
Total other income |
|
|
1,165 |
|
|
1,158 |
|
|
7 |
|
|
Loss before income taxes |
|
|
(70,698) |
|
|
(40,141) |
|
|
|
|
|
Income tax provision |
|
|
— |
|
|
52 |
|
|
(52) |
|
|
Net loss |
|
$ |
(70,698) |
|
$ |
(40,193) |
|
$ |
(52) |
|
Collaboration Revenue
Collaboration revenue was $10.1 million for the year ended December 31, 2017, and $14.2 million for the year ended December 31, 2016, all of which related to the Sanofi Genzyme Collaboration. In October 2017, Sanofi Genzyme decided not to exercise its option for the ex-U.S. rights to the Parkinson’s program, (the “PD Option”). Therefore, in the year ended December 31, 2017, we recognized $5.5 million of revenue related to the portion of the upfront consideration which had been allocated to the PD Option. In addition, revenue recognized during the year ended December 31, 2017 and 2016 includes amounts recognized related to consideration allocated to research and development services for various programs under the Sanofi Genzyme collaboration agreement. During 2017 we reassessed the estimated period of performance for each of the units of accounting and determined that the estimated period would be extended for two units of accounting. During 2016 we deprioritized the development of VY-SMN101. These adjustments were made on a prospective basis and resulted in decreases in revenue recognized by $2.1 million and $9.5 million, respectively, for the year ended December 31, 2017.
121
Research and Development Expense
Research and development expense increased by $20.0 million from $42.2 million for the year ended December 31, 2016 to $62.2 million for the year ended December 31, 2017. The following table summarizes our research and development expenses, for years ended December 31, 2017 and 2016:
|
|
|
Year ended |
|
|
|
|||||
|
|
|
December 31, |
|
|
|
|||||
|
|
|
2017 |
|
2016 |
|
Change |
|
|||
|
|
|
(in thousands) |
|
|||||||
|
External research and development expenses |
|
$ |
33,816 |
|
$ |
20,413 |
|
$ |
13,403 |
|
|
Employee and contractor related expenses |
|
|
20,919 |
|
|
15,530 |
|
|
5,389 |
|
|
Facility and other expenses |
|
|
6,705 |
|
|
4,553 |
|
|
2,152 |
|
|
License fees |
|
|
820 |
|
|
1,753 |
|
|
(933) |
|
|
Total research and development expenses |
|
$ |
62,260 |
|
$ |
42,249 |
|
$ |
20,011 |
|
The change in research and development expense for the year ended December 31, 2017 was primarily attributable to the following:
|
· |
approximately $14.5 million for increased costs of funding research performed by third parties that conduct research and development, preclinical and clinical activities, manufacturing and production design on our behalf, increased purchases of lab supplies and non‑capital equipment used in designing, developing and manufacturing preclinical study materials, partially offset by a decrease in expense of approximately $1.1 million attributable to in‑kind research and development services incurred by Sanofi Genzyme and provided to us under the Sanofi Genzyme Collaboration; |
|
· |
approximately $5.4 million for increased research and development employee compensation costs as we continue to increase research and development headcount; |
|
· |
approximately $2.2 million for increased facility and other costs including rent, depreciation, maintenance and other expenses due to the additional space leased at 64 Sidney Street; |
|
· |
offset by approximately $0.9 million related to decreased licensing costs. |
General and Administrative Expense
General and administrative expense increased by $6.5 million from $13.3 million for the year ended December 31, 2016 to $19.7 million for the year ended December 31, 2017. The change in general and administrative expense was primarily attributable to the following:
|
· |
approximately $3.5 million related to compensation costs associated with the increase in administrative function headcount; |
|
· |
approximately $2.1 million for increased legal and patent expenses; and |
|
· |
approximately $0.8 million for increased facility and other costs including rent, depreciation, maintenance and other expenses. |
122
Other Income, Net
Other income of approximately $1.2 million was recognized in the years ended December 31, 2017 and 2016 related to interest income on marketable securities balances offset by losses on our warrants to purchase shares of common stock in MRI Interventions, Inc., or MRIC.
Income Tax
We recorded an income tax provision of $0.2 million related to our alternative minimum tax, or AMT, liability resulting in an income tax payable of $0.1 million for the year ended December 31, 2016. The payable was due to the recognition of deferred revenue related to the Sanofi Genzyme Collaboration for income tax purposes. There was no income tax payable for the year ended December 31, 2017. Our overall income tax provision was offset by an income tax benefit recorded to continuing operations of $0.1 million associated with the recognition of the corresponding income tax associated with unrealized gains included in other comprehensive income. The net tax effect resulted in an overall income tax provision recorded to continuing operations of $0.1 million. We recorded no income tax provision (benefit) for the year ended December 31, 2017.
Comparison of year ended December 31, 2016 and 2015:
The following table summarizes our results of operations for the year ended December 31, 2016 and 2015, respectively, together with the changes in those items in dollars:
|
|
|
Year ended |
|
|
|
|
||||
|
|
|
December 31, |
|
|
|
|
||||
|
|
|
2016 |
|
2015 |
|
Change |
|
|||
|
|
|
(in thousands) |
|
|||||||
|
Collaboration revenue |
|
$ |
14,220 |
|
$ |
17,334 |
|
$ |
(3,114) |
|
|
Operating expenses: |
|
|
|
|
|
|
|
|
|
|
|
Research and development |
|
|
42,249 |
|
|
27,679 |
|
|
14,570 |
|
|
General and administrative |
|
|
13,270 |
|
|
9,909 |
|
|
3,361 |
|
|
Total operating expenses |
|
|
55,519 |
|
|
37,588 |
|
|
17,931 |
|
|
Other income (expense), net: |
|
|
|
|
|
|
|
|
|
|
|
Interest income |
|
|
976 |
|
|
332 |
|
|
644 |
|
|
Other income (expense), net |
|
|
182 |
|
|
(9,750) |
|
|
9,932 |
|
|
Total other income (expense), net |
|
|
1,158 |
|
|
(9,418) |
|
|
10,576 |
|
|
Loss before income taxes |
|
|
(40,141) |
|
|
(29,672) |
|
|
(10,469) |
|
|
Income tax provision |
|
|
52 |
|
|
— |
|
|
52 |
|
|
Net loss |
|
$ |
(40,193) |
|
$ |
(29,672) |
|
$ |
52 |
|
Collaboration Revenue
Collaboration revenue was $14.2 million for the year ended December 31, 2016, and $17.3 million for the year ended December 31, 2015, all of which related to the Sanofi Genzyme Collaboration in recognition of amounts allocated to research and development services for various programs under the Sanofi Genzyme collaboration agreement. During 2016 we reassessed the estimated period of performance for each of the units of accounting and determined that the estimated period would be extended for two units of accounting, we deprioritized the development of VY-SMN101, and reduced the estimates related to the amount of “in-kind” services that would be provided by Sanofi Genzyme. These adjustments were made on a prospective basis and resulted in decreases in revenue recognized by $5.5 million, in the year ended December 31, 2016.
123
Research and Development Expense
Research and development expense increased by $14.6 million from $27.6 million for the year ended December 31, 2015 to $42.2 million for the year ended December 31, 2016. The following table summarizes our research and development expenses, for the year ended December 31, 2016 and 2015, respectively:
|
|
|
Year ended |
|
|
|
|||||
|
|
|
December 31, |
|
|
|
|||||
|
|
|
2016 |
|
2015 |
|
Change |
|
|||
|
|
|
(in thousands) |
|
|||||||
|
External research and development expenses |
|
$ |
20,413 |
|
$ |
14,128 |
|
$ |
6,285 |
|
|
Employee and contractor related expenses |
|
|
15,530 |
|
|
11,351 |
|
|
4,179 |
|
|
Facility and other expenses |
|
|
4,553 |
|
|
1,906 |
|
|
2,647 |
|
|
License fees |
|
|
1,753 |
|
|
294 |
|
|
1,459 |
|
|
Total research and development expenses |
|
$ |
42,249 |
|
$ |
27,679 |
|
$ |
14,570 |
|
The change in research and development expense was primarily attributable to research and development, and included the following:
|
· |
approximately $5.1 million or increased costs of funding research performed by third parties that conduct research and development, preclinical and clinical activities and manufacturing and production design on our behalf and increased purchases of lab supplies and non‑capital equipment used in designing, developing and manufacturing preclinical study materials, and an additional expense of approximately $1.2 million attributable to in-kind research and development services incurred by Sanofi Genzyme and provided to us under the Sanofi Genzyme Collaboration; |
|
· |
approximately $4.2 million for increased research and development employee compensation costs; |
|
· |
approximately $2.6 million for increased facility and other costs including rent, depreciation, maintenance and other expenses; and |
|
· |
approximately $1.5 million related to increases licensing costs. |
General and Administrative Expense
General and administrative expense increased by $3.4 million from $9.9 million for the year ended December 31, 2015 to $13.3 million for the year ended December 31, 2016. The change in general and administrative expense was primarily attributable to the following:
|
· |
approximately $2.3 million for increased administrative function headcount; |
|
· |
approximately $0.6 million for increased facility and other costs including rent, depreciation, maintenance and other expenses; and |
|
· |
approximately $0.4 million for increased legal and patent expenses. |
Other Income (Expense), Net
Investment income of approximately $1.0 million was recognized in the year ended December 31, 2016 due to increased marketable securities balances resulting from our underwritten initial public offering in November 2015.
124
Other income of approximately $0.2 million was recognized due to grants. Additionally, the expense recorded in the year ended December 31, 2015 of $9.4 million related to the mark to market adjustments recorded on our Series A Preferred Stock Tranche Right liability as of the year ended December 31, 2015. The increase in value of the Series A Preferred Stock Tranche Rights liability was a result of the increase in the fair value of our Series A Preferred Stock and the increase in the probability of closing the tranche during the year ended December 31, 2015. The Series A Preferred Stock Tranche Rights liability was settled in February 2015 upon the issuance of the final tranche of Series A Preferred Stock.
Income Tax Provision (Benefit)
We recorded an income tax provision of $0.2 million related to our alternative minimum tax, or AMT, liability resulting in an income tax payable of $0.1 million for the year ended December 31, 2016. There was no income tax payable for the year ended December 31, 2015. The payable was due to the recognition of deferred revenue related to the Sanofi Genzyme Collaboration for income tax purposes. Our overall income tax provision was offset by an income tax benefit recorded to continuing operations of $0.1 million associated with the recognition of the corresponding income tax associated with unrealized gains included in other comprehensive income. The net tax effect resulted in an overall income tax provision recorded to continuing operations of $0.1 million. We recorded no income tax provision (benefit) for the year ended December 31, 2015.
Liquidity and Capital Resources
Sources of Liquidity
We have funded our operations primarily through private placements of redeemable convertible preferred stock, public offerings of our common stock, and our collaboration with Sanofi Genzyme, or the Sanofi Genzyme Collaboration, which commenced in February 2015.
On November 16, 2015, we closed our IPO whereby we sold 5,750,000 shares of common stock, at a public offering price of $14.00 per share, including 750,000 shares of common stock issued upon the full exercise by the underwriters of their option to purchase additional shares, resulting in net proceeds to us of $72.9 million after deducting underwriting discounts and commissions and offering expenses payable by us. On November 7, 2017, we sold 5,175,000 shares of common stock to the public at an offering price of $12.00 per share, including 675,000 shares of common stock issued upon the full exercise by the underwriters of their option to purchase additional shares, resulting in net proceeds to us of $58.0 million after deducting underwriting discounts, commissions, and offering expenses payable by us.
As of December 31, 2017, we had cash, cash equivalents, and marketable debt securities of $169.1 million. Subsequent to December 31, 2017, we received $69.0 million in cash due to the execution of our collaboration agreement with AbbVie, which we refer to as the AbbVie Collaboration Agreement.
125
Cash Flows
The following table provides information regarding our cash flows for the years ended December 31, 2017, 2016, and 2015:
|
|
|
Year ended |
|
|||||||
|
|
|
December 31, |
|
|||||||
|
|
|
2017 |
|
2016 |
|
2015 |
|
|||
|
|
|
(in thousands) |
|
|||||||
|
Net cash (used in) provided by: |
|
|
|
|
|
|
|
|
|
|
|
Operating activities |
|
$ |
(61,350) |
|
$ |
(42,482) |
|
$ |
41,299 |
|
|
Investing activities |
|
|
(3,681) |
|
|
47,300 |
|
|
(194,769) |
|
|
Financing activities |
|
|
59,920 |
|
|
514 |
|
|
177,744 |
|
|
Net (decrease) increase in cash and cash equivalents |
|
$ |
(5,111) |
|
$ |
5,332 |
|
$ |
24,274 |
|
Cash Flows from Operating Activities
Net cash used in operating activities was $61.4 million during the year ended December 31, 2017 compared to $42.5 million during the year ended December 31, 2016. The increase in cash used for operation activities was primarily due to an increase in operating expenses. The increase in operating expenses is primarily due to increased research and development activities as we move our clinical and preclinical programs forward, as well as higher general and administrative expenses to support the increased research and development operations.
Net cash used in operating activities was $42.5 million during the year ended December 31, 2016 compared to $41.3 million of cash provided by operating activities during the year ended December 31, 2015. The decrease in cash provided by operating activities year over year was due to the $65.0 million upfront payment from Sanofi Genzyme under the Sanofi Genzyme collaboration agreement in February 2015, and increases in cash used for increased operating expenses, adjusted for non-cash items. The increases in operating expenses are primarily due to increased research and development activities, as well as higher general and administrative expenses as a result of operating as a public company during the year ended December 31, 2016.
Cash Flows from Investing Activities
Net cash used in investing activities was $3.7 million during the year ended December 31, 2017. The cash used in investing activities for the year ended December 31, 2017 was primarily due to purchases of property and equipment of $4.0 million, offset by net proceeds from maturities and purchases of marketable securities of $0.3 million.
Net cash provided by investing activities was $47.3 million during the year ended December 31, 2016. The cash provided by investing activities for the year ended December 31, 2016 was primarily due to proceeds from maturities of marketable securities of $165.1 million, partially offset by purchases of marketable securities of $112.4 million and purchases of property and equipment of $5.0 million.
Net cash used in investing activities was $194.8 million during the year ended December 31, 2015. The cash used in investing activities was due to purchases of marketable securities of $220.4 million offset by the proceeds from maturities of marketable securities of $26.7 million, and $1.0 million in purchases of property and equipment.
Cash Flows from Financing Activities
Net cash provided by financing activities was $59.9 million during the year ended December 31, 2017 and was largely driven by the $58.0 million of net proceeds from our sale of common stock in November 2017 and proceeds from exercises of stock options.
Net cash provided by financing activities was $0.5 million during the year ended December 31, 2016 related to proceeds from exercises of stock options.
126
Net cash provided by financing activities was $177.7 million during the year ended December 31, 2015. The increase in cash provided by financing activities was from the receipt of IPO proceeds (net of underwriting discounts and commissions, but prior to deducting other transaction expenses) of $72.9 million, the issuance of $20.0 million of Series A Preferred Stock, and $90.0 million of Series B Preferred Stock, of which $5.0 million in proceeds were in excess of the Series B Preferred Stock’s fair value and were allocated to deferred revenue. Cash payments of IPO related expenses totaled $1.9 million during the year ended December 31, 2015.
Funding Requirements
We expect our expenses to increase in connection with our ongoing activities, particularly as we continue the research and development of, continue or initiate clinical trials of, and seek marketing approval for, our product candidates. In addition, if we obtain marketing approval for any of our product candidates, we expect to incur significant expenses related to program sales, marketing, manufacturing and distribution to the extent that such sales, marketing and distribution are not the responsibility of potential collaborators. Furthermore, we expect to incur additional costs associated with operating as a public company. Accordingly, we will need to obtain substantial additional funding in connection with our continuing operations. If we are unable to raise capital or enter into business development transactions when needed or on acceptable terms, we could be forced to delay, reduce or eliminate our research and development programs or any future commercialization efforts.
Based upon our current operating plan, we expect our existing cash, cash equivalents, and marketable debt securities, as well as funds received upon the execution of the AbbVie Collaboration Agreement in 2018, will enable us to fund our operating expenses and capital expenditure requirements into 2020. Our future capital requirements will depend on many factors, including:
|
· |
the scope, progress, results, and costs of product discovery, preclinical studies and clinical trials for our product candidates; |
|
· |
the scope, progress, results, costs, prioritization, and number of our research and development programs; |
|
· |
the progress and status of our collaborations with Sanofi Genzyme and AbbVie, including any research and development costs for which we are responsible, the potential exercise by our collaboration partners of options to develop or license certain compounds, and our potential receipt of future milestone payments and royalties from our collaboration partners; |
|
· |
the extent to which we are obligated to reimburse, or entitled to reimbursement of, preclinical development and clinical trial costs, or the achievement of milestones or occurrence of other developments that trigger payments, under any other collaboration agreement to which we might become a party; |
|
· |
the costs, timing and outcome of regulatory review of our product candidates; |
|
· |
our ability to establish and maintain collaboration, distribution, or other marketing arrangements for our product candidates on favorable terms, if at all; |
|
· |
the costs and timing of preparing, filing and prosecuting patent applications, maintaining and enforcing our intellectual property rights and defending intellectual property‑related claims; |
|
· |
the extent to which we acquire or in‑license other product candidates and technologies or acquire or invest in other businesses, such as our investment in MRI Interventions, Inc.; |
|
· |
the costs related to evaluating possible alternative devices that may be useful in the delivery of our product candidates, including our ongoing development of our V-TAG device; |
127
|
· |
the costs of securing manufacturing arrangements for commercial production; |
|
· |
the level of product sales from any product candidates for which we obtain marketing approval in the future; and |
|
· |
the costs of establishing or contracting for sales, manufacturing, marketing, distribution, and other commercialization capabilities if we obtain regulatory approvals to market our product candidates. |
Identifying potential product candidates and conducting preclinical studies and clinical trials is a time‑consuming, expensive and uncertain process that takes years to complete. We may never generate the necessary data or results required to obtain marketing approval and achieve product sales. In addition, our product candidates, if approved, may not achieve commercial success. Our product revenues, if any, and any commercial milestones or royalty payments under our collaboration agreements, will be derived from sales of products that may not be commercially available for many years, if at all. Accordingly, we will need to continue to rely on additional financing and business development transactions to achieve our business objectives. Adequate additional financing may not be available to us on acceptable terms, or at all.
Until such time, if ever, as we can generate product revenues sufficient to achieve profitability, we expect to finance our cash needs through a combination of equity offerings, debt financings, collaborations, strategic alliances and licensing arrangements. To the extent that we raise additional capital through the sale of equity or equity-linked securities, including convertible debt, our stockholders’ ownership interests will be diluted, and the terms of these securities may include liquidation or other preferences that adversely affect our existing stockholders’ rights as holders of our common stock. Debt financing and preferred equity financing, if available, may involve agreements that include covenants limiting or restricting our ability to take specific actions, such as incurring additional debt, obtaining additional capital, acquiring or divesting businesses, making capital expenditures or declaring dividends.
If we raise additional funds through collaborations, strategic alliances or licensing arrangements with third parties, we may have to relinquish valuable rights to our technologies, future revenue streams, research programs or product candidates or to grant licenses on terms that may not be favorable to us. If we are unable to raise additional funds through equity or debt financings when needed, we may be required to delay, limit, reduce or terminate our product development or future commercialization efforts or grant rights to develop and market product candidates that we would otherwise prefer to develop and market ourselves.
Contractual Obligations
The following table summarizes our significant contractual obligations as of payment due date by period at December 31, 2017:
|
|
|
|
|
|
Less Than |
|
|
|
|
|
|
|
More than |
|
||
|
|
|
Total |
|
1 Year |
|
1 to 3 Years |
|
3 to 5 Years |
|
5 Years |
|
|||||
|
|
|
(in thousands) |
|
|||||||||||||
|
Operating lease commitments(1) |
|
$ |
26,574 |
|
$ |
3,290 |
|
$ |
7,144 |
|
$ |
7,845 |
|
$ |
8,295 |
|
|
(1) |
We lease office space at 75 Sidney Street and 64 Sidney Street in Cambridge, Massachusetts under non‑cancelable operating leases that expire in December 2024. |
In February 2018, we executed an amendment for additional space located at 75 Sidney Street in Cambridge, Massachusetts, concurrent to the existing leases with terms going through December 2024.
We enter into agreements in the normal course of business with CROs and institutions to license intellectual property. We have not included these future payments in the table of contractual obligations above since the contracts are cancelable at any time by us, generally upon 30 to 90 days prior written notice.
128
Our agreements to license intellectual property include potential milestone payments that are dependent upon the development of products using the intellectual property licensed under the agreements and contingent upon the achievement of clinical trial or regulatory approval milestones. The maximum aggregate potential milestone payments payable by us total approximately $18.0 million. Additionally, under the terms of one agreement, we have options to license intellectual property to be used in the development of therapies for four disease indications. If we exercise all of the options under the agreement, we would be obligated to pay aggregate upfront fees of up to approximately $1.6 million and milestone payments that are contingent upon clinical trial results and regulatory approval of $5.0 million per disease indication, or up to $20.0 million in total. We may also be required to pay annual maintenance fees or minimum amounts payable ranging from low‑four digits to low five‑digits depending upon the terms of the applicable agreement.
Off‑Balance Sheet Arrangements
We did not have, during the periods presented, and we do not currently have, any off‑balance sheet arrangements, as defined under applicable Securities and Exchange Commission rules.
JOBS Act
In April 2012, the JOBS Act, was enacted. Section 107 of the JOBS Act provides that an emerging growth company, or EGC, can take advantage of the extended transition period provided in Section 7(a)(2)(B) of the Securities Act of 1933, as amended, or the Securities Act, for complying with new or revised accounting standards. Thus, an EGC can delay the adoption of certain accounting standards until those standards would otherwise apply to private companies.
Subject to certain conditions, as an EGC, we intend to rely on certain of these exemptions, including without limitation, (i) providing an auditor’s attestation report on our system of internal controls over financial reporting pursuant to Section 404(b) of the Sarbanes‑Oxley Act and (ii) complying with any requirement that may be adopted by the Public Company Accounting Oversight Board, or PCAOB, regarding mandatory audit firm rotation or a supplement to the auditor’s report providing additional information about the audit and the financial statements, known as the auditor discussion and analysis. We will remain an EGC until the earlier of (i) the last day of the fiscal year in which we have total annual gross revenues of $1.07 billion or more; (ii) December 31, 2020; (iii) the date on which we have issued more than $1.0 billion in nonconvertible debt during the previous three years; or (iv) the date on which we are deemed to be a large accelerated filer under the rules of the SEC.
ITEM 7A. QUANTITATIVE AND QUALITATIVE DISCLOSURES ABOUT MARKET RISK
We are exposed to market risk related to changes in interest rates. We have policies requiring us to invest in high-quality issuers, limit our exposure to any individual issuer, and ensure adequate liquidity. Our primary exposure to market risk is interest rate sensitivity, which is affected by changes in the general level of U.S. interest rates, particularly because our investments, including cash equivalents, are in the form of money market fund and marketable securities and are invested in U.S. Treasury and U.S. government agency obligations. Due to the short-term duration of our investment portfolio and the low risk profile of our investments, an immediate 100 basis point change in interest rates would not have had a material effect on the fair market value of our portfolio.
We are not currently exposed to market risk related to changes in foreign currency exchange rates; however, we may contract with vendors that are located in Asia and Europe in the future and may be subject to fluctuations in foreign currency rates at that time.
Inflation generally affects us by increasing our cost of labor and clinical trial costs. We do not believe that inflation had a material effect on our business, financial condition, or results of operations during the year ended December 31, 2017.
129
ITEM 8. FINANCIAL STATEMENTS AND SUPPLEMENTARY DATA
The financial statements required to be filed pursuant to this Item 8 are appended to this report. An index of those financial statements is found in Item 15.
ITEM 9. CHANGES IN AND DISAGREEMENTS WITH ACCOUNTANTS ON ACCOUNTING AND FINANCIAL DISCLOSURE
None.
ITEM 9A. CONTROLS AND PROCEDURES
Management’s Evaluation of Disclosure Controls and Procedures
We maintain disclosure controls and procedures that are designed to ensure that information required to be disclosed in the reports that we file or submit under the Securities and Exchange Act of 1934 is (1) recorded, processed, summarized, and reported within the time periods specified in the SEC’s rules and forms and (2) accumulated and communicated to our management, including our President and Chief Executive Officer, who is our principal executive officer, and our Chief Financial Officer and Senior Vice President of Corporate Development, who is our principal financial and accounting officer, to allow timely decisions regarding required disclosure.
As of December 31, 2017, our management, with the participation of our principal executive officer and principal financial and accounting officer, evaluated the effectiveness of our disclosure controls and procedures (as defined in Rules 13a-15(e) and 15d-15(e) under the Securities and Exchange Act of 1934). Our management recognizes that any controls and procedures, no matter how well designed and operated, can provide only reasonable assurance of achieving their objectives, and management necessarily applies its judgment in evaluating the cost-benefit relationship of possible controls and procedures. Our principal executive officer and principal financial and accounting officer have concluded based upon the evaluation described above that, as of December 31, 2017, our disclosure controls and procedures were effective at the reasonable assurance level.
Management’s Annual Report on Internal Control over Financial Reporting
Our management is responsible for establishing and maintaining adequate internal control over financial reporting. Internal control over financial reporting is defined in Rules 13a-15(f) and 15d-15(f) under the Exchange Act as a process designed by, or under the supervision of, a company’s principal executive officer and principal financial officer, or persons performing similar functions, and effected by a company’s board of directors, management, and other personnel, to provide reasonable assurance regarding the reliability of financial reporting and the preparation of financial statements for external purposes in accordance with generally accepted accounting principles and includes those policies and procedures that:
|
· |
pertain to the maintenance of records that in reasonable detail accurately and fairly reflect the transactions and dispositions of a company’s assets; |
|
· |
provide reasonable assurance that transactions are recorded as necessary to permit preparation of financial statements in accordance with generally accepted accounting principles, and that a company’s receipts and expenditures are being made only in accordance with authorizations of the company’s management and directors; and |
|
· |
provide reasonable assurance regarding prevention or timely detection of unauthorized acquisition, use or disposition of our assets that could have a material effect on the financial statements. |
Because of its inherent limitations, internal control over financial reporting may not prevent or detect misstatements. Projections of any evaluation of effectiveness to future periods are subject to the risk that controls may become inadequate because of changes in conditions, or that the degree of compliance with the policies or procedures may deteriorate.
130
Under the supervision of and with the participation of our principal executive officer and principal financial and accounting officer, our management assessed the effectiveness of our internal control over financial reporting as of December 31, 2017 based on the criteria set forth by the Committee of Sponsoring Organizations of the Treadway Commission (COSO) in Internal Control—Integrated Framework (2013 framework). Based on this assessment, management concluded that our internal control over financial reporting was effective as of December 31, 2017.
Not applicable.
ITEM 10. DIRECTORS, EXECUTIVE OFFICERS AND CORPORATE GOVERNANCE
Incorporated by reference from the information in our Proxy Statement for our 2018 Annual Meeting of Stockholders, which we expect to file with the SEC within 120 days of the end of the fiscal year to which this Annual Report on Form 10-K relates.
ITEM 11. EXECUTIVE COMPENSATION
Incorporated by reference from the information in our Proxy Statement for our 2018 Annual Meeting of Stockholders, which we expect to file with the SEC within 120 days of the end of the fiscal year to which this Annual Report on Form 10-K relates.
ITEM 12. SECURITY OWNERSHIP OF CERTAIN BENEFICIAL OWNERS AND MANAGEMENT AND RELATED STOCKHOLDER MATTERS
Incorporated by reference from the information in our Proxy Statement for our 2018 Annual Meeting of Stockholders, which we expect to file with the SEC within 120 days of the end of the fiscal year to which this Annual Report on Form 10-K relates.
ITEM 13. CERTAIN RELATIONSHIPS AND RELATED TRANSACTIONS, AND DIRECTOR INDEPENDENCE
Incorporated by reference from the information in our Proxy Statement for our 2018 Annual Meeting of Stockholders, which we expect to file with the SEC within 120 days of the end of the fiscal year to which this Annual Report on Form 10-K relates.
ITEM 14. PRINCIPAL ACCOUNTANT FEES AND SERVICES
Incorporated by reference from the information in our Proxy Statement for our 2018 Annual Meeting of Stockholders, which we expect to file with the SEC within 120 days of the end of the fiscal year to which this Annual Report on Form 10-K relates.
131
ITEM 15. EXHIBITS, FINANCIAL STATEMENT SCHEDULES
(a)(1) Financial Statements.
|
|
|
Pages |
|
|
F-1 |
|
|
|
F-2 |
|
|
Consolidated Statements of Operations and Comprehensive Loss |
|
F-3 |
|
Consolidated Statements of Redeemable Convertible Preferred Stock and Stockholders’ Equity (Deficit) |
|
F-4 |
|
F-5 |
||
|
|
F-6 |
|
(a)(2) Financial Statement Schedules.
All schedules have been omitted because they are not required or because the required information is given in the Consolidated Financial Statements or Notes thereto set forth under Item 8 above.
(a)(3) Exhibits.
See the Exhibit Index immediately preceding the signature page of this Annual Report on Form 10-K. The exhibits listed in the Exhibit Index below are filed or incorporated by reference as part of this Annual Report on Form 10-K.
This Annual Report on Form 10-K does not include a summary.
132
Report of Independent Registered Public Accounting Firm
To the Stockholders and the Board of Directors of Voyager Therapeutics, Inc.
Opinion on the Financial Statements
We have audited the accompanying consolidated balance sheets of Voyager Therapeutics, Inc. as of December 31, 2017 and 2016, the related consolidated statements of operations and comprehensive loss, redeemable convertible preferred stock and stockholders’ equity (deficit), and cash flows for each of the three years in the period ended December 31, 2017, and the related notes (collectively referred to as the “consolidated financial statements”). In our opinion, the consolidated financial statements present fairly, in all material respects, the financial position of the Company at December 31, 2017 and 2016, and the results of its operations and its cash flows for each of the three years in the period ended December 31, 2017, in conformity with U.S. generally accepted accounting principles.
Basis for Opinion
These financial statements are the responsibility of the Company’s management. Our responsibility is to express an opinion on the Company’s financial statements based on our audits. We are a public accounting firm registered with the Public Company Accounting Oversight Board (United States) (PCAOB) and are required to be independent with respect to the Company in accordance with the U.S. federal securities laws and the applicable rules and regulations of the Securities and Exchange Commission and the PCAOB.
We conducted our audits in accordance with the standards of the PCAOB. Those standards require that we plan and perform the audit to obtain reasonable assurance about whether the financial statements are free of material misstatement, whether due to error or fraud. The Company is not required to have, nor were we engaged to perform, an audit of its internal control over financial reporting. As part of our audits we are required to obtain an understanding of internal control over financial reporting but not for the purpose of expressing an opinion on the effectiveness of the Company’s internal control over financial reporting. Accordingly, we express no such opinion.
Our audits included performing procedures to assess the risks of material misstatement of the financial statements, whether due to error or fraud, and performing procedures that respond to those risks. Such procedures included examining, on a test basis, evidence regarding the amounts and disclosures in the financial statements. Our audits also included evaluating the accounting principles used and significant estimates made by management, as well as evaluating the overall presentation of the financial statements. We believe that our audits provide a reasonable basis for our opinion.
/S/ Ernst & Young LLP
We have served as the Company’s auditor since 2015.
Boston, Massachusetts
March 14, 2018
F-1
Voyager Therapeutics, Inc.
(amounts in thousands, except share and per share data)
|
|
|
December 31, |
|
||||
|
|
|
2017 |
|
2016 |
|
||
|
Assets |
|
|
|
|
|
|
|
|
Current assets: |
|
|
|
|
|
|
|
|
Cash and cash equivalents |
|
$ |
31,530 |
|
$ |
36,641 |
|
|
Marketable securities, current |
|
|
137,522 |
|
|
137,777 |
|
|
Prepaid expenses and other current assets |
|
|
2,738 |
|
|
4,368 |
|
|
Total current assets |
|
|
171,790 |
|
|
178,786 |
|
|
Property and equipment, net |
|
|
10,283 |
|
|
7,893 |
|
|
Deposits and other non-current assets |
|
|
1,304 |
|
|
1,527 |
|
|
Marketable securities, non-current |
|
|
1,100 |
|
|
1,360 |
|
|
Total assets |
|
$ |
184,477 |
|
$ |
189,566 |
|
|
Liabilities and stockholders’ equity |
|
|
|
|
|
|
|
|
Current liabilities: |
|
|
|
|
|
|
|
|
Accounts payable |
|
$ |
1,020 |
|
$ |
550 |
|
|
Accrued expenses |
|
|
11,497 |
|
|
6,488 |
|
|
Deferred revenue, current portion |
|
|
3,380 |
|
|
6,764 |
|
|
Total current liabilities |
|
|
15,897 |
|
|
13,802 |
|
|
Deferred rent |
|
|
5,337 |
|
|
4,999 |
|
|
Deferred revenue, net of current portion |
|
|
28,180 |
|
|
34,818 |
|
|
Other non-current liabilities |
|
|
1,012 |
|
|
25 |
|
|
Total liabilities |
|
|
50,426 |
|
|
53,644 |
|
|
Commitments and contingencies (see note 7) |
|
|
|
|
|
|
|
|
Stockholders’ equity: |
|
|
|
|
|
|
|
|
Preferred stock, $0.001 par value: 5,000,000 shares authorized; no shares issued and outstanding at December 31, 2017 and 2016 |
|
|
— |
|
|
— |
|
|
Common stock, $0.001 par value: 120,000,000 shares authorized; 31,572,044 and 25,597,912 shares issued and outstanding at December 31, 2017 and 2016, respectively |
|
|
32 |
|
|
26 |
|
|
Additional paid-in capital |
|
|
295,019 |
|
|
225,963 |
|
|
Accumulated other comprehensive loss |
|
|
(287) |
|
|
(52) |
|
|
Accumulated deficit |
|
|
(160,713) |
|
|
(90,015) |
|
|
Total stockholders’ equity |
|
|
134,051 |
|
|
135,922 |
|
|
Total liabilities and stockholders’ equity |
|
$ |
184,477 |
|
$ |
189,566 |
|
The accompanying notes are an integral part of these consolidated financial statements.
F-2
Voyager Therapeutics, Inc.
Consolidated Statements of Operations and Comprehensive Loss
(amounts in thousands, except share and per share data)
|
|
|
Year ended |
|
|||||||
|
|
|
December 31, |
|
|||||||
|
|
|
2017 |
|
2016 |
|
2015 |
|
|||
|
Collaboration revenue |
|
$ |
10,135 |
|
$ |
14,220 |
|
$ |
17,334 |
|
|
Operating expenses: |
|
|
|
|
|
|
|
|
|
|
|
Research and development |
|
|
62,260 |
|
|
42,249 |
|
|
27,679 |
|
|
General and administrative |
|
|
19,738 |
|
|
13,270 |
|
|
9,909 |
|
|
Total operating expenses |
|
|
81,998 |
|
|
55,519 |
|
|
37,588 |
|
|
Operating loss |
|
|
(71,863) |
|
|
(41,299) |
|
|
(20,254) |
|
|
Other income (expense), net: |
|
|
|
|
|
|
|
|
|
|
|
Interest income |
|
|
1,227 |
|
|
976 |
|
|
332 |
|
|
Other (expense) income, net |
|
|
(62) |
|
|
182 |
|
|
(9,750) |
|
|
Total other income (expense), net |
|
|
1,165 |
|
|
1,158 |
|
|
(9,418) |
|
|
Loss before income taxes |
|
|
(70,698) |
|
|
(40,141) |
|
|
(29,672) |
|
|
Income tax provision |
|
|
— |
|
|
52 |
|
|
— |
|
|
Net loss |
|
$ |
(70,698) |
|
$ |
(40,193) |
|
$ |
(29,672) |
|
|
Other comprehensive loss |
|
|
|
|
|
|
|
|
|
|
|
Net unrealized (loss) gain on available-for-sale-securities, net of tax expense of $128 for the year ended December 31, 2016 |
|
|
(235) |
|
|
199 |
|
|
(251) |
|
|
Total other comprehensive (loss) income |
|
|
(235) |
|
|
199 |
|
|
(251) |
|
|
Comprehensive loss |
|
$ |
(70,933) |
|
$ |
(39,994) |
|
$ |
(29,923) |
|
|
Reconciliation of net loss to net loss attributable to common stockholders: |
|
|
|
|
|
|
|
|
|
|
|
Net loss |
|
$ |
(70,698) |
|
$ |
(40,193) |
|
$ |
(29,672) |
|
|
Accretion of redeemable convertible preferred stock to redemption value |
|
|
— |
|
|
— |
|
|
(7,373) |
|
|
Accrued dividends on Series A preferred stock |
|
|
— |
|
|
— |
|
|
(1,245) |
|
|
Net loss attributable to common stockholders |
|
$ |
(70,698) |
|
$ |
(40,193) |
|
$ |
(38,290) |
|
|
Net loss per share attributable to common stockholders, basic and diluted |
|
$ |
(2.64) |
|
$ |
(1.59) |
|
$ |
(9.14) |
|
|
Weighted-average common shares outstanding, basic and diluted |
|
|
26,803,711 |
|
|
25,302,414 |
|
|
4,191,210 |
|
The accompanying notes are an integral part of these consolidated financial statements.
F-3
Voyager Therapeutics, Inc.
Statements of Redeemable Convertible Preferred Stock and Stockholders’ Equity (Deficit)
(amounts in thousands, except share data)
|
|
|
Series A |
|
Series B |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
||||||
|
|
|
Redeemable |
|
Redeemable |
|
|
|
|
|
|
|
|
|
|
Accumulated |
|
|
|
|
|
|
|
|||||||
|
|
|
Convertible |
|
Convertible |
|
|
|
|
|
|
|
Additional |
|
Other |
|
|
|
|
|
|
|||||||||
|
|
|
Preferred Stock |
|
Preferred Stock |
|
|
Common Stock |
|
Paid-In |
|
Comprehensive |
|
Accumulated |
|
Stockholders’ |
|
|||||||||||||
|
|
|
Shares |
|
Amount |
|
Shares |
|
Amount |
|
|
Shares |
|
Amount |
|
Capital |
|
Loss |
|
Deficit |
|
Equity (Deficit) |
|
|||||||
|
Balance at December 31, 2014 |
|
25,000,000 |
|
$ |
21,979 |
|
— |
|
$ |
— |
|
|
814,834 |
|
$ |
1 |
|
$ |
— |
|
$ |
— |
|
$ |
(20,831) |
|
$ |
(20,830) |
|
|
Issuance of Series A preferred stock, net of issuance costs of $1 |
|
20,000,000 |
|
|
19,999 |
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
Reclassification of tranche rights upon issuance of preferred stock |
|
— |
|
|
16,055 |
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
Issuance of Series B preferred stock, net of discount of $5,000 and issuance costs of $220 |
|
— |
|
|
— |
|
30,000,001 |
|
|
84,780 |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
Vesting of restricted stock |
|
— |
|
|
— |
|
— |
|
|
— |
|
|
717,747 |
|
|
— |
|
|
22 |
|
|
— |
|
|
— |
|
|
22 |
|
|
Exercises of vested stock options |
|
— |
|
|
— |
|
— |
|
|
— |
|
|
1,344 |
|
|
— |
|
|
10 |
|
|
— |
|
|
— |
|
|
10 |
|
|
Issuance of common stock from initial public offering (net of underwriters discounts and issuance costs of $7,500) |
|
— |
|
|
— |
|
— |
|
|
— |
|
|
5,750,000 |
|
|
6 |
|
|
72,948 |
|
|
— |
|
|
— |
|
|
72,954 |
|
|
Stock-based compensation expense |
|
— |
|
|
— |
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
4,027 |
|
|
— |
|
|
— |
|
|
4,027 |
|
|
Unrealized loss on available-for-sale securities, net of tax |
|
— |
|
|
— |
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
(251) |
|
|
— |
|
|
(251) |
|
|
Accretion of preferred stock to redemption value |
|
— |
|
|
2,149 |
|
— |
|
|
5,225 |
|
|
— |
|
|
— |
|
|
(2,560) |
|
|
— |
|
|
(4,813) |
|
|
(7,373) |
|
|
Conversion of redeemable convertible preferred stock to common stock |
|
(45,000,000) |
|
|
(60,182) |
|
(30,000,001) |
|
|
(90,005) |
|
|
17,647,054 |
|
|
18 |
|
|
144,675 |
|
|
— |
|
|
5,494 |
|
|
150,187 |
|
|
Net loss |
|
— |
|
|
— |
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
(29,672) |
|
|
(29,672) |
|
|
Balance at December 31, 2015 |
|
— |
|
$ |
— |
|
— |
|
$ |
— |
|
|
24,930,979 |
|
$ |
25 |
|
$ |
219,122 |
|
$ |
(251) |
|
$ |
(49,822) |
|
$ |
169,074 |
|
|
Vesting of restricted stock |
|
— |
|
|
— |
|
— |
|
|
— |
|
|
601,501 |
|
|
1 |
|
|
17 |
|
|
— |
|
|
— |
|
|
18 |
|
|
Exercises of vested stock options |
|
— |
|
|
— |
|
— |
|
|
— |
|
|
65,432 |
|
|
— |
|
|
514 |
|
|
— |
|
|
— |
|
|
514 |
|
|
Stock-based compensation expense |
|
— |
|
|
— |
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
6,310 |
|
|
— |
|
|
— |
|
|
6,310 |
|
|
Unrealized loss on available-for-sale securities, net of tax |
|
— |
|
|
— |
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
199 |
|
|
— |
|
|
199 |
|
|
Net loss |
|
— |
|
|
— |
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
(40,193) |
|
|
(40,193) |
|
|
Balance at December 31, 2016 |
|
— |
|
$ |
— |
|
— |
|
$ |
— |
|
|
25,597,912 |
|
$ |
26 |
|
$ |
225,963 |
|
$ |
(52) |
|
$ |
(90,015) |
|
$ |
135,922 |
|
|
Vesting of restricted stock |
|
— |
|
|
— |
|
— |
|
|
— |
|
|
573,803 |
|
|
1 |
|
|
12 |
|
|
— |
|
|
— |
|
|
13 |
|
|
Exercises of vested stock options |
|
— |
|
|
— |
|
— |
|
|
— |
|
|
158,677 |
|
|
— |
|
|
1,363 |
|
|
— |
|
|
— |
|
|
1,363 |
|
|
Issuance of common stock under ESPP |
|
— |
|
|
— |
|
— |
|
|
— |
|
|
66,652 |
|
|
— |
|
|
563 |
|
|
— |
|
|
— |
|
|
563 |
|
|
Issuance of common stock from public offering (net of underwriters discounts and issuance costs of $4,100) |
|
— |
|
|
— |
|
— |
|
|
— |
|
|
5,175,000 |
|
|
5 |
|
|
57,989 |
|
|
— |
|
|
— |
|
|
57,994 |
|
|
Stock-based compensation expense |
|
— |
|
|
— |
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
9,129 |
|
|
— |
|
|
— |
|
|
9,129 |
|
|
Unrealized loss on available-for-sale securities, net of tax |
|
— |
|
|
— |
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
(235) |
|
|
— |
|
|
(235) |
|
|
Net loss |
|
— |
|
|
— |
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
— |
|
|
(70,698) |
|
|
(70,698) |
|
|
Balance at December 31, 2017 |
|
— |
|
$ |
— |
|
— |
|
$ |
— |
|
|
31,572,044 |
|
$ |
32 |
|
$ |
295,019 |
|
$ |
(287) |
|
$ |
(160,713) |
|
$ |
134,051 |
|
The accompanying notes are an integral part of these consolidated financial statements
F-4
Voyager Therapeutics, Inc.
Condensed Statements of Cash Flows
(amounts in thousands)
|
|
|
Year ended |
|
|||||||
|
|
|
December 31, |
|
|||||||
|
|
|
2017 |
|
2016 |
|
2015 |
|
|||
|
Cash flow from operating activities |
|
|
|
|
|
|
|
|
|
|
|
Net loss |
|
$ |
(70,698) |
|
$ |
(40,193) |
|
$ |
(29,672) |
|
|
Adjustments to reconcile net loss to net cash (used in) provided by operating activities: |
|
|
|
|
|
|
|
|
|
|
|
Stock-based compensation expense |
|
|
9,238 |
|
|
6,310 |
|
|
4,027 |
|
|
Depreciation |
|
|
1,595 |
|
|
612 |
|
|
600 |
|
|
Amortization of premiums and discounts on marketable securities |
|
|
(24) |
|
|
696 |
|
|
452 |
|
|
Change in fair value of preferred stock tranche liability |
|
|
— |
|
|
— |
|
|
9,750 |
|
|
In-kind research and development expenses |
|
|
113 |
|
|
1,182 |
|
|
2,316 |
|
|
Other non-cash items |
|
|
46 |
|
|
709 |
|
|
(277) |
|
|
Changes in operating assets and liabilities: |
|
|
|
|
|
|
|
|
|
|
|
Prepaid expenses and other current assets |
|
|
1,630 |
|
|
(847) |
|
|
(234) |
|
|
Other non-current assets |
|
|
— |
|
|
7 |
|
|
14 |
|
|
Deferred revenue |
|
|
(10,135) |
|
|
(14,582) |
|
|
52,666 |
|
|
Accounts payable |
|
|
470 |
|
|
(62) |
|
|
(942) |
|
|
Accrued expenses |
|
|
4,900 |
|
|
2,636 |
|
|
2,788 |
|
|
Other non-current liabilities |
|
|
1,000 |
|
|
— |
|
|
(189) |
|
|
Lease incentive benefit |
|
|
515 |
|
|
1,050 |
|
|
— |
|
|
Net cash (used in) provided by operating activities |
|
|
(61,350) |
|
|
(42,482) |
|
|
41,299 |
|
|
Cash flow from investing activities |
|
|
|
|
|
|
|
|
|
|
|
Purchases of property and equipment |
|
|
(3,985) |
|
|
(5,029) |
|
|
(1,030) |
|
|
Change in restricted cash |
|
|
— |
|
|
(421) |
|
|
— |
|
|
Purchases of marketable securities |
|
|
(147,296) |
|
|
(112,350) |
|
|
(220,399) |
|
|
Proceeds from maturities or sales of marketable securities |
|
|
147,600 |
|
|
165,100 |
|
|
26,660 |
|
|
Net cash (used in) provided by investing activities |
|
|
(3,681) |
|
|
47,300 |
|
|
(194,769) |
|
|
Cash flow from financing activities |
|
|
|
|
|
|
|
|
|
|
|
Proceeds from the issuance of stock net of discount and issuance costs |
|
|
57,994 |
|
|
— |
|
|
104,779 |
|
|
Proceeds from the exercise of stock options |
|
|
1,363 |
|
|
514 |
|
|
72,965 |
|
|
Proceeds from the purchase of common stock under ESPP |
|
|
563 |
|
|
— |
|
|
— |
|
|
Net cash provided by financing activities |
|
|
59,920 |
|
|
514 |
|
|
177,744 |
|
|
Net (decrease) increase in cash and cash equivalents |
|
|
(5,111) |
|
|
5,332 |
|
|
24,274 |
|
|
Cash and cash equivalents, beginning of period |
|
|
36,641 |
|
|
31,309 |
|
|
7,035 |
|
|
Cash and cash equivalents, end of period |
|
$ |
31,530 |
|
$ |
36,641 |
|
$ |
31,309 |
|
|
Supplemental disclosure of cash and non-cash activities |
|
|
|
|
|
|
|
|
|
|
|
Capital expenditures incurred but not yet paid |
|
$ |
— |
|
$ |
242 |
|
$ |
— |
|
|
Accretion of redeemable convertible preferred stock to redemption value |
|
$ |
— |
|
$ |
— |
|
$ |
7,373 |
|
|
Conversion of redeemable convertible preferred stock to common stock |
|
$ |
— |
|
$ |
— |
|
$ |
150,187 |
|
The accompanying notes are an integral part of these consolidated financial statements.
F-5
VOYAGER THERAPEUTICS INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
1. Nature of business
The Company is a clinical-stage gene therapy company focused on developing life-changing treatments for patients suffering from severe neurological diseases. The Company is focused on neurological diseases where it believes an adeno-associated virus (“AAV”) gene therapy approach that either increases or decreases the production of a specific protein can slow or reduce the symptoms experienced by patients, and therefore have a clinically meaningful impact. The Company has built a product engine that it believes positions itself to be the leading company at the intersection of AAV gene therapy and severe neurological disease. The Company’s product engine enables it to engineer, optimize, manufacture and deliver its AAV-based gene therapies that have the potential to provide durable efficacy following a single administration. Additionally, the Company is working to identify novel AAV capsids, which are the outer viral protein shells that enclose the genetic material of the virus payload. The Company’s team of experts in the fields of AAV gene therapy and neuroscience first identifies and selects severe neurological diseases that are well-suited for treatment using AAV gene therapy. The Company then engineers and optimizes AAV vectors for delivery of the virus payload to the targeted tissue or cells. The Company’s manufacturing process employs an established system that it believes will enable production of high quality AAV vectors at commercial-scale. Finally, the Company leverages established routes of administration and advances in dosing techniques to optimize delivery of its AAV gene therapies to target cells that are critical to the disease of interest either directly to discrete regions of the brain or, more broadly, to the spinal cord region.
The Company is devoting substantially all of its efforts to product research and development, market development, and raising capital. The Company is subject to risks common to companies in the biotechnology and gene therapy industry, including but not limited to, risks of failure of preclinical studies and clinical trials, the need to obtain marketing approval for its drug product candidates, the need to successfully commercialize and gain market acceptance of its drug product candidates, dependence on key personnel, protection of proprietary technology, compliance with government regulations, development by competitors of technological innovations, and ability to transition from pilot-scale manufacturing to large-scale production of products
The Company has incurred annual net operating losses in every year since inception. As of December 31, 2017, the Company had an accumulated deficit of $160.7 million. The Company has not generated any product revenue and has financed its operations primarily through public offerings and private placements of its equity securities and funding from its collaboration with Sanofi Genzyme. There can be no assurance that the Company will be able to obtain additional debt or equity financing or generate product revenue or revenue from collaborative partners on terms acceptable to the Company, on a timely basis or at all. The failure of the Company to obtain sufficient funds on acceptable terms when needed could have a material adverse effect on the Company’s business, results of operations, and financial condition.
2. Summary of significant accounting policies
The following is a summary of significant accounting policies followed in the preparation of these financial statements.
Basis of presentation
The accompanying consolidated financial statements include those of the Company and its subsidiary, Voyager Securities Corporation, after elimination of all intercompany accounts and transactions. The accompanying consolidated financial statements have been prepared in conformity with accounting principles generally accepted in the United States of America (“GAAP”).
Public offerings
On October 29, 2015, in preparation for the Company’s IPO, the Company’s Board of Directors and stockholders approved a 1-for-4.25 reverse split of the Company’s common stock, which became effective on October
F-6
29, 2015. All share and per share amounts in the consolidated financial statements and notes thereto have been retroactively adjusted for all periods presented to give effect to this reverse split, including reclassifying an amount equal to the reduction in par value of common stock to additional paid-in capital.
On November 16, 2015, the Company completed the sale of 5,750,000 shares of its common stock in its initial public offering (the “IPO”), at a price to the public of $14.00 per share, resulting in net proceeds to the Company of $72.9 million after deducting underwriting discounts, commissions and offering expenses payable by the Company.
Upon the closing of the IPO, all of the Company’s outstanding redeemable convertible preferred stock automatically converted into shares of common stock, resulting in the issuance of an additional 17,647,054 shares of common stock. The significant increase in shares outstanding in November 2015 effected the year-over-year comparability of the Company’s net loss per share calculations.
On November 7, 2017, the Company completed the sale of 5,175,000 shares of its common stock in a public offering at a price to the public of $12.00 per share, resulting in net proceeds to the Company of $58.0 million after deducting underwriting discounts, commissions, and offering expenses payable by the Company.
Use of Estimates
The preparation of consolidated financial statements in conformity with GAAP requires management to make estimates and assumptions that affect the amounts reported in the consolidated financial statements and accompanying notes. On an ongoing basis, the Company’s management evaluates its estimates, which include, but are not limited to, estimates related to revenue recognition, accrued expenses, valuation of the tranche rights, stock‑based compensation expense, income taxes and the fair value of common stock. The Company bases its estimates on historical experience and other market specific or other relevant assumptions that it believes to be reasonable under the circumstances. Actual results may differ from those estimates or assumptions.
Fair Value of Financial Instruments
ASC Topic 820, Fair Value Measurement (“ASC 820”), establishes a fair value hierarchy for instruments measured at fair value that distinguishes between assumptions based on market data (observable inputs) and the Company’s own assumptions (unobservable inputs). Observable inputs are inputs that market participants would use in pricing the asset or liability based on market data obtained from sources independent of the Company. Unobservable inputs are inputs that reflect the Company’s assumptions about the inputs that market participants would use in pricing the asset or liability, and are developed based on the best information available in the circumstances.
ASC 820 identifies fair value as the exchange price, or exit price, representing the amount that would be received to sell an asset or paid to transfer a liability in an orderly transaction between market participants. As a basis for considering market participant assumptions in fair value measurements, ASC 820 establishes a three‑tier fair value hierarchy that distinguishes between the following:
|
· |
Level 1—Quoted market prices in active markets for identical assets or liabilities. |
|
· |
Level 2—Inputs other than Level 1 inputs that are either directly or indirectly observable, such as quoted market prices, interest rates, and yield curves. |
|
· |
Level 3—Unobservable inputs developed using estimates of assumptions developed by the Company, which reflect those that a market participant would use. |
To the extent that the valuation is based on models or inputs that are less observable or unobservable in the market, the determination of fair value requires more judgment. Accordingly, the degree of judgment exercised by the Company in determining fair value is greatest for instruments categorized in Level 3. A financial instrument’s level within the fair value hierarchy is based on the lowest level of any input that is significant to the fair value measurement.
F-7
The carrying amounts reflected in the balance sheets for cash and cash equivalents, prepaid expenses and other current assets, accounts payable and accrued expenses approximate their fair values, due to their short‑term nature.
Cash and Cash Equivalents
The Company considers all highly liquid investments purchased with original maturities of 90 days or less at acquisition to be cash equivalents. Cash and cash equivalents include cash held in banks and amounts held in money market funds.
Marketable Securities
The Company classifies marketable debt securities with a remaining maturity of greater than three months when purchased as available‑for‑sale. Marketable debt securities with a remaining maturity date greater than one year and marketable equity securities are classified as non‑current where the Company has the intent and ability to hold these securities for at least the next 12 months. During 2016, the Company invested in a supplier and received common stock and warrants to purchase common stock in that entity. The common stock is considered an available-for-sale marketable equity security and is included in non-current marketable securities, and the warrants are included in non-current assets.
All available for sale securities are carried at fair value with the unrealized gains and losses included in other comprehensive income (loss) as a component of stockholders’ equity until realized. Any premium or discount arising at purchase is amortized and/or accreted to interest income and/or expense. Realized gains and losses are determined using the specific identification method and are included in other income (expense). If any adjustment to fair value reflects a decline in value of the investment, the Company considers all available evidence to evaluate the extent to which the decline is “other than temporary” and, if so, recognizes the loss through a charge to the Company’s statement of operations and comprehensive loss. No other than temporary losses have been recognized.
Cash, cash equivalents, and marketable securities as of December 31, 2017 and 2016 consist of the following:
|
|
|
Amortized |
|
Unrealized |
|
Unrealized |
|
Fair |
|
||||
|
|
|
Cost |
|
Gains |
|
Losses |
|
Value |
|
||||
|
|
|
(in thousands) |
|
||||||||||
|
As of December 31, 2017 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Money market funds included in cash and cash equivalents |
|
$ |
30,469 |
|
$ |
— |
|
$ |
— |
|
$ |
30,469 |
|
|
Marketable securities: |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
U.S. Treasury notes |
|
|
137,560 |
|
|
— |
|
|
38 |
|
|
137,522 |
|
|
Equity securities |
|
|
1,220 |
|
|
— |
|
|
120 |
|
|
1,100 |
|
|
Total marketable securities |
|
$ |
138,780 |
|
$ |
— |
|
$ |
158 |
|
$ |
138,622 |
|
|
Total money market funds and marketable securities |
|
$ |
169,249 |
|
$ |
— |
|
$ |
158 |
|
$ |
169,091 |
|
|
As of December 31, 2016 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Money market funds included in cash and cash equivalents |
|
$ |
36,003 |
|
$ |
— |
|
$ |
— |
|
$ |
36,003 |
|
|
Marketable securities: |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
U.S. Treasury notes |
|
|
130,237 |
|
|
2 |
|
|
66 |
|
|
130,173 |
|
|
U.S. Government agency bonds |
|
|
7,604 |
|
|
— |
|
|
— |
|
|
7,604 |
|
|
Total debt securities |
|
$ |
137,841 |
|
$ |
2 |
|
$ |
66 |
|
$ |
137,777 |
|
|
Equity securities |
|
|
1,220 |
|
|
140 |
|
|
— |
|
|
1,360 |
|
|
Total marketable securities |
|
$ |
139,061 |
|
$ |
142 |
|
$ |
66 |
|
$ |
139,137 |
|
|
Total money market funds and marketable securities |
|
$ |
175,064 |
|
$ |
142 |
|
$ |
66 |
|
$ |
175,140 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
All of the Company’s marketable debt securities at December 31, 2017 and 2016 have a contractual maturity of one year or less.
F-8
Restricted Cash
At December 31, 2017 and 2016, the Company maintained restricted cash totaling approximately $0.7 million held in the form of money market accounts as collateral for the Company’s facility lease obligation. The balance is included within deposits in other non‑current assets in the accompanying consolidated balance sheets.
Property and Equipment
Property and equipment consists of laboratory equipment, furniture and office equipment, and leasehold improvements and is stated at cost, less accumulated depreciation. Maintenance and repairs that do not improve or extend the lives of the respective assets are expensed to operations as incurred; while costs of major additions and betterments are capitalized. Depreciation is calculated over the estimated useful lives of the assets using the straight‑line method.
Impairment of Long‑Lived Assets
The Company evaluates long‑lived assets for potential impairment when events or changes in circumstances indicate the carrying value of the assets may not be recoverable. Recoverability is measured by comparing the book values of the assets to the expected future net undiscounted cash flows that the assets are expected to generate. If such assets are considered to be impaired, the impairment to be recognized is measured by the amount by which the book values of the assets exceed their fair value. The Company has not recognized any impairment losses from inception through December 31, 2017.
Revenue Recognition
As of December 31, 2017, all of the Company’s revenue is generated exclusively from its collaboration agreement with Sanofi Genzyme Corporation, a Sanofi company (“Sanofi Genzyme”).
The Company recognizes revenue in accordance with ASC Topic 605, Revenue Recognition (“ASC 605”). Accordingly, revenue is recognized for each unit of accounting when all of the following criteria are met:
|
· |
Persuasive evidence of an arrangement exists; |
|
· |
Delivery has occurred or services have been rendered; |
|
· |
The seller’s price to the buyer is fixed or determinable; and |
|
· |
Collectability is reasonably assured. |
Amounts received prior to satisfying the revenue recognition criteria are recorded as deferred revenue in the Company’s balance sheet. Amounts expected to be recognized as revenue within 12 months following the balance sheet date are classified as deferred revenue, current portion. Amounts not expected to be recognized as revenue within the 12 months following the balance sheet date are included in noncurrent liabilities and classified as deferred revenue, net of current portion.
The Company analyzes the multiple element arrangements based on the guidance in ASC Topic 605‑25, Revenue Recognition—Multiple Element Arrangements (“ASC 605‑25”). Pursuant to the guidance in ASC 605‑25, the Company evaluates multiple element arrangements to determine (1) the deliverables included in the arrangement and (2) whether the individual deliverables represent separate units of accounting or whether they must be accounted for as a combined unit of accounting. This evaluation involves subjective determinations and requires management to make judgments about the individual deliverables and whether such deliverables are separate from other aspects of the contractual relationship. Deliverables are considered separate units of accounting provided that: (i) the delivered item(s) has value to the customer on a standalone basis and (ii) if the arrangement includes a general right of return relative to the delivered item(s), delivery or performance of the undelivered item(s) is considered probable and substantially within control of the Company. In assessing whether an item has standalone value, the Company considers factors such as the research, manufacturing and commercialization capabilities of the collaboration partner and the availability of the associated expertise in the general marketplace. In addition, the Company considers whether the collaboration partner
F-9
can use the other deliverable(s) for their intended purpose without the receipt of the remaining element(s), whether the value of the deliverable is dependent on the undelivered item(s) and whether there are other vendors that can provide the undelivered element(s). The Company’s collaboration agreement does not contain a general right of return relative to any delivered items.
Arrangement consideration that is fixed or determinable is allocated among the separate units of accounting using the relative selling price method. Then the applicable revenue recognition criteria in ASC 605 are applied to each of the separate units of accounting in determining the appropriate period and pattern of recognition. The Company determines the selling price of a unit of accounting following the hierarchy of evidence prescribed by ASC 605‑25. Accordingly, the Company determines the estimated selling price for units of accounting within each arrangement using vendor specific objective evidence (“VSOE”) of selling price, if available, third-party evidence (“TPE”) of selling price if VSOE is not available, or best estimate of selling price (“BESP”) if neither VSOE or TPE is available. The Company has only used BESP to estimate the selling price, since it has not had VSOE or TPE of selling price of any units of accounting to date. Determining BESP for a unit of accounting requires significant judgment. In developing the BESP for a unit of accounting, the Company considers applicable market conditions and relevant entity specific factors, including factors that were contemplated in negotiating the agreement with the customer and estimated costs. The Company validates BESP for units of accounting by evaluating whether changes in the key assumptions used to determine the BESP will have a significant effect on the allocation of arrangement consideration between multiple units of accounting.
Options are considered substantive if, at the inception of the arrangement, the Company is at risk as to whether the collaboration partner will choose to exercise the option. Factors that the Company considers in evaluating whether an option is substantive include the cost to exercise the option, the overall objective of the arrangement, the benefit the collaborator might obtain from the arrangement without exercising the option and the likelihood the option will be exercised. When an option is considered substantive, the Company does not consider the option or item underlying the option to be a deliverable at the inception of the arrangement and the associated option fees are not included in allocable consideration, assuming the option is not priced at a significant and incremental discount. Conversely, when an option is not considered substantive, the Company would consider the option, including other deliverables contingent upon the exercise of the option, to be a deliverable at the inception of the arrangement and a corresponding amount would be included in allocable arrangement consideration. In addition, if the price of the option includes a significant incremental discount, the option would be included as a deliverable at the inception of the arrangement.
The Company recognizes arrangement consideration allocated to each unit of accounting when all of the revenue recognition criteria in ASC 605 are satisfied for that particular unit of accounting. The Company will recognize revenue associated with license options upon exercise of the option, if the underlying license has standalone value from the other deliverables to be provided subsequent to delivery of the license. If the license does not have standalone value, the amounts allocated to the license option will be combined with the related undelivered items as a single unit of accounting. The amounts allocated to the license option in the Sanofi Genzyme agreement will be deferred until the option is exercised. The revenue recognition upon option exercise will be determined based on whether the license has standalone value from the remaining deliverables under the arrangement at the time of exercise.
The Company recognizes the amounts associated with research and development services, alliance joint steering committees and development advisory committees ratably over the associated period of performance. If there is no discernible pattern of performance and/or objectively measurable performance measures do not exist, then the Company recognizes revenue under the arrangement on a straight‑line basis over the period the Company is expected to complete its performance obligations. Conversely, if the pattern of performance in which the service is provided to the customer can be determined and objectively measurable performance exist, then the Company recognizes revenue under the arrangement using the proportional performance method. Revenue recognized is limited to the lesser of the cumulative amount of payments received or the cumulative revenue earned determined using the straight line method or proportional performance, as applicable, as of the period end date.
F-10
At the inception of an arrangement that includes milestone payments, the Company evaluates whether each milestone is substantive and at risk to both parties on the basis of the contingent nature of the milestone. This evaluation includes an assessment of whether: (i) the consideration is commensurate with either the Company’s performance to achieve the milestone or the enhancement of the value of the delivered item(s) as a result of a specific outcome resulting from the Company’s performance to achieve the milestone, (ii) the consideration relates solely to past performance and (iii) the consideration is reasonable relative to all the deliverables and payment terms within the arrangement. The Company evaluates factors such as clinical, regulatory, commercial and other risks that must be overcome to achieve the respective milestone and the level of effort and investment required to achieve the respective milestone in making this assessment. There is considerable judgment involved in determining whether a milestone satisfies all the criteria required to conclude that a milestone is substantive. In accordance with ASC Topic 605‑28, Revenue Recognition—Milestone Method (“ASC 605‑28”) clinical and regulatory milestones that are considered substantive, will be recognized as revenue in their entirety upon successful accomplishment of the milestone, assuming all other revenue recognition criteria are met. Milestones that are not considered substantive would be recognized as revenue over the remaining period of performance, assuming all other revenue recognition criteria are met. Revenue from commercial milestone payments will be accounted for as royalties and recorded as revenue upon achievement of the milestone, assuming all other revenue recognition criteria are met.
The Company will recognize royalty revenue in the period of sale of the related product(s), based on the underlying contract terms, provided that the reported sales are reliably measurable and the Company has no remaining performance obligations, assuming all other revenue recognition criteria are met.
The Company also considers the impact of potential future payments it makes in its role as a vendor to its customers or collaboration partners and evaluates if these potential future payments could be reductions of revenue from that customer. If the potential future payments to the customer are (i) a separately identifiable benefit and (ii) the fair value of the identifiable benefit can be reasonably estimated, then the payments are accounted for separately from the revenue received from the customer. If however, both of these criteria are not satisfied, then the payments are treated as a reduction of revenue.
Research and Development
Research and development costs are charged to expense as incurred in performing research and development activities. The costs include employee compensation costs, external research, consultant costs, sponsored research, in‑kind services provided under the Sanofi Genzyme agreement, license fees, process development and facilities costs. Facilities costs primarily include the allocation of rent, utilities and depreciation.
Research Contract Costs and Accruals
The Company has entered into various research and development contracts with research institutions and other companies. These agreements are generally cancelable. The Company records accruals for estimated ongoing research costs. When evaluating the adequacy of the accrued liabilities, the Company analyzes progress of the studies, including the phase or completion of events, invoices received and contracted costs. Significant judgments and estimates may be made in determining the accrued balances at the end of any reporting period. Actual results could differ from the Company’s estimates. The Company’s historical accrual estimates have not been materially different from the actual costs.
Patent Costs
The Company expenses patent application and related legal costs as incurred and classifies such costs as general and administrative expenses in the accompanying statements of operations.
Stock‑Based Compensation Expense
The Company accounts for its stock‑based compensation awards in accordance with ASC Topic 718 Compensation—Stock Compensation (“ASC 718”). ASC 718 requires all stock‑based payments to employees and directors, including grants of restricted stock and stock options, to be recognized as expense in the statements of operations based on their grant date fair values. Grants of restricted stock and stock options to other service providers, referred to as non‑employees, are required to be recognized as expense in the statements of operations based on their
F-11
vesting date fair values. The Company estimates the fair value of options granted using the Black‑Scholes option pricing model. The Company uses the fair value of its common stock to determine the fair value of restricted stock awards.
The Black‑Scholes option pricing model requires inputs based on certain subjective assumptions, including (a) the expected stock price volatility, (b) the calculation of expected term of the award, (c) the risk‑free interest rate and (d) expected dividends. Due to a lack of company-specific historical and implied volatility data, the Company bases the estimate of expected volatility on the historical volatility of a group of similar companies that are publicly traded, blended with the most recent period of historic volatility of its common stock. The historical volatility is calculated based on a period of time commensurate with the expected term assumption. The computation of expected volatility is based on the historical volatility of a representative group of companies with similar characteristics to the Company, including stage of product development and life science industry focus. The Company uses the simplified method as prescribed by the SEC Staff Accounting Bulletin No. 107, Share‑Based Payment, to calculate the expected term for stock options granted to employees as it does not have sufficient historical exercise data to provide a reasonable basis upon which to estimate the expected term. For stock options granted to non‑employees, the Company utilizes the contractual term of the arrangement as the basis for the expected term assumption. The risk‑free interest rate is based on a treasury instrument whose term is consistent with the expected term of the stock options. The expected dividend yield is assumed to be zero as the Company has never paid dividends and has no current plans to pay any dividends on its common stock.
The Company expenses the fair value of its stock‑based compensation awards to employees on a straight‑line basis over the associated service period, which is generally the period in which the related services are received. Stock‑based compensation awards to non‑employees are adjusted through stock‑based compensation expense at each reporting period end to reflect the current fair value of such awards and are expensed on a straight‑line basis.
The Company records the expense for stock‑based compensation awards subject to performance conditions over the remaining service period when management determines that achievement of the performance condition is probable. Management evaluates when the achievement of a performance condition is probable based on the expected satisfaction of the performance conditions as of the reporting date.
Income Taxes
Income taxes are recorded in accordance with ASC Topic 740, Income Taxes (“ASC 740”), which provides for deferred taxes using an asset and liability approach. Under this method, deferred tax assets and liabilities are determined based on the difference between the financial reporting and the tax reporting basis of assets and liabilities and are measured using the enacted tax rates and laws that are expected to be in effect when the differences are expected to reverse. The Company provides a valuation allowance against net deferred tax assets unless, based upon the weight of available evidence, it is more likely than not that the deferred tax assets will be realized.
The Company accounts for uncertain tax positions in accordance with the provisions of ASC 740. When uncertain tax positions exist, the Company recognizes the tax benefit of tax positions to the extent that the benefit will more likely than not be realized. The determination as to whether the tax benefit will more likely than not be realized is based upon the technical merits of the tax position as well as consideration of the available facts and circumstances. As of December 31, 2017, the Company does not have any significant uncertain tax positions.
Comprehensive Loss
Comprehensive loss is comprised of net loss and other comprehensive income or loss. Other comprehensive gain or loss consists of unrealized gains or losses on marketable securities.
Net Loss Per Share Attributable to Common Stockholders
Basic net loss per share attributable to common stockholders is calculated by dividing the net loss attributable to common stockholders by the weighted‑average number of shares of common stock outstanding during the period, without consideration for potentially dilutive securities. Diluted net loss per share attributable to common stockholders is computed by dividing the net loss attributable to common stockholders by the weighted‑average number of shares of common stock and potentially dilutive securities outstanding for the period determined using the treasury‑stock and if‑converted methods.
F-12
For purposes of the diluted net loss per share attributable to common stockholders calculation, redeemable convertible preferred stock, unvested restricted common stock, and outstanding stock options are considered to be potentially dilutive securities, but are excluded from the calculation of diluted net loss per share attributable to common stockholders because their effect would be anti‑dilutive and therefore, basic and diluted net loss per share attributable to common stockholders were the same for all periods presented.
The following table sets forth the outstanding potentially dilutive securities that have been excluded in the calculation of diluted net loss per share attributable to common stockholders because to do so would be anti‑dilutive:
|
|
|
As of December 31, |
|
||||
|
|
|
2017 |
|
2016 |
|
2015 |
|
|
Unvested restricted common stock |
|
557,979 |
|
1,167,984 |
|
1,818,261 |
|
|
Shares reserved for issuance under stock plans |
|
5,375,431 |
|
4,226,265 |
|
2,905,458 |
|
|
Total |
|
5,933,410 |
|
5,394,249 |
|
4,723,719 |
|
All of the Company’s outstanding convertible preferred stock automatically converted into shares of common stock as of November 16, 2015, resulting in the issuance by the Company of an additional 17,647,054 shares of common stock.
Concentrations of Credit Risk and Off‑Balance Sheet Risk
The Company has no financial instruments with off‑balance sheet risk such as foreign exchange contracts, option contracts or other foreign hedging arrangements. Financial instruments that potentially subject the Company to a concentration of credit risk are cash and cash equivalents. The Company’s cash is held in accounts at a financial institution that may exceed federally insured limits. The Company has not experienced any credit losses in such accounts and does not believe it is exposed to any significant credit risk on these funds.
Concentration of Suppliers
The Company is dependent on a third‑party manufacturer to supply certain products for research and development activities in its programs. In particular, the Company relies on a sole manufacturer to supply it with specific vectors related to the Company’s research and development programs.
Segment Information
Operating segments are defined as components of an enterprise about which separate discrete information is available for evaluation by the chief operating decision maker in deciding how to allocate resources and assess performance. The Company and the Company’s chief operating decision maker, the Company’s Chief Executive Officer, views the Company’s operations and manages its business as a single operating segment, which is the business of developing and commercializing gene therapies.
Recent Accounting Pronouncements
In May 2014, the FASB issued ASU No. 2014-09, Revenue from Contracts with Customers (Topic 606) (“ASU 2014-09”). Subsequently, the FASB also issued ASU 2015-14, Revenue from Contracts with Customers (Topic 606), which adjusted the effective date of ASU 2014-09; ASU No. 2016-08, Revenue from Contracts with Customers (Topic 606): Principal versus Agent Considerations (Reporting Revenue Gross versus Net), which amends the principal-versus-agent implementation guidance and illustrations in ASU 2014-09; ASU No. 2016-10, Revenue from Contracts with Customers (Topic 606): Identifying Performance Obligations and Licensing, which clarifies identifying performance obligation and licensing implementation guidance and illustrations in ASU 2014-09; and ASU No. 2016-12, Revenue from Contracts with Customers (Topic 606): Narrow-Scope Improvements and Practical Expedients, which addresses implementation issues and is intended to reduce the cost and complexity of applying the new revenue standard in ASU 2014-09 (collectively, the “Revenue ASUs”).
The Revenue ASUs provide an accounting standard for a single comprehensive model for use in accounting for revenue arising from contracts with customers and supersedes most current revenue recognition guidance. The
F-13
accounting standard is effective for interim and annual periods beginning after December 15, 2017, with an option to early adopt for interim and annual periods beginning after December 15, 2016. The guidance permits two methods of adoption: retrospectively to each prior reporting period presented (the full retrospective method), or retrospectively with the cumulative effect of initially applying the guidance recognized at the date of initial application (the modified retrospective method).
As of December 31, 2017, the Company had one revenue generating arrangement, which was the Sanofi Genzyme Collaboration, as defined below. The Company has elected to adopt the Revenue ASUs effective as of January 1, 2018, under the modified retrospective method. The Company has substantially completed its assessment of the effect that this new standard will have on its consolidated financial statements. The most significant effect of the adoption is expected to be the method of revenue recognition for services performed over time. Under the previous accounting standards, revenue was recognized over the estimated period of performance while revenue will be recognized based on a proportional performance model under the Revenue ASUs. This change in accounting policy, along with certain other factors, is expected to result in an adjustment of approximately $18.0 million to $23.0 million, representing an increase of deferred revenue with an offset to accumulated deficit on January 1, 2018 to reflect the cumulative effect of the accounting changes made upon the adoption of the standard. In addition, the Company expects that the changes in accounting for contingent milestone payments will have a significant effect on the future accounting treatment for the arrangement. The previous accounting guidance contained specific guidance related to the accounting for milestone payments, including, if certain criteria were met, the ability to recognize all consideration related to the milestone once that milestone was achieved. The Revenue ASUs do not contain guidance specific to milestone payments, thereby requiring potential milestone payments to be considered in accordance with the overall revenue recognition model. As a result, revenue from contingent milestone payments may be recognized earlier under the Revenue ASUs than under ASC 605, based on an assessment of the probability of achievement of the milestone and the likelihood of a significant reversal of such milestone revenue at each reporting date. This assessment may result in recognizing milestone revenue before the milestone event has been achieved. As of the adoption date, no consideration from contingent milestones was included in the arrangement consideration. The finalization of the Company’s assessment may result in significant changes to its estimates that may materially impact its preliminary estimate of the cumulative effect. The Company has implemented appropriate changes to its internal controls to support revenue recognition and additional revenue-related disclosures under the new standards.
In October 2016, the FASB issued ASU No. 2016-16, Income Taxes (Topic 740): Intra-Entity Transfers of Assets Other Than Inventory (“ASU 2016-16”), which removes the prohibition in ASC 740 against the immediate recognition of the current and deferred income tax effects of intra-entity transfers of assets other than inventory. ASU 2016-16 is effective for the Company for annual periods beginning after December 15, 2017, and interim periods within those annual periods. Early adoption is permitted as of the beginning of a fiscal year for which neither the annual nor the interim (if applicable) financial statements have been issued. The Company is currently in the process of evaluating the impact that the adoption of this guidance will have on its consolidated financial statements and related disclosures.
In February 2016, the FASB issued ASU No. 2016-02, a comprehensive new lease accounting standard, which provides revised guidance on accounting for lease arrangements by both lessors and lessees and requires lessees to recognize a lease liability and a right-of-use asset for most leases. The new guidance is effective for fiscal years beginning after December 15, 2018, and interim periods within those fiscal years, with early adoption permitted. The new standard must be applied using a modified retrospective transition approach which requires application of the new guidance for all periods presented. The Company is currently in the process of evaluating the impact that the adoption of this guidance will have on its consolidated financial statements and related disclosures.
F-14
3. Fair value measurements
Assets and liabilities measured at fair value on a recurring basis as of December 31, 2017 and 2016 are as follows:
|
|
|
|
|
|
Quoted Prices |
|
Significant |
|
|
|
|
||
|
|
|
|
|
|
in Active |
|
Other |
|
Significant |
|
|||
|
|
|
|
|
|
Markets for |
|
Observable |
|
Unobservable |
|
|||
|
|
|
|
|
|
Identical Assets |
|
Inputs |
|
Inputs |
|
|||
|
Assets |
|
Total |
|
(Level 1) |
|
(Level 2) |
|
(Level 3) |
|
||||
|
|
|
(in thousands) |
|
||||||||||
|
December 31, 2017 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Money market funds included in cash and cash equivalents |
|
$ |
30,469 |
|
$ |
30,469 |
|
$ |
— |
|
$ |
— |
|
|
Marketable securities: |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
U.S. Treasury notes |
|
|
137,522 |
|
|
137,522 |
|
|
— |
|
|
— |
|
|
Equity securities |
|
|
1,100 |
|
|
1,100 |
|
|
— |
|
|
— |
|
|
Total marketable securities |
|
$ |
138,622 |
|
$ |
138,622 |
|
$ |
— |
|
$ |
— |
|
|
Warrants to purchase equity securities |
|
|
569 |
|
|
— |
|
|
569 |
|
|
— |
|
|
Total |
|
$ |
169,660 |
|
$ |
169,091 |
|
$ |
569 |
|
$ |
— |
|
|
December 31, 2016 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Money market funds included in cash and cash equivalents |
|
$ |
36,003 |
|
$ |
36,003 |
|
$ |
— |
|
$ |
— |
|
|
Marketable securities: |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
U.S. Treasury notes |
|
|
130,173 |
|
|
130,173 |
|
|
— |
|
|
— |
|
|
U.S. Government agency securities |
|
|
7,604 |
|
|
— |
|
|
7,604 |
|
|
— |
|
|
Equity securities |
|
|
1,360 |
|
|
1,360 |
|
|
— |
|
|
— |
|
|
Total marketable securities |
|
$ |
139,137 |
|
$ |
131,533 |
|
$ |
7,604 |
|
$ |
— |
|
|
Warrants to purchase equity securities |
|
|
792 |
|
|
— |
|
|
792 |
|
|
— |
|
|
Total |
|
$ |
175,932 |
|
$ |
167,536 |
|
$ |
8,396 |
|
$ |
— |
|
The Company measures the fair value of money market funds, U.S. Treasuries and equity securities based on quoted prices in active markets for identical securities. The Level 2 debt securities include U.S. Government agency securities that are valued either based on recent trades of securities in inactive markets or based on quoted market prices of similar instruments and other significant inputs derived from or corroborated by observable market data. The Level 2 equity securities include warrants used to purchase equity securities that are valued using the Black-Scholes model. The Black-Scholes option pricing model requires inputs based on certain subjective assumptions, including (a) the expected stock price volatility, (b) the calculation of expected term of the awards, (c) the risk-free interest rate, and (d) expected dividends. The assumptions utilized to value the warrants to purchase equity securities as of December 31, 2017 and 2016 are as follows:
|
|
|
As of December 31, |
|
||||
|
|
|
2017 |
|
2016 |
|
||
|
Risk-free interest rate |
|
2.0 |
% |
|
1.8 |
% |
|
|
Expected dividend yield |
|
— |
% |
|
— |
% |
|
|
Expected term (in years) |
|
3.7 |
|
|
4.7 |
|
|
|
Expected volatility |
|
103.5 |
% |
|
97.5 |
% |
|
The expected volatility is based on the historic volatility for the equity securities underlying the warrants and is calculated based on a period of time commensurate with the expected term assumption. The expected term is based on the remaining contractual life of the warrants on each measurement date. The risk-free interest rate is based on a treasury instrument whose term is consistent with the expected term of the warrants. The expected dividend yield is assumed to be zero as the entity that issued the warrants has never paid and has not indicated any intention to pay dividends.
F-15
4. Prepaid expenses and other current assets
Prepaid expenses and other current assets consist of the following:
|
|
|
As of December 31, |
|
||||
|
|
|
2017 |
|
2016 |
|
||
|
|
|
(in thousands) |
|
||||
|
Prepaid research and development contracts |
|
$ |
1,330 |
|
$ |
1,094 |
|
|
Other current assets |
|
|
766 |
|
|
541 |
|
|
Prepaid insurance |
|
|
520 |
|
|
430 |
|
|
Accrued interest receivable |
|
|
122 |
|
|
339 |
|
|
Tenant improvement receivable |
|
|
— |
|
|
1,964 |
|
|
Total |
|
$ |
2,738 |
|
$ |
4,368 |
|
5. Property and equipment, net
Property and equipment, net consists of the following:
|
|
|
As of December 31, |
|
||||
|
|
|
2017 |
|
2016 |
|
||
|
|
|
(in thousands) |
|
||||
|
Leasehold improvements |
|
$ |
6,421 |
|
$ |
1,341 |
|
|
Laboratory equipment |
|
|
5,262 |
|
|
3,306 |
|
|
Furniture and office equipment |
|
|
1,565 |
|
|
526 |
|
|
Other |
|
|
25 |
|
|
242 |
|
|
Construction in progress |
|
|
— |
|
|
3,873 |
|
|
Total property and equipment |
|
|
13,273 |
|
|
9,288 |
|
|
Less: accumulated depreciation |
|
|
(2,990) |
|
|
(1,395) |
|
|
Property and equipment, net |
|
$ |
10,283 |
|
$ |
7,893 |
|
The Company recorded $1.6 million, $0.6 million, and $0.6 million in depreciation expense during the years ended December 31, 2017, 2016, and 2015, respectively. Construction-in-progress as of December 31, 2016 includes $3.0 million related to costs which were reimbursable by the landlord. Refer to Note 7 “Commitments and contingencies” for further details.
6. Accrued expenses
Accrued expenses consist of the following:
|
|
|
As of December 31, |
|
||||
|
|
|
2017 |
|
2016 |
|
||
|
|
|
(in thousands) |
|
||||
|
Research and development costs |
|
$ |
5,780 |
|
$ |
2,384 |
|
|
Employee compensation costs |
|
|
3,383 |
|
|
2,399 |
|
|
Professional services |
|
|
1,762 |
|
|
698 |
|
|
Accrued goods and services |
|
|
388 |
|
|
842 |
|
|
Patent costs |
|
|
120 |
|
|
89 |
|
|
Other |
|
|
64 |
|
|
76 |
|
|
Total |
|
$ |
11,497 |
|
$ |
6,488 |
|
7. Commitments and contingencies
Operating Leases
During March 2014, the Company entered into an agreement to lease the 75 Sidney Street facility under a non‑cancelable operating lease that would expire December 15, 2019. The lease includes two renewal options, each for
F-16
five-year terms and at fair market value upon exercise. The lease contains escalating rent clauses which require higher rent payments in future years. The Company expenses rent on a straight‑line basis over the term of the lease, including any rent‑free periods.
In January 2016, the Company executed an amendment to extend the 75 Sidney Street lease and executed an agreement to lease the 64 Sidney Street facility until December 31, 2024. The additional facility includes laboratory and office space, and was ready for occupancy in early 2017.
In February 2018, the Company executed an amendment to lease an additional approximately 11,000 square feet at 75 Sidney Street that is intended to support its continued growth. The additional facility includes laboratory and office space, and will be ready for occupancy in the first half of 2018.
The table below includes estimated payments related to the amended 75 Sidney Street lease and the lease for 64 Sidney Street as of December 31, 2017 and does not include the effect of the amendment executed in February 2018.
The Company has received leasehold improvement incentives from the landlord totaling $1.3 million and $3.5 million for 75 Sidney Street and 64 Sidney Street, respectively, as of December 31, 2017. The Company recorded these incentives as a component of deferred rent and is amortizing these incentives as a reduction of rent expense over the life of the lease. The leasehold improvements have been recorded as fixed assets. The Company is entitled to receive approximately $0.3 million of leasehold improvements for the space related to the amendment of the lease executed in February 2018.
Rent expense of approximately $2.9 million, $2.0 million, and $0.9 million was incurred during the years ended December 31, 2017, 2016, and 2015, respectively.
Future annual minimum lease payments at December 31, 2017 are as follows:
|
|
|
Total Minimum |
|
|
|
|
|
Lease Payments |
|
|
|
|
|
(in thousands) |
|
|
|
2018 |
|
|
3,290 |
|
|
2019 |
|
|
3,382 |
|
|
2020 |
|
|
3,762 |
|
|
2021 |
|
|
3,868 |
|
|
2022 |
|
|
3,977 |
|
|
2023+ |
|
|
8,295 |
|
|
|
|
$ |
26,574 |
|
.
Significant Agreements
Sanofi Genzyme Collaboration Agreement
Summary of Agreement
In February 2015, the Company entered into an agreement with Sanofi Genzyme (the “Sanofi Genzyme Collaboration Agreement”) which included a non‑refundable upfront payment of $65.0 million. In addition, contemporaneous with entering into the Sanofi Genzyme Collaboration Agreement, Sanofi Genzyme entered into a Series B Stock Purchase Agreement, under which Sanofi Genzyme purchased 10,000,000 shares of Series B Preferred Stock for $30.0 million. The fair value of the Series B Preferred Stock at the time of issuance was approximately $25.0 million. The $5.0 million premium over the fair value is accounted for as additional consideration under the Sanofi Genzyme Collaboration Agreement.
Under the Sanofi Genzyme Collaboration Agreement, the Company granted Sanofi Genzyme an exclusive option to license, develop and commercialize (i) ex‑U.S. rights to the following programs, which are referred to as Split Territory Programs; VY‑AADC (“Parkinson’s Program”), VY‑FXN01 (“Friedreich’s Ataxia Program”), a future program to be designated by Sanofi Genzyme (“Future Program), and VY‑HTT01 (“Huntington’s Program”), with an incremental option to co‑commercialize VY‑HTT01 in the United States and (ii) worldwide rights to VY‑SMN101
F-17
(“Spinal Muscular Atrophy Program”). Sanofi Genzyme’s option for the Split Territory Programs and the Spinal Muscular Atrophy Program is triggered following the completion of the first proof‑of‑principle human clinical study (“POP Study”), on a program by program basis.
Prior to any option exercise by Sanofi Genzyme, the Company will collaborate with Sanofi Genzyme in the development of products under each Split Territory Program and the Spinal Muscular Atrophy Program pursuant to a written development plan and under the guidance of an Alliance Joint Steering Committee (“AJSC”), comprised of an equal number of employees from the Company and Sanofi Genzyme.
The Company is required to use commercially reasonable efforts to develop products under each Split Territory Program and the Spinal Muscular Atrophy Program through the completion of the applicable POP Study. During the development of these joint programs, the activities are guided by a Development Advisory Committee (“DAC”). The DAC may elect to utilize certain Sanofi Genzyme technology relating to the Parkinson’s Program, the Huntington’s Program or generally with the manufacture of Split Territory Program products.
The Company is solely responsible for all costs incurred in connection with the development of the Split Territory Programs and the Spinal Muscular Atrophy Program products prior to the exercise of an option by Sanofi Genzyme with the exception of the following: (i) at the Company’s request and upon mutual agreement, Sanofi Genzyme will provide “in‑kind” services valued at up to $5.0 million and (ii) Sanofi Genzyme shall be responsible for the costs and expenses of activities under the Huntington’s Program development plan to the extent such activities are covered by financial support Sanofi Genzyme is entitled to receive from a patient advocacy group, collectively Sanofi Genzyme “in‑kind” and other funding.
Other than the Parkinson’s Program (for which a POP Study has already been completed), if the Company does not initiate a POP Study for a given Split Territory Program by December 31, 2026 (or for the Future Program by the tenth anniversary of the date the Future Program is nominated by Sanofi Genzyme), and Sanofi Genzyme has not terminated the Sanofi Genzyme Collaboration Agreement with respect to the collaboration program, then Sanofi Genzyme shall be entitled, as its sole and exclusive remedy, to a credit of $10.0 million for each such program against other milestone or royalty payments payable by Sanofi Genzyme under the Sanofi Genzyme Collaboration Agreement. However, if the POP Study is not initiated due to a regulatory delay or a force majeure event, such time period shall be extended for so long as such delay continues.
With the exception of the Parkinson’s Program, Sanofi Genzyme is required to pay an option exercise payment of $20.0 million or $30.0 million for each Split Territory Program, as well as the Spinal Muscular Atrophy Program.
Upon Sanofi Genzyme’s exercise of its option to license a given product in a Split Territory Program (“Split Territory Licensed Product”), the Company will have sole responsibility for the development of such Split Territory Licensed Product in the United States and Sanofi Genzyme shall have sole responsibility for development of such Split Territory Licensed Product in the rest of the world. The Company and Sanofi Genzyme will have shared responsibility for execution of ongoing development of such Split Territory Licensed Product that is not specific to either territory, including costs associated therewith. The Company is responsible for all commercialization activities relating to Split Territory Licensed Products in the United States, including all of the associated costs. Sanofi Genzyme is responsible for all commercialization activities relating to the Split Territory Licensed Products in the rest of the world, including all of the associated costs. If Sanofi Genzyme exercised its co‑commercialization rights, Sanofi Genzyme will be the lead party responsible for all commercialization activities related to Huntington’s Licensed Product in the United States.
Upon exercise of the option, Sanofi Genzyme shall have the sole right to develop the Spinal Muscular Atrophy Product worldwide. Sanofi Genzyme shall be responsible for all of the development costs that occur after the option exercise date for the Spinal Muscular Atrophy Program. Sanofi Genzyme is also responsible for commercialization activities relating to the Spinal Muscular Atrophy Product worldwide.
Sanofi Genzyme is required to pay the Company for specified regulatory and commercial milestones, if achieved, up to $540.0 million across all programs. The Company is no longer entitled to receive a total of $105.0 million related to regulatory and commercial milestone payments for VY-AADC as a result of Sanofi Genzyme’s decision to not exercise its option for the Parkinson’s Program (the “PD Opt-Out”). The regulatory approval milestones are payable upon either regulatory approval in the United States or regulatory and reimbursement approval in the European Union and range from $40.0 million to $50.0 million per milestone, with an aggregate total of $220.0 million,
F-18
after accounting for the PD Opt-Out. The commercial milestones are payable upon achievement of specified annual net sales in each program and range from $50.0 million to $100.0 million per milestone, with an aggregate total of $320.0 million, after accounting for the PD Opt-Out.
In addition, to the extent any Split Territory Licensed Products or the Spinal Muscular Atrophy Licensed Product are commercialized, the Company is entitled to tiered royalty payments ranging from the mid‑single digits to mid‑teens based on a percentage of net sales by Sanofi Genzyme. Sanofi Genzyme is entitled to receive tiered royalty payments related to sales of Split Territory Licensed Product ranging from the low‑single digits to mid‑single digits based on a percentage of net sales by the Company depending on whether the Company uses Sanofi Genzyme technology in the Split Territory Licensed Product. If Sanofi Genzyme elects to co‑commercialize VY‑HTT01 in the United States, the Company and Sanofi Genzyme will share in any profits or losses from VY‑HTT01 product sales.
The Sanofi Genzyme Collaboration Agreement will continue in effect until the later of (i) the expiration of the last to expire of the option rights and (ii) the expiration of all payment obligations unless sooner terminated by the Company or Sanofi Genzyme. The Company and Sanofi Genzyme have customary termination rights including the right to terminate for an uncured material breach of the agreement committed by the other party and Sanofi Genzyme has the right to terminate for convenience.
Accounting Analysis
The Sanofi Genzyme Collaboration Agreement includes the following deliverables: (i) research and development services for each of the Split Territory License Programs and the Spinal Muscular Atrophy Program, (ii) participation in the AJSC, (iii) participation in the DAC and (iv) the option to obtain a development and commercial license in the Parkinson’s Program and related deliverables. The Company has determined that the option to obtain a development and commercial license in the Parkinson’s program is not a substantive option for accounting purposes, primarily because there is no additional option exercise payment payable by Sanofi Genzyme at the time the option is exercised. Therefore, the option to obtain a license and other obligations of the Company that are contingent upon exercise of the option are considered deliverables at the inception of the arrangement. The options in the other Split Territory Programs and the Spinal Muscular Atrophy Program are considered substantive as there is substantial option exercise payments payable by Sanofi Genzyme upon exercise. In addition, as a result of the uncertainties related to the discovery, research, development and commercialization activities, the Company is at risk with regard to whether Sanofi Genzyme will exercise the options. Moreover, the substantive options are not priced at a significant incremental discount. Accordingly, the substantive options are not considered deliverables at the inception of the arrangement and the associated option exercise payments are not included in allocable arrangement consideration. The Company has also determined that any obligations which are contingent upon the exercise of a substantive option are not considered deliverables at the outset of the arrangement, as these deliverables are contingent upon the exercise of the options. In addition, any option exercise payments associated with the substantive options are not included in the allocable arrangement consideration.
The Company has concluded that each of the deliverables identified at the inception of the arrangement has standalone value from the other undelivered elements. Additionally, the Sanofi Genzyme Collaboration Agreement does not include return rights related to the initial collaboration term. Accordingly, each deliverable qualifies as a separate unit of accounting.
The Company has identified $79.3 million of allocable arrangement consideration consisting of the $65.0 million upfront fee, the $5.0 million premium paid in excess of fair value of the Series B Preferred Stock and $9.3 million of Sanofi Genzyme “in‑kind” and other funding.
The Company has allocated the allocable arrangement consideration based on the relative selling price of each unit of accounting. For all units of accounting, the Company determined the selling price using the BESP. The Company determined the BESP for the service related deliverable for the research and development activities based on internal estimates of the costs to perform the services, including expected internal expenses and expenses with third parties for services and supplies, marked up to include a reasonable profit margin and adjusted for the scope of the potential license. Significant inputs used to determine the total expense of the research and development activities include, the length of time required and the number and costs of various studies that will be performed to complete the POP Study. The BESP for the AJSC and DAC have been estimated based on the costs incurred to participate in the committees, marked up to
F-19
include a reasonable profit margin. The BESP for the license option was determined based on the estimated value of the license and related deliverables adjusted for the estimated probability that the option would be exercised by Sanofi Genzyme.
Based on the relative selling price allocation, the allocable arrangement consideration was allocated as follows:
|
|
|
|
|
|
|
Unit of Accounting |
|
Amount |
|
|
|
|
|
(in thousands) |
|
|
|
Research and Development Services for: |
|
|
|
|
|
Huntington’s Program |
|
$ |
15,662 |
|
|
Parkinson’s Program |
|
|
6,648 |
|
|
Friedreich’s Ataxia Program |
|
|
16,315 |
|
|
Spinal Muscular Atrophy Program |
|
|
32,050 |
|
|
Future Program |
|
|
2,464 |
|
|
Committee Obligations: |
|
|
|
|
|
AJSC |
|
|
147 |
|
|
DAC |
|
|
227 |
|
|
License Option and related deliverables |
|
|
5,743 |
|
|
Total |
|
$ |
79,256 |
|
The Company recognizes the amounts associated with research and development services on a straight-line basis over the period of service as there is no discernable pattern or objective measure of performance for the services. Similarly, the Company recognizes the amount associated with the committee obligations on a straight-line basis over the period of service consistent with the expected pattern of performance. The amount allocated to the license option was deferred until October 2017, when Sanofi Genzyme decided that it would not exercise its option to the Parkinson’s Program (the “PD Option”).
In October 2017, Sanofi Genzyme decided not to exercise the PD Option. Therefore, in the year ended December 31, 2017, the Company recognized revenue of $5.5 million of consideration which had been allocated to the PD Option. In addition, revenue recognized during the years ended December 31, 2017 and 2016 include amounts recognized related to consideration allocated to research and development services for various programs under the Sanofi Genzyme Collaboration Agreement. During 2017 the Company reassessed the estimated period of performance for each of the units of accounting and determined that the estimated period would be extended for two units of accounting. During 2016 the Company deprioritized the development of VY-SMN101 for the treatment of Spinal Muscular Atrophy. As a result, the Company ceased recognizing the revenue allocated to this program. These adjustments were made on a prospective basis and resulted in decreases in revenue recognized by $2.1 million and $9.5 million, respectively, for the year ended December 31, 2017.
The Company has evaluated all of the milestones that may be received in connection with the Split Territory Licensed Product and the Spinal Muscular Atrophy Program Licensed Product. In evaluating if a milestone is substantive, the Company assesses whether: (i) the consideration is commensurate with either the Company’s performance to achieve the milestone or the enhancement of the value of the delivered item(s) as a result of a specific outcome resulting from the Company performance to achieve the milestone, (ii) the consideration relates solely to past performance and (iii) the consideration is reasonable relative to all of the deliverables and payment terms within the arrangement. All regulatory milestones are considered substantive on the basis of the contingent nature of the milestone, specifically reviewing factors such as the scientific, clinical, regulatory, and other risks that must be overcome to achieve the milestone as well as the level of effort and investment required. Accordingly, such amounts will be recognized as revenue in full in the period in which the associated milestone is achieved, assuming all other revenue recognition criteria are met. All commercial milestones will be accounted for in the same manner as royalties and recorded as revenue upon achievement of the milestone, assuming all other revenue recognition criteria are met.
During the years ended December 31, 2017, 2016, and 2015, the Company recognized $10.1 million, $14.2 million, and $17.3 million, respectively, of revenue associated with its collaboration with Sanofi Genzyme related to research and development services performed during the period and for consideration allocated to the PD Option, which was recognized during 2017. As of December 31, 2017, there is $31.6 million of deferred revenue related to the Sanofi
F-20
Genzyme Collaboration Agreement, which is classified as either current or noncurrent in the accompanying balance sheet based on the period the services are expected to be delivered.
Costs incurred relating to the programs that Sanofi Genzyme has the option to license under the Sanofi Genzyme Collaboration Agreement consist of internal and external research and development costs, which primarily include: salaries and benefits, lab supplies and preclinical research studies. All costs are included in research and development expenses in the Company’s statement of operations during the year ended December 31, 2017. The Company estimates that the majority of research and development expense during the period relate to programs for which Sanofi Genzyme had or has an option right.
MRI Interventions License and Securities Purchase Agreements
Summary of Agreement
In September 2016, the Company entered into securities purchase and license agreements with MRI Interventions, Inc. (“MRIC”). MRIC is the primary supplier of the ClearPoint System, which is being used by the Company in ongoing development and clinical trials. The Company paid $2.0 million for shares of MRIC common stock and a warrant to purchase additional shares of MRIC common stock under a securities purchase agreement. The license agreement provided for certain rights to MRIC technology and for MRIC to transfer the rights and know-how to manufacture the ClearPoint System to enable the Company to utilize an alternative supplier for the ClearPoint System for use in the Company’s development and clinical trials.
Accounting Analysis
During the three months ended March 31, 2017, the Company terminated the license agreement with MRIC, and all prior and future commitments and obligations under such agreement became null and void. As of December 31, 2017, the Company continued to hold the common stock and warrants to purchase additional shares of common stock as an available-for-sale security and non-current asset, respectively.
Other Agreements
During 2017, 2016, and 2015, the Company entered into various agreements with contract research organizations and institutions to license intellectual property. In consideration for the licensed rights the Company generally made upfront payments, which were recorded as research and development expense as the acquired technologies were considered in‑process research and development. During the years ended December 31, 2017, 2016, and 2015, the Company paid $0.3 million, $0.6 million, and $0.1 million, respectively, in upfront license fees. The license agreements also obligate the Company to make additional payments that are contingent upon specific clinical trial and regulatory approval milestones being achieved as well as royalties on future product sales. The agreements to license intellectual property include potential milestone payments that are dependent upon the development of products licensed under the agreements and contingent upon the achievement of clinical trial or regulatory approval milestones. The maximum aggregate potential milestone payments payable by the Company total approximately $18.0 million. Additionally, under the terms of one agreement, the Company has options to license intellectual property to be used in the development of therapies for four additional disease indications. If the Company exercises all of the options under the agreement, it would be obligated to pay aggregate upfront fees of up to approximately $1.6 million and milestone payments that are contingent upon clinical trial results and regulatory approval of $5.0 million per disease indication, or up to $20.0 million in total. As of December 31, 2017 and 2016, there have been no milestones achieved. The Company can generally terminate the license agreements upon 30‑90 days prior written notice.
F-21
Additionally, certain license agreements require the Company to reimburse the licensor for certain past and ongoing patent related expenses. During the year ended December 31, 2017, 2016, and 2015, the Company incurred $0.8 million, $1.8 million, and $0.3 million of expense, respectively, related to these reimbursable patent costs which are recorded as general and administrative expense
During September 2016, the Company entered into a research and development funding arrangement with a non-profit organization that provides up to $4.0 million in funding to the Company upon the achievement of clinical and development milestones. The agreement provides that the Company repay amounts received under certain circumstances including termination of the agreement, and to pay an amount up to 2.6 times the funding received upon successful development and commercialization of any products developed. During 2017, the Company earned a milestone payment of $1.0 million. The Company has evaluated the arrangement and has concluded that it represents a research and development financing arrangement as it is probable that the Company will repay amounts received under the arrangement. As a result, the $1.0 million earned through 2017 is recorded as a non-current liability in the consolidated balance sheet.
Litigation
The Company is not a party to any litigation and does not have contingency reserves established for any litigation liabilities as of December 31, 2017 or December 31, 2016.
8. Redeemable convertible preferred stock
In November 2015, upon the closing of the Company’s IPO, all issued and outstanding redeemable convertible preferred stock was automatically converted into 17,647,054 shares of common stock, see Note 2.
The Company’s redeemable convertible preferred stock (“Preferred Stock”), has been classified as temporary equity on the accompanying balance sheets instead of in stockholders’ deficit in accordance with authoritative guidance for the classification and measurement of redeemable securities as the redeemable convertible preferred stock is redeemable at the option of the holder after the redemption date, February 2021.
The Company has authorized preferred stock amounting to 5,000,000 shares as of December 31, 2017 and 2016. The authorized preferred stock was classified under stockholders’ equity at December 31, 2017.
Series A Preferred Stock
The Company issued 45,000,000 shares of Series A Preferred Stock during 2014 and 2015. These shares were issued at various closings in 2014 and 2015 for $1.00 per share. The shares were issued in exchange for cash proceeds of $42.0 million, net of issuance costs of $32.0 thousand, and the exchange of outstanding redeemable Convertible Notes, including accrued interest, of approximately $2.9 million.
Tranche Rights Issued with Series A Preferred Stock
Included in the terms of the January 2014 Series A Preferred Stock Purchase Agreement were certain rights (“Tranche Rights”), granted to the investors of Series A Preferred Stock purchased in January 2014, including the holders of the redeemable Convertible Notes who exchanged the redeemable Convertible Notes. The Tranche Rights obligated the investors in Series A Preferred Stock to purchase and the Company to sell an additional 18,500,000 shares of Series A Preferred Stock at $1.00 per share contingent upon successful near term in licensing and progress on initial experiments and research and development planning (“Tranche Right I”). In addition, the investors were obligated to purchase, and the Company was obligated to sell an additional 20,000,000 shares of Series A Preferred Stock upon the development of project engine and achievement of certain clinical milestones (“Tranche Right II”). In addition, the Tranche Rights allowed the investors the ability to purchase the additional shares at their option at any time. The Tranche Rights were transferrable by the investors, subject to approval by the Board.
The Company has concluded the Tranche Rights meet the definition of a freestanding financial instrument, as the Tranche Rights were legally detachable and separately exercisable from the Series A Preferred Stock. Therefore, the Company allocated the proceeds between the Tranche Rights and the Series A Preferred Stock. As the Series A Preferred
F-22
Stock was redeemable at the holder’s option, the Tranche Rights were classified as an asset or liability and were initially recorded at fair value. The Tranche Rights were measured at fair value at each reporting period. Since the Tranche Rights were subject to fair value accounting, the Company allocated the proceeds to the Tranche Rights based on the fair value at the date of issuance with the remaining proceeds being allocated to the Series A Preferred Stock. The estimated fair value of the Tranche Rights was determined using a probability weighted present value model that considers the probability of closing a tranche, the estimated future value of Series A Preferred Stock each closing, and the investment required at each closing. Future values were converted to present value using a discount rate appropriate for probability adjusted cash flows.
Tranche Right I was initially recorded as an asset of $1.5 million as the purchase price of the additional shares was greater than the estimated value of the Series A Preferred Stock at the expected settlement date. The Company issued 18,500,000 additional shares under Tranche Right I, in three separate closings during the year ended December 31, 2014 with total proceeds of $18.5 million, net of issuance costs. Prior to each closing, any change in the value of Tranche Right I was recorded as other financing expense. The fair value of the portion of the Tranche Right I settled at each closing was reclassified to Series A Preferred Stock. Tranche Right II was initially recorded as a liability of $4.1 million as the purchase price of the additional shares was less than the estimated price of the Series A Preferred Stock at the expected settlement date. In February 2015, Tranche Right II was settled when the Company closed the final issuance of Series A Preferred Stock. The Company recognized expense of $9.8 million related to the mark to market of Tranche Right II during the year ended December 31, 2015, which was included in other financing expense. The fair value of the Tranche Right II settled at closing was reclassified to Series A Preferred Stock. The initial carrying amount of the Series A Preferred Stock issued upon the closing of Tranche Right II amounted to approximately $36.1 million which exceeded the redemption value, therefore the carrying value was not subsequently adjusted. However, the Company reflected accrued dividends of approximately $1.2 million related to this issuance in the net loss attributable to common stockholders for the year ended December 31, 2015.
Series B Preferred Stock
The Company issued 30,000,001 shares of Series B Preferred Stock during 2015. These shares were issued for $3.00 per share. This issuance resulted in cash proceeds of $89.8 million, net of issuance costs of $0.2 million. Additionally, a discount of $5.0 million was recorded against the proceeds as the amount paid by Sanofi Genzyme was in excess of fair value of the Series B Preferred Stock at issuance.
9. Common stock
As of December 31, 2017 and 2016, the Company had authorized 120,000,000 shares of Common Stock, at $0.001 par value per share.
General
The voting, dividend and liquidation rights of the holders of the Common Stock are subject to and qualified by the rights, powers and preferences of the holders of Preferred Stock. The Common Stock has the following characteristics:
Voting
The holders of shares of Common Stock are entitled to one vote for each share of Common Stock held at all meetings of stockholders and written actions in lieu of meetings.
Dividends
The holders of shares of Common Stock are entitled to receive dividends, if and when declared by the Board of Directors. No dividends have been declared or paid by the Company since its inception.
F-23
Liquidation
The holders of shares of Common Stock are entitled to share ratably in the Company’s remaining assets available for distribution to its stockholders in the event of any voluntary or involuntary liquidation, dissolution or winding up of the Company or upon occurrence of a deemed liquidation event.
Shares Reserved For Future Issuance
|
|
|
As of December 31, |
|
||
|
|
|
2017 |
|
2016 |
|
|
Shares reserved for vesting of restricted stock awards under the Founder Agreements |
|
366,914 |
|
628,679 |
|
|
Shares reserved for vesting of restricted stock awards under the 2014 Option and Stock Plan |
|
191,065 |
|
539,305 |
|
|
Shares reserved for exercise of stock options |
|
3,143,566 |
|
1,871,237 |
|
|
Shares reserved for issuances under the 2015 Stock Option Plan |
|
1,501,005 |
|
1,825,174 |
|
|
Shares reserved for issuances under the 2015 Employee Stock Purchase Plan |
|
730,860 |
|
529,854 |
|
|
|
|
5,933,410 |
|
5,394,249 |
|
10. Stock‑based compensation
2015 Stock Option Plan
In October 2015, the Company’s board of directors and stockholders approved the 2015 Stock Option and Incentive Plan “(2015 Stock Option Plan”), which became effective upon the completion of the IPO. The 2015 Stock Option Plan provides the Company with the flexibility to use various equity-based incentive and other awards as compensation tools to motivate its workforce. These tools include stock options, stock appreciation rights, restricted stock, restricted stock units, unrestricted stock, performance share awards and cash-based awards. The 2015 Stock Option Plan replaced the 2014 Plan (as defined below). Any options or awards outstanding under the 2014 Plan remained outstanding and effective. The number of shares initially reserved for issuance under the 2015 Stock Option Plan is the sum of (i) 1,311,812 shares of common stock and (ii) the number of shares under the 2014 Plan that are not needed to fulfill the Company’s obligations for awards issued under the 2014 Plan as a result of forfeiture, expiration, cancellation, termination or net issuances of awards thereunder. The number of shares of common stock that may be issued under the 2015 Stock Option Plan is also subject to increase on the first day of each fiscal year by up to 4% of the Company’s issued and outstanding shares of common stock on the immediately preceding December 31.
Effective January 1, 2016, 2017, and 2018 an additional 1,069,971, 1,070,635, and 1,285,200 shares, respectively, were added to the Company’s 2015 Stock Option Plan for future issuance. During the year ended December 31, 2017, the Company issued 1,700,000 stock options to employees and directors and 20,000 stock options to non‑employees. As of December 31, 2017, there were 1,501,005 shares available for future issuance under the 2015 Stock Option Plan.
2014 Stock Option and Grant Plan
In January 2014, the Company adopted the 2014 Stock Option and Grant Plan (the “2014 Plan”), under which it could grant incentive stock options, non‑qualified stock options, restricted stock awards, unrestricted stock awards, or restricted stock units to purchase up to 823,529 shares of Common Stock to employees, officers, directors and consultants of the Company.
In April 2014, the Company amended the Plan to allow for the issuance of up to 1,411,764 shares of Common Stock. In August 2014, April 2015, August 2015 and October 2015 the Company further amended the Plan to allow for the issuance of up to 2,000,000, 2,047,058, 2,669,411 and 2,998,823 shares of Common Stock, respectively. During 2014 the Company issued only restricted stock awards under the Plan and during 2015 the Company only granted stock options.
The terms of stock awards agreements, including vesting requirements, were determined by the Board of Directors and were subject to the provisions of the 2014 Plan. Restricted stock awards granted by the Company generally vest based on each grantee’s continued service with the Company during a specified period following grant. Awards
F-24
granted to employees generally vest over four years, with 25% vesting on the one year anniversary and 75% vesting ratably, on a monthly basis, over the remaining three years. Awards granted to non‑employee consultants generally vest monthly over a period of one to four years.
Founder Awards
In January 2014, the Company issued 1,188,233 shares of restricted stock to its Founders at an original issuance price of $0.0425 per share. Of the total restricted shares awarded to the Founders, 835,292 shares generally vest over one to four years, based on each Founder’s continued service to the Company in varying capacity as a Scientific Advisory Board member, consultant, director, officer or employee, as set forth in each grantee’s individual restricted stock purchase agreement.
The remaining 352,941 of the shares issued will begin vesting upon the achievement of certain performance objectives as well as continued service to the Company, as set forth in the agreements. These performance conditions are tied to certain milestone events specific to the Company’s corporate goals, including but not limited to preclinical and clinical development milestones related to the Company’s product candidates. Stock‑based compensation expense associated with these performance‑based awards will be recognized when the achievement of the performance condition is considered probable, using management’s best estimates. Management concluded that the achievement of the performance milestone for one of the three performance-based awards had been met during 2016. Accordingly, stock‑based compensation expense in the amount of $1.4 million and $1.1 million was recorded in the years ended December 31, 2017 and 2016, respectively. No stock-based compensation expense was recorded related to the performance-based awards in the year ended December 31, 2015.
2015 Employee Stock Purchase Plan
In October 2015, the Company’s board of directors and stockholders approved the 2015 Employee Stock Purchase Plan (the “2015 ESPP”). Under the 2015 ESPP, all full-time employees of the Company are eligible to purchase common stock of the Company twice per year, at the end of each six-month payment period. During each payment period, eligible employees who so elect, may authorize payroll deductions in an amount of 1% to 10% (whole percentages only) of the employee’s base pay for each payroll period. At the end of each payment period, the accumulated deductions are used to purchase shares of common stock from the Company at a discount. A total of 262,362 shares of common stock were initially authorized for issuance under this plan. The 2015 ESPP became effective upon the completion of the IPO. Effective January 1, 2016, 2017, and 2018, a total of 267,492, 267,658, and 321,300 shares of common stock, respectively, were added to the 2015 ESPP. The Company issued 66,652 shares of common stock under the 2015 ESPP in the year ended December 31, 2017.
Stock-based Compensation Expense
Total compensation cost recognized for all stock-based compensation awards in the statements of operations and comprehensive loss is as follows:
|
|
|
Year ended December 31, |
|
|||||||
|
|
|
2017 |
|
2016 |
|
2015 |
|
|||
|
|
|
(in thousands) |
|
|||||||
|
Research and development |
|
$ |
5,367 |
|
$ |
4,296 |
|
$ |
3,218 |
|
|
General and administrative |
|
|
3,871 |
|
|
2,014 |
|
|
809 |
|
|
Total stock-compensation expense |
|
$ |
9,238 |
|
$ |
6,310 |
|
$ |
4,027 |
|
F-25
Restricted Stock
A summary of the status of and changes in unvested restricted stock was as follows:
|
|
|
|
|
Weighted |
|
|
|
|
|
|
|
Average |
|
|
|
|
|
|
|
Grant Date |
|
|
|
|
|
|
|
Fair Value |
|
|
|
|
|
Shares |
|
Per Share |
|
|
|
Unvested restricted common stock as of December 31, 2016 |
|
1,167,984 |
|
$ |
0.76 |
|
|
Issued |
|
— |
|
|
|
|
|
Vested |
|
(573,803) |
|
$ |
0.77 |
|
|
Repurchased |
|
(36,202) |
|
$ |
0.67 |
|
|
Unvested restricted common stock as of December 31, 2017 |
|
557,979 |
|
$ |
0.70 |
|
The expense related to awards granted to employees and non‑employees was $0.5 million and $2.7 million, respectively, for the year ended December 31, 2017. The expense related to awards granted to employees and non-employees was $0.5 million and $2.6 million, respectively, for the year ended December 31, 2016. The expense related to awards granted to employees and non-employees was $0.5 million and $2.6 million, respectively, for the year ended December 31, 2015.
As of December 31, 2017, the Company had unrecognized stock‑based compensation expense related to its unvested restricted stock awards of $4.5 million, which is expected to be recognized over the remaining weighted average vesting period of 0.38 years.
Stock Options
A summary of the status of, and changes in, stock options was as follows:
|
|
|
|
|
Weighted |
|
Remaining |
|
Aggregate |
|
||
|
|
|
|
|
Average |
|
Contractual |
|
Intrinsic |
|
||
|
|
|
|
|
Exercise |
|
Life |
|
Value |
|
||
|
|
|
Shares |
|
Price |
|
(in years) |
|
(in thousands) |
|
||
|
Outstanding at December 31, 2016 |
|
1,871,237 |
|
$ |
10.21 |
|
|
|
|
|
|
|
Granted |
|
1,720,000 |
|
$ |
13.07 |
|
|
|
|
|
|
|
Exercised |
|
(158,677) |
|
$ |
8.59 |
|
|
|
|
|
|
|
Cancelled or forfeited |
|
(288,994) |
|
$ |
10.50 |
|
|
|
|
|
|
|
Outstanding at December 31, 2017 |
|
3,143,566 |
|
$ |
11.82 |
|
8.6 |
|
$ |
15,991 |
|
|
Exercisable at December 31, 2017 |
|
955,587 |
|
$ |
10.45 |
|
8.1 |
|
$ |
5,933 |
|
|
Vested and expected to vest at December 31, 2017 |
|
3,143,566 |
|
$ |
11.82 |
|
8.6 |
|
$ |
15,991 |
|
Using the Black‑Scholes option pricing model, the weighted average fair value of options granted to employees and directors during the year ended December 31, 2017 was $8.48. The stock-based compensation expense related to stock option awards granted to employees and directors was $5.5 million, $3.0 million, and $0.7 million for the years ended December 31, 2017, 2016, and 2015, respectively.
The fair value of each option issued to employees and directors was estimated at the date of grant using the Black‑Scholes option pricing model with the following weighted‑average assumptions:
|
|
|
Year ended December 31, |
|
|||||||
|
|
|
2017 |
|
2016 |
|
2015 |
|
|||
|
Risk-free interest rate |
|
2.0 |
% |
|
1.5 |
% |
|
1.6 |
% |
|
|
Expected dividend yield |
|
— |
% |
|
— |
% |
|
— |
% |
|
|
Expected term (in years) |
|
6.0 |
|
|
6.0 |
|
|
6.0 |
|
|
|
Expected volatility |
|
73.7 |
% |
|
73.1 |
% |
|
78.6 |
% |
|
F-26
Using the Black‑Scholes option pricing model, the weighted average grant date fair value of options granted to non‑employees during the year ended December 31, 2017 was $6.88. Unvested options granted to non‑employees are revalued at each measurement period until they vest. The expense related to stock option awards granted to non‑employees was $0.4 million, $0.2 million, and $0.3 million for the years ended December 31, 2017, 2016, and 2015, respectively. As of December 31, 2017, the Company had unrecognized stock‑based compensation expense related to its unvested stock options of $16.1 million which is expected to be recognized over the remaining weighted average vesting period of 2.66 years.
The fair value of each option issued to non‑employees was estimated at each vesting and reporting date using the Black‑Scholes option pricing model. The reporting date fair value was determined using the following weighted‑average assumptions:
|
|
|
As of December 31, |
|
|||||||
|
|
|
2017 |
|
2016 |
|
2015 |
|
|||
|
Risk-free interest rate |
|
2.4 |
% |
|
2.1 |
% |
|
2.0 |
% |
|
|
Expected dividend yield |
|
— |
% |
|
— |
% |
|
— |
% |
|
|
Expected term (in years) |
|
8.5 |
|
|
9.1 |
|
|
10.0 |
|
|
|
Expected volatility |
|
76.2 |
% |
|
83.3 |
% |
|
84.0 |
% |
|
11. 401(k) Savings plan
The Company has a defined‑contribution savings plan under Section 401(k) of the Internal Revenue Code (the “401(k) Plan”). The 401(k) Plan covers all employees who meet defined minimum age and service requirements, and allows participants to defer a portion of their annual compensation on a pretax basis. The Company expensed approximately $0.5 million and $0.3 million related to employer contributions made during the years ended December 31, 2017 and 2016, respectively. The Company did not make any contributions to the 401(k) Plan during 2015.
12. Income taxes
The Company recognizes deferred tax assets and liabilities for the expected future tax consequences of events that have been recognized in the Company’s financial statements or tax returns. Under this method, deferred tax assets and liabilities are determined based on differences between the financial statement carrying amounts and the tax bases of the assets and liabilities using the enacted tax rates in effect in the years in which the differences are expected to reverse. A valuation allowance against deferred tax assets is recorded if, based on the weight of the available evidence, it is more likely than not that some or all of the deferred tax assets will not be realized. The Company accounts for uncertain tax positions using a more-likely-than-not threshold for recognizing and resolving uncertain tax positions. The evaluation of uncertain tax positions is based on factors including, but not limited to, changes in the law, the measurement of tax positions taken or expected to be taken in tax returns, the effective settlement of matters subject to audit, new audit activity, and changes in facts or circumstances related to a tax position. The Company evaluates its tax positions on an annual basis.
On December 22, 2017, legislation commonly known as the Tax Cuts and Jobs Act (the “Tax Act”) was signed into law. The Tax Act, among other changes, reduces the U.S. federal corporate tax rate from 34% to 21%, requires taxpayers to pay a one-time transition tax on earnings of certain foreign subsidiaries that were previously tax deferred and creates new taxes on certain foreign sourced earnings. As of December 31, 2017, the Company did not have any foreign subsidiaries and the international aspects of the Tax Act are not applicable.
In connection with the initial analysis on the impact of the Tax Act, the Company remeasured certain deferred tax assets and liabilities based on the rates at which they are expected to reverse in the future, which is generally 21%. The remeasurement of the Company's deferred tax balance was primarily offset by application of its valuation allowance. However, the reduction of the U.S. federal corporate tax rate resulted in increases to the amounts reflected in “Deferred Rate Change” and “Change in valuation allowance” captions for the year ended December 31, 2017 in the Company’s tax reconciliation table compared to those amounts disclosed for the years ended December 31, 2016 and 2015. The
F-27
change in the U.S. federal corporate tax rate, which is effective January 1, 2018, is also reflected in the Company’s deferred tax table.
The Company is still in the process of analyzing the impact to the Company of the Tax Act. On December 22, 2017, the SEC staff issued SAB 118 to address the application of GAAP in situations when a registrant does not have the necessary information available, prepared, or analyzed (including computations) in reasonable detail to complete the accounting for certain income tax effects of the Tax Act. The Company has recognized the provisional tax impacts related to the revaluation of the deferred tax assets and liabilities and included these amounts in its consolidated financial statements for the year ended December 31, 2017. The ultimate impact may differ from these provisional amounts due to, among other things, additional analysis, changes in interpretations and assumptions the Company has made, additional regulatory guidance that may be issued, and actions the Company may take as a result of the Tax Act, which could result in changes to the provisional tax impacts during 2018.
The provision for income taxes is as follows:
|
|
Year ended December 31, |
|
||||
|
|
2017 |
|
2016 |
|
||
|
|
(in thousands) |
|
||||
|
Current |
|
|
|
|
|
|
|
Federal |
$ |
— |
|
$ |
180 |
|
|
State |
|
— |
|
|
— |
|
|
Total current |
|
— |
|
|
180 |
|
|
Deferred |
|
|
|
|
|
|
|
Federal |
|
— |
|
|
(111) |
|
|
State |
|
— |
|
|
(17) |
|
|
Total deferred |
|
— |
|
|
(128) |
|
|
Total tax expense |
$ |
— |
|
$ |
52 |
|
A reconciliation of the expected income tax (benefit) computed using the federal statutory income tax rate at the Company’s effective tax rate is as follows:
|
|
Year ended December 31, |
|
|
|||||||
|
|
2017 |
|
2016 |
|
2015 |
|
|
|||
|
Income tax computed at federal statutory tax rate |
|
34.0 |
% |
|
34.0 |
% |
|
34.0 |
% |
|
|
State taxes, net of federal benefit |
|
6.1 |
% |
|
5.6 |
% |
|
4.1 |
% |
|
|
General business credit carryovers |
|
5.0 |
% |
|
4.2 |
% |
|
3.1 |
% |
|
|
Non-deductible expenses |
|
(4.1) |
% |
|
(4.0) |
% |
|
(15.5) |
% |
|
|
Deferred rate change |
|
(21.8) |
% |
|
— |
% |
|
— |
% |
|
|
Change in valuation allowance |
|
(19.2) |
% |
|
(40.2) |
% |
|
(25.7) |
% |
|
|
Total |
|
— |
% |
|
(0.4) |
% |
|
— |
% |
|
The Company has incurred net operating losses (“NOLs”) since June 2013. At December 31, 2017, the Company had federal and state net operating loss carryforwards of $89.8 million and $91.7 million, respectively, which expire beginning in 2033. As of December 31, 2017, the Company also had federal and state research and development tax credit carryforwards of $6.6 million and $2.3 million, respectively, which expire beginning in 2028. As of December 31, 2017, the Company had state investment credits of $0.3 million, which expire beginning in 2018.
Under the provisions of the Internal Revenue Code, certain substantial changes in the Company’s ownership may result in a limitation on the amount of NOL carryforwards and research and development credit carryforwards that may be utilized annually to offset future taxable income and taxes payable. In general, an ownership change, as defined by Section 382, results from transactions that increase the ownership of 5% stockholders or public groups in the stock of a corporation by more than 50 percent in the aggregate over a three-year period. During 2016, the Company completed a study through June 30, 2016, to determine whether any ownership change has occurred since the Company’s formation and has determined that transactions have resulted in three ownership changes, as defined by Section 382. There could be
F-28
additional ownership changes in the future that could further limit the amount of NOLs and tax credit carryforwards that the Company can utilize.
The significant components of the Company’s deferred tax assets and (liabilities) as of December 31, 2017 and 2016 are as follows:
|
|
Year ended December 31, |
|
||||
|
|
2017 |
|
2016 |
|
||
|
|
(in thousands) |
|
||||
|
Deferred tax assets: |
|
|
|
|
|
|
|
Net operating loss carryforwards |
$ |
24,642 |
|
$ |
8,927 |
|
|
Tax credit carryforwards |
|
8,832 |
|
|
4,284 |
|
|
Deferred rent |
|
1,458 |
|
|
1,964 |
|
|
Deferred revenue |
|
8,622 |
|
|
16,333 |
|
|
Non-deductible expenses |
|
817 |
|
|
714 |
|
|
Intangibles |
|
832 |
|
|
998 |
|
|
Stock compensation |
|
1,361 |
|
|
672 |
|
|
Total deferred tax assets |
|
46,564 |
|
|
33,892 |
|
|
Less valuation allowance |
|
(44,953) |
|
|
(31,361) |
|
|
Net deferred tax assets |
|
1,611 |
|
|
2,531 |
|
|
Deferred tax liabilities |
|
|
|
|
|
|
|
Depreciation and amortization |
|
(1,611) |
|
|
(2,501) |
|
|
Unrealized gain on available-for-sale securities |
|
— |
|
|
(30) |
|
|
Net deferred taxes |
$ |
— |
|
$ |
— |
|
As required by ASC 740, management has evaluated the positive and negative evidence bearing upon the realizability of its deferred tax assets, which principally comprise NOL carryforwards, research and development credit carryforwards, and capitalized license and organization costs. Management has determined that it is more likely than not that the Company will not recognize the benefits of its federal and state deferred tax assets, and as a result, a valuation allowance of $45.0 million and $31.4 million has been established at December 31, 2017 and 2016, respectively. The change in valuation allowance was $13.6 million for the year ended December 31, 2017, primarily due to additional operating losses incurred by the Company for the year ended December 31, 2017, partially offset by the federal rate reduction from 34% to 21% as a result of the Tax Act. The primary reason for the difference between the income tax expense recorded by the Company and the amount of income tax expense at statutory income tax rates was the change in the valuation allowance.
At December 31, 2017 and 2016, the Company had no unrecognized tax benefits. The Company has not as yet conducted a study of its research and development credit carryforwards. This study may result in an adjustment to the Company’s research and development credit carryforwards; however, until a study is completed, and any adjustment is known, no amounts are being presented as an uncertain tax position. A full valuation allowance has been provided against the Company’s research and development credits, and if an adjustment is required, this adjustment would be offset by an adjustment to the valuation allowance. Thus, there would be no impact to the balance sheets or statements of operations if an adjustment were required.
Interest and penalty charges, if any, related to unrecognized tax benefits would be classified as income tax expense in the accompanying statements of operations. As of December 31, 2017 and 2016, the Company has no accrued interest related to uncertain tax positions. Since the Company is in a loss carryforward position, it is generally subject to examination by the U.S. federal, state, and local income tax authorities for all tax years in which a loss carryforward is available.
13. Related‑party transactions
Since inception, the Company received consulting and management services from one of its investors. The total amount of consulting and management services provided by this investor was approximately $31.8 thousand, $0.1 million, and $1.3 million during the years ended December 31, 2017, 2016, and 2015, respectively.
F-29
During the years ended December 31, 2017, 2016, and 2015, the Company recognized $10.1 million, $14.2 million, and $17.3 million, respectively, of revenue associated with its collaboration with Sanofi Genzyme related to research and development services provided during these periods. The Company also recognized $0.1 million, $1.2 million, and $2.3 million of expense during the years ended December 31, 2017, 2016, and 2015, respectively, related to in‑kind services provided by Sanofi Genzyme associated with the collaboration arrangement.
14. Selected quarterly financial data (unaudited)
The following table contains quarterly financial information for 2017 and 2016. The Company believes that the following information reflects all normal recurring adjustments necessary for a fair statement of the information for the periods presented. The operating results for any quarter are not necessarily indicative of results for any future period.
|
|
2017 |
|
|||||||||||||
|
|
First |
|
Second |
|
Third |
|
Fourth |
|
|
|
|||||
|
|
Quarter |
|
Quarter |
|
Quarter |
|
Quarter |
|
Total |
|
|||||
|
|
(amounts in thousands, except per share data) |
|
|||||||||||||
|
Collaboration revenue |
$ |
1,464 |
|
$ |
1,177 |
|
$ |
1,148 |
|
$ |
6,346 |
|
$ |
10,135 |
|
|
Total operating expenses |
|
18,986 |
|
|
19,816 |
|
|
24,503 |
|
|
18,693 |
|
|
81,998 |
|
|
Loss from operations |
|
(17,522) |
|
|
(18,639) |
|
|
(23,355) |
|
|
(12,347) |
|
|
(71,863) |
|
|
Net loss attributable to common stockholders |
|
(16,648) |
|
|
(18,876) |
|
|
(23,346) |
|
|
(11,828) |
|
|
(70,698) |
|
|
Net loss per share applicable to common stockholders – basic and diluted |
$ |
(0.65) |
|
$ |
(0.73) |
|
$ |
(0.89) |
|
$ |
(0.40) |
|
$ |
(2.64) |
|
|
|
2016 |
|
|||||||||||||
|
|
First |
|
Second |
|
Third |
|
Fourth |
|
|
|
|||||
|
|
Quarter |
|
Quarter |
|
Quarter |
|
Quarter |
|
Total |
|
|||||
|
|
(amounts in thousands, except per share data) |
|
|||||||||||||
|
Collaboration revenue |
$ |
4,830 |
|
$ |
3,720 |
|
$ |
3,308 |
|
$ |
2,362 |
|
$ |
14,220 |
|
|
Total operating expenses |
|
12,297 |
|
|
13,338 |
|
|
13,679 |
|
|
16,205 |
|
|
55,519 |
|
|
Loss from operations |
|
(7,467) |
|
|
(9,618) |
|
|
(10,371) |
|
|
(13,843) |
|
|
(41,299) |
|
|
Net loss attributable to common stockholders |
|
(7,188) |
|
|
(9,335) |
|
|
(8,996) |
|
|
(14,674) |
|
|
(40,193) |
|
|
Net loss per share applicable to common stockholders – basic and diluted |
$ |
(0.29) |
|
$ |
(0.37) |
|
$ |
(0.35) |
|
$ |
(0.57) |
|
$ |
(1.59) |
|
15. Subsequent events
Lease Amendment
In February 2018, the Company executed an amendment to lease an additional approximately 11,000 square feet at 75 Sidney Street that is intended to support its continued growth. The additional facility includes laboratory and office space, and will be ready for occupancy in the first half of 2018.
AbbVie Collaboration
In February 2018, the Company entered into an exclusive collaboration and option agreement with AbbVie Biotechnology Ltd (“AbbVie”), for the research, development, and commercialization of AAV and other virus-based gene therapy products for the treatment of diseases of the central nervous system and other neurodegenerative diseases related to defective or excess aggregation of tau protein in the human brain, including Alzheimer’s disease. Under the terms of the agreement, the Company received an upfront payment of $69.0 million and may receive future development and regulatory milestone payments and royalties. Under the terms of the agreement, the Company will perform specified research, preclinical, and Phase 1 development activities regarding vectorized antibodies directed against tau, after which AbbVie may select one or more vectorized antibodies to proceed into IND-enabling studies and clinical development. The Company will be responsible for the research, IND-enabling, and Phase 1 clinical trial activities and costs. Following the completion of Phase 1 clinical development, AbbVie has an option to license the vectorized tau antibody program and would then lead further clinical development and global commercialization for the product candidates pursuant to the agreement. The Company has an option to share in the costs of clinical development for higher royalty
F-30
rates. In addition to the upfront and potential option exercise payments, the Company is eligible to receive up to $895.0 million in development and regulatory milestones for each vectorized tau antibody compound. The Company is also eligible to receive tiered, escalating royalties in a range, subject to certain specified exceptions, from a high-single digit to a mid-to-high teen percentage of the global net sales of the vectorized antibodies for tauopathies, including Alzheimer's disease and other neurodegenerative diseases. Under the terms of the agreement, each party will own the entire right, title, and interest in and to all know-how and patent rights first made or invented solely by it or its affiliates or its or their sublicensees in the course of the collaboration, with certain specified exceptions. The Company has agreed to grant AbbVie worldwide license to certain know-how and patent rights developed by us or jointly by the parties arising from the collaboration.
EXHIBIT INDEX
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Incorporated by Reference to: |
||||||
|
Exhibit |
|
Description |
|
Form or |
|
Exhibit |
|
Filing |
|
SEC File |
|
|
|
|
|
|
|
|
|
|
|
|
|
1.1 |
|
Sales Agreement by and between the Registrant and Cowen and Company, LLC, dated as of December 1, 2016. |
|
S-3 |
|
1.2 |
|
12/01/2016 |
|
333-207367 |
|
|
|
|
|
|
|
|
|
|
|
|
|
3.1 |
|
Amended and Restated Certificate of Incorporation of the Registrant. |
|
8-K |
|
3.1 |
|
11/16/2015 |
|
001-37625 |
|
|
|
|
|
|
|
|
|
|
|
|
|
3.2 |
|
|
8-K |
|
3.2 |
|
11/16/2015 |
|
001-37625 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
4.1 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
4.2 |
|
Form of Indenture to be entered into between the Registrant and Trustee. |
|
S-3/A |
|
4.2 |
|
12/19/2016 |
|
333-207367 |
|
|
|
|
|
|
|
|
|
|
|
|
|
10.1# |
|
2014 Stock Option and Grant Plan and forms of award agreements thereunder. |
|
S-1/A |
|
10.1 |
|
10/28/2015 |
|
333-207367 |
|
|
|
|
|
|
|
|
|
|
|
|
|
10.2# |
|
2015 Stock Option and Incentive Plan and forms of award agreements thereunder. |
|
S-1/A |
|
10.2 |
|
10/28/2015 |
|
333-207367 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
S-1/A |
|
10.3 |
|
11/06/2015 |
|
333-207367 |
||
|
|
|
|
|
|
|
|
|
|
|
|
|
10.4† |
|
|
S-1 |
|
10.4 |
|
|
333-207367 |
||
|
|
|
|
|
|
|
|
|
|
|
|
|
10.5 |
|
|
|
10.5 |
|
|
333-207367 |
|||
|
|
|
|
|
|
|
|
|
|
|
|
|
10.6 |
|
First Amendment to Lease Agreement by and between the Registrant and 45/75 Sidney Street, LLC, dated as of December 23, 2015. |
|
10-Q |
|
|
05/12/2016 |
|
||
F-31
F-32
|
23.1 |
|
Consent of Ernst & Young, Independent Registered Public Accounting Firm. |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
24.1 |
|
Power of Attorney (see signature page of this Annual Report on Form 10-K) |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
31.1 |
|
Certification of Chief Executive Officer pursuant to Exchange Act Rules 13a-14 or 15d-14. |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
31.2 |
|
Certification of Chief Financial Officer pursuant to Exchange Act Rules 13a-14 or 15d-14. |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
32.1+ |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
101.INS |
|
XBRL Instance Document. |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
101.SCH |
|
XBRL Taxonomy Extension Schema Document. |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
101.CAL |
|
XBRL Taxonomy Extension Calculation Document. |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
101.LAB |
|
XBRL Taxonomy Extension Definition Linkbase Document. |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
101.PRE |
|
XBRL Taxonomy Extension Labels Linkbase Document. |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
101.DEF |
|
XBRL Taxonomy Extension Presentation Link Document. |
|
|
|
|
|
|
|
|
#Management contract or compensatory plan or arrangement filed in response to Item 15(a)(3) of the Instructions to the Annual Report on Form 10-K.
†Confidential treatment has been granted as to certain portions, which portions have been omitted and separately filed with the Securities and Exchange Commission.
††Confidential treatment has been requested as to certain portions, which portions have been omitted and separately filed with the Securities and Exchange Commission.
+The certification furnished in Exhibit 32.1 hereto is deemed to be furnished with this Annual Report on Form 10-K and will not be deemed to be “filed” for purposes of Section 18 of the Securities Exchange Act of 1934, as amended, except to the extent that the Registrant specifically incorporates it by reference.
F-33
Pursuant to the requirements of Section 13 or 15(d) of the Securities Exchange Act of 1934, the registrant has duly caused this Form 10-K to be signed on its behalf by the undersigned, thereunto duly authorized.
|
|
|
|
|
|
|
|
March 14, 2018 |
VOYAGER THERAPEUTICS, INC. |
||
|
By: |
/s/Steven Paul, M.D.
Steven Paul, M.D. |
|||
SIGNATURES AND POWER OF ATTORNEY
We, the undersigned directors and officers of Voyager Therapeutics, Inc. (the “Company”), hereby severally constitute and appoint Steven Paul, M.D. and Jane Henderson, and each of them singly, our true and lawful attorneys, with full power to them, and to each of them singly, to sign for us and in our names in the capacities indicated below, any and all amendments to this Annual Report on Form 10-K, and to file or cause to be filed the same, with all exhibits thereto and other documents in connection therewith, with the Securities and Exchange Commission, granting unto said attorneys, and each of them, full power and authority to do and perform each and every act and thing requisite and necessary to be done in connection therewith, as fully to all intents and purposes as each of us might or could do in person, and hereby ratifying and confirming all that said attorneys, and each of them, or their substitute or substitutes, shall do or cause to be done by virtue of this Power of Attorney.
Pursuant to the requirements of the Securities Exchange Act of 1934, this Annual Report on Form 10-K has been signed by the following persons in the capacities and on the dates indicated.
|
Name |
|
Title |
|
Date |
|
|
|
|
|
|
|
/s/Steven Paul, M.D. |
|
Chief Executive Officer, President, and Director |
|
March 14, 2018 |
|
Steven Paul, M.D. |
|
(Principal Executive Officer) |
|
|
|
|
|
|
|
|
|
/s/Jane Henderson |
|
Chief Financial Officer and Senior Vice President of Corporate Development |
|
March 14, 2018 |
|
Jane Henderson |
|
(Principal Financial and Accounting Officer) |
|
|
|
|
|
|
|
|
|
/s/Mark Levin |
|
Director |
|
March 14, 2018 |
|
Mark Levin |
|
|
|
|
|
|
|
|
|
|
|
/s/Jim Geraghty |
|
Director |
|
March 14, 2018 |
|
Jim Geraghty |
|
|
|
|
|
|
|
|
|
|
|
/s/Michael Higgins |
|
Director |
|
March 14, 2018 |
|
Michael Higgins |
|
|
|
|
|
|
|
|
|
|
|
/s/Perry A. Karsen |
|
Director |
|
March 14, 2018 |
|
Perry A. Karsen |
|
|
|
|
|
|
|
|
|
|
|
/s/Steven Hyman, M.D. |
|
Director |
|
March 14, 2018 |
|
Steven Hyman, M.D. |
|
|
|
4 |
|
|
|
|
|
|
|
/s/Wendy Dixon, Ph.D. |
|
Director |
|
March 14, 2018 |
|
Wendy Dixon, Ph. D. |
|
|
|
|
|
|
|
|
|
|
|
/s/Glenn Pierce, M.D., Ph.D. |
|
Director |
|
March 14, 2018 |
|
Glenn Pierce, M.D., Ph.D. |
|
|
|
|
F-34
