Attached files
| file | filename |
|---|---|
| EX-23.1 - CONSENT OF INDEPENDENT REGISTERED PUBLIC ACCOUNTING FIRM - RadNet, Inc. | radnet_10k-ex2301.htm |
| EX-32.2 - CERTIFICATION - RadNet, Inc. | radnet_10k-ex3202.htm |
| EX-32.1 - CERTIFICATION - RadNet, Inc. | radnet_10k-ex3201.htm |
| EX-31.2 - CERTIFICATION - RadNet, Inc. | radnet_10k-ex3102.htm |
| EX-31.1 - CERTIFICATION - RadNet, Inc. | radnet_10k-ex3101.htm |
| EX-21.1 - SUBSIDIARIES - RadNet, Inc. | radnet_10k-ex2101.htm |
| EX-12.1 - COMPUTATION OF RATION OF EARNINGS TO FIXED CHARGES - RadNet, Inc. | radnet_10k-ex1201.htm |
UNITED STATES
SECURITIES AND EXCHANGE COMMISSION
Washington D.C. 20549
FORM 10-K
ANNUAL REPORT PURSUANT TO SECTION 13 OR 15(d) OF THE SECURITIES EXCHANGE ACT OF 1934
For the fiscal year ended December 31, 2017
Commission File Number 001-33307
RadNet, Inc.
(Exact name of registrant as specified in its charter)
| Delaware | 13-3326724 |
(State or other jurisdiction of incorporation or organization) |
(I.R.S. Employer Identification No.) |
| 1510 Cotner Avenue | |
| Los Angeles, California | 90025 |
| (Address of principal executive offices) | (Zip Code) |
Registrant’s telephone number, including area code: (310) 478-7808
Securities registered pursuant to Section 12(b) of the Act:
| Title of Each Class | Name of each exchange on which registered |
| Common Stock, $.0001 par value | NASDAQ Global Market |
Securities registered pursuant to Section 12(g) of the Act: None
Indicate by check mark if the registrant is a well-known seasoned issuer, as defined in Rule 405 of the Securities Act. Yes ¨ No x
Indicate by check mark if the registrant is not required to file reports pursuant to Section 13 or Section 15(d) of the Act. Yes ¨ No x
Indicate by check mark whether the registrant (1) has filed all reports required to be filed by Section 13 or 15(d) of the Securities Exchange Act of 1934 during the preceding 12 months (or for such shorter period that the registrant was required to file such reports), and (2) has been subject to such filing requirements for the past 90 days. Yes x No ¨
Indicate by check mark whether the registrant has submitted electronically and posted on its corporate Website, if any, every Interactive Data File required to be submitted and posted pursuant to Rule 405 of Regulation S-T (§232.405 of this chapter) during the preceding 12 months (or for such shorter period that the registrant was required to submit and post such files). Yes x No ¨
Indicate by check mark if disclosure of delinquent filers pursuant to Item 405 of Regulation S-K (§229.405 of this chapter) is not contained herein, and will not be contained, to the best of registrant’s knowledge, in definitive proxy or information statements incorporated by reference in Part III of this Form 10-K or any amendment to this Form 10-K. x
Indicate by check mark whether the registrant is a large accelerated filer, an accelerated filer, a non-accelerated filer, or a smaller reporting company. See the definitions of “large accelerated filer,” “accelerated filer”, “smaller reporting company”, and “emerging growth company” in Rule 12b-2 of the Exchange Act. (Check one):
| Large accelerated filer | o | Accelerated filer | þ |
| Non-accelerated filer | o (Do not check if a smaller reporting company) | Smaller reporting company | o |
| Emerging growth company | o |
If an emerging growth company, indicate by check mark if the registrant has elected not to use the extended transition period for complying with any new or revised financial accounting standards provided pursuant to Section 13(a) of the Exchange Act. ¨
Indicate by check mark whether the registrant is a shell company (as defined in Rule 12b-2 of the Act) Yes ¨ No x
The aggregate market value of the registrant’s common stock held by non-affiliates of the registrant was approximately $335,616,695 on June 30, 2017 (the last business day of the registrant’s most recently completed second quarter) based on the closing price for the common stock on the NASDAQ Global Market on June 30, 2017.
The number of shares of the registrant’s common stock outstanding on March 5, 2018, was 48,232,117.
DOCUMENTS INCORPORATED BY REFERENCE
Portions of the registrant’s definitive proxy statement for the 2018 Annual Meeting of Stockholders are incorporated herein by reference in Part III of this annual report on Form 10-K to the extent stated herein. Such proxy statement will be filed with the Securities and Exchange Commission pursuant to Regulation 14A not later than 120 days after the close of the registrant’s fiscal year.
RADNET, INC.
| i |
Cautionary Note Regarding Forward-Looking Statements
This annual report contains forward-looking statements within the meaning of Section 27A of the Securities Act of 1933, as amended and Section 21E of the Securities Exchange Act of 1934, as amended. Forward-looking statements reflect current views about future events and are based on our currently available financial, economic and competitive data and on current business plans. Actual events or results may differ materially depending on risks and uncertainties that may affect our operations, markets, services, prices and other factors.
Statements in this annual report concerning our ability to successfully acquire and integrate new operations, to grow our contract management business, our financial guidance, our future cost saving efforts, our increased business from new equipment or operations and our ability to finance our operations are forward-looking statements. In some cases, you can identify forward-looking statements by terminology such as “may,” “will,” “should,” “expect,” “intend,” “plan,” “anticipate,” “believe,” “estimate,” “predict,” “potential,” “continue,” “assumption” or the negative of these terms or other comparable terminology.
Forward-looking statements involve known and unknown risks, uncertainties and other factors that may cause our actual results, levels of activity, performance or achievements to be materially different from any future results, levels of activity, performance or achievements expressed or implied by these forward-looking statements. These risks include those factors listed in Item 1 — “Business,” Item 1A— “Risk Factors,” Item 3— “Legal Proceedings,” Item 7 — “Management’s Discussion and Analysis of Financial Condition and Results of Operations” and elsewhere in this annual report and in other reports that we file with the Securities and Exchange Commission.
We do not undertake any responsibility to release publicly any revisions to these forward-looking statements to take into account events or circumstances that occur after the date of this annual report or any unanticipated events which may cause actual results to differ from those expressed or implied by the forward-looking statements contained in this annual report, except to the extent required by law.
| ii |
| Item 1. | Business |
Business Overview
We are a leading national provider of freestanding, fixed-site outpatient diagnostic imaging services in the United States based on number of locations and annual imaging revenue. At December 31, 2017, we operated directly or indirectly through joint ventures with hospitals, 297 centers located in California, Delaware, Florida, Maryland, New Jersey, and New York. Our centers provide physicians with imaging capabilities to facilitate the diagnosis and treatment of diseases and disorders and may reduce unnecessary invasive procedures, often reducing the cost and amount of care for patients. Our services include magnetic resonance imaging (MRI), computed tomography (CT), positron emission tomography (PET), nuclear medicine, mammography, ultrasound, diagnostic radiology (X-ray), fluoroscopy and other related procedures. The vast majority of our centers offer multi-modality imaging services, a key point of differentiation from our competitors. Our multi-modality strategy diversifies revenue streams, reduces exposure to reimbursement changes and provides patients and referring physicians one location to serve the needs of multiple procedures.
We seek to develop leading positions in regional markets in order to leverage operational efficiencies. Our scale and density within selected geographies provide close, long-term relationships with key payors, radiology groups and referring physicians. Each of our center-level and regional operations teams is responsible for managing relationships with local physicians and payors, meeting our standards of patient service and maintaining profitability. We provide training programs, standardized policies and procedures and sharing of best practices among the physicians in our regional networks.
In addition to our imaging services, one of our subsidiaries, eRAD, Inc., develops and sells computerized systems for the imaging industry, including Picture Archiving Communications Systems (“PACS”). Another one of our subsidiaries, Imaging On Call LLC, provides teleradiology services for remote interpretation of images on behalf of radiology groups, hospitals and imaging center customers. Teleradiology is the process of transmitting radiological patient images, such as X-rays, CTs, and MRIs, from one location to another for the purposes of interpretation and/or consultation. Teleradiology allows radiologists to provide services without actually having to be at the location of the patient and allows trained specialists to be available 24/7. In addition to providing alternative revenue sources for us, the capabilities of both eRAD and Imaging On Call are designed to make the RadNet imaging center operations more efficient and cost effective.
Since December 2015 we have been engaged in a multi-year strategic relationship with Imaging Advantage LLC (“IA”) through which we collaborate in developing business models for radiology services. As part of our arrangement, we contract with IA for 85 radiologist physicians to provide services at our facilities. In addition, our relationship with the State of Qatar to help direct Screen for Life, a public-private partnership with the Qatari government to provide screening services, is on-going.
We derive substantially all of our revenue from fees charged for the diagnostic imaging services performed at our facilities. For the years ended December 31, 2017, 2016 and 2015, we performed 6,196,398, 6,109,622, and 5,638,979, diagnostic imaging procedures and generated net revenue of $922.2 million, $884.5 million, and $809.6 million, respectively. Additional information concerning RadNet, Inc., including our consolidated subsidiaries, for each of the years ended December 31, 2017, 2016 and 2015 is included in the consolidated financial statements and notes thereto in this annual report.
History of our Business
We became incorporated in Delaware in 2008 and have been in business since 1985.
We develop our medical imaging business through a combination of organic growth and acquisitions. For a discussion of acquisitions, see Item 7 - “Management’s Discussion and Analysis and Results of Operations—Recent Developments and Facility Acquisitions” below.
In addition to our imaging business, our eRAD, Inc. subsidiary is a provider of PACS and related workflow solutions to the radiology industry. Over 250 hospitals, teleradiology businesses, imaging centers and specialty physician groups use eRAD’s technology to distribute, display, store and retrieve digital images taken from all diagnostic imaging modalities. eRAD has approximately 76 employees, including a research and development team of 21 software engineers in Budapest, Hungary.
We have also assembled an industry leading team of software developers, based out of Prince Edward Island, Canada, to create a workflow solution known as Radiology Information Systems (“RIS”) focused exclusively on RadNet’s internal use. All 25 members of this Canadian based team have significant software development expertise in radiology, and together with eRAD and its PACS technology, are creating fully integrated solutions to manage all aspects of RadNet’s internal information needs.
| 1 |
Through our teleradiology business, Imaging On Call, LLC, located in Fishkill, New York, we provide interpretation services to approximately 51 hospitals and hospital-based radiology groups.
References to “RadNet,” “we,” “us,” “our” or the “Company” in this report refer to RadNet, Inc., its subsidiaries and affiliated entities. See “Management’s Discussion and Analysis and Results of Operations—Overview.”
Available Information
All reports we file with the Securities and Exchange Commission are available free of charge via EDGAR through the SEC website at www.sec.gov. In addition you may read and copy any materials that we file with the SEC at the SEC’s Public Reference Room at 100 F Street, NE., Washington, DC 20549, and may obtain information on the operation of the Public Reference Room by calling the SEC at 1-800-SEC-0330. We also maintain a website at www.radnet.com. where we make available, free of charge, our annual report on Form 10-K, quarterly reports on Form 10-Q, current reports on Form 8-K and all amendments to those reports as soon as is reasonably practicable after the material is electronically filed with the Securities and Exchange Commission. References to our website in this report are provided as a convenience and the information contained on, or otherwise accessible through, the website is not incorporated by reference into, nor does it form a part of this annual report on Form 10-K or any other document that we file with the Securities and Exchange Commission.
Industry Overview
Diagnostic imaging involves the use of non-invasive procedures to generate representations of internal anatomy and function that can be recorded on film or digitized for display on a video monitor. Diagnostic imaging procedures facilitate the early diagnosis and treatment of diseases and disorders and may reduce unnecessary invasive procedures, often minimizing the cost and amount of care for patients. Diagnostic imaging procedures include MRI, CT, PET, nuclear medicine, ultrasound, mammography, X-ray and fluoroscopy.
While X-ray remains the most commonly performed diagnostic imaging procedure, the fastest growing and higher margin procedures are MRI, CT and PET. The rapid growth in PET scans is attributable to the increasing recognition of the efficacy of PET scans in the diagnosis and monitoring of cancer. The number of MRI and CT scans performed annually in the United States continues to grow due to their wider acceptance by physicians and payors, an increasing number of applications for their use and a general increase in demand due to the aging population.
Diagnostic Imaging Settings
Diagnostic imaging services are typically provided in one of the following settings:
Fixed-site, freestanding outpatient diagnostic facilities
These facilities range from single-modality to multi-modality facilities and are generally not owned by hospitals or clinics. These facilities depend upon physician referrals for their patients and generally do not maintain dedicated, contractual relationships with hospitals or clinics. In fact, these facilities may compete with hospitals or clinics that have their own imaging systems to provide services to these patients. These facilities bill third-party payors, such as managed care organizations, insurance companies, Medicare or Medicaid. All of our facilities are in this category.
Hospitals
Many hospitals provide both inpatient and outpatient diagnostic imaging services, typically on site. These inpatient and outpatient centers are owned and operated by the hospital or clinic, or jointly by both, and are primarily used by patients of the hospital or clinic. The hospital or clinic bills third-party payors, such as managed care organizations, insurance companies, Medicare or Medicaid. We have entered into joint ventures with certain hospitals to provide diagnostic imaging services at those hospitals.
Mobile Imaging
While many hospitals own or lease their own equipment, certain hospitals provide diagnostic imaging services by contracting with providers of mobile imaging services. Using specially designed trailers, mobile imaging service providers transport imaging equipment and provide services to hospitals and clinics on a part-time or full-time basis, thus allowing small to mid-size hospitals and clinics that do not have the patient demand to justify fixed on-site access to advanced diagnostic imaging technology. Diagnostic imaging providers contract directly with the hospital or clinic and are typically reimbursed directly by them. We do not provide mobile imaging services.
| 2 |
Diagnostic Imaging Modalities
The principal diagnostic imaging modalities we use at our facilities are:
MRI
MRI has become widely accepted as the standard diagnostic tool for a wide and fast-growing variety of clinical applications for soft tissue anatomy, such as those found in the brain, spinal cord, abdomen, heart and interior ligaments of body joints such as the knee. MRI uses a strong magnetic field in conjunction with low energy electromagnetic waves that are processed by a computer to produce high-resolution, three-dimensional, cross-sectional images of body tissue. A typical MRI examination takes from 20 to 45 minutes. MRI systems are designed as either open or closed and have magnetic field strength of 0.2 Tesla to 3.0 Tesla and are priced in the range of $0.6 million to $2.5 million. As of December 31, 2017, we had 257 MRI systems in operation.
CT
CT provides higher resolution images than conventional X-rays, but generally not as well defined as those produced by MRI. CT uses a computer to direct the movement of an X-ray tube to produce multiple cross-sectional images of a particular organ or area of the body. CT is used to detect tumors and other conditions affecting bones and internal organs. It is also used to detect the occurrence of strokes, hemorrhages and infections. A typical CT examination takes from 15 to 45 minutes. CT systems are priced in the range of $0.3 million to $1.2 million. As of December 31, 2017, we had 152 CT systems in operation.
PET
PET scanning involves the administration of a radiopharmaceutical agent with a positron-emitting isotope and the measurement of the distribution of that isotope to create images for diagnostic purposes. PET scans provide the capability to determine how metabolic activity impacts other aspects of physiology in the disease process by correlating the reading for the PET with other tools such as CT or MRI. PET technology has been found highly effective and appropriate in certain clinical circumstances for the detection and assessment of tumors throughout the body, the evaluation of some cardiac conditions and the assessment of epilepsy seizure sites. The information provided by PET technology often obviates the need to perform further highly invasive or diagnostic surgical procedures. PET systems are priced in the range of $0.8 million to $2.5 million. In addition, we employ combined PET/CT systems that blend the PET and CT imaging modalities into one scanner. These combined systems are priced in the range of $1.1 million to $2.8 million. As of December 31, 2017, we had 49 PET or combination PET/CT systems in operation.
Nuclear Medicine
Nuclear medicine uses short-lived radioactive isotopes that release small amounts of radiation that can be recorded by a gamma camera and processed by a computer to produce an image of various anatomical structures or to assess the function of various organs such as the heart, kidneys, thyroid and bones. Nuclear medicine is used primarily to study anatomic and metabolic functions. Nuclear medicine systems are priced in the range of $300,000 to $400,000. As of December 31, 2017, we had 52 nuclear medicine systems in operation.
X-ray
X-rays use roentgen rays to penetrate the body and record images of organs and structures on film. Digital X-ray systems add computer image processing capability to traditional X-ray images, which provides faster transmission of images with a higher resolution and the capability to store images more cost-effectively. X-ray systems are priced in the range of $95,000 to $440,000. As of December 31, 2017, we had 285 X-ray systems in operation.
Ultrasound
Ultrasound imaging uses sound waves and their echoes to visualize and locate internal organs. It is particularly useful in viewing soft tissues that do not X-ray well. Ultrasound is used in pregnancy to avoid X-ray exposure as well as in gynecological, urologic, vascular, cardiac and breast applications. Ultrasound systems are priced in the range of $90,000 to $250,000. As of December 31, 2017, we had 614 ultrasound systems in operation.
| 3 |
Mammography
Mammography is a specialized form of radiology using low dosage X-rays to visualize breast tissue and is the primary screening tool for breast cancer. Mammography procedures and related services assist in the diagnosis of and treatment planning for breast cancer. Analog mammography systems are priced in the range of $70,000 to $100,000, and digital mammography systems are priced in the range of $250,000 to $400,000. As of December 31, 2017, we had 261 mammography systems in operation.
Fluoroscopy
Fluoroscopy uses ionizing radiation combined with a video viewing system for real time monitoring of organs. Fluoroscopy systems are priced in the range of $100,000 to $400,000. As of December 31, 2017, we had 102 fluoroscopy systems in operation.
Industry Trends
We believe the diagnostic imaging services industry will continue to grow as a result of a number of factors, including the following:
Escalating Demand for Healthcare Services from an Aging Population
According to the United States Census Bureau estimates released in June 2017, the number of US residents age 65 or over increased from 35.0 million in 2000 to 49.2 million in 2016, and the median age for the United States is expected to continue to increase. Because diagnostic imaging use tends to increase as a person ages, we believe the aging population will generate more demand for diagnostic imaging procedures.
New Effective Applications for Diagnostic Imaging Technology
New technological developments are expected to extend the clinical uses of diagnostic imaging technology and increase the number of scans performed. Recent technological advancements include:
| · | MRI spectroscopy, which can differentiate malignant from benign lesions; |
| · | MRI angiography, which can produce three-dimensional images of body parts and assess the status of blood vessels; |
| · | enhancements in teleradiology systems, which permit the digital transmission of radiological images from one location to another for interpretation by radiologists at remote locations; and |
| · | the development of combined PET/CT scanners, which combine the technology from PET and CT to create a powerful diagnostic imaging system. |
Additional improvements in imaging technologies, contrast agents and scan capabilities are leading to new non-invasive diagnostic imaging application, including methods of diagnosing blockages in the heart’s vital coronary arteries, liver metastases, pelvic diseases and vascular abnormalities without exploratory surgery. We believe that the use of the diagnostic capabilities of MRI and other imaging services will continue to increase because they are cost-effective, time-efficient and non-invasive, as compared to alternative procedures, including surgery, and that newer technologies and future technological advancements will further increase the use of imaging services. At the same time, the industry has increasingly used upgrades to existing equipment to expand applications, extend the useful life of existing equipment, improve image quality, reduce image acquisition time and increase the volume of scans that can be performed. We believe the use of equipment upgrades rather than equipment replacements will continue, as we do not foresee new imaging technologies on the near-term horizon that will displace MRI, CT or PET as the principal advanced diagnostic imaging modalities.
| 4 |
Wider Physician and Payor Acceptance of the Use of Imaging
During the last 30 years, there has been a major effort undertaken by the medical and scientific communities to develop higher quality, cost-effective diagnostic imaging technologies and to minimize the risks associated with the application of these technologies. The thrust of product development during this period has largely been to reduce the hazards associated with conventional X-ray and nuclear medicine techniques and to develop new, less harmful imaging technologies. As a result, the use of advanced diagnostic imaging modalities, such as MRI, CT and PET, which provide superior image quality compared to other diagnostic imaging technologies, has increased rapidly in recent years. These advanced modalities allow physicians to diagnose a wide variety of diseases and injuries quickly and accurately without exploratory surgery or other surgical or invasive procedures, which are usually more expensive, involve greater risk to patients and result in longer rehabilitation time. Because advanced imaging systems are increasingly seen as a tool for reducing long-term healthcare costs, they are gaining wider acceptance among payors.
Greater Consumer Awareness of and Demand for Preventive Diagnostic Screening
Diagnostic imaging, such as elective full-body scans, is increasingly being used as a screening tool for preventive care procedures. Consumer awareness of diagnostic imaging as a less invasive and preventive screening method has added to the growth in diagnostic imaging procedures. We believe that further technological advancements allowing for early diagnosis of diseases and disorders using less invasive procedures will create additional demand for diagnostic imaging.
Expansion of Teleradiology Services
As hiring radiologists has become more difficult, the use of teleradiology is expected to continue to expand to provide patients better, more specialized care and 24/7 services.
Our Competitive Strengths
Our Scale and Position as the Largest Provider of Freestanding, Fixed-site Outpatient Diagnostic Imaging Services in the United States, Based on Number of Centers and Revenue
As of December 31, 2017, we operated 297 centers in California, Delaware, Florida, Maryland, New Jersey, and New York. Our size and scale allow us to achieve operating, sourcing and administrative efficiencies, including equipment and medical supply sourcing savings and favorable maintenance contracts from equipment manufacturers and other suppliers. Our specific knowledge of our geographic markets drives strong relationships with key payors, radiology groups and referring physicians within our markets.
Our Comprehensive "Multi-Modality" Diagnostic Imaging Offering
The vast majority of our centers offer multiple types of imaging procedures, driving strong relationships with referring physicians and payors in our markets and a diversified revenue base. At each of our multi-modality facilities, we offer patients and referring physicians one location to serve their needs for multiple procedures. This prevents multiple patient visits or unnecessary travel between facilities, thereby increasing patient throughput and decreasing costs and time delays. Our revenue is generated by a broad mix of modalities. We believe our multi-modality strategy lessens our exposure to reimbursement changes in any specific modality.
Our Competitive Pricing
We believe our fees are generally lower than hospital fees for the services we provide.
Our Facility Density in Many Highly Populated Areas of the United States
The strategic organization of our diagnostic imaging facilities into regional networks concentrated in major population centers in six states offers unique benefits to our patients, our referring physicians, our payors and us. We are able to increase the convenience of our services to patients by implementing scheduling systems within geographic regions, where practical. For example, many of our diagnostic imaging facilities within a particular region can access the patient appointment calendars of other facilities within the same regional network to efficiently allocate time available and to meet a patient's appointment, date, time, or location preferences. The grouping of our facilities within regional networks enables us to easily move technologists and other personnel, as well as equipment, from under-utilized to over-utilized facilities on an as-needed basis, and drive referrals. Our organization of referral networks results in increased patient throughput, greater operating efficiencies, better equipment utilization rates and improved response time for our patients. We believe our networks of facilities and tailored service offerings for geographic areas drives local physician referrals, makes us an attractive candidate for selection as a preferred provider by third-party payors, creates economies of scale and provides barriers to entry by competitors in our markets.
| 5 |
Our Strong Relationships with Payors and Diversified Payor Mix
Our revenue is derived from a diverse mix of payors, including private payors, managed care capitated payors and government payors, which should mitigate our exposure to possible unfavorable reimbursement trends within any one payor class. In addition, our experience with capitation arrangements has provided us with the expertise to manage utilization and pricing effectively, resulting in a predictable and recurring stream of revenue. We believe that third-party payors representing large groups of patients often prefer to enter into managed care contracts with providers that offer a broad array of diagnostic imaging services at convenient locations throughout a geographic area. In 2017, we received approximately 59% of our net service revenue before provision for bad debt from commercial insurance payors, 12% from managed care capitated payors, 20% from Medicare and 3% from Medicaid. No single payor accounted for more than 5% of our net revenue for the twelve months ended December 31, 2017.
Our Strong Relationships with Experienced and Highly Regarded Radiologists
Our contracted radiologists have outstanding credentials, strong relationships with referring physicians, and a broad mix of sub-specialties. The collective experience and expertise of these radiologists translates into more accurate and efficient service to patients. Our close relationship with Howard G. Berger, M.D., our President and Chief Executive Officer, and Beverly Radiology Medical Group (“BRMG”) in California and our long-term arrangements with radiologists outside of California enable us to better ensure that medical service provided at our facilities is consistent with the needs and expectations of our referring physicians, patients and payors.
Our Experienced and Committed Management Team
Our senior management group has more than 100 years of combined healthcare management experience. Our executive management team has created our differentiated approach based on their comprehensive understanding of the diagnostic imaging industry and the dynamics of our regional markets. We have a track record of successful acquisitions and integration of acquired businesses into RadNet, and have managed the business through a variety of economic and reimbursement cycles.
Our Technologically Advanced Imaging Systems
Our eRad subsidiary develops and sells computerized imaging systems for the industry and Imaging On Call provides teleradiology services for interpretation of images for radiology groups, hospitals and other medical groups. In addition, we have assembled an industry leading team of software developers to create radiology workflow solutions for our internal use.
Business Strategy
Maximize Performance at Our Existing Facilities
We intend to enhance our operations and increase scan volume and revenue at our existing facilities by expanding physician relationships and increasing the procedure offerings.
Expansion Into Related Businesses
With our acquisition of eRad we entered the business of the development and sale of software systems essential to the imaging industry. Similarly, with our acquisition of Imaging On Call, we entered the teleradiology business. We intend to regularly evaluate potential acquisitions of other businesses to the extent they complement our imaging business.
Focus on Profitable Contracting
We regularly evaluate our contracts with third-party payors, industry vendors and radiology groups, as well as our equipment and real property leases, to determine how we may improve the terms to increase our revenues and reduce our expenses. Because many of our contracts with third party payors are short-term in nature, we can regularly renegotiate these contracts, if necessary. We believe our position as a leading provider of diagnostic imaging services and our long-term relationships with physician groups in our markets enable us to obtain more favorable contract terms than would be available to smaller or less experienced imaging services providers.
| 6 |
Optimize Operating Efficiencies
We try to maximize our equipment utilization by adding, upgrading and re-deploying equipment where we experience excess demand. We will continue to trim excess operating and general and administrative costs where it is feasible to do so. We may also continue to use, where appropriate, highly trained radiology physician assistants to perform, under appropriate supervision of radiologists, basic services traditionally performed by radiologists. We will continue to upgrade our advanced information technology system to create cost reductions for our facilities in areas such as image storage, support personnel and financial management.
Expand Our Networks
We intend to continue to expand the number of our facilities both organically and through targeted acquisitions, using a disciplined approach for evaluating and entering new areas, including consideration of whether we have adequate financial resources to expand. Our current plans are to strengthen our market presence in geographic areas where we currently have existing operations and to expand into neighboring and other areas where we believe we can compete effectively. We perform extensive due diligence before developing a new facility or acquiring an existing facility or entering into a joint venture with a hospital to manage a facility, including surveying local referral sources and radiologists, as well as examining the demographics, reimbursement environment, competitive landscape and intrinsic demand of the geographic market. We generally will only enter new markets where:
| · | there is sufficient patient demand for outpatient diagnostic imaging services; |
| · | we believe we can gain significant market share; |
| · | we can build key referral relationships or we have already established such relationships; and |
| · | payors are receptive to our entry into the market. |
Expand Our Joint Ventures
As part of our growth strategy we have entered into joint ventures with hospitals, health systems or radiology practices that were formed for the purpose of owning and operating diagnostic imaging centers. We have created a number of joint ventures in California, Maryland, and New Jersey with well-established hospital systems to manage additional facilities. We intend to continue to expand in established markets through additional joint ventures, particularly with hospital systems. We believe that such joint ventures strengthen and expand our strength in markets where we are already strong.
Our Services
We offer a comprehensive set of imaging services including MRI, CT, PET, nuclear medicine, X-ray, ultrasound, mammography, fluoroscopy and other related procedures. We focus on providing standardized high quality imaging services, regardless of location, to ensure patients, physicians and payors consistency in service and quality. To ensure the high quality of our services, we monitor patient satisfaction, timeliness of services to patients and reports to physicians.
The key features of our services include:
| · | patient-friendly, non-clinical environments; |
| · | a 24-hour turnaround on routine examinations; |
| · | interpretations within one to two hours, if needed; |
| · | flexible patient scheduling, including same-day appointments; |
| · | extended operating hours, including weekends; |
| · | reports delivered by courier, facsimile or email; |
| · | availability of second opinions and consultations; |
| · | availability of sub-specialty interpretations at no additional charge; and |
| · | standardized fee schedules by region. |
| 7 |
Radiology Professionals
In the states in which we provide services (except Florida), a lay person or any entity other than a professional corporation or similar professional organization is not allowed to practice medicine, including by employing professional persons or by having any ownership interest or profit participation in or control over any medical professional practice. This doctrine is commonly referred to as the prohibition on the “corporate practice” of medicine. In order to comply with this prohibition, we contract with radiologists to provide professional medical services in our facilities, including the supervision and interpretation of diagnostic imaging procedures. The radiology practice maintains full control over the physicians it employs. Pursuant to each management contract, we make available the imaging facility and all of the furniture and medical equipment at the facility for use by the radiology practice, and the practice is responsible for staffing the facility with qualified professional medical personnel. In addition, we provide management services and administration of the non-medical functions relating to the professional medical practice at the facility, including among other functions, provision of clerical and administrative personnel, bookkeeping and accounting services, billing and collection, provision of medical and office supplies, secretarial, reception and transcription services, maintenance of medical records, and advertising, marketing and promotional activities. As compensation for the services furnished under contracts with radiologists, we generally receive an agreed percentage of the medical practice billings for, or collections from, services provided at the facility, typically 75% of global net service fee revenue or collections after deduction of the professional component of the medical practice billings.
At all but 5 of our California facilities, we contract for the provision of professional medical services directly with BRMG, or indirectly through BRMG with other radiology groups.
Many states have also enacted laws prohibiting a licensed professional from splitting fees derived from the practice of medicine with an unlicensed person or business entity. We do not believe that the management, administrative, technical and other non-medical services we provide to each of our contracted radiology groups violate the corporate practice of medicine prohibition or that the fees we charge for such services violate the fee splitting prohibition. However, the enforcement and interpretation of these laws by regulatory authorities and state courts vary from state to state. If our arrangements with our independent contractor radiology groups are found to violate state laws prohibiting the practice of medicine by general business corporations or fee splitting, our business, financial condition and ability to operate in those states could be adversely affected.
BRMG and New York Groups
Howard G. Berger, M.D., is our President and Chief Executive Officer, a member of our Board of Directors, and also owns, indirectly, 99% of the equity interests in BRMG. BRMG is responsible for all of the professional medical services at nearly all of our facilities located in California under a management agreement with us, and employs physicians or contracts with various other independent physicians and physician groups to provide the professional medical services at most of our California facilities. We generally obtain professional medical services from BRMG in California, rather than provide such services directly or through subsidiaries, in order to comply with California’s prohibition against the corporate practice of medicine. However, as a result of our close relationship with Dr. Berger and BRMG, we believe that we are able to better ensure that medical service is provided at our California facilities in a manner consistent with our needs and expectations and those of our referring physicians, patients and payors than if we obtained these services from unaffiliated physician groups.
We believe that physicians are drawn to BRMG and the other radiologist groups with whom we contract by the opportunity to work with the state-of-the-art equipment we make available to them, as well as the opportunity to receive specialized training through our fellowship programs, and engage in clinical research programs, which generally are available only in university settings and major hospitals.
| 8 |
As of December 31, 2017, BRMG and the NY Groups (defined below) employed or contracted for 145 full-time and 34 part-time radiologists. In addition to our BRMG staff, we contract 85 full-time physicians through our strategic relationship with Imaging Advantage LLC. Under our management agreement with BRMG, we are paid a percentage of the amounts collected for the professional services BRMG physicians render as compensation for our services and for the use of our facilities and equipment. For the year ended December 31, 2017, this percentage was 79%. The percentage may be adjusted, if necessary, to ensure that the parties receive the fair value for the services they render. The following are the other principal terms of our management agreement with BRMG:
| · | The agreement expires on January 1, 2024. The agreement automatically renews for consecutive 10-year periods, unless either party delivers a notice of non-renewal to the other party no later than six months prior to the scheduled expiration date. Either party may terminate the agreement if the other party defaults under its obligations, after notice and an opportunity to cure. We may terminate the agreement if Dr. Berger no longer owns at least 60% of the equity of BRMG; as of December 31, 2017, he owned indirectly 99% of the equity interests of BRMG. |
| · | At its expense, BRMG employs or contracts with an adequate number of physicians necessary to provide all professional medical services at all of our California facilities, except for 5 facilities for which we contract with separate medical groups. |
| · | At our expense, we provide all furniture, furnishings and medical equipment located at the facilities and we manage and administer all non-medical functions at, and provide all nurses and other non-physician personnel required for the operation of, the facilities. |
| · | If BRMG wants to open a new facility, we have the right of first refusal to provide the space and services for the facility under the same terms and conditions set forth in the management agreement. |
| · | If we want to open a new facility in California, BRMG must use its best efforts to provide medical personnel under the same terms and conditions set forth in the management agreement. If BRMG cannot provide such personnel, we have the right to contract with other physicians to provide services at the facility. |
| · | BRMG must maintain medical malpractice insurance for each of its physicians with coverage limits not less than $1 million per incident and $3 million in the aggregate per year. BRMG also has agreed to indemnify us for any losses we suffer that arise out of the acts or omissions of BRMG and its employees, contractors and agents. |
We contract with nine medical groups which provide professional medical services at all of our facilities in Manhattan and Brooklyn, New York. These contracts are similar to our contract with BRMG. Seven of these groups are owned by John V. Crues, III, M.D., RadNet’s Medical Director, a member of our Board of Directors, and a 1% owner of BRMG. Dr. Berger owns a controlling interest in two of these medical groups which provide professional medical services at one of our Manhattan facilities.
Non-BRMG and NY Groups entity locations
At the 5 centers in California where BRMG does not provide professional medical services, and at all of the centers which are located outside of California, with the exception of centers located in the New York, New York area, we have entered into long-term contracts with prominent third-party radiology groups in the area to provide physician services at those facilities. These arrangements also allow us to comply with the prohibition against the “corporate practice” of medicine in other states in which we operate (except in Florida which does not have an equivalent statute prohibiting the corporate practice of medicine).
These third-party radiology practice groups provide professional services, including supervision and interpretation of diagnostic imaging procedures, in our diagnostic imaging centers. The radiology practices maintain full control over the provision of professional services. The contracted radiology practices have outstanding physician and practice credentials and reputations; strong competitive market positions; a broad sub-specialty mix of physicians; a history of growth and potential for continued growth. In these facilities we have entered into long-term agreements (typically 10-40 years in length) under which, in addition to obtaining technical fees for the use of our diagnostic imaging equipment and the provision of technical services, we provide management services and receive a fee based on the practice group’s professional revenue. We typically receive 100% of the technical reimbursements associated with imaging procedures plus certain fees paid to us for providing additional management services. The radiology practice groups retain the professional reimbursements associated with imaging procedures after deducting management service fees paid to us.
| 9 |
Additionally, we perform certain management services for a portion of the professional groups with whom we contract who provide professional radiology services at local hospitals. For performing these management services, which include billing, collecting, transcription and medical coding, we receive management fees.
Payors
The fees charged for diagnostic imaging services performed at our facilities are paid by a diverse mix of payors, as illustrated for the following periods presented in the table below:
| % of Net Revenue Before Bad Debt Provision | ||||||||||||
| Year Ended December 31, 2017 | Year Ended December 31, 2016 | Year Ended December 31, 2015 | ||||||||||
| Commercial Insurance (1) | 59% | 58% | 57% | |||||||||
| Managed Care Capitated Payors | 12% | 12% | 12% | |||||||||
| Medicare& Medicaid | 23% | 23% | 23% | |||||||||
(1) Includes co-payments, direct patient payments and payments through contracts with physician groups and other non-insurance company payors.
We have described below the types of reimbursement arrangements we have with third-party payors.
Commercial Insurance
Generally, insurance companies reimburse us, directly or indirectly, including through BRMG in California or through the contracted radiology groups elsewhere, on the basis of agreed upon rates. These rates are negotiated and may differ materially with rates set forth in the Medicare Physician Fee Schedule for the particular service. The patients may be responsible for certain co-payments or deductibles.
Managed Care Capitation Agreements
Under these agreements, which are generally between BRMG in California and outside of California between the contracted radiology group (typically an independent physician group or other medical group) and the payor (which in most cases are large medical groups or Independent Practice Associations), the payor pays a pre-determined amount per-member per-month in exchange for the radiology group providing all necessary covered services to the managed care members included in the agreement. These contracts pass much of the financial risk of providing outpatient diagnostic imaging services, including the risk of over-use, from the payor to the radiology group and, as a result of our management agreement with the radiology group, to us.
We believe that through our comprehensive utilization management, or UM, program we have become highly skilled at assessing and moderating the risks associated with the capitation agreements, so that these agreements are profitable for us. Our UM program is managed by our UM department, which consists of administrative and nursing staff as well as BRMG medical staff who are actively involved with the referring physicians and payor management in both prospective and retrospective review programs. Our UM program includes the following features, all of which are designed to manage our costs while ensuring that patients receive appropriate care:
| · | Physician Education |
At the inception of a new capitation agreement, we provide the new referring physicians with binders of educational material comprised of proprietary information that we have prepared and third-party information we have compiled, which are designed to address diagnostic strategies for common diseases. We distribute additional material according to the referral practices of the group as determined in the retrospective analysis described below.
| · | Prospective Review |
Referring physicians are required to submit authorization requests for non-emergency high-intensity services: MRI, CT, special procedures and nuclear medicine studies. The UM medical staff, according to accepted practice guidelines, considers the necessity and appropriateness of each request. Notification is then sent to the imaging facility, referring physician and medical group. Appeals for cases not approved are directed to us. The capitated payor has the final authority to uphold or deny our recommendation.
| 10 |
| · | Retrospective Review |
We collect and sort encounter activity by payor, place of service, referring physician, exam type and date of service. The data is then presented in quantitative and analytical form to facilitate understanding of utilization activity and to provide a comparison between fee-for-service and Medicare equivalents. Our Medical Director prepares a quarterly report for each payor and referring physician. When we find that a referring physician is over utilizing services, we work with the physician to modify referral patterns.
Medicare/Medicaid
Medicare is the federal health insurance program for people age 65 or older and people under age 65 with certain disabilities. Medicaid, funded by both the federal government and states, is a state-administered health insurance program for qualifying low-income and medically needy persons. For services for which we bill Medicare directly or indirectly, including through contracted radiologists, we are paid under the Medicare Physician Fee Schedule. Under the Protecting Access to Medicare Act of 2014, Congress introduced a new quality incentive program that, effective January 1, 2016, reduces Medicare payments for certain CT services reimbursed through the Medicare Physician Fee Schedule that are furnished using equipment that does not meet certain dose optimization and management standards. Medicare patients usually pay a 20% co-payment unless they have secondary insurance. Medicaid rates are set by the individual states for each state program and Medicaid patients may be responsible for a modest co-payment.
Contracts with Physician Groups and Other Non-Insurance Company Payors
For some of our contracts with physician groups and other providers, we do not bill payors, but instead accept agreed upon rates for our radiology services. These rates are typically at or below the rates set forth in the current Medicare Fee Schedule for the particular service. However, we often agree to a specified rate for MRI and CT procedures that is not tied to the Medicare Fee Schedule.
Facilities
We operate 132 fixed-site, freestanding outpatient diagnostic imaging facilities in California, 13 in Delaware, 3 in Florida, 60 in Maryland, 20 in New Jersey, 19 in the Rochester and Hudson Valley areas of New York and 50 in New York City. We lease the premises at which these facilities are located.
Our facilities are primarily located in geographic networks that we refer to as regions. The majority of our facilities are multi-modality sites, offering various combinations of MRI, CT, PET, nuclear medicine, ultrasound, X-ray, fluoroscopy services and other related procedures. A portion of our facilities are single-modality sites, offering either X-ray or MRI services. Consistent with our regional network strategy, we locate our single-modality facilities near multi-modality facilities, to help accommodate overflow in targeted demographic areas.
The following table sets forth the number of our facilities operated directly or through joint ventures for each year during the five-year period ended December 31, 2017:
| Years Ended | ||||||||||||||||||||
| December 31, | ||||||||||||||||||||
| 2013 | 2014 | 2015 | 2016 | 2017 | ||||||||||||||||
| Total facilities owned or managed (at beginning of the year) | 246 | 250 | 259 | 300 | 305 | |||||||||||||||
| Facilities added by: | ||||||||||||||||||||
| Acquisition | 12 | 22 | 43 | 10 | 8 | |||||||||||||||
| Internal development | – | – | 1 | 8 | 4 | |||||||||||||||
| Facilities closed or sold | -8 | -13 | -3 | -13 | -20 | |||||||||||||||
| Total facilities owned (at year end) | 250 | 259 | 300 | 305 | 297 | |||||||||||||||
| 11 |
Diagnostic Imaging Equipment
The following table indicates, as of December 31, 2017, the quantity of principal diagnostic equipment available at our facilities operated directly or through joint ventures, by state:
| Equipment Count | ||||||||||||||||||||||||||||||||||||||||
| MRI | Open/MRI | CT | PET/CT | Mammo | Ultrasound | X-ray | NucMed | Fluoroscopy | Total | |||||||||||||||||||||||||||||||
| California | 81 | 23 | 58 | 22 | 106 | 294 | 136 | 22 | 58 | 800 | ||||||||||||||||||||||||||||||
| Florida | 3 | 0 | 2 | 1 | 3 | 5 | 2 | 2 | 1 | 19 | ||||||||||||||||||||||||||||||
| Delaware | 8 | – | 7 | 0 | 10 | 19 | 15 | 2 | 4 | 65 | ||||||||||||||||||||||||||||||
| New Jersey | 18 | 5 | 15 | 3 | 18 | 30 | 16 | 2 | 6 | 113 | ||||||||||||||||||||||||||||||
| New York | 49 | 9 | 33 | 9 | 63 | 141 | 51 | 9 | 12 | 376 | ||||||||||||||||||||||||||||||
| Maryland | 56 | 5 | 37 | 14 | 61 | 125 | 65 | 15 | 21 | 399 | ||||||||||||||||||||||||||||||
| Total | 215 | 42 | 152 | 49 | 261 | 614 | 285 | 52 | 102 | 1,772 | ||||||||||||||||||||||||||||||
The average age of our MRI and CT units is less than five years, and the average age of our PET units is less than four years. The useful life of our MRI, CT and PET units is typically ten years.
Facility Acquisitions
Information regarding our facility acquisitions can be found within Item 7 - “Management’s Discussion and Analysis of Financial Condition and Results of Operations”, as well as Note 4 to our consolidated financial statements included in this annual report on Form 10-K.
Information Technology
Our corporate headquarters and many of our facilities are interconnected through a state-of-the-art information technology system. This system, which is compliant with the Health Insurance Portability and Accountability Act of 1996, is comprised of a number of integrated applications and provides a single operating platform for billing and collections, electronic medical records, practice management and image management.
This technology has created cost reductions for our facilities in areas such as image storage, support personnel and financial management and has further allowed us to optimize the productivity of all aspects of our business by enabling us to:
| · | capture patient demographic, history and billing information at point-of-service; |
| · | automatically generate bills and electronically file claims with third-party payors; |
| · | record and store diagnostic report images in digital format; |
| · | digitally transmit in real-time diagnostic images from one location to another, thus enabling networked radiologists to cover larger geographic markets by using the specialized training of other networked radiologists; |
| · | perform claims, rejection and collection analysis; and |
| · | perform sophisticated financial analysis, such as analyzing cost and profitability, volume, charges, current activity and patient case mix, with respect to each of our managed care contracts. |
Diagnostic reports and images are currently accessible via the Internet by our California referring providers. We have worked with some of the larger medical groups in California with whom we have contracts to provide access to this content through their web portals. We are in the process of making such services available outside of California.
We have historically utilized third-party software for our front desk patient tracking system, which we refer to as a Radiology Information System, or RIS. We have developed our own RIS through our team of software development engineers and began running this internally developed system in the first quarter of 2015.
Personnel
At December 31, 2017, we had a total of 5,356 full-time, 631 part-time and 1,453 per diem employees, including those employed by BRMG and NY Groups. These numbers include 145 full-time and 34 part-time physicians and 1,735 full-time, 425 part-time and 993 per-diem technologists. In addition to our company personnel, we contract 85 full-time physicians through our strategic relationship with Imaging Advantage LLC.
| 12 |
We employ site managers who are responsible for overseeing day-to-day and routine operations at each of our facilities, including staffing, modality and schedule coordination, referring physician and patient relations and purchasing of materials. These site managers report to regional managers and directors, who are responsible for oversight of the operations of all facilities within their region, including sales, marketing and contracting. The regional managers and directors, along with our directors of contracting, marketing, facilities, management/purchasing and human resources all report to our chief operating officers. These officers, our chief financial officer, our director of information services and our medical director report to our chief executive officer.
None of our employees is subject to a collective bargaining agreement nor have we experienced any work stoppages. We believe our relationship with our employees is good.
Sales and Marketing
At December 31, 2017, our California sales and marketing team consisted of three directors of marketing and 42 customer service representatives, while our eastern marketing team consisted of seven directors of marketing and 114 customer service representatives. Our sales and marketing team employs a multi-pronged approach to marketing, including physician, payor and sports marketing programs, each of which are described below:
Physician Marketing
Each customer service representative on our physician marketing team is responsible for marketing activity on behalf of one or more facilities. The representatives act as a liaison between the facility and referring physicians, holding meetings periodically and on an as-needed basis with them and their staff to present educational programs on new applications and uses of our systems and to address particular patient service issues that have arisen. In our experience, consistent hands-on contact with a referring physician and his or her staff generates goodwill and increases referrals to our facilities. The representatives also continually seek to establish referral relationships with new physicians and physician groups. In addition to a base salary, each representative receives a bonus based upon success.
Payor Marketing
Our marketing team regularly meets with managed care organizations and insurance companies to solicit contracts and meet with existing contracting payors to solidify those relationships. The comprehensiveness of our services, the geographic location of our facilities and the reputation of the physicians with whom we contract all serve as tools for obtaining new or repeat business from payors.
Sports Marketing Program
RadNet Inc. has a sports marketing division. Via our west coast operations, we provide diagnostic digital X-ray services for the Los Angeles Lakers, Clippers, Kings and Sparks at the Staples Center. X-ray is performed at the Coliseum for the University of Southern California and the Los Angeles Rams football teams. In exchange for these services, each team provides RadNet with season tickets, parking and advertising space in the program book. RadNet also provides radiology services at many of our imaging centers for the Los Angeles Angels, Anaheim Ducks, and the Oakland Athletics organizations.
Through our east coast operations, we have entered into sponsorship agreements with the Baltimore Ravens of the National Football League and the Baltimore Orioles of Major League Baseball which permits us to state we are the exclusive imaging provider to each organization. The sponsorship agreement with the Ravens lasts through 2019 and the Orioles through 2020.
Suppliers
Historically, we have acquired our diagnostic imaging equipment from large suppliers such as Carestream, GE Medical Systems, Inc., Hologic, Hitachi, Phillips, Siemens and others, and we purchase medical supplies from various national vendors. We believe that we have excellent working relationships with all of our major vendors. There are several comparable vendors for our supplies that would be available to us if one of our current vendors becomes unavailable.
We primarily acquire our equipment with cash or through various financing arrangements with equipment vendors and third party equipment finance companies involving the use of capital leases with purchase options at minimal prices at the end of the lease term. At December 31, 2017, capital lease minimum payment obligations, excluding interest, totaled approximately $6.9 million through 2022, including current payment installments totaling approximately $4.1 million. If we open or acquire additional imaging facilities, we may have to incur material capital lease obligations.
| 13 |
Timely, effective maintenance is essential for achieving high utilization rates of our imaging equipment. We have an arrangement with GE Medical Systems, Inc. under which it has agreed to be responsible for the maintenance and repair of a majority of our equipment for a fee that is based upon a percentage of our revenue, subject to a minimum payment.
Competition
The market for outpatient diagnostic imaging services is highly competitive. We compete locally for patients with groups of radiologists, established hospitals, clinics and other independent organizations that own and operate imaging equipment. Our competitors include the formerly public, now privately held, Alliance Healthcare Services, Inc., to the extent it sells diagnostic services directly to outpatients, Diagnostic Imaging Group and several smaller regional competitors. In addition, some physician practices have established their own diagnostic imaging facilities within their group practices. We experience additional competition as a result of those activities.
We compete principally on the basis of our reputation, our ability to provide multiple modalities at many of our facilities, the location of our facilities, the quality of our diagnostic imaging services and technologists and our ability to establish and maintain relationships with healthcare providers and referring physicians. See “Competitive Strengths” above. Some of our competitors may now or in the future have access to greater financial resources than we do, which could allow them to establish more facilities and provide access to newer, more advanced equipment.
Each of the non-BRMG contracted radiology practices has entered into agreements with its physician shareholders and full-time employed radiologists that generally prohibit those shareholders and radiologists from competing for a period of two years within defined geographic regions after they cease to be owners or employees, as applicable. In certain states, like California, a covenant not to compete is enforced in limited circumstances involving the sale of a business. In other states, a covenant not to compete will be enforced only:
| · | to the extent it is necessary to protect a legitimate business interest of the party seeking enforcement; |
| · | if it does not unreasonably restrain the party against whom enforcement is sought; and |
| · | if it is not contrary to public interest. |
Enforceability of a non-compete covenant is determined by a court based on all of the facts and circumstances of the specific case at the time enforcement is sought. For this reason, it is not possible to predict whether or to what extent a court will enforce the contracted radiology practices’ covenants. The inability of the contracted radiology practices or us to enforce radiologist’s non-compete covenants could result in increased competition from individuals who are knowledgeable about our business strategies and operations.
Liability Insurance
We maintain insurance policies with coverage we believe is appropriate in light of the risks attendant to our business and consistent with industry practice. We maintain general liability insurance and professional liability insurance in commercially reasonable amounts. Additionally, we maintain workers’ compensation insurance on all of our employees. Coverage is placed on a statutory basis and corresponds to individual state’s requirements. However, adequate liability insurance may not be available to us in the future at acceptable costs or at all. In addition, insurers from which we purchase such insurance may experience financial hardship which would impact their ability to pay covered policyholder claims.
Pursuant to our agreements with physician groups with whom we contract, including BRMG, each group must maintain medical malpractice insurance for each physician in the group, having coverage limits of not less than $1.0 million per incident and $3.0 million in the aggregate per year.
California’s medical malpractice cap further reduces our exposure. California places a $250,000 limit on non-economic damages for medical malpractice cases. Non-economic damages are defined as compensation for pain, suffering, inconvenience, physical impairment, disfigurement and other non-pecuniary injury. The cap applies whether the case is for injury or death, and it allows only one $250,000 recovery in a wrongful death case. No cap applies to economic damages. Other states in which we now operate do not have similar limitations and in those states we believe our insurance coverage to be sufficient.
| 14 |
Regulation
General
The healthcare industry is highly regulated, and we can give no assurance that the regulatory environment in which we operate will not change significantly in the future. Our ability to operate profitably will depend in part upon us, and the contracted radiology practices and their affiliated physicians obtaining and maintaining all necessary licenses and other approvals, and operating in compliance with applicable healthcare regulations. We believe that healthcare regulations will continue to change. Therefore, we monitor developments in healthcare law and modify our operations from time to time as the business and regulatory environment changes.
Licensing and Certification Laws
Ownership, construction, operation, expansion and acquisition of diagnostic imaging facilities are subject to various federal and state laws, regulations and approvals concerning licensing of facilities and personnel. In addition, free-standing diagnostic imaging facilities that provide services not performed as part of a physician office must meet Medicare requirements to be certified as an independent diagnostic testing facility before it can be authorized to bill the Medicare program. We have experienced a slowdown in the credentialing of our physicians over the last several years which has lengthened our billing and collection cycle.
Corporate Practice of Medicine
In the states in which we operate, other than Florida, a lay person or any entity other than a professional corporation or other similar professional organization is not allowed to practice medicine, including by employing professional persons or by having any ownership interest or profit participation in or control over any medical professional practice. The laws of such states also prohibit a lay person or a non-professional entity from exercising control over the medical judgments or decisions of physicians and from engaging in certain financial arrangements, such as splitting professional fees with physicians. We structure our relationships with the radiology practices, including the purchase of diagnostic imaging facilities, in a manner that we believe keeps us from engaging in the practice of medicine, exercising control over the medical judgments or decisions of the radiology practices or their physicians, or violating the prohibitions against fee-splitting.
Medicare and Medicaid Fraud and Abuse – Federal Anti-kickback Statute
During the year ended December 31, 2017, approximately 20% of our revenue before provision for bad debt generated at our diagnostic imaging centers was derived from federal government sponsored healthcare programs (Medicare) and 3% from state sponsored programs (Medicaid).
Federal law known as the Anti-kickback Statute prohibits the knowing and willful offer, payment, solicitation or receipt of any form of remuneration in return for, or to induce, (i) the referral of a person, (ii) the furnishing or arranging for the furnishing of items or services reimbursable under the Medicare, Medicaid or other governmental programs or (iii) the purchase, lease or order or arranging or recommending purchasing, leasing or ordering of any item or service reimbursable under the Medicare, Medicaid or other governmental programs. Enforcement of this anti-kickback law is a high priority for the federal government, which has substantially increased enforcement resources and is scheduled to continue increasing such resources. Noncompliance with the federal Anti-kickback Statute can result in exclusion from the Medicare, Medicaid or other governmental programs and civil and criminal penalties.
The Anti-kickback Statute is broad, and it prohibits many arrangements and practices that are lawful in businesses outside of the healthcare industry. Recognizing that the Anti-kickback Statute is broad and may technically prohibit many innocuous or beneficial arrangements within the healthcare industry, the Office of the Inspector General of the U.S. Department of Health and Human Services issued regulations in July of 1991, which the Department has referred to as “safe harbors.” These safe harbor regulations set forth certain provisions which, if met in form and substance, will assure healthcare providers and other parties that they will not be prosecuted under the federal Anti-kickback Statute. Additional safe harbor provisions providing similar protections have been published intermittently since 1991. Our arrangements with physicians, physician practice groups, hospitals and other persons or entities who are in a position to refer may not fully meet the stringent criteria specified in the various safe harbors. Although full compliance with these provisions ensures against prosecution under the federal Anti-kickback Statute, the failure of a transaction or arrangement to fit within a specific safe harbor does not necessarily mean that the transaction or arrangement is illegal or that prosecution under the federal Anti-kickback Statute will be pursued.
| 15 |
Although some of our arrangements may not fall within a safe harbor, we believe that such business arrangements do not violate the Anti-kickback Statute because we are careful to structure them to reflect fair value and ensure that the reasons underlying our decision to enter into a business arrangement comport with reasonable interpretations of the Anti-kickback Statute. However, even though we continuously strive to comply with the requirements of the Anti-kickback Statute, liability under the Anti-kickback Statute may still arise because of the intentions or actions of the parties with whom we do business. While we are not aware of any such intentions or actions, we have only limited knowledge regarding the intentions or actions underlying those arrangements. Conduct and business arrangements that do not fully satisfy one of these safe harbor provisions may result in increased scrutiny by government enforcement authorities such as the Office of the Inspector General.
Medicare and Medicaid Fraud and Abuse – Stark Law
Congress has placed significant legal prohibitions against physician referrals including the Ethics in Patient Referral Act of 1989 which is commonly known as the Stark Law. The Stark Law prohibits a physician from referring Medicare patients to an entity providing designated health services, as defined under the Stark Law, including, without limitation, radiology services, in which the physician (or immediate family member) has an ownership or investment interest or with which the physician (or immediate family member) has entered into a compensation arrangement. The Stark Law also prohibits the entity from billing for any such prohibited referral. The penalties for violating the Stark Law include a prohibition on payment by these governmental programs and civil penalties of as much as $15,000 for each violation referral and $100,000 for participation in a circumvention scheme. We believe that, although we receive fees under our service agreements for management and administrative services, we are not in a position to make or influence referrals of patients.
Under the Stark Law, radiology and certain other imaging services and radiation therapy services and supplies are services included in the designated health services subject to the self-referral prohibition. Such services include the professional and technical components of any diagnostic test or procedure using X-rays, ultrasound or other imaging services, CT, MRI, radiation therapy and diagnostic mammography services (but not screening mammography services). PET and nuclear medicine procedures are also included as designated health services under the Stark Law. The Stark Law, however, excludes from designated health services: (i) X-ray, fluoroscopy or ultrasound procedures that require the insertion of a needle, catheter, tube or probe through the skin or into a body orifice; (ii) radiology procedures that are integral to the performance of, and performed during, non-radiological medical procedures; and (iii) invasive or interventional radiology, because the radiology services in these procedures are merely incidental or secondary to another procedure that the physician has ordered.
The Stark Law provides that a request by a radiologist for diagnostic radiology services or a request by a radiation oncologist for radiation therapy, if such services are furnished by or under the supervision of such radiologist or radiation oncologist pursuant to a consultation requested by another physician, does not constitute a referral by a referring physician. If such requirements are met, the Stark Law self-referral prohibition would not apply to such services. The effect of the Stark Law on the radiology practices, therefore, will depend on the precise scope of services furnished by each such practice’s radiologists and whether such services derive from consultations or are self-generated.
We believe that, other than self-referred patients, all of the services covered by the Stark Law provided by the contracted radiology practices derive from requests for consultation by non-affiliated physicians. Therefore, we believe that the Stark Law is not implicated by the financial relationships between our operations and the contracted radiology practices. In addition, we believe that we have structured our acquisitions of the assets of existing practices, and we intend to structure any future acquisitions, so as not to violate the Anti-kickback Statute and Stark Law and regulations. Specifically, we believe the consideration paid by us to physicians to acquire the tangible and intangible assets associated with their practices is consistent with fair value in arms’ length transactions and is not intended to induce the referral of patients or other business generated by such physicians. Should any such practice be deemed to constitute an arrangement designed to induce the referral of Medicare or Medicaid patients, then our acquisitions could be viewed as possibly violating anti-kickback and anti-referral laws and regulations. A determination of liability under any such laws could have a material adverse effect on our business, financial condition and results of operations.
Medicare and Medicaid Fraud and Abuse – General
The federal government embarked on an initiative to audit all Medicare carriers, which are the companies that adjudicate and pay Medicare claims. These audits are expected to intensify governmental scrutiny of individual providers. An unsatisfactory audit of any of our diagnostic imaging facilities or contracted radiology practices could result in any or all of the following: significant repayment obligations, exclusion from the Medicare, Medicaid or other governmental programs, and civil and criminal penalties.
Federal regulatory and law enforcement authorities have increased enforcement activities with respect to Medicare, Medicaid fraud and abuse regulations and other reimbursement laws and rules, including laws and regulations that govern our activities and the activities of the radiology practices. The federal government also has increased funding to fight healthcare fraud and is coordinating its enforcement efforts among various agencies, such as the U.S. Department of Justice, the U.S. Department of Health and Human Services Office of Inspector General, and state Medicaid fraud control units. The government may investigate our or the radiology practices’ activities, claims may be made against us or the radiology practices and these increased enforcement activities may directly or indirectly have an adverse effect on our business, financial condition and results of operations.
| 16 |
State Anti-kickback and Physician Self-referral Laws
Many states have adopted laws similar to the federal Anti-kickback Statute. Some of these state prohibitions apply to referral of patients for healthcare services reimbursed by any source, not only the Medicare and Medicaid programs. Although we believe that we comply with both federal and state Anti-kickback laws, any finding of a violation of these laws could subject us to criminal and civil penalties or possible exclusion from federal or state healthcare programs. Such penalties would adversely affect our financial performance and our ability to operate our business.
Federal False Claims Act
The federal False Claims Act provides, in part, that the federal government may bring a lawsuit against any person who it believes has knowingly presented, or caused to be presented, a false or fraudulent request for payment from the federal government, or who has made a false statement or used a false record to get a claim approved. The federal False Claims Act further provides that a lawsuit thereunder may be initiated in the name of the United States by an individual, a “whistleblower,” who is an original source of the allegations. The government has taken the position that claims presented in violation of the federal anti-kickback law or Stark Law may be considered a violation of the federal False Claims Act. Penalties include civil penalties of not less than $5,500 and not more than $11,000 for each false claim, plus three times the amount of damages that the federal government sustained because of the act of that person.
Further, on May 20, 2009, President Obama signed into law the Fraud Enforcement and Recovery Act of 2009 (FERA), which greatly expanded the types of entities and conduct subject to the False Claims Act. Also, various states are considering or have enacted laws modeled after the federal False Claims Act. Under the Deficit Reduction Act of 2005, or DRA, states are being encouraged to adopt false claims acts similar to the federal False Claims Act, which establish liability for submission of fraudulent claims to the State Medicaid program and contain whistleblower provisions. Even in instances when a whistleblower action is dismissed with no judgment or settlement, we may incur substantial legal fees and other costs relating to an investigation. Future actions under the False Claims Act may result in significant fines and legal fees, which would adversely affect our financial performance and our ability to operate our business.
We believe that we are in compliance with the rules and regulations that apply to the federal False Claims Act as well as its state counterparts.
Healthcare Reform Legislation
Healthcare reform legislation enacted in the first quarter of 2010 by the Patient Protection and Affordable Care Act or PPACA, specifically requires the U.S. Department of Health and Human Services, in computing physician practice expense relative value units, to increase the equipment utilization factor for advanced diagnostic imaging services (such as MRI, CT and PET) from a presumed utilization rate of 50% to 65% for 2010 through 2012, 70% in 2013, and 75% thereafter. Excluded from the adjustment is low-technology imaging modalities such as ultrasound, X-ray and fluoroscopy. The Health Care and Education Reconciliation Act of 2010 (H.R. 4872) or Reconciliation Act, which was passed by the Senate and approved by the President on March 30, 2010, amends the provision for higher presumed utilization of advanced diagnostic imaging services to a presumed rate of 75%. The higher utilization rate was fully implemented in the beginning of 2011 and replaced the phase-in approach provided in the PPACA. This utilization rate was further increased to 90% by the American Taxpayer Relief Act of 2012 (“ATRA”), effective as of January 1, 2014.
The aim of increased utilization of diagnostic imaging services is to spread the cost of the equipment and services over a greater number of scans, resulting in a lower cost per scan. These changes have precipitated reductions in federal reimbursement for medical imaging and result in decreased revenue for the scans we perform for Medicare beneficiaries. Other changes in reimbursement for services rendered by Medicare Advantage plans may also reduce the revenues we receive for services rendered to Medicare Advantage enrollees.
On November 8, 2016, Donald Trump was elected President of the United States and members of the Republican Party retained majority control over both the United States House of Representatives and the United States Senate. President Trump has repeatedly signaled his intent to repeal and replace the PPACA and members of the Republican Party in Congress have also advocated the repeal or modification of the PPACA. On January 20, 2017, President Trump signed an “Executive Order Minimizing the Economic Burden of the Patient Protection and Affordable Care Act Pending Repeal.” (the “PPACA Executive Order”). Under the PPACA Executive Order it is the policy of the Trump Administration to seek prompt repeal of the PPACA.
| 17 |
On December 22, 2017, President Trump signed into law the Act to provide for reconciliation pursuant to titles II and V of the concurrent resolution on the budget for fiscal year 2018 (originally introduced as the Tax Cuts and Jobs Act (the “TCJA”)). Among numerous changes to the tax code, the TCJA repealed the individual mandate tax penalty (the “Individual Mandate”), a PPACA provision that required individuals to pay additional taxes if he or she was uninsured during the year.
Repeal of the Individual Mandate may lead to more people being uninsured, and could raise premium rates for insured persons. Such a development, as well as other changes to (or the full repeal of) the PPACA, could affect reimbursement, coverage, and utilization of diagnostic imaging services in ways that are currently unpredictable.
Health Insurance Portability and Accountability Act of 1996
Congress enacted the Health Insurance Portability and Accountability Act of 1996, or HIPAA, in part, to combat healthcare fraud and to protect the privacy and security of patients’ individually identifiable healthcare information. HIPAA, among other things, amends existing crimes and criminal penalties for Medicare fraud and enacts new federal healthcare fraud crimes, including actions affecting non-government healthcare benefit programs. Under HIPAA, a healthcare benefit program includes any private plan or contract affecting interstate commerce under which any medical benefit, item or service is provided. A person or entity that knowingly and willfully obtains the money or property of any healthcare benefit program by means of false or fraudulent representations in connection with the delivery of healthcare services is subject to a fine or imprisonment, or potentially both. In addition, HIPAA authorizes the imposition of civil money penalties against entities that employ or enter into contracts with excluded Medicare or Medicaid program participants if such entities provide services to federal health program beneficiaries. A finding of liability under HIPAA could have a material adverse effect on our business, financial condition and results of operations.
Further, HIPAA requires healthcare providers and their business associates to maintain the privacy and security of individually identifiable protected health information (“PHI”). HIPAA imposes federal standards for electronic transactions, for the security of electronic health information and for protecting the privacy of PHI. The Health Information Technology for Economic and Clinical Health Act of 2009 (“HITECH”), signed into law on February 17, 2009, dramatically expanded, among other things, (1) the scope of HIPAA to now apply directly to “business associates,” or independent contractors who receive or obtain PHI in connection with providing a service to a covered entity, (2) substantive security and privacy obligations, including new federal security breach notification requirements to affected individuals, DHHS and prominent media outlets, of certain breaches of unsecured PHI, (3) restrictions on marketing communications and a prohibition on covered entities or business associates from receiving remuneration in exchange for PHI, and (4) the civil and criminal penalties that may be imposed for HIPAA violations, increasing the annual cap in penalties from $25,000 to $1.5 million per year.
In addition, many states have enacted comparable privacy and security statutes or regulations that, in some cases, are more stringent than HIPAA requirements. In those cases it may be necessary to modify our operations and procedures to comply with the more stringent state laws, which may entail significant and costly changes for us. We believe that we are in compliance with such state laws and regulations. However, if we fail to comply with applicable state laws and regulations, we could be subject to additional sanctions.
We believe that we are in compliance with the current HIPAA requirements, as amended by HITECH, and comparable state laws, but we anticipate that we may encounter certain costs associated with future compliance. Moreover, we cannot guarantee that enforcement agencies or courts will not make interpretations of the HIPAA standards that are inconsistent with ours, or the interpretations of our contracted radiology practices or their affiliated physicians. A finding of liability under the HIPAA standards may result in significant criminal and civil penalties. Noncompliance also may result in exclusion from participation in government programs, including Medicare and Medicaid. These actions could have a material adverse effect on our business, financial condition, and results of operations.
U.S. Food and Drug Administration or FDA
The FDA has issued the requisite pre-market approval for all of the MRI and CT systems we use.
| 18 |
Our mammography systems are regulated by the FDA pursuant to the Mammography Quality Standards Act of 1992, as amended by the Mammography Quality Standards Reauthorization Acts of 1998 and 2004 (collectively, the “MQSA”). All mammography facilities are required to meet the applicable MQSA requirements, including quality standards, be accredited by an approved accreditation body or state agency and certified by the FDA or an FDA-approved certifying state agency. Pursuant to the accreditation process, each facility providing mammography services must comply with certain standards that include, among other things, annual inspection of the facility's equipment, personnel (interpreting physicians, technologists and medical physicists) and practices.
Compliance with these MQSA requirements and standards is required to obtain Medicare payment for services provided to beneficiaries and to avoid various sanctions, including monetary penalties, or suspension of certification. Although the Mammography Accreditation Program of the American College of Radiology is an approved accreditation body and currently accredits all of our facilities which provide mammography services, and although we anticipate continuing to meet the requirements for accreditation, if we lose such accreditation, the FDA could revoke our certification. Congress has extended Medicare benefits to include coverage of screening mammography but coverage is subject to the facility performing the mammography meeting prescribed quality standards described above. The Medicare requirements to meet the standards apply to diagnostic mammography and image quality examination as well as screening mammography.
We do not believe that any further FDA approval is required in connection with the majority of equipment currently in operation or proposed to be operated.
Radiologist Licensing
The radiologists providing professional medical services at our facilities are subject to licensing and related regulations by the states in which they provide services. As a result, we require BRMG and the other radiology groups with which we contract to require those radiologists to have and maintain appropriate licensure. We do not believe that such laws and regulations will either prohibit or require licensure approval of our business operations, although no assurances can be made that such laws and regulations will not be interpreted to extend such prohibitions or requirements to our operations.
Insurance Laws and Regulation
States in which we operate have adopted certain laws and regulations affecting risk assumption in the healthcare industry, including those that subject any physician or physician network engaged in risk-based managed care to applicable insurance laws and regulations. These laws and regulations may require physicians and physician networks to meet minimum capital requirements and other safety and soundness requirements. Implementing additional regulations or compliance requirements could result in substantial costs to the contracted radiology practices, limiting their ability to enter into capitated or other risk-sharing managed care arrangements and indirectly affecting our revenue from the contracted practices.
U.S. Federal Budget
We derive a substantial portion of our revenue from direct billings to governmental healthcare programs, such as Medicare and Medicaid, and private health insurance companies and/or health plans, including but not limited to those participating in the Medicare Advantage program. As a result, any negative changes in governmental capitation or fee-for-service rates or methods of reimbursement for the services we provide could have a significant adverse impact on our revenue and financial results.
Because governmental healthcare programs generally reimburse on a fee schedule basis rather than on a charge-related basis, we generally cannot increase our revenues from these programs by increasing the amount of charges for services. Moreover, if our costs increase, we may not be able to recover our increased costs from these programs. Government and private payors have taken and may continue to take steps to control the cost, eligibility for, use, and delivery of healthcare services as a result of budgetary constraints, cost containment pressures and other reasons. We believe that these trends in cost containment will continue. These cost containment measures, and other market changes in non-governmental insurance plans have generally restricted our ability to recover, or shift to non-governmental payors, any increased costs that we experience. Our integrated care business and financial operations may be materially affected by these developments.
Environmental Matters
The facilities we operate or manage generate hazardous and medical waste subject to federal and state requirements regarding handling and disposal. We believe that the facilities that we operate and manage are currently in compliance in all material respects with applicable federal, state and local statutes and ordinances regulating the handling and disposal of such materials. We do not believe that we will be required to expend any material additional amounts in order to remain in compliance with these laws and regulations or that compliance will materially affect our capital expenditures, earnings or competitive position.
| 19 |
Compliance Program
We maintain a program to monitor compliance with federal and state laws and regulations applicable to healthcare entities. We have a compliance officer who is charged with implementing and supervising our compliance program, which includes the adoption of (i) Standards of Conduct for our employees and affiliates and (ii) a process that specifies how employees, affiliates and others may report regulatory or ethical concerns to our compliance officer. We believe that our compliance program meets the relevant standards provided by the Office of Inspector General of the Department of Health and Human Services.
An important part of our compliance program consists of conducting periodic audits of various aspects of our operations and that of the contracted radiology practices. We also conduct mandatory educational programs designed to familiarize our employees with the regulatory requirements and specific elements of our compliance program.
| Item 1A. | Risk Factors |
If BRMG or any of our other contracted radiology practices terminate their agreements with us, our business could substantially diminish.
Our relationship with BRMG is an integral part of our business. Through our management agreement, BRMG provides all of the professional medical services at 127 of our 132 California facilities. Professional medical services are provided at our other facilities through management contracts with IA, the NY Groups, and other radiology groups. BRMG and these other radiology groups contract with various other independent physicians and physician groups to provide all of the professional medical services at most of our facilities, and they must use their best efforts to provide the professional medical services at any new facilities that we open or acquire in their areas of operation. In addition, BRMG and the other radiology groups’ strong relationships with referring physicians are largely responsible for the revenue generated at the facilities they service. Although our management agreement with BRMG runs until 2024, with automatic renewals for 10-year periods, and our management agreements with other groups are also for multiple years, BRMG and the other radiology groups have the right to terminate the agreements if we default on our obligations and fail to cure the default. Also, the various radiology groups’ ability to continue performing under the management agreements may be curtailed or eliminated due to the groups’ financial difficulties, loss of physicians or other circumstances. If the radiology groups cannot perform their obligations to us, we would need to contract with one or more other radiology groups to provide the professional medical services at the facilities serviced by the group. We may not be able to locate radiology groups willing to provide those services on terms acceptable to us, if at all. Even if we were able to do so, any replacement radiology group’s relationships with referring physicians may not be as extensive as those of the terminated group. In any such event, our business could be seriously harmed. In addition, the radiology groups are party to substantially all of the managed care contracts from which we derive revenue. If we were unable to readily replace these contracts, our revenue would be negatively affected.
We may experience risks associated with our strategic partnership with Imaging Advantage LLC
In December 2015, we entered into a multi-year strategic relationship with Imaging Advantage LLC. Under the terms of such agreement, we have agreed to collaborate to deploy innovative models of delivering radiology services. While we expect this strategic relationship to increase our profitability and expand our operations, we may never realize the anticipated benefits of such relationship.
Our ability to generate revenue depends in large part on referrals from physicians.
We derive substantially all of our net revenue, directly or indirectly, from fees charged for the diagnostic imaging services performed at our facilities. We depend on referrals of patients from unaffiliated physicians and other third parties who have no contractual obligations to refer patients to us for a substantial portion of the services we perform. If a sufficiently large number of these physicians and other third parties were to discontinue referring patients to us, our scan volume could decrease, which would reduce our net revenue and operating margins. Further, commercial third-party payors have implemented programs that could limit the ability of physicians to refer patients to us. For example, prepaid healthcare plans, such as health maintenance organizations, sometimes contract directly with providers and require their enrollees to obtain these services exclusively from those providers. Some insurance companies and self-insured employers also limit these services to contracted providers. These “closed panel” systems are now common in the managed care environment. Other systems create an economic disincentive for referrals to providers outside the system’s designated panel of providers. If we are unable to compete successfully for these managed care contracts, our results and prospects for growth could be adversely affected.
| 20 |
If our contracted radiology practices, including BRMG and the NY Groups, lose a significant number of their radiologists, our financial results could be adversely affected.
At times, there has been a shortage of qualified radiologists in some of the regional markets we serve. In addition, competition in recruiting radiologists may make it difficult for our contracted radiology practices to maintain adequate levels of radiologists. If a significant number of radiologists terminate their relationships with our contracted radiology practices and those radiology practices cannot recruit sufficient qualified radiologists to fulfill their obligations under our agreements with them, our ability to maximize the use of our diagnostic imaging facilities and our financial results could be adversely affected. Increased expenses to BRMG and the NY Groups will impact our financial results because the management fee we receive from BRMG and the NY Groups, which is based on a percentage of their collections, is adjusted annually to take into account the expenses of BRMG or the NY Groups, as applicable. Neither we, nor our contracted radiology practices, maintain insurance on the lives of any affiliated physicians.
We may become subject to professional malpractice liability, which could be costly and negatively impact our business.
The physicians employed by our contracted radiology practices are from time to time subject to malpractice claims. We structure our relationships with the practices under our management agreements in a manner that we believe does not constitute the practice of medicine by us or subject us to professional malpractice claims for acts or omissions of physicians employed by the contracted radiology practices. Nevertheless, claims, suits or complaints relating to services provided by the contracted radiology practices have been asserted against us in the past and may be asserted against us in the future. In addition, we may be subject to professional liability claims, including, without limitation, for improper use or malfunction of our diagnostic imaging equipment or for accidental contamination or injury from exposure to radiation. We may not be able to maintain adequate liability insurance to protect us against those claims at acceptable costs or at all.
Historically, we have sought to manage this risk of loss by, among other things, purchasing professional liability insurance. However, the insurer from which we purchased such insurance for the period ending July 15, 2017, Fairway Physicians Insurance Company, A Risk Retention Group (“Fairway”), recently experienced financial hardship. As a result, on August 29, 2017, the District of Columbia Department of Insurance, Securities and Banking (“DISB”) found that Fairway was statutorily insolvent and that its continued operation would be hazardous to its policyholders, creditors and the general public. On October 25, 2017, the Superior Court for the District of Columbia issued an order authorizing the DISB Commissioner to liquidate Fairway. Fairway’s liquidation is currently pending, and it is presently unknown whether the Fairway liquidation estate will be able to pay covered policyholder claims, including claims asserted against us.
Any claim made against us that is not fully covered by insurance could be costly to defend, result in a substantial damage award against us and divert the attention of our management from our operations, all of which could have an adverse effect on our financial performance. In addition, successful claims against us may adversely affect our business or reputation. Although California places a $250,000 limit on non-economic damages for medical malpractice cases, no limit applies to economic damages and no such limits exist in the other states in which we provide services.
We may not receive payment from some of our healthcare provider customers because of their financial circumstances.
Some of our healthcare provider customers do not have significant financial resources, liquidity or access to capital. If these customers experience financial difficulties they may be unable to pay us for the equipment and services that we provide. A significant deterioration in general or local economic conditions could have a material adverse effect on the financial health of certain of our healthcare provider customers. As a result, we may have to increase the amounts of accounts receivables that we write-off, which would adversely affect our financial condition and results of operations.
Capitation fee arrangements could reduce our operating margins.
For the year ended December 31, 2017, we derived approximately 11.5% of our net service fee revenue before provision for bad debt from capitation arrangements, and we intend to increase the revenue we derive from capitation arrangements in the future. Under capitation arrangements, the payor pays a pre-determined amount per-patient per-month in exchange for us providing all necessary covered services to the patients covered under the arrangement. These contracts pass much of the financial risk of providing diagnostic imaging services, including the risk of over-use, from the payor to the provider. Our success depends in part on our ability to negotiate effectively, on behalf of the contracted radiology practices and our diagnostic imaging facilities, contracts with health maintenance organizations, employer groups and other third-party payors for services to be provided on a capitated basis and to efficiently manage the utilization of those services. If we are not successful in managing the utilization of services under these capitation arrangements or if patients or enrollees covered by these contracts require more frequent or extensive care than anticipated, we would incur unanticipated costs not offset by additional revenue, which would reduce operating margins.
| 21 |
Changes in the method or rates of third-party reimbursement could have a negative impact on our results
From time to time, changes designed to contain healthcare costs have been implemented, some of which have resulted in decreased reimbursement rates for diagnostic imaging services that impact our business. For services for which we bill Medicare directly, we are paid under the Medicare Physician Fee Schedule, which is updated on an annual basis. Under the Medicare statutory formula, payments under the Physician Fee Schedule would have decreased for the past several years if Congress failed to intervene.
Medicare program reimbursements for physician services as well as other services to Medicare beneficiaries who are not enrolled in Medicare Advantage plans are based upon the fee-for-service rates set forth in the Medicare Physician Fee Schedule, which relies, in part, on a target-setting formula system called the Sustainable Growth Rate or SGR. Each year, on January 1st, the Medicare program updates the Medicare Physician Fee Schedule reimbursement rates. Many private payors use the Medicare Physician Fee Schedule to determine their own reimbursement rates.
On April 16, 2015, President Obama signed into law the Medicare Access and CHIP Reauthorization Act (H.R. 2), which provides for sweeping changes to how Medicare pays physicians, as well as averts the 21% reduction to Medicare payments under the Medicare Physician Fee Schedule that was scheduled to take effect on April 1, 2016. H.R. 2, among other things, repealed the SGR formula. The SGR formula was enacted in 1997 and was linked to the growth in the U.S. gross domestic product, which led Congress to repeatedly intervene to mitigate the negative reimbursement impact associated with it. H.R. 2 provides that for services paid under the physician fee schedule and furnished during calendar years 2016 through 2019, Medicare’s payment rates will increase by 0.5% per year over calendar year 2015. Fees will remain at the 2019 level through 2025, but providers have the ability to participate in the Quality Payment Program (“QPP”) and have the opportunity for additional payments. Under one track, incentive payments will be based upon participating in an innovative payment model (e.g., participating in the Medicare Shared Savings Program), and under the other track, incentive payments will be based upon quality, resource use, clinical practice improvement activities and meaningful use of electronic health record technology. Given that the QPP remains under CMS’ continued development, we cannot determine the impact of such payments models on our business at this time. However, in general, shifting to value-based care may decrease our revenue and require us to invest heavily in new IT infrastructure and analytic tools.
In 2013, Congress adjusted Medicare payment rates for physician imaging services in an attempt to better reflect actual usage, by revising upward the assumed usage rate for diagnostic imaging equipment costing more than $1 million to 90% effective January, 1, 2014. Additionally, under the Protecting Access to Medicare Act of 2014 (“PAMA”), Congress introduced a new quality incentive program that, effective January 1, 2016, reduces Medicare payment for certain CT services reimbursed through the Medicare Physician Fee Schedule that are furnished using equipment that does not meet certain dose optimization and management standards. Other changes in reimbursement for services rendered by Medicare Advantage plans may reduce the revenues we receive for services rendered to Medicare Advantage enrollees.
Pressure to control healthcare costs could have a negative impact on our results.
One of the principal objectives of health maintenance organizations and preferred provider organizations is to control the cost of healthcare services. Healthcare providers participating in managed care plans may be required to refer diagnostic imaging tests to certain providers depending on the plan in which a covered patient is enrolled. In addition, managed care contracting has become very competitive, and reimbursement schedules are at or below Medicare reimbursement levels. The expansion of health maintenance organizations, preferred provider organizations and other managed care organizations within the geographic areas covered by our network could have a negative impact on the utilization and pricing of our services, because these organizations will exert greater control over patients’ access to diagnostic imaging services, the selections of the provider of such services and reimbursement rates for those services.
We experience competition from other diagnostic imaging companies and hospitals, and this competition could adversely affect our revenue and business.
The market for diagnostic imaging services is highly competitive. We compete for patients principally on the basis of our reputation, our ability to provide multiple modalities at many of our facilities, the location of our facilities and the quality of our diagnostic imaging services. We compete locally with groups of radiologists, established hospitals, clinics and other independent organizations that own and operate imaging equipment. Our competitors include the privately held Alliance Healthcare Services, Inc., to the extent it sells diagnostic imaging services directly to outpatients, Diagnostic Imaging Group, and several smaller regional competitors. Some of our competitors may now or in the future have access to greater financial resources than we do and may have access to newer, more advanced equipment. In addition, some physician practices have established their own diagnostic imaging facilities within their group practices and compete with us. We are experiencing increased competition as a result of such activities, and if we are unable to successfully compete, our business and financial condition would be adversely affected.
| 22 |
Our success depends in part on our key personnel and loss of key executives could adversely affect our operations. In addition, former employees and radiology practices we have previously contracted with could use the experience and relationships developed while employed or under contract with us to compete with us.
Our success depends in part on our ability to attract and retain qualified senior and executive management, and managerial and technical personnel. Competition in recruiting these personnel may make it difficult for us to continue our growth and success. The loss of their services or our inability in the future to attract and retain management and other key personnel could hinder the implementation of our business strategy. The loss of the services of Dr. Howard G. Berger, our President and Chief Executive Officer, and Norman R. Hames or Stephen M. Forthuber, our Chief Operating Officers, West Coast and East Coast, respectively, could have a significant negative impact on our operations. We believe that they could not easily be replaced with executives of equal experience and capabilities. We do not maintain key person insurance on the life of any of our executive officers. Additionally, if we lose the services of Dr. Berger, our relationship with BRMG could deteriorate, which would materially adversely affect our business.
Many of the states in which we operate do not enforce agreements that prohibit a former employee from competing with a former employer. As a result, many of our employees whose employment is terminated are free to compete with us, subject to prohibitions on the use of trade secret information and, depending on the terms of the employee’s employment agreement, on solicitation of existing employees and customers (if enforceable). A former executive, manager or other key employee who joins one of our competitors could use the relationships he or she established with third party payors, radiologists or referring physicians while our employee and the industry knowledge he or she acquired during that tenure to enhance the new employer’s ability to compete with us.
The agreements with most of our radiology practices contain non-compete provisions; however the enforceability of these provisions is determined by a court based on all the facts and circumstances of the specific case at the time enforcement is sought. Our inability to enforce radiologists’ non-compete provisions could result in increased competition from individuals who are knowledgeable about our business strategies and operations.
Our failure to successfully, and in a timely manner, integrate similar businesses and/or new lines of businesses we acquire could reduce our profitability.
We may never realize expected synergies, business opportunities and growth prospects in connection with our acquisitions and joint ventures. We may not be able to capitalize on expected business opportunities, assumptions underlying estimates of expected cost savings may be inaccurate, or general industry and business conditions may deteriorate. In addition, integrating operations will require significant efforts and expenses on our part. Personnel may leave or be terminated because of an acquisition. Our management may have its attention diverted while trying to integrate an acquisition. If these factors limit our ability to integrate the operations of an acquisition successfully or on a timely basis, our expectations of future results of operations, including certain cost savings and synergies as a result of the acquisition, may not be met. In addition, our growth and operating strategies for a target’s business may be different from the strategies that the target company pursued prior to our acquisition. If our strategies are not the proper strategies, they could have a material adverse effect on our business, financial condition and results of operations.
In the past we have acquired, and may again in the future acquire, companies that create a new line of business. The process of integrating the acquired business, technology, service and research and development component into our business and operations and entry into a new line of business in which we are inexperienced may result in unforeseen operating difficulties and expenditures. In developing a new line of business we may invest significant time and resources that take away the attention of management that would otherwise be available for ongoing development of our business which may affect our results of operations and we may not be able to take full advantage of the business opportunities available to us as we expand a new lines of business. In addition, there can be no assurance that our new lines of business will ultimately be successful. The failure to successfully manage these risks in the development and implementation of new lines of business could have a material, adverse effect on the Company’s business, financial condition, and results of operations.
| 23 |
We may not be able to successfully grow our business, which would adversely affect our financial condition and results of operations.
Historically, we have experienced substantial growth through acquisitions that have increased our size, scope and geographic distribution. During the past two fiscal years, we have completed 8 acquisitions. These acquisitions have added 13 centers to our fixed-site outpatient diagnostic imaging services. Our ability to successfully expand through acquiring facilities, developing new facilities, adding equipment at existing facilities, and directly or indirectly entering into contractual relationships with high-quality radiology practices depends upon many factors, including our ability to:
| · | identify attractive and willing candidates for acquisitions; |
| · | identify locations in existing or new markets for development of new facilities; |
| · | comply with legal requirements affecting our arrangements with contracted radiology practices, including state prohibitions on fee-splitting, corporate practice of medicine and self-referrals; |
| · | obtain regulatory approvals where necessary and comply with licensing and certification requirements applicable to our diagnostic imaging facilities, the contracted radiology practices and the physicians associated with the contracted radiology practices; |
| · | recruit a sufficient number of qualified radiology technologists and other non-medical personnel; |
| · | expand our infrastructure and management; and |
| · | compete for opportunities. |
We may not be able to compete effectively for the acquisition of diagnostic imaging facilities. Our competitors may have more established operating histories and greater resources than we do. Competition may also make any acquisitions more expensive.
Managing our recent acquisitions, as well as any other future acquisitions, will entail numerous operational and financial risks, including:
| · | inability to obtain adequate financing; |
| · | failure to achieve our targeted operating results; |
| · | diversion of management’s attention and resources; |
| · | failure to retain key personnel; |
| · | difficulties in integrating new operations into our existing infrastructure; and |
| · | amortization or write-offs of acquired intangible assets, including goodwill. |
If we are unable to successfully grow our business through acquisitions it could have an adverse effect on our financial condition and results of operations. Further we cannot ensure we will be able to receive the required regulatory approvals for any future acquisitions, expansions or replacements, and the failure to obtain these approvals could limit the market for our services and have an adverse effect on our financial condition and results of operations.
We have experienced operating losses in the past. If we are unable to continue to generate sufficient income, we may be unable to pay our obligations.
We had income before taxes of $26.4 million, $12.4 million, and $14.6 million for the years ended December 31, 2017, 2016, and 2015 respectively. As of December 31, 2017, our equity was $69.9 million. As a whole, results have shown improvement over the past three years. However, if we cannot continue to generate income in sufficient amounts, we will not be able to pay our obligations as they become due, which could adversely impact our business, financial condition and results of operations.
| 24 |
Our substantial debt could adversely affect our financial condition and prevent us from fulfilling our obligations under our outstanding indebtedness.
Our current substantial indebtedness and any future indebtedness we incur could adversely affect our financial condition. We are highly leveraged. As of December 31, 2017, our total combined indebtedness of term loans, capital leases and notes payable, excluding discount on term loan debt, was $627.6 million, $620.3 million of which constituted first lien term loan indebtedness. Our substantial indebtedness could also:
| · | make it difficult for us to satisfy our payment obligations with respect to our outstanding indebtedness; |
| · | require us to dedicate a substantial portion of our cash flow from operations to payments on our debt, reducing the availability of our cash flow to fund working capital, capital expenditures, acquisitions and other general corporate purposes; |
| · | expose us to the risk of interest rate increases on our variable rate borrowings, including borrowings under our new senior secured credit facilities; |
| · | increase our vulnerability to adverse general economic and industry conditions; |
| · | limit our flexibility in planning for, or reacting to, changes in our business and the industry in which we operate; |
| · | place us at a competitive disadvantage compared to our competitors that have less debt; and |
| · | limit our ability to borrow additional funds on terms that are satisfactory to us or at all. |
We could be subject to tax audits, challenges to its tax positions, or adverse changes or interpretations of tax laws.
We are subject to federal and applicable state income tax laws and regulations. Income tax laws and regulations are often complex and require significant judgment in determining our effective tax rate and in evaluating our tax positions. Our determination of our tax liability is subject to review by applicable tax authorities. Any audits or challenges of such determinations may adversely affect our effective tax rate, tax payments or financial condition. Recently enacted U.S. tax legislation made significant changes to federal tax law, including the taxation of corporations, by, among other things, reducing the corporate income tax rate, disallowing certain deductions that had previously been allowed, and altering the expensing of capital expenditures. The implementation and evaluation of these changes may require significant judgment and substantial planning. These judgments and plans may require the US to take new and different tax positions that if challenged could adversely affect our effective tax rate, tax payments or financial condition.
In addition, the new tax legislation remains subject to potential amendments, technical corrections, and further regulatory guidance and interpretation, any of which could lessen or increase certain adverse impacts on us. Furthermore, as the new tax legislation goes into effect, future changes may occur at the federal or state level that could result in unfavorable adjustments to our tax liability.
Increases in interest rates could increase the amount of our debt payments and reduce out operating cash flows.
We have incurred significant indebtedness that accrues interest at variable rate borrowing and we may incur additional debt in the future. Increases in interest rates on our current outstanding debt or any other debt we may incur will reduce our operating cash flows and if we need to repay any of our variable rate borrowing during period of high interest rates, we could be required to forgo other opportunities in order to repay the debt which may not permit us to realize future earnings of those forgone opportunities. To mitigate this risk, we have entered into an interest rate cap contract on our term loan debt facilities. See note 8 in the notes to financial statements contained herein.
| 25 |
We may not be able to finance future needs or adapt our business plan to changes because of restrictions placed on us by our credit facilities and instruments governing our other indebtedness.
Our credit facilities contain affirmative and negative covenants which restrict, among other things, our ability to:
| · | pay dividends or make certain other restricted payments or investments; |
| · | incur additional indebtedness and certain disqualified equity interests; |
| · | create liens (other than permitted liens) securing indebtedness or trade payables; |
| · | sell certain assets or merge with or into other companies or otherwise dispose of all or substantially all of our assets; |
| · | enter into certain transactions with affiliates; |
| · | create restrictions on dividends or other payments by our restricted subsidiaries; and |
| · | create guarantees of indebtedness by restricted subsidiaries. |
All of these restrictions could affect our ability to operate our business and may limit our ability to take advantage of potential business opportunities as they arise. A failure to comply with these covenants and restrictions would permit the relevant creditors to declare all amounts borrowed under the applicable agreement governing such indebtedness, together with accrued interest and fees, to be immediately due and payable. If the indebtedness under our credit facilities is accelerated, we may not have sufficient assets to repay amounts due under the credit facilities or on other indebtedness then outstanding.
A restriction in our ability to make capital expenditures would restrict our growth and could adversely affect our business.
We operate in a capital intensive, high fixed-cost industry that requires significant amounts of capital to fund operations, particularly the initial start-up and development expenses of new diagnostic imaging facilities and the acquisition of additional facilities and new diagnostic imaging equipment. We incur capital expenditures to, among other things, upgrade and replace equipment for existing facilities and expand within our existing markets and enter new markets. If we open or acquire additional imaging facilities, we may have to incur material capital lease obligations. To the extent we are unable to generate sufficient cash from our operations, funds are not available from our lenders or we are unable to structure or obtain financing through operating leases, long-term installment notes or capital leases, we may be unable to meet our capital expenditure requirements to support the maintenance and continued growth of our operations.
We may be impacted by eligibility changes to government and private insurance programs.
Due to potential decreased availability of healthcare through private employers, the number of patients who are uninsured or participate in governmental programs may increase. Healthcare reform legislation will increase the participation of individuals in the Medicaid program in states that elect to participate in the expanded Medicaid coverage. A shift in payor mix from managed care and other private payors to government payors as well as an increase in the number of uninsured patients may result in a reduction in the rates of reimbursement or an increase in uncollectible receivables or uncompensated care, with a corresponding decrease in net revenue. Changes in the eligibility requirements for governmental programs such as the Medicaid program and state decisions on whether to participate in the expansion of such programs also could increase the number of patients who participate in such programs and the number of uninsured patients. Even for those patients who remain in private insurance plans, changes to those plans could increase patient financial responsibility, resulting in a greater risk of uncollectible receivables. Furthermore, additional changes to, or repeal of, the PPACA under the Trump Administration may also affect reimbursement and coverage in ways that are currently unpredictable. These factors and events could have a material adverse effect on our business, financial condition, and results of operations.
Our business could be adversely impacted if there are deficiencies in our disclosure controls and procedures or internal control over financial reporting.
The design and effectiveness of our disclosure controls and procedures and internal control over financial reporting may not prevent all errors, misstatements or misrepresentations. While management will review the effectiveness of our disclosure controls and procedures and internal control over financial reporting, there can be no guarantee that our disclosure controls and procedures or our internal control over financial reporting will be effective in accomplishing all control objectives all of the time. Deficiencies, including any material weakness, in our internal control over financial reporting that may occur in the future could result in misstatements of our results of operations, restatements of our financial statements, or otherwise adversely impact our financial condition, results of operations, cash flows, and our ability to satisfy our debt service obligations. As of December 31, 2017, we have identified a material weakness in internal controls with respect to our processes surrounding the occurrence and measurement of revenue and valuation of accounts receivable. See Item 9 for further information.
| 26 |
The regulatory framework in which we operate is uncertain and evolving.
Although we believe that we are operating in compliance with applicable federal and state laws, neither our current or anticipated business operations nor the operations of the contracted radiology practices have been the subject of judicial or regulatory interpretation. We cannot assure you that a review of our business by courts or regulatory authorities will not result in a determination that could adversely affect our operations or that the healthcare regulatory environment will not change in a way that restricts our operations. In addition, healthcare laws and regulations may change significantly in the future. We continuously monitor these developments and modify our operations from time to time as the regulatory environment changes. We cannot assure you however, that we will be able to adapt our operations to address new regulations or that new regulations will not adversely affect our business.
Certain states have enacted statutes or adopted regulations affecting risk assumption in the healthcare industry, including statutes and regulations that subject any physician or physician network engaged in risk-based managed care contracting to applicable insurance laws and regulations. These laws and regulations, if adopted in the states in which we operate, may require physicians and physician networks to meet minimum capital requirements and other safety and soundness requirements. Implementing additional regulations or compliance requirements could result in substantial costs to us and the contracted radiology practices and limit our ability to enter into capitation or other risk-sharing managed care arrangements.
State and federal anti-kickback and anti-self-referral laws may adversely affect income.
Various federal and state laws govern financial arrangements among healthcare providers. The federal Anti-Kickback Law prohibits the knowing and willful offer, payment, solicitation or receipt of any form of remuneration in return for, or to induce, the referral of Medicare, Medicaid, or other federal healthcare program patients, or in return for, or to induce, the purchase, lease or order of items or services that are covered by Medicare, Medicaid, or other federal healthcare programs. Similarly, many state laws prohibit the solicitation, payment or receipt of remuneration in return for, or to induce the referral of patients in private as well as government programs. Violation of these Anti-Kickback Laws may result in substantial civil or criminal penalties for individuals or entities and/or exclusion from federal or state healthcare programs. We believe we are operating in compliance with applicable law and believe that our arrangements with providers would not be found to violate the Anti-Kickback Laws. However, these laws could be interpreted in a manner inconsistent with our operations.
Federal law prohibiting physician self-referrals, known as the Stark Law, prohibits a physician from referring Medicare or Medicaid patients to an entity for certain “designated health services” if the physician has a prohibited financial relationship with that entity, unless an exception applies. Certain radiology services are considered “designated health services” under the Stark Law. Although we believe our operations do not violate the Stark Law, our activities may be challenged. If a challenge to our activities is successful, it could have an adverse effect on our operations. In addition, legislation may be enacted in the future that further addresses Medicare and Medicaid fraud and abuse or that imposes additional requirements or burdens on us.
In addition, under the DRA, states enacting false claims statutes similar to the federal False Claims Act, which establish liability for submission of fraudulent claims to the State Medicaid program and contain qui tam or whistleblower provisions, receive an increased percentage of any recovery from a State Medicaid judgment or settlement. Adoption of new false claims statutes in states where we operate may impose additional requirements or burdens on us.
Federal and state privacy and information security laws are complex, and if we fail to comply with applicable laws, regulations and standards, or if we fail to properly maintain the integrity of our data, protect our proprietary rights to our systems, or defend against cybersecurity attacks, we may be subject to government or private actions due to privacy and security breaches, and our business, reputation, results of operations, financial position and cash flows could be materially and adversely affected.
We must comply with numerous federal and state laws and regulations governing the collection, dissemination, access, use, security and privacy of PHI, including HIPAA and its implementing privacy and security regulations, as amended by the federal HITECH Act and collectively referred to as HIPAA. If we fail to comply with applicable privacy and security laws, regulations and standards, properly maintain the integrity of our data, protect our proprietary rights to our systems, or defend against cybersecurity attacks, our business, reputation, results of operations, financial position and cash flows could be materially and adversely affected.
Information security risks have significantly increased in recent years in part because of the proliferation of new technologies, the use of the internet and telecommunications technologies to conduct our operations, and the increased sophistication and activities of organized crime, hackers, terrorists and other external parties, including foreign state agents. Our operations rely on the secure processing, transmission and storage of confidential, proprietary and other information in our computer systems and networks.
| 27 |
We are continuously implementing multiple layers of security measures through technology, processes, and our people; utilize current security technologies; and our defenses are monitored and routinely tested internally and by external parties. Despite these efforts, our facilities and systems may be vulnerable to privacy and security incidents; security attacks and breaches; acts of vandalism or theft; computer viruses; coordinated attacks by activist entities; emerging cybersecurity risks; misplaced or lost data; programming and/or human errors; or other similar events. Emerging and advanced security threats, including coordinated attacks, require additional layers of security which may disrupt or impact efficiency of operations.
Any security breach involving the misappropriation, loss or other unauthorized disclosure or use of confidential information, including protected health information, financial data, competitively sensitive information, or other proprietary data, whether by us or a third party, could have a material adverse effect on our business, reputation, financial condition, cash flows, or results of operations. The occurrence of any of these events could result in interruptions, delays, the loss or corruption of data, cessations in the availability of systems or liability under privacy and security laws, all of which could have a material adverse effect on our financial position and results of operations and harm our business reputation. If we are unable to protect the physical and electronic security and privacy of our databases and transactions, we could be subject to potential liability and regulatory action, our reputation and relationships with our patients and vendors would be harmed, and our business, operations, and financial results may be materially adversely affected. Failure to adequately protect and maintain the integrity of our information systems (including our networks) and data, or to defend against cybersecurity attacks, could subject us to monetary fines, civil suits, civil penalties or criminal sanctions and requirements to disclose the breach publicly, and may further result in a material adverse effect on our results of operations, financial position, and cash flows.
Complying with federal and state regulations is an expensive and time-consuming process, and any failure to comply could result in substantial penalties.
We are directly or indirectly, through the radiology practices with which we contract, subject to extensive regulation by both the federal government and the state governments in which we provide services, including:
| · | the federal False Claims Act; |
| · | the federal Medicare and Medicaid Anti-Kickback Laws, and state anti-kickback prohibitions; |
| · | federal and state billing and claims submission laws and regulations; |
| · | the federal Health Insurance Portability and Accountability Act of 1996, as amended by the Health Information Technology for Economic and Clinical Health Act of 2009, and comparable state laws; |
| · | the federal physician self-referral prohibition commonly known as the Stark Law and the state equivalent of the Stark Law; |
| · | state laws that prohibit the practice of medicine by non-physicians and prohibit fee-splitting arrangements involving physicians; |
| · | federal and state laws governing the diagnostic imaging and therapeutic equipment we use in our business concerning patient safety, equipment operating specifications and radiation exposure levels; and |
| · | state laws governing reimbursement for diagnostic services related to services compensable under workers compensation rules. |
If our operations are found to be in violation of any of the laws and regulations to which we or the radiology practices with which we contract are subject, we may be subject to the applicable penalty associated with the violation, including civil and criminal penalties, damages, fines and the curtailment of our operations. Any penalties, damages, fines or curtailment of our operations, individually or in the aggregate, could adversely affect our ability to operate our business and our financial results. The risks of our being found in violation of these laws and regulations is increased by the fact that many of them have not been fully interpreted by the regulatory authorities or the courts, and their provisions are open to a variety of interpretations. Any action brought against us for violation of these laws or regulations, even if we successfully defend against it, could cause us to incur significant legal expenses and divert our management’s attention from the operation of our business.
| 28 |
If we fail to comply with various licensure, certification and accreditation standards, we may be subject to loss of licensure, certification or accreditation, which would adversely affect our operations.
Ownership, construction, operation, expansion and acquisition of our diagnostic imaging facilities are subject to various federal and state laws, regulations and approvals concerning licensing of personnel, other required certificates for certain types of healthcare facilities and certain medical equipment. In addition, freestanding diagnostic imaging facilities that provide services independent of a physician’s office must be enrolled by Medicare as an independent diagnostic treatment facility, or IDTF, to bill the Medicare program. Medicare carriers have discretion in applying the IDTF requirements and therefore the application of these requirements may vary from jurisdiction to jurisdiction. In addition, federal legislation requires all suppliers that provide the technical component of diagnostic MRI, PET/CT, CT, and nuclear medicine to be accredited by an accreditation organization designated by CMS (which currently include the American College of Radiology (ACR), the Intersocietal Accreditation Commission (IAC) and the Joint Commission). Our MRI, CT, nuclear medicine, ultrasound and mammography facilities are currently accredited by the American College of Radiology. We may not be able to receive the required regulatory approvals or accreditation for any future acquisitions, expansions or replacements, and the failure to obtain these approvals could limit the opportunity to expand our services.
Our facilities are subject to periodic inspection by governmental and other authorities to assure continued compliance with the various standards necessary for licensure and certification. If any facility loses its certification under the Medicare program, then the facility will be ineligible to receive reimbursement from the Medicare and Medicaid programs. For the year ended December 31, 2017, approximately 23% of our net service fee revenue before provision for bad debt came from the Medicare and Medicaid programs. A change in the applicable certification status of one of our facilities could adversely affect our other facilities and in turn us as a whole. Credentialing of physicians is required by our payors prior to commencing payment. We have experienced a slowdown in the credentialing of our physicians over the last several years which has lengthened our billing and collection cycle, and could negatively impact our ability to collect revenue from patients covered by Medicare.
Our agreements with the contracted radiology practices must be structured to avoid the corporate practice of medicine and fee-splitting.
State law prohibits us from exercising control over the medical judgments or decisions of physicians and from engaging in certain financial arrangements, such as splitting professional fees with physicians. These laws are enforced by state courts and regulatory authorities, each with broad discretion. A component of our business has been to enter into management agreements with radiology practices. We provide management, administrative, technical and other non-medical services to the radiology practices in exchange for a service fee typically based on a percentage of the practice’s revenue. We structure our relationships with the radiology practices, including the purchase of diagnostic imaging facilities, in a manner that we believe keeps us from engaging in the practice of medicine or exercising control over the medical judgments or decisions of the radiology practices or their physicians, or violating the prohibitions against fee-splitting. There can be no assurance that our present arrangements with BRMG or the physicians providing medical services and medical supervision at our imaging facilities will not be challenged, and, if challenged, that they will not be found to violate the corporate practice of medicine or fee splitting prohibitions, thus subjecting us to potential damages, injunction and/or civil and criminal penalties or require us to restructure our arrangements in a way that would affect the control or quality of our services and/or change the amounts we receive under our management agreements. Any of these results could jeopardize our business.
Some of our imaging modalities use radioactive materials, which generate regulated waste and could subject us to liabilities for injuries or violations of environmental and health and safety laws.
Some of our imaging procedures use radioactive materials, which generate medical and other regulated wastes. For example, patients are injected with a radioactive substance before undergoing a PET scan. Storage, use and disposal of these materials and waste products present the risk of accidental environmental contamination and physical injury. We are subject to federal, state and local regulations governing storage, handling and disposal of these materials. We could incur significant costs and the diversion of our management’s attention in order to comply with current or future environmental and health and safety laws and regulations. Also, we cannot completely eliminate the risk of accidental contamination or injury from these hazardous materials. Although we maintain professional liability insurance coverage in amounts we believe is consistent with industry practice in the event of an accident, we could be held liable for any resulting damages, and any liability could exceed the limits of or fall outside the coverage of our professional liability insurance.
| 29 |
Technological change in our industry could reduce the demand for our services and require us to incur significant costs to upgrade our equipment.
The development of new technologies or refinements of existing modalities may require us to upgrade and enhance our existing equipment before we may otherwise intend. Many companies currently manufacture diagnostic imaging equipment. Competition among manufacturers for a greater share of the diagnostic imaging equipment market may result in technological advances in the speed and imaging capacity of new equipment. This may accelerate the obsolescence of our equipment, and we may not have the financial ability to acquire the new or improved equipment and may not be able to maintain a competitive equipment base. In addition, advances in technology may enable physicians and others to perform diagnostic imaging procedures without us. If we are unable to deliver our services in the efficient and effective manner that payors, physicians and patients expect our revenue could substantially decrease.
Because we have high fixed costs, lower scan volumes per system could adversely affect our business.
The principal components of our expenses, excluding depreciation, consist of debt service, capital lease payments, compensation paid to technologists, salaries, real estate lease expenses and equipment maintenance costs. Because a majority of these expenses are fixed, a relatively small change in our revenue could have a disproportionate effect on our operating and financial results depending on the source of our revenue. Thus, decreased revenue as a result of lower scan volumes per system could result in lower margins, which could materially adversely affect our business.
We may be unable to effectively maintain our equipment or generate revenue when our equipment is not operational.
Timely, effective service is essential to maintaining our reputation and high use rates on our imaging equipment. Although we have an agreement with GE Medical Systems pursuant to which it maintains and repairs the majority of our imaging equipment, this agreement does not compensate us for loss of revenue when our systems are not fully operational and our business interruption insurance may not provide sufficient coverage for the loss of revenue. Also, GE Medical Systems may not be able to perform repairs or supply needed parts in a timely manner, which could result in a loss of revenue. Therefore, if we experience more equipment malfunctions than anticipated or if we are unable to promptly obtain the service necessary to keep our equipment functioning effectively, our ability to provide services would be adversely affected and our revenue could decline.
Disruption or malfunction in our information systems could adversely affect our business.
We rely on information technology systems to process, transmit and store electronic information. A significant portion of the communication between personnel, customers, business partners, and suppliers depends on information technology. We rely on our information systems to perform functions critical to our ability to operate, including patient scheduling, billing, collections, image storage and image transmission. We also use information technology systems and networks in our operations and supporting departments such as marketing, accounting, finance, and human resources. The future success and growth of our business depends on streamlined processes made available through information systems, global communications, internet activity and other network processes.
Despite our current security measures, our information technology systems, and those of our third-party service providers, may be vulnerable to information security breaches, acts of vandalism, computer viruses and interruption or loss of valuable business data. Our information technology system is vulnerable to damage or interruption from:
| · | earthquakes, fires, floods and other natural disasters; |
| · | power losses, computer systems failures, internet and telecommunications or data network failures, operator negligence, improper operation by or supervision of employees, physical and electronic losses of data and similar events; and |
| · | computer viruses, penetration by hackers seeking to disrupt operations or misappropriate information and other breaches of security. |
We have technology security initiatives and disaster recovery plans in place to mitigate our risk to these vulnerabilities, but these measures may not be adequate or implemented properly to ensure that our operations are not disrupted or that data security breaches do not occur.
We could face attempts by others to gain unauthorized access through the Internet or to introduce malicious software to our information technology systems. If a malicious hacker gained unauthorized access to our systems and network, it could have a material adverse impact on our business or operations. Such incidents, whether or not successful, could result in our incurring significant costs related to, for example, rebuilding internal systems, defending against litigation, responding to regulatory inquiries or actions, paying damages, or taking other remedial steps with respect to third parties. In addition, these threats are constantly changing, thereby increasing the difficulty of successfully defending against them or implementing adequate preventive measures. Accordingly, an extended interruption in our information technology system’s function could significantly curtail, directly and indirectly, our ability to conduct our business and generate revenue.
| 30 |
If our network was compromised, it could give rise to unwanted media attention, materially damage our payor and physician relationships, harm our business, reputation, results of operations, cash flows and financial condition, result in fines or lawsuits, and may increase the costs we incur to protect against such information security breaches, such as increased investment in technology, the costs of compliance with consumer protection laws and costs resulting from consumer fraud. While we maintain cyber liability insurance, our insurance may not be sufficient to protect against all losses we may incur if we suffer significant or multiple attacks.
Adverse changes in general domestic and worldwide economic conditions and instability and disruption of credit markets could adversely affect our operating results, financial condition, or liquidity.
We are subject to risk arising from adverse changes in general domestic and global economic conditions, including recession or economic slowdown and disruption of credit markets. Continued concerns about the systemic impact of potential long-term and wide-spread recession, inflation, energy costs, geopolitical issues, the availability and cost of credit have contributed to increased market volatility and diminished expectations for the United States economy. The United States and other western countries have responded to this economic situation by exercising monetary policy to keep interest rates low. Any significant change in economic conditions or change in fiscal monetary policy could result in material changes in interest rates.
Continued turbulence in domestic and international markets and economies may adversely affect our liquidity and financial condition, and the liquidity and financial condition of our patients. If these market conditions continue, they may increase expenses associated with borrowing, limit our ability and the ability of our patients, to timely replace maturing liabilities, and access the capital markets to meet liquidity needs, resulting in adverse effects on our financial condition and results of operations.
Budget decisions by the California State Legislature could have an impact on our revenue.
132 of our 297 facilities are located in California and one to one-and-one-half percent (1% to 1.5%) of our revenues come from the California Medicaid program. To the extent California is unable to provide these payments on a timely basis, or at all, our revenues will be negatively impacted.
We are vulnerable to earthquakes, harsh weather and other natural disasters.
Our corporate headquarters and 132 of our facilities are located in California, an area prone to earthquakes and other natural disasters. Several of our facilities are located in areas of Florida and the east coast that have suffered from hurricanes and other harsh weather, including winter snow storms that have in the past caused us to close our facilities. An earthquake, harsh weather conditions or other natural disaster could decrease scan volume during affected periods and seriously impair our operations. Damage to our equipment or interruption of our business would adversely affect our financial condition and results of operations.
Possible volatility in our stock price could negatively affect us and our stockholders.
The trading price of our common stock on the NASDAQ Global Market has fluctuated significantly in the past. During the period from January 1, 2016 through December 31, 2017, the trading price of our common stock fluctuated from a high of $11.90 per share to a low of $4.66 per share. In the past, we have experienced a drop in stock price following an announcement of disappointing earnings or earnings guidance. Any such announcement in the future could lead to a similar drop in stock price. The price of our common stock could also be subject to wide fluctuations in the future as a result of a number of other factors, including the following:
| · | changes in expectations as to future financial performance or buy/sell recommendations of securities analysts; |
| · | our, or a competitor’s, announcement of new services, or significant acquisitions, strategic partnerships, joint ventures or capital commitments; and |
| · | the operating and stock price performance of other comparable companies. |
| 31 |
In addition, the U.S. securities markets have experienced significant price and volume fluctuations. These fluctuations often have been unrelated to the operating performance of companies in these markets. Broad market and industry factors may lead to volatility in the price of our common stock, regardless of our operating performance. Moreover, our stock has limited trading volume, and this illiquidity may increase the volatility of our stock price.
In the past, following periods of volatility in the market price of an individual company’s securities, securities class action litigation often has been instituted against that company. The institution of similar litigation against us could result in substantial costs and a diversion of management’s attention and resources, which could negatively affect our business, results of operations or financial condition.
Provisions of the Delaware General Corporation Law and our organizational documents may discourage an acquisition of us.
In the future, we could become the subject of an unsolicited attempted takeover of our company. Although an unsolicited takeover could be in the best interests of our stockholders, our organizational documents and the General Corporation Law of the State of Delaware both contain provisions that will impede the removal of directors and may discourage a third-party from making a proposal to acquire us. For example, the provisions:
| · | permit the board of directors to increase its own size, within the maximum limitations set forth in the bylaws, and fill the resulting vacancies; |
| · | authorize the issuance of shares of preferred stock in one or more series without a stockholder vote; |
| · | establish an advance notice procedure for stockholder proposals to be brought before an annual meeting of our stockholders, including proposed nominations of persons for election to the board of directors; and |
| · | prohibit transfers and/or acquisitions of stock (without consent of the Board of Directors ) that would result in any stockholder owning greater than 5% of the currently outstanding stock resulting in a limitation on net operating loss carryovers, capital loss carryovers, general business credit carryovers, alternative minimum tax credit carryovers and foreign tax credit carryovers, as well as any loss or deduction attributable to a “net unrealized built-in loss” within the meaning of Section 382 of the internal revenue code of 1986, as amended. |
We are subject to Section 203 of the Delaware General Corporation Law, which could have the effect of delaying or preventing a change in control.
| Item 1B. | Unresolved Staff Comments |
None.
| Item 2. | Properties |
Our corporate headquarters is located in adjoining premises at 1508, 1510 and 1516 Cotner Avenue, Los Angeles, California 90025, and approximately 21,500 square feet is occupied under these leases, which expire (with options to extend) on June 30, 2027. We also have a regional office of approximately 39,000 square feet in Baltimore, Maryland under a lease, which expires September 30, 2028. In addition, we lease approximately 62,000 square feet of warehouse space under leases nationwide, which expire at various dates, including options, through August 2031. As of December 31, 2017, total square footage under lease, including medical office, administrative and storage locations was approximately 2.0 million square feet.
We operate 132 fixed-site, freestanding outpatient diagnostic imaging facilities in California, 13 in Delaware, 3 in Florida, 60 in Maryland, 20 in New Jersey, 19 in the Rochester and Hudson Valley areas of New York and 50 in New York City. We lease the premises at which these facilities are located. Our most common initial term varies in length from 5 to 15 years. Including renewal options negotiated with the landlord, we can have a total span of 10 to 25 years at the facilities we lease. We also lease smaller satellite X-Ray locations on mutually renewable terms, usually lasting one year. Rental increases can range from 1% to 7% on an annual basis, depending on the location and market conditions where we do business. We do not have options to purchase the facilities we rent.
| Item 3. | Legal Proceedings |
We are engaged from time to time in the defense of lawsuits arising out of the ordinary course and conduct of our business. We believe that the outcome of our current litigation will not have a material adverse impact on our business, financial condition and results of operations. However, we could be subsequently named as a defendant in other lawsuits that could adversely affect us.
| Item 4. | Mine Safety Disclosures |
Not applicable.
| 32 |
| Item 5. | Market for the Registrant’s Common Equity, Related Stockholder Matters and Issuer Purchases of Equity Securities |
Our common stock is quoted on the NASDAQ Global Market under the symbol “RDNT”. The following table indicates the high and low prices for our common stock for the periods indicated based upon information supplied by the NASDAQ Global Market.
| Low | High | |||||||||
| Quarter Ended | ||||||||||
| December 31, 2017 | $ | 9.50 | $ | 11.90 | ||||||
| September 30, 2017 | 7.45 | 11.90 | ||||||||
| June 30, 2017 | 5.40 | 7.90 | ||||||||
| March 31, 2017 | 5.25 | 6.78 | ||||||||
| December 31, 2016 | $ | 5.35 | $ | 7.98 | ||||||
| September 30, 2016 | 5.28 | 7.42 | ||||||||
| June 30, 2016 | 4.66 | 5.55 | ||||||||
| March 31, 2016 | 4.73 | 6.33 | ||||||||
The last low and high prices for our common stock on the NASDAQ Global Market for the period from January 1 to March 5, 2018 were $9.65 and $10.70, respectively.
Holders
As of March 5, 2018, the number of holders of record of our common stock was 1,083. However, Cede & Co., the nominee for The Depository Trust Company, the clearing agency for most broker-dealers, owned a substantial number of our outstanding shares of common stock of record on that date. Our management believes that the number of beneficial owners of our common stock is approximately 5,000.
Dividends
We have never declared or paid cash dividends on our capital stock and we do not expect to pay any dividends in the foreseeable future. We currently intend to retain future earnings, if any, to finance the growth and development of our business. Our current credit facilities place restrictions on our ability to issue dividends. See discussion under “Liquidity and Capital Resources” regarding our current credit facilities. Payment of future dividends, if any, will be at the discretion of our board of directors and will depend on our financial condition, results of operations, capital requirements and such other factors as the board of directors deems relevant.
Equity Compensation Plans Information
The information required by this item will be contained in our definitive proxy statement, to be filed with the SEC in connection with our 2018 annual meeting of stockholders, which is expected to be filed not later than 120 days after the end of our fiscal year ended December 31, 2017, and is incorporated in this report by reference.
Stock Performance Graph
The following graph compares the yearly percentage change in cumulative total stockholder return of our common stock during the period from 2012 to 2017 with (i) the cumulative total return of the S&P 500 index and (ii) the cumulative total return of the S&P 500 – Healthcare Sector index. The comparison assumes $100 was invested on December 31, 2012 in our common stock and in each of the foregoing indices and the reinvestment of dividends through December 31, 2017. The stock price performance on the following graph is not necessarily indicative of future stock price performance.
This graph shall not be deemed incorporated by reference by any general statement incorporating by reference this Form 10-K into any filing under the Securities Act or under the Exchange Act, except to the extent that RadNet specifically incorporates this information by reference, and shall not otherwise be deemed filed under the Securities Act or the Exchange Act.
| 33 |
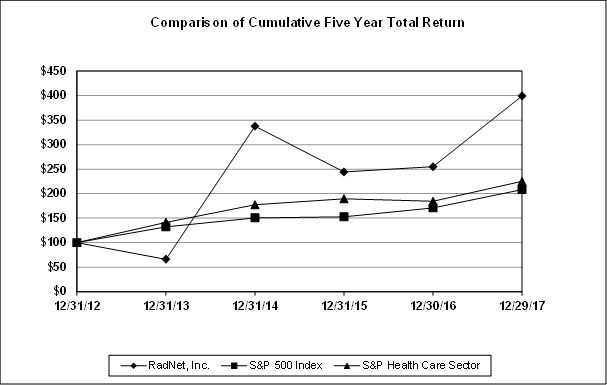
| ANNUAL RETURN PERCENTAGE | ||||||||||||||||||||
| Years Ending | ||||||||||||||||||||
| Company / Index | 12/31/13 | 12/31/14 | 12/31/15 | 12/30/16 | 12/29/17 | |||||||||||||||
| RadNet, Inc. | -33.99 | 411.38 | -27.63 | 4.37 | 56.59 | |||||||||||||||
| S&P 500 Index | 32.39 | 13.69 | 1.38 | 11.96 | 21.83 | |||||||||||||||
| S&P Health Care Sector | 41.46 | 25.34 | 6.89 | -2.69 | 22.08 | |||||||||||||||
| INDEXED RETURNS | ||||||||||||||||||||||||
| Base | Years Ending | |||||||||||||||||||||||
| Period | ||||||||||||||||||||||||
| Company / Index | 12/31/12 | 12/31/13 | 12/31/14 | 12/31/15 | 12/30/16 | 12/29/17 | ||||||||||||||||||
| RadNet, Inc. | 100 | 66.01 | 337.55 | 244.27 | 254.94 | 399.21 | ||||||||||||||||||
| S&P 500 Index | 100 | 132.39 | 150.51 | 152.59 | 170.84 | 208.14 | ||||||||||||||||||
| S&P Health Care Sector | 100 | 141.46 | 177.30 | 189.52 | 184.42 | 225.13 | ||||||||||||||||||
Recent Sales of Unregistered Securities
None.
| Item 6. | Selected Consolidated Financial Data |
The following table sets forth our selected historical consolidated financial data. The selected consolidated statements of operations data set forth below for the years ended December 31, 2017, 2016 and 2015, and the consolidated balance sheet data as of December 31, 2017 and 2016, are derived from our audited consolidated financial statements and notes thereto included elsewhere herein. The selected historical consolidated statements of operations data set forth below for the years ended December 31, 2014 and 2013, and the consolidated balance sheet data set forth below as of December 31, 2015, 2014 and 2013, are derived from our audited consolidated financial statements not included herein. This data should be read in conjunction with and is qualified in its entirety by reference to the audited consolidated financial statements and the related notes included elsewhere in this annual report and Item 7 - “Management’s Discussion and Analysis of Financial Condition and Results of Operations.”
| 34 |
The financial data set forth below and discussed in this annual report are derived from the consolidated financial statements of RadNet, its subsidiaries and certain affiliates. As a result of the contractual and operational relationship among BRMG, Dr. Berger, the NY Groups, Dr. Crues and the Company, we are considered to have a controlling financial interest in BRMG and the NY Groups (collectively, the “Professional Entities”) pursuant to applicable accounting guidance. Due to the deemed controlling financial interest, we are required to include the Professional Entities as consolidated entities in our consolidated financial statements. This means, for example, that revenue generated by the Professional Entities from the provision of professional medical services to our patients, as well as the Professional Entities costs of providing those services, are included as net revenue and cost of operations in our consolidated statement of operations, whereas the management fee that the Professional Entities’ pay to us under our management agreement with the Professional Entities is eliminated as a result of the consolidation of our results with those of the Professional Entities. Also, because the Professional Entities are consolidated in our financial statements, any borrowings or advances we have received from or made to the Professional Entities have been eliminated in our consolidated balance sheet. If the Professional Entities were not treated as consolidated entities in our consolidated financial statements, the presentation of certain items in our income statement, such as net service fee revenue and costs and expenses, would change but our net income would not, because in operation and historically, the annual revenue of the Professional Entities from all sources closely approximates its expenses, including Dr. Berger’s and Dr. Crues’ compensation, fees payable to us and amounts payable to third parties.
| Years Ended December 31, | ||||||||||||||||||||
| 2017 | 2016 | 2015 | 2014 | 2013 | ||||||||||||||||
| (in thousands, except per share data) | ||||||||||||||||||||
| Statement of Operations Data: | ||||||||||||||||||||
| Net revenue | $ | 922,186 | $ | 884,535 | $ | 809,628 | $ | 717,569 | $ | 702,986 | ||||||||||
| Operating expenses: | ||||||||||||||||||||
| Cost of operations, excluding depreciation and amortization | 802,377 | 775,801 | 708,289 | 602,652 | 598,655 | |||||||||||||||
| Depreciation and amortization | 66,796 | 66,610 | 60,611 | 59,258 | 58,890 | |||||||||||||||
| Loss on sale and disposal of equipment, net | 1,142 | 767 | 866 | 1,113 | 1,032 | |||||||||||||||
| Gain on sale of imaging center and medical practice | (3,146 | ) | – | (5,434 | ) | – | (2,108 | ) | ||||||||||||
| Gain on return of common stock | – | (5,032 | ) | – | – | – | ||||||||||||||
| Meaningful use incentive | (250 | ) | (2,808 | ) | (3,270 | ) | (2,034 | ) | – | |||||||||||
| Loss on extinguishment of debt | – | – | – | 15,927 | – | |||||||||||||||
| Net income attributable to RadNet common stockholders | 53 | 7,230 | 7,709 | 1,376 | 2,120 | |||||||||||||||
| Basic income per share attributable to RadNet common stockholders | 0.00 | 0.16 | 0.18 | 0.03 | 0.05 | |||||||||||||||
| Diluted income per share attributable to RadNet common stockholders | 0.00 | 0.15 | 0.17 | 0.03 | 0.05 | |||||||||||||||
| Balance Sheet Data: | ||||||||||||||||||||
| Cash and cash equivalents | $ | 51,322 | $ | 20,638 | $ | 446 | $ | 307 | $ | 8,412 | ||||||||||
| Total assets | 868,979 | 849,476 | 836,427 | 740,680 | 722,576 | |||||||||||||||
| Total long-term liabilities | 607,448 | 642,082 | 643,007 | 599,708 | 601,977 | |||||||||||||||
| Total liabilities | 799,054 | 797,423 | 799,966 | 732,982 | 720,366 | |||||||||||||||
| Working capital | 43,745 | 62,573 | 72,410 | 58,746 | 57,955 | |||||||||||||||
| Equity | 69,925 | 52,053 | 36,461 | 7,698 | 2,210 | |||||||||||||||
| 35 |
| Item 7. | Management’s Discussion and Analysis of Financial Condition and Results of Operations |
Overview
We are a leading national provider of freestanding, fixed-site outpatient diagnostic imaging services in the United States based on number of locations and annual imaging revenue. At December 31, 2017, we operated directly or indirectly through joint ventures, 297 centers located in California, Delaware, Florida, Maryland, New Jersey, and New York. Our centers provide physicians with imaging capabilities to facilitate the diagnosis and treatment of diseases and disorders and may reduce unnecessary invasive procedures, often reducing the cost and amount of care for patients.
Our services include magnetic resonance imaging (MRI), computed tomography (CT), positron emission tomography (PET), nuclear medicine, mammography, ultrasound, diagnostic radiology (X-ray), fluoroscopy and other related procedures. The following table shows the number of systems that we had in operation as of the years ended December 31, 2017, 2016 and 2015:
| Years Ended December 31, | ||||||||||||
| 2017 | 2016 | 2015 | ||||||||||
| MRI | 257 | 257 | 231 | |||||||||
| CT | 152 | 157 | 144 | |||||||||
| PET/CT | 49 | 47 | 46 | |||||||||
| Mammography | 261 | 279 | 260 | |||||||||
| Ultrasound | 614 | 551 | 498 | |||||||||
| X-ray | 285 | 272 | 393 | |||||||||
| Nuclear Medicine | 52 | 48 | 49 | |||||||||
| Fluoroscopy | 102 | 104 | 105 | |||||||||
| Total equipment | 1,772 | 1,715 | 1,726 | |||||||||
We derive substantially all of our revenue from fees charged for the diagnostic imaging services performed at our facilities. The following table shows our facilities in operation at year end, diagnostic volumes and revenues for the years ended December 31, 2017, 2016 and 2015:
| Years Ended December 31, | ||||||||||||
| 2017 | 2016 | 2015 | ||||||||||
| Facilities in operation | 297 | 305 | 300 | |||||||||
| Diagnostic imaging procedures | 6,196,398 | 6,109,622 | 5,638,979 | |||||||||
| Net revenues (millions) | $ | 922.2 | $ | 884.5 | $ | 809.6 | ||||||
During 2017 we continued to focus on our most established markets, growing there through joint ventures and acquisitions. In conjunction with Cedars Sinai Medical Center, we entered into two new joint ventures in the city of Los Angeles. We acquired our main competitor in the state of Delaware, picking up an additional 5 multi-modality centers to consolidate our leadership position in that market. We sold our wholly-owned breast oncology practice, Breastlink Medical Group, completely divesting that practice along with 3 facilities. We also divested all of our holdings in the state of Rhode Island through the sale of 5 centers, concentrating our geographic focus on the Maryland to New York corridor with our Delaware acquisition. We also agreed to create a new joint venture with another hospital system consisting of 34 outpatient centers spread across southern Los Angeles and Orange counties in California.
| 36 |
Our revenue is derived from a diverse mix of payors, including private payors, managed care capitated payors and government payors. We believe our payor diversity mitigates our exposure to possible unfavorable reimbursement trends within any one payor class. In addition, our experience with capitation arrangements over the last several years has provided us with the expertise to manage utilization and pricing effectively, resulting in a predictable stream of revenue. Our service fee revenue, net of contractual allowances and discounts, the provision for bad debts, and revenue under capitation arrangements for the years ended December 31, are summarized in the following table (in thousands):
| Years Ended December 31, | ||||||||||||
| 2017 | 2016 | 2015 | ||||||||||
| Commercial insurance | $ | 571,369 | $ | 539,793 | $ | 486,489 | ||||||
| Medicare | 193,166 | 187,941 | 168,545 | |||||||||
| Medicaid | 25,821 | 28,170 | 23,948 | |||||||||
| Workers' compensation/personal injury | 35,195 | 36,548 | 32,728 | |||||||||
| Other (1) | 31,627 | 29,135 | 35,046 | |||||||||
| Service fee revenue, net of contractual allowances and discounts | 857,178 | 821,587 | 746,756 | |||||||||
| Provision for bad debts | (46,555 | ) | (45,387 | ) | (36,033 | ) | ||||||
| Net service fee revenue | 810,623 | 776,200 | 710,723 | |||||||||
| Revenue under capitation arrangements | 111,563 | 108,335 | 98,905 | |||||||||
| Total net revenue | $ | 922,186 | $ | 884,535 | $ | 809,628 | ||||||
(1) Other consist of revenue from teleradiology services, consulting fees and software revenue.
We have developed our medical imaging business through a combination of organic growth, acquisitions and joint venture formations. For further information, see “Recent Developments and Facility Acquisitions and Dispositions” below.
We typically experience some seasonality to our business. During the first quarter of each year we generally experience the lowest volumes of procedures and the lowest level of revenue for any quarter during the year. This is primarily the result of two factors. First, our volumes and revenue are typically impacted by winter weather conditions in our northeastern operations. It is common for snowstorms and other inclement weather to result in patient appointment cancellations and, in some cases, imaging center closures. Second, in recent years, we have observed greater participation in high deductible health plans by patients. As these high deductibles reset in January for most of these patients, we have observed that patients utilize medical services less during the first quarter, when securing medical care will result in significant out-of-pocket expenditures.
The consolidated financial statements in this annual report include the accounts of Radnet Management, BRMG and the NY Groups. The consolidated financial statements also include Radnet Management I, Inc., Radnet Management II, Inc., Radiologix, Inc., Radnet Management Imaging Services, Inc., Delaware Imaging Partners, Inc., New Jersey Imaging Partners, Inc. and Diagnostic Imaging Services, Inc. (DIS), all wholly owned subsidiaries of Radnet Management.
Accounting Standards Codification (ASC) 810-10-15-14, Consolidation, stipulates that generally any entity with a) insufficient equity to finance its activities without additional subordinated financial support provided by any parties, or b) equity holders that, as a group, lack the characteristics specified in the Codification which evidence a controlling financial interest, is considered a Variable Interest Entity (“VIE”). We consolidate all VIEs in which we own a majority voting interest and all VIEs for which we are the primary beneficiary. We determine whether we are the primary beneficiary of a VIE through a qualitative analysis that identifies which variable interest holder has the controlling financial interest in the VIE. The variable interest holder that has both of the following has the controlling financial interest and is the primary beneficiary: (1) the power to direct the activities of the VIE that most significantly impact the VIE’s economic performance and (2) the obligation to absorb losses of, or the right to receive benefits from, the VIE that could potentially be significant to the VIE. In performing our analysis, we consider all relevant facts and circumstances, including: the design and activities of the VIE, the terms of the contracts the VIE has entered into, the nature of the VIE’s variable interests issued and how they were negotiated with or marketed to potential investors, and which parties participated significantly in the design or redesign of the entity.
Facility Acquisitions, Formation of Joint Ventures and Dispositions
Facility acquisitions
On October 5, 2017 we completed our acquisition of all of the outstanding equity interests in RadSite, LLC, for $1.0 million in common stock and $856,000 in cash. RadSite provides both quality certification and accreditation programs for imaging providers in accordance with standards of private insurance payors and federal regulations under Medicare. We have made a fair value determination of the acquired assets and approximately $91,000 of current assets, $25,000 in fixed assets, a $150,000 covenant not to compete, $75,000 in liabilities and $1.7 million in goodwill were recorded.
| 37 |
On October 1, 2017 we completed our acquisition of certain assets of Remote Diagnostic Imaging P.L.L.C., consisting of a single multi-modality center located in New York, New York, for purchase consideration of $3.9 million. We have made a fair value determination of the acquired assets and approximately $2.6 million in fixed assets, a $50,000 covenant not to compete, and $1.2 million in goodwill were recorded.
On August 7, 2017 we acquired Diagnostic Imaging Associates (“DIA”) for $13.0 million in cash and $1.5 million in RadNet common stock. Located in the state of Delaware, DIA operates five multi-modality imaging locations which provide MRI, CT, Ultrasound, Mammography and X-Ray services. We have made a fair value determination of the acquired assets and approximately $3.1 million of fixed assets and equipment, $1.2 million in current assets, and $10.2 million in goodwill were recorded.
On June 1, 2017 we completed our acquisition of certain assets of Stockton MRI and Molecular Imaging Medical Center Inc., consisting of a multi-modality center located in Stockton, CA, for consideration of $4.4 million. The facility provides MRI, CT, Ultrasound, X-Ray and Nuclear Medicine services. We have made a fair value determination of the acquired assets and approximately $1.2 million of fixed assets and equipment, a $50,000 covenant not to compete, and $3.1 million of goodwill were recorded.
On May 3, 2017 we completed our acquisition of certain assets of D&D Diagnostics Inc., consisting of a single multi-modality imaging center located in Silver Spring, Maryland, for total purchase consideration of $2.4 million. We have made a fair value determination of the acquired assets and approximately $820,000 of fixed assets, $16,000 of other assets, and $1.5 million of goodwill were recorded. The facility provides MRI, CT, X-Ray and related services.
On February 1, 2017, we completed our acquisition of certain assets of MRI Centers, Inc., consisting of one single-modality imaging center located in Torrance, CA providing MRI and sports medicine services, for cash consideration of $800,000 and the payoff of $81,000 in debt. We have made a fair value determination of the acquired assets and approximately $289,000 of fixed assets, $9,800 of other assets, $100,000 covenant not to compete and $401,000 of goodwill were recorded.
On January 13, 2017, we completed our acquisition of certain assets of Resolution Medical Imaging Corporation for consideration of $4.0 million. The purchase of Resolution was enacted to contribute its assets to a joint venture with Cedars Sinai Medical Corporation which was effective April 1, 2017. See the formation of new joint ventures section in Note 2 in the financial statements contained herein for further information.
Formation of new joint ventures
On April 1, 2017, we formed in conjuncture with Cedars Sinai Medical Center (“CSMC”) the Santa Monica Imaging Group, LLC (“SMIG”), consisting of two multi-modality imaging centers located in Santa Monica, CA. Total agreed contribution was $2.7 million of cash and assets with RadNet contributing $1.1 million for a 40% economic interest and CSMC contributing $1.6 million for a 60% economic interest. For its contribution, RadNet transferred $80,000 in cash and the net assets acquired in the acquisition of Resolution Imaging of $2.5 million. CSMC contributed $120,000 in cash and paid RadNet $1.5 million for the Resolution Imaging assets transferred to the venture. RadNet does not have controlling economic interest in SMIG and the investment is accounted for under the equity method.
On January 6, 2017, Image Medical Inc. (“Image Medical”), a wholly owned subsidiary of RadNet, acquired a 49% economic interest ScriptSender, LLC, a partnership held by two individuals which provides secure data transmission services of medical information. Through a management agreement, RadNet provides management and accounting services and receives an agreed upon fee. Image Medical will contribute $3.0 million to the partnership for its 49% ownership stake over a three year period representing the maximum risk in the venture. ScriptSender LLC is dependent on this contribution to finance its own activities, and as such we determined that it is a VIE, but we are not a primary beneficiary since we do not have the power to direct the activities of the entity that most significantly impact the entity’s economic performance. As of December 31, 2017, the carrying amount of the investment is $2.5 million.
| 38 |
Dispositions and Sales of Noncontrolling Interest
On September 1, 2017 we completed the equity sale of a wholly owned breast oncology practice, Breastlink Medical Group, Inc., to Verity Medical Foundation for approximately $2.8 million. We recorded a gain of approximately $845,000 and incurred severance expense of approximately $1.2 million from this transaction.
On July 1, 2017 we formed a majority owned subsidiary, Advanced Imaging at Timonium Crossing, LLC, in conjunction with the University of Maryland St. Joseph Medical Center. As part of that transaction, we sold a 25% noncontrolling interest in an imaging center of our wholly owned subsidiary, Advanced Imaging Partners, Inc., to the University of Maryland St. Joseph Medical Center for $3.9 million. On the date of sale, the net book value of the 25% interest was $1.1 million and the proceeds in excess of net book value amounting to $2.8 million were recorded to equity.
On April 28, 2017 we completed the sale of five imaging centers operating in Rhode Island to Rhode Island Medical Imaging, Inc. for approximately $4.5 million. We recorded a gain of approximately $1.9 million in the second quarter with regard to this transaction and have no remaining imaging centers in the state.
On April 1, 2017 we received from Cedars Sinai Medical Center $5.9 million in exchange for a 25% noncontrolling interest in the West Valley Imaging Group, LLC (“WVI”). The determined net book value of the 25% interest was approximately $3.0 million. The proceeds in excess of the net book value, amounting to $1.8 million net of taxes, were recorded to equity.
On April 1, 2017 we completed the sale of 2 wholly owned oncology practices to Cedars Sinai Medical Center in connection with the sale of non-controlling interest of the WVI subsidiary described above for approximately $1.2 million. We recorded a gain of approximately $361,000 on this transaction on the statement of operations.
| 39 |
Results of Operations
The following table sets forth, for the periods indicated, the percentage that certain items in the statements of operations bears to net revenue before provision for bad debts.
| Years Ended December 31, | ||||||||||||
| 2017 | 2016 | 2015 | ||||||||||
| NET REVENUE | ||||||||||||
| Service fee revenue, net of contractual allowances and discounts | 88.5% | 88.4% | 88.3% | |||||||||
| Provision for bad debts | -4.8% | -4.9% | -4.3% | |||||||||
| Net service fee revenue | 83.7% | 83.5% | 84.0% | |||||||||
| Revenue under capitation arrangements | 11.5% | 11.6% | 11.7% | |||||||||
| Total net revenue | 95.2% | 95.1% | 95.7% | |||||||||
| OPERATING EXPENSES | ||||||||||||
| Cost of operations, excluding depreciation and amortization | 82.8% | 83.4% | 83.8% | |||||||||
| Depreciation and amortization | 6.9% | 7.2% | 7.2% | |||||||||
| Loss on sale and disposal of equipment | 0.1% | 0.1% | 0.1% | |||||||||
| Severance costs | 0.2% | 0.3% | 0.1% | |||||||||
| Total operating expenses | 90.0% | 91.0% | 91.1% | |||||||||
| INCOME FROM OPERATIONS | 5.2% | 4.1% | 4.6% | |||||||||
| OTHER INCOME AND EXPENSES | ||||||||||||
| Interest expense | 4.2% | 4.7% | 4.9% | |||||||||
| Meaningful use incentive | 0.0% | -0.3% | -0.4% | |||||||||
| Equity in earnings of joint ventures | -1.4% | -1.1% | -1.1% | |||||||||
| Gain on sale of imaging centers and medical practice | -0.3% | 0.0% | -0.6% | |||||||||
| Gain on return of common stock | 0.0% | -0.5% | 0.0% | |||||||||
| Loss on early extinguishment of senior notes | 0.0% | 0.0% | 0.0% | |||||||||
| Other expenses | 0.0% | 0.0% | 0.0% | |||||||||
| Total other expenses | 2.4% | 2.8% | 2.8% | |||||||||
| INCOME BEFORE INCOME TAXES | 2.7% | 1.4% | 1.8% | |||||||||
| Provision for income taxes | -2.5% | -0.5% | -0.7% | |||||||||
| NET INCOME | 0.2% | 0.9% | 1.1% | |||||||||
| Net income attributable to noncontrolling interests | 0.2% | 0.1% | 0.1% | |||||||||
| NET INCOME ATTRIBUTABLE TO RADNET, INC. | ||||||||||||
| COMMON STOCKHOLDERS | 0.0% | 0.8% | 1.0% | |||||||||
Year Ended December 31, 2017 Compared to the Year Ended December 31, 2016
Service Fee Revenue, net of contractual allowances and discounts
Service fee revenue, net of contractual allowances and discounts for the year ended December 31, 2017 was $857.2 million compared to $821.6 million for the year ended December 31, 2016, an increase of $35.6 million, or 4.3%.
Service fee revenue, net of contractual allowances and discounts, for only those centers in operation throughout the full fiscal years of both 2017 and 2016, increased $40.4 million, or 5.3%. The overall 5.3% increase was precipitated by a 4% hike in volumes of advanced imaging modalities at the higher 2017 fee schedule reimbursement rates plus a 1.4% revenue increase on digital tomography procedures. This comparison excludes revenue contributions from centers that were acquired subsequent to January 1, 2016. For the year ended December 31, 2017, service fee revenue, net of contractual allowances and discounts, from centers that were acquired subsequent to January 1, 2016 and excluded from the above comparison was $47.1 million. For the year ended December 31, 2016, net revenue from centers that were acquired subsequent to January 1, 2016 and excluded from the above comparison was $51.9 million.
| 40 |
Provision for bad debts
Provision for bad debts increased $1.2 million, or 2.6%, to $46.6 million, or 4.8% of net revenue, for the year ended December 31, 2017 compared to $45.4 million, or 4.9% of net revenue, for the year ended December 31, 2016. We review our provision by the application of judgment based on factors such as contractual reimbursement rates, payor mix, the age of receivables, historical cash collection experience and other relevant information.
Revenue under capitation arrangements
Revenue under capitation arrangements for the year ended December 31, 2017 was $111.5 million compared to $108.3 million for the year ended December 31, 2016, an increase of $3.2 million, or 3.0%%.
Revenue under capitation arrangements, including only those centers which were in operation throughout the full fiscal years of both 2017 and 2016, increased $3.6 million, or 3.3%. This comparison excludes revenue contributions from centers that were acquired subsequent to January 1, 2016. For the year ended December 31, 2017, revenue under capitation arrangements from centers that were acquired subsequent to January 1, 2016 and excluded from the above comparison was $129,000. For the year ended December 31, 2016, net revenue from centers that were acquired subsequent to January 1, 2016 and excluded from the above comparison was $484,000.
Operating expenses
Cost of operations for the year ended December 31, 2017 increased approximately $26.6 million, or 3.4%, from $775.8 million for the year ended December 31, 2016 to $802.4 million for the year ended December 31, 2017. The following table sets forth our operating expenses for the years ended December 31, 2017 and 2016 (in thousands):
| Years Ended December 31, | ||||||||
| 2017 | 2016 | |||||||
| Salaries and professional reading fees, excluding stock-based compensation | $ | 470,382 | $ | 445,690 | ||||
| Stock-based compensation | 6,787 | 5,826 | ||||||
| Building and equipment rental | 78,627 | 74,214 | ||||||
| Medical supplies | 42,625 | 51,735 | ||||||
| Other operating expenses * | 203,956 | 198,336 | ||||||
| Cost of operations | 802,377 | 775,801 | ||||||
| Depreciation and amortization | 66,796 | 66,610 | ||||||
| Loss on sale and disposal of equipment | 1,142 | 767 | ||||||
| Severance costs | 1,821 | 2,877 | ||||||
| Total operating expenses | $ | 872,136 | $ | 846,055 | ||||
* Includes billing fees, office supplies, repairs and maintenance, insurance, business tax and license, outside services, utilities, marketing, travel and other expenses.
| 41 |
| · | Salaries and professional reading fees, excluding stock-based compensation and severance |
Salaries and professional reading fees increased $24.7 million, or 5.5%, to $470.4 million for the year ended December 31, 2017, compared to $445.7 million for the year ended December 31, 2016.
Salaries and professional reading fees, limited to centers which were in operation throughout the full fiscal years of both 2017 and 2016, increased $25.4 million, or 6.1%. 2% of the 6.1% increase was due to physician staffing in correlation with the increase in net revenue. The other 4% increase was attributable to non-physician staffing cost due to increased volumes at centers along with ramping up our staffing in Reimbursement Operations and Self Pay team in an effort to increase collection and improve our collection rates. This comparison excludes contributions from centers that were acquired subsequent to January 1, 2016. For the year ended December 31, 2017, salaries and professional reading fees from centers that were acquired subsequent to January 1, 2016 and excluded from the above comparison was $24.9 million. For the year ended December 31, 2016, salaries and professional reading fees from centers that were acquired subsequent to January 1, 2016, and excluded from the above comparison was $25.6 million.
| · | Stock-based compensation |
Stock-based compensation increased $960,000, or 16.5%, to $6.8 million for the year ended December 31, 2017 compared to $5.8 million for the year ended December 31, 2016. This increase was driven by the higher fair value of stock based compensation awarded and vested in the year 2017 as compared to 2016.
| · | Building and equipment rental |
Building and equipment rental expenses increased $4.4 million, or 6.0 %, to $78.6 million for the year ended December 31, 2017, compared to $74.2 million for the year ended December 31, 2016.
Building and equipment rental expenses, including only those centers which were in operation throughout the full fiscal years of both 2017 and 2016, increased $4.7 million, or 6.7%, mainly related to new facility and radiology equipment leases in support of imaging operations. This comparison excludes contributions from centers that were acquired subsequent to January 1, 2017. For the year ended December 31, 2017, building and equipment rental expenses from centers that were acquired subsequent to January 1, 2016, and excluded from the above comparison, was $3.7 million. For the year ended December 31, 2016, building and equipment rental expenses from centers that were acquired subsequent to January 1, 2016, and excluded from the above comparison, was $4.0 million.
| · | Medical supplies |
Medical supplies expense decreased $9.1 million, or 17.6%, to $42.6 million for the year ended December 31, 2017, compared to $51.7 million for the year ended December 31, 2016.
Medical supplies expense, including only those centers which were in operation throughout the full fiscal years of both 2017 and 2016, increased $508,000, or 1.7%. This comparison excludes contributions from centers that were acquired or divested subsequent to January 1, 2017. For the year ended December 31, 2017, medical supplies expense from centers that were acquired subsequent to January 1, 2016, and excluded from the above comparison was $11.4 million. For the year ended December 31, 2016, medical supplies expense from centers that were acquired subsequent to January 1, 2016, and excluded from the above comparison was $21.0 million.
| · | Other operating expenses |
Other operating expenses increased $5.6 million, or 2.8%, to $204.0 million for the year ended December 31, 2017 compared to $198.3 million for the year ended December 31, 2016.
Other operating expenses, limited to only those centers which were in operation throughout the full fiscal years of both 2017 and 2016, increased $7.7 million or 4.1%. The increase was primarily related to insurance reserve charges, higher utility usage rates in the fourth quarter of the year, and billing services. This comparison excludes contributions from centers that were acquired or divested subsequent to January 1, 2016. For the year ended December 31, 2017, other operating expenses from centers that were acquired subsequent to January 1, 2016, and excluded from the above comparison were $8.8 million. For the year ended December 31, 2016, other operating expenses from centers that were acquired subsequent to January 1, 2016, and excluded from the above comparison were $10.9 million.
| 42 |
| · | Depreciation and amortization expense |
Depreciation and amortization expense increased $186,000, or 0.3%, to $66.8 million for the year ended December 31, 2017 when compared $66.6 million for the year ended December 31, 2016.
Depreciation and amortization expense at those centers which were in operation throughout the full fiscal years of both 2017 and 2016, decreased $32,000 or 0.1%. This comparison excludes contributions from centers that were acquired or divested subsequent to January 1, 2016. For the year ended December 31, 2017, depreciation and amortization from centers that were acquired or divested subsequent to January 1, 2016 and excluded from the above comparison was $2.8 million. For the year ended December 31, 2016, depreciation and amortization from centers that were acquired subsequent to January 1, 2016, and excluded from the above comparison was $2.6 million.
| · | Loss on sale and disposal of equipment |
Loss on sale of equipment was $1.1 million and $767,000 for the years ended December 31, 2017 and 2016, respectively, and primarily related to the difference between the net book value of certain equipment sold and proceeds we received from the sale.
| · | Severance costs |
During the year ended December 31, 2017, we had severance costs of $1.8 million compared to $2.9 recorded during the year ended December 31, 2016. In the third quarter of 2017, we incurred severance expenses of $1.2 million specifically related to the disposition of Breastlink Medical Group.
Interest expense
Interest expense decreased approximately $2.8 million, or 6.5%, to $40.6 million for the year ended December 31, 2017 compared to $43.5 million for the year ended December 31, 2016. Interest expense for the year ended December 31, 2016 included $3.5 million of amortization of deferred financing and discount on issuance of debt, and $24,000 of other non cash interest. Interest expense for the year ended December 31, 2016 included $4.3 million of amortization of deferred financing costs and discount on issuance of debt as well as $709,000 of deferred financing costs in relation to the Restatement Amendment and $93,000 in other non cash interest.
The cash portion of our interest expense decreased approximately $1.2 million for the year ended December 31, 2017 compared to the year ended December 31, 2016. The decrease was primarily due to lower interest rates on our term loan debt stemming from the Fifth Amendment (defined below). See “Liquidity and Capital Resources” below for more details on our financing activity during 2017.
Meaningful use incentive
For the years ended December 31, 2017 and December 31, 2016, we recognized other income from meaningful use incentive in the amount of $250,000 and $2.8 million, respectively. This amount was earned under a Medicare program to promote the use of electronic health record technology.
Equity in earnings from unconsolidated joint ventures
Equity in earnings from our unconsolidated joint ventures increased $3.8 million or 38.8% to $13.6 million for the year ended December 31, 2017 compared to $9.8 million for the year ended December 31, 2016. The increase relates mainly to equity in earnings stemming from New Jersey Imaging Networks, a joint venture where we hold a 49% non-controlling interest, and strong performances in other joint ventures based in the state of Maryland.
Gain on Sale of Imaging Center
In separate sale transactions over 2017, we recognized a combined gain on the sale of 5 wholly owned imaging centers in Rhode Island and 3 oncology practices, including the sale of Breastlink Medical Group, in the amount of $3.1 million.
| 43 |
Gain on return of common stock
In the second quarter of 2016, we recorded a gain on return of common stock of $5.0 million.
Other expenses / income
For the year ended December 31, 2017 we recorded approximately $8,000 of other income. For the year ended December 31, 2016, we recorded $196,000 of other expenses.
Provision for income tax expense
We had a tax provision for the year ended December 31, 2017 of $24.3 million or 92.1% of income before income taxes, compared to a tax provision for year ended December 31, 2016 of $4.4 million or 35.6% of income before income taxes. The increase in provision for income tax expense was significantly impacted by the recent changes in federal tax law. The Tax Cuts and Jobs Act or Tax Act was enacted on December 22, 2017 and reduces the US federal corporate tax rate to 21%, requires companies to pay a one-time transition tax on earnings of certain foreign subsidiaries that were previously tax deferred, and creates new taxes on certain foreign secured earnings. We have not completed our accounting for the tax effects of the Tax Act, however in certain cases we have made a reasonable estimate of the effects on our existing deferred tax balances and one-time transition tax. For the items for which we were able to determine a reasonable estimate, we remeasured certain deferred tax assets and liabilities based on the rates at which they are expected to reverse in the future, which is generally 21%. The changes effected by the Tax Act resulted in an increase in tax expense of $13.6 million. Of this provision amount, $13.5 million is related to the revaluation of certain deferred tax balances and $0.1 million is related to one-time transition tax on deemed repatriation of foreign earnings. See Note 10 to our consolidated financial statement contained herein for more details.
Year Ended December 31, 2016 Compared to the Year Ended December 31, 2015
Service Fee Revenue, net of contractual allowances and discounts
Service fee revenue, net of contractual allowances and discounts for the year ended December 31, 2016 was $821.6 million compared to $746.8 million for the year ended December 31, 2015, an increase of $74.8 million, or 10.0%.
Service fee revenue, net of contractual allowances and discounts, for only those centers in operation throughout the full fiscal years of both 2016 and 2015, increased $17.6 million, or 2.6%. This comparison excludes revenue contributions from centers that were acquired subsequent to January 1, 2015. For the year ended December 31, 2016, service fee revenue, net of contractual allowances and discounts, from centers that were acquired subsequent to January 1, 2015 and excluded from the above comparison was $122.1 million. For the year ended December 31, 2015, net revenue from centers that were acquired subsequent to January 1, 2015 and excluded from the above comparison was $64.9 million.
Provision for bad debts
Provision for bad debts increased $9.4 million, or 26.0%, to $45.4 million, or 4.9% of net revenue, for the year ended December 31, 2016 compared to $36.0 million, or 4.3% of net revenue, for the year ended December 31, 2015. The 26% increase was related to service fee revenue growth from our 2015 acquisition activity combined with additional reserves based on management determination that collection efforts for certain accounts appear to have been exhausted. We review our provision by the application of judgment based on factors such as contractual reimbursement rates, payor mix, the age of receivables, historical cash collection experience and other relevant information.
Revenue under capitation arrangements
Revenue under capitation arrangements for the year ended December 31, 2016 was $108.3 million compared to $98.9 million for the year ended December 31, 2015, an increase of $9.4 million, or 9.5%.
| 44 |
Revenue under capitation arrangements, including only those centers which were in operation throughout the full fiscal years of both 2016 and 2015, increased $1.7 million, or 1.7%. This comparison excludes revenue contributions from centers that were acquired subsequent to January 1, 2015. For the year ended December 31, 2016, revenue under capitation arrangements from centers that were acquired subsequent to January 1, 2015 and excluded from the above comparison was $9.0 million. For the year ended December 31, 2015, net revenue from centers that were acquired subsequent to January 1, 2015 and excluded from the above comparison was $1.3 million.
Operating expenses
Cost of operations for the year ended December 31, 2016 increased approximately $67.5 million, or 9.5%, from $708.3 million for the year ended December 31, 2015 to $775.8 million for the year ended December 31, 2016. The following table sets forth our operating expenses for the years ended December 31, 2016 and 2015 (in thousands):
| Years Ended December 31, | ||||||||
| 2016 | 2015 | |||||||
| Salaries and professional reading fees, excluding stock-based compensation | $ | 445,690 | $ | 402,528 | ||||
| Stock-based compensation | 5,826 | 7,647 | ||||||
| Building and equipment rental | 74,214 | 71,666 | ||||||
| Medical supplies | 51,735 | 49,417 | ||||||
| Other operating expenses * | 198,336 | 177,031 | ||||||
| Cost of operations | 775,801 | 708,289 | ||||||
| Depreciation and amortization | 66,610 | 60,611 | ||||||
| Loss on sale and disposal of equipment | 767 | 866 | ||||||
| Severance costs | 2,877 | 745 | ||||||
| Total operating expenses | $ | 846,055 | $ | 770,511 | ||||
* Includes billing fees, office supplies, repairs and maintenance, insurance, business tax and license, outside services, utilities, marketing, travel and other expenses.
| · | Salaries and professional reading fees, excluding stock-based compensation and severance |
Salaries and professional reading fees increased $43.2 million, or 10.7%, to $445.7 million for the year ended December 31, 2016, compared to $402.5 million for the year ended December 31, 2015.
Salaries and professional reading fees for only those centers in operation throughout the full fiscal years of both 2016 and 2015, increased $16.2 million, or 4.2%. This comparison excludes contributions from centers that were acquired subsequent to January 1, 2015. For the year ended December 31, 2016, salaries and professional reading fees from centers that were acquired subsequent to January 1, 2015 and excluded from the above comparison was $48.0 million. For the year ended December 31, 2015, salaries and professional reading fees from centers that were acquired subsequent to January 1, 2015, and excluded from the above comparison was $21.0 million.
| · | Stock-based compensation |
Stock-based compensation decreased $1.8 million, or 23.8%, to $5.8 million for the year ended December 31, 2016 compared to $7.6 million for the year ended December 31, 2015. This decrease was driven by the lower fair value of stock based compensation awarded and vested in the year 2016 as compared to 2015.
| · | Building and equipment rental |
Building and equipment rental expenses increased $2.5 million, or 3.6%, to $74.2 million for the year ended December 31, 2016, compared to $71.7 million for the year ended December 31, 2015.
Building and equipment rental expenses, including only those centers which were in operation throughout the full fiscal years of both 2016 and 2015, decreased $3.3 million, or 5.2%, mainly due to favorable lease negotiations at existing facilities. This comparison excludes contributions from centers that were acquired subsequent to January 1, 2016. For the year ended December 31, 2016, building and equipment rental expenses from centers that were acquired subsequent to January 1, 2015, and excluded from the above comparison, was $12.9 million. For the year ended December 31, 2015, building and equipment rental expenses from centers that were acquired subsequent to January 1, 2015, and excluded from the above comparison, was $7.1 million.
| 45 |
| · | Medical supplies |
Medical supplies expense increased $2.3 million, or 4.7%, to $51.7 million for the year ended December 31, 2016, compared to $49.4 million for the year ended December 31, 2015.
Medical supplies expense, including only those centers which were in operation throughout the full fiscal years of both 2016 and 2015, decreased $2.2 million, or 4.6%. This 4.6% decrease is primarily due to renegotiation of our medical supplier contracts. This comparison excludes contributions from centers that were acquired or divested subsequent to January 1, 2016. For the year ended December 31, 2016, medical supplies expense from centers that were acquired subsequent to January 1, 2015, and excluded from the above comparison was $7.1 million. For the year ended December 31, 2015, medical supplies expense from centers that were acquired subsequent to January 1, 2015, and excluded from the above comparison was $2.6 million.
| · | Other operating expenses |
Other operating expenses increased $21.3 million, or 12.0%, to $198.3 million for the year ended December 31, 2016 compared to $177.0 million for the year ended December 31, 2015.
Other operating expenses, including only those centers which were in operation throughout the full fiscal years of both 2016 and 2015, decreased $2.5 million or 1.6%. This comparison excludes contributions from centers that were acquired or divested subsequent to January 1, 2015. For the year ended December 31, 2016, other operating expenses from centers that were acquired subsequent to January 1, 2015, and excluded from the above comparison were $43.5 million. For the year ended December 31, 2015, other operating expenses from centers that were acquired subsequent to January 1, 2015, and excluded from the above comparison were $19.7 million.
| · | Depreciation and amortization expense |
Depreciation and amortization expense increased $6.0 million, or 9.9%, to $66.6 million for the year ended December 31, 2016 when compared $60.6 million for the year ended December 31, 2015.
Depreciation and amortization expense at those centers which were in operation throughout the full fiscal years of both 2016 and 2015, increased $793,000 or 1.4%. This comparison excludes contributions from centers that were acquired or divested subsequent to January 1, 2015. For the year ended December 31, 2016, depreciation and amortization from centers that were acquired or divested subsequent to January 1, 2015 and excluded from the above comparison was $10.0 million. For the year ended December 31, 2015, depreciation and amortization from centers that were acquired subsequent to January 1, 2015 and excluded from the above comparison was $4.8 million.
| · | Loss on sale and disposal of equipment |
Loss on sale of equipment was $767,000 and $866,000 for the years ended December 31, 2016 and 2015, respectively, and primarily related to the difference between the net book value of certain equipment sold and proceeds we received from the sale.
| · | Severance costs |
During the year ended December 31, 2016, we had severance costs of $2.9 million compared to $745,000 recorded during the year ended December 31, 2015. In the third quarter of 2016, we incurred severance expenses of $2.2 million specifically related to the integration of acquisitions in the state of New York.
Interest expense
Interest expense increased approximately $1.8 million, or 4.3%, to $43.5 million for the year ended December 31, 2016 compared to $41.7 million for the year ended December 31, 2015. Interest expense for the year ended December 31, 2016 included $4.3 million of amortization of deferred financing and discount on issuance of debt, as well as a write off of $709,000 of deferred financing costs in relation to the Restatement Amendment and $93,000 of other non cash interest. Interest expense for the year ended December 31, 2015 included $5.4 million of amortization of deferred financing costs and discount on issuance of debt as well as $61,000 in other non cash interest.
| 46 |
The cash portion of interest expense increased approximately $2.1 million for the year ended December 31, 2016 compared to the year ended December 31, 2015. The increase was primarily due to higher interest rates on our term loan debt stemming from the Restatement Amendment and First Lien Credit Agreement. See “Liquidity and Capital Resources” below for more details on our financing activity during 2016.
Meaningful use incentive
For the years ended December 31, 2016 and December 31, 2015, we recognized other income from meaningful use incentive in the amount of $2.8 million and $3.3 million, respectively. This amount was earned under a Medicare program to promote the use of electronic health record technology.
Equity in earnings from unconsolidated joint ventures
Equity in earnings from our unconsolidated joint ventures increased $840,000 or 9.4% to $9.8 million for the year ended December 31, 2016 compared to $8.9 million for the year ended December 31, 2015. The increase relates mainly to equity in earnings stemming from the September 30, 2015 sale of 10 wholly owned centers from our subsidiary New Jersey Imaging Partners to New Jersey Imaging Networks, a joint venture where we hold a 49% non-controlling interest.
Gain on Sale of Imaging Center
On September 30, 2015, we recognized a gain on the sale of 10 wholly owned imaging centers to the New Jersey Imaging Networks in the amount of $5.4 million.
Gain on return of common stock
In the second quarter of 2016, we recorded a gain on return of common stock of $5.0 million.
Other expenses / income
For the year ended December 31, 2016 we recorded approximately $196,000 of other expenses. For the year ended December 31, 2015, we recorded $419,000 of other expenses mainly related to acquisition activity.
Provision for income tax expense
For the years ended December 31, 2016 and December 31, 2015, we recorded income tax expense of $4.4 million and $6.0 million, respectively.
Non-GAAP Financial Measures
We use both GAAP and non-GAAP metrics to measure our financial results. We believe that, in addition to GAAP metrics, non-GAAP metrics such as Adjusted EBITDA and Free Cash Flow assist us in measuring our cash generated from operations and ability to service our debt obligations.
Adjusted EBITDA
Our Adjusted EBITDA metric removes non-cash and non-recurring charges that occur in the affected period and provides a basis for measuring the Company’s core financial performance against other periods.
We define Adjusted EBITDA as earnings before interest, taxes, depreciation and amortization, as adjusted to exclude losses or gains on the disposal of equipment, other income or loss, loss on debt extinguishments, bargain purchase gains, loss on de-consolidation of joint ventures and non-cash equity compensation. Adjusted EBITDA includes equity earnings in unconsolidated operations and subtracts allocations of earnings to non-controlling interests in subsidiaries, and is adjusted for non-cash or one-time events that take place during the period.
| 47 |
Adjusted EBITDA is a non-GAAP financial measure used as an analytical indicator by us and the healthcare industry to assess business performance, and is a measure of leverage capacity and ability to service debt. Adjusted EBITDA should not be considered a measure of financial performance under GAAP, and the items excluded from Adjusted EBITDA should not be considered in isolation or as alternatives to net income, cash flows generated by operating, investing or financing activities or other financial statement data presented in the consolidated financial statements as an indicator of financial performance or liquidity. As Adjusted EBITDA is not a measurement determined in accordance with GAAP and is therefore susceptible to varying methods of calculation, this metric, as presented, may not be comparable to other similarly titled measures of other companies.
The following is a reconciliation of the nearest comparable GAAP financial measure, net income, to Adjusted EBITDA for the years ended December 31, 2017, 2016, and 2015, respectively (in thousands):
| Years Ended December 31, | ||||||||||||
| 2017 | 2016 | 2015 | ||||||||||
| Net income attributable to RadNet, Inc. common stockholders | $ | 53 | $ | 7,230 | $ | 7,709 | ||||||
| Plus provision for income taxes | 24,310 | 4,432 | 6,007 | |||||||||
| Plus other expenses | – | 196 | 419 | |||||||||
| Plus interest expense | 40,623 | 43,455 | 41,684 | |||||||||
| Plus severance costs | 1,821 | 2,877 | 745 | |||||||||
| Plus loss on sale and disposal of equipment | 1,142 | 767 | 866 | |||||||||
| Plus acquisition related working capital adjustment | – | 6,072 | – | |||||||||
| Plus legal settlements | – | – | 1,425 | |||||||||
| Plus reimbursable legal expenses | 723 | – | – | |||||||||
| Plus refinancing fees | 235 | 606 | – | |||||||||
| Plus expenses of divested/closed operations | 3,186 | – | – | |||||||||
| Less gain on sale of imaging center and medical practice | (3,146 | ) | – | (5,434 | ) | |||||||
| Less gain on return of common stock | – | (5,032 | ) | |||||||||
| Less other income | (8 | ) | – | – | ||||||||
| Plus depreciation and amortization | 66,796 | 66,610 | 60,611 | |||||||||
| Plus non-cash employee stock-based compensation | 6,787 | 5,826 | 7,647 | |||||||||
| Adjusted EBITDA | $ | 142,522 | $ | 133,039 | $ | 121,679 | ||||||
Free Cash Flow
Another non-GAAP measure that we use is “Free Cash Flow”. We use free cash flow as an additional way of viewing our liquidity that, when viewed with our GAAP results, provides a more complete understanding of factors and trends affecting our cash flows, and consequently our ability to service debt and make capital expenditures. Free cash flow is used in addition to and in conjunction with results presented in accordance with GAAP and free cash flow should not be relied upon to the exclusion of GAAP financial measures.
We define free cash flow as Adjusted EBITDA, less capital expenditures, and less the cash portion of our interest expense. We reconcile free cash flow to “net cash flows provided by operating activities”. We use free cash flow to conduct and evaluate our business because, although it is similar to cash flow from operations, we believe it is a more conservative measure of cash flows since purchases of fixed assets and the cash portion of our interest expense are a necessary component of our ongoing operations. In limited circumstances in which proceeds from sales of fixed assets exceed purchases, free cash flow could exceed cash flow from operations. This occurred in the year ended December 31, 2015 and was related to the sale of our wholly-owned imaging centers in the state of New Jersey to the New Jersey Imaging Networks. However, since we do not anticipate being a net seller of fixed assets, we expect free cash flow to be less than operating cash flows.
Free cash flow has limitations due to the fact that it does not represent the residual cash flow available for discretionary expenditures. For example, free cash flow does not incorporate payments made on capital lease obligations or cash payments for business acquisitions. Therefore, we believe it is important to view Free Cash Flow as a complement to our entire consolidated statements of cash flows.
| 48 |
The following table provides a reconciliation of free cash flow to “net cash flows from operations” the most directly comparable amounts reported in accordance with GAAP for the years ended December 31, 2017, 2016 and 2015:
| Years Ended December 31, | ||||||||||||
| 2017 | 2016 | 2015 | ||||||||||
| Adjusted EBITDA | $ | 142,522 | $ | 133,039 | $ | 121,679 | ||||||
| Less cash paid for interest | (34,197 | ) | (37,487 | ) | (36,028 | ) | ||||||
| Less cash capital purchases | (61,336 | ) | (59,251 | ) | (42,964 | ) | ||||||
| Less new capital lease debt | (5,504 | ) | (1,268 | ) | (7,753 | ) | ||||||
| Plus proceeds from sale of equipment | 852 | 481 | 1,282 | |||||||||
| Plus proceeds from sale of imaging and medical practice assets | 8,429 | – | 35,500 | |||||||||
| Free cash flow | $ | 50,766 | $ | 35,514 | $ | 71,716 | ||||||
| Free cash flow as a percent of | ||||||||||||
| cash flow from operations | 35.7 | % | 38.8 | % | 107.0 | % | ||||||
Liquidity and Capital Resources
We had net income attributable to RadNet, Inc.’s common stockholders of $53,000, $7.2 million and $7.7 million for the years ended December 31, 2017, 2016 and 2015, respectively. We had cash and cash equivalents of $51.3 million and accounts receivable of $155.5 million at December 31, 2017, compared to cash of $20.6 and accounts receivable of $164.2 million at December 31, 2016. We had a working capital balance of $43.7 million and $62.6 million at December 31, 2017 and 2016, respectively. We also had total equity of $69.9 million and $52.1 million at December 31, 2017 and 2016, respectively.
We operate in a capital intensive, high fixed-cost industry that requires significant amounts of capital to fund operations. In addition to operations, we require a significant amount of capital for the initial start-up and development of new diagnostic imaging facilities, the acquisition of additional facilities and new diagnostic imaging equipment. Because our cash flows from operations have been insufficient to fund all of these capital requirements, we have depended on the availability of financing under credit arrangements with third parties.
Based on our current level of operations, we believe that cash flow from operations and over the next twelve months available cash, together with available borrowings from our senior secured credit facilities, will be adequate to meet our short-term liquidity needs. Our future liquidity requirements will be for working capital, capital expenditures, debt service and general corporate purposes. Our ability to meet our working capital and debt service requirements, however, is subject to future economic conditions and to financial, business and other factors, many of which are beyond our control. If we are not able to meet such requirements, we may be required to seek additional financing. There can be no assurance that we will be able to obtain financing from other sources on the terms acceptable to us, if at all.
On a continuing basis, we also consider various transactions to increase stockholder value and enhance our business results, including acquisitions, divestitures and joint ventures. These types of transactions may result in future cash proceeds or payments but the general timing, size or success of any acquisition, divestiture or joint venture effort and the related potential capital commitments cannot be predicted. We expect to fund any future acquisitions primarily with cash flow from operations and borrowings, including borrowing from amounts available under our senior secured credit facilities or through new equity or debt issuances.
We and our subsidiaries or affiliates may from time to time, in our or their sole discretion, continue to purchase, repay, redeem or retire any of our outstanding debt or equity securities in privately negotiated or open market transactions, by tender offer or otherwise. However, we have no formal plan of doing so at this time.
Sources and Uses of Cash
Cash provided by operating activities was $142.2 million, $91.6 million, and $67.0 million, for the years ended December 31, 2017, 2016 and 2015, respectively.
Cash used in investing activities was $79.3 million, $65.5 million, and $96.8 million, for the years ended December 31, 2017, 2016 and 2015, respectively. For the year ended December 31, 2017, we purchased property and equipment for approximately $61.3 million, acquired the assets and businesses of additional imaging facilities for approximately $27.6 million. Offsetting our cash used in investing activities we received $8.4 million in proceeds from the sale of imaging and medical practice assets and $1.5 million received from joint venture partners.
| 49 |
Cash used in financing activities was $32.2 million for the year ended December 31, 2017, compared to cash used in financing activities of $5.9 million and cash provided by financing activities of $29.9 million for the years ended December 31, 2016 and December 31, 2015, respectively. The cash used by financing for the year ended December 31, 2017 consisted of $170.0 million in new borrowings from the Fifth Amendment and Incremental Joinder Agreement with respect to our First Lien Credit Agreement. See financing activity in 2017 below for a further description on this event. Payments on secured debt and revolver loans amounted to $196.7 million, which included a full payoff of the balance of our Second Lien Credit and Guaranty Agreement and contractual payments of equipment notes and capital leases totaled $6.8 million.
Senior Secured Credit Facilities
At December 31, 2017, our credit facilities were comprised of one tranche of senior secured first lien term loans (the “First Lien Term Loans”) and a revolving credit facility (the “Revolving Credit Facility”), both of which are provided pursuant to the Amended and Restated First Lien Credit and Guaranty Agreement dated as of July 1, 2016 (as amended, the “First Lien Credit Agreement”). At December 31, 2017, we had $620.3 million aggregate principal amount of First Lien Term Loans outstanding and no principal borrowed under our Revolving Credit Facility. The Revolving Credit Facility provides for a maximum borrowing limit of $117.5 million and fully available to us at December 31, 2017, subject to customary drawing conditions.
As of December 31, 2017, we were in compliance with all covenants under out credit facilities.
The following describes our 2017 financing activities:
Amendment No. 5, Consent and Incremental Joinder Agreement to Credit and Guaranty Agreement
On August 22, 2017, we entered into Amendment No. 5, Consent and Incremental Joinder Agreement to Credit and Guaranty Agreement (the “Fifth Amendment”) with respect to our First Lien Credit Agreement. Pursuant to the Fifth Amendment, we issued $170.0 million in incremental First Lien Term Loans, the proceeds of which were used to repay in full all outstanding Second Lien Term Loans and all other obligations under the Second Lien Credit Agreement.
Pursuant to the Fifth Amendment, we also changed the interest rate margin applicable to borrowings under the First Lien Credit Agreement. While borrowings under the First Lien Credit Agreement continue to bear interest at either an Adjusted Eurodollar Rate or a Base Rate (in each case, as more fully defined in the First Lien Credit Agreement) or a combination of both, at the election of the Company, plus an applicable margin. The applicable margin for Adjusted Eurodollar Rate borrowings and Base Rate borrowings was changed from 3.25% and 2.25%, respectively, to 3.75% and 2.75%, respectively, through an initial period which ends when financial reporting is delivered for the period ending September 30, 2017. Thereafter, the rates of the applicable margin for borrowing under the First Lien Credit Agreement will adjust depending on our leverage ratio, according to the following schedule:
| First Lien Leverage Ratio | Eurodollar Rate Spread | Base Rate Spread |
| > 5.50x | 4.50% | 3.50% |
| > 4.00x but ≤ 5.50x | 3.75% | 2.75% |
| >3.50x but ≤ 4.00x | 3.50% | 2.50% |
| ≤ 3.50x | 3.25% | 2.25% |
At December 31, 2017 the effective Adjusted Eurodollar Rate and the Base Rate for the First Lien Term Loans was 1.36% and 4.50%, respectively, and the applicable margin for Adjusted Eurodollar Rate and Base Rate borrowings remained at 3.75% and 2.75%, respectively.
Pursuant to the Fifth Amendment, the First Lien Credit Agreement was amended so that we can elect to request 1) an increase to the existing Revolving Credit Facility and/or 2) additional First Lien Term Loans, provided that the aggregate amount of such increases and additions does not exceed (a) $100.0 million and (b) as long as the First Lien Leverage Ratio (as defined in the First Lien Credit Agreement) would not exceed 4.00:1.00 after giving effect to such incremental facilities, an uncapped amount of incremental facilities, in each case subject to the conditions and limitations set forth in the First Lien Credit Agreement. Each lender approached to provide all or a portion of any incremental facility may elect or decline, in its sole discretion, to provide an incremental commitment or loan.
Pursuant to the Fifth Amendment, the First Lien Credit Agreement was also amended to (i) provide for quarterly payments of principal of the First Lien Term Loans in the amount of approximately $8.3 million, as compared to approximately $6.1 million prior to the Fifth Amendment, (ii) extend the call protection provided to the holders of the First Lien Term Loans for a period of twelve months following the date of the Fifth Amendment and (iii) provide us with additional operating flexibility, including the ability to incur certain additional debt and to make certain additional restricted payments, investments and dispositions, in each case as more fully set forth in the Fifth Amendment. Total issue costs for the Fifth Amendment aggregated to approximately $4.7 million. Of this amount, $4.1 million was identified and capitalized as discount on debt, $350,000 was capitalized as deferred financing costs and the remaining $235,000 was expensed. Amounts capitalized will be amortized over the remaining term of the agreement.
| 50 |
Fourth Amendment to First Lien Credit Agreement
On February 2, 2017, we entered into Amendment No. 4 to Credit and Guaranty Agreement (the “Fourth Amendment”) with respect to our First Lien Credit Agreement. Pursuant to the Fourth Amendment, the interest rate margin per annum on the First Lien Term Loans and the Revolving Credit Facility was reduced by 50 basis points, from 3.75% to 3.25%. Except for such reduction in the interest rate on credit extensions, the Fourth Amendment did not result in any other material modifications to the First Lien Credit Agreement. RadNet incurred expenses for the transaction in the amount of $543,000, which was recorded to discount on debt and will be amortized over the remaining term of the agreement.
The following describes our applicable financing prior to giving effect to the Fourth Amendment and Fifth Amendment discussed above.
First Lien Credit Agreement
On July 1, 2016, we entered into the First Lien Credit Agreement pursuant to which we amended and restated our then existing first lien credit facilities. Pursuant to the First Lien Credit Agreement, we originally issued $485 million of First Lien Term Loans and established the $117.5 million Revolving Credit Facility. Proceeds from the First Lien Credit Agreement were used to repay the previously outstanding first lien loans under the First Lien Credit Agreement, make a $12.0 million principal payment of the Second Lien Term Loans, pay costs and expenses related to the First Lien Credit Agreement and provide approximately $10.0 million for general corporate purposes.
Interest. The interest rates payable on the First Lien Term Loans were (a) the Adjusted Eurodollar Rate (as defined in the First Lien Credit Agreement) plus 3.75% per annum or (b) the Base Rate (as defined in the First Lien Credit Agreement) plus 2.75% per annum. As applied to the First Lien Term Loans, the Adjusted Eurodollar Rate has a minimum floor of 1.0%.
Payments. The scheduled quarterly principal payments of the First Lien Term Loans was approximately $6.1 million, with the balance due at maturity.
Maturity Date. The maturity date for the First Lien Term Loans shall be on the earliest to occur of (i) July 1, 2023, (ii) the date on which all First Lien Term Loans shall become due and payable in full under the First Lien Credit Agreement, whether by acceleration or otherwise, and (iii) September 25, 2020 if our indebtedness under the Second Lien Credit Agreement had not been repaid, refinanced or extended prior to such date.
Revolving Credit Facility: The First Lien Credit Agreement provides for a $117.5 million Revolving Credit Facility. Revolving loans borrowed under the Revolving Credit Facility bear interest at either an Adjusted Eurodollar Rate or a Base Rate (in each case, as more fully defined in the First Lien Credit Agreement), plus an applicable margin. Pursuant to the Fifth Amendment, the applicable margin was amended to vary based on our leverage ratio in accordance with the following schedule:
| First Lien Leverage Ratio | Eurodollar Rate Spread | Base Rate Spread |
| > 5.50x | 4.50% | 3.50% |
| > 4.00x but ≤ 5.50x | 3.75% | 2.75% |
| >3.50x but ≤ 4.00x | 3.50% | 2.50% |
| ≤ 3.50x | 3.25% | 2.25% |
For letters of credit issued under the Revolving Credit Facility, letter of credit fees accrue at the applicable margin (see table above) for Adjusted Eurodollar Rate revolving loans and fronting fees accrue at 0.25% per annum, in each case on the average aggregate daily maximum amount available to be drawn under all letters of credit issued under the First Lien Credit Agreement. In addition a commitment fee of 0.5% per annum accrues on the unused revolver commitments under the Revolving Credit Facility. As of December 31, 2017, the interest rate payable on revolving loans was 7.0%.
The Revolving Credit Facility will terminate on the earliest to occur of (i) July 1, 2021, (ii) the date we voluntarily agree to permanently reduce the Revolving Credit Facility to zero pursuant to section 2.13(b) of the First Lien Credit Agreement, and (iii) the date the Revolving Credit Facility is terminated due to specific events of default pursuant to section 8.01 of the First Lien Credit Agreement.
| 51 |
Second Lien Credit Agreement:
On March 25, 2014, we entered into the Second Lien Credit and Guaranty Agreement (the “Second Lien Credit Agreement”) pursuant to which we issued $180 million of second lien term loans (the “Second Lien Term Loans”). The proceeds from the Second Lien Term Loans were used to redeem our 10 3/8% senior unsecured notes, due 2018, to pay the expenses related to the transaction and for general corporate purposes. On July 1, 2016, in conjunction with the restated First Lien Credit Agreement, a $12.0 million principal payment was made on the Second Lien Term Loans. On August 22, 2017 the Second Lien Credit Agreement was repaid in full with the proceeds of First Lien Term Loans issued under the Fifth Amendment, as described above.
Contractual Commitments
Our future obligations for notes payable, equipment under capital leases, lines of credit, equipment and building operating leases and purchase and other contractual obligations for the next five years and thereafter include (dollars in thousands):
| 2018 | 2019 | 2020 | 2021 | 2022 | Thereafter | Total | ||||||||||||||||||||||
| Notes payable (1) | $ | 67,285 | $ | 65,215 | $ | 63,196 | $ | 61,266 | $ | 59,432 | $ | 467,450 | $ | 783,844 | ||||||||||||||
| Capital leases (2) | 4,080 | 2,276 | 282 | 162 | 59 | – | 6,859 | |||||||||||||||||||||
| Operating leases (3) | 68,458 | 60,128 | 51,073 | 42,076 | 31,954 | 105,954 | 359,643 | |||||||||||||||||||||
| Total | $ | 139,823 | $ | 127,619 | $ | 114,551 | $ | 103,504 | $ | 91,445 | $ | 573,404 | $ | 1,150,346 | ||||||||||||||
| (1) | Includes variable rate debt for which the contractual obligation was estimated using the applicable rate at December 31, 2017. |
| (2) | Includes interest component of capital lease obligations. |
| (3) | Includes all operating leases through the end of their main lease term, excluding options on facility leases. |
We have an arrangement with GE Medical Systems under which it has agreed to be responsible for the maintenance and repair of a majority of our equipment for a fee that is based on the type and age of the equipment. Under this agreement, we are committed to minimum payments of approximately $27.0 million per year through 2019.
Critical Accounting Policies
USE OF ESTIMATES - The financial statements were prepared in accordance with U.S. generally accepted accounting principles (GAAP), which requires management to make estimates and assumptions that affect the amounts reported in the financial statements and accompanying notes. These estimates and assumptions affect various matters, including our reported amounts of assets and liabilities in our consolidated balance sheets at the dates of the financial statements; our disclosure of contingent assets and liabilities at the dates of the financial statements; and our reported amounts of revenues and expenses in our consolidated statements of operations during the reporting periods. These estimates involve judgments with respect to numerous factors that are difficult to predict and are beyond management’s control. As a result, actual amounts could materially differ from these estimates.
REVENUES - Service fee revenue, net of contractual allowances and discounts, consists of net patient fees received from various payors and patients themselves based mainly upon established contractual billing rates, less allowances for contractual adjustments and discounts. As it relates to BRMG and the NY Groups centers, this service fee revenue includes payments for both the professional medical interpretation revenue recognized by BRMG and the NY Groups as well as the payment for all other aspects related to our providing the imaging services, for which we earn management fees from BRMG and the NY Groups. As it relates to non-BRMG and NY Groups centers, namely the affiliated physician groups, this service fee revenue is earned through providing the use of our diagnostic imaging equipment and the provision of technical services as well as providing administration services such as clerical and administrative personnel, bookkeeping and accounting services, billing and collection, provision of medical and office supplies, secretarial, reception and transcription services, maintenance of medical records, and advertising, marketing and promotional activities.
| 52 |
Service fee revenues are recorded during the period the services are provided based upon the estimated amounts due from the patients and third-party payors. Third-party payors include federal and state agencies (under the Medicare and Medicaid programs), managed care health plans, commercial insurance companies and employers. Estimates of contractual allowances are based on historical collection rates of payor reimbursement contract agreements. We also record a provision for doubtful accounts based primarily on historical collection rates related to patient copayments and deductible amounts for patients who have health care coverage under one of our third-party payors.
Under capitation arrangements with various health plans, we earn a per-enrollee amount each month for making available diagnostic imaging services to all plan enrollees under the capitation arrangement. Revenue under capitation arrangements is recognized in the period in which we are obligated to provide services to plan enrollees under contracts with various health plans.
Our service fee revenue, net of contractual allowances and discounts, the provision for bad debts, and revenue under capitation arrangements for the years ended December 31, are summarized in the following table (in thousands) :
| Years Ended December 31, | ||||||||||||
| 2017 | 2016 | 2015 | ||||||||||
| Commercial insurance | $ | 571,369 | $ | 539,793 | $ | 486,489 | ||||||
| Medicare | 193,166 | 187,941 | 168,545 | |||||||||
| Medicaid | 25,821 | 28,170 | 23,948 | |||||||||
| Workers' compensation/personal injury | 35,195 | 36,548 | 32,728 | |||||||||
| Other (1) | 31,627 | 29,135 | 35,046 | |||||||||
| Service fee revenue, net of contractual allowances and discounts | 857,178 | 821,587 | 746,756 | |||||||||
| Provision for bad debts | (46,555 | ) | (45,387 | ) | (36,033 | ) | ||||||
| Net service fee revenue | 810,623 | 776,200 | 710,723 | |||||||||
| Revenue under capitation arrangements | 111,563 | 108,335 | 98,905 | |||||||||
| Total net revenue | $ | 922,186 | $ | 884,535 | $ | 809,628 | ||||||
(1) Other consists of revenue from teleradiology services, consulting fees and software revenue.
PROVISION FOR BAD DEBTS - We provide for an allowance against accounts receivable that could become uncollectible to reduce the carrying value of such receivables to their estimated net realizable value. We estimate this allowance based on the aging of our accounts receivable by the historical payment patterns of each type of payor, write-off trends, and other relevant factors. A significant portion of our provision for bad debt relates to co-payments and deductibles owed to us from patients with insurance. Although we attempt to collect deductibles and co-payments due from patients with insurance at the time of service, this attempt to collect at the time of service is not an assessment of the patient’s ability to pay nor are revenues recognized based on an assessment of the patient’s ability to pay. There are various factors that can impact collection trends, such as changes in the economy, which in turn have an impact on the increased burden of co-payments and deductibles to be made by patients with insurance. These factors continuously change and can have an impact on collection trends and our estimation process. Our allowance for bad debts at December 31, 2017 and 2016 was $34.6 million and $20.7 million, respectively.
GOODWILL AND INDEFINITE LIVED INTANGIBLES - Goodwill at December 31, 2017 totaled $256.8 million and $239.6 million at December 31, 2016. Indefinite lived intangible assets at December 31, 2017 and 2016 totaled $7.9 million and are associated with the value of certain trade name intangibles. Goodwill and trade name intangibles are recorded as a result of business combinations. Management evaluates goodwill and trade name intangibles, at a minimum, on an annual basis and whenever events and changes in circumstances suggest that the carrying amount may not be recoverable. Impairment of goodwill is tested at the reporting unit level by comparing the reporting unit’s carrying amount, including goodwill, to the fair value of the reporting unit. The fair value of a reporting unit is estimated using a combination of the income or discounted cash flows approach and the market approach, which uses comparable market data. If the carrying amount of the reporting unit exceeds its fair value, goodwill is considered impaired and a second step is performed to measure the amount of impairment loss, if any. Impairment of trade name intangibles is tested at the subsidiary level by comparing the subsidiary’s trade name carrying amount to its respective fair value. We tested both goodwill and trade name intangibles for impairment on October 1, 2017, noting no impairment, and have not identified any indicators of impairment through December 31, 2017.
| 53 |
Recent Accounting Standards
Stated below are accounting policies which are under evaluation for their potential impact on our statement of operations and cash flows.
In May 2014, the FASB issued ASU No. 2014-09, Revenue from Contracts with Customers, (Topic 606). ASU 2014-09 requires an entity to recognize as revenue the amount that reflects the consideration to which it expects to be entitled in exchange for goods or services as it transfers control to its customers. It also requires more detailed disclosures to enable users of the financial statements to understand the nature, amount, timing and uncertainty of revenue and cash flows arising from contracts with customers. The Company’s current revenue recognition policies for our most significant revenue streams, materially comply with the amended guidance. The primary change for healthcare providers under the new guidance is the requirement to report the allowance for uncollectible accounts associated with patient responsibility amounts as a reduction in net revenue as opposed to bad debt expense as a component of operating expenses. The new standard supersedes most current revenue guidance, including industry-specific guidance, and may be applied retrospectively with cumulative effect recognized in retained earnings as of the date of adoption (modified retrospective method). The guidance became effective for the Company on January 1, 2018 and the Company adopted the new standard using the modified retrospective approach. As part of adopting the standard, the Company identified revenue streams of like contracts to allow for ease of implementation. The Company used primarily a portfolio approach to apply the new model to classes of customers with similar characteristics. The impact of adopting the new standard on our total revenue; and income from operations is not material. The immaterial impact of adopting Topic 606 primarily relates to recognizing certain credit and collection issues not known at the date of service, including bankruptcy, in the provision for uncollectible accounts included in expenses on the consolidated statement of operations, which previously were netted against service revenue. The impact to income from current activities is not material because the analysis of our contracts under the new revenue recognition standard supports the recognition of revenue consistent with our current revenue recognition model. In addition, the number of our performance obligations under the new standard is not materially different from our contract segments under the existing standard. Lastly, the accounting for the estimate of variable consideration is not materially different compared to our current practice. As such, the adoption of this guidance is not expected to have a material impact on our Consolidated Financial Statements.
In February 2016, the FASB issued ASU No. 2016-02, Leases, (Topic 842): Amendments to the FASB Accounting Standards Codification. ASU 2016-02 amends the existing accounting standards for lease accounting, including requiring lessees to recognize most leases on their balance sheets and making targeted changes to lessor accounting. The new standard requires a modified retrospective transition approach for all leases existing at, or entered into after, the date of initial application, with an option to use certain transition relief. The amendments in this update are effective for fiscal years (and interim reporting periods within fiscal years) beginning after December 15, 2018. Early adoption of the amendments is permitted for all entities. We are currently evaluating the impact this guidance will have on our consolidated financial statements, but expect this adoption will result in a significant increase in the assets and liabilities related to our leased properties and equipment.
In February 2018, the FASB issued ASU No. 2018-02 (“ASU 2018-02”), Reclassification of Certain Tax Effects from Accumulated Other Comprehensive Income. ASU 2018-02 allows for the reclassification of certain income tax effects related to the Tax Cuts and Jobs Act between “Accumulated other comprehensive income” and “Retained earnings.” This ASU relates to the requirement that adjustments to deferred tax liabilities and assets related to a change in tax laws or rates be included in “Income from continuing operations”, even in situations where the related items were originally recognized in “Other comprehensive income” (rather than in “Income from continuing operations”). ASU 2018-02 is effective for all entities for fiscal years beginning after December 15, 2018, and interim periods within those fiscal years, with early adoption permitted. Adoption of this ASU is to be applied either in the period of adoption or retrospectively to each period in which the effect of the change in the tax laws or rates were recognized. We are evaluating the effect of this guidance.
In January 2017, the FASB issued ASU No. 2017-04 (“ASU 2017-04”), Simplifying the Test for Goodwill Impairment. ASU 2017-04 eliminates the requirement to calculate the implied fair value of goodwill (i.e., Step 2 of the current goodwill impairment test) to measure a goodwill impairment charge. Instead, entities will record an impairment charge based on the excess of a reporting unit’s carrying amount over its fair value (i.e., measure the charge based on the current Step 1). ASU 2017-04 is effective for annual and any interim impairment tests for periods beginning after December 15, 2019, with early adoption permitted. We are evaluating the effect of this guidance.
In January 2017, the FASB issued ASU No. 2017-01 (“ASU 2017-01”), Clarifying the Definition of a Business. ASU 2017-01 changes the definition of a business to assist entities with evaluating when a set of transferred assets and activities is considered a business. ASU 2017-01 is effective for annual periods beginning after December 31, 2017 including interim periods within those periods. We do not anticipate any material impact on our financial position.
| 54 |
Subsequent Events
On January 1, 2018 we completed our acquisition of certain assets of Imaging Services Company of New York, LLC, consisting of a single multi-modality center located in New York, New York, for purchase consideration of $5.8 million.
On January 1, 2018, we formed Beach Imaging Group, LLC (“Beach Imaging”) and contributed the operations of 24 imaging facilities spread across southern Los Angeles and Orange Counties in exchange for a 60% economic interest. MemorialCare Medical Foundation (MCMF), a hospital system in southern California, contributed $22.9 million in cash along with the operations of 10 of its imaging facilities in southern California to receive a 40% economic interest in Beach Imaging. In connection with the same transaction, Beach Imaging agreed to sell one of its newly acquired imaging center from RadNet to MCMF for $1.7 million.
Additional Information
Additional information concerning RadNet, Inc., including our consolidated subsidiaries, for each of the years ended December 31, 2017, 2016 and 2015 is included in the consolidated financial statements and notes thereto in this annual report.
| Item 7A. | Quantitative and Qualitative Disclosures About Market Risk |
Foreign Currency Exchange Risk. We receive payment for our services exclusively in United States dollars. As a result, our financial results are unlikely to be affected by factors such as changes in foreign currency, exchange rates or weak economic conditions in foreign markets.
We maintain research and development facilities in Prince Edward Island, Canada and Budapest, Hungary for which expenses are paid in the local currency. Accordingly, we do have currency risk resulting from fluctuations between such local currency and the United States Dollar. At the present time, we do not have any foreign currency exchange contracts to mitigate this risk. At December 31, 2017, a hypothetical 1% decline in the currency exchange rates between the U.S. dollar against the Canadian dollar and the Hungarian Forint would have resulted in an annual increase of approximately $33,000 in operating expenses.
Interest Rate Sensitivity We pay interest on various types of debt instruments to our suppliers and lending institutions. The agreements entail either fixed or variable interest rates. Instruments which have fixed rates are mainly leases on radiology equipment. Variable rate interest obligations relate primarily to amounts borrowed under our outstanding credit facilities. Accordingly, our interest expense and consequently, our earnings, are affected by changes in short term interest rates. However due to our purchase of caps, described below, the effects of interest rate changes are limited.
At December 31, 2017, we had $620.3 million outstanding subject to an adjusted Eurodollar election on First Lien Term Loans. We can elect Eurodollar or Base Rate (Prime) interest rate options on amounts outstanding under the First Lien Term Loans.
To mitigate interest rate risk sensitivity, in the fourth quarter of 2016 we entered into two forward interest rate cap agreements (the “2016 Caps”) which were designated at inception as cash flow hedges of future cash interest payments. The 2016 Caps are designed to provide a hedge against interest rate increases. Under these arrangements, we purchased a cap on 3 month LIBOR at 2.0%. At December 31, 2017, our effective 3 month LIBOR was 1.36%. The 2016 Caps have a notional amount of $150,000,000 and $350,000,000 and will mature in September and October 2020. We are liable for a $5.3 million premium to enter into the caps which is being accrued over the life of the 2016 Caps. See Note 2 to the consolidated financial statements contained herein.
A hypothetical 1% increase in the adjusted Eurodollar rates under the First Lien Credit Agreement over the rates experienced in 2016 would, after considering the effects of the 2016 Caps, result in an increase of $4.0 million in annual interest expense and a corresponding decrease in income before taxes. At December 31, 2017, an additional $8.1 million in debt instruments is tied to the prime rate. A hypothetical 1% increase in the prime rate would result in an annual increase in interest expense of approximately $81,000 and a corresponding decrease in income before taxes. These amounts are determined by considering the impact of the hypothetical interest rates on the borrowing costs and cap agreements. These analyses do not consider the effects of the reduced level of overall economic activity that could exist in such an environment. Further, in the event of a change of such magnitude, our management would likely take actions to further mitigate its exposure to the change. However, due to the uncertainty of the specific actions that would be taken and their possible effects, the sensitivity analysis assumes no changes in our financial structure.
| 55 |
| Item 8. | Financial Statements and Supplementary Data |
The Financial Statements are attached hereto and begin on page 57.
| 56 |
Report of Independent Registered Public Accounting Firm
To the Stockholders and the Board of Directors of RadNet, Inc.
Opinion on the Financial Statements
We have audited the accompanying consolidated balance sheets of RadNet, Inc. and subsidiaries (the Company) as of December 31, 2017 and 2016, the related consolidated statements of operations, comprehensive (loss) income, equity, and cash flows for each of the three years in the period ended December 31, 2017, and the related notes and the financial statement schedule listed in the Index at Item 15(a)(2) (collectively referred to as the “consolidated financial statements”). In our opinion, the consolidated financial statements present fairly, in all material respects, the financial position of the Company at December 31, 2017 and 2016, and the results of its operations and its cash flows for each of the three years in the period ended December 31, 2017, in conformity with U.S. generally accepted accounting principles.
We also have audited, in accordance with the standards of the Public Company Accounting Oversight Board (United States) (PCAOB), the Company's internal control over financial reporting as of December 31, 2017, based on criteria established in Internal Control-Integrated Framework issued by the Committee of Sponsoring Organizations of the Treadway Commission (2013 framework), and our report dated March 16, 2018 expressed an adverse opinion thereon.
Basis for Opinion
These financial statements are the responsibility of the Company's management. Our responsibility is to express an opinion on the Company’s financial statements based on our audits. We are a public accounting firm registered with the PCAOB and are required to be independent with respect to the Company in accordance with the U.S. federal securities laws and the applicable rules and regulations of the Securities and Exchange Commission and the PCAOB.
We conducted our audits in accordance with the standards of the PCAOB. Those standards require that we plan and perform the audit to obtain reasonable assurance about whether the financial statements are free of material misstatement, whether due to error or fraud. Our audits included performing procedures to assess the risks of material misstatement of the financial statements, whether due to error or fraud, and performing procedures that respond to those risks. Such procedures included examining, on a test basis, evidence regarding the amounts and disclosures in the financial statements. Our audits also included evaluating the accounting principles used and significant estimates made by management, as well as evaluating the overall presentation of the financial statements. We believe that our audits provide a reasonable basis for our opinion.
/s/ Ernst & Young LLP
We have served as the Company’s auditor since 2007.
Los Angeles, California
March 16, 2018
| 57 |
RADNET, INC. AND SUBSIDIARIES
(IN THOUSANDS EXCEPT SHARE AND PER SHARE DATA)
| As of December 31, | ||||||||
| 2017 | 2016 | |||||||
| ASSETS | ||||||||
| CURRENT ASSETS | ||||||||
| Cash and cash equivalents | $ | 51,322 | $ | 20,638 | ||||
| Accounts receivable, net | 155,518 | 164,210 | ||||||
| Due from affiliates | 2,343 | 2,428 | ||||||
| Prepaid expenses and other current assets | 26,168 | 28,435 | ||||||
| Assets held for sale | – | 2,203 | ||||||
| Total current assets | 235,351 | 217,914 | ||||||
| PROPERTY AND EQUIPMENT, NET | 244,301 | 247,725 | ||||||
| OTHER ASSETS | ||||||||
| Goodwill | 256,776 | 239,553 | ||||||
| Other intangible assets | 40,422 | 42,682 | ||||||
| Deferred financing costs, net of current portion | 1,895 | 2,004 | ||||||
| Investment in joint ventures | 52,435 | 43,509 | ||||||
| Deferred tax assets, net of current portion | 30,852 | 50,356 | ||||||
| Deposits and other | 6,947 | 5,733 | ||||||
| Total assets | $ | 868,979 | $ | 849,476 | ||||
| LIABILITIES AND EQUITY | ||||||||
| CURRENT LIABILITIES | ||||||||
| Accounts payable, accrued expenses and other | $ | 135,809 | $ | 111,166 | ||||
| Due to affiliates | 16,387 | 13,141 | ||||||
| Deferred revenue related to software sales | 2,606 | 1,516 | ||||||
| Current portion of deferred rent | 2,714 | 2,961 | ||||||
| Current portion of notes payable | 30,224 | 22,031 | ||||||
| Current portion of obligations under capital leases | 3,866 | 4,526 | ||||||
| Total current liabilities | 191,606 | 155,341 | ||||||
| LONG-TERM LIABILITIES | ||||||||
| Deferred rent, net of current portion | 26,251 | 24,799 | ||||||
| Notes payable, net of current portion | 572,365 | 609,445 | ||||||
| Obligations under capital lease, net of current portion | 2,672 | 2,730 | ||||||
| Other non-current liabilities | 6,160 | 5,108 | ||||||
| Total liabilities | 799,054 | 797,423 | ||||||
| EQUITY | ||||||||
| RadNet, Inc. stockholders' equity: | ||||||||
| Common stock - $.0001 par value, 200,000,000 shares authorized; 47,723,915 and 46,574,904 shares issued and outstanding at December 31, 2017 and 2016, respectively | 5 | 4 | ||||||
| Additional paid-in-capital | 212,261 | 198,387 | ||||||
| Accumulated other comprehensive (loss) gain | (548 | ) | 306 | |||||
| Accumulated deficit | (150,158 | ) | (150,211 | ) | ||||
| Total RadNet, Inc.'s stockholders' equity | 61,560 | 48,486 | ||||||
| Non-controlling interests | 8,365 | 3,567 | ||||||
| Total equity | 69,925 | 52,053 | ||||||
| Total liabilities and equity | $ | 868,979 | $ | 849,476 | ||||
The accompanying notes are an integral part of these financial statements.
| 58 |
RADNET, INC. AND SUBSIDIARIES
CONSOLIDATED STATEMENTS OF OPERATIONS
(IN THOUSANDS EXCEPT SHARE AND PER SHARE DATA)
| Years Ended December 31, | ||||||||||||
| 2017 | 2016 | 2015 | ||||||||||
| NET REVENUE | ||||||||||||
| Service fee revenue, net of contractual allowances and discounts | $ | 857,178 | $ | 821,587 | $ | 746,756 | ||||||
| Provision for bad debts | (46,555 | ) | (45,387 | ) | (36,033 | ) | ||||||
| Net service fee revenue | 810,623 | 776,200 | 710,723 | |||||||||
| Revenue under capitation arrangements | 111,563 | 108,335 | 98,905 | |||||||||
| Total net revenue | 922,186 | 884,535 | 809,628 | |||||||||
| OPERATING EXPENSES | ||||||||||||
| Cost of operations, excluding depreciation and amortization | 802,377 | 775,801 | 708,289 | |||||||||
| Depreciation and amortization | 66,796 | 66,610 | 60,611 | |||||||||
| Loss on sale and disposal of equipment | 1,142 | 767 | 866 | |||||||||
| Severance costs | 1,821 | 2,877 | 745 | |||||||||
| Total operating expenses | 872,136 | 846,055 | 770,511 | |||||||||
| INCOME FROM OPERATIONS | 50,050 | 38,480 | 39,117 | |||||||||
| OTHER INCOME AND EXPENSES | ||||||||||||
| Interest expense | 40,623 | 43,455 | 41,684 | |||||||||
| Meaningful use incentive | (250 | ) | (2,808 | ) | (3,270 | ) | ||||||
| Equity in earnings of joint ventures | (13,554 | ) | (9,767 | ) | (8,927 | ) | ||||||
| Gain on sale of imaging centers and medical practice | (3,146 | ) | – | (5,434 | ) | |||||||
| Gain on return of common stock | – | (5,032 | ) | – | ||||||||
| Other (income) expenses | (8 | ) | 196 | 419 | ||||||||
| Total other expenses | 23,665 | 26,044 | 24,472 | |||||||||
| INCOME BEFORE INCOME TAXES | 26,385 | 12,436 | 14,645 | |||||||||
| Provision for income taxes | (24,310 | ) | (4,432 | ) | (6,007 | ) | ||||||
| NET INCOME | 2,075 | 8,004 | 8,638 | |||||||||
| Net income attributable to noncontrolling interests | 2,022 | 774 | 929 | |||||||||
| NET INCOME ATTRIBUTABLE TO RADNET, INC. COMMON STOCKHOLDERS | $ | 53 | $ | 7,230 | $ | 7,709 | ||||||
| BASIC NET INCOME PER SHARE ATTRIBUTABLE TO RADNET, INC. COMMON STOCKHOLDERS | $ | 0.00 | $ | 0.16 | $ | 0.18 | ||||||
| DILUTED NET INCOME PER SHARE ATTRIBUTABLE TO RADNET, INC. COMMON STOCKHOLDERS | $ | 0.00 | $ | 0.15 | $ | 0.17 | ||||||
| WEIGHTED AVERAGE SHARES OUTSTANDING | ||||||||||||
| Basic | 46,880,775 | 46,244,188 | 43,805,794 | |||||||||
| Diluted | 47,401,921 | 46,655,032 | 45,171,372 | |||||||||
The accompanying notes are an integral part of these financial statements.
| 59 |
RADNET, INC. AND SUBSIDIARIES
CONSOLIDATED STATEMENTS OF COMPREHENSIVE (LOSS) INCOME
(IN THOUSANDS)
| Years Ended December 31, | ||||||||||||
| 2017 | 2016 | 2015 | ||||||||||
| NET INCOME | $ | 2,075 | $ | 8,004 | $ | 8,638 | ||||||
| Foreign currency translation adjustments | 26 | (49 | ) | (41 | ) | |||||||
| Change in fair value of cash flow hedge, net of taxes | (880 | ) | 508 | – | ||||||||
| COMPREHENSIVE INCOME | 1,221 | 8,463 | 8,597 | |||||||||
| Less comprehensive income attributable to non-controlling interests | 2,022 | 774 | 929 | |||||||||
| COMPREHENSIVE (LOSS) INCOME ATTRIBUTABLE TO RADNET, INC. COMMON STOCKHOLDERS | $ | (801 | ) | $ | 7,689 | $ | 7,668 | |||||
The accompanying notes are an integral part of these financial statements.
| 60 |
RADNET, INC. AND SUBSIDIARIES
CONSOLIDATED STATEMENT OF EQUITY
(IN THOUSANDS EXCEPT SHARE DATA)
| Additional | Accumulated Other | Radnet, Inc. | ||||||||||||||||||||||||||||||
| Common Stock | Paid-in | Comprehensive | Accumulated | Stockholders' | Noncontrolling | Total | ||||||||||||||||||||||||||
| Shares | Amount | Capital | (Loss) Income | Deficit | Equity | Interests | Equity | |||||||||||||||||||||||||
| BALANCE - JANUARY 1, 2015 | 42,825,676 | $ | 4 | $ | 177,750 | $ | (112 | ) | $ | (172,280 | ) | $ | 5,362 | $ | 2,336 | $ | 7,698 | |||||||||||||||
| Issuance of common stock upon exercise of options/warrants | 835,098 | – | 594 | – | – | 594 | – | 594 | ||||||||||||||||||||||||
| Stock-based compensation | – | – | 7,635 | – | – | 7,635 | – | 7,635 | ||||||||||||||||||||||||
| Issuance of restricted stock and other awards | 1,014,423 | – | – | – | – | – | – | – | ||||||||||||||||||||||||
| Forfeiture of restricted stock | (59,053 | ) | – | – | – | – | – | – | – | |||||||||||||||||||||||
| Issuance of stock for acquisitions | 1,665,045 | – | 9,241 | – | – | 9,241 | – | 9,241 | ||||||||||||||||||||||||
| Sale to noncontrolling interests, net of taxes | – | – | 2,077 | – | – | 2,077 | 1,348 | 3,425 | ||||||||||||||||||||||||
| Distributions paid to noncontrolling interests | – | – | – | – | – | – | (729 | ) | (729 | ) | ||||||||||||||||||||||
| Change in cumulative foreign currency translation adjustment | – | – | – | (41 | ) | – | (41 | ) | – | (41 | ) | |||||||||||||||||||||
| Net income | – | – | – | – | 7,709 | 7,709 | 929 | 8,638 | ||||||||||||||||||||||||
| BALANCE - DECEMBER 31, 2015 | 46,281,189 | $ | 4 | $ | 197,297 | $ | (153 | ) | $ | (164,571 | ) | $ | 32,577 | $ | 3,884 | $ | 36,461 | |||||||||||||||
| Cumulative effect of accounting change due to adoption of ASU 2016-09 | – | – | – | – | 7,130 | 7,130 | – | 7,130 | ||||||||||||||||||||||||
| Issuance of common stock upon exercise of options/warrants | 314,448 | – | 150 | – | – | 150 | – | 150 | ||||||||||||||||||||||||
| Stock-based compensation | – | – | 5,767 | – | – | 5,767 | – | 5,767 | ||||||||||||||||||||||||
| Issuance of restricted stock and other awards | 937,803 | – | – | – | – | – | – | – | ||||||||||||||||||||||||
| Return of common stock | (958,536 | ) | – | (5,032 | ) | – | – | (5,032 | ) | – | (5,032 | ) | ||||||||||||||||||||
| Purchase of noncontrolling interests | – | – | (495 | ) | – | – | (495 | ) | (599 | ) | (1,094 | ) | ||||||||||||||||||||
| Sale to noncontrolling interests, net of taxes | – | – | 700 | – | – | 700 | – | 700 | ||||||||||||||||||||||||
| Distributions paid to noncontrolling interests | – | – | – | – | – | – | (492 | ) | (492 | ) | ||||||||||||||||||||||
| Change in cumulative foreign currency translation adjustment | – | – | – | (49 | ) | – | (49 | ) | – | (49 | ) | |||||||||||||||||||||
| Change in fair value cash flow hedge, net of taxes | – | – | – | 508 | – | 508 | – | 508 | ||||||||||||||||||||||||
| Net income | – | – | – | – | 7,230 | 7,230 | 774 | 8,004 | ||||||||||||||||||||||||
| BALANCE - DECEMBER 31, 2016 | 46,574,904 | $ | 4 | $ | 198,387 | $ | 306 | $ | (150,211 | ) | $ | 48,486 | $ | 3,567 | $ | 52,053 | ||||||||||||||||
| Stock-based compensation | 867,248 | 1 | 7,833 | – | – | 7,834 | – | 7,834 | ||||||||||||||||||||||||
| Issuance of stock for acquisitions | 281,763 | – | 2,500 | – | – | 2,500 | – | 2,500 | ||||||||||||||||||||||||
| Sale to noncontrolling interests, net of taxes | – | – | 3,541 | – | – | 3,541 | – | 3,541 | ||||||||||||||||||||||||
| Contributions from noncontrolling interests | – | – | – | – | – | – | 4,304 | 4,304 | ||||||||||||||||||||||||
| Distributions paid to noncontrolling interests | – | – | – | – | – | – | (1,528 | ) | (1,528 | ) | ||||||||||||||||||||||
| Change in cumulative foreign currency translation adjustment | – | – | – | 26 | – | 26 | – | 26 | ||||||||||||||||||||||||
| Change in fair value cash flow hedge, net of taxes | – | – | – | (880 | ) | – | (880 | ) | – | (880 | ) | |||||||||||||||||||||
| Net income | – | – | – | – | 53 | 53 | 2,022 | 2,075 | ||||||||||||||||||||||||
| BALANCE - DECEMBER 31, 2017 | 47,723,915 | $ | 5 | $ | 212,261 | $ | (548 | ) | $ | (150,158 | ) | $ | 61,560 | $ | 8,365 | $ | 69,925 | |||||||||||||||
The accompanying notes are an integral part of these financial statements.
| 61 |
RADNET, INC. AND SUBSIDIARIES
CONSOLIDATED STATEMENTS OF CASH FLOWS
(IN THOUSANDS)
| Years Ended December 31, | ||||||||||||
| 2017 | 2016 | 2015 | ||||||||||
| CASH FLOWS FROM OPERATING ACTIVITIES | ||||||||||||
| Net income | $ | 2,075 | $ | 8,004 | $ | 8,638 | ||||||
| Adjustments to reconcile net income to net cash provided by operating activities: | ||||||||||||
| Depreciation and amortization | 66,796 | 66,610 | 60,611 | |||||||||
| Provision for bad debts | 46,555 | 45,387 | 36,033 | |||||||||
| Gain on return from common stock | – | (5,032 | ) | – | ||||||||
| Equity in earnings of joint ventures | (13,554 | ) | (9,767 | ) | (8,927 | ) | ||||||
| Distributions from joint ventures | 8,690 | 2,926 | 7,731 | |||||||||
| Amortization and write off of deferred financing costs and loan discount | 3,483 | 5,045 | 5,369 | |||||||||
| Loss on sale and disposal of equipment | 1,142 | 767 | 866 | |||||||||
| Gain on sale of imaging centers | (3,146 | ) | – | (5,434 | ) | |||||||
| Stock-based compensation | 6,787 | 5,826 | 7,647 | |||||||||
| Non cash severance | 1,047 | – | – | |||||||||
| Changes in operating assets and liabilities, net of assets acquired and liabilities assumed in purchase transactions: | ||||||||||||
| Accounts receivable | (37,164 | ) | (47,055 | ) | (34,514 | ) | ||||||
| Other current assets | 1,461 | 11,038 | (14,198 | ) | ||||||||
| Other assets | (801 | ) | 1,267 | (3,813 | ) | |||||||
| Deferred taxes | 19,504 | 3,446 | 4,036 | |||||||||
| Deferred rent | 2,135 | (1,668 | ) | 7,011 | ||||||||
| Deferred revenue | 1,034 | (82 | ) | (366 | ) | |||||||
| Accounts payable, accrued expenses and other | 36,181 | 4,929 | (3,653 | ) | ||||||||
| Net cash provided by operating activities | 142,225 | 91,641 | 67,037 | |||||||||
| CASH FLOWS FROM INVESTING ACTIVITIES | ||||||||||||
| Purchase of imaging facilities | (27,612 | ) | (6,641 | ) | (90,792 | ) | ||||||
| Investment at cost | (500 | ) | ||||||||||
| Purchase of property and equipment | (61,336 | ) | (59,251 | ) | (42,964 | ) | ||||||
| Proceeds from sale of equipment | 852 | 481 | 1,282 | |||||||||
| Proceeds from sale of imaging and medical practice assets | 8,429 | – | 35,500 | |||||||||
| Proceeds from sale of internal use software | 492 | 301 | 443 | |||||||||
| Cash contribution from partner in JV formation | 1,473 | 994 | – | |||||||||
| Equity contributions in existing and purchase of interest in joint ventures | (1,118 | ) | (1,374 | ) | (265 | ) | ||||||
| Net cash used in investing activities | (79,320 | ) | (65,490 | ) | (96,796 | ) | ||||||
| CASH FLOWS FROM FINANCING ACTIVITIES | ||||||||||||
| Principal payments on notes and leases payable | (6,836 | ) | (11,880 | ) | (9,773 | ) | ||||||
| Proceeds from borrowings | 170,000 | 476,504 | 73,869 | |||||||||
| Payments on senior notes | (196,666 | ) | (469,086 | ) | (23,727 | ) | ||||||
| Payments on deferred financing costs and debt discount | (5,062 | ) | (945 | ) | – | |||||||
| Distributions paid to noncontrolling interests | (1,528 | ) | (492 | ) | (729 | ) | ||||||
| Proceeds from sale of noncontrolling interest, net of taxes | 7,720 | 992 | 5,005 | |||||||||
| Contributions from noncontrolling partners | 125 | – | – | |||||||||
| Proceeds from revolving credit facility | 200,800 | 435,900 | 248,400 | |||||||||
| Payments on revolving credit facility | (200,800 | ) | (435,900 | ) | (263,700 | ) | ||||||
| Purchase of non-controlling interests | – | (1,153 | ) | – | ||||||||
| Proceeds from issuance of common stock upon exercise of options | – | 150 | 594 | |||||||||
| Net cash (used in) provided by financing activities | (32,247 | ) | (5,910 | ) | 29,939 | |||||||
| EFFECT OF EXCHANGE RATE CHANGES ON CASH | 26 | (49 | ) | (41 | ) | |||||||
| NET INCREASE IN CASH AND CASH EQUIVALENTS | 30,684 | 20,192 | 139 | |||||||||
| CASH AND CASH EQUIVALENTS, beginning of period | 20,638 | 446 | 307 | |||||||||
| CASH AND CASH EQUIVALENTS, end of period | $ | 51,322 | $ | 20,638 | $ | 446 | ||||||
| SUPPLEMENTAL DISCLOSURE OF CASH FLOW INFORMATION | ||||||||||||
| Cash paid during the period for interest | $ | 34,197 | $ | 37,487 | $ | 36,028 | ||||||
| Cash paid during the period for income taxes | $ | 4,939 | $ | 2,798 | $ | 1,781 | ||||||
The accompanying notes are an integral part of these financial statements.
| 62 |
RADNET, INC. AND SUBSIDIARIES
CONSOLIDATED STATEMENTS OF CASH FLOWS (CONTINUED)
Supplemental Schedule of Non-Cash Investing and Financing Activities
We acquired equipment and certain leasehold improvements for approximately $18.5 million, $28.8 million, and $32.4 million during the years ended December 31, 2017, 2016 and 2015, respectively, that we had not paid for as of December 31, 2017, 2016 and 2015, respectively. The offsetting amount due was recorded in our consolidated balance sheets under “accounts payable, accrued expenses and other.”
We added capital lease debt of approximately $5.5 million, $1.3 million, and $7.8 million for the years ended December 31, 2017, 2016 and 2015 respectively, relating to radiology equipment.
We recorded an investment in joint venture of $3.0 million to ScriptSender, LLC representing our capital contribution to the venture. The offsetting amount was recorded on the due to affiliates account of ScriptSender, LLC. As of December 31, 2017, the balance remaining to be contributed is approximately $2.0 million. See Note 2, Investment in Joint Ventures section to the consolidated financial statements contain herein for further information.
We transferred approximately $2.5 million in net assets in April 2017 to our new joint venture, Santa Monica Imaging Group LLC. See Note 4, Facility Acquisitions and Dispositions, to the consolidated financial statements contain herein for further information.
We transferred approximately $4.6 million in net assets in July 2017 to a new majority owned subsidiary, Advanced Imaging at Timonium Crossing, LLC. See Note 4, Facility Acquisitions and Dispositions, to the consolidated financial statements contain herein for further information.
On August 7, 2017 we acquired Diagnostic Imaging Associates for $13.0 million in cash and $1.5 million in RadNet common stock. See Note 4, Facility Acquisitions and Dispositions, to the consolidated financial statements contain herein for further information.
On October 5, 2017 we completed our acquisition of all of the outstanding equity interests in RadSite, LLC, for $1.0 million in common stock and $856,000 in cash. See Note 4, Facility Acquisitions and Dispositions, to the consolidated financial statements contain herein for further information.
We recognized a non-cash gain on return of common stock of $5.0 million in June 2016. See Note 2, Gain On Return of Common Stock section.
We transferred $2.7 million in fixed assets in June 2016 to our new joint venture, Glendale Advanced Imaging, LLC; see Note 2, Investment in Joint Ventures section.
| 63 |
RADNET, INC. AND SUBSIDIARIES
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
NOTE 1 – NATURE OF BUSINESS
We are a leading national provider of freestanding, fixed-site outpatient diagnostic imaging services in the United States based on number of locations and annual imaging revenue. At December 31, 2017, we operated directly or indirectly through joint ventures with hospitals, 297 centers located in California, Delaware, Florida, Maryland, New Jersey, and New York. Our centers provide physicians with imaging capabilities to facilitate the diagnosis and treatment of diseases and disorders. Our services include magnetic resonance imaging (MRI), computed tomography (CT), positron emission tomography (PET), nuclear medicine, mammography, ultrasound, diagnostic radiology (X-ray), fluoroscopy and other related procedures. The vast majority of our centers offer multi-modality imaging services. Our multi-modality strategy diversifies revenue streams, reduces exposure to reimbursement changes and provides patients and referring physicians one location to serve the needs of multiple procedures. In addition to our imaging services, we have two other subsidiaries, eRAD, Inc and Imaging On Call LLC. eRAD, Inc., develops and sells computerized systems for the imaging industry. Imaging On Call LLC, provides teleradiology services for remote interpretation of images. The capabilities of both eRAD and Imaging On Call are designed to make the RadNet imaging center operations more efficient and cost effective. As such, our operations comprise a single segment for financial reporting purposes.
The consolidated financial statements include the accounts of Radnet Management, Inc. (or “Radnet Management”) and Beverly Radiology Medical Group III, a professional partnership (“BRMG”). BRMG is a partnership of ProNet Imaging Medical Group, Inc. and Beverly Radiology Medical Group, Inc. The consolidated financial statements also include Radnet Management I, Inc., Radnet Management II, Inc., Radiologix, Inc., Radnet Managed Imaging Services, Inc., Delaware Imaging Partners, Inc., New Jersey Imaging Partners, Inc. and Diagnostic Imaging Services, Inc. (“DIS”), all wholly owned subsidiaries of Radnet Management. All of these affiliated entities are referred to collectively as “RadNet”, “we”, “us”, “our” or the “Company” in this report.
Accounting Standards Codification (“ASC”) 810-10-15-14, Consolidation, stipulates that generally any entity with a) insufficient equity to finance its activities without additional subordinated financial support provided by any parties, or b) equity holders that, as a group, lack the characteristics specified in the ASC which evidence a controlling financial interest, is considered a Variable Interest Entity (“VIE”). We consolidate all VIEs in which we are the primary beneficiary. We determine whether we are the primary beneficiary of a VIE through a qualitative analysis that identifies which variable interest holder has the controlling financial interest in the VIE. The variable interest holder who has both of the following has the controlling financial interest and is the primary beneficiary: (1) the power to direct the activities of the VIE that most significantly impact the VIE’s economic performance and (2) the obligation to absorb losses of, or the right to receive benefits from, the VIE that could potentially be significant to the VIE. In performing our analysis, we consider all relevant facts and circumstances, including: the design and activities of the VIE, the terms of the contracts the VIE has entered into, the nature of the VIE’s variable interests issued and how they were negotiated with or marketed to potential investors, and which parties participated significantly in the design or redesign of the entity.
Howard G. Berger, M.D., is our President and Chief Executive Officer, a member of our Board of Directors, and also owns, indirectly, 99% of the equity interests in BRMG. BRMG is responsible for all of the professional medical services at nearly all of our facilities located in California under a management agreement with us, and employs physicians or contracts with various other independent physicians and physician groups to provide the professional medical services at most of our California facilities. We generally obtain professional medical services from BRMG in California, rather than provide such services directly or through subsidiaries, in order to comply with California’s prohibition against the corporate practice of medicine. However, as a result of our close relationship with Dr. Berger and BRMG, we believe that we are able to better ensure that medical service is provided at our California facilities in a manner consistent with our needs and expectations and those of our referring physicians, patients and payors than if we obtained these services from unaffiliated physician groups.
We contract with nine medical groups which provide professional medical services at all of our facilities in Manhattan and Brooklyn, New York. These contracts are similar to our contract with BRMG. Seven of these groups are owned by John V. Crues, III, M.D., RadNet’s Medical Director, a member of our Board of Directors, and a 1% owner of BRMG. Dr. Berger owns a controlling interest in two of these medical groups which provide professional medical services at one of our Manhattan facilities.
RadNet provides non-medical, technical and administrative services to BRMG and the nine medical groups mentioned above (“NY Groups”) for which it receives a management fee, pursuant to the related management agreements. Through the management agreements we have exclusive authority over all non-medical decision making related to the ongoing business operations of BRMG and the NY Groups and we determine the annual budget of BRMG and the NY Groups. BRMG and the NY Groups both have insignificant operating assets and liabilities, and de minimis equity. Through management agreements with us, substantially all cash flows of BRMG and the NY Groups after expenses including professional salaries are transferred to us.
| 64 |
We have determined that BRMG and the NY Groups are variable interest entities, that we are the primary beneficiary, and consequently, we consolidate the revenue and expenses, assets and liabilities of each. BRMG and the NY Groups on a combined basis recognized $134.6 million, $135.7 million, and $113.1 million of revenue, net of management services fees to RadNet, for the years ended December 31, 2017, 2016, and 2015, respectively and $134.6 million, $135.7 million, and $113.1 million of operating expenses for the years ended December 31, 2017, 2016, and 2015, respectively. RadNet, Inc. recognized $435.5 million, $430.4 million, and $343.9 million of total billed net service fee revenue for the years ended December 31, 2017, 2016 and 2015, respectively, for management services provided to BRMG and the NY Groups relating primarily to the technical portion of billed revenue.
The cash flows of BRMG and the NY Groups are included in the accompanying consolidated statements of cash flows. All intercompany balances and transactions have been eliminated in consolidation. In our consolidated balance sheets at December 31, 2017 and December 31, 2016, we have included approximately $96.3 million and $100.0 million, respectively, of accounts receivable and approximately $7.4 million and $9.0 million of accounts payable and accrued liabilities related to BRMG and the NY Groups, respectively.
The creditors of BRMG and the NY Groups do not have recourse to our general credit and there are no other arrangements that could expose us to losses on behalf of BRMG and the NY Groups. However, RadNet may be required to provide financial support to cover any operating expenses in excess of operating revenues.
At all of our centers we have entered into long-term contracts with radiology groups in the area to provide physician services at those facilities. These radiology practices provide professional services, including supervision and interpretation of diagnostic imaging procedures, in our diagnostic imaging centers. The radiology practices maintain full control over the provision of professional services. In these facilities we enter into long-term agreements with radiology practice groups (typically 40 years). Under these arrangements, in addition to obtaining technical fees for the use of our diagnostic imaging equipment and the provision of technical services, we provide management services and receive a fee based on the value of the services we provide. Except in New York City, the fee is based on the practice group’s professional revenue, including revenue derived outside of our diagnostic imaging centers. In New York City we are paid a fixed fee set in advance for our services. We own the diagnostic imaging equipment and, therefore, receive 100% of the technical reimbursements associated with imaging procedures. The radiology practice groups retain the professional reimbursements associated with imaging procedures after deducting management service fees paid to us and we have no financial controlling interest in the radiology practices.
NOTE 2 - SUMMARY OF SIGNIFICANT ACCOUNTING POLICIES
PRINCIPLES OF CONSOLIDATION – The operating activities of subsidiaries are included in the accompanying consolidated financial statements (“financial statements”) from the date of acquisition. Investments in companies in which we have the ability to exercise significant influence, but not control, are accounted for by the equity method. All intercompany transactions and balances, with our consolidated entities and the unsettled amount of intercompany transactions with our equity method investees, have been eliminated in consolidation. As stated in Note 1 above, the BRMG and NY Groups are variable interest entities and we consolidate the operating activities and balance sheets of each. Additionally, we determined that our unconsolidated joint venture, ScriptSender, LLC, is also a VIE as it is dependent on our operational funding but we are not a primary beneficiary since RadNet does not have the power to direct the activities of the entity that most significantly impact the entity’s economic performance. See Investment in Joint Ventures section of Note 2 for further explanation.
USE OF ESTIMATES - The financial statements were prepared in accordance with U.S. generally accepted accounting principles (GAAP), which requires management to make estimates and assumptions that affect the amounts reported in the financial statements and accompanying notes. These estimates and assumptions affect various matters, including our reported amounts of assets and liabilities in our consolidated balance sheets at the dates of the financial statements; our disclosure of contingent assets and liabilities at the dates of the financial statements; and our reported amounts of revenues and expenses in our consolidated statements of operations during the reporting periods. These estimates involve judgments with respect to numerous factors that are difficult to predict and are beyond management’s control. As a result, actual amounts could materially differ from these estimates.
RECLASSIFICATION – We have reclassified certain amounts within accrued expenses for 2016 to conform to our 2017 presentation.
REVENUES – Service fee revenue, net of contractual allowances and discounts, consists of net patient fees received from various payors and patients themselves based mainly upon established contractual billing rates, less allowances for contractual adjustments and discounts. As it relates to BRMG and the NY Groups centers, this service fee revenue includes payments for both the professional medical interpretation revenue recognized by BRMG and the NY Groups as well as the payment for all other aspects related to our providing the imaging services, for which we earn management fees from BRMG and the NY Groups. As it relates to non-BRMG and NY Groups centers, namely the affiliated physician groups, this service fee revenue is earned through providing the use of our diagnostic imaging equipment and the provision of technical services as well as providing administration services such as clerical and administrative personnel, bookkeeping and accounting services, billing and collection, provision of medical and office supplies, secretarial, reception and transcription services, maintenance of medical records, and advertising, marketing and promotional activities.
| 65 |
Service fee revenues are recorded during the period the services are provided based upon the estimated amounts due from the patients and third-party payors. Third-party payors include federal and state agencies (under the Medicare and Medicaid programs), managed care health plans, commercial insurance companies and employers. Estimates of contractual allowances are based on historical collection rates of payor reimbursement contract agreements. We also record a provision for doubtful accounts based primarily on historical collection rates related to patient copayments and deductible amounts for patients who have health care coverage under one of our third-party payors.
Under capitation arrangements with various health plans, we earn a per-enrollee amount each month for making available diagnostic imaging services to all plan enrollees under the capitation arrangement. Revenue under capitation arrangements is recognized in the period in which we are obligated to provide services to plan enrollees under contracts with various health plans.
Our service fee revenue, net of contractual allowances and discounts, the provision for bad debts, and revenue under capitation arrangements for the years ended December 31, are summarized in the following table (in thousands) :
| Years Ended December 31, | ||||||||||||
| 2017 | 2016 | 2015 | ||||||||||
| Commercial insurance | $ | 571,369 | $ | 539,793 | $ | 486,489 | ||||||
| Medicare | 193,166 | 187,941 | 168,545 | |||||||||
| Medicaid | 25,821 | 28,170 | 23,948 | |||||||||
| Workers' compensation/personal injury | 35,195 | 36,548 | 32,728 | |||||||||
| Other (1) | 31,627 | 29,135 | 35,046 | |||||||||
| Service fee revenue, net of contractual allowances and discounts | 857,178 | 821,587 | 746,756 | |||||||||
| Provision for bad debts | (46,555 | ) | (45,387 | ) | (36,033 | ) | ||||||
| Net service fee revenue | 810,623 | 776,200 | 710,723 | |||||||||
| Revenue under capitation arrangements | 111,563 | 108,335 | 98,905 | |||||||||
| Total net revenue | $ | 922,186 | $ | 884,535 | $ | 809,628 | ||||||
(1) Other consists of revenue from teleradiology services, consulting fees and software revenue
PROVISION FOR BAD DEBTS – We provide for an allowance against accounts receivable that could become uncollectible to reduce the carrying value of such receivables to their estimated net realizable value. We estimate this allowance based on the aging of our accounts receivable by the historical payment patterns of each type of payor, write-off trends, and other relevant factors. A significant portion of our provision for bad debt relates to co-payments and deductibles owed to us from patients with insurance. Although we attempt to collect deductibles and co-payments due from patients with insurance at the time of service, this attempt to collect at the time of service is not an assessment of the patient’s ability to pay nor are revenues recognized based on an assessment of the patient’s ability to pay. There are various factors that can impact collection trends, such as changes in the economy, which in turn have an impact on the increased burden of co-payments and deductibles to be made by patients with insurance. These factors continuously change and can have an impact on collection trends and our estimation process. Our allowance for bad debts at December 31, 2017 and 2016 was $34.6 million and $20.7 million, respectively.
ACCOUNTS RECEIVABLE – Substantially all of our accounts receivable are due under fee-for-service contracts from third party payors, such as insurance companies and government-sponsored healthcare programs, or directly from patients. We continuously monitor collections from our payors and maintain an allowance for bad debts based upon specific payor collection issues that we have identified and our historical experience.
MEANINGFUL USE INCENTIVE – Under the American Recovery and Reinvestment Act of 2009, a program was enacted that provides financial incentives for providers that successfully implement and utilize electronic health record technology to improve patient care. Our software development team in Canada developed a Radiology Information System (RIS) software platform that has been awarded meaningful use certification. As this certified RIS system is implemented throughout our imaging centers, the radiologists that utilize this software can be eligible for the available financial incentives. In order to receive such incentive payments, providers must attest that they have demonstrated meaningful use of the certified RIS in each stage of the program. We account for this meaningful use incentive under the Gain Contingency Model outlined in ASC 450-30, and record the meaningful use incentive within non-operating income only after Medicare accepts an attestation from the qualified eligible professional demonstrating meaningful use. We recorded approximately $250,000, $2.8 million and $3.3 million during the twelve months ended December 31, 2017, 2016 and 2015, respectively, relating to this incentive.
| 66 |
GAIN ON RETURN OF COMMON STOCK – In the second quarter of 2016, we determined that certain pre-acquisition financial information of Diagnostic Imaging Group (“DIG”) provided to us by the sellers contained errors. As a result of this, we negotiated and reached a settlement with the sellers of DIG in June 2016 for the return of 958,536 shares of common stock which had a fair value of $5.0 million on the date of return. Such return has been recognized as a gain on return of common stock in our statement of operations.
SOFTWARE REVENUE RECOGNITION – Our subsidiary, eRAD, Inc., sells Picture Archiving Communications Systems (“PACS”) and related services, primarily in the United States. The PACS systems sold by eRAD are primarily composed of certain elements: hardware, software, installation and training, and support. Sales are made primarily through eRAD’s sales force. These sales are multiple-element arrangements that generally include hardware, software, software installation, configuration, system installation, training and first-year warranty support. Hardware, which is not unique or special purpose, is purchased from a third-party and resold to eRAD’s customers with a small mark-up.
We have determined that our core software products, such as PACS, are essential to most of our arrangements as hardware, software and related services are sold as an integrated package. Therefore, these transactions are accounted for under ASC 605-25, Multiple-Element Arrangements (as modified by ASU 2009-13). Non-essential software and related services, and essential software sold on a stand-alone basis without hardware, would continue to be accounted for under ASC 985-605, Software.
For the years ended December 31, 2017, 2016 and 2015, we recorded approximately $6.1 million, $6.2 million and $6.1 million, respectively, in revenue related to our eRAD business which is included in net service fee revenue in our consolidated statement of operations. At December 31, 2017 we had a deferred revenue liability of approximately $2.5 million associated with eRAD sales which we expect to recognize into revenue over the next 12 months.
SOFTWARE DEVELOPMENT COSTS – Costs related to the research and development of new software products and enhancements to existing software products all for resale to our customers are expensed as incurred.
We utilize a variety of computerized information systems in the day to day operation of our diagnostic imaging facilities. One such system is our front desk patient tracking system or Radiology Information System (“RIS”). We have historically utilized third party RIS software solutions and pay monthly fees to outside third party software vendors for the use of this software. We have developed our own RIS solution through our wholly owned subsidiary, Radnet Management Information Systems (“RMIS”) and began utilizing this system beginning in the first quarter of 2015.
In accordance with ASC 350-40, Accounting for the Costs of Computer Software Developed for Internal Use, the costs incurred by RMIS toward the development of our RIS system, which began in August, 2010 and continued until December 2014, were capitalized and are being amortized over its useful life which we determined to be 5 years. Total costs capitalized were approximately $6.4 million. We began recording amortization of $107,000 per month for our use of this software in January 2015.
We have entered into multiple agreements to license our RIS system to outside customers. For the twelve months December 31, 2017 and December 31, 2016, we received approximately $492,000 and $301,000 with respect to this licensing agreement, respectively. In accordance with ASC 350-40, we recorded the receipt of these funds against the capitalized software costs explained above. As of December 31, 2017, the net carrying value of our capitalized software costs was approximately $1.3 million.
CONCENTRATION OF CREDIT RISKS – Financial instruments that potentially subject us to credit risk are primarily cash equivalents and accounts receivable. We have placed our cash and cash equivalents with one major financial institution. At times, the cash in the financial institution is temporarily in excess of the amount insured by the Federal Deposit Insurance Corporation, or FDIC. Substantially all of our accounts receivable are due under fee-for-service contracts from third party payors, such as insurance companies and government-sponsored healthcare programs, or directly from patients. We continuously monitor collections and maintain an allowance for bad debts based upon our historical collection experience.
CASH AND CASH EQUIVALENTS – We consider all highly liquid investments that mature in three months or less when purchased to be cash equivalents. The carrying amount of cash and cash equivalents approximates their fair market value.
DEFERRED FINANCING COSTS – Costs of financing are deferred and amortized on a straight-line basis over the life of the associated loan, which approximates the effective interest rate method. Deferred financing costs, net of accumulated amortization, were $1.9 million for the twelve month period ended December 31, 2017, and $2.0 million for the twelve month period ended December 31, 2016. Deferred financing costs are solely related to our Revolving Credit Facility. In conjunction with our Fourth Amendment and Fifth Amendment to our First Lien Credit Agreement, a net addition of approximately $371,000 was added to deferred financing costs for the twelve months ended December 31, 2017. See Note 8, Revolving Credit Facility, Notes Payable, and Capital Leases for more information.
| 67 |
INVENTORIES – Inventories, consisting mainly of medical supplies, are stated at the lower of cost or net realizable value with cost determined by the first-in, first-out method.
PROPERTY AND EQUIPMENT – Property and equipment are stated at cost, less accumulated depreciation and amortization. Depreciation and amortization of property and equipment are provided using the straight-line method over the estimated useful lives, which range from 3 to 15 years. Leasehold improvements are amortized at the lesser of lease term or their estimated useful lives, which range from 3 to 30 years. Maintenance and repairs are charged to expense as incurred.
BUSINESS COMBINATION – Accounting for acquisitions requires us to recognize separately from goodwill the assets acquired and the liabilities assumed at their acquisition date fair values. Goodwill as of the acquisition date is measured as the excess of consideration transferred over the net of the acquisition date fair values of the assets acquired and the liabilities assumed. While we use our best estimates and assumptions to accurately value assets acquired and liabilities assumed at the acquisition date, our estimates are inherently uncertain and subject to refinement. As a result, during the measurement period, which may be up to one year from the acquisition date, we record adjustments to the assets acquired and liabilities assumed with the corresponding offset to goodwill. Upon the conclusion of the measurement period or final determination of the values of assets acquired or liabilities assumed, whichever comes first, any subsequent adjustments are recorded to our consolidated statements of operations.
GOODWILL AND INDEFINITE LIVED INTANGIBLES – Goodwill at December 31, 2017 totaled $256.8 million and $239.6 million at December 31, 2016. Indefinite lived intangible assets at December 31, 2017 and 2016 totaled $7.9 million and are associated with the value of certain trade name intangibles. Goodwill and trade name intangibles are recorded as a result of business combinations. Management evaluates goodwill and trade name intangibles, at a minimum, on an annual basis and whenever events and changes in circumstances suggest that the carrying amount may not be recoverable. Impairment of goodwill is tested at the reporting unit level by comparing the reporting unit’s carrying amount, including goodwill, to the fair value of the reporting unit. The fair value of a reporting unit is estimated using a combination of the income or discounted cash flows approach and the market approach, which uses comparable market data. If the carrying amount of the reporting unit exceeds its fair value, goodwill is considered impaired and a second step is performed to measure the amount of impairment loss, if any. Impairment of trade name intangibles is tested at the subsidiary level by comparing the subsidiary’s trade name carrying amount to its respective fair value. We tested both goodwill and trade name intangibles for impairment on October 1, 2017, noting no impairment, and have not identified any indicators of impairment through December 31, 2017.
LONG-LIVED ASSETS – We evaluate our long-lived assets (property and equipment) and intangibles, other than goodwill, for impairment when events or changes indicate the carrying amount of an asset may not be recoverable. U.S. GAAP requires that if the sum of the undiscounted expected future cash flows from a long-lived asset or definite-lived intangible is less than the carrying value of that asset, an asset impairment charge must be recognized. The amount of the impairment charge is calculated as the excess of the asset’s carrying value over its fair value, which generally represents the discounted future cash flows from that asset or in the case of assets we expect to sell, at fair value less costs to sell. We determined that there were no events or changes in circumstances that indicated our long-lived assets were impaired during any periods presented.
INCOME TAXES – Income tax expense is computed using an asset and liability method and using expected annual effective tax rates. Under this method, deferred income tax assets and liabilities result from temporary differences in the financial reporting bases and the income tax reporting bases of assets and liabilities. The measurement of deferred tax assets is reduced, if necessary, by the amount of any tax benefit that, based on available evidence, is not expected to be realized. When it appears more likely than not that deferred taxes will not be realized, a valuation allowance is recorded to reduce the deferred tax asset to its estimated realizable value. For net deferred tax assets we consider estimates of future taxable income in determining whether our net deferred tax assets are more likely than not to be realized. Income taxes are further explained in Note 10.
UNINSURED RISKS – On November 1, 2008 we obtained a fully funded and insured workers’ compensation policy, thereby eliminating any uninsured risks for employee injuries occurring on or after that date. This fully funded policy remained in effect through November 1, 2013 and continues to cover any claims incurred through this date.
On November 1, 2013 we entered into a high-deductible workers’ compensation insurance policy. We have recorded liabilities of $2.8 million for the year ending December 31, 2017 and $2.9 million for the year ended December 31, 2016, respectively, for the estimated future cash obligations associated with the unpaid portion of the workers compensation claims incurred.
| 68 |
We and our affiliated physicians carry an annual medical malpractice insurance policy that protects us for claims that are filed during the policy year and that fall within policy limits. The policy has a deductible for which is $10,000 per incidence at for the years ending December 31, 2017 and December 31, 2016, respectively.
In December 2008, in order to eliminate the exposure for claims not reported during the regular malpractice policy period, we purchased a medical malpractice tail policy, which provides coverage for any claims reported in the event that our medical malpractice policy expires. As of December 31, 2017, this policy remains in effect.
We have entered into an arrangement with Blue Shield to administer and process claims under a self-insured plan that provides health insurance coverage for our employees and dependents. We have recorded liabilities as of December 31, 2017 and 2016 of $4.5 million and $2.4 million, respectively, for the estimated future cash obligations associated with the unpaid portion of the medical and dental claims incurred by our participants. Additionally, we entered into an agreement with Blue Shield for a stop loss policy that provides coverage for any claims that exceed $250,000 up to a maximum of $1.0 million in order for us to limit our exposure for unusual or catastrophic claims.
LOSS AND OTHER UNFAVORABLE CONTRACTS – We assess the profitability of our contracts to provide management services to our contracted physician groups and identify those contracts where current operating results or forecasts indicate probable future losses. Anticipated future revenue is compared to anticipated costs. If the anticipated future cost exceeds the revenue, a loss contract accrual is recorded. In connection with the acquisition of Radiologix in November 2006, we acquired certain management service agreements for which forecasted costs exceeds forecasted revenue. As such, an $8.9 million loss contract accrual was established in purchase accounting, and is included in other non-current liabilities. The recorded loss contract accrual is being accreted into operations over the remaining term of the acquired management service agreements, which ends in 2031. As of December 31, 2017 and 2016, the remaining accrual balance is $5.0 million, and $5.6 million, respectively.
In addition and related to acquisition activity, we have certain operating lease commitments for facilities where the fair market rent differs from the lease contract rate. We have recorded an unfavorable contract liability representing the difference between the total value of the fair market rent and the contract rent over the current term of the lease applicable from the date of acquisition. As of December 31, 2017 and 2016, the unfavorable contract liability on these leases is $1.4 million and $1.6 million, respectively.
EQUITY BASED COMPENSATION – We have one long-term incentive plan that we adopted in 2006 and which we first amended and restated as of April 20, 2015, and again on March 9, 2017 (the “Restated Plan”). The Restated Plan was approved by our stockholders at our annual stockholders meeting on June 8, 2017. We have reserved for issuance under the Restated Plan 14,000,000 shares of common stock. We can issue options, stock awards, stock appreciation rights, stock units and cash awards under the Restated Plan. Certain options granted under the Restated Plan to employees are intended to qualify as incentive stock options under existing tax regulations. Stock options and warrants generally vest over three to five years and expire five to ten years from date of grant. The compensation expense recognized for all equity-based awards is recognized over the awards’ service periods. Equity-based compensation is classified in operating expenses within the same line item as the majority of the cash compensation paid to employees. See Note 11 Stock-Based Compensation for more information.
FOREIGN CURRENCY TRANSLATION – The functional currency of our foreign subsidiaries is the local currency. In accordance with ASC 830, Foreign Currency Matters, assets and liabilities denominated in foreign currencies are translated using the exchange rate at the balance sheet dates. Revenues and expenses are translated using average exchange rates prevailing during the reporting period. Any translation adjustments resulting from this process are shown separately as a component of accumulated other comprehensive (loss) income. Foreign currency transaction gains and losses are included in the determination of net income.
COMPREHENSIVE (LOSS) INCOME – ASC 220, Comprehensive Income, establishes rules for reporting and displaying comprehensive (loss) income and its components. Our unrealized gains or losses on foreign currency translation adjustments are included in comprehensive (loss) income. In December, 2016, we entered into an interest rate cap agreement, as discussed in Note 2, Derivative Instruments. Assuming perfect effectiveness, any unrealized gains or losses related to the cap agreement that qualify for cash flow hedge accounting are classified as a component of income. Any ineffectiveness is recognized in earnings. The components of comprehensive (loss) income for the three years in the period ended December 31, 2017 are included in the consolidated statements of comprehensive (loss) income.
DERIVATIVE INSTRUMENTS – In the fourth quarter of 2016, we entered into two forward interest rate cap agreements ("2016 Caps"). The 2016 Caps will mature in September and October 2020. The 2016 Caps had notional amounts of $150,000,000 and $350,000,000, respectively, which were designated at inception as cash flow hedges of future cash interest payments associated with portions of our variable rate bank debt. Under these arrangements, we purchased a cap on 3 month LIBOR at 2.0%. We are liable for a $5.3 million premium to enter into the caps which is being accrued over the life of the 2016 Caps.
ADOPTION of ASU 2017-12 – Targeted Improvements to Accounting for Hedging Activities - In August 2017, the FASB issued ASU 2017-12, Targeted Improvements to Accounting for Hedging Activities, (Topic 815). ASU 2017-12 is intended to improve the financial reporting of hedging relationships to better portray the economic results of an entity's risk management activities in its financial statements. These amendments also make targeted improvements to simplify the application of the hedge accounting guidance in current GAAP. The amendments are effective beginning on January 1, 2019, although early adoption is permitted. Upon adoption, entities are required to apply the amendments in this update to hedging relationships existing on the date of adoption, reflected as of the beginning of the fiscal year. We elected to early adopt the new guidance and the adoption had no effect on our financial statements, as our 2016 Caps were continuously effective since their inception in the fourth quarter of 2016.
| 69 |
At inception, we designated our 2016 Caps as cash flow hedges of floating-rate borrowings. In accordance with ASC Topic 815, derivatives that have been designated and qualify as cash flow hedging instruments are reported at fair value. The gain or loss of the hedge (i.e., change in fair value) is reported as a component of accumulated other comprehensive (loss) income in the consolidated statement of equity.
Below represents the fair value of our 2016 Caps and loss (gain) recognized:
| For the twelve months ended December 31, 2017 | ||||||
| Derivatives | Balance Sheet Location | Fair Value – Liabilities | ||||
| Interest rate contracts | Current and other non-current liabilities | $ | (595 | ) | ||
| For the twelve months ended December 31, 2016 | ||||||
| Derivatives | Balance Sheet Location | Fair Value – Asset Derivatives | ||||
| Interest rate contracts | Current assets | $ | 818 | |||
A tabular presentation of the effect of derivative instruments on our consolidated statement of comprehensive (loss) income, net of taxes is as follows (amounts in thousands):
| For the twelve months ended December 31, 2017 | ||
| Effective Interest Rate Cap | Amount of Loss Recognized on Derivative | Location of Loss Recognized
in Income on Derivative |
| Interest rate contracts | ($880) | Other Comprehensive Loss |
| For the twelve months ended December 31, 2016 | ||
| Effective Interest Rate Cap | Amount of Gain Recognized on Derivative | Location of Gain Recognized in Income on Derivative |
| Interest rate contracts | $508 | Other Comprehensive Income |
FAIR VALUE MEASUREMENTS – Assets and liabilities subject to fair value measurements are required to be disclosed within a fair value hierarchy. The fair value hierarchy ranks the quality and reliability of inputs used to determine fair value. Accordingly, assets and liabilities carried at, or permitted to be carried at, fair value are classified within the fair value hierarchy in one of the following categories based on the lowest level input that is significant to a fair value measurement:
Level 1—Fair value is determined by using unadjusted quoted prices that are available in active markets for identical assets and liabilities.
Level 2—Fair value is determined by using inputs other than Level 1 quoted prices that are directly or indirectly observable. Inputs can include quoted prices for similar assets and liabilities in active markets or quoted prices for identical assets and liabilities in inactive markets. Related inputs can also include those used in valuation or other pricing models such as interest rates and yield curves that can be corroborated by observable market data.
Level 3—Fair value is determined by using inputs that are unobservable and not corroborated by market data. Use of these inputs involves significant and subjective judgment.
The table below summarizes the estimated fair values of certain of our financial assets that are subject to fair value measurements, and the classification of these assets in our consolidated balance sheets, as follows (in thousands):
| As of December 31, 2017 | ||||||||||||||||
| Level 1 | Level 2 | Level 3 | Total | |||||||||||||
| Current and other non-current liabilities | ||||||||||||||||
| Interest Rate Contracts | $ | – | $ | (595 | ) | $ | – | $ | (595 | ) | ||||||
| As of December 31, 2016 | ||||||||||||||||
| Level 1 | Level 2 | Level 3 | Total | |||||||||||||
| Current assets | ||||||||||||||||
| Interest Rate Contracts | $ | – | $ | 818 | $ | – | $ | 818 | ||||||||
| 70 |
The estimated fair value of these contracts was determined using Level 2 inputs. More specifically, the fair value was determined by calculating the value of the difference between the fixed interest rate of the interest rate swaps and the counterparty’s forward LIBOR curve. The forward LIBOR curve is readily available in the public markets or can be derived from information available in the public markets.
The table below summarizes the estimated fair value and carrying amount of our long-term debt as follows (in thousands):
| As of December 31, 2017 | ||||||||||||||||||||
| Level 1 | Level 2 | Level 3 | Total Fair Value | Total Face Value | ||||||||||||||||
| First Lien Term Loans | $ | – | $ | 628,801 | $ | – | $ | 628,801 | $ | 620,272 | ||||||||||
| As of December 31, 2016 | ||||||||||||||||||||
| Level 1 | Level 2 | Level 3 | Total | Total Face Value | ||||||||||||||||
| First Lien Term Loans | $ | – | $ | 483,129 | $ | – | $ | 483,129 | $ | 478,938 | ||||||||||
| Second Lien Term Loans | $ | – | $ | 167,580 | $ | – | $ | 167,580 | $ | 168,000 | ||||||||||
Our revolving credit facility had no aggregate principal amount outstanding as of December 31, 2017.
The estimated fair value of our long-term debt, which is discussed in Note 8, was determined using Level 2 inputs primarily related to comparable market prices.
We consider the carrying amounts of cash and cash equivalents, receivables, other current assets, current liabilities and other notes payables to approximate their fair value because of the relatively short period of time between the origination of these instruments and their expected realization or payment. Additionally, we consider the carrying amount of our capital lease obligations to approximate their fair value because the weighted average interest rate used to formulate the carrying amounts approximates current market rates.
EARNINGS PER SHARE - Earnings per share is based upon the weighted average number of shares of common stock and common stock equivalents outstanding, net of common stock held in treasury, as follows (in thousands except share and per share data):
| Years Ended December 31, | ||||||||||||
| 2017 | 2016 | 2015 | ||||||||||
| Net income attributable to RadNet, Inc. common stockholders | $ | 53 | $ | 7,230 | $ | 7,709 | ||||||
| BASIC NET INCOME PER SHARE ATTRIBUTABLE TO RADNET, INC. COMMON STOCKHOLDERS | ||||||||||||
| Weighted average number of common shares outstanding during the period | 46,880,775 | 46,244,188 | 43,805,794 | |||||||||
| Basic net income per share attributable to RadNet, Inc. common stockholders | $ | 0.00 | $ | 0.16 | $ | 0.18 | ||||||
| DILUTED NET INCOME PER SHARE ATTRIBUTABLE TO RADNET, INC. COMMON STOCKHOLDERS | ||||||||||||
| Weighted average number of common shares outstanding during the period | 46,880,775 | 46,244,188 | 43,805,794 | |||||||||
| Add nonvested restricted stock subject only to service vesting | 274,940 | 220,416 | 865,326 | |||||||||
| Add additional shares issuable upon exercise of stock options and warrants | 246,206 | 190,428 | 500,252 | |||||||||
| Weighted average number of common shares used in calculating diluted net income per share | 47,401,921 | 46,655,032 | 45,171,372 | |||||||||
| Diluted net income per share attributable to RadNet, Inc. common stockholders | $ | 0.00 | $ | 0.15 | $ | 0.17 | ||||||
| Stock options excluded from the computation of diluted per share amounts: | ||||||||||||
| Weighted average shares for which the exercise price exceeds average market price of common stock | 175,037 | 245,313 | 260,000 | |||||||||
| 71 |
INVESTMENT AT COST – On March 24, 2017, we acquired a 12.5% equity interest in Medic Vision – Imaging Solutions Ltd. for $1.0 million. We also have an option to acquire an additional 12.5% equity interest for $1.4 million exercisable within one year from the initial share purchase date. Medic Vision, based in Israel, specializes in software packages that provide compliant radiation dose structured reporting and enhanced images from reduced dose CT scans. In accordance with ASC 325-20, Cost Method Investments, the investment is recorded at its cost of $1.0 million. No impairment in our investment was noted as of the year ended December 31, 2017. As such, we do not estimate the fair value as no identified events or changes in circumstances occurred that would have a significant adverse effect on the value of the investment.
INVESTMENT IN JOINT VENTURES – We have fourteen unconsolidated joint ventures with ownership interests ranging from 35% to 55%. These joint ventures represent partnerships with hospitals, health systems or radiology practices and were formed for the purpose of owning and operating diagnostic imaging centers. Professional services at the joint venture diagnostic imaging centers are performed by contracted radiology practices or a radiology practice that participates in the joint venture. Our investment in these joint ventures is accounted for under the equity method, since RadNet does not have a controlling financial interest in such ventures. We evaluate our investment in joint ventures, including cost in excess of book value (equity method goodwill) for impairment whenever indicators of impairment exist. No indicators of impairment existed as of December 31, 2017.
Acquisition of new facilities
On August 15, 2016 our joint venture, Franklin Imaging, LLC, acquired a single multi-modality imaging center located in Rosedale, Maryland for cash consideration of $1.0 million and the assumption of capital lease debt of $241,000. Franklin Imaging, LLC made a fair value determination of the acquired assets and approximately $600,000 of fixed assets, $30,000 of other assets and goodwill of $648,000 was recorded in respect to the transaction.
Formation of new joint ventures
On April 1, 2017, we formed in conjuncture with Cedars Sinai Medical Center (“CSMC”) the Santa Monica Imaging Group, LLC (“SMIG”), consisting of two multi-modality imaging centers located in Santa Monica, CA. Total agreed contribution was $2.7 million of cash and assets with RadNet contributing $1.1 million for a 40% economic interest and CSMC contributing $1.6 million for a 60% economic interest. For its contribution, RadNet transferred $80,000 in cash and the net assets acquired in the acquisition of Resolution Imaging of $2.5 million. CSMC contributed $120,000 in cash and paid RadNet $1.5 million for the Resolution Imaging assets transferred to the venture. RadNet does not have controlling economic interest in SMIG and the investment is accounted for under the equity method.
On January 6, 2017, Image Medical Inc. (“Image Medical”), a wholly owned subsidiary of RadNet, acquired a 49% economic interest ScriptSender, LLC, a partnership held by two individuals which provides secure data transmission services of medical information. Through a management agreement, RadNet provides management and accounting services and receives an agreed upon fee. Image Medical will contribute $3.0 million to the partnership for its 49% ownership stake over a three year period representing the maximum risk in the venture. ScriptSender LLC is dependent on this contribution to finance its own activities, and as such we determined that it is a VIE, but we are not a primary beneficiary since we do not have the power to direct the activities of the entity that most significantly impact the entity’s economic performance. As of December 31, 2017, the carrying amount of the investment is $2.5 million.
On April 1, 2016, Community Imaging Partners Inc., a wholly owned subsidiary of RadNet, entered into a joint venture with Mt. Airy Health Services, LLC, a partnership of Frederick Memorial Hospital and Carroll Hospital Center. On August 31, 2016, Community Imaging Partners Inc. contributed $200,000 for a 40% economic interest in the partnership and funded an additional $440,000 in relation to a capital call. Mt. Airy Health Services, LLC, contributed $300,000 for a 60% economic interest and an additional $660,000 in relation to the capital call.
On May 9, 2016, RadNet, through a newly formed subsidiary, Glendale Advanced Imaging LLC, entered into a joint venture with Dignity Health, a California nonprofit public benefit corporation. On June 1, 2016, RadNet contributed net assets of $2.2 million for a 55% economic interest and Dignity Health contributed net assets of $1.8 million for a 45% economic interest.
Joint venture investment and financial information
The following table is a summary of our investment in joint ventures during the years ended December 31, 2017 and December 31, 2016 (in thousands):
| Balance as of December 31, 2015 | $ | 33,584 | ||
| Equity contributions in existing and purchase of interest in joint ventures | 3,084 | |||
| Equity in earnings in these joint ventures | 9,767 | |||
| Distribution of earnings | (2,926 | ) | ||
| Balance as of December 31, 2016 | $ | 43,509 | ||
| Equity contributions in existing and purchase of interest in joint ventures | 4,062 | |||
| Equity in earnings in these joint ventures | 13,554 | |||
| Distribution of earnings | (8,690 | ) | ||
| Balance as of December 31, 2017 | $ | 52,435 |
| 72 |
We received management service fees from the centers underlying these joint ventures of approximately $13.1 million for the year ended December 31, 2017, $11.9 million for the year ended December 31, 2016 and $9.3 million per year for the year ended December 31, 2015. We eliminate any unrealized portion of our management service fees with our equity in earnings of joint ventures.
The following table is a summary of key unaudited financial data for these joint ventures as of December 31, 2017 and 2016, respectively, and for the years ended December 31, 2017, 2016 and 2015, respectively, (in thousands):
| December 31, | ||||||||
| Balance Sheet Data: | 2017 | 2016 | ||||||
| Current assets | $ | 47,813 | $ | 40,093 | ||||
| Noncurrent assets | 107,481 | 100,146 | ||||||
| Current liabilities | (16,655 | ) | (14,077 | ) | ||||
| Noncurrent liabilities | (42,072 | ) | (44,405 | ) | ||||
| Total net assets | $ | 96,567 | $ | 81,757 | ||||
| Book value of RadNet joint venture interests | $ | 45,935 | $ | 38,539 | ||||
| Cost in excess of book value of acquired joint venture interests accounted for as equity method goodwill | 6,500 | 4,970 | ||||||
| Total value of RadNet joint venture interests | $ | 52,435 | $ | 43,509 | ||||
| Total book value of other joint venture partner interests | $ | 50,632 | $ | 43,218 | ||||
| 2017 | 2016 | 2015 | ||||||||||
| Net revenue | $ | 188,849 | $ | 160,134 | $ | 125,544 | ||||||
| Net income | $ | 28,644 | $ | 21,933 | $ | 19,485 | ||||||
NOTE 3 – RECENT ACCOUNTING STANDARDS
Accounting standards adopted
In March 2016, the Financial Accounting Standards Board (“FASB”) issued Accounting Standards Update (“ASU”) No. 2016-09 (“ASU 2016-09”), Compensation—Stock Compensation, (Topic 718): Improvements to Employee Share-Based Payment Accounting. ASU 2016-09 requires excess tax benefits and tax deficiencies, which arise due to differences between the measure of compensation expense and the amount deductible for tax purposes, to be recorded directly through the statement of operations when awards vest or are settled. In addition, cash flows related to excess tax benefits will no longer be classified separately as a financing activity apart from other tax cash flows. We elected to early adopt the new guidance for the year ended December 31, 2016. Upon adoption using the modified retrospective transition method, we recorded a cumulative effect adjustment to recognize previously unrecognized excess tax benefits which increased deferred tax assets and reduced accumulated deficit by $7.1 million. The current net tax benefit for 2016 resulting from adoption of the new guidance is approximately $400,000 and is reflected in our tax provision.
Accounting standards not yet adopted
In May 2014, the FASB issued ASU No. 2014-09, Revenue from Contracts with Customers, (Topic 606). ASU 2014-09 requires an entity to recognize as revenue the amount that reflects the consideration to which it expects to be entitled in exchange for goods or services as it transfers control to its customers. It also requires more detailed disclosures to enable users of the financial statements to understand the nature, amount, timing and uncertainty of revenue and cash flows arising from contracts with customers. The Company’s current revenue recognition policies for our most significant revenue streams, materially comply with the amended guidance. The primary change for healthcare providers under the new guidance is the requirement to report the allowance for uncollectible accounts associated with patient responsibility amounts as a reduction in net revenue as opposed to bad debt expense as a component of operating expenses. The new standard supersedes most current revenue guidance, including industry-specific guidance, and may be applied retrospectively with cumulative effect recognized in retained earnings as of the date of adoption (modified retrospective method). The guidance became effective for the Company on January 1, 2018 and the Company adopted the new standard using the modified retrospective approach. As part of adopting the standard, the Company identified revenue streams of like contracts to allow for ease of implementation. The Company used primarily a portfolio approach to apply the new model to classes of customers with similar characteristics. The impact of adopting the new standard on our total revenue; and income from operations is not material. The immaterial impact of adopting Topic 606 primarily relates to recognizing certain credit and collection issues not known at the date of service, including bankruptcy, in the provision for uncollectible accounts included in expenses on the consolidated statement of operations, which previously were netted against service revenue. In addition, the number of our performance obligations under the new standard is not materially different from our contract segments under the existing standard. Lastly, the accounting for the estimate of variable consideration is not materially different compared to our current practice. As such, the adoption of this guidance is not expected to have a material impact on our Consolidated Financial Statements.
| 73 |
In February 2016, the FASB issued ASU No. 2016-02, Leases, (Topic 842): Amendments to the FASB Accounting Standards Codification. ASU 2016-02 amends the existing accounting standards for lease accounting, including requiring lessees to recognize most leases on their balance sheets and making targeted changes to lessor accounting. The new standard requires a modified retrospective transition approach for all leases existing at, or entered into after, the date of initial application, with an option to use certain transition relief. The amendments in this update are effective for fiscal years (and interim reporting periods within fiscal years) beginning after December 15, 2018. Early adoption of the amendments is permitted for all entities. We are currently evaluating the impact this guidance will have on our consolidated financial statements, but expect this adoption will result in a significant increase in the assets and liabilities related to our leased properties and equipment.
In February 2018, the FASB issued ASU No. 2018-02 (“ASU 2018-02”), Reclassification of Certain Tax Effects from Accumulated Other Comprehensive Income. ASU 2018-02 allows for the reclassification of certain income tax effects related to the Tax Cuts and Jobs Act between “Accumulated other comprehensive income” and “Retained earnings.” This ASU relates to the requirement that adjustments to deferred tax liabilities and assets related to a change in tax laws or rates to be included in “Income from continuing operations”, even in situations where the related items were originally recognized in “Other comprehensive income” (rather than in “Income from continuing operations”). ASU 2018-02 is effective for all entities for fiscal years beginning after December 15, 2018, and interim periods within those fiscal years, with early adoption permitted. Adoption of this ASU is to be applied either in the period of adoption or retrospectively to each period in which the effect of the change in the tax laws or rates were recognized. We are evaluating the effect of this guidance.
In January 2017, the FASB issued ASU No. 2017-04 (“ASU 2017-04”), Simplifying the Test for Goodwill Impairment. ASU 2017-04 eliminates the requirement to calculate the implied fair value of goodwill (i.e., Step 2 of the current goodwill impairment test) to measure a goodwill impairment charge. Instead, entities will record an impairment charge based on the excess of a reporting unit’s carrying amount over its fair value (i.e., measure the charge based on the current Step 1). ASU 2017-04 is effective for annual and any interim impairment tests for periods beginning after December 15, 2019, with early adoption permitted. We are evaluating the effect of this guidance.
In January 2017, the FASB issued ASU No. 2017-01 (“ASU 2017-01”), Clarifying the Definition of a Business. ASU 2017-01 changes the definition of a business to assist entities with evaluating when a set of transferred assets and activities is considered a business. ASU 2017-01 is effective for annual periods beginning after December 31, 2017 including interim periods within those periods. There was no material impact on our financial statements.
NOTE 4 – FACILITY ACQUISITIONS, ASSETS HELD FOR SALE AND DISPOSITIONS
Acquisitions
On October 5, 2017 we completed our acquisition of all of the outstanding equity interests in RadSite, LLC, for $1.0 million in common stock and $856,000 in cash. RadSite provides both quality certification and accreditation programs for imaging providers in accordance with standards of private insurance payors and federal regulations under Medicare. We have made a fair value determination of the acquired assets and approximately $91,000 of current assets, $25,000 in fixed assets, a $150,000 covenant not to compete, $75,000 in liabilities and $1.7 million in goodwill were recorded.
On October 1, 2017 we completed our acquisition of certain assets of Remote Diagnostic Imaging P.L.L.C., consisting of a single multi-modality center located in New York, New York, for purchase consideration of $3.9 million. We have made a fair value determination of the acquired assets and approximately $2.6 million in fixed assets, a $50,000 covenant not to compete, and $1.2 million in goodwill were recorded.
On August 7, 2017 we acquired Diagnostic Imaging Associates (“DIA”) for $13.0 million in cash and $1.5 million in RadNet common stock. Located in the state of Delaware, DIA operates five multi-modality imaging locations which provide MRI, CT, Ultrasound, Mammography and X-Ray services. We have made a fair value determination of the acquired assets and approximately $3.1 million of fixed assets and equipment, $1.2 million in current assets, and $10.2 million in goodwill were recorded.
On June 1, 2017 we completed our acquisition of certain assets of Stockton MRI and Molecular Imaging Medical Center Inc., consisting of a multi-modality center located in Stockton, CA, for consideration of $4.4 million. The facility provides MRI, CT, Ultrasound, X-Ray and Nuclear Medicine services. We have made a fair value determination of the acquired assets and approximately $1.2 million of fixed assets and equipment, a $50,000 covenant not to compete, and $3.1 million of goodwill were recorded.
| 74 |
On May 3, 2017 we completed our acquisition of certain assets of D&D Diagnostics Inc., consisting of a single multi-modality imaging center located in Silver Spring, Maryland, for total purchase consideration of $2.4 million, including cash consideration of $1.2 million and settlement of liabilities of $1.2 million. We have made a fair value determination of the acquired assets and approximately $820,000 of fixed assets, $16,000 of other assets, and $1.5 million of goodwill were recorded. The facility provides MRI, CT, X-Ray and related services.
On February 1, 2017, we completed our acquisition of certain assets of MRI Centers, Inc., consisting of one single-modality imaging center located in Torrance, CA providing MRI and sports medicine services, for cash consideration of $800,000 and the payoff of $81,000 in debt. We have made a fair value determination of the acquired assets and approximately $289,000 of fixed assets, $9,800 of other assets, $100,000 covenant not to compete and $401,000 of goodwill were recorded.
On January 13, 2017, we completed our acquisition of certain assets of Resolution Medical Imaging Corporation for consideration of $4.0 million. The purchase of Resolution was enacted to contribute its assets to a joint venture with Cedars Sinai Medical Corporation which was effective April 1, 2017. See the formation of new joint ventures section in Note 2 above for further information.
In separate purchases occurring on July 1 and October 1 2016, we acquired for approximately $1.2 million the remaining non-controlling interest of 47.6% in the Park West joint venture, thus increasing our ownership percentage from 52.4% to 100%. The difference between the consideration paid and the carrying value of the non-controlling interest purchased was recorded as additional paid-in capital.
On March 1, 2016 we completed our acquisition of certain assets of Advanced Radiological Imaging – Astoria P.C. consisting of two multi-modality imaging centers located in Astoria, NY for cash consideration of $5.0 million. The facility provides MRI, PET/CT, Ultrasound and X-ray services. We have made a fair value determination of the acquired assets and approximately $3.6 million of fixed assets, $47,000 of prepaid assets, $100,000 covenant not to compete, and $1.3 million of goodwill were recorded.
Dispositions and Sales of Noncontrolling Interest
On September 1, 2017 we completed the equity sale of a wholly owned breast oncology practice, Breastlink Medical Group, Inc., to Verity Medical Foundation for approximately $2.8 million. We recorded a gain of approximately $845,000 and incurred severance expense of approximately $1.2 million on this transaction.
On July 1, 2017 we formed a majority owned subsidiary, Advanced Imaging at Timonium Crossing, LLC, in conjunction with the University of Maryland St. Joseph Medical Center. As part of that transaction, we sold a 25% noncontrolling interest in an imaging center of our wholly owned subsidiary, Advanced Imaging Partners, Inc., to the University of Maryland St. Joseph Medical Center for $3.9 million. On the date of sale, the net book value of the 25% interest was $1.1 million and the proceeds in excess of net book value amounting to $2.8 million were recorded to equity.
On April 28, 2017 we completed the sale of five imaging centers operating in Rhode Island to Rhode Island Medical Imaging, Inc. for approximately $4.5 million. We recorded a gain of approximately $1.9 million in the second quarter with regard to this transaction and have no remaining imaging centers in the state.
On April 1, 2017 we received from Cedars Sinai Medical Center $5.9 million in exchange for a 25% noncontrolling interest in the West Valley Imaging Group, LLC (“WVI”). The determined net book value of the 25% interest was approximately $3.0 million. The proceeds in excess of the net book value, amounting to $1.8 million net of taxes, were recorded to equity.
On April 1, 2017 we completed the sale of 2 wholly owned oncology practices to Cedars Sinai Medical Center in connection with the sale of non-controlling interest of the WVI subsidiary described above for approximately $1.2 million. We recorded a gain of approximately $361,000 on this transaction.
| 75 |
On November 4, 2016, the Board of Directors resolved to sell the ownership interest in all five of its Rhode Island imaging centers operating under the name The Imaging Institute within the upcoming 12 months. The following table summarizes the major categories of assets classified as held for sale in the accompanying Consolidated Balance Sheets at December 31, 2016 (in thousands):
| Property and equipment, net | $ | 1,056 | ||
| Other assets | 21 | |||
| Goodwill | 1,126 | |||
| Total assets held for sale | $ | 2,203 |
As the sale of these assets does not represent a strategic shift that will have a major effect on the Company’s operations and financial results, it is not classified as a discontinued operation. The disposition occurred on April 28, 2017.
NOTE 5 – GOODWILL AND OTHER INTANGIBLE ASSETS
Goodwill is recorded as a result of business combinations. Activity in goodwill for the years ended December 31, 2016 and 2017 is provided below (in thousands):
| Balance as of December 31, 2015 | $ | 239,408 | ||
| Goodwill acquired through the acquisition of Advanced Radiological Imaging | 1,280 | |||
| Adjustments to our preliminary allocation of the purchase price of Diagnostic Imaging Group, LLC | (47 | ) | ||
| Goodwill acquired through the acquisition of Landmark Imaging, LLC | 38 | |||
| Goodwill held for sale | (1,126 | ) | ||
| Balance as of December 31, 2016 | 239,553 | |||
| Goodwill acquired through the acquisition of Resolution Imaging Medical Corp | 1,901 | |||
| Goodwill acquired through the acquisition of MRI Centers Inc. | 401 | |||
| Goodwill disposed through the transfer to Santa Monica Imaging Group JV | (1,901 | ) | ||
| Goodwill acquired through the acquisition of D&D Diagnostics, Inc. | 1,519 | |||
| Goodwill acquired through the acquisition of Stockton MRI, Inc. | 3,101 | |||
| Goodwill disposed through the sale of Hematology Oncology | (110 | ) | ||
| Goodwill acquired through the acquisition of DIA, Inc. | 9,185 | |||
| Goodwill disposed through the sale of Breastlink Medical Group, Inc. | (509 | ) | ||
| Goodwill acquired through the acquisition of RDI, Inc. | 1,202 | |||
| Adjustments to our preliminary allocation of the purchase price of DIA, Inc. | 1,058 | |||
| Goodwill acquired through the acquisition of RadSite, LLC | 1,665 | |||
| Goodwill transferred to other assets | (289 | ) | ||
| Balance as of December 31, 2017 | $ | 256,776 |
The amount of goodwill from these acquisitions that is deductible for tax purposes as of December 31, 2017 is $110.1 million.
Other intangible assets are primarily related to the value of management service agreements obtained through our acquisition of Radiologix, Inc. in 2006 and are recorded at a cost of $57.5 million less accumulated amortization of $25.7 million at December 31, 2017. Also included in other intangible assets is the value of covenant not to compete contracts associated with our facility acquisitions totaling $6.4 million less accumulated amortization of $5.8 million, as well as the value of trade names associated with acquired imaging facilities totaling $10.2 million less accumulated amortization of $1.5 million and dispositions of $750,000.
Total amortization expense was $2.6 million for each of the years ended December 31, 2017 and 2016 and $3.0 million for the year ended December 31, 2015. Intangible assets are amortized using the straight-line method. Management service agreements are amortized over 25 years using the straight line method.
| 76 |
The following table shows annual amortization expense, by asset classes that will be recorded over the next five years (in thousands):
| 2018 | 2019 | 2020 | 2021 | 2022 | Thereafter | Total | Weighted average amortization period remaining in years | |||||||||||||||||||||||||
| Management Service Contracts | $ | 2,287 | $ | 2,287 | $ | 2,287 | $ | 2,287 | $ | 2,287 | $ | 20,396 | $ | 31,831 | 13.9 | |||||||||||||||||
| Covenant not to compete contracts | 279 | 199 | 119 | 43 | 14 | – | 654 | 2.8 | ||||||||||||||||||||||||
| Trade Names* | – | – | – | – | – | 7,937 | 7,937 | – | ||||||||||||||||||||||||
| Total Annual Amortization | $ | 2,566 | $ | 2,486 | $ | 2,406 | $ | 2,330 | $ | 2,301 | $ | 28,333 | $ | 40,422 | ||||||||||||||||||
* These trade name intangibles have an indefinite life
NOTE 6 - PROPERTY AND EQUIPMENT
Property and equipment and accumulated depreciation and amortization are as follows (in thousands):
| December 31, | ||||||||
| 2017 | 2016 | |||||||
| Land | $ | 250 | $ | 250 | ||||
| Medical equipment | 380,439 | 393,001 | ||||||
| Computer and office equipment, furniture and fixtures | 96,382 | 99,434 | ||||||
| Software development costs | 6,391 | 6,391 | ||||||
| Leasehold improvements | 273,436 | 252,595 | ||||||
| Equipment under capital lease | 17,180 | 26,758 | ||||||
| Total property and equipment cost | 774,078 | 778,429 | ||||||
| Accumulated depreciation | (529,511 | ) | (529,648 | ) | ||||
| Total net property and equipment | 244,567 | 248,781 | ||||||
| Equipment transferred to other assets | (266 | ) | (1,056 | ) | ||||
| Total property and equipment | $ | 244,301 | $ | 247,725 | ||||
Depreciation and amortization expense of property and equipment, including amortization of equipment under capital leases, for the years ended December 31, 2017, 2016 and 2015 was $64.2 million, $64.0 million, and $57.6 million, respectively.
NOTE 7 – ACCOUNTS PAYABLE AND ACCRUED EXPENSES
Accounts payable and accrued expenses were comprised of the following (in thousands):
| December 31, | ||||||||
| 2017 | 2016 | |||||||
| Accounts payable | $ | 28,538 | $ | 40,952 | ||||
| Accrued expenses | 67,298 | 36,993 | ||||||
| Accrued salary and benefits | 30,670 | 25,009 | ||||||
| Accrued professional fees | 9,303 | 8,212 | ||||||
| Total | $ | 135,809 | $ | 111,166 | ||||
| 77 |
NOTE 8 - NOTES PAYABLE, REVOLVING CREDIT FACILITY AND CAPITAL LEASES
Revolving credit facility, notes payable, and capital lease obligations:
| December 31, | December 31, | |||||||
| 2017 | 2016 | |||||||
| First Lien Term Loans | $ | 620,272 | $ | 478,938 | ||||
| Second Lien Term Loans | – | 168,000 | ||||||
| Discounts on term loans | (18,470 | ) | (16,783 | ) | ||||
| Promissory note payable to the former owner of a practice acquired at an interest rate of 1.5% due through 2019 | 592 | 980 | ||||||
| Equipment notes payable at interest rates ranging from 3.3% to 5.6%, due through 2020, collateralized by medical equipment | 195 | 341 | ||||||
| Obligations under capital leases at interest rates ranging from 4.3% to 11.2%, due through 2022, collateralized by medical and office equipment | 6,538 | 7,256 | ||||||
| Total debt obligations | 609,127 | 638,732 | ||||||
| Less current portion | (34,090 | ) | (26,557 | ) | ||||
| Long-term portion debt obligations | $ | 575,037 | $ | 612,175 | ||||
The following is a listing of annual principal maturities of notes payable exclusive of all related discounts, capital leases and repayments on our revolving credit facilities for years ending December 31 (in thousands):
| 2018 | $ | 33,582 | ||
| 2019 | 33,357 | |||
| 2020 | 33,092 | |||
| 2021 | 33,081 | |||
| 2022 | 33,081 | |||
| Thereafter | 454,866 | |||
| Total notes payable obligations | $ | 621,059 |
We lease equipment under capital lease arrangements. Future minimum lease payments under capital leases for years ending December 31 (in thousands) is as follows:
| 2018 | $ | 4,080 | ||
| 2019 | 2,276 | |||
| 2020 | 282 | |||
| 2021 | 162 | |||
| 2022 | 60 | |||
| Thereafter | – | |||
| Total minimum payments | 6,860 | |||
| Amount representing interest | (322 | ) | ||
| Present value of net minimum lease payments | 6,538 | |||
| Less current portion | (3,866 | ) | ||
| Long-term portion lease obligations | $ | 2,672 |
| 78 |
Term Loans, Revolving Credit Facility and Financing Activity Information:
At December 31, 2017, our credit facilities were comprised of one tranche of term loans (“First Lien Term Loans”) and a revolving credit facility of $117.5 million (the “Revolving Credit Facility”). As of December 31, 2017, we were in compliance with all covenants under our credit facilities.
Included in our consolidated balance sheets at December 31, 2017 are $601.8 million of senior secured term loan debt (net of unamortized discounts of $18.5 million) in thousands:
| Face Value | Discount | Total Carrying Value | ||||||||||
| Total First Lien Term Loans | $ | 620,272 | $ | (18,470 | ) | $ | 601,802 | |||||
We had no balance under our $117.5 million Revolving Credit Facility at December 31, 2017.
The following describes our 2017 financing activities:
Amendment No. 5, Consent and Incremental Joinder Agreement to Credit and Guaranty Agreement
On August 22, 2017, we entered into Amendment No. 5, Consent and Incremental Joinder Agreement to Credit and Guaranty Agreement (the “Fifth Amendment”) with respect to our First Lien Credit Agreement. Pursuant to the Fifth Amendment, we issued $170.0 million in incremental First Lien Term Loans, the proceeds of which were used to repay in full all outstanding Second Lien Term Loans and all other obligations under the Second Lien Credit Agreement.
Pursuant to the Fifth Amendment, we also changed the interest rate margin applicable to borrowings under the First Lien Credit Agreement. While borrowings under the First Lien Credit Agreement continue to bear interest at either an Adjusted Eurodollar Rate or a Base Rate (in each case, as more fully defined in the First Lien Credit Agreement) or a combination of both, at the election of the Company, plus an applicable margin. The applicable margin for Adjusted Eurodollar Rate borrowings and Base Rate borrowings was changed from 3.25% and 2.25%, respectively, to 3.75% and 2.75%, respectively, through an initial period which ends when financial reporting is delivered for the period ending September 30, 2017. Thereafter, the rates of the applicable margin for borrowing under the First Lien Credit Agreement will adjust depending on our leverage ratio, according to the following schedule:
| First Lien Leverage Ratio | Eurodollar Rate Spread | Base Rate Spread |
| > 5.50x | 4.50% | 3.50% |
| > 4.00x but ≤ 5.50x | 3.75% | 2.75% |
| >3.50x but ≤ 4.00x | 3.50% | 2.50% |
| ≤ 3.50x | 3.25% | 2.25% |
At December 31, 2017 the effective Adjusted Eurodollar Rate and the Base Rate for the First Lien Term Loans was 1.36% and 4.50%, respectively and the applicable margin for Adjusted Eurodollar Rate and Base Rate borrowings remained at 3.75% and 2.75%, respectively.
Pursuant to the Fifth Amendment, the First Lien Credit Agreement was amended so that we can elect to request 1) an increase to the existing Revolving Credit Facility and/or 2) additional First Lien Term Loans, provided that the aggregate amount of such increases and additions does not exceed (a) $100.0 million and (b) as long as the First Lien Leverage Ratio (as defined in the First Lien Credit Agreement) would not exceed 4.00:1.00 after giving effect to such incremental facilities, an uncapped amount of incremental facilities, in each case subject to the conditions and limitations set forth in the First Lien Credit Agreement. Each lender approached to provide all or a portion of any incremental facility may elect or decline, in its sole discretion, to provide an incremental commitment or loan.
Pursuant to the Fifth Amendment, the First Lien Credit Agreement was also amended to (i) provide for quarterly payments of principal of the First Lien Term Loans in the amount of approximately $8.3 million, as compared to approximately $6.1 million prior to the Fifth Amendment, (ii) extend the call protection provided to the holders of the First Lien Term Loans for a period of twelve months following the date of the Fifth Amendment and (iii) provide us with additional operating flexibility, including the ability to incur certain additional debt and to make certain additional restricted payments, investments and dispositions, in each case as more fully set forth in the Fifth Amendment. Total issue costs for the Fifth Amendment aggregated to approximately $4.7 million. Of this amount, $4.1 million was identified and capitalized as discount on debt, $350,000 was capitalized as deferred financing costs and the remaining $235,000 was expensed. Amounts capitalized will be amortized over the remaining term of the agreement.
| 79 |
Fourth Amendment to First Lien Credit Agreement
On February 2, 2017, we entered into Amendment No. 4 to Credit and Guaranty Agreement (the “Fourth Amendment”) with respect to our First Lien Credit Agreement. Pursuant to the Fourth Amendment, the interest rate margin per annum on the First Lien Term Loans and the Revolving Credit Facility was reduced by 50 basis points, from 3.75% to 3.25%. Except for such reduction in the interest rate on credit extensions, the Fourth Amendment did not result in any other material modifications to the First Lien Credit Agreement. RadNet incurred expenses for the transaction in the amount of $543,000, which was recorded to discount on debt and will be amortized over the remaining term of the agreement.
The following describes our applicable financing prior to giving effect to the Fourth Amendment and Fifth Amendment discussed above.
First Lien Credit Agreement
On July 1, 2016, we entered into the First Lien Credit Agreement pursuant to which we amended and restated our then existing first lien credit facilities. Pursuant to the First Lien Credit Agreement, we originally issued $485 million of First Lien Term Loans and established the $117.5 million Revolving Credit Facility. Proceeds from the First Lien Credit Agreement were used to repay the previously outstanding first lien loans under the First Lien Credit Agreement, make a $12.0 million principal payment of the Second Lien Term Loans, pay costs and expenses related to the First Lien Credit Agreement and provide approximately $10.0 million for general corporate purposes.
Interest. The interest rates payable on the First Lien Term Loans were (a) the Adjusted Eurodollar Rate (as defined in the First Lien Credit Agreement) plus 3.75% per annum or (b) the Base Rate (as defined in the First Lien Credit Agreement) plus 2.75% per annum. As applied to the First Lien Term Loans, the Adjusted Eurodollar Rate has a minimum floor of 1.0%.
Payments. The scheduled quarterly principal payment of the First Lien Term Loans was approximately $6.1 million, with the balance due at maturity.
Maturity Date. The maturity date for the First Lien Term Loans shall be on the earliest to occur of (i) July 1, 2023, (ii) the date on which all First Lien Term Loans shall become due and payable in full under the First Lien Credit Agreement, whether by acceleration or otherwise, and (iii) September 25, 2020 if our indebtedness under the Second Lien Credit Agreement had not been repaid, refinanced or extended prior to such date.
Revolving Credit Facility: The First Lien Credit Agreement provides for a $117.5 million Revolving Credit Facility. Revolving loans borrowed under the Revolving Credit Facility bear interest at either an Adjusted Eurodollar Rate or a Base Rate (in each case, as more fully defined in the First Lien Credit Agreement), plus an applicable margin. Pursuant to the Fifth Amendment, the applicable margin was amended to vary based on our leverage ratio in accordance with the following schedule:
| First Lien Leverage Ratio | Eurodollar Rate Spread | Base Rate Spread |
| > 5.50x | 4.50% | 3.50% |
| > 4.00x but ≤ 5.50x | 3.75% | 2.75% |
| >3.50x but ≤ 4.00x | 3.50% | 2.50% |
| ≤ 3.50x | 3.25% | 2.25% |
For letters of credit issued under the Revolving Credit Facility, letter of credit fees accrue at the applicable margin (see table above) for Adjusted Eurodollar Rate revolving loans and fronting fees accrue at 0.25% per annum, in each case on the average aggregate daily maximum amount available to be drawn under all letters of credit issued under the First Lien Credit Agreement. In addition a commitment fee of 0.5% per annum accrues on the unused revolver commitments under the Revolving Credit Facility. As of December 31, 2017, the interest rate payable on revolving loans was 7.0% and the amount available to borrow under the Revolving Credit Facility was $117.5 million.
The Revolving Credit Facility will terminate on the earliest to occur of (i) July 1, 2021, (ii) the date we voluntarily agree to permanently reduce the Revolving Credit Facility to zero pursuant to section 2.13(b) of the First Lien Credit Agreement, and (iii) the date the Revolving Credit Facility is terminated due to specific events of default pursuant to section 8.01 of the First Lien Credit Agreement.
| 80 |
Second Lien Credit Agreement:
On March 25, 2014, we entered into the Second Lien Credit and Guaranty Agreement (the “Second Lien Credit Agreement”) pursuant to which we issued $180 million of second lien term loans (the “Second Lien Term Loans”). The proceeds from the Second Lien Term Loans were used to redeem our 10 3/8% senior unsecured notes, due 2018, to pay the expenses related to the transaction and for general corporate purposes. On July 1, 2016, in conjunction with the restated First Lien Credit Agreement, a $12.0 million principal payment was made on the Second Lien Term Loans. On August 22, 2017 the Second Lien Credit Agreement was repaid in full with the proceeds of First Lien Term Loans issued under the Fifth Amendment, as described above.
NOTE 9 – COMMITMENTS AND CONTINGENCIES
Leases – We lease various operating facilities and certain medical equipment under operating leases with renewal options expiring through 2041. Certain leases contain renewal options from two to ten years and escalation based either on the consumer price index or fixed rent escalators. Leases with fixed rent escalators are recorded on a straight-line basis. We record deferred rent for tenant leasehold improvement allowances received from certain lessors and amortize the deferred rent expense over the term of the lease agreement. Minimum annual payments under operating leases for future years ending December 31 are as follows (in thousands):
| Facilities | Equipment | Total | ||||||||||
| 2018 | $ | 58,907 | $ | 9,551 | $ | 68,458 | ||||||
| 2019 | 51,177 | 8,950 | 60,127 | |||||||||
| 2020 | 43,237 | 7,836 | 51,073 | |||||||||
| 2021 | 36,089 | 5,986 | 42,075 | |||||||||
| 2022 | 28,287 | 3,667 | 31,954 | |||||||||
| Thereafter | 102,837 | 3,118 | 105,955 | |||||||||
| $ | 320,534 | $ | 39,108 | $ | 359,642 | |||||||
Total rent expense, including equipment rentals, for the years ended December 31, 2017, 2016 and 2015 was $67.2 million, $74.2 million and $71.7 million, respectively.
Litigation – We are engaged from time to time in the defense of lawsuits arising out of the ordinary course and conduct of our business. We believe that the outcome of our current litigation will not have a material adverse impact on our business, financial condition and results of operations. However, we could be subsequently named as a defendant in other lawsuits that could adversely affect us.
NOTE 10 – INCOME TAXES
On December 22, 2017, the U.S. government enacted comprehensive tax legislation commonly referred to as the Tax Cuts and Jobs Act (“Tax Act”). Among other items, the Tax Act reduced the U.S. federal corporate tax rate to 21%, effective for tax years beginning after December 31, 2017, and established a one-time deemed repatriation transition tax on earnings of certain foreign subsidiaries that were previously tax deferred.
Due to the timing of the enactment and the complexity involved in applying the provisions of the Tax Act, the SEC issued guidance on December 22, 2017 to address the application of US GAAP in situations when a registrant does not have the necessary information available, prepared, or analyzed in reasonable detail to complete the accounting for certain income tax effects of the Tax Act. In accordance with this guidance, we have made reasonable estimates below of the effects of the Tax Act and recorded provisional amounts in our financial statements as of December 31, 2017. For the items for which we were able to determine a reasonable estimate, we recognized a provisional amount of $13.6 million, which is included as a component of income tax expense from continuing operations. As we collect and prepare necessary data, and interpret the Tax Act and any additional guidance issued by the U.S. Treasury Department, the IRS, and other standard-setting bodies, we may make adjustments to the provisional amounts. Those adjustments may materially impact our provision for income taxes and effective tax rate in the period in which the adjustments are made. The accounting for the tax effects of the Tax Act will be completed in 2018.
| 81 |
For the year ended December 31, 2017, the Company recorded a provisional net tax provision of $13.5 million related to the remeasurement of its net deferred tax assets using the new U.S. federal corporate tax rate of 21%, which is estimated to result in significantly lower federal cash taxes for the Company in 2018 and beyond. Although the tax rate reduction is known, we have not collected the necessary data to complete our analysis of the effect of the Tax Act on the underlying deferred taxes and as such, the amounts recorded as of December 31, 2017 are provisional.
The Tax Act requires the Company to pay U.S. income taxes on accumulated foreign subsidiary earnings not previously subject to U.S. income tax at a rate of 15.5% to the extent of foreign cash and certain other net current assets and 8% on the remaining earnings. Given that the transition tax analysis requires significant data from our foreign subsidiaries that is not regularly collected or analyzed, we recorded a provisional amount for the one-time transitional tax liability for our foreign subsidiaries of approximately $0.1 million. Additional work is necessary for a more detailed analysis of the Company’s deferred tax assets and liabilities and its historical foreign earnings as well as potential correlative adjustments. If the final tax outcome of these matters is different than the provisional amounts recorded by the Company, then adjustments to the provisional amounts will impact the tax provision and effective tax rate in the period recorded.
Tax Act includes new anti-deferral, anti-base erosion, and base broadening provisions. Given the complexity of these provisions, we are still evaluating the effects and impact of these provisions.
For the years ended December 31, 2017, 2016 and 2015, we recognized income tax expense comprised of the following (in thousands):
| December 31, | ||||||||||||
| 2017 | 2016 | 2015 | ||||||||||
| Federal current tax | $ | 871 | $ | 88 | $ | 237 | ||||||
| State current tax | 4,906 | 914 | 1,705 | |||||||||
| Other current tax | 23 | 28 | 28 | |||||||||
| Federal deferred tax | 21,389 | 2,539 | 3,625 | |||||||||
| State deferred tax | (2,879 | ) | 863 | 412 | ||||||||
| Income tax expense (benefit) | $ | 24,310 | $ | 4,432 | $ | 6,007 | ||||||
A reconciliation of the statutory U.S. federal rate and effective rates is as follows:
| Years Ended December 31, | ||||||||||||||||||||||||
| 2017 | 2016 | 2015 | ||||||||||||||||||||||
| Federal tax | $ | 8,971 | 34.00 | % | $ | 4,229 | 34.00 | % | $ | 4,979 | 34.00 | % | ||||||||||||
| State franchise tax, net of federal benefit | 1,799 | 6.82 | % | 224 | 1.80 | % | 1,245 | 8.50 | % | |||||||||||||||
| Other Non deductible expenses | 91 | 0.35 | % | (11 | ) | -0.09 | % | (1 | ) | -0.01 | % | |||||||||||||
| Changes in valuation allowance | (1,045 | ) | -3.96 | % | 585 | 4.70 | % | (2,536 | ) | -17.32 | % | |||||||||||||
| Tax Cuts and Jobs Act | 13,527 | 51.27 | % | – | 0.00 | % | – | 0.00 | % | |||||||||||||||
| Deferred true-ups and other | (194 | ) | -0.74 | % | (3,142 | ) | -25.25 | % | 1,964 | 13.41 | % | |||||||||||||
| Other reconciling items | 1,161 | 4.39 | % | 2,547 | 20.47 | % | 356 | 2.43 | % | |||||||||||||||
| Income tax expense (benefit) | $ | 24,310 | 92.13 | % | $ | 4,432 | 35.64 | % | $ | 6,007 | 41.02 | % | ||||||||||||
| 82 |
Deferred income taxes reflect the net tax effects of temporary differences between carrying amounts of assets and liabilities for financial and income tax reporting purposes and operating loss carryforwards.
Our deferred tax assets and liabilities comprise the following (in thousands):
| December 31, | ||||||||
| Deferred tax assets: | 2017 | 2016 | ||||||
| Net operating losses | $ | 47,212 | $ | 84,509 | ||||
| Accrued expenses | 3,242 | 4,400 | ||||||
| Straight-Line rent adjustment | 7,749 | 10,750 | ||||||
| Unfavorable contract liability | 1,288 | 2,114 | ||||||
| Equity compensation | 871 | 950 | ||||||
| Allowance for doubtful accounts | 8,720 | 6,033 | ||||||
| Other | 2,504 | 1,357 | ||||||
| Valuation allowance | (4,049 | ) | (4,428 | ) | ||||
| Total Deferred Tax Assets | $ | 67,537 | $ | 105,685 | ||||
| Deferred tax liabilities: | ||||||||
| Property and equipment | (373 | ) | (6,994 | ) | ||||
| Goodwill | (17,568 | ) | (23,350 | ) | ||||
| Intangibles | (7,839 | ) | (12,066 | ) | ||||
| Non accrual experience method reserve | (2,778 | ) | (8,483 | ) | ||||
| Other | (8,127 | ) | (4,436 | ) | ||||
| Total Deferred Tax Liabilities | $ | (36,685 | ) | $ | (55,329 | ) | ||
| Net Deferred Tax Asset | $ | 30,852 | $ | 50,356 | ||||
As of December 31, 2017, the Company had federal net operating loss carryforwards of approximately $191.6 million, which expire at various intervals from the years 2018 to 2034 if not utilized. The Company also had state net operating loss carryforwards of approximately $132.3 million, which expire at various intervals from the years 2018 through 2037. As of December 31, 2017, $23.5 million of our federal net operating loss carryforwards acquired in connection with the 2011 acquisition of Raven Holdings U.S., Inc. are subject to limitations related to their utilization under Section 382 of the Internal Revenue Code. Future ownership changes as determined under Section 382 of the Internal Revenue Code could further limit the utilization of net operating loss carryforwards.
| 83 |
We considered all evidence available when determining whether deferred tax assets are more likely-than-not to be realized, including projected future taxable income, scheduled reversals of deferred tax liabilities, prudent tax planning strategies, and recent financial operations. The evaluation of this evidence requires significant judgment about the forecasts of future taxable income, based on the plans and estimates we are using to manage the underlying businesses. In evaluating the objective evidence that historical results provide, we consider three years of cumulative operating income. As of December 31, 2017, we have determined that deferred tax assets of $67.5 million are more likely-than-not to be realized. We have also determined that deferred tax liabilities of $17.6 million are required related to book basis in goodwill that has an indefinite life.
We file consolidated income tax returns in the U.S. federal jurisdiction and various states and foreign jurisdictions. We continue to reinvest earnings of the non-US entities for the foreseeable future and therefore have not recognized any U.S. tax expense on these earnings. With limited exceptions, we are no longer subject to U.S. federal, state and local, or non-U.S. income tax examinations by tax authorities for years before 2013. We do not anticipate the results of any open examinations would result in a material change to its financial position.
At December 31, 2017, the Company has unrecognized tax benefits of $3.6 million of which $2.9 million will affect the effective tax rate if recognized.
A reconciliation of the total gross amounts of unrecognized tax benefits for the years ended as follows (in thousands):
| December 31, | ||||||||||||
| 2017 | 2016 | 2015 | ||||||||||
| Balance at beginning of year | $ | 3,861 | $ | 94 | $ | 3,761 | ||||||
| Increases (Decreases) related to prior year tax positions | 1 | 3,861 | (3,667 | ) | ||||||||
| Expiration of the statute of limitations for the assessment of taxes | – | (94 | ) | – | ||||||||
| Increase (Decreases) related to change in rate | (247 | ) | – | – | ||||||||
| Balance at end of year | $ | 3,615 | $ | 3,861 | $ | 94 | ||||||
The Company believes it is reasonably possible it will not materially reduce its unrecognized tax benefits within the next twelve months.
The Company recognizes accrued interest and penalties related to unrecognized tax benefits in income tax expense. During the year ended December 31, 2017 the Company accrued an insignificant amount of interest expense. As of December 31, 2017, accrued interest and penalties were insignificant.
NOTE 11 – STOCK-BASED COMPENSATION
Stock Incentive Plans
Options
We have one long-term equity incentive plan which we refer to as the 2006 Equity Incentive Plan, which we first amended and restated as of April 20, 2015 and again on March 9, 2017 (“the Restated Plan”). The Restated Plan was approved by our stockholders at our annual stockholders meeting on June 8, 2017. We have reserved for issuance under the 2017 Restated Plan 14,000,000 shares of common stock. We can issue options, stock awards, stock appreciation rights, stock units and cash awards under the 2017 Restated Plan. Certain options granted under the Restated Plan to employees are intended to qualify as incentive stock options under existing tax regulations. Stock options generally vest over three to five years and expire five to ten years from the date of grant.
As of December 31, 2017, we had outstanding options to acquire 420,149 shares of our common stock, of which options to acquire 43,334 shares were exercisable. The following summarizes all of our option transactions for the twelve months ended December 31, 2017:
| Outstanding Options Under the 2006 Plan |
Shares | Weighted Average Exercise price Per Common Share |
Weighted Average Remaining Contractual Life(in years) |
Aggregate Intrinsic Value |
||||||||||||
| Balance, December 31, 2016 | 375,626 | $ | 6.82 | |||||||||||||
| Granted | 209,523 | 6.95 | ||||||||||||||
| Exercised | – | – | ||||||||||||||
| Canceled, forfeited or expired | (165,000 | ) | 8.83 | |||||||||||||
| Balance, December 31, 2017 | 420,149 | 6.10 | 7.74 | $ | 1,722,210 | |||||||||||
| Exercisable at December 31, 2017 | 43,334 | 2.27 | 0.97 | 339,503 | ||||||||||||
| 84 |
Aggregate intrinsic value in the table above represents the total pretax intrinsic value (the difference between our closing stock price on December 31, 2017 and the exercise price, multiplied by the number of in-the-money options as applicable) that would have been received by the holder had all holders exercised their options on December 31, 2017. No options were exercised during the twelve months ended December 31, 2017. As of December 31, 2017, total unrecognized stock-based compensation expense related to non-vested employee awards was $842,343 which is expected to be recognized over a weighted average period of approximately 2.6 years.
Restricted Stock Awards (“RSA’s”)
The Restated Plan permits the award of restricted stock awards (“RSA’s”). As of December 31, 2017, we have issued a total of 4,945,460 RSA’s of which 447,351 were unvested at December 31, 2017. The following summarizes all unvested RSA’s activities during the twelve months ended December 31, 2017:
| Weighted-Average | ||||||||||||
| Remaining | ||||||||||||
| Contractual | Weighted-Average | |||||||||||
| RSA's | Term (Years) | Fair Value | ||||||||||
| RSA's unvested at December 31, 2016 | 573,145 | $ | 6.18 | |||||||||
| Changes during the period | ||||||||||||
| Granted | 681,448 | $ | 5.98 | |||||||||
| Vested | (807,242 | ) | $ | 6.02 | ||||||||
| RSA's unvested at December 31, 2017 | 447,351 | 0.32 | $ | 6.17 | ||||||||
We determine the fair value of all RSA’s based of the closing price of our common stock on award date.
Other stock bonus awards
The Restated Plan also permits the award of stock bonuses not subject to any future service period. These awards are valued and expensed based on the closing price of our common stock on the date of award. During the twelve months ended December 31, 2017 we issued 35,800 shares relating to these awards, amounting to $361,370 of compensation expense.
Plan summary
In summary, of the 14,000,000 shares of common stock reserved for issuance under the Restated Plan, at December 31, 2017, we had issued 13,195,159 total shares between options, RSA’s and other stock awards. With options cancelled and RSA’s forfeited amounting to 3,140,009 and 59,053 shares, respectively, there remain 4,003,903 shares available under the Restated Plan for future issuance.
NOTE 12 – EMPLOYEE BENEFIT PLAN
We adopted a profit-sharing/savings plan pursuant to Section 401(k) of the Internal Revenue Code that covers substantially all non-professional employees. Eligible employees may contribute on a tax-deferred basis a percentage of compensation, up to the maximum allowable under tax law. Employee contributions vest immediately. As of January 1, 2017, RadNet provides a matching contribution in the amount to a maximum of 1.0% per 4.0% of employee contribution and is expected to contribute approximately $2.5 million for the year ended December 31, 2017.
| 85 |
NOTE 13 – QUARTERLY RESULTS OF OPERATIONS (unaudited)
The following table sets forth a summary of our unaudited quarterly operating results for each of the last eight quarters in the years ended December 31, 2017 and 2016. This quarterly data has been derived from our unaudited consolidated interim financial statements which, in our opinion, have been prepared on substantially the same basis as the audited financial statements contained elsewhere in this report and include all normal recurring adjustments necessary for a fair presentation of the financial information for the periods presented. These unaudited quarterly results should be read in conjunction with our financial statements and notes thereto, included elsewhere in this report. The operating results in any quarter are not necessarily indicative of the results that may be expected for any future period (in thousands except per share data).
| 2017 Quarter Ended | 2016 Quarter Ended | |||||||||||||||||||||||||||||||
| Mar 31 | June 30 | Sept 30 | Dec 31 | Mar 31 | June 30 | Sept 30 | Dec 31 | |||||||||||||||||||||||||
| Statement of Operations Data: | ||||||||||||||||||||||||||||||||
| Net revenue | $ | 229,013 | $ | 230,014 | $ | 227,607 | $ | 235,552 | $ | 216,388 | $ | 218,565 | $ | 224,643 | $ | 224,939 | ||||||||||||||||
| Total operating expenses | 222,266 | 215,853 | 216,765 | 217,252 | 213,405 | 210,487 | 212,192 | 209,971 | ||||||||||||||||||||||||
| Total other expenses | 9,993 | 8,009 | 9,328 | 9,889 | 7,875 | 5,717 | 11,578 | 10,641 | ||||||||||||||||||||||||
| Equity in earnings of joint ventures | (1,928 | ) | (2,994 | ) | (3,450 | ) | (5,182 | ) | (2,279 | ) | (3,274 | ) | (2,576 | ) | (1,638 | ) | ||||||||||||||||
| Benefit from (provision for) income taxes | 458 | (3,523 | ) | (1,112 | ) | (20,133 | ) | 1,180 | (2,253 | ) | (1,458 | ) | (1,901 | ) | ||||||||||||||||||
| Net (loss) income | (860 | ) | 5,623 | 3,852 | (6,540 | ) | (1,433 | ) | 3,382 | 1,991 | 4,064 | |||||||||||||||||||||
| Net income (loss) attributable to noncontrolling interests | 350 | 313 | 623 | 736 | 290 | (243 | ) | 344 | 383 | |||||||||||||||||||||||
| Net (loss) income attributable to Radnet, Inc. common stockholders | $ | (1,210 | ) | $ | 5,310 | $ | 3,229 | $ | (7,276 | ) | $ | (1,723 | ) | $ | 3,625 | $ | 1,647 | $ | 3,681 | |||||||||||||
| Basic net (loss) income attributable to Radnet, Inc. common stockholders (loss) earnings per share: | $ | (0.03 | ) | $ | 0.11 | $ | 0.07 | $ | (0.15 | ) | $ | (0.04 | ) | $ | 0.08 | $ | 0.04 | $ | 0.08 | |||||||||||||
| Diluted net (loss) income attributable to Radnet, Inc. common stockholders (loss) earnings per share: | $ | (0.03 | ) | $ | 0.11 | $ | 0.07 | $ | (0.15 | ) | $ | (0.04 | ) | $ | 0.08 | $ | 0.04 | $ | 0.08 | |||||||||||||
| Weighted average shares outstanding | ||||||||||||||||||||||||||||||||
| Basic | 46,560 | 46,756 | 46,954 | 47,237 | 46,581 | 46,559 | 45,869 | 45,967 | ||||||||||||||||||||||||
| Diluted | 46,560 | 47,196 | 47,578 | 47,886 | 46,581 | 46,882 | 46,334 | 46,389 | ||||||||||||||||||||||||
NOTE 14 – RELATED PARTY TRANSACTIONS
We used World Wide Express, a package delivery company formerly owned by our western operations chief operating officer, to provide delivery services for us. For the years ended December 31, 2016 and 2015, we paid approximately $670,000 and $693,000 respectively, to World Wide Express for those services. At December 31, 2016, we had outstanding amounts due to World Wide Express of $273,000. World Wide Express is no longer affiliated with the Company as a related party for the year ended December 31, 2017.
NOTE 15 – SUBSEQUENT EVENTS
On January 1, 2018 we completed our acquisition of certain assets of Imaging Services Company of New York, LLC, consisting of a single multi-modality center located in New York, New York, for purchase consideration of $5.8 million.
On January 1, 2018, we formed Beach Imaging Group, LLC (“Beach Imaging”) and contributed the operations of 24 imaging facilities spread across southern Los Angeles and Orange Counties in exchange for a 60% economic interest. MemorialCare Medical Foundation (MCMF), a hospital system in southern California, contributed $22.9 million in cash along with the operations of 10 of its imaging facilities in southern California to receive a 40% economic interest in Beach Imaging. In connection with the same transaction, Beach Imaging agreed to sell one of its newly acquired imaging center from RadNet to MCMF for $1.7 million.
| 86 |
| Item 9. | Changes In and Disagreements with Accountants on Accounting and Financial Disclosure |
None.
| Item 9A | Controls and Procedures |
Evaluation of Disclosure Controls and Procedures
Under the supervision of our management, including our Chief Executive Officer and Chief Financial Officer, we conducted an evaluation of the effectiveness of the design and operation of our disclosure controls and procedures under Rules 13a-15(e) and 15d-15(e) of the Securities Exchange Act of 1934, as amended, as of December 31, 2016. Based on this evaluation, our Chief Executive Officer and Chief Financial Officer concluded that our disclosure controls and procedures were not effective as of December 31, 2017 because deficiencies in the operating effectiveness of several information technology dependent manual controls related to the revenue and accounts receivable process caused a material weakness in our internal control over financial reporting as described in more detail below.
Limitations on Effectiveness of Controls and Procedures
Because of its inherent limitations, internal control over financial reporting may not prevent or detect misstatements. Also, projections of any evaluation of effectiveness to future periods are subject to the risk that controls may become inadequate because of changes in conditions, or that the degree of compliance with existing policies or procedures may deteriorate.
Management's Report on Internal Control over Financial Reporting
Our management is responsible for establishing and maintaining adequate internal control over financial reporting. Internal control over financial reporting is a process designed to provide reasonable assurance regarding the reliability of financial reporting and the preparation of financial statements for external purposes in accordance with U.S. generally accepted accounting principles (“GAAP”). Internal control over financial reporting includes policies and procedures that (i) pertain to the maintenance of records that, in reasonable detail, accurately and fairly reflect the transactions and dispositions of the assets of the Company; (ii) provide reasonable assurance that transactions are recorded as necessary to permit preparation of financial statements in accordance with GAAP, and that receipts and expenditures of the Company are transacted in accordance with authorizations of management and directors of the Company; and (iii) provide reasonable assurance regarding prevention or timely detection of unauthorized acquisition, use, or disposition of the Company’s assets that could have a material effect on the financial statements.
Our management, under the supervision of our Chief Executive Officer and Chief Financial Officer, conducted an assessment of the effectiveness of its internal control over financial reporting as of December 31, 2017 based on the criteria established in Internal Control - Integrated Framework (2013) issued by the Committee of Sponsoring Organizations of the Treadway Commission (“COSO”). Based on this assessment, management concluded that our internal control over financial reporting was not effective as of December 31, 2017 because of the material weakness described below.
A material weakness is defined as “a deficiency, or a combination of deficiencies, in internal control over financial reporting, such that there is a reasonable possibility that a material misstatement of the Company’s annual or interim financial statements will not be prevented or detected on a timely basis.”
Management concluded that, as of December 31, 2015 and 2016, certain user access, program change and operations control components of information technology general controls and information technology dependent manual control deficiencies related to the Company’s revenue and accounts receivable process were not designed and operating effectively, which aggregate to a material weakness in the Company’s internal control over financial reporting.
Management concluded that our internal controls over financial reporting were not effective as of December 31, 2017 because the following control deficiency related to the Company’s revenue and accounts receivable process identified in the years ended December 31, 2015 and 2016 has not been remediated and therefore a material weakness continues to be present in the Company’s internal control over financial reporting:
| · | Certain information technology dependent manual controls which are (i) designed to ensure the completeness of revenue transaction processing, and (ii) designed to ensure a reasonable valuation of the Company’s accounts receivable balance were not performed timely, accurately or reviewed with sufficient precision. |
| 87 |
The ineffective operation of these information technology dependent manual controls impacts a material portion of our revenue transactions.
Ernst & Young LLP, the Company’s independent registered public accounting firm, has audited the Company’s internal control over financial reporting as of December 31, 2017, as stated in their report, which is included below in this Annual Report on Form 10-K.
Remediation Plan for Material Weakness
Management, with oversight of our Audit Committee, has been actively engaged in developing and executing a remediation plan to address the material weakness originally identified in the year ended December 31, 2015. The remediation efforts, which are ongoing, are to continue to focus on executing certain information technology dependent manual controls which are designed to ensure the completeness of revenue transaction processing, and to ensure a reasonable valuation of the Company’s accounts receivable balance on a timely basis and with an adequate level of precision.
If the remedial measures described above are insufficient to address the material weakness described above, or are not implemented timely, or additional deficiencies arise in the future, material misstatements in our interim or annual financial statements may occur in the future and could have the effects described in “Item 1A. Risk Factors” in Part I of this Form 10-K.
Changes in Internal Control over Financial Reporting
Management identified the following changes in internal control over financial reporting occurring during the fourth quarter that materially affected, or was reasonably likely to materially affect, the Company’s internal control over financial reporting:
| · | Certain user access, program change and operations control components of information technology general controls pertaining to multiple systems which capture and bill revenue transactions and design components relating to certain information technology dependent manual controls related to the Company’s revenue and accounts receivable process were modified. |
| 88 |
Report of Independent Registered Public Accounting Firm
Board of Directors and Stockholders of RadNet, Inc.
Opinion on Internal Control over Financial Reporting
We have audited RadNet, Inc. and subsidiaries’ internal control over financial reporting as of December 31, 2017, based on criteria established in Internal Control—Integrated Framework issued by the Committee of Sponsoring Organizations of the Treadway Commission (2013 framework), (the COSO criteria). In our opinion, because of the effect of the material weakness described below on the achievement of the objectives of the control criteria, RadNet, Inc. and subsidiaries’ (the Company) has not maintained effective internal control over financial reporting as of December 31, 2017, based on the COSO criteria.
A material weakness is a deficiency, or combination of deficiencies, in internal control over financial reporting, such that there is a reasonable possibility that a material misstatement of the company’s annual or interim financial statements will not be prevented or detected on a timely basis. The following material weakness has been identified and included in management’s assessment. Management has identified a material weakness in the operating effectiveness of certain information technology dependent manual controls related to the Company’s revenue and accounts receivables process.
We also have audited, in accordance with the standards of the Public Company Accounting Oversight Board (United States) (PCAOB), the 2017 consolidated balance sheets of the Company as of December 31, 2017 and 2016, the related consolidated statements of operations, comprehensive (loss) income, equity, and cash flows for each of the three years in the period ended December 31, 2017, and the related notes and financial statement schedule listed in the Index at Item 15(a)(2). This material weakness was considered in determining the nature, timing and extent of audit tests applied in our audit of the 2017 consolidated financial statements, and this report does not affect our report dated March 16, 2018, which expressed an unqualified opinion thereon.
Basis for Opinion
The Company’s management is responsible for maintaining effective internal control over financial reporting and for its assessment of the effectiveness of internal control over financial reporting included in the accompanying Management’s Report on Internal Control over Financial Reporting. Our responsibility is to express an opinion on the Company’s internal control over financial reporting based on our audit. We are a public accounting firm registered with the PCAOB and are required to be independent with respect to the Company in accordance with the U.S. federal securities laws and the applicable rules and regulations of the Securities and Exchange Commission and the PCAOB.
We conducted our audit in accordance with the standards of the PCAOB. Those standards require that we plan and perform the audit to obtain reasonable assurance about whether effective internal control over financial reporting was maintained in all material respects.
Our audit included obtaining an understanding of internal control over financial reporting, assessing the risk that a material weakness exists, testing and evaluating the design and operating effectiveness of internal control based on the assessed risk, and performing such other procedures as we considered necessary in the circumstances. We believe that our audit provides a reasonable basis for our opinion.
Definition and Limitations of Internal Control Over Financial Reporting
A company’s internal control over financial reporting is a process designed to provide reasonable assurance regarding the reliability of financial reporting and the preparation of financial statements for external purposes in accordance with generally accepted accounting principles. A company’s internal control over financial reporting includes those policies and procedures that (1) pertain to the maintenance of records that, in reasonable detail, accurately and fairly reflect the transactions and dispositions of the assets of the company; (2) provide reasonable assurance that transactions are recorded as necessary to permit preparation of financial statements in accordance with generally accepted accounting principles, and that receipts and expenditures of the company are being made only in accordance with authorizations of management and directors of the company; and (3) provide reasonable assurance regarding prevention or timely detection of unauthorized acquisition, use, or disposition of the company’s assets that could have a material effect on the financial statements.
Because of its inherent limitations, internal control over financial reporting may not prevent or detect misstatements. Also, projections of any evaluation of effectiveness to future periods are subject to the risk that controls may become inadequate because of changes in conditions, or that the degree of compliance with the policies or procedures may deteriorate.
/s/ Ernst & Young LLP
Los Angeles, California
March 16, 2018
| 89 |
| Item 9B. | Other Information. |
None
| Item 10. | Directors, Executive Officers and Corporate Governance |
The information required by this Item 10 will be included under the captions “Election of Directors,” “Executive Officers,” “Board of Directors and Corporate Governance,” and “Section 16(a) Beneficial Ownership Reporting Compliance” in our definitive Proxy Statement for the 2018 Annual Meeting of Stockholders to be filed with the SEC within 120 days after the end of our fiscal year (the “Proxy Statement”) and is incorporated herein by reference.
We have adopted a code of financial ethics applicable to our directors, officers and employees which is designed to deter wrongdoing and to promote:
| · | honest and ethical conduct; | |
| · | full, fair, accurate, timely and understandable disclosure in reports and documents that we file with the SEC and in our other public communications; | |
| · | compliance with applicable laws, rules and regulations, including insider trading compliance; and | |
| · | accountability for adherence to the code and prompt internal reporting of violations of the code, including illegal or unethical behavior regarding accounting or auditing practices. |
You may obtain a copy of our Code of Financial Ethics on our website at www.radnet.com under Investor Relations — Corporate Governance. The Audit Committee is responsible for reviewing the Code of Financial Ethics and amending as necessary. Any amendments will be disclosed on our website.
| Item 11. | Executive Compensation |
The information required by this Item 11 will be included under the captions “Compensation of Directors,” “Compensation of Executive Officers,” “Compensation Discussion and Analysis,” “Compensation Committee Interlocks and Insider Participation,” and “Compensation Committee Report “in the Proxy Statement and is incorporated herein by reference.
| Item 12. | Security Ownership of Certain Beneficial Owners and Management and Related Stockholder Matters |
The information required by this Item 12 will be included under the captions “Security Ownership of Certain Beneficial Owners and Management” and “Equity Compensation Plan Information” in the Proxy Statement and is incorporated herein by reference.
| Item 13. | Certain Relationships and Related Transactions, and Director Independence |
The information required by this Item 13 will be included under the captions “Certain Relationships and Related Party Transactions” and “Board of Directors and Corporate Governance” in the Proxy Statement and is incorporated herein by reference.
| Item 14. | Principal Accountant Fees and Services |
The information required by this Item 14 will be included under the caption “Independent Registered Public Accounting Firm Fees” in the Proxy Statement and is incorporated herein by reference.
| 90 |
| Item 15. Exhibits and Financial Statements Schedule | ||
| (a) Documents filed as part of this annual report on Form 10-K | ||
| (1) Financial Statements | Page No. | |
The following financial statements are included in this report |
||
| Report of Independent Registered Public Accounting Firm | 57 | |
| Consolidated Balance Sheets | 58 | |
| Consolidated Statements of Operations | 59 | |
| Consolidated Statements of Comprehensive (Loss) Income | 60 | |
| Consolidated Statements of Equity) | 61 | |
| Consolidated Statements of Cash Flows | 62 | |
| Notes to Consolidated Financial Statements | 64 to 86 | |
| (2) Financial Statement Schedules | ||
| The following financial statement schedules are filed herewith: | |
SCHEDULE II – VALUATION AND QUALIFYING ACCOUNTS
RADNET, INC. AND SUBSIDIARIES
| Balance at Beginning of Year | Additional Charges Against Income | Deductions from Reserve | Balance at End of Year | |||||||||||||
| Year Ended December 31, 2017 | ||||||||||||||||
| Accounts Receivable-Allowance for Bad Debts | $ | 20,674 | $ | 46,555 | $ | (32,585 | ) | $ | 34,644 | |||||||
| Year Ended December 31, 2016 | ||||||||||||||||
| Accounts Receivable-Allowance for Bad Debts | $ | 20,794 | $ | 45,387 | $ | (45,507 | ) | $ | 20,674 | |||||||
| Year Ended December 31, 2015 | ||||||||||||||||
| Accounts Receivable-Allowance for Bad Debts | $ | 15,109 | $ | 36,033 | $ | (30,348 | ) | $ | 20,794 | |||||||
All other schedules are omitted because they are not applicable or the required information is shown in the consolidated financial statements or notes thereto.
| 91 |
The following exhibits are filed herewith or incorporated by reference herein:
| 92 |
| 10.15 | Employment Agreement dated as of June 12, 1992 with Howard G. Berger, M.D. (incorporated by reference to exhibit filed with an amendment to Form 8-K report for June 12, 1992).* | ||
| 10.16 | Amendment to Employment Agreement dated January 30, 2004 with Howard G. Berger, M.D. (incorporated by reference to exhibit filed with Form 10-Q for the quarter ended January 31, 2004).* | ||
| 10.17 | Second Amendment to Employment Agreement dated November 16, 2015 with Howard G. Berger, M.D. (incorporated by reference to exhibit filed with Form 10-K on March 15, 2016). | ||
| 10.18 | Employment Agreement dated as of April 16, 2001 with Jeffrey L. Linden (incorporated by reference to exhibit filed with Form 10-K for the year ended October 31, 2001).* | ||
| 10.19 | Amendment to Employment Agreement dated January 30, 2004 with Jeffrey L. Linden (incorporated by reference to exhibit filed with Form 10-Q for the quarter ended January 31, 2004).* | ||
| 10.20 | Second Amendment to Employment Agreement dated November 16, 2015 with Jeffrey L. Linden (incorporated by reference to exhibit filed with Form 10-K on March 15, 2016). | ||
| 10.21 | Employment Agreement dated as of May 1, 2001 with Norman R. Hames (incorporated by reference to exhibit filed with Form 10-K for the year ended October 31, 2001).* | ||
| 10.22 | Amendment to Employment Agreement dated January 30, 2004 with Norman R. Hames (incorporated by reference to exhibit filed with Form 10-Q for the quarter ended January 31, 2004).* | ||
| 10.23 | Second Amendment to Employment Agreement dated November 16, 2015 with Norman R. Hames (incorporated by reference to exhibit filed with Form 10-K on March 15, 2016). | ||
| 10.24 | Employment Agreement with Mark Stolper effective January 1, 2009 (incorporated by reference to exhibit filed with Form 10-K for the year ended December 31, 2009).* | ||
| 10.25 | First Amendment to Employment Agreement dated November 16, 2015 with Mark Stolper (incorporated by reference to exhibit filed with Form 10-K on March 15, 2016).* |
| 93 |
| 10.26 | Retention Agreement with Stephen Forthuber dated November 15, 2006 (incorporated by reference to exhibit filed with Form 10-K/T for the year ended December 31, 2006).* | ||
| 10.27 | First Amendment to Retention Agreement dated November 16, 2015 with Stephen Forthuber (incorporated by reference to exhibit filed with Form 10-K on March 15, 2016).* | ||
| 10.28 | Amended and Restated Management and Service Agreement between Radnet Management, Inc. and Beverly Radiology Medical Group III dated January 1, 2004 (incorporated by reference to exhibit filed with Form 10-K for the year ended October 31, 2003). | ||
| 12.1 | Computation of Ratios of Earnings to Fixed Charges. | ||
| 21.1 | List of Subsidiaries. | ||
| 23.1 | Consent of Registered Independent Public Accounting Firm. | ||
| 24.1 | Power of Attorney (included on signature page attached hereto). | ||
| 31.1 | CEO Certification pursuant to Section 302. | ||
| 31.2 | CFO Certification pursuant to Section 302. | ||
| 32.1 | CEO Certification pursuant to Section 906. | ||
| 32.2 | |||
| 101.INS | XBRL Instance Document | ||
| 101.SCH | XBRL Schema Document | ||
| 101.CAL | XBRL Calculation Linkbase Document | ||
| 101.LAB | XBRL Label Linkbase Document | ||
| 101.PRE | XBRL Presentation Linkbase Document | ||
| 101.DEF | XBRL Definition Linkbase Document |
* Indicates management contract
or compensatory plan.
†Certain schedules to this exhibit have been omitted in accordance with Regulation S-K Item 601(b)(2). The company agrees to furnish supplementally a copy of all omitted schedules to the SEC upon its request.
| 94 |
SIGNATURES
Pursuant to the requirements of Section 13 or 15(d) of the Securities Exchange Act of 1934, the registrant has duly caused this report to be signed on its behalf by the undersigned, thereunto duly authorized.
| RADNET, INC. | |||
| Date: March 16, 2018 | /s/ HOWARD G. BERGER, M.D . | ||
| Howard G. Berger, M.D., President, | |||
| Chief Executive Officer and Director | |||
KNOW ALL PERSONS BY THESE PRESENTS, that each person whose signature appears below hereby severally constitutes and appoints Howard G. Berger, M.D. and Mark D. Stolper, and each of them, his true and lawful attorney-in-fact and agent, with full power of substitution and re-substitution for him and in his name, place and stead, in any and all capacities to sign any and all amendments to this report, and to file the same, with all exhibits thereto, and other documents in connection therewith, with the SEC, granting unto said attorney-in-fact and agents, and each of them, full power and authority to do and perform each and every act and thing requisite or necessary fully to all intents and purposes as he might or could do in person, hereby ratifying and confirming all that each said attorneys-in-fact and agents or any of them or their or his substitute or substitutes, may lawfully do or cause to be done by virtue hereof.
Pursuant to the requirements of the Securities Exchange Act of 1934, this report has been signed below by the following persons on behalf of registrant in the capacities and on the dates indicated.
| By | /s/ HOWARD G. BERGER, M.D. |
| Howard G. Berger, M.D., Director, Chief Executive Officer and President | |
| Date: March 16, 2018 | |
| By | /s/ MARVIN S. CADWELL |
| Marvin S. Cadwell, Director | |
| Date: March 16, 2018 | |
| By | /s/ JOHN V. CRUES, III, M.D. |
| John V. Crues, III, M.D., Director | |
| Date: March 16, 2018 | |
| By | /s/ NORMAN R. HAMES |
| Norman R. Hames, Director | |
| Date: March 16, 2018 | |
| By | /s/ DAVID L. SWARTZ |
David L. Swartz, Director
| |
| Date: March 16, 2018 | |
| By | /s/ LAWRENCE L. LEVITT |
| Lawrence L. Levitt, Director | |
| Date: March 16, 2018 | |
| By | /s/ MICHAEL L. SHERMAN, M.D. |
| Michael L. Sherman, M.D., Director | |
| Date: March 16, 2018 | |
| By | /s/ MARK D. STOLPER |
| Mark D. Stolper,Chief Financial Officer (Principal Accounting Officer) | |
| Date: March 16, 2018 | |
| 95 |
