Attached files
| file | filename |
|---|---|
| EX-23.1 - EXHIBIT 23.1 - Surgery Partners, Inc. | exhibit231consent-ey.htm |
| EX-10.21 - EXHIBIT 10.21 - Surgery Partners, Inc. | exhibit1021highwoodslease.htm |
| EX-31.1 - EXHIBIT 31.1 - Surgery Partners, Inc. | a201510-kexhibit311.htm |
| EX-32.1 - EXHIBIT 32.1 - Surgery Partners, Inc. | a201510-kexhibit321.htm |
| EX-31.2 - EXHIBIT 31.2 - Surgery Partners, Inc. | a201510-kexhibit312.htm |
| EX-32.2 - EXHIBIT 32.2 - Surgery Partners, Inc. | a201510-kexhibit322.htm |
| EX-23.2 - EXHIBIT 23.2 - Surgery Partners, Inc. | exhibit232consent-bdo.htm |
| EX-21.1 - EXHIBIT 21.1 - Surgery Partners, Inc. | exhibit211subsidiaries.htm |
UNITED STATES
SECURITIES AND EXCHANGE COMMISSION
Washington, D.C. 20549
________________________________________________________________
Form 10-K
(Mark One)
x | ANNUAL REPORT PURSUANT TO SECTION 13 OR 15(d) OF THE SECURITIES EXCHANGE ACT OF 1934 |
For the fiscal year ended December 31, 2015
or
o TRANSITION REPORT PURSUANT TO SECTION 13 OR 15(d) OF THE
SECURITIES EXCHANGE ACT OF 1934
Commission file number: 001-37576
Surgery Partners, Inc.
(Exact name of registrant as specified in its charter)
Delaware | 47-3620923 | |
(State or other jurisdiction of incorporation or organization) | (I.R.S. Employer Identification No.) | |
40 Burton Hills Boulevard, Suite 500
Nashville, Tennessee 37215
(Address of principal executive offices and zip code)
(615) 234-5900
(Registrant’s telephone number, including area code)
Securities registered pursuant to Section 12(b) of the Act:
Title of Class | Name of Exchange on Which Registered | |
Common Stock, par value $0.01 per share | NASDAQ Global Select Market | |
Securities registered pursuant to section 12(g) of the Act: None
Indicate by check mark if the registrant is a well-known seasoned issuer, as defined in Rule 405 of the Securities Act. Yes o No x
Indicate by check mark if the registrant is not required to file reports pursuant to Section 13 or Section 15(d) of the Act. Yes o No x
Indicate by check mark whether the registrant (1) has filed all reports required to be filed by Section 13 or 15(d) of the Securities Exchange Act of 1934 during the preceding 12 months (or for such shorter period that the registrant was required to file such reports), and (2) has been subject to such filing requirements for the past 90 days. Yes x No o
Indicate by check mark whether the registrant has submitted electronically and posted on its corporate Web site, if any, every Interactive Data File required to be submitted and posted pursuant to Rule 405 of Regulation S-T (§ 232.405 of this chapter) during the preceding 12 months (or for such shorter period that the registrant was required to submit and post such files). Yes x No o
Indicate by check mark if disclosure of delinquent filers pursuant to Item 405 of Regulation S-K (§ 229.405 of this chapter) is not contained herein, and will not be contained, to the best of registrant’s knowledge, in definitive proxy or information statements incorporated by reference in Part III of this Form 10-K or any amendment to this Form 10-K. Yes o No x
Indicate by check mark whether the registrant is a large accelerated filer, an accelerated filer, a non-accelerated filer, or a smaller reporting company. See the definitions of “large accelerated filer,” “accelerated filer” and “smaller reporting company” in Rule 12b-2 of the Exchange Act.
Large accelerated filer o | Accelerated filer o | |
Non-accelerated filer x | Smaller reporting company o | |
Indicate by check mark whether the registrant is a shell company (as defined in Rule 12b-2 of the Exchange Act). Yes o No x
The aggregate market value of the registrant’s voting and non-voting common equity held by non-affiliates of the registrant based on the closing price of the shares of common stock on The NASDAQ Stock Market on March 10, 2016, was $13.77. The registrant has provided this information as of March 10, 2016 because its common stock was not publicly traded as of the last business day of its most recently completed second fiscal quarter.
As of March 10, 2016, there were 48,156,990 shares of the registrant’s common stock outstanding.
DOCUMENTS INCORPORATED BY REFERENCE
Portions of the definitive proxy statement for the registrant’s annual stockholders’ meeting to be held May 3, 2016 are incorporated by reference into Part III of this report.
SURGERY PARTNERS, INC.
FORM 10-K
TABLE OF CONTENTS
Page | ||
Item 1. | Business | |
Item 1A. | Risk Factors | |
Item 1B. | Unresolved Staff Comments | |
Item 2. | Properties | |
Item 3. | Legal Proceedings | |
Item 4. | Mine Safety Disclosures | |
Item 5. | Market for Registrant’s Common Equity, Related Stockholder Matters and Issuer Purchases of Equity Securities | |
Item 6. | Selected Financial Data | |
Item 7. | Management's Discussion and Analysis of Financial Condition and Results of Operations | |
Item 7A. | Quantitative and Qualitative Disclosure About Market Risk | |
Item 8. | Financial Statements and Supplementary Data | |
Item 9. | Changes in and Disagreements With Accountants on Accounting and Financial Disclosure. | |
Item 9A. | Controls and Procedures | |
Item 9B. | Other Information | |
PART III | ||
Item 10. | Directors, Executive Officers and Corporate Governance | |
Item 11. | Executive Compensation. | |
Item 12. | Security Ownership of Certain Beneficial Owners and Management and Related Stockholder Matters | |
Item 13. | Certain Relationships and Related Transactions, and Director Independence | |
Item 14. | Principal Accounting Fees and Services | |
PART IV | ||
Item 15. | Exhibits, Financial Statement Schedules | |
Cautionary Note Regarding Forward-Looking Statements
This Annual Report on Form 10-K contains forward-looking statements based on our current expectations, estimates and assumptions about future events. All statements other than statements of current or historical fact contained in this report, including statements regarding our future financial position, business strategy, budgets, projected costs and plans and objectives of management for future operations, are forward-looking statements. The words “anticipate,” “believe,” “continue,” “estimate,” “expect,” “intend,” “may,” “plan,” “will” and similar expressions are generally intended to identify forward-looking statements.
These forward-looking statements involve various risks and uncertainties, some of which are beyond our control. Any or all of our forward-looking statements in this report may turn out to be wrong. We have based these forward-looking statements largely on our current expectations and projections about future events and financial trends that we believe may affect our financial condition, results of operations, business strategy and financial needs. They can be affected by inaccurate assumptions we might make or by known or unknown risks, uncertainties and assumptions, including the risks, uncertainties and assumptions described in Item 1A. “Risk Factors."
In light of these risks, uncertainties and assumptions, the forward-looking events and circumstances discussed in this report may not occur and actual results could differ materially from those anticipated or implied in the forward-looking statements. When you consider these forward-looking statements, you should keep in mind these risk factors and other cautionary statements in this report.
Our forward-looking statements speak only as of the date made. Other than as required by law, we undertake no obligation to publicly update or revise any forward-looking statements, whether as a result of new information, future events or otherwise.
The facilities, operations and businesses described in this Report are owned and operated, and management services provided, by distinct and indirect subsidiaries of Surgery Partners, Inc.
1
PART 1
Item 1. Business
Overview
We are a leading healthcare services company with a differentiated outpatient delivery model focused on providing high quality, cost effective solutions for surgical and related ancillary care in support of our patients and physicians. Founded in 2004 as a limited liability company, to own and operate ambulatory surgery centers (“ASCs”), render anesthesia services, and operate physician practices, we expanded our business in 2011 by acquiring NovaMed, Inc. and in 2014 we acquired Symbion Holdings Corporation (“Symbion”). Further, we completed an initial public offering ("IPO") in October 2015. We are now one of the largest and fastest growing surgical services businesses in the country.
As of December 31, 2015, we owned or operated primarily in partnership with physicians, a portfolio of 101 surgical facilities comprised of 96 ASCs and five surgical hospitals (“surgical hospitals,” and together with ASCs referred to as “surgical facilities” or “facilities”) across 29 states and we owned a majority interest in 72 of these facilities. Additionally, approximately 72% of these facilities were multi-specialty focused. During 2015, over 4,000 physicians provided services to over 500,000 patients in our surgical facilities generating $879.7 million in revenue.
Our innovative strategy provides a suite of targeted and complementary ancillary services in support of our patients and physicians. This suite of ancillary services is comprised of a diagnostic laboratory, multi-specialty physician practices, urgent care facilities, anesthesia services, optical services and specialty pharmacy services (our “ancillary services”). We believe this approach improves the quality of care provided to our patients, results in superior clinical outcomes and allows us to realize the revenue associated with these ancillary services that are otherwise outsourced to unrelated third-party providers.
Our patient- and physician-centric culture, our commitment to high quality care, our differentiated approach to physician engagement and our suite of complementary ancillary services have been instrumental to our growth. These areas of focus, along with investments in systems and processes, strategic acquisitions and favorable industry trends, have all contributed to our industry leading track record of growth.
Our Growth Strategies
Our differentiated operating model employs a multifaceted strategy to grow revenue, earnings and cash flow. We believe the following are key components to this strategy:
• | Deliver Outstanding Patient Care and Clinical Outcomes; |
• | Expand Ancillary Services Across Our National Platform; |
• | Continue to Execute and Expand Upon our Physician Engagement Strategy in Attractive Markets; |
• | Drive Organic Growth at Existing Facilities through Targeted Physician Recruitment, Service Line Expansion and Implementing our Efficient Operating Model; |
• | Continue our Disciplined Acquisition Strategy; and |
• | Introduce New Service Offerings to Provide a More Comprehensive Continuum of Care. |
Deliver Outstanding Patient Care and Clinical Outcomes
Rising consumerism in healthcare services, along with greater transparency in outcomes data, is expected to empower patients to make more informed healthcare decisions. We expect this trend will significantly benefit overall outpatient surgical facility case volume due to the clinical and cost benefits that surgical facilities offer relative to alternative sites of care such as outpatient departments of acute care hospitals. Our culture of delivering high quality care and achieving superior levels of patient and physician satisfaction are keys to success and integral to our ability to continue to be a preferred site of care for surgical and related ancillary services. For example, on average, our facilities exceeded industry averages for each of CMS’ 2015 ASCQR Program’s five key core ambulatory surgery center quality measures. We believe the industry wide implementation of CMS’ ASCQR Program will further differentiate our facilities as high quality locations based on the strength of our performance across the key quality measure providing an additional opportunity to capture market share.
We have established a dedicated clinical team of experienced professionals focused on ensuring that the highest level of quality is targeted throughout our platform. This team is responsible for maintaining best practices across our platform. They lead numerous quality initiatives such as inspection readiness, policies and procedures, compliance and clinical training. Our proprietary quality reporting system generates detailed case-level analytics that we use to measure our clinical results on a physician-by-physician basis against a robust set of quality metrics, providing opportunities to quickly and effectively identify areas for improvement, implement initiatives and track progress. Additionally, our complementary ancillary services strategy allows us to provide greater coordination over the provision of these services.
Expand Ancillary Services Across Our National Platform
Our differentiated business strategy and established infrastructure allow us to retain ancillary service revenue that is otherwise outsourced to unrelated third-party providers. We have a successful track record of executing on our strategy of incorporating ancillary services throughout our surgical facilities portfolio, which has been a key contributor to our strong same-facility revenue growth of approximately 10.7% in 2015 and annual average of approximately 8.0% from 2012 to 2014, on a pro forma basis assuming the inclusion of the Symbion transaction. As an example, over the course of four years following the acquisition of one of our other surgical hospitals, capacity was expanded via the addition of multiple operating rooms, a state of the art radiation oncology center, several oncology practices, multiple urgent care facilities and several high volume physicians.
1
While many of our ancillary service lines have been established and growing for a number of years, we see significant growth opportunities from further penetration of these services across our national portfolio. We expect the introduction of more recently added service offerings will further benefit our overall growth profile as these services are rolled out to our employed and partnered physicians.
Continue to Execute and Expand Upon our Physician Engagement Strategy in Attractive Markets
In addition to our network of over 4,000 physicians who provided services to patients in our facilities in 2015, we have a successful track record of owning and operating physician groups dating back to our inception. We believe our flexible approach to physician engagement, including employing, partnering and affiliating with physicians, best allows us to drive high quality patient care, efficiently utilize the capacity in our facilities, implement our complementary ancillary services strategy and drive organic growth. Through our recruiting efforts and capital-efficient acquisitions, as of December 31, 2015, we had 46 owned or operated physician practices comprised of over 100 physicians across multiple surgical specialties (including otolaryngology ("ENT"), gastroenterology ("GI"), general surgery, ophthalmology, orthopedics, cardiology and pain management) complementing our surgical facilities. Our infrastructure, including scheduling, billing and collections, regulatory compliance, staffing and analytics, among other services, facilitates significant improvement in efficiency and performance of our practices.
Our physician engagement strategy also benefits our existing physician partners. We focus on strategically recruiting physicians and acquiring high quality physician practices complementary to our existing surgical facilities to better utilize the capacity in our facilities. We believe our ability to implement this strategy improves our relationships with our physician partners and is a powerful differentiator for our platform.
We also believe there is significant opportunity to accelerate our physician engagement strategy. We believe there is significant opportunity to continue to add practices across multiple specialties in our existing markets to support our surgical facilities, and believe there will be additional opportunities as we look to expand our presence in new markets.
Drive Organic Growth at Existing Facilities through Targeted Physician Recruitment, Service Line Expansion and Implementing our Efficient Operating Model
We have achieved industry leading organic growth through our differentiated operating strategy. We work closely with our physicians to achieve greater efficiency through optimal scheduling and facility utilization, reduction in administrative costs, and better procurement and management of supply utilization. As a complement to our initiatives to drive organic growth, we have executed and will continue to execute on select, strategic service line expansion opportunities to capture and address patient needs in our markets, exemplified by our successful introduction of orthopedic and spine services in legacy NovaMed facilities.
Continue our Disciplined Acquisition Strategy
We have historically pursued, and successfully executed, a disciplined acquisition strategy to diversify our geographic footprint and revenue mix, while driving greater scale. Our scale has, in part, enabled our significant investment in resources and infrastructure to drive growth, improve quality and enhance efficiencies. Acquiring facilities has been a core component of our strategy since inception. We have a long track record of meticulously and methodically identifying, evaluating, executing and integrating accretive and value enhancing acquisitions. Through these acquisitions, we have achieved meaningful cost and revenue synergies, enhancing the value of our acquired facilities and meaningfully reducing the effective purchase multiple paid.
Surgical Facilities
With the top ten providers in the industry operating less than 20% of the 5,400 Medicare-certified ASCs in the United States, we believe there is a significant opportunity to continue our strategy of consolidating in a highly fragmented market, thus expanding our footprint.
We have a dedicated business development team focused on identifying and managing our pipeline of potential acquisition opportunities that closely coordinates efforts with our dedicated physician recruitment team. We believe our operating strategy is a powerful differentiator when physicians are considering an affiliation with our Company. We plan to continue acquiring facilities in partnership with high quality physicians and physician groups in both current and new markets. The common denominator to an attractive acquisition target is the potential to leverage our infrastructure and expertise to grow case volume, enhance surgical specialty mix and revenue-per-case and improve facility performance. We have a strong track record of successfully integrating acquisitions and achieving meaningful cost and revenue synergies to enhance the value of our acquired facilities and meaningfully reduce the effective purchase multiple paid.
In addition to increasing scale to enhance operating leverage and broadening our footprint to further diversify our geographic presence, facility acquisitions also serve as platforms for entering new markets. Each facility added to our platform establishes multiple physician relationships. These relationships provide opportunities to market our ancillary services in a focused manner as well as to supplement the newly acquired facility with new physician practices focused on complementary surgical specialties.
Ancillary Services
We also expect to grow our Company by acquiring businesses which provide select ancillary services that complement our surgical facilities and support our physicians. Our differentiated and capital-efficient ancillary services strategy substantially broadens our pool of potential acquisitions beyond physician and surgical facility opportunities. This broader set of opportunities enables us to be even more selective in our investments and focus our efforts on high quality targets with differentiated value creation potential. Our ancillary services strategy also enhances our ability to enter new markets by supplementing typical surgical facility revenue with ancillary revenue otherwise outsourced to unrelated third-party providers. By capturing ancillary services revenue in our newly acquired facilities, it also allows us to achieve lower effective purchase multiples. Additionally, our strategy has the potential to facilitate our surgical facility business development effort as we begin marketing ancillary service offerings to currently unaffiliated physicians.
2
We believe our experience executing on a variety of acquisition types enables us to continue the successful employment of our disciplined acquisition strategy and continue to make selective acquisitions to drive growth. Taken together, our differentiated ancillary services strategy not only increases our target acquisition opportunity set, but capturing ancillary services revenue in our newly acquired facilities allows us to achieve lower effective purchase multiples.
Introduce New Service Offerings to Provide a More Comprehensive Continuum of Care
We are committed to building a differentiated outpatient delivery model to better serve the needs of patients, physicians and payors. In addition to our current suite of services, we see significant opportunity to better position our Company in an evolving healthcare landscape and accelerate growth through the expansion of services supporting our physicians. We believe offering services across the continuum of outpatient care will better position our Company for evolving reimbursement structures, further support our physicians, enhance the quality of care for our patients and drive exceptional organic growth. In addition to new revenue generated from procedures in our facilities, we also believe certain service offerings could broaden the types of procedures we can offer in our surgical facilities. For instance, providing patients with rehabilitation and physical therapy services would allow our ASCs to offer more complex spine and orthopedic procedures that typically occur in a hospital setting.
Industry Overview
Surgical Facilities
For many years, government programs, private insurance companies, managed care organizations and self-insured employers have implemented cost containment measures intended to limit the growth of healthcare expenditures. These cost-containment measures, together with technological advances, have contributed to the significant shift in the delivery of healthcare services away from traditional inpatient hospital settings to more cost effective surgical facilities, including ASCs and surgical hospitals. ASCs have been viewed as a successful way to increase efficiency by improving the quality of, and access to, healthcare and increasing patient satisfaction, while simultaneously reducing costs. Surgical hospitals are larger than a typical ASC and include inpatient hospital rooms and, in some cases, a limited scope emergency department. The offerings in a surgical hospital also include acute care services, such as diagnostic imaging, pharmacy, laboratory, obstetrics, physical therapy, oncology and wound care. As the focus on containing healthcare expenditures grows in response to the Affordable Care Act, surgical procedures are expected to continue to shift dramatically from inpatient to outpatient settings.
Increasing Demand for Surgical Procedures in Outpatient Settings
According to the Centers for Medicare and Medicaid Services ("CMS"), the percentage share of outpatient surgery has increased from 15% in 1985 to 77% in 2012. This shift has occurred for a variety of reasons, including an increase in the number of procedures that can be performed safely in an outpatient environment, the high quality outcomes at lower cost of the outpatient setting relative to the inpatient setting, patient preference due to increased convenience, physician preference due to increased efficiency, patient and payor preference due to the lower cost setting.
Advancements in Medical Technology
New technologies, faster acting and more effective anesthesia and less invasive surgical techniques have increased the number of procedures that can be performed in an ambulatory surgery center. Lasers, arthroscopy, enhanced endoscopic techniques and fiber optics have reduced the trauma and recovery time for patients. Advances in the use of anesthesia have shortened recovery time by minimizing postoperative side effects such as nausea and drowsiness. Procedures that only a few years ago required major incisions, long-acting anesthetics and extended convalescence can now be performed through closed techniques utilizing short-acting anesthetics and with minimal recovery time. Of these new techniques and technologies, more complex surgical procedures that previously were performed only on an inpatient basis can now be performed in an ambulatory surgery center. Medicare, often the benchmark for other insurance plans, has approved approximately 3,400 procedures to be performed in a surgery center. We believe that ASCs are likely to receive continued regulatory support as more cost effective alternative surgical procedures can be performed in the ambulatory surgery center setting compared to traditional, in-hospital care.
Improved Outcomes and Convenience for Patients at Lower Costs
ASCs provide outstanding patient safety and superior clinical outcomes due to the focus and specialization of a center’s professional staff. ASCs have lower rates of inpatient hospital admission, hospital-acquired infections and mortality than hospital outpatient surgery departments. Finally, ASCs often offer patients greater convenience than hospital outpatient departments with more convenient locations and ability to schedule surgery.
Compelling Value Proposition for Physicians
Many physicians prefer surgical facilities over general acute care hospitals because of greater scheduling flexibility, more consistent nurse staffing and faster turnaround times between cases, which allows physicians to increase the number of surgical procedures they can perform in a given period of time. Due to the non-emergency, elective nature of most ambulatory surgery center procedures, physicians’ schedules are rarely interrupted, enabling physicians to more efficiently secure preferred blocks of time in the operating room. This is in contrast to acute care hospitals, where medical emergencies often demand the unplanned use of operating rooms and result in the postponement or delay of scheduled surgical procedures, disrupting physicians’ practices and inconveniencing patients. Physicians are also increasingly interested in pursuing partnerships with other physicians in order to gain greater stability, access to scaled clinical and operating systems and a pathway to participating in new payment models. These partnerships help relieve physicians of the financial and administrative burdens resulting from uncertainty regarding reimbursement and healthcare legislation. In addition, our in-house ancillary services provide support for our surgical specialists who are then relieved from the additional burden of coordinating third-party support services.
Reduced Costs for Payors
3
There has been an increased focus on controlling the growth of healthcare expenditures and as a result, cost containment measures have contributed to the significant shift in the delivery of healthcare services away from traditional inpatient hospitals to more cost effective alternate sites, including ASCs. Government programs, private insurance companies, managed care organizations and self-insured employers have implemented these cost containment measures to limit increases in healthcare expenditures, including procedure reimbursement. In addition, as patients are facing increased financial responsibility through higher co-pays and deductibles, there is increased consumerism as patients are encouraged to find more cost effective options for their healthcare. Surgery performed at an ambulatory surgery center is generally less expensive than hospital-based outpatient surgery because of lower facility development costs, more efficient staffing and space utilization, a specialized operating environment focused on quality of care and aligned incentives for physicians and ASCs to control costs and improve efficiency. A procedure in an ambulatory surgery center costs, on average, approximately 73% of what the same procedure costs when performed in a hospital surgery department, according to an Ambulatory Surgery Center Association analysis of 2014 Medicare fee schedules. These cost savings will continue to incentivize constituents across the healthcare continuum to shift the delivery of surgical procedures to ASCs.
Ancillary Services
A broad market of ancillary and related services facilitates operational efficiencies for physicians. In the areas of specialty where our physicians are focused, the associated ancillary services include a diagnostic laboratory, multi-specialty physician practices, urgent care facilities, anesthesia services, optical services and specialty pharmacy services. These industries represent approximately $127 billion of annual healthcare expenditures and provide a broad opportunity for us to expand our Ancillary Services outreach to support patients and physicians.
Operations
For more detailed financial information regarding our Company, see the consolidated financial statements and the accompanying notes, which are attached at Page F-1 to this Annual Report on Form 10-K. As described below, we have three reportable operating segments. Financial information regarding our reportable segments is found in Note 15 to our consolidated financial statements that are attached beginning on Page F-1 of this Annual Report on Form 10-K.
We operate in three lines of business throughout the United States: surgical facility services, ancillary services and optical services.
Surgical Facility Services Segment: Our surgical facility services segment consists of the operation of ASCs and surgical hospitals, and includes our anesthesia services. Our surgical facilities primarily provide non-emergency surgical procedures across many specialties, including, among others, ENT, GI, general surgery, ophthalmology, orthopedics, cardiology and pain management.
Ancillary Services Segment: Our ancillary services segment consists of a diagnostic laboratory, a specialty pharmacy and multi-specialty physician practices. These physician practices include our owned and operated physician practices pursuant to long-term management service agreements.
Optical Services Segment: Our optical services segment consists of an optical laboratory, an optical products group purchasing organization and a marketing business. Our optical laboratory manufactures eyewear, while our optical products purchasing organization negotiates volume buying discounts with optical product manufacturers.
Surgical Facility Services Segment
Surgical Facility Operations
As of December 31, 2015, we owned (primarily with physician investors or healthcare systems) or operated 101 surgical facilities including five that are licensed as hospitals.
Our typical ambulatory surgery center is a free-standing facility for planned, surgical procedures performed on an outpatient basis on patients not requiring hospitalization and for whom an overnight stay is not expected after surgery. Each center typically has one to four operating or procedure rooms with areas for reception, pre-operative care, recovery and administration. The average facility size is 8,000 to 12,000 square feet. Centers are specifically tailored to meet the needs of physician-partners and their specialties. Of our 96 ASCs, 94 utilize leased real property. We expect to be able to renew or replace a substantial majority of these leases on substantially similar terms. The staff of our ASCs generally includes a center administrator, registered nurses, operating room technicians, as well as other administrative staff.
Our surgical hospitals are generally larger than our ASCs and include inpatient hospital rooms and, in two cases, a limited scope emergency department. Our surgical hospitals also provide ancillary services such as diagnostic imaging, pharmacy, laboratory, obstetrics, physical therapy, oncology and wound care.
As of December 31, 2015, we provided anesthesia in 34 of our 101 surgical facilities. These services are provided by our certified registered nurse anesthetists or physician anesthesiologists. These employment or contract relationships vary by state to comply with corporate practice of medicine laws.
Each facility is licensed by the state and certified as a provider under federal programs. The facilities are available for use only by licensed physicians performing surgical procedures. We ensure consistent quality of care by assisting our partners with establishing and maintaining accreditation with the Accreditation Association for Ambulatory Health Care (“AAAHC”) or the Joint Commission, the accrediting bodies for the ambulatory surgery center and hospital industries. As of December 31, 2015, 86 of our 101 surgical facilities were accredited by either AAAHC or the Joint Commission, and the remainder were in the process of obtaining accreditation.
We operate both multi-specialty and single-specialty facilities. In multi-specialty facilities, a variety of surgical procedures are performed, including: ENT, GI, general surgery, ophthalmology, orthopedics, cardiology and pain management. We have diversified our
4
facility procedure mix by strategically introducing select specialties that will complement existing facilities. In many cases, we keep certain facilities as single-specialty where it suits an individual facility or market demand.
Our surgical facilities are generally located in close proximity to physicians’ offices. We provide each of our surgical facilities with a full range of financial, marketing and operating services. For example, our regional managed care directors assist the local management team at each of our surgical facilities in developing relationships with managed care providers and negotiating managed care contracts.
Surgical Facility Ownership Structure
We own and operate our surgical facilities through partnerships or limited liability companies with physicians, physician groups and healthcare systems. One of our wholly owned subsidiaries typically serves as the general partner or managing member of our surgical facilities. We generally seek to own a majority interest in our surgical facilities, or otherwise have sufficient control over the facilities to be able to consolidate the financial results of operations of the facilities with ours. In some instances, we will acquire ownership in a surgical facility with the prior owners retaining ownership, and, in some cases, we offer new ownership to other physicians or healthcare systems. We hold majority ownership in 72 of the 101 surgical facilities in which we own an interest. We provide intercompany loans to our consolidated facilities which often are secured by a pledge of assets of the partnership or limited liability company. We also have a management agreement with the majority of our surgical facilities, under which we provide day-to-day management services for a management fee, which is typically equal to a percentage of the revenues of the facility.
Each of the partnerships and limited liability companies through which we own and operate our surgical facilities is governed by a partnership or operating agreement. These partnership and operating agreements typically provide, among other things, for voting rights and limited transfer of ownership. The partnership and operating agreements also provide for the distribution of available cash to the owners. In addition, the agreements typically restrict the physician owners from owning an interest in a competing surgical facility during the period in which the physician owns an interest in our surgical facility and for one year after that period. The partnership and operating agreements for our surgical facilities may provide that the facilities will purchase all of the physicians’ ownership if certain adverse regulatory events occur, such as it becoming illegal for the physicians to own an interest in a surgical facility, refer patients to a surgical facility or receive cash distributions from a surgical facility. The purchase price that we would be required to pay for the ownership is based on predetermined formulas, typically either a multiple of the surgical facility’s EBITDA, as defined in our partnership and operating agreements, or the fair market value of the ownership as determined by an independent third-party appraisal. Some of these agreements require us to make a good faith effort to restructure our relationships with the physician investors in a manner that preserves the economic terms of the relationship prior to purchasing these interests. In certain circumstances, we have the right to purchase a physician’s ownership, including upon a physician’s breach of the restriction on ownership provisions of a partnership or operating agreement. In some cases, we have the right to require the physician owners to purchase our ownership in the event our management agreement with a surgical facility is terminated.
Surgical Facilities
The following table sets forth information regarding each of our surgical facilities as of December 31, 2015:
Facility / State | City | Number of Operating Rooms | Number of Treatment Rooms | Surgery Partners Percentage Ownership | ||||||
Alabama | ||||||||||
Birmingham Surgery Center | Birmingham | 5 | 3 | 37 | % | |||||
Arkansas | ||||||||||
NovaMed Surgery Center of Jonesboro | Jonesboro | 2 | 1 | 51 | % | |||||
California | ||||||||||
Specialty Surgical Center of Beverly Hills / Brighton Way | Beverly Hills | 3 | 1 | 26 | % | |||||
Specialty Surgical Center of Beverly Hills / Wilshire Boulevard | Beverly Hills | 4 | 2 | 27 | % | |||||
Specialty Surgical Center of Encino | Encino | 4 | 2 | 34 | % | |||||
Specialty Surgical Center of Irvine | Irvine | 4 | 1 | 52 | % | |||||
Specialty Surgical Center of Thousand Oaks | Westlake Village | 4 | 2 | 20 | % | (1) | ||||
Center for Outpatient Surgery | Whittier | 2 | 2 | 64 | % | |||||
Colorado | ||||||||||
United Ambulatory Surgery Center | Colorado Springs | 1 | 0 | 60 | % | |||||
NovaMed Surgery Center of Denver | Denver | 1 | 1 | 51 | % | |||||
Animas Surgical Hospital | Durango | 4 | 1 | 69 | % | (2) | ||||
12 Hospital Rooms | ||||||||||
Minimally Invasive Spine Institute | Lafayette | 2 | 1 | 40 | % | |||||
Delaware | ||||||||||
Delaware Outpatient Center for Surgery | Newark | 4 | 4 | 51 | % | |||||
5
Facility / State | City | Number of Operating Rooms | Number of Treatment Rooms | Surgery Partners Percentage Ownership | ||||||
Florida | ||||||||||
Cape Coral Surgery Center | Cape Coral | 5 | 7 | 80 | % | |||||
Lee Island Coast Surgery Center | Fort Myers | 5 | 3 | 43 | % | |||||
Laser and Outpatient Surgery Center | Gainesville | 2 | 1 | 51 | % | |||||
Jacksonville Beach Surgery Center | Jacksonville | 4 | 1 | 81 | % | |||||
Lake Mary Surgery Center | Lake Mary | 2 | 1 | 63 | % | |||||
Lake Worth Surgical Center | Lake Worth | 3 | 1 | 87 | % | |||||
Palm Beach Outpatient Surgical Center | Lake Worth | 2 | 1 | 60 | % | |||||
Tampa Bay Regional Surgery Center | Largo | 1 | 2 | 51 | % | |||||
West Bay Surgery Center | Largo | 4 | 4 | 51 | % | |||||
Park Place Surgery Center | Maitland | 2 | 1 | 94 | % | |||||
Space Coast Surgery Center | Merritt Island | 1 | 0 | 100 | % | |||||
The Gables Surgical Center | Miami | 2 | 0 | 76 | % | |||||
Miami Surgical Center | Miami | 6 | 1 | 58 | % | |||||
Suncoast Surgery Center | New Port Richey | 2 | 1 | 25 | % | (5) | ||||
The Surgery Center of Ocala | Ocala | 4 | 2 | 41 | % | |||||
Orange City Surgery Center | Orange City | 2 | 1 | 51 | % | |||||
Downtown Surgery Center | Orlando | 4 | 1 | 61 | % | |||||
Millenia Surgery Center | Orlando | 2 | 0 | 60 | % | |||||
Sarasota Ambulatory Surgery Center | Sarasota | 2 | 0 | 66 | % | |||||
Armenia Ambulatory Surgery Center | Tampa | 2 | 4 | 94 | % | |||||
Westchase Surgery Center | Tampa | 4 | 0 | 51 | % | |||||
New Tampa Surgery Center | Wesley Chapel | 2 | 2 | 61 | % | |||||
Georgia | ||||||||||
Atlanta Eye Surgery Center | Atlanta | 2 | 1 | 100 | % | |||||
Premier Surgery Center | Brunswick | 3 | 0 | 63 | % | |||||
Coastal Pain Centers | Brunswick | 1 | 0 | 15 | % | (5) | ||||
The Surgery Center | Columbus | 4 | 2 | 63 | % | |||||
Coastal Pain Centers | Vidalia | 1 | 0 | 15 | % | (5) | ||||
Hawaii | ||||||||||
Honolulu Spine Center | Honolulu | 2 | 0 | 41 | % | |||||
Idaho | ||||||||||
Mountain View Hospital | Idaho Falls | 10 | 2 | 62 | % | (2) | ||||
43 hospital rooms | ||||||||||
Illinois | ||||||||||
NovaMed Eye Surgery Center -Northshore | Chicago | 1 | 1 | 67 | % | |||||
Eyes of Illinois Surgery Center | Maryville | 1 | 1 | 48 | % | (5) | ||||
Center for Reconstructive Surgery | Oak Lawn | 4 | 0 | 57 | % | |||||
NovaMed Surgery Center of River Forest | River Forest | 2 | 0 | 51 | % | |||||
Valley Ambulatory Surgery Center | St. Charles | 7 | 1 | 44 | % | |||||
Indiana | ||||||||||
Surgical Center of New Albany | New Albany | 3 | 1 | 53 | % | |||||
NovaMed Eye Surgery Center of New Albany | New Albany | 2 | 1 | 51 | % | |||||
Kansas | ||||||||||
NovaMed Eye Surgery Center of Overland Park | Overland Park | 4 | 1 | 51 | % | |||||
Cypress Surgery Center | Wichita | 6 | 5 | 52 | % | |||||
Kentucky | ||||||||||
DuPont Surgery Center | Louisville | 5 | 0 | 70 | % | |||||
Louisiana | ||||||||||
6
Facility / State | City | Number of Operating Rooms | Number of Treatment Rooms | Surgery Partners Percentage Ownership | ||||||
Interventional Pain Management Center | Baton Rouge | 4 | 0 | 51 | % | |||||
Physicians Medical Center | Houma | 5 | 8 | 57 | % | (2) | ||||
30 hospital rooms | ||||||||||
Michigan | ||||||||||
The Cataract Specialty Surgical Center | Berkley | 2 | 1 | 51 | % | |||||
Surgery Center of Kalamazoo | Portage | 4 | 0 | 64 | % | |||||
Mississippi | ||||||||||
DeSoto Surgery Center | DeSoto | 2 | 1 | — | % | (3) | ||||
Physicians Outpatient Center | Oxford | 4 | 2 | — | % | (3) | ||||
Missouri | ||||||||||
St. Louis Women's Surgery Center | Ballwin | 3 | 0 | 62 | % | |||||
Orthopedic Ambulatory Surgery Center of Chesterfield | Chesterfield | 4 | 1 | 12 | % | (1) | ||||
Timberlake Surgery Center | Chesterfield | 4 | 1 | 62 | % | |||||
NovaMed Eye Surgery Center of North County | Florissant | 1 | 0 | 100 | % | |||||
Central Missouri Medical Park Surgical Center | Jefferson City | 4 | 1 | 40 | % | |||||
Blue Ridge Surgical Center | Kansas City | 2 | 1 | 51 | % | |||||
St. Peters Ambulatory Surgery Center | St. Peters | 2 | 0 | 54 | % | |||||
St. Louis Spine and Orthopedic Surgery Center | Town and Country | 3 | 1 | 56 | % | |||||
NovaMed Surgery Center of Warrensburg | Warrensburg | 2 | 1 | 51 | % | |||||
Montana | ||||||||||
Great Falls Clinic Medical Center | Great Falls | 3 | 20 hospital rooms | 50 | % | (2) | ||||
Great Falls Clinic Surgery Center | Great Falls | 3 | 2 | 93 | % | |||||
Nebraska | ||||||||||
Surgery Center of Fremont | Fremont | 1 | 1 | 51 | % | |||||
New Hampshire | ||||||||||
New Hampshire Eye SurgiCenter | Bedford | 1 | 0 | 67 | % | |||||
Nashua Eye Surgery Center | Nashua | 2 | 0 | 51 | % | |||||
North Carolina | ||||||||||
Orthopaedic Surgery Center of Asheville | Asheville | 3 | 0 | 54 | % | |||||
Wilmington SurgCare | Wilmington | 7 | 3 | 72 | % | |||||
North Dakota | ||||||||||
Grand Forks Surgery Center | Grand Forks | 1 | 0 | 51 | % | |||||
Ohio | ||||||||||
Surgery Center of Sandusky | Sandusky | 1 | 1 | 60 | % | |||||
Valley Surgery Center | Steubenville | 3 | 1 | 34 | % | |||||
Pennsylvania | ||||||||||
The Center for Specialized Surgery | Bethlehem | 2 | 2 | 63 | % | |||||
Village SurgiCenter of Erie | Erie | 5 | 1 | 71 | % | |||||
Crozer Keystone Surgery Center at Haverford | Haverford | 5 | 1 | — | % | (1)(4) | ||||
Physicians Surgical Center | Lebanon | 3 | 1 | 67 | % | |||||
Rhode Island | ||||||||||
East Greenwich Endoscopy Center | East Greenwich | 0 | 4 | 45 | % | |||||
East Bay Endoscopy Center | Portsmouth | 0 | 1 | 75 | % | |||||
Bayside Endoscopy Center | Providence | 0 | 6 | 75 | % | |||||
Ocean State Endoscopy Center | Providence | 0 | 3 | 54 | % | |||||
Tennessee | ||||||||||
Renaissance Surgery Center | Bristol | 2 | 1 | 46 | % | |||||
NovaMed Surgery Center of Chattanooga | Chattanooga | 1 | 1 | 52 | % | |||||
7
Facility / State | City | Number of Operating Rooms | Number of Treatment Rooms | Surgery Partners Percentage Ownership | ||||||
The Surgery Center of Cleveland | Cleveland | 2 | 1 | 64 | % | |||||
Cool Springs Surgery Center | Franklin | 5 | 2 | 36 | % | (1) | ||||
Germantown Surgery Center | Germantown | 6 | 1 | — | % | (3) | ||||
Physicians Surgery Center | Jackson | 4 | 1 | 20 | % | (1) | ||||
East Memphis Surgery Center | Memphis | 6 | 2 | — | % | (3) | ||||
UroCenter | Memphis | 3 | 0 | — | % | (3) | ||||
Union City Surgery Center | Union City | 2 | 1 | — | % | (3) | ||||
Texas | ||||||||||
Lubbock Heart and Surgical Hospital | Lubbock | 10 | 8 | 60 | % | (2) | ||||
74 hospital rooms | ||||||||||
American Surgery Center of South Texas | San Antonio | 2 | 1 | 65 | % | |||||
Texarkana Surgery Center | Texarkana | 4 | 3 | 58 | % | |||||
The Cataract Center of East Texas | Tyler | 2 | 0 | 60 | % | |||||
Washington | ||||||||||
Bellingham Ambulatory Surgery Center | Bellingham | 3 | 0 | 79 | % | |||||
Microsurgical Spine Center | Puyallup | 1 | 1 | 60 | % | |||||
Wisconsin | ||||||||||
NovaMed Surgery Center of Madison | Madison | 2 | 0 | 51 | % | |||||
(1) | We do not consolidate this surgical facility for financial reporting purposes. |
(2) | This surgical facility is licensed as a hospital. |
(3) | We manage this surgical facility, but do not have ownership in the facility. |
(4) | We hold a 48% non-consolidating ownership interest in a management service company that provides various management services to this surgical facility. We also have a management services agreement with the management service company. |
(5) | This facility is a variable interest entity and is consolidated for financial reporting purposes. |
Strategic Relationships
When attractive opportunities arise, we may develop, acquire or operate surgical facilities through strategic relationships with healthcare systems and other healthcare providers. We believe that forming a relationship with a healthcare system can enhance our ability to attract physicians and access managed care contracts for our surgical facilities in that market.
The strategic relationships through which we own and operate surgical facilities are governed by partnership and operating agreements that are generally comparable to the partnership and operating agreements of the other surgical facilities in which we own an interest. The primary difference between the structure of these strategic relationships and the other surgical facilities in which we hold ownership is that, in these strategic relationships, a healthcare system holds ownership in the surgical facility, in addition to physician investors. For a general description of the terms of our partnership and operating agreements, see “—Operations—Surgical Facility Services Segment—Surgical Facility Ownership Structure.” In each of these strategic relationships, we also have entered into a management agreement under which we provide day-to-day management services for a management fee equal to a percentage of the revenues of the surgical facility. The terms of those management agreements are comparable to the terms of our management agreements with other surgical facilities in which we own an interest.
As of December 31, 2015, we have relationships with eight healthcare systems relating to 12 ASC's. These healthcare systems include:
▪ | Baptist Memorial Health Services, Inc. (“Baptist Memorial”), for which we manage six surgical facilities in Memphis, Tennessee and surrounding areas; |
▪ | Crozer-Keystone Health Systems, for which we manage and operate a surgical facility in Havertown, Pennsylvania; |
▪ | Lee Health Ventures, with which we own and operate a surgical facility in Ft. Myers, Florida; |
▪ | Munroe Regional Health Systems, with which we own and operate a surgical facility in Ocala, Florida; |
▪ | Trinity Health System, with which we own and operate a surgical facility in Steubenville, Ohio; |
▪ | UCLA Health, with which we own and operate a surgical facility in Encino, California; |
▪ | Vanderbilt Health Services, Inc., with which we own and operate a surgical facility in Franklin, Tennessee; and |
▪ | Wellmont Health Systems, with which we own and operate a surgical facility in Bristol, Tennessee. |
We manage six surgical facilities owned by Baptist Memorial under management agreements with Baptist Memorial in exchange for a management fee based on a percentage of the revenues of these surgical facilities. The management agreements terminate in 2019 and may be terminated earlier by either party for material breach after notice and an opportunity to cure.
8
Ancillary Services Segment
Our portfolio of outpatient surgical facilities is complemented by our suite of ancillary services, which support our physicians in providing high quality and cost-efficient patient care. Rather than contracting with third-party providers, we own ancillary businesses including diagnostics, physician practices, urgent care, anesthesia, optical and pharmacy. Our Company, physicians and patients benefit from these services through improved clinical efficiency and scheduling, and from incremental revenue and profitability associated with retaining these fees.
• | Diagnostic Laboratory: We offer physicians both toxicology and DNA testing services through our diagnostic laboratory, Logan Laboratories ("Logan Labs"), a wholly-owned subsidiary of the Company based in Tampa, Florida. Advanced toxicology screening provides physicians with the ability to identify when a patient is taking too much of a prescribed substance, when a patient is non-compliant with a prescribed substance or when a patient is taking unprescribed or illicit substances. Logan Labs provides quantitative confirmation testing of all drugs requested within 24 hours of receipt of a specimen, and results are available the following business day. Certified clinical chemists provide detailed laboratory reports that summarize and identify inconsistencies relating to test results and a patient's prescribed medications. The goal of our DNA testing services is to provide testing that helps guide physicians to the best treatment plan based on a patient’s DNA profile. Testing also ensures that regular toxicology screenings are appropriately interpreted. We intend to broaden our diagnostic laboratory offerings in support of the needs of our physicians across our existing specialties and new service lines. |
• | Multi-Specialty Physician Practices: We employ two models in connection with our network of physician practices. In the state of Florida, where the law does not preclude a business corporation from employing physicians, we own and operate Tampa Pain Relief Center, Inc., a wholly-owned subsidiary with several locations throughout Florida. In states other than Florida, we operate physician practices pursuant to long-term management service agreements with separate professional corporations that are wholly-owned by physicians. We derive revenues from these practice operations through management fees and expense reimbursement as set forth in the management services agreements. As of December 31, 2015, we owned or operated 46 physician practices with facilities in nine states. In total, through our physician practices, we employed over 100 physicians who focus on a number of specialties. We also provide our physician practices with relief from scheduling, billing and collections, staffing, regulatory compliance and other administrative and operational activities to allow them to focus on patient care. |
• | Urgent Care Facilities: Our urgent care facilities primarily treat injuries or illnesses requiring immediate care, but not serious enough to require an emergency room visit. Urgent care centers have become an increasingly viable alternative for patients as wait times for both primary care and emergency care providers continue to rise. Our urgent care facilities fill an access gap by providing walk-in care, especially during evening and weekend hours. In addition to the convenience they provide patients, our urgent care facilities also offer one of the lowest cost settings for both patients and payors. As the demands on primary care providers increase and insurance coverage expands, the urgent care industry is expected to continue growing. As of December 31, 2015, we owned and operated eight urgent care facilities in proximity to our surgical hospitals. Our urgent care facilities provide support and additional access points to our surgical hospitals. The fragmentation in the urgent care market creates significant room for consolidation and growth. |
• | Specialty Pharmacy Services: Our specialty pharmacy service line supports our physicians and provides expansion opportunities across multiple specialties within our delivery system, including ENT, GI, general surgery, ophthalmology, orthopedic, cardiology and pain management specialties. Our specialty pharmacy service line allows us to maintain control of quality and compliance with treatment programs. To ensure a high standard of care and appropriately expand these offerings, we have hired experienced pharmacists to supervise operations of our specialty pharmacy service offerings, which include compounding to meet the unique needs of our patients and distribution of these complex medications. Our specialty pharmacy service line affords us the ability to expand services across new specialties, such as infusion therapy and sterile products and support future growth into new service lines. |
Optical Services Segment
We offer group discounts and pricing structures for optical and medical products to independent eye care professionals through our wholly-owned subsidiary, The Alliance Product Purchasing Organization ("The Alliance").
Our wholly-owned optometric practice, Family Vision Care, provides full spectrum vision care to patients, including eye exams and vision testing, and offers an extensive collection of prescription eye wear. We provide operations oversight through ongoing management, finance, product and marketing support. We share in the primary goal of ensuring the highest level of patient care while maintaining costs and growing practice revenue and income.
Our wholly-owned subsidiary, Optical Synergies, was founded in 1995 as a buying group for independent optical laboratories whose common goal is to bring quality eye wear and related services to the ophthalmic industry. Member laboratories are provided with a forum for the exchange of information and ideas; this is accomplished through supplier sponsored sales promotions, networking opportunities within the group, and an annual educational conference. With the combined purchasing power of the group, members receive cost savings from Optical Synergies suppliers, thus increasing their competitiveness in the marketplace.
With locations in Indianola, IA and Chicago, IL, our wholly-owned, full-service wholesale optical laboratories, Midwest Labs, have served eye care professionals for over 35 years. Our extensive lens inventory allows us to process all major lens products, whether digitally or traditionally processed, with quick turnaround. To ensure the highest quality of finished products, we continue to invest in the latest equipment and technology.
9
Acquisitions and Developments
We continuously evaluate opportunities to expand our presence in the surgical facility market by making strategic acquisitions of existing surgical facilities and by developing new surgical facilities in cooperation with local physician partners and, when appropriate, with healthcare systems and other strategic partners. We have the flexibility to structure our partnerships as two-way arrangements where either we are a majority owner partnered with physicians or we are a minority owner with buy-up rights. These buy-up rights give us the option to own a controlling interest at some point in the future. Alternatively, we may choose to pursue a three-way arrangement with physicians and a healthcare system.
Effective November 3, 2014, we completed the acquisition of Symbion, a privately owned national operator of surgical facilities. The acquisition of Symbion added 55 surgical facilities, which includes 49 ASCs and six surgical hospitals, to our network of existing facilities. At closing, we paid approximately $300.1 million in cash and assumed or paid down approximately $472.4 million of outstanding indebtedness of Symbion, including related accrued and unpaid interest.
Acquisition Program. We employ a dedicated acquisition team with experience in healthcare services. Our team seeks to acquire surgical facilities that meet our criteria, including prominence and quality of physician partners, specialty mix, opportunities for growth, level of competition in the local market, level of managed care penetration and our ability to access managed care organization contracts. Our team utilizes its extensive industry contacts, as well as referrals from current physician partners and other sources, to identify, contact and develop potential acquisition candidates.
We believe there are numerous acquisition opportunities that would pass our general screening criteria. We carefully evaluate each of our acquisition opportunities through an extensive due diligence process to determine which facilities have the greatest potential for growth and profitability improvements under our operating structure. In many cases, the acquisition team identifies specific opportunities to enhance a facility’s productivity post-acquisition. For example, we may renovate or construct additional operating or treatment rooms in existing facilities to meet anticipated demand for procedures based on an analysis of local market characteristics. Our team may also identify opportunities to attract additional physicians to increase the acquired facility’s revenues and profitability.
Development Program. We develop surgical facilities in markets in which we identify substantial interest by physicians and payors. We have experience in developing both single and multi-specialty surgical facilities. When we develop a new surgical facility, we generally provide all of the services necessary to complete the project. We offer in-house capabilities for structuring partnerships and financing facilities and work with architects and construction firms in the design and development of surgical facilities. Before and during the development phase of a new surgical facility, we analyze the competitive environment in the local market, review market data to identify appropriate services to provide, prepare and analyze financial forecasts, evaluate regulatory and licensing issues and assist in designing the surgical facility and identifying appropriate equipment to purchase or lease. After the surgical facility is developed, we generally provide startup operational support, including information systems, equipment procurement and financing.
Information Systems and Controls
Each of our surgical facilities uses a financial reporting system that provides information to our corporate office to track financial performance on a timely basis. In addition, each of our surgical facilities uses an operating system to manage its business that provides critical support in areas such as scheduling, billing and collection, accounts receivable management, purchasing and other essential operational functions. We have implemented systems to support all of our surgical facilities and to enable us to more easily access information about our surgical facilities on a timely basis.
The American Recovery and Reinvestment Act of 2009 (the "ARRA") provides for Medicare and Medicaid incentive payments for eligible hospitals and professionals that implement and achieve meaningful use of certified Electronic Health Records ("EHR") technology. Our surgical hospitals have implemented systems to comply with the EHR meaningful use requirements of the Health Information Technology for Economic and Clinical Health Act (the “HITECH Act”) in time to qualify for the maximum available incentive payments. Compliance with the meaningful use requirements has and will continue to result in significant costs including business process changes, professional services focused on successfully designing and implementing EHR solutions along with costs associated with the hardware and software components of the project.
We calculate net revenues through a combination of manual and system generated processes. Our operating systems include insurance modules that allow us to establish profiles of insurance plans and their respective payment rates. The systems then match the charges with the insurance plan rates and compute a contractual adjustment estimate for each patient account. We then manually review the reasonableness of the systems’ contractual adjustment estimate using the insurance profiles. This estimate is adjusted, if needed, when the insurance payment is received and posted to the account. Net revenues are computed and reported by the systems as a result of this activity.
It is our policy to collect co-payments and deductibles prior to providing services. It is also our policy to verify a patient’s insurance 72 hours prior to the patient’s procedure. Because our services are primarily non-emergency, our surgical facilities have the ability to control these processes. We do not track exceptions to these policies, but we believe that they occur infrequently and involve insignificant amounts. When exceptions do occur, we require patients whose insurance coverage is not verified to assume full responsibility for the fees prior to services being rendered, and we seek prompt payment of co-payments and deductibles and verification of insurance following the procedure.
Claims are submitted electronically if the payor accepts electronic claims. We use clearinghouses for electronic claims, which then forward the claims to the respective payors. Payments are manually input to the respective patient accounts.
We have developed proprietary measurement tools to track key operating statistics at each of our surgical facilities by integrating data from our local operating systems and our financial reporting systems. Management uses these tools to measure operating results against target thresholds and to identify, monitor and adjust areas such as specialty mix, staffing, operating costs, employee expenses and accounts receivable management. Our corporate and facility-level management teams are compensated in part using performance-based incentives focused on revenue growth and improving operating income.
10
Marketing
We primarily direct our sales and marketing efforts at physicians who would utilize our surgical facilities. Marketing activities directed at physicians and other healthcare providers are coordinated locally by the individual surgical facility and are supplemented by dedicated corporate personnel. These activities generally emphasize the benefits offered by our surgical facilities compared to other facilities in the market, such as the proximity of our surgical facilities to physicians’ offices, the ability to schedule consecutive cases without preemption by inpatient or emergency procedures, the efficient turnaround time between cases, our advanced surgical equipment and our simplified administrative procedures. Although the facility administrator is the primary point of contact, physicians who utilize our surgical facilities are important sources of recommendations to other physicians regarding the benefits of using our surgical facilities. Recruiting teams develop a target list of physicians, and we continually review our progress in successfully recruiting additional local physicians.
We also market our surgical facilities directly to payors, such as health maintenance organizations ("HMOs"), preferred provider organizations ("PPOs"), and other managed care organizations and employers. Payor marketing activities conducted by our corporate office management and facility administrators emphasize the high quality of care, cost advantages and convenience of our surgical facilities, and are focused on making each surgical facility an approved provider under local managed care plans.
Competition
In each market in which we operate a surgical facility, we compete with hospitals and operators of other surgical facilities to attract physicians and patients. We believe that the competitive factors that affect our surgical facilities’ ability to compete for physicians are convenience of location of the surgical facilities, access to capital and participation in managed care programs. In addition, we believe the national prominence, scale and reputation of our company are instrumental in attracting physicians. We believe that our surgical facilities attract patients based upon our quality of care, the specialties and reputations of the physicians who operate in our surgical facilities, participation in managed care programs, ease of access and convenient scheduling and registration procedures.
In developing or acquiring existing surgical facilities, we compete with other public and private surgical facility and hospital companies. Several large national companies own and/or manage surgical facilities, including HCA Holdings, Inc., Surgical Care Affiliates, Inc., AmSurg Corp. and Tenet Healthcare Corporation. We also face competition from local hospitals, physician groups and other providers who may compete with us in the ownership and operation of surgical facilities, as well as the trend of physicians choosing to perform procedures in an office-based setting rather than in a surgical facility.
Seasonality
Our net revenue fluctuates based on the number of business days in each calendar quarter, because the majority of services provided by physicians in our surgical facilities consist of scheduled procedures and office visits that occur during business hours. Revenue in the fourth quarter could also be impacted by an increased utilization of services due to annual deductibles which are not usually met until later in the year and also as patients try to utilize their healthcare benefits before they expire at year-end.
Employees
At December 31, 2015, we had approximately 5,100 employees, including approximately 3,500 full-time employees. None of our employees are represented by a collective bargaining agreement. We believe that we have a good relationship with our employees.
Environmental
We are subject to various federal, state and local laws and regulations relating to the protection of the environment and human health and safety, including those governing the management and disposal of hazardous substances and wastes, the cleanup of contaminated sites and the maintenance of a safe workplace. Our operations include the use, generation and disposal of hazardous materials. We may, in the future, incur liability under environmental statutes and regulations with respect to contamination of sites we own or operate (including contamination caused by prior owners or operators of such sites, adjoining properties or other persons) and the off-site disposal of hazardous substances. We believe that we have been and are in substantial compliance with the terms of all applicable environmental laws and regulations and that we have no liabilities under environmental requirements that we would expect to have a material adverse effect on our business, results of operations or financial condition (including our capital expenditures, earnings and competitive position).
Insurance
We maintain liability insurance in amounts that we believe are appropriate for our operations. Currently, we maintain professional liability insurance that provides coverage on a claims-made basis of $1.0 million per occurrence with a retention of $100,000 per occurrence and $3.0 million in annual aggregate coverage per surgical facility, including the facility and employed staff. We maintain general liability insurance that provides coverage on an occurrence basis of $1.0 million per occurrence with a retention of $25,000 per occurrence and $3.0 million in annual aggregate coverage per surgical facility. We also maintain business interruption insurance and property damage insurance. Coverage under certain of these policies is contingent upon the policy being in effect when a claim is made regardless of when the events which caused the claim occurred. The cost and availability of such coverage has varied widely in recent years.
In addition, physicians who provide professional services in our surgical facilities are required to maintain separate malpractice coverage with similar minimum coverage limits. While we believe that our insurance policies are adequate in amount and coverage for our anticipated operations, we cannot assure you that the insurance coverage is sufficient to cover all future claims or will continue to be available in adequate amounts or at a reasonable cost.
Sources of Revenue - Surgical Facilities
Revenue from our surgical facilities is obtained from facility fees related to healthcare services performed in our surgical facilities and is included in our patient service revenues, which accounted for 98.0%, 96.2%, and 94.4% of our total revenue for the years ended December 31,
11
2015, 2014 and 2013, respectively. The fee charged for surgical services varies depending on the type of service provided, but usually includes all charges for usage of an operating room, a recovery room, special equipment, supplies, nursing staff and medications. Our fees do not typically include professional fees charged by the patient's surgeon, anesthesiologist or other attending physician, which are billed directly by such physicians to the patient or third-party payor. We recognize our facility fees on the date of service, net of estimated contractual adjustments and discounts for third-party payors, including Medicare and Medicaid. Any changes in estimated contractual adjustments and discounts are recorded in the period of change.
We are dependent upon private and government third-party sources of payment for the surgical services we provide. The amounts that our surgical facilities receive in payment for their services may be adversely affected by market and cost factors as well as other factors over which we have no control, including Medicare, Medicaid and state regulations as well as cost containment and utilization decisions and reduced reimbursement schedules of third-party payors. Approximately 38.2%, 34.5% and 28.0% of our patient service revenues were from government sources, mostly Medicare, for the years ended December 31, 2015, 2014 and 2013, respectively.
The following table sets forth the percentage of our total patient service revenues for our consolidated surgical facilities by type of payor for the periods indicated:
Year Ended December 31, | |||||||||
2015 | 2014 | 2013 | |||||||
Private Insurance | 55.0 | % | 52.1 | % | 60.6 | % | |||
Government | 38.2 | % | 34.5 | % | 28.0 | % | |||
Self-pay | 1.7 | % | 3.5 | % | 2.8 | % | |||
Other | 5.1 | % | 9.9 | % | 8.6 | % | |||
Total patient service revenues | 100.0 | % | 100.0 | % | 100.0 | % | |||
We receive reimbursement from Medicare for surgical services based on three different payment systems depending on the site of service: outpatient hospital surgical services, hospital inpatient surgical services and outpatient surgical services provided in our ASCs.
Medicare Reimbursement - Hospital Outpatient Departments
Surgical services that are provided in hospital outpatient departments are reimbursed by Medicare on the Outpatient Prospective Payment System (“OPPS”). The OPPS is a system established by the Secretary of the Department of Health and Human Services (“HHS”) that determines payment amounts prospectively for various categories of medical services performed in hospital outpatient departments (“HOPDs”). On November 13, 2015, CMS published its OPPS final rule for CY 2016. Among other things, the final rule provides for a payment rate decrease of 0.3% for hospitals that meet the reporting requirements of the Medicare Hospital Outpatient Quality Reporting ("OQR") Program and a further 2.0% payment rate decrease for hospitals that do not meet the requirements of the OQR Program. The rate decrease is based on a hospital market basket increase of 2.4%, which is reduced by a multi-factor productivity adjustment of 0.5% and an additional 0.2% reduction required by the Patient Protection and Affordable Care Act (the “Affordable Care Act”) and the Health Care and Education Reconciliation Act of 2010 (together with the Affordable Care Act, the “Healthcare Reform Acts”). This is further reduced by a 2.0% decrease to recoup an approximately $1 billion overestimation of laboratory test packaging under a policy implemented in 2014.
Medicare Reimbursement - ASCs
Payments under the Medicare program to ASCs are also made based on the OPPS. However, the payment received from the Medicare program by an ASC is a percentage of the payment to HOPDs. Reimbursement rates for ASCs are updated annually based on changes in the consumer price index offset by multifactor productivity adjustments. In 2015, ASC reimbursement rates increased by 1.4% and, based on the OPPS Final Rule, will increase by an additional 0.3% for 2016. CMS has established the Ambulatory Surgical Center Quality Reporting (“ASCQR”) Program as a pay-for-reporting, quality data program. Our ASCs that participate in the ASCQR Program receive the full annual update to the ASC payment rate. Those ASCs that do not successfully report quality data under the ASCQR Program may receive a payment reduction.
Medicare Reimbursement - Hospital Inpatient Services
Five of our surgical facilities are licensed as hospitals. Most inpatient services provided by hospitals are reimbursed by Medicare under the inpatient prospective payment system (“IPPS”). Under the IPPS, a hospital receives a fixed amount for inpatient hospital services based on each patient's final assigned Medicare-severity diagnosis related group (“MS-DRG”). Each MS-DRG is assigned a payment rate that is prospectively set using national average resources used per case for treating a patient with a particular diagnosis. This MS-DRG assignment also affects the prospectively determined capital rate paid with each MS-DRG. MS-DRG and capital payments are adjusted by a predetermined geographic adjustment factor assigned to the geographic area in which the hospital is located. The index used to adjust the MS-DRG rates, known as the “hospital market basket index,” gives consideration to the inflation experienced by hospitals in purchasing goods and services.
On July 31, 2015, CMS published the IPPS final rule for federal fiscal year (“FFY”) 2016, which began on October 1, 2015. Under the FFY 2016 final rule, rates for inpatient stays in hospitals paid under the IPPS that successfully report certain quality data under the Hospital Inpatient Quality Reporting (“IQR”) Program and demonstrate meaningful use of certified electronic health record technology will be increased by 0.9%. Those hospitals that do not successfully report quality data under the IQR Program may receive a payment rate decrease of 0.6%. In addition to the IQR Program, hospitals will be subject to payment adjustments under the Value Based Purchasing Program, Readmissions Reduction Program and Hospital Acquired Conditions Reduction Programs that have been implemented by HHS.
Annual Cost Reports
12
Hospitals participating in the Medicare and some Medicaid programs, whether paid on a reasonable cost basis or under a prospective payment system, are required to meet certain financial reporting requirements. Federal and, where applicable, state regulations require submission of annual cost reports identifying medical costs and expenses associated with the services provided by each hospital to Medicare beneficiaries and Medicaid recipients. Annual cost reports required under the Medicare and some Medicaid programs are subject to routine governmental audits. These audits may result in adjustments to the amounts ultimately determined to be payable to us under these reimbursement programs. Finalization of these audits often takes several years. Providers may appeal any final determination made in connection with an audit.
Sources of Revenue - Optical and Ancillary Services
Our ancillary services segment derives revenue from the provision of physician services and laboratory services. The fees charged for ancillary and optical services depend on the type of service provided, the location in which the service is provider and the provider of the service. Ancillary and optical services fees are received from both private and government third-party sources of payment. The amounts that we receive in payment for the provision of ancillary and optical services may be adversely affected by market and cost factors as well as other factors over which we have no control, including Medicare, Medicaid and state regulations as well as cost containment and utilization decisions and reduced reimbursement schedules of third-party payors.
Our ancillary services revenue primarily consists of fee for service revenue that is derived principally from the provision of physician and laboratory services to patients of our surgical facilities. Medicare pays for physician services based upon the Medicare Physician Fee Schedule (“MPFS”). Payment rates under the MPFS are determined based on (i) relative value units for the services provided, (ii) a geographic adjustment factor and (iii) a conversion factor. Payment rates under the MPFS are updated annually by HHS. The primary element in each year’s update calculation is the Medicare Economic Index (“MEI”), which is a measure of the inflation of the cost of operating a physician practice. The update was then adjusted based on a system called the sustainable growth rate (“SGR”). The SGR wass a target rate of growth in spending for physician services which was intended to control the growth of Medicare spending on physician services. Because it became apparent that rigorous implementation of the SGR would have produced significant reductions in Medicare’s physician payments, beginning in 2003 Congress continuously delayed application of the SGR, leading ultimately to the replacement of the SGR in April 2015 through enactment of the Medicare Access and CHIP Reauthorization Act of 2015. That Act established a fixed 0.5% annual adjustment through calendar year 2019. For years 2020-2025, the base rates will be maintained and physician compensation will be subject to adjustment under the Merit-Based Incentive Payment System. Beginning in 2026, physicians who receive a significant portion of revenues through alternative payment models (that is, payments not fee-for-service based) will receive a 0.75% increase, while physicians who do not participate in these alternatives will receive an increase of 0.25%. Certain of our laboratory ancillary services are reimbursed by Medicare under the Medicare Clinical Laboratory Fee Schedule (“CLFS”). Under a September 25, 2015 proposed rule that implements the Protecting Access to Medicare Act of 2014 (“PAMA”), as of January 1, 2017 the CLFS payment methodology will be adjusted so that payment amounts for laboratory tests on the CLFS will be determined by calculating a weighted median of private payor rates using reported private payor rates and associated volume (number of tests). For tests that were paid on the CLFS prior to the implementation of PAMA, any reduction in payment amount will be phased in over the first 6 years of payment under the new system.”
Private Third-Party Payors
Most third-party payors reimburse us for surgical and ancillary services pursuant to a written contract. These contracts generally require that we offer discounts from our established charges. Some of our payments come from third-party payors with which we do not have written contracts. In those situations, commonly known as “out-of-network” services, we generally charge the patients the same co-payment or other patient responsibility amounts that we would have charged had we had a contract with the third-party payor. We also submit a claim for the services to the third-party payor along with full disclosure that we have charged the patient an in-network patient responsibility amount.
Governmental Regulation
General
The healthcare industry is highly regulated, and we cannot provide any assurance that the regulatory environment in which we operate will not significantly change in the future or that we will be able to successfully address any such changes.
Every state imposes licensing requirements on individual physicians and healthcare facilities. In addition, federal and state laws regulate HMOs and other managed care organizations. Many states require regulatory approval, including licensure and accreditation, and in some cases, certificates of need, before establishing certain types of healthcare facilities, including surgical hospitals and ASCs, offering certain services, including the services we offer, or making expenditures in excess of certain amounts for healthcare equipment, facilities or programs. Our ability to operate profitably will depend in part upon our surgical facilities obtaining and maintaining all necessary licenses, accreditation, certificates of need and other approvals and operating in compliance with applicable healthcare regulations. Failure to do so could have a material adverse effect on our business.
Our surgical facilities are subject to federal, state and local laws dealing with issues such as occupational safety, employment, medical leave, insurance regulations, civil rights, discrimination, building codes and medical waste and other environmental issues. Federal, state and local governments are expanding the regulatory requirements on businesses like ours. The imposition of these regulatory requirements may have the effect of increasing operating costs and reducing the profitability of our operations.
We believe that hospital, outpatient surgery, physician, laboratory and other diagnostic and healthcare services will continue to be subject to intense regulation at the federal and state levels. We are unable to predict what additional government regulations, if any, affecting our business may be enacted in the future or how existing or future laws and regulations might be interpreted. If we, or any of our surgical facilities, fail to comply with applicable laws, it might have a material adverse effect on our business.
13
Certificates of Need and Licensure
Capital expenditures for the construction of new healthcare facilities, the addition of beds or new healthcare services or the acquisition of existing healthcare facilities may be reviewable by state regulators under statutory schemes that are sometimes referred to as certificate of need laws. States with certificate of need laws place limits on the construction and acquisition of healthcare facilities and the expansion of existing facilities and services. In these states, approvals, generally known as certificates of need, are required for capital expenditures exceeding certain preset monetary thresholds for the development, acquisition and/or expansion of certain facilities or services, including surgical facilities. We have a concentration of surgical facilities in certificate of need states as we believe the regulations present a competitive advantage to existing operators.
Our healthcare facilities also are subject to state licensing requirements for medical providers. Our ASC facilities have licenses to operate in the states in which they operate and must meet all applicable requirements for ASCs. In addition, even though our surgical facilities that are licensed as hospitals primarily provide surgical services, they must meet all applicable requirements for general hospital licensure. To assure continued compliance with these regulations, governmental and other authorities periodically inspect our surgical facilities. The failure to comply with these regulations could result in the suspension or revocation of a facility’s license. In addition, based on the specific operations of our surgical facilities, some of these facilities maintain a pharmacy license, a controlled substance registration, a clinical laboratory certification waiver, and environmental protection permits for biohazards and/or radioactive materials, as required by applicable law.
Healthcare Reform
The Affordable Care Act has been subject to a number of challenges to its constitutionality. On June 28, 2012, the United States Supreme Court upheld challenges to the constitutionality of the “individual mandate” provision, which generally requires all individuals to purchase healthcare insurance or pay a penalty, but struck down as unconstitutional the provision that would have allowed the federal government to revoke all federal Medicaid funding to any state that did not expand its Medicaid program. As a result, many states have refused to extend Medicaid eligibility to more individuals as envisioned by the law.
On June 25, 2015, the United States Supreme Court upheld the legality of premium subsidies made available by the federal government to individuals residing in the 36 states that have federally-run health insurance exchanges. The subsidies are provided to low-income individuals to assist with the cost of purchasing health insurance through federally-run health insurance exchanges. Other legal challenges to the Affordable Care Act are pending.
In addition, several bills have been and will likely continue to be advanced in Congress that would defund, repeal or amend all or significant provisions of the Affordable Care Act, and a number of provisions of the Affordable Care Act that were supposed to become effective have been delayed by the Obama administration. As a result, it is difficult to predict the impact the Affordable Care Act will have on our business given the threats to and uncertainty surrounding key provisions of the Affordable Care Act. However, depending on how the Affordable Care Act is ultimately interpreted, amended and implemented, it could have an adverse effect on our business, financial condition and results of operations.
Moreover, other legislative changes have also been proposed and adopted since the Affordable Care Act was enacted. On August 2, 2011, the Budget Control Act of 2011, among other things, created measures for spending reductions by Congress. A Joint Select Committee on Deficit Reduction, tasked with recommending a targeted deficit reduction of at least $1.2 trillion for the years 2013 through 2021, was unable to reach required goals, thereby triggering the legislation’s automatic reduction to several government programs. This included aggregate reductions to Medicare payments to providers of 2% per fiscal year, which went into effect on April 1, 2013 and, due to subsequent legislative amendments, will remain in effect through 2025 unless additional Congressional action is taken. On January 2, 2013, President Obama signed into law the American Taxpayer Relief Act of 2012, which, among other things, further reduced Medicare payments to several providers, including hospitals, and increased the statute of limitations period for the government to recover overpayments to providers from three to five years. These and other similar new laws may result in additional reductions in Medicare and other health care funding, which could have a material adverse effect on our financial operations.
Medicare and Medicaid Private Contractor Audits
CMS has implemented a number of programs that use private contractors that contract with CMS to identify overpayments and underpayments and other potential sources of billing fraud. These contractors, known as Recovery Audit Contractors (“RACs”) and Zone Program Integrity Contractors (“ZPICs”) conduct both post-payment and pre-payment review of claims submitted by Medicare providers. In addition, CMS employs Medicaid Integrity Contractors (“MICs”) to perform post-payment audits of Medicaid claims and identify overpayments. Our facilities and providers continue to receive letters from auditors such as RACs and ZPICs requesting repayment of alleged overpayments for services and incur expenses associated with responding to and appealing these determinations, as well as the costs of repaying any overpayments. Moreover, in recent years, the increase in Medicare payment appeals has created a backlog such that resolving appeals often takes multiple years.
For instance, we recently received the results of a MIC audit that resulted in an overpayment obligation. HMS Federal Solutions, a MIC, completed the audit of one of our surgical hospitals for the period July 1, 2009 through May 31, 2012 and determined an overpayment obligation in the amount of approximately $4.6 million based on its extrapolation of a statistical sampling of claims, as well as a civil monetary penalty in the amount of $162,000, for a total amount owed to Idaho’s Department of Health and Welfare, Medicaid Program Integrity Unit of approximately $4.7 million for failure to comply with Medicaid rules by billing for (i) non-covered services, (ii) services provided by non-eligible providers, (iii) services not provided and (iv) unauthorized services. We have appealed the audit and are currently awaiting the result.
14
Although all other repayments requested to date as a result of RAC, MIC and ZPIC audits have not been material to our Company, we are unable to quantify the aggregate financial impact of these audits on our facilities given the pending appeals and uncertainty about the extent of future audits.
Quality Improvement
The Medicare program presently requires hospitals and ambulatory surgery centers to report performance data on a variety of quality metrics. Facilities that fail to report are penalized with reduced Medicare payments. Additionally, payments to hospitals are adjusted based on the hospital’s performance on these quality measures. A substantial portion of hospital payment is at risk depending on its individual performance relative to benchmarks and other hospitals’ performance. There is a substantial risk that our Medicare payments could be reduced if our hospitals fail to perform adequately on these measures. Additionally, there is a risk that Medicare payments could be reduced if our facilities-hospitals and ASCs-fail to adequate report data as required by CMS. Ambulatory surgery center payments are not yet adjusted based on performance against quality measures, but there is a substantial risk that Congress may soon link ASC Medicare payments to actual performance, in addition to reporting. The Obama administration in early 2015 announced its intent to subject even more Medicare fee-for-service payments to value-based payment program, and has proposed several specific changes that could increase the percentage of our payments at risk based on quality performance.
If the public performance data becomes a primary factor in determining where patients choose to receive care, and if competing hospitals and ASCs have better results than our facilities on those measures, we would expect that our patient volumes could decline.
Medicare and Medicaid Participation
The majority of our revenue is expected to continue to be received from third-party payors, including federal and state programs, such as Medicare and Medicaid, and commercial payors. To participate in the Medicare program and receive Medicare payment, our surgical facilities must comply with regulations promulgated by the Department of Health and Human Services (“HHS”). Among other things, these regulations, known as “conditions for coverage” or “conditions of participation,” impose numerous requirements on our facilities, their equipment, their personnel and their standards of medical care, as well as compliance with all applicable state and local laws and regulations. On April 26, 2007, CMS issued a policy memorandum that reaffirmed its prior interpretation of its conditions of participation that all hospitals (other than critical access hospitals) participating in the Medicare program are required to provide basic emergency care interventions regardless of whether or not the hospital maintains an emergency department. Our five facilities licensed as hospitals are required to meet this requirement to maintain their participating provider status in the Medicare program. As of December 31, 2015, two of our hospitals, which do not have an emergency room, maintain a protocol for the transfer of patients requiring emergency treatment, which protocol may be interpreted as inconsistent with the 2007 CMS policy memorandum. Our surgical facilities must also satisfy the conditions of participation to be eligible to participate in the various state Medicaid programs. The requirements for certification under Medicare and Medicaid are subject to change and, in order to remain qualified for these programs, we may have to make changes from time to time in our facilities, equipment, personnel or services. Although we intend to continue to participate in these reimbursement programs, we cannot assure you that our surgical facilities will continue to qualify for participation.
The Affordable Care Act and its implementing regulations require a hospital to provide written disclosure of physician ownership interests to the hospital’s patients and on the hospital’s website and in any advertising, along with annual reports to the government detailing such interests. Additionally, hospitals that do not have 24/7 physician coverage are required to inform patients of this fact and receive signed acknowledgment from the patients of the disclosure. A hospital’s provider agreement may be terminated if it fails to provide the required notices. In 2010, CMS issued a “self-referral disclosure protocol” for hospitals and other providers that wish to self-disclose potential violations of the Stark Law to CMS and to attempt to resolve those potential violations and any related overpayment liabilities at levels below the maximum penalties and amounts set forth in the statute. The disclosure requirements set forth in the Affordable Care Act and the self-referral disclosure protocol reflect a move towards increasing government scrutiny of the financial relationships between hospitals and referring physicians and increasing disclosure of potential violations of the Stark Law to the government by hospitals and other healthcare providers. We intend for all of our facilities to meet their disclosure obligations.
Survey and Accreditation
Hospitals and healthcare facilities are subject to periodic inspection by federal, state and local authorities to determine their compliance with applicable regulations and requirements necessary for licensing, certification and accreditation. All of our hospitals and surgical facilities currently are licensed under appropriate state laws and are qualified to participate in the Medicare and Medicaid programs. Renewal and continuation of certain of these licenses, certifications and accreditations are based on inspections or other reviews generally conducted in the normal course of business of health facilities. Loss of, or limitations imposed on, licenses or accreditations could reduce a facility’s utilization or revenue, or its ability to operate all or a portion of its facilities.
Utilization Review
Federal law contains numerous provisions designed to ensure that services rendered by hospitals to Medicare and Medicaid patients meet professionally recognized standards and are medically necessary and that claims for reimbursement are properly filed. These provisions include a requirement that a sampling of admissions of Medicare and Medicaid patients must be reviewed by quality improvement organizations, which review the appropriateness of Medicare and Medicaid patient admissions and discharges, the quality of care provided, the validity of MS-DRG classifications and the appropriateness of cases of extraordinary length of stay or cost. Quality improvement organizations may deny payment for services provided or assess fines and also have the authority to recommend to HHS that a provider which is in substantial noncompliance with the standards of the quality improvement organization be excluded from participation in the Medicare program. Utilization review is also a requirement of most non-governmental managed care organizations.
15
Federal Anti-Kickback Statute and Medicare Fraud and Abuse Laws
The Social Security Act includes provisions addressing false statements, illegal remuneration and other instances of fraud and abuse in federal health care programs. These provisions include the statute commonly known as the federal Anti-Kickback statute (the “Anti-Kickback Statute”). The Anti-Kickback Statute prohibits providers and others from, among other things, soliciting, receiving, offering or paying, directly or indirectly, any remuneration in return for either making a referral for, or ordering or arranging for, or recommending the order of, any item or service covered by a federal healthcare program, including, but not limited to, the Medicare and Medicaid programs. Violations of the Anti-Kickback Statute are criminal offenses punishable by imprisonment and fines of up to $25,000 for each violation. Civil violations are punishable by fines of up to $50,000 for each violation, as well as damages of up to three times the total amount of remuneration received from the government for healthcare claims.
Because physician-investors in our surgical facilities are in a position to generate referrals to the facilities, the distribution of available cash to those investors could come under scrutiny under the Anti-Kickback Statute. Some courts have held that the Anti-Kickback Statute is violated if one purpose (as opposed to a primary or the sole purpose) of a payment to a provider is to induce referrals. Further, Section 6402(f)(2) of the Affordable Care Act amends the Anti-Kickback Statute by adding a provision to clarify that a person need not have actual knowledge of such section or specific intent to commit a violation of the Anti-Kickback Statute. Because none of these cases involved a joint venture such as those owning and operating our surgical facilities, it is not clear how a court would apply these holdings to our activities. It is clear, however, that a physician’s investment income from a surgical facility may not vary with the number of his or her referrals to the surgical facility, and we believe that we comply with this prohibition.
Under regulations issued by the OIG, certain categories of activities are deemed not to violate the Anti-Kickback Statute (commonly referred to as the safe harbors). According to the preamble to these safe harbor regulations, the failure of a particular business arrangement to comply with the regulations does not determine whether the arrangement violates the Anti-Kickback Statute. The safe harbor regulations do not make conduct illegal, but instead outline standards that, if complied with, protect conduct that might otherwise be deemed in violation of the Anti-Kickback Statute. Failure to meet a safe harbor does not indicate that the arrangement violates the Anti-Kickback Statute, although it may be subject to additional scrutiny.
We believe the ownership and operations of our surgery centers and hospitals do not fit wholly within any of the safe harbors, but we attempt to structure our ASCs to fit as closely as possible within the safe harbor designed to protect distributions to physician-investors in ambulatory surgery centers who directly refer patients to the ambulatory surgery center and personally perform the procedures at the center as an extension of their practice (the “ASC Safe Harbor”). The ASC Safe Harbor protects four categories of investors, including ASCs owned by (1) general surgeons, (2) single-specialty physicians, (3) multi-specialty physicians and (4) hospital/physician joint ventures, provided that certain requirements are satisfied. These requirements include the following:
• | The ambulatory surgery center must be certified to participate in the Medicare program, and its operating and recovery room space must be dedicated exclusively to the center and not a part of a hospital (although such space may be leased from a hospital if such lease meets the requirements of the safe harbor for space rental). |
• | Each investor must be either (a) a physician who derived at least one-third of his or her medical practice income for the previous fiscal year or 12-month period from performing procedures on the list of Medicare-covered procedures for ASCs, (b) a hospital, or (c) a person or entity not in a position to make or influence referrals to the center, nor to provide items or services to the center, nor employed by the center or any investor. |
• | Unless all physician-investors are members of a single specialty, each physician-investor must perform at least one-third of his or her procedures at the ambulatory surgery center each year. This requirement is in addition to the requirement that the physician-investor has derived at least one-third of his or her medical practice income for the past year from performing procedures. |
• | Physician-investors must have fully informed their referred patients of the physician’s investment. |
• | The terms on which an investment interest is offered to an investor are not related to the previous or expected volume of referrals, services furnished or the amount of business otherwise generated from that investor to the entity. |
• | Neither the ambulatory surgery center nor any other investor nor any person acting on their behalf may loan funds to or guarantee a loan for an investor if the investor uses any part of such loan to obtain the investment interest. |
• | The amount of payment to an investor in return for the investment interest is directly proportional to the amount of the capital investment (including the fair market value of any pre-operational services rendered) of that investor. |
• | All physician-investors, any hospital-investor and the center agree to treat patients receiving benefits or assistance under a federal healthcare program in a non-discriminatory manner. |
• | All ancillary services performed at the ambulatory surgery center for beneficiaries of federal healthcare programs must be directly and integrally related to primary procedures performed at the center and may not be billed separately. |
• | No hospital-investor may include on its cost report or any claim for payment from a federal healthcare program any costs associated with the ambulatory surgery center. |
• | The ambulatory surgery center may not use equipment owned by or services provided by a hospital-investor unless such equipment is leased in accordance with a lease that complies with the Anti-Kickback Statute equipment rental safe harbor and such services are provided in accordance with a contract that complies with the Anti-Kickback Statute personal services and management contract safe harbor. |
16
• | No hospital-investor may be in a position to make or influence referrals directly or indirectly to any other investor or the center. |
We believe that the ownership and operations of our surgical centers will not satisfy this ASC Safe Harbor for investment interests in ASCs because, among other things, we or one of our subsidiaries will generally be an investor in and provide management services to each ambulatory surgery center. We cannot assure you that the OIG would view our activities favorably even though we strive to achieve compliance with the remaining elements of this safe harbor.
In addition, although we expect each physician-investor to utilize our ASCs as an extension of his or her practice and ask each physician-investor to certify this practice, we cannot assure you that all physician-investors will derive at least one-third of their medical practice income from performing Medicare-covered ambulatory surgery center procedures, perform one-third of their procedures at the centers or inform their referred patients of their investment interests. Interests in our joint venture ASCs are purchased at what we believe to be fair market value. Investors who purchase at a later time generally pay more for a given percentage interest than founding investors. The result is that while all investors are paid distributions in accordance with their ownership interests, for ASCs where there are later purchases, we cannot meet the safe harbor requirement that return on investment is directly proportional to the amount of capital investment. The OIG has on several occasions reviewed investments relating to ASCs, and in Advisory Opinion No. 07-05, raised concerns that (a) purchases of interests from physicians might yield gains on investment rather than capital infusion to the ASCs, (b) such purchases could be meant to reward or influence the selling physicians’ referrals to the ambulatory surgery center or the hospital, and (c) such returns might not be directly proportional to the amount of capital invested. Nonetheless, we believe our fair market value purchase requirements and distribution policies comply with the Anti-Kickback Statute.
In OIG Advisory Opinion No. 09-09 (July 29, 2009), the OIG concluded that an arrangement involving an ambulatory surgery center joint venture between a hospital and physicians involving the combination of their two ASCs into a single, larger center presented minimal risk of fraud or abuse, despite the fact that it did not fit within any applicable Anti-Kickback safe harbors. Additionally, the OIG stated that fair market value should be determined based only on the tangible assets of each facility since the physician investors are referral sources for the ambulatory surgery center. The OIG stated that a cash flow-based valuation of the business contributed by the physician investors potentially would include the value of the physician investors’ referrals over the time that their ambulatory surgery center was in existence prior to the merger with the hospital’s ambulatory surgery center. The OIG went on to note that a valuation involving intangible assets would not necessarily result in a violation of the Anti-Kickback Statute, but would require a review of all the facts and circumstances. It is not clear whether the OIG is concerned about using a cash flow-based valuation in most healthcare transactions involving referral sources, or just transactions, similar to this one, where the parties’ contributions would be valued differently for contributing the same assets if only one party’s contribution is valued as a going concern based on cash flow. Also, the OIG appears to be focused on historical cash flow rather than a projected, discounted cash flow, which is a commonly used valuation methodology. What is clear is that for the first time, the OIG addressed valuation methodologies, which could lead to increased scrutiny of all transactions involving physicians.
Our hospital investments do not fit wholly within the safe harbor for investments in small entities because more than 40.0% of the investment interests are held by investors who are either in a position to refer to the hospital or who provide services to the hospital and more than 40.0% of the hospital’s gross revenue last year were derived from referrals generated by investors. However, we believe we comply with the remaining elements of the safe harbor.
In addition to the physician ownership in our surgical facilities, other financial relationships of ours with potential referral sources could potentially be scrutinized under the Anti-Kickback Statute. We have entered into management agreements to manage the majority of our surgical facilities. Most of these agreements call for our subsidiary to be paid a percentage-based management fee. Although there is a safe harbor for personal services and management contracts (the “Personal Services and Management Safe Harbor”), the Personal Services and Management Safe Harbor requires, among other things, that the amount of the aggregate compensation paid to the manager over the term of the agreement be set in advance. Because our management fees are generally based on a percentage of revenue, our management agreements do not typically meet this requirement. We do, however, believe that our management arrangements satisfy the other requirements of the Personal Services and Management Safe Harbor for personal services and management contracts. The OIG has taken the position in several advisory opinions that percentage-based management agreements are not protected by a safe harbor, and consequently, may violate the Anti-Kickback Statute. We have implemented formal compliance programs designed to safeguard against overbilling and believe that our management agreements comply with the requirements of the Anti-Kickback Statute. However, we cannot assure you that the OIG would find our compliance programs to be adequate or that our management agreements would be found to comply with the Anti-Kickback Statute.
Certain of our ASCs have entered into arrangements for professional services, including arrangements for anesthesia services. In a Special Advisory Bulletin issued in April 2003, the OIG focused on “questionable” contractual arrangements where a health care provider in one line of business (the “Owner”) expands into a related health care business by contracting with an existing provider of a related item or service (the “Manager/Supplier”) to provide the new item or service to the Owner’s existing patient population, including federal health care program patients (so called “suspect Contractual Joint Ventures”). The Manager/Supplier not only manages the new line of business, but may also supply it with inventory, employees, space, billing, and other services. In other words, the Owner contracts out substantially the entire operation of the related line of business to the Manager/Supplier-otherwise a potential competitor-receiving in return the profits of the business as remuneration for its referrals. Through an Advisory Opinion, the OIG extended this suspect contractual joint venture analysis to arrangements between anesthesiologists and physician owners of ASCs. In Advisory Opinion 12-06, the OIG concluded that certain proposed arrangements between anesthesia groups and physician-owned ASCs could result in prohibited remuneration under the federal Anti-Kickback Statute. We believe our arrangements for anesthesia services are distinguishable from those described in Advisory Opinion 12-06 (May 25, 2012) and are in compliance with the requirements of the federal Anti-Kickback Statute. However, we cannot assure you that regulatory authorities would agree with that position.
We also may guarantee a surgical facility’s third-party debt financing and certain lease obligations as part of our obligations under a management agreement. Physician investors are generally not required to enter into similar guarantees. The OIG might take the position that
17
the failure of the physician investors to enter into similar guarantees represents a special benefit to the physician investors given to induce patient referrals and that such failure constitutes a violation of the Anti-Kickback Statute. We believe that the management fees (and in some cases guarantee fees) are adequate compensation to us for the credit risk associated with the guarantees and that the failure of the physician investors to enter into similar guarantees does not create a material risk of violating the Anti-Kickback Statute. However, the OIG has not issued any guidance in this regard.
The OIG is authorized to issue advisory opinions regarding the interpretation and applicability of the Anti-Kickback Statute, including whether an activity constitutes grounds for the imposition of civil or criminal sanctions. We have not, however, sought such an opinion regarding any of our arrangements. If it were determined that our activities, or those of our surgical facilities or hospitals, violate the Anti-Kickback Statute, we, our subsidiaries, our officers, our directors and each surgical facility and hospital investor could be subject, individually, to substantial monetary liability, prison sentences and/or exclusion from participation in any healthcare program funded in whole or in part by the U.S. government, including Medicare, Medicaid, TRICARE or state healthcare programs.
Evolving interpretations of current, or the adoption of new, federal or state laws or regulations could affect many of our arrangements. Law enforcement authorities, including the OIG, the courts and Congress, are increasing their scrutiny of arrangements between healthcare providers and potential referral sources to ensure that the arrangements are not designed as a mechanism to exchange remuneration for patient care referrals or opportunities. Investigators have also demonstrated a willingness to look behind the formalities of a business transaction to determine the underlying purposes of payments between healthcare providers and potential referral sources.
Federal Physician Self-Referral Law
Congress has enacted the federal physician self-referral law, or Stark Law, that prohibits certain self-referrals for healthcare services. As currently enacted, the Stark Law prohibits a practitioner, including a physician, dentist or podiatrist, from referring patients to an entity with which the practitioner or a member of his or her immediate family has a “financial relationship” for the provision of certain “designated health services” that are paid for in whole or in part by Medicare or Medicaid unless an exception applies. The term “financial relationship” is broadly defined and includes most types of ownership and compensation relationships. The Stark Law also prohibits the entity from seeking payment from Medicare or Medicaid for services that are rendered through a prohibited referral. If an entity is paid for services provided through a prohibited referral, it may be required to refund the payments. Violations of the Stark Law may also result in the imposition of damages equal to three times the amount improperly claimed and civil monetary penalties of up to $15,000 per prohibited claim and $100,000 per prohibited circumvention scheme and exclusion from participation in the Medicare and Medicaid programs. For the purposes of the Stark Law, the term “designated health services” is defined to include:
• | clinical laboratory services; |
• | physical therapy services; |
• | occupational therapy services; |
• | radiology services, including magnetic resonance imaging, computerized axial tomography scan and ultrasound services; |
• | radiation therapy services and supplies; |
• | durable medical equipment and supplies; |
• | parenteral and enteral nutrients, equipment and supplies; |
• | prosthetics, orthotics and prosthetic devices and supplies; |
• | home health services; |
• | outpatient prescription drugs; and |
• | inpatient and outpatient hospital services. |
The list of designated health services does not, however, include surgical services that are provided in ASCs. Furthermore, in final Stark Law regulations published by HHS on January 4, 2001, the term “designated health services” was specifically defined to not include services that are reimbursed by Medicare as part of a composite rate, such as services that are provided in ASCs. However, if designated health services are provided by an ambulatory surgery center and separately billed, referrals to the ambulatory surgery center by a physician-investor would be prohibited by the Stark Law. Because our facilities that are licensed as ASCs do not have independent laboratories and do not provide designated health services apart from surgical services, we do not believe referrals to these facilities by physician-investors are prohibited. If legislation or regulations are implemented that prohibit physicians from referring patients to surgical facilities in which the physician has a beneficial interest, our business and financial results would be materially adversely affected.
Five of our facilities are licensed as hospitals as of December 31, 2015. The Stark Law currently includes the Whole Hospital Exception, which applies to physician ownership of a hospital, provided such ownership is in the whole hospital and the physician is authorized to perform services at the hospital. We believe that physician investments in our facilities licensed as hospitals meet this requirement. However, changes to the Whole Hospital Exception have been the subject of recent regulatory action and legislation. Changes in the Affordable Care Act include:
• | a prohibition on hospitals from having any physician ownership unless the hospital already had physician ownership and a Medicare provider agreement in effect as of December 31, 2010; |
• | a limitation on the percentage of total physician ownership or investment interests in the hospital or entity whose assets include the hospital to the percentage of physician ownership or investment as of March 23, 2010; |
18
• | a prohibition from expanding the number of beds, operating rooms, and procedure rooms for which it is licensed after March 23, 2010, unless the hospital obtains an exception from the Secretary; |
• | a requirement that return on investment be proportionate to the investment by each investor; |
• | restrictions on preferential treatment of physician versus non-physician investors; |
• | a requirement for written disclosures of physician ownership interests to the hospital’s patients and on the hospital’s website and in any advertising, along with annual reports to the government detailing such interests; |
• | a prohibition on the hospital or other investors from providing financing to physician investors; |
• | a requirement that any hospital that does not have 24/7 physician coverage inform patients of this fact and receive signed acknowledgments from the patients of the disclosure; and |
• | a prohibition on “grandfathered” status for any physician owned hospital that converted from an ASC to a hospital on or after March 23, 2010. |
The Affordable Care Act also requires that each hospital with physician ownership submit an annual report of ownership and/or investment interest. Our hospitals have submitted their first reports. CMS has delayed the collection of the second report and publication of the first annual report. We cannot predict whether other proposed amendments to the Whole Hospital Exception will be included in any future legislation or if Congress will adopt any similar provisions that would prohibit or otherwise restrict physicians from holding ownership interests in hospitals. Any such changes could have an adverse effect on our financial condition and results of operations.
In addition to the physician ownership in our surgical facilities, we have other financial relationships with potential referral sources that potentially could be scrutinized under the Stark Law. We have entered into personal service agreements, such as medical director agreements, with physicians at our hospitals. We believe that our agreements with referral sources satisfy the requirements of the personal service arrangements exception to the Stark Law and have implemented formal compliance programs designed to ensure continued compliance. However, we cannot assure you that the OIG or CMS would find our compliance programs to be adequate or that our agreements with referral sources would be found to comply with the Stark Law.
False and Other Improper Claims
The U.S. government is authorized to impose criminal, civil and administrative penalties on any person or entity that files a false claim for payment from the Medicare or Medicaid programs or other federal and state healthcare programs. Claims filed with private insurers can also lead to criminal and civil penalties, including, but not limited to, penalties relating to violations of federal mail and wire fraud statutes, as well as penalties under the anti-fraud provisions of HIPAA. While the criminal statutes are generally reserved for instances of fraudulent intent, the U.S. government is applying its criminal, civil and administrative penalty statutes in an ever-expanding range of circumstances. For example, the U.S. government has taken the position that a pattern of claiming reimbursement for unnecessary services violates these statutes if the claimant merely should have known the services were unnecessary, even if the government cannot demonstrate actual knowledge. The U.S. government has also taken the position that claiming payment for low-quality services is a violation of these statutes if the claimant should have known that the care being provided was substandard.
Over the past several years, the U.S. government has investigated an increasing number of healthcare providers for potential violations of the federal False Claims Act. The federal False Claims Act prohibits a person from knowingly presenting, or causing to be presented, a false or fraudulent claim to the U.S. government. The statute defines “knowingly” to include not only actual knowledge of a claim’s falsity, but also reckless disregard for or intentional ignorance of the truth or falsity of a claim. The Fraud Enforcement and Recovery Act of 2009 further expanded the scope of the False Claims Act by, among other things, creating liability for knowingly and improperly avoiding or decreasing an obligation to pay money to the federal government. The Affordable Care Act also created federal False Claims Act liability for the knowing failure to report and return an overpayment within 60 days of the identification of the overpayment or the date by which a corresponding cost report is due, whichever is later. This requirement has led to an increasing use of the self-disclosure protocols that have been implemented by CMS, the OIG and other governmental agencies by the healthcare industry. The Affordable Care Act also provided that claims submitted in connection with patient referrals that result from violations of the Anti-Kickback Statute constitute false claims for the purposes of the federal False Claims Act, and some courts have held that a violation of the Stark Law can result in False Claims Act liability as well. Because our surgical facilities perform hundreds of similar procedures a year for which they are paid by Medicare and other government health care programs, and there is a relatively long statute of limitations, a billing error or cost reporting error could result in significant civil or criminal penalties.
Under the qui tam, or whistleblower, provisions of the False Claims Act, private parties may bring actions on behalf of the U.S. government. These private parties, often referred to as relators, are entitled to share in any amounts recovered by the government through trial or settlement. Both whistleblower lawsuits and direct enforcement activity by the government have increased significantly in recent years and have increased the risk that a healthcare company, like us, will have to defend a false claims action, pay fines or be excluded from the Medicare and Medicaid programs and other federal and state healthcare programs as a result of an investigation resulting from a whistleblower case. Although we believe that our operations materially comply with both federal and state laws, they may nevertheless be the subject of a whistleblower lawsuit or may otherwise be challenged or scrutinized by governmental authorities. Providers found liable for False Claims Act violations are subject to damages of up to three times the actual damage sustained by the government plus mandatory civil monetary penalties between $5,500 and $11,000 for each separate false claim. A determination that we have violated these laws could have a material adverse effect on us.
Other Fraud and Abuse Laws
The Medicare Patient and Program Protection Act of 1987, as amended by the Health Insurance Portability and Accountability Act of 1996, (“HIPAA”), and the Balanced Budget Act of 1997, impose civil monetary penalties and exclusion from state and federal healthcare
19
programs on providers who commit violations of fraud and abuse laws. HIPAA authorizes the Secretary of the Department of Health & Human Services (“Secretary”), and in some cases requires the Secretary, to exclude individuals and entities that the Secretary determines have “committed an act” in violation of applicable fraud and abuse laws or improperly filed claims in violation of such laws from participating in any federal healthcare program. HIPAA also expanded the Secretary’s authority to exclude a person involved in fraudulent activity from participating in a program providing health benefits, whether directly or indirectly, in whole or in part, by the U.S. government. Additionally, under HIPAA, individuals who hold a direct or indirect ownership or controlling interest in an entity that is found to violate these laws may also be excluded from Medicare and Medicaid and other federal and state healthcare programs if the individual knew or should have known, or acted with deliberate ignorance or reckless disregard of, the truth or falsity of the information of the activity leading to the conviction or exclusion of the entity, or where the individual is an officer or managing employee of such entity. This standard does not require that specific intent to defraud be proven by OIG. Under HIPAA it is also a crime to defraud any commercial healthcare benefit program.
Federal and State Privacy and Security Requirements
On January 16, 2009, CMS published its 10th Edition of International Statistical Classification of Diseases and Related Health Problems (“ICD-10”) and related changes to the formats used for certain electronic transactions. ICD-10 contains significantly more diagnostic and procedural codes than the existing ICD-9 coding system, and as a result, the coding for the services provided in our surgical facilities and hospitals require much greater specificity. ICD-10 has required a significant investment in technology and training. As a result, we may experience delays in reimbursement while our surgical facilities and the payors from which we seek reimbursement make the transition and adjustment to ICD-10. We have met CMS’s October 1, 2015 deadline for ICD-10 implementation.
We are subject to HIPAA, including The HITECH Act, which was enacted as part of The American Recovery and Reinvestment Act of 2009. The HITECH Act strengthened the requirements and significantly increased the penalties for violations of the HIPAA privacy and security regulations. On January 25, 2013, HHS issued the HIPAA Omnibus Rule, which became effective on March 26, 2013. Prior to the HIPAA Omnibus Rule, the HITECH Act required us to notify patients of any unauthorized access, acquisition, or disclosure of their unsecured protected health information that poses significant risk of financial, reputational or other harm to a patient. The HIPAA Omnibus Rule eliminated this harm threshold standard and instead we are now required to notify patients of any unauthorized access, acquisition, or disclosure of their unsecured protected health information in all situations except those in which we can demonstrate that there is a low probability that the protected health information has been compromised. We now have the burden of demonstrating through a risk assessment that a breach of protected health information has not occurred. This new more objective standard may lead to an increased number of occurrences that require breach notifications. In addition, the HIPAA Omnibus Rule also modified the following aspects of the HIPAA privacy and security regulations:
• | makes our facilities’ business associates directly liable for compliance with certain of HIPAA’s requirements; |
• | makes our facilities liable for violations by their business associates if HHS determines an agency relationship exists between the facility and the business associate under federal agency law; |
• | adds limitations on the use and disclosure of health information for marketing and fund-raising purposes, and prohibits the sale of protected health information without individual authorization; |
• | expands our patients’ rights to receive electronic copies of their health information and to restrict disclosures to a health plan concerning treatment for which our patient has paid out of pocket in full; |
• | requires modifications to, and redistribution of, our facilities’ notice of privacy practices; |
• | requires modifications to existing agreements with business associates; |
• | adopts the additional HITECH Act provisions not previously adopted addressing enforcement of noncompliance with HIPAA due to willful neglect; |
• | incorporates the increased and tiered civil money penalty structure provided by the HITECH Act; and |
• | revises the HIPAA privacy rule to increase privacy protections for genetic information as required by the Genetic Information Nondiscrimination Act of 2008. |
The HIPAA privacy standards apply to individually identifiable information held or disclosed by a covered entity in any form, whether communicated electronically, on paper or orally. These standards impose extensive administrative requirements on us. These standards require our compliance with rules governing the use and disclosure of this health information. They create rights for patients in their health information, such as the right to amend their health information, and they require us to impose these rules, by contract, on any business associate to whom we disclose such information in order to perform functions on our behalf.
The HIPAA security standards require us to establish and maintain reasonable and appropriate administrative, technical and physical safeguards to ensure the integrity, confidentiality and the availability of electronic protected health and related financial information. Although the security standards do not reference or advocate a specific technology, and covered healthcare providers, plans and clearinghouses have the flexibility to choose their own technical solutions, the security standards have required us to implement significant new systems, business procedures and training programs.
Violations of the HIPAA privacy and security regulations may result in civil and criminal penalties. The HITECH Act strengthened the requirements of the HIPAA privacy and security regulations and significantly increased the penalties for violations by introducing a tiered penalty system, with penalties of up to $50,000 per violation with a maximum civil penalty of $1.5 million in a calendar year for violations of the same requirement. However, a single breach incident can result in violations of multiple requirements, resulting in possible penalties well in excess of $1.5 million. Under the HITECH Act, HHS is required to conduct periodic compliance audits of covered entities and their
20
business associates. The HITECH Act and the HIPAA Omnibus Rule also extend the application of certain provisions of the security and privacy regulations to business associates and subjects business associates to civil and criminal penalties for violation of the regulations.
The HITECH Act authorizes State Attorneys General to bring civil actions seeking either an injunction or damages in response to violations of HIPAA privacy and security regulations or the new data breach law that affects the privacy of their state residents. We expect vigorous enforcement of the HITECH Act’s requirements by HHS and State Attorneys General. Additionally, HHS conducted a pilot audit program that concluded December 2012 in the first phase of HHS’ implementation of the HITECH Act’s requirements of periodic audits of covered entities and business associates to ensure their compliance with the HIPAA privacy and security regulations. HHS has allocated increased funding towards HIPAA enforcement activity and such enforcement activity has seen a marked increase over recent years. We cannot predict whether our surgical facilities will be able to comply with the final rules and the financial impact to our surgical facilities in implementing the requirements under the final rules when they take effect, or whether our hospitals will be selected for an audit, or the results of such an audit.
Our facilities also remain subject to any state laws that relate to privacy or the reporting of data breaches that are more restrictive than the regulations issued under HIPAA and the requirements of the HITECH Act. For example, various state laws and regulations may require us to notify affected individuals in the event of a data breach involving certain personal information, such as social security numbers, dates of birth and credit card information.
Adoption of Electronic Health Records
The HITECH Act includes provisions designed to increase the use of EHR by both physicians and hospitals. Beginning in 2011 and extending through 2016, eligible hospitals may receive incentive payments based upon successfully demonstrating meaningful use of its certified EHR technology. Beginning in 2015, those hospitals that do not successfully demonstrate meaningful use of EHR technology are subject to reduced payments from Medicare. EHR meaningful use objectives and measures that hospitals and physicians must meet in order to qualify for incentive payments will be implemented in three stages. Stage 1 has been in effect since 2011 and Stage 2 took effect for hospitals beginning in fiscal year 2014. On October 16, 2015, CMS published a final rule that consolidated Stage 1 and Stage 2 into a “Modified Stage 2” effective as of 2015 and set out requirements for Stage 3, which is set to take full effect in 2018. In connection with the acquisition of Symbion, we acquired six surgical facilities that are licensed as hospitals, five of which we own as of December 31, 2015. These hospitals began the implementation of EHR initiatives in 2012. We strive to comply with the EHR meaningful use requirements of the HITECH Act so as to qualify for incentive payments. Continued implementation of EHR and compliance with the HITECH Act will result in significant costs. We recorded income from electronic health record incentives of $1.8 million and $3.4 million which was recognized during the years ended December 31, 2015 and 2014, respectively. We incurred negligible costs for hardware, software and implementation expenses during the same periods. We do not currently know the extent of additional costs that will be associated with implementation of additional systems or the amount of future incentives that we will receive.
HIPAA Administrative Simplification Requirements
The HIPAA transaction regulations were issued to encourage electronic commerce in the healthcare industry. These regulations include standards that healthcare providers must follow when electronically transmitting certain healthcare transactions, such as healthcare claims.
Emergency Medical Treatment and Active Labor Act
Our hospitals are subject to the Emergency Medical Treatment and Active Labor Act (“EMTALA”). This federal law requires any hospital that participates in the Medicare program to conduct an appropriate medical screening examination of every person who presents to the hospital’s emergency department for treatment and, if the patient is suffering from an emergency medical condition, to either stabilize that condition or make an appropriate transfer of the patient to a facility that can handle the condition. The obligation to screen and stabilize emergency medical conditions or transfer exists regardless of a patient’s ability to pay for treatment. Off-campus facilities such as surgery centers that lack emergency departments or otherwise do not treat emergency medical conditions generally are not subject to EMTALA. They must, however, have policies in place that explain how the location should proceed in an emergency situation, such as transferring the patient to the closest hospital with an emergency department. There are severe penalties under EMTALA if a hospital fails to screen or appropriately stabilize or transfer a patient or if the hospital delays appropriate treatment in order to first inquire about the patient’s ability to pay, including civil monetary penalties and exclusion from participation in the government health care programs. In addition, an injured patient, the patient’s family or a medical facility that suffers a financial loss as a direct result of another hospital’s violation of the law can bring a civil suit against that other hospital. CMS has actively enforced EMTALA and has indicated that it will continue to do so in the future. Although we believe that our hospitals comply with EMTALA, we cannot predict whether CMS will implement new requirements in the future and, if so, whether our hospitals will comply with any new requirements.
State Regulation
Many of the states in which our surgical facilities operate have adopted statutes and/or regulations that prohibit the payment of kickbacks or any type of remuneration in exchange for patient referrals and that prohibit healthcare providers from, in certain circumstances, referring a patient to a healthcare facility in which the provider has an ownership or investment interest. While these statutes generally mirror the federal Anti-Kickback Statute and Stark Law, they vary widely in their scope and application. Some are specifically limited to healthcare services that are paid for in whole or in part by the Medicaid program; others apply to all healthcare services regardless of payor; and others apply only to state-defined designated services, which may differ from the designated health services under the Stark Law. In addition, many states have adopted statutes that mirror the False Claims Act and that prohibit the filing of a false or fraudulent claim with a state governmental agency. We intend to comply with all applicable state healthcare laws, rules and regulations. However, these laws, rules and regulations have typically been the subject of limited judicial and regulatory interpretation. As a result, we cannot assure you that our surgical facilities will not be investigated or scrutinized by the governmental authorities empowered to do so or, if challenged, that their activities would be found to be lawful. A determination of non-compliance with the applicable state healthcare laws, rules, and regulations could subject our surgical facilities to civil and criminal penalties and could have a material adverse effect on our operations.
21
We are also subject to various state insurance statutes and regulations that prohibit us from submitting inaccurate, incorrect or misleading claims. Many state insurance laws and regulations are broadly worded and could be implicated, for example, if our surgical facilities were to adjust an out-of-network co-payment or other patient responsibility amounts without fully disclosing the adjustment on the claim submitted to the payor. While some of our surgical facilities adjust the out-of-network costs of patient co-payment and deductible amounts to reflect in-network co-payment costs when providing services to patients whose health insurance is covered by a payor with which the surgical facilities are not contracted, our policy is to fully disclose adjustments in the claims submitted to the payors. We believe that our surgical facilities are in compliance with all applicable state insurance laws and regulations regarding the submission of claims. We cannot assure you, however, that none of our surgical facilities’ insurance claims will ever be challenged. If we were found to be in violation of a state’s insurance laws or regulations, we could be forced to discontinue the violative practice, which could have an adverse effect on our financial position and results of operations, and we could be subject to fines and criminal penalties.
Fee Splitting; Corporate Practice of Medicine
The laws of many states prohibit physicians from splitting fees with non-physicians (i.e., sharing in a percentage of professional fees), prohibit non-physician entities (such as us) from practicing medicine and exercising control over or employing physicians and prohibit referrals to facilities in which physicians have a financial interest. The existence, interpretation and enforcement of these laws vary significantly from state to state. In light of these restrictions, in certain states we facilitate the provision of physician services by maintaining long-term management services agreements through our subsidiaries with affiliated professional contractors, which employ or contract with physicians and other healthcare professionals to provide physician professional services. Under these arrangements, our subsidiaries perform only non-medical administrative services, do not represent that they offer medical services and do not exercise influence or control over the practice of medicine by the physicians employed by the affiliated professional contractors. Although we believe that the fees we receive from affiliated professional contractors have been structured in a manner that is compliant with applicable fee-splitting laws, it is possible that a government regulator could interpret such fee arrangements to be in violation of certain fee-splitting laws. Future interpretations of, or changes in, these laws might require structural and organizational modifications of our existing relationships, and we cannot assure you that we would be able to appropriately modify such relationships. In addition, statutes in some states could restrict our expansion into those states.
Clinical Laboratory Regulation
Our clinical laboratories are subject to federal oversight under the Clinical Laboratory Improvement Amendments of 1988 (“CLIA”) which extends federal oversight to virtually all clinical laboratories by requiring that they be certified by the federal government or by a federally-approved accreditation agency. CLIA requires that all clinical laboratories meet quality assurance, quality control and personnel standards. Laboratories also must undergo proficiency testing and are subject to inspections. Standards for testing under CLIA are based on the complexity of the tests performed by the laboratory, with tests classified as “high complexity,” “moderate complexity,” or “waived.” Laboratories performing high complexity testing are required to meet more stringent requirements than moderate complexity laboratories. Laboratories performing only waived tests, which are tests determined by the Food and Drug Administration to have a low potential for error and requiring little oversight, may apply for a certificate of waiver exempting them from most of the requirements of CLIA. Our operations also subject to state and local laboratory regulation. CLIA provides that a state may adopt laboratory regulations different from or more stringent than those under federal law, and a number of states have implemented their own laboratory regulatory requirements. State laws may require that laboratory personnel meet certain qualifications, specify certain quality controls, or require maintenance of certain records. We believe that we are in material compliance with all applicable laboratory requirements, but no assurances can be given that our laboratories will pass all future licensure or certification inspections.
Regulatory Compliance Program
It is our policy to conduct our business with integrity and in compliance with the law. We have in place and continue to enhance a company-wide compliance program that focuses on all areas of regulatory compliance including billing, reimbursement, cost reporting practices and contractual arrangements with referral sources.
This regulatory compliance program is intended to help ensure that high standards of conduct are maintained in the operation of our business and that policies and procedures are implemented so that employees act in full compliance with all applicable laws, regulations and company policies. Under the regulatory compliance program, every employee and certain contractors involved in patient care, and coding and billing, receive initial and periodic legal compliance and ethics training. In addition, we regularly monitor our ongoing compliance efforts and develop and implement policies and procedures designed to foster compliance with the law. The program also includes a mechanism for employees to report, without fear of retaliation, any suspected legal or ethical violations to their supervisors, designated compliance officers in our facilities, our compliance hotline or directly to our corporate compliance office. We believe our compliance program is consistent with standard industry practices. However, we cannot provide any assurances that our compliance program will detect all violations of law or protect against qui tam suits or government enforcement actions.
Where You Can Find More Information
As a result of the initial public offering of the shares of our common stock, we must now file reports and other information with the SEC, such as Annual Reports on Form 10-K, Quarterly Reports on Form 10-Q and Current Reports on Form 8-K. Such reports (and amendments to those reports), along with certain other Company filings and information, can be inspected and copied at the Public Reference Room of the SEC located at 100 F Street, N.E., Washington, D.C. 20549. Copies of such materials can be obtained from the Public Reference Room of the SEC at prescribed rates. You can call the SEC at 1-800-SEC-0330 to obtain information on the operation of the Public Reference Room. Such materials may also be accessed electronically by means of the SEC’s website at www.sec.gov.
22
Item 1A. Risk Factors
We are subject to risks and uncertainties that could cause our actual financial condition, results of operations, business and prospects to differ materially from those contemplated by the forward-looking statements contained in this report or our other filings with the SEC. Some of these risks and uncertainties are discussed below. If any of the following risks, or other risks and uncertainties, actually occurred, our business, financial condition and operating results could suffer.
Risks Related to Our Business and Industry
We depend on payments from third-party payors, including government healthcare programs and managed care organizations. If these payments are reduced or eliminated, our revenue and profitability could be materially and adversely affected.
We depend upon private and governmental third-party sources of payment for the services provided by physicians in our physician network, to patients in our surgical facilities and by our laboratory and diagnostic services. The amount that we receive in payment for our services may be adversely affected by market and cost factors that we do not control, including Medicare, Medicaid and state regulation changes, cost containment decisions and changes in reimbursement schedules of payors, legislative changes, refinements to the Medicare Ambulatory Surgery Center payment system and refinements made by CMS to Medicare’s reimbursement policies. For instance, cuts to the federal budget caused a 2.0% reduction in Medicare provider payments starting in 2013. Similarly, third-party payors may be successful in negotiating reduced reimbursement schedules with our facilities. Fixed fee schedules, capitation payment arrangements, exclusion from participation in or inability to reach agreements with managed care programs, reduction or elimination of payments or an increase in the payments at a rate that is less than the increase in our costs, or other factors affecting payments for healthcare services over which we have no control could have a material adverse effect on our business, prospects, results of operations and financial condition.
If we are unable to negotiate and enter into favorable contracts or maintain satisfactory relationships and renew existing contracts on favorable terms with managed care organizations or other private third-party payors, our revenue and profitability may decrease.
Payments from private third-party payors, including state workers’ compensation programs and managed care organizations, represented 55.0%, 52.1% and 60.6% of our patient service revenue for the years ended December 31, 2015, 2014 and 2013, respectively. Most of these payments came from third-party payors with which our facilities have contracts. Managed care companies such as HMOs and PPOs, which offer prepaid and discounted medical service packages, represent a growing segment of private third-party payors. If we fail to enter into favorable contracts or maintain satisfactory relationships with managed care organizations, our revenue may decrease. Our competitive position has been, and will continue to be, affected by initiatives undertaken during the past several years by major purchasers of healthcare services, including insurance companies and employers, to revise payment methods and monitor healthcare expenditures in an effort to contain healthcare costs. For instance, managed care payors may lower reimbursement rates in response to increased obligations on payors imposed by the Affordable Care Act or future reductions in Medicare reimbursement rates. Further, managed care payors may narrow their provider networks in response to the need to negotiate lower reimbursement rates with providers. If we are unable to maintain strong relationships with payors, we may not be able to ensure participation in these narrow provider networks. Cost containment measures, such as fixed fee schedules, capitation payment arrangements, reductions in reimbursement schedules by third-party payors and closed provider networks, could also cause a reduction of our revenue in the future.
Some of our payments from third-party payors come from third-party payors with which our surgical facilities, physicians or subsidiaries that provide diagnostic services do not have a contract. In those cases where we provide services to a patient that does not use a third-party payor with which we have contracted, commonly known as “out-of-network” services, we generally charge the patients the same co-payment or other patient responsibility amounts that we would have charged had our surgical facilities had a contract with the payor. In accordance with insurance laws and regulations, we submit a claim for the services to the payor along with full disclosure that our surgical facility has charged the patient an in-network patient responsibility amount. Historically, those third-party payors who do not have contracts with our surgical facilities typically have paid our claims at higher than comparable contracted rates. However, over the past five years we have observed an increase in third-party payors adopting out-of-network fee schedules that are more comparable to our contracted rates or to take other steps to discourage their enrollees from seeking treatment at out-of-network surgical facilities. In these cases, we seek to enter into contracts with the payors.
Payments from workers’ compensation payors represented approximately 7% of our patient service revenue for the year ended December 31, 2015. A majority of states have implemented workers’ compensation provider fee schedules. In some cases, the fee schedule rates contain lower rates than the rates our surgical facilities have historically been paid for the same services. If states reduce the amounts paid to providers under the workers’ compensation fee schedules, it could have a material adverse effect on our financial condition and results of operations.
Significant changes in our payor mix or surgical case mix resulting from fluctuations in the types of cases performed at our facilities could have a material adverse effect on our business, prospects, results of operations and financial condition.
Our results may change from period to period due to fluctuations in payor mix or surgical case mix or other factors relating to the type of cases performed by physicians at our facilities. Payor mix refers to the relative share of total cases provided to patients with no insurance, commercial insurance, Medicare coverage, Medicaid coverage and workers’ compensation insurance, respectively. Since, generally speaking, we receive relatively higher payment rates from commercial and workers’ compensation insurers than Medicare, Medicaid and other government-funded programs, a significant shift in our payor mix toward a higher percentage of Medicare and Medicaid cases, which could occur for reasons beyond our control, could have an adverse effect on our business, prospects, results of operations and financial condition.
Surgical case mix refers to the relative share of total cases performed by specialty, such as ENT, GI, general surgery, ophthalmology, orthopedic, cardiology and pain management. Generally speaking, certain types of our cases, such as orthopedic cases, generate relatively
23
higher revenue than other types of cases, such as pain management and GI cases. Therefore, a significant shift in our surgical case mix toward a higher percentage of lower revenue cases, which could occur for reasons beyond our control, could result in a material adverse effect on our business, prospects, results of operations and financial condition.
As we operate in multiple markets, each with a different competitive landscape, shifts within our payor mix or surgical case mix may not be uniform across all of our affiliated facilities. Rather, these shifts may be concentrated within certain markets due to local competitive factors. Therefore, the results of our individual affiliated facilities, including facilities that are material to our results, may be volatile, which could result in a material adverse effect on our business, prospects, results of operations and financial condition.
Should we fail to continue to successfully integrate the operations of Surgery Partners and legacy Symbion, our results of operations and profitability could be materially and adversely impacted.
We may not continue to be successful in integrating the operations of Surgery Partners and legacy Symbion, and the combined company may not perform as we expect or achieve the net cost savings and other synergies that we anticipate. A significant element of our business strategy is the improvement of our operating efficiencies and a reduction of our operating costs. A variety of factors could cause us not to achieve the benefits of the cost savings plan, or could result in harm to our business, including delays in the anticipated timing of activities related to our cost savings plan and our inability to reduce corporate and administrative expenses. As a result, we may not achieve our expected cost savings in the time anticipated, or at all. In such case, our results of operations and profitability could be negatively impaired.
We have a history of net losses and may not achieve or sustain profitability in the future.
Although we have a net income in 2015 of $1.4 million, we have historically incurred periods of net losses, including net losses of approximately $65.9 million in 2014, which includes a $21.7 million loss attributable to a one-time transaction cost associated with the acquisition of Symbion and a loss on debt extinguishment of $23.4 million and net losses of $9.1 million in 2013, which includes a loss on debt extinguishment of $9.9 million. We cannot assure you that our revenue will grow or that we will achieve or maintain profitability in the future. Growth of our revenue may slow or revenue may decline and expenses may increase for a number of possible reasons, including reduced demand for our services, regulatory shifts, failure to successfully continue to integrate the operations of Surgery Partners and Symbion and other risks and uncertainties. Even if we have achieved profitability during 2015, we may not sustain or increase profitability on a quarterly or annual basis in the future. Our ability to achieve profitability will be affected by the other risks and uncertainties described in this section and in “Management’s Discussion and Analysis of Financial Condition and Results of Operations.” All of these factors could contribute to further net losses and, if we are unable to meet these risks and challenges as we encounter them, our business may suffer. If we are not able to achieve, sustain or increase profitability, our business will be adversely affected and our stock price may decline.
We depend on physician utilization of our surgical facilities, which could decrease if we fail to maintain good relationships with affiliated physicians. Our ability to provide medical services at our facilities would be impaired and our revenue reduced if we are not able to maintain these relationships.
Our business depends, among other things, upon the efforts and success of affiliated physicians who provide medical services at our surgical facilities and the strength of our relationships with these physicians. Most physicians are not employees of our surgical facilities and are not contractually required to use our facilities. We generally do not enter into contracts with physicians who use our surgical facilities, other than partnership and operating agreements with physicians who own interests in our surgical facilities, provider agreements with anesthesiology groups that provide anesthesiology services in our surgical facilities, medical director agreements, among others. Physicians who use our surgical facilities also use other facilities or hospitals and may choose to perform procedures in an office-based setting that might otherwise be performed at our surgical facilities. In recent years, pain management and gastrointestinal procedures have been performed increasingly in an office-based setting because of potential cost savings or better access. Although physicians who own interests in our surgical facilities are subject to agreements restricting ownership of competing facilities, these agreements may not restrict procedures performed in a physician office or in other unrelated facilities. Also, these agreements restricting ownership of competing facilities are difficult to enforce, and we may be unsuccessful in preventing physicians who own interests in our surgical facilities from acquiring interests in competing facilities.
The financial success of our facilities is in part dependent upon the volume of procedures performed by the physicians who use our facilities, which is affected by the economy, healthcare reform, increases in patient co-payments and deductibles and other factors outside our or their control. The physicians who use our surgical facilities may choose not to accept patients who pay for services through certain third-party payors, which could reduce our revenue. From time to time, we may have disputes with physicians who use our surgical facilities and/or own interests in our surgical facilities or our Company. Our revenue and profitability could be significantly reduced if we lost our relationship with one or more key physicians or groups of physicians, or if such physicians or groups reduce their use of any of our surgical facilities. In addition, any damage to the reputation of a key physician or group of physicians or the failure of these physicians to provide quality medical care or adhere to professional guidelines at our surgical facilities could damage our reputation, subject us to liability and significantly reduce our revenue.
Physician treatment methodologies and governmental or commercial health insurance controls designed to reduce the number of surgical procedures may reduce our revenue and profitability.
Controls imposed by Medicare and Medicaid, employer-sponsored healthcare plans and commercial health insurance payors designed to reduce surgical volumes, in some instances referred to as “utilization review,” could adversely affect our facilities. Although we are unable to predict the effect these changes will have on our operations, significant limits on the scope of services reimbursed and on reimbursement rates and fees may reduce our revenue and profitability. Additionally, trends in physician treatment protocols and commercial health insurance plan design, such as plans that shift increased costs and accountability for care to patients, could reduce our surgical volumes in favor of lower intensity and lower cost treatment methodologies, each of which could, in turn, have a material adverse effect on our business, prospects, results of operations and financial condition.
24
Our growth strategy depends in part on our ability to integrate operations of acquired surgical facilities, attract new physician partners, and to acquire and develop additional surgical facilities, on favorable terms. If we are unable to achieve any of these goals, our future growth could be limited and our operating results could be adversely affected.
We believe that an important component of our financial performance and growth is our ability to provide physicians who use our facilities with the opportunity to purchase ownership interests in our facilities. We may not be successful in attracting new physician investment in our surgical facilities, and that failure could result in a reduction in the quality, efficiency and profitability of our facilities. Based on competitive factors and market conditions, physicians may be able to negotiate relatively higher levels of equity ownership in our facilities, consequently limiting or reducing our share of the profits from these facilities. In addition, physician ownership in our facilities is subject to certain regulatory restrictions.
In addition, our growth strategy includes the acquisition and development of existing surgical facilities and the development of new surgical facilities jointly with local physicians and, in some cases, healthcare systems and other strategic partners. We have acquired interests in or developed all of our surgical facilities since our inception and we expect to continue to expand our operations in the future. We are currently evaluating potential acquisitions and development projects and expect to continue to evaluate acquisitions and development projects in the foreseeable future. If we are unable to successfully execute on this strategy in the future, our future growth could be limited. We may be unable to identify suitable acquisition and development opportunities, or to complete acquisitions and new projects in a timely manner and on favorable terms. Further, the companies or assets we acquire in the future may not ultimately produce returns that justify our related investment.
Our acquisition activities, and our limited development activities, require substantial capital resources, and we may need to obtain additional capital or financing, from time to time, to fund these activities. Historically, we have funded acquisition and development activities through our credit facilities. As a result, we may take actions that could have a material adverse effect on our business, prospects, results of operations and financial condition, including incurring substantial debt with certain restrictive terms. Further, sufficient capital or financing may not be available to us on satisfactory terms, if at all. In addition, our ability to acquire and develop additional surgical facilities may be limited by state certificate of need programs, licensure requirements, antitrust laws, and other regulatory restrictions on expansion. We also face significant competition from local, regional and national health systems and other owners of surgical facilities in pursuing attractive acquisition candidates. The limited number of surgical facilities we develop typically incur losses in their early months of operation (more so in the case of surgical hospitals) and, until their case loads grow, they generally experience lower total revenue and operating margins than established surgical facilities, and we expect this trend to continue.
If we are not successful in integrating newly acquired surgical facilities, we may not realize the potential benefits of such acquisitions. Likewise, if we are not able to integrate acquired facilities’ operations and personnel with ours in a timely and efficient manner, then the potential benefits of the transaction may not be realized. Further, any delays or unexpected costs incurred in connection with integration could have a material adverse effect on our operations and earnings. In particular, if we experience the loss of key personnel or if the effort devoted to the integration of acquired facilities diverts significant management or other resources from other operational activities, our operations could be impaired.
If we acquire or develop additional facilities, we may experience difficulty in retaining or integrating their operations, key physicians, systems and personnel. In some acquisitions, we may have to renegotiate, or risk losing, one or more of the facility’s commercial payor contracts. We may also be unable to immediately collect the accounts receivable of an acquired facility while we align the payors’ payment systems and accounts with our own systems. Certain transactions can require licensure changes which, in turn, result in disruptions in payment for services.
In addition, although we conduct extensive due diligence prior to the acquisition of surgical facilities and seek indemnification from prospective sellers covering unknown or contingent liabilities, we may acquire facilities with unknown or contingent liabilities, including liabilities for failure to comply with healthcare laws and regulations. Although we maintain professional liability insurance that provides coverage on a claims-made basis of $1.0 million per occurrence with a retention of $100,000 per occurrence and $3.0 million in annual aggregate coverage per surgical facility, we do not maintain insurance specifically covering all unknown or contingent liabilities that may have occurred prior to the acquisition of facilities. In some cases, our right to indemnification for these liabilities from the seller may be subject to negotiated limits or limits on our ability to enforce indemnification rights.
Our rapid growth has placed, and will continue to place, increased demands on our management, operational and financial information systems and other resources. Furthermore, expansions into new geographic markets and services may require us to comply with new and unfamiliar legal and regulatory requirements, which could impose substantial obligations on us and our management, cause us to expend additional time and resources, and increase our exposure to penalties or fines for non-compliance with such requirements. To accommodate our past and anticipated future growth, and to compete effectively, we will need to continue to improve our management, operational and financial information systems and to expand, train, manage and motivate our workforce. Our personnel, systems, procedures or controls may not be adequate to support our operations in the future. Further, focusing our financial resources and management attention on the expansion of our operations may negatively impact our financial results. Any failure to improve our management, operational and financial information systems, or to expand, train, manage or motivate our workforce, could reduce or prevent our growth.
Shortages of surgery-related products, equipment and medical supplies and quality control issues with such products, equipment and medical supplies could disrupt our operations and adversely affect our case volume, surgical case mix and profitability.
Our operations depend significantly upon our ability to obtain sufficient surgery-related products, drugs, equipment and medical supplies from suppliers on a timely basis. If we are unable to obtain such necessary products, or if we fail to properly manage existing inventory levels, the surgical facilities may be unable to perform certain surgeries, which could adversely affect case volume or result in a negative shift in surgical case mix. In addition, as a result of shortages, we could suffer, among other things, operational disruptions,
25
disruptions in cash flows, increased costs and reductions in profitability. At times, supply shortages have occurred in our industry, and such shortages may be expected to recur from time to time.
Medical supplies and services can also be subject to supplier product quality control incidents and recalls. In addition to contributing to materials shortages, product quality can affect patient care and safety. Material quality control incidents have occurred in the past and may occur again in the future, for reasons beyond our control, and such incidents can negatively impact case volume, product costs and our reputation. In addition, we may have to incur costs to resolve quality control incidents related to medical supplies and services regardless of whether they were caused by us. Our inability to obtain the necessary amount and quality of surgery-related products, equipment and medical supplies due to a quality control incident or recall could have a material adverse effect on our business, prospects, results of operations and financial condition.
We face competition for patients, physicians and commercial payor contracts.
The healthcare business is highly competitive and each of the individual geographic areas in which we operate has a different competitive landscape. In each of our markets we compete with other healthcare providers for patients and in contracting with commercial payors. In addition, because the number of physicians available to utilize and invest in our facilities is finite, we face intense competition from other surgery centers, hospitals, health systems and other healthcare providers in recruiting physicians to utilize and invest in our facilities. We are in competition with other surgery centers, hospitals and healthcare systems in the communities we serve to attract patients and provide them with the care they need.
There are also unaffiliated hospitals in each market in which we operate. These hospitals have established relationships with physicians and payors. In addition, other companies either currently are in the same or similar business of developing, acquiring and operating surgical facilities or may decide to enter our business. Many of these companies have greater resources than we do, including financial, marketing, staff and capital resources. We also may compete with some of these companies for entry into strategic relationships with healthcare systems and healthcare professionals. In addition, many physician groups develop surgical facilities without a corporate partner. In recent years, more physicians are choosing to perform procedures, including pain management and gastrointestinal procedures, in an office-based setting rather than in a surgical facility. If we are unable to compete effectively with any of these entities or groups, we may be unable to implement our business strategies successfully and our financial position and results of operations could be adversely affected.
Competition for physicians and nurses, shortages of qualified personnel or other factors could increase our labor costs and adversely affect our revenue, profitability and cash flows.
Our operations are dependent on the efforts, abilities and experience of our physicians and clinical personnel. We compete with other healthcare providers, primarily hospitals and other surgical facilities, in attracting physicians to utilize our surgical facilities, nurses and medical staff to support our surgical facilities, recruiting and retaining qualified management and support personnel responsible for the daily operations of each of our facilities and in contracting with managed care payors in each of our markets. In some markets, the lack of availability of clinical personnel, such as nurses, has become a significant operating issue facing all healthcare providers. This shortage may require us to continue to enhance wages and benefits to recruit and retain qualified personnel or to contract for more expensive temporary personnel. For the year-ended December 31, 2015, our salary and benefit expenses represented 27.3% of our revenue. We also depend on the available labor pool of semi-skilled and unskilled workers in each of the markets in which we operate.
If our labor costs increase, we may not be able to raise rates to offset these increased costs. Because a significant percentage of our revenue consist of fixed, prospective payments, our ability to pass along increased labor costs is limited. In particular, if labor costs rise at an annual rate greater than our net annual consumer price index basket update from Medicare, our results of operations and cash flows will likely be adversely affected. Any union activity at our facilities that may occur in the future could contribute to increased labor costs. Certain proposed changes in federal labor laws and the National Labor Relations Board’s modification of its election procedures could increase the likelihood of employee unionization attempts. Although none of our employees are currently represented by a collective bargaining agreement, to the extent a significant portion of our employee base unionizes, it is possible our labor costs could increase materially. Our failure to recruit and retain qualified management and medical personnel, or to control our labor costs, could have a material adverse effect on our business, prospects, results of operations and financial condition.
Some jurisdictions preclude us from entering into non-compete agreements with our physicians, and other non-compete agreements and restrictive covenants applicable to certain physicians and other clinical employees may not be enforceable.
We have contracts with physicians and other health professionals in many states. Some of our physician services contracts, as well as many of our physician services contracts with hospitals, include provisions preventing these physicians and other health professionals from competing with us both during and after the term of our contract with them. The law governing non-compete agreements and other forms of restrictive covenants varies from state to state. Some jurisdictions prohibit us from entering into non-compete agreements with our professional staff. Other states are reluctant to strictly enforce non-compete agreements and restrictive covenants against physicians and other healthcare professionals. Therefore, there can be no assurance that our non-compete agreements related to employed or otherwise contracted physicians and other health professionals will be enforceable if challenged in certain states. In such event, we would be unable to prevent former employed or otherwise contracted physicians and other health professionals from competing with us, potentially resulting in the loss of some of our hospital contracts and other business. Additionally, certain facilities have the right to employ or engage our providers after the termination or expiration of our contract with those facilities and cause us not to enforce our non-compete provisions related to those providers.
We may become involved in litigation which could negatively impact the value of our business.
From time-to-time we are involved in lawsuits, claims, audits and investigations, including those arising out of services provided, personal injury claims, professional liability claims, billing and marketing practices, employment disputes and contractual claims. We may become subject to future lawsuits, claims, audits and investigations that could result in substantial costs and divert our attention and
26
resources and adversely affect our business condition. In addition, since our current growth strategy includes acquisitions, among other things, we may become exposed to legal claims for the activities of an acquired business prior to the acquisition. These lawsuits, claims, audits or investigations, regardless of their merit or outcome, may also adversely affect our reputation and ability to expand our business.
In addition, from time to time we have received, and expect to continue to receive, correspondence from former employees terminated by us who threaten to bring claims against us alleging that we have violated one or more labor and employment regulations. In certain instances former employees have brought claims against us and we expect that we will encounter similar actions against us in the future. An adverse outcome in any such litigation could require us to pay contractual damages, compensatory damages, punitive damages, attorneys’ fees and costs.
If we become subject to large malpractice or other legal claims, we could be required to pay significant damages, which may not be covered by insurance.
In recent years, physicians, hospitals and other healthcare providers have become subject to an increasing number of legal actions alleging malpractice, product liability or related legal theories. Many of these actions involve large monetary claims and significant defense costs. We also owe certain defense and indemnity obligations to our officers and directors.
We maintain liability insurance in amounts that we believe are customary for the industry. Currently, we maintain professional liability insurance that provides coverage on a claims-made basis of $1.0 million per occurrence with a retention of $100,000 per occurrence and $3.0 million in annual aggregate coverage per surgical facility, including the facility and employed staff. We maintain general liability insurance that provides coverage on a occurrence basis of $1.0 million per occurrence with a retention of $25,000 per occurrence and $3.0 million in annual aggregate coverage per surgical facility. We also maintain business interruption insurance and property damage insurance. We also maintain business interruption insurance and property damage insurance. We also maintain business interruption insurance and property damage insurance, as well as an additional umbrella liability insurance policy in the aggregate amount of $35.0 million. Coverage under certain of these policies is contingent upon the policy being in effect when a claim is made regardless of when the events which caused the claim occurred. In addition, physicians who provide professional services in our surgical facilities are required to maintain separate malpractice coverage with similar minimum coverage limits. We also maintain a directors’ and officers’ insurance policy, which insures our directors and officers against unindemnified losses arising from certain wrongful acts in their capacities as directors and officers and reimburses us for those losses for which we have lawfully indemnified the directors and officers.
This insurance coverage may not cover all claims against us. Insurance coverage may not continue to be available at a cost allowing us to maintain adequate levels of insurance. If one or more successful claims against us were not covered by or exceeded the coverage of our insurance, our financial condition and results of operations could be adversely affected. Our business, profitability and growth prospects could suffer if we face negative publicity or we pay damages or defense costs in connection with a claim that is outside the scope or limits of coverage of any applicable insurance coverage, including claims related to adverse patient events, contractual disputes, professional and general liability, and directors’ and officers’ duties.
In addition, if our costs of insurance and claims increase, then our earnings could decline. Market rates for insurance premiums and deductibles have been steadily increasing. Our earnings and cash flows could be materially and adversely affected by any of the following:
• | the collapse or insolvency of our insurance carriers; |
• | further increases in premiums and deductibles; |
• | increases in the number of liability claims against us or the cost of settling or trying cases related to those claims; or |
• | an inability to obtain one or more types of insurance on acceptable terms, if at all. |
Financial pressures on patients, and current and future economic condition, may adversely affect our volume and surgical case mix.
Even as the U.S. economy shows signs of sustained, if modest, growth, many individuals throughout the country continue to experience difficult financial conditions. Our case volume and surgical case mix may be adversely affected by patients’ unwillingness to pay for procedures in our facilities. Higher numbers of unemployed individuals generally translates into more individuals without healthcare insurance to help pay for procedures, thereby increasing the potential for persons to elect not to have procedures performed. Even procedures normally thought to be non-elective may be delayed or may not be performed if the patient cannot afford the procedure due to a lack of insurance or money to pay their portion of our facilities’ fee. Although we have taken steps to minimize the impact of these conditions, it is difficult to predict the degree to which our business will continue to be impacted by such conditions or the course of the economy in the future.
In addition, the difficult conditions of the U.S. economy have adversely affected and could continue to adversely affect the budgets of individual states and the federal government, which has resulted in and could continue to result in attempts to reduce payments made to us by federal and state government healthcare programs, including Medicare, military services, Medicaid and workers’ compensation programs, a reduction in the scope of services covered by those programs and an increase in taxes and assessments on our activities. Additionally, even though the Supreme Court upheld an IRS rule extending tax credits to individuals purchasing health insurance under the Affordable Care Act through federally established exchanges in its decision in King v. Burwell, there continues to be uncertainty regarding the future implementation of the Affordable Care Act, and any such result could adversely affect our business by exacerbating the financial pressures on patients, leading them to further delay or cancel non-emergency surgical procedures.
Our surgical facilities are sensitive to regulatory, economic and other conditions in the states where they are located. In addition, three of our surgical facilities account for a significant portion of our patient service revenue.
Our revenue are particularly sensitive to regulatory, economic and other conditions in the states of Florida and Texas. As of December 31, 2015, we owned and operated four consolidated surgical facilities in Texas and 22 consolidated surgical facilities in Florida.
27
The Texas facilities represented 11.2%, 12.7% and 5.0% of our revenue during the years ended December 31, 2015, 2014 and 2013, respectively. The Florida facilities represented 14.9%, 14.3% and 30.9% of our revenue during the years ended December 31, 2015, 2014 and 2013, respectively.
In addition, our surgical hospital in Idaho Falls, Idaho represented 18.8% and 16.5% of our revenue during the years ended December 31, 2015 and 2014, respectively. This surgical hospital also provides ancillary services, including physician practices, radiation oncology and anesthesia services. If there were an adverse regulatory, economic or other development in any of the states in which we have a higher concentration of facilities, including Idaho, our case volumes could decline in such states or there could be other unanticipated adverse impacts on our business in those states, which could have a material adverse effect on our business, prospects, results of operations and financial condition.
If any of our existing healthcare facilities lose their accreditation status or any of our new facilities fail to receive accreditation, such facilities could become ineligible to receive reimbursement under Medicare or Medicaid or other third-party payors.
The construction and operation of healthcare facilities are subject to extensive federal, state and local regulation relating to, among other things, the adequacy of medical care, equipment, personnel, operating policies and procedures, fire prevention, rate-setting and compliance with building codes and environmental protection. Additionally, such facilities are subject to periodic inspection by government authorities and accreditation organizations to assure their continued compliance with these various standards.
All of our facilities are deemed certified, meaning that they are accredited, properly licensed under the relevant state laws and regulations and certified under the Medicare program or are in the process of applying for such accreditation, licensing or certification. The effect of maintaining certified facilities is to allow such facilities to participate in the Medicare and Medicaid programs. We believe that all of our facilities are in material compliance with applicable federal, state, local and other relevant accreditation and certification regulations and standards. However, should any of our healthcare facilities lose their deemed certified status and thereby lose certification under the Medicare or Medicaid programs, such facilities would be unable to receive reimbursement from either or both of those programs, and possibly from other third-party payors, and our business could be materially adversely affected.
Certain of our partnership and operating agreements contain provisions giving rights to our partners and other members that may be adverse to our interests.
Certain of the agreements governing the limited partnerships ("LPs"), general partnerships ("GP") and limited liability companies ("LLCs") through which we own and operate our facilities contain provisions that give our partners or other members rights that may, in certain circumstances, be adverse to our interests. These rights include, but are not limited to, rights to purchase our interest in the partnership or LLC, rights to require us to purchase the interests of our partners or other members, or rights requiring the consent of our partners and other members prior to our transferring our ownership interest in a facility or prior to a change in control of us or certain of our subsidiaries. With respect to these purchase rights, the agreements generally include a specified formula or methodology to determine the applicable purchase price, which may or may not reflect fair market value.
Additionally, many of our partnership and operating agreements contain restrictions on actions that we can take, even though we may be the general partner or the managing member. Examples of these restrictions include the rights of our partners and other members to approve the sale of substantially all of the assets of the partnership or LLC, to dissolve the partnership or LLC, to appoint a new or additional general partner or managing member and to amend the partnership or operating agreements. Many of our agreements also restrict our ability in certain instances to compete with our existing facilities or with our partners. Where we hold only a limited partner or a non-managing member interest, the general partner or managing member may take certain actions without our consent, although we typically have certain protective rights to approve major decisions such as the sale of substantially all of the assets of the entity, dissolution of the partnership or LLC and the amendment of the partnership or operating agreement. These management and governance rights held by our partners and other members limit and restrict our ability to make unilateral decisions about the management and operation of the facilities without the approval of our partners and other members.
We may have a special legal responsibility to the holders of ownership interests in the entities through which we own our facilities, which may conflict with, and prevent us from acting solely in, our own best interests or the interests of our stockholders.
We generally hold our ownership interests in facilities through limited or general partnerships, LLCs or limited liability partnerships (“LLPs”) in which we maintain an ownership interest along with physicians and, in some cases, physicians and health systems. As general partner and manager of most of these entities, we may have a special responsibility, known as a fiduciary duty, to manage these entities in the best interests of the other owners. We also have a duty to operate our business for the benefit of our stockholders. As a result, we may encounter conflicts between our responsibility to the other owners and our responsibility to our stockholders. For example, we have entered into management agreements to provide management services to our surgical facilities in exchange for a fee. Disputes may arise as to the nature of the services to be provided or the amount of the fee to be paid. In these cases, we may be obligated to exercise reasonable, good faith judgment to resolve the disputes and may not be free to act solely in our own best interests or the stockholders best interest. Disputes may also arise between us and our physician investors with respect to a particular business decision or regarding the interpretation of the provisions of the applicable partnership or limited liability company agreement. We seek to avoid these disputes but have not implemented any measures to resolve these conflicts if they arise. If we are unable to resolve a dispute on terms favorable or satisfactory to us, it could have a material adverse effect on our business, prospects, results of operations and financial condition.
Growth of patient receivables or deterioration in the ability to collect on these accounts, due to changes in economic conditions or otherwise, could have a material adverse effect on our business, prospects, results of operations and financial condition.
The current practice of providing medical services in advance of payment or, in many cases, prior to assessment of ability to pay for such services, may have significant negative impact on our revenue, bad debt expense and cash flow. We bill numerous and varied payors, such as self-pay patients, managed care payors and Medicare and Medicaid. These different payors typically have different billing
28
requirements that must be satisfied prior to receiving payment for services rendered. Reimbursement is typically conditioned on our documenting medical necessity and correctly applying diagnosis codes. Incorrect or incomplete documentation and billing information could result in non-payment for services rendered. The primary collection risks with respect to our patient receivables relate to patient accounts for which the primary third-party payor has paid the amounts covered by the applicable agreement, but patient responsibility amounts (deductibles and co-payments) remain outstanding.
Additional factors that could complicate our billing include:
• | disputes between payors as to which party is responsible for payment; |
• | failure of information systems and processes to submit and collect claims in a timely manner; |
• | variation in coverage for similar services among various payors; |
• | the difficulty of adherence to specific compliance requirements, diagnosis coding and other procedures mandated by various payors; and |
• | failure to obtain proper physician credentialing and documentation in order to bill various payors. |
We provide for bad debts principally based upon the type of payor and the age of the receivables. Our allowance for doubtful accounts at December 31, 2015 and 2014, represented 9.3% and 3.5% of our accounts receivable balance, respectively. Due to the difficulty in assessing future trends, including the effects of changes in economic conditions, we could be required to increase our provision for doubtful accounts. An increase in the amount of patient receivables or a deterioration in the collectability of these accounts could have a material adverse effect on our business, prospects, results of operations and financial condition.
We depend on our senior management, and we may be adversely affected if we lose any member of our senior management.
Because our senior management has been key to our growth and success, we are highly dependent on our senior management, including Michael Doyle, our Chief Executive Officer, and Teresa Sparks, our Executive Vice President and Chief Financial Officer. We do not maintain “key man” life insurance policies on any of our officers. Competition for senior management generally, and within the healthcare industry specifically, is intense and we may not be able to recruit and retain the personnel we need if we were to lose an existing member of senior management. Because our senior management has contributed greatly to our growth since inception, the loss of key management personnel, without adequate replacements, or our inability to attract, retain and motivate sufficient numbers of qualified management personnel could have a material adverse effect on our financial condition and results of operations.
The loss of certain physicians can have a disproportionate impact on certain of our facilities.
Generally, the top referring physicians within each of our facilities represent a large share of our revenue and admissions. The loss of one or more of these physicians, even if temporary, could cause a material reduction in our revenue, which could take significant time to replace given the difficulty and cost associated with recruiting and retaining physicians.
We may write-off intangible assets, such as goodwill.
As a result of purchase accounting for our various acquisition transactions, our balance sheet at December 31, 2015 contained intangible assets designated as either goodwill or intangibles totaling approximately $1.4 billion in goodwill and approximately $53.6 million in intangibles. Additional acquisitions that result in the recognition of additional intangible assets would cause an increase in these intangible assets. On an ongoing basis, we evaluate whether facts and circumstances indicate any impairment of the value of intangible assets. As circumstances change, we cannot assure you that the value of these intangible assets will be realized by us. If we determine that a significant impairment has occurred, we will be required to write-off the impaired portion of intangible assets, which could have a material adverse effect on our results of operations in the period in which the write-off occurs.
Our substantial leverage could adversely affect our ability to raise additional capital to fund our operations, limit our ability to react to changes in the economy or our industry, expose us to interest rate risk to the extent of our variable rate debt and prevent us from meeting our obligations under our outstanding indebtedness.
As of December 31, 2015, we had total indebtedness of approximately $1.2 billion under our $870.0 million senior secured first lien term loan (the “First Lien Term Loan”), which includes $150.0 million under a revolving credit facility (the “Revolver”) of which approximately $21.6 million was undrawn, and $490.0 million senior secured second lien credit facility (the “Second Lien Term Loan” and, together with the First Lien Term Loan and the Revolver, the “Term Loans and Revolving Facility”), where our subsidiary, Surgery Center Holdings, Inc., is the borrower. In addition, subject to the restrictions in our Term Loans and Revolving Facility, we may incur significant additional indebtedness, which may be secured, from time to time, which could have important consequences, including:
• | making it more difficult for us to satisfy our obligations with respect to our indebtedness, and any failure to comply with the obligations under any of our debt instruments, including restrictive covenants, could result in an event of default under such instruments; |
• | making us more vulnerable to adverse changes in general economic, industry and competitive conditions and adverse changes in government regulation; |
• | limiting cash flow available for general corporate purposes, including capital expenditures and acquisitions, because a substantial portion of our cash flow from operations must be dedicated to servicing our debt; |
• | limiting our ability to obtain additional debt financing in the future for working capital, capital expenditures or acquisitions; |
• | limiting our flexibility in reacting to competitive and other changes in our industry and economic conditions generally; and |
29
• | exposing us to risks inherent in interest rate fluctuations because some of our borrowings will be at variable rates of interest, which could result in higher interest expense in the event of increases in interest rates. |
Our ability to pay or to refinance our indebtedness will depend upon our future operating performance, which will be affected by general economic, financial, competitive, legislative, regulatory, business and other factors beyond our control.
Restrictive covenants in our debt instruments may adversely affect us.
Our Term Loans and Revolving Facility contain various covenants that limit, among other things, our ability and the ability of our restricted subsidiaries to:
• | incur additional indebtedness; |
• | make certain distributions, investments and other restricted payments; |
• | dispose of our assets; |
• | grant liens on our assets; |
• | engage in transactions with affiliates; |
• | merge, consolidate or transfer substantially all of our assets; and |
• | make payments to us (in the case of our restricted subsidiaries). |
In addition, our Term Loans and Revolving Facility contain other and more restrictive covenants, including covenants requiring us to maintain specified financial ratios triggered in certain situations and to satisfy other financial condition tests. Our ability to meet those financial ratios and tests can be affected by events beyond our control, and we cannot assure you that we will continue to meet those tests. A breach of any of these covenants could result in a default under our Term Loans and Revolving Facility. Upon the occurrence of an event of default under our Term Loans and Revolving Facility, the lenders could elect to declare all amounts outstanding under our Term Loans and Revolving Facility to be immediately due and payable and terminate all commitments to extend further credit. If we were unable to repay those amounts, the lenders could proceed against the collateral granted to them to secure that indebtedness. We have pledged substantially all of our assets, other than assets of our non-guarantor subsidiaries, as security under our Term Loans and Revolving Facility. If the lenders under our Term Loans and Revolving Facility accelerate the repayment of borrowings, we cannot assure you that we will have sufficient assets to repay our Term Loans and Revolving Facility and our other indebtedness.
We cannot assure you that our business will generate sufficient cash flow from operations, that currently anticipated revenue growth and operating improvements will be realized or that future borrowings will be available to us under our Term Loans and Revolving Facility in amounts sufficient to enable us to pay our indebtedness, or to fund our other liquidity needs. If we are unable to meet our debt service obligations or fund our other liquidity needs, we could attempt to restructure or refinance our indebtedness or seek additional equity capital. We cannot assure you that we will be able to accomplish those actions on satisfactory terms, if at all.
Despite our current indebtedness levels, we and our subsidiaries may still be able to incur substantially more debt, which could further exacerbate the risks associated with our substantial leverage.
We and our subsidiaries may be able to incur substantial additional indebtedness in the future, including secured indebtedness. Although the credit agreements governing our Term Loans and Revolving Facility contain restrictions on the incurrence of additional indebtedness, these restrictions are subject to a number of significant qualifications and exceptions, and the indebtedness incurred in compliance with these restrictions could be substantial. In addition, as of December 31, 2015 we had approximately $21.6 million available for additional borrowings under our Revolver, all of which is permitted to be incurred under the credit agreement governing our Term Loans and Revolving Facility. If new debt is added to our or our subsidiaries’ current debt levels, the related risks that we face would be increased.
To service our indebtedness, we will require a significant amount of cash. Our ability to generate cash depends on many factors beyond our control, and any failure to meet our debt service obligations could have a material adverse effect on our business, prospects, results of operations and financial condition.
Our ability to pay interest on and principal of our debt obligations principally depends upon our operating performance. As a result, prevailing economic conditions and financial, business and other factors, many of which are beyond our control, will affect our ability to make these payments.
In addition, we conduct our operations through our subsidiaries. Accordingly, repayment of our indebtedness is dependent on the generation of cash flow by our subsidiaries and their ability to make such cash available to us by dividend, debt repayment or otherwise. Our subsidiaries may not be able to, or may not be permitted to, make distributions to enable us to make payments in respect of our indebtedness. Each of our subsidiaries is a distinct legal entity and, under certain circumstances, legal and contractual restrictions may limit our ability to obtain cash from our subsidiaries. In particular, the constituent documents governing many of our non-wholly owned subsidiaries limit, under certain circumstances, our ability to access the cash generated by those subsidiaries in a timely manner.
If we do not generate sufficient cash flow from operations to satisfy our debt service obligations, we may have to undertake alternative financing plans, such as refinancing or restructuring our indebtedness, selling assets, reducing or delaying capital investments or capital expenditures or seeking to raise additional capital. Our ability to restructure or refinance our debt, if at all, will depend on the condition of the capital markets and our financial condition at such time. Any refinancing of our debt could be at higher interest rates and may require us to comply with more onerous covenants, which could further restrict our business operations. In addition, the terms of existing or future debt instruments may restrict us from adopting some of these alternatives. Our inability to generate sufficient cash flow to satisfy our debt service obligations, or to refinance our obligations at all or on commercially reasonable terms, could affect our ability to satisfy our debt obligations and have a material adverse effect on our business, prospects, results of operations and financial condition.
30
We are a holding company with no operations of our own.
We are a holding company, and our ability to service our debt is dependent upon the earnings from the business conducted by our subsidiaries that operate the surgical facilities. The effect of this structure is that we depend on the earnings of our subsidiaries, and the distribution or payment to us of a portion of these earnings to meet our obligations, including those under our Term Loans and Revolving Facility and any of our other debt obligations. The distributions of those earnings or advances or other distributions of funds by these entities to us, all of which are contingent upon our subsidiaries’ earnings, are subject to various business considerations. In addition, distributions by our subsidiaries could be subject to statutory restrictions, including state laws requiring that such subsidiaries be solvent, or contractual restrictions. Some of our subsidiaries may become subject to agreements that restrict the sale of assets and significantly restrict or prohibit the payment of dividends or the making of distributions, loans or other payments to stockholders, partners or members.
We make significant loans to, and are generally liable for debts and other obligations of, the partnerships and limited liability companies that own and operate some of our surgical facilities.
We own and operate our surgical facilities through limited partnerships and limited liability companies. Local physicians, physician groups and healthcare systems also own an interest in all but three of these partnerships and limited liability companies. In the partnerships in which we are the general partner, we are liable for 100% of the debts and other obligations of the partnership, even if we do not own all of the partnership interests. For some of our surgical facilities, indebtedness at the partnership level is funded through intercompany loans that we provide. At December 31, 2015, our intercompany loans totaled $24.5 million. Through these loans we have a security interest in the partnership’s or limited liability company’s assets. However, our financial condition and results of operations would be materially adversely affected if our surgical facilities are unable to repay these intercompany loans, or such loans are challenged under certain health care laws. Additionally, at December 31, 2015, our global intercompany note, which we use to transfer debt balances between our subsidiaries, had a zero balance.
Our Term Loans and Revolving Facility allow us to borrow funds that we can lend to the partnerships and limited liability companies in which we own an interest. Although most of our intercompany loans are secured by the assets of the partnership or limited liability company, the physicians and physician groups that own an interest in these partnerships and limited liability companies generally do not guarantee a pro rata amount of this debt or the other obligations of these partnerships and limited liability companies.
From time to time, we may guarantee our pro-rata share of the third-party debts and other obligations of many of the non-consolidated partnerships and limited liability companies in which we own an interest, subject to a limit provided in our credit agreements. In most instances of these guarantees, the physicians and/or physician groups have also guaranteed their pro-rata share of the indebtedness to secure the financing.
Our variable rate indebtedness subjects us to interest rate risk, which could cause our indebtedness service obligations to increase significantly.
Borrowings under our Term Loans and Revolving Facility are at variable rates of interest and expose us to interest rate risk. As of December 31, 2015, we had total indebtedness of approximately $1.2 billion under our Term Loans and Revolving Facility, including (i) $841.1 million (after giving effect to discount and issuance costs) outstanding under our First Lien Term Loan at an annual interest rate of 4.25% plus the adjusted LIBOR Rate, (ii) $125.3 million outstanding under our Revolver at an interest rate of 4.25% plus the adjusted LIBOR Rate, and (iii) $238.3 million (after giving effect to discount and issuance costs) outstanding under our Second Lien Term Loan at an annual interest rate of 7.50% plus the adjusted LIBOR Rate. If interest rates increase, our debt service obligations on variable rate indebtedness would increase even though the amount borrowed remained the same, and our net income and cash flows, including cash available for servicing our indebtedness, would correspondingly decrease.
Any refinancing of our debt could be at higher interest rates and may require us to comply with more onerous covenants, which could further restrict our business operations.
Our First Lien Term Loan is a senior secured first lien obligation of Surgery Center Holdings, Inc. and is guaranteed on a senior secured first priority basis and secured by substantially all of the assets, including pledges of equity interests, of Surgery Center Holdings, Inc., SP Holdco I, Inc. and the subsidiary guarantors described in the documentation, which are comprised of material wholly-owned non-excluded subsidiaries of Surgery Center Holdings, Inc. We have the option of classifying the First Lien Term Loan as either an ABR loan or an ED loan. The interest base rate on an ABR loan is equal to the greatest of (a) the Prime Rate in effect on such day, (b) the Federal Funds Effective Rate in effect on such day plus 0.5%, and (c) the Adjusted LIBO Rate for a Eurodollar Borrowing with a one-month interest period plus 1.0%; provided that the base rate shall not be less than 2.0% per annum. In addition to the base rate, we are required to pay a 3.25% margin for ABR loans. The interest base rate on an ED loan is equal to (x) the LIBO Rate for such Eurodollar borrowing in effect for such Interest Period divided by (y) one minus the Statutory Reserves (if any) for such Eurodollar Borrowing for such interest period; provided that the rate shall not be less than 1.0% per annum. In addition to the base rate, we are required to pay a 4.25% margin for ED loans. In 2015, we classified the First Lien Term Loan as an ED loan with an interest rate of 5.25% (1.0% base rate plus a 4.25% margin). Accrued interest is payable in arrears on a quarterly basis.
Our Second Lien Term Loan is a senior secured second lien obligation of Surgery Center Holdings, Inc. and is guaranteed on a senior secured second priority basis and secured by substantially all of the assets, including pledges of equity interests, of Surgery Center Holdings, Inc., SP Holdco I, Inc. and the subsidiary guarantors described in the documentation, which are comprised of material wholly-owned non-excluded subsidiaries of Surgery Center Holdings, Inc. We have the option of classifying the Second Lien Term Loan as either an ABR loan or an ED loan. The interest base rate on an ABR loan is equal to the greatest of (a) the Prime Rate in effect on such day, (b) the Federal Funds Effective Rate in effect on such day plus 0.5% and (c) the Adjusted LIBO Rate for a Eurodollar Borrowing with a one-month interest period plus 1.0%; provided that the base rate shall not be less than 2.0% per annum. In addition to the base rate, we are required to pay a 6.5% margin for ABR loans. The interest base rate on an ED loan is equal to (x) the LIBO Rate for such Eurodollar Borrowing in effect for such interest period divided by (y) one minus the Statutory Reserves (if any) for such Eurodollar Borrowing for such interest period;
31
provided that the base rate shall not be less than 1.0% per annum. In addition to the base rate, we are required to pay a 7.50% margin for ED loans. During 2015, we classified the Second Lien Term Loan as an ED loan with an interest rate of 8.50% (1.00% base rate plus a 7.50% margin). Accrued interest is payable in arrears on a quarterly basis, on the last business day of each of March, June, September and December.
We may be limited in our ability to utilize, or may not be able to utilize, net operating loss carryforwards to reduce our future tax liability.
As of December 31, 2015, we had U.S. federal net operating loss (“NOL”) carryforwards of approximately $360.3 million and state NOL carryforwards of approximately $495.9 million, which may be limited annually due to certain change in ownership provisions of Section 382 of the Internal Revenue Code of 1986, as amended (the “Code”). In addition, as a result of the Symbion acquisition, approximately $179 million in NOL carryforwards are subject to an annual Section 382 base limitation of $4.9 million, and, as a result of the Novamed acquisition, approximately $17 million in NOL carryforwards are subject to an annual Section 382 base limitation of $4.9 million. These limitations, when combined with amounts allowable due to net unrecognized built in gains, are not expected to impact the realization of the deferred tax assets associated with these NOLs. Our federal NOL carryforwards will begin to expire in 2025 and will completely expire in 2035, and our state NOL carryforwards will begin to expire in 2016 and will completely expire in 2035. Future ownership changes may subject our NOL carryforwards to further annual limitations, which could restrict our ability to use them to offset our taxable income in periods following the ownership changes.
We entered into a tax receivable agreement that will require us to pay to the pre-IPO owners of Surgery Center Holdings, LLC (the "Pre-IPO Owners") for certain tax benefits, including for tax benefits attributable to pre-IPO NOLs, which amounts are expected to be material.
We indirectly acquired favorable tax attributes in connection with the Reorganization. These tax attributes would not be available to us in the absence of the consummation of the Reorganization. As part of the Reorganization, we entered into a tax receivable agreement (the “TRA”) under which generally we will be required to pay to the Pre-IPO Owners 85% of the cash savings, if any, in U.S. federal, state or local tax that we actually realize (or are deemed to realize in certain circumstances) as a result of (i) certain tax attributes, including NOLs, capital losses, charitable deductions, alternative minimum tax credit carryforwards and federal and state tax credits of Surgery Center Holdings, Inc. and its affiliates relating to taxable years ending on or before the date of the Reorganization (calculated by assuming the taxable year of the relevant entity closes on the date of the Reorganization) that are or become available to us and our wholly-owned subsidiaries as a result of the Reorganization, and (ii) tax benefits attributable to payments made under the TRA. Under the TRA, generally we will retain the benefit of the remaining 15% of the applicable tax savings. See “Management’s Discussion and Analysis of Financial Condition and Results of Operations—Income Taxes and Tax Receivable Agreement.”
The actual utilization of the tax attributes that are the subject of the TRA, as well as the timing of any payments under the TRA, will vary depending upon a number of factors, including the amount, character and timing of our and our subsidiaries’ taxable income in the future, our use of NOL carryforwards and the portion of our payments under the TRA constituting imputed interest. Limitations on the use of the NOLs may apply, including limitations under Section 382 of the Code.
Payments under the TRA are not conditioned on the Pre-IPO Owners continuing to own shares of our common stock. Payments under the TRA are expected to give rise to certain additional tax benefits attributable to deductions for imputed interest. Any such benefits are the subject of the TRA and will increase the amounts due thereunder. In addition, the TRA provides for interest, at a rate equal to LIBOR plus 300 basis points, accrued from the due date (without extensions) of the corresponding federal, state or local tax return to the date of payment specified by the TRA. Payments under the TRA will be based on the tax reporting positions that we determine, consistent with the terms of the TRA. We will not be reimbursed for any payments previously made under the TRA if the utilization of any tax attributes that are the subject of the TRA are subsequently disallowed; if it is determined that excess payments have been made under the TRA, certain future payments, if any, otherwise to be made will be reduced. As a result, in certain circumstances, payments could be made under the TRA in excess of the benefits that we actually realize in respect of the attributes to which the TRA relates.
We expect the payments we will be required to make under the TRA will be substantial. It is also possible we will be required to make withholding tax payments in respect of one or more Pre-IPO Owners. Because we are a holding company with no operations of our own, our ability to make payments under the TRA is dependent on the ability of our subsidiaries to make distributions to us. The TRA restricts our and our subsidiaries’ ability to enter into any agreement or indenture that would restrict or encumber our ability to make payments under the TRA. To the extent that we are unable to make payments under the TRA, and such inability is a result of the terms of credit agreements and other debt documents that are materially more restrictive than those existing as of the date of the TRA, such payments will be deferred and will accrue interest at a rate of LIBOR plus 500 basis points until paid. If the terms of such credit agreements and other debt documents cause us to be unable to make payments under the TRA and such terms are not materially more restrictive than those existing as of the date of the TRA, such payments will be deferred and will accrue interest at a rate of LIBOR plus 300 basis points until paid. There can be no assurance that we will be able to finance our obligations under the TRA in a manner that does not adversely affect our working capital and growth requirements.
The TRA contains provisions that require, in certain cases, the acceleration of payments under the TRA to the Pre-IPO Owners, or payments which may significantly exceed the actual benefits we realize in respect of the tax attributes that are the subject of the TRA.
The terms of the TRA will, in certain circumstances, including certain changes of control, divestitures, or breaches of any material obligations under it (such as a failure to make any payment when due, subject to a specified cure period), provide for our (or our successor’s) obligations under the TRA to accelerate and become payable in a lump sum amount equal to the present value of the anticipated future tax benefits calculated based on certain assumptions, including that we would have at such time sufficient taxable income to fully utilize the tax attributes that are the subject of the TRA. Additionally, if we or any of our subsidiaries transfers any asset to a corporation
32
with which we do not file a consolidated tax return, we will be treated as having sold that asset in a taxable transaction for purposes of determining certain amounts payable pursuant to the TRA. As a result of the foregoing, (i) we could be required to make payments under the TRA that are greater than or less than the specified percentage of the actual tax savings we realize in respect of the tax attributes that are the subject of the TRA and (ii) we may be required to make an immediate lump sum payment equal to the present value of the anticipated future tax savings, which payment may be made years in advance of the actual realization of such future benefits, if any such benefits are ever realized. In these situations, our obligations under the TRA could have a substantial negative impact on our liquidity and could have the effect of adversely affecting our working capital and growth, and of delaying, deferring or preventing certain mergers, asset sales, other forms of business combinations or other changes of control.
Unanticipated changes in effective tax rates or adverse outcomes resulting from examination of our income or other tax returns could adversely affect our financial condition and results of operations.
We are subject to income taxes in the United States, and our domestic tax liabilities are subject to the allocation of expenses in differing jurisdictions. Our future effective tax rates could be subject to volatility or adversely affected by a number of factors, including:
• | changes in the valuation of our deferred tax assets and liabilities; |
• | expected timing and amount of the release of any tax valuation allowances; |
• | tax effects of equity-based compensation; |
• | costs related to intercompany restructurings; |
• | changes in tax laws, regulations or interpretations thereof; or |
• | lower than anticipated future earnings in jurisdictions where we have lower statutory tax rates and higher than anticipated future |
• | earnings in jurisdictions where we have higher statutory tax rates. |
In addition, we may be subject to audits of our income, sales and other transaction taxes by U.S. federal, state and local authorities. Outcomes from these audits could have an adverse effect on our financial condition and results of operations.
Our facilities may be adversely impacted by weather and other factors beyond our control, and disruptions in our disaster recovery systems or management continuity planning could limit our ability to operate our business effectively.
The financial results of our facilities may be negatively impacted by adverse weather conditions, such as tornadoes, earthquakes and hurricanes, or other factors beyond our control, such as wildfires. These weather conditions or other factors could disrupt patient scheduling, displace our patients, employees and physician partners and force certain of our facilities to close temporarily or for an extended period of time. In certain markets, we have a large concentration of surgery centers that may be simultaneously affected by adverse weather condition or events beyond our control.
While we have disaster recovery systems and business continuity plans in place, any disruptions in our disaster recovery systems or the failure of these systems to operate as expected could, depending on the magnitude of the problem, adversely affect our operating results by limiting our capacity to effectively monitor and control our operations. Despite our implementation of a variety of security measures, our technology systems could be subject to physical or electronic break-ins, and similar disruptions from unauthorized tampering or weather related disruptions where our headquarters is located. In addition, in the event that a significant number of our management personnel were unavailable in the event of a disaster, our ability to effectively conduct business could be adversely affected.
Risks Related to Government Regulation
We cannot predict the effect that healthcare reform and other changes in government programs may have on our business, financial condition or results of operations.
The Patient Protection and Affordable Care Act, as amended by the Health Care and Education Reconciliation Act of 2010, or collectively, the Affordable Care Act, dramatically alter the United States healthcare system and are intended to decrease the number of uninsured Americans and reduce overall healthcare costs. The Affordable Care Act attempts to achieve these goals by, among other things, requiring most Americans to obtain health insurance, expanding Medicare and Medicaid eligibility, reducing Medicare and Medicaid payments, expanding the Medicare program’s use of value-based purchasing programs, tying hospital payments to the satisfaction of certain quality criteria, and bundling payments to hospitals and other providers. The Affordable Care Act also contains a number of measures that are intended to reduce fraud and abuse in the Medicare and Medicaid programs, such as requiring the use of Recovery Audit Contractors (“RACs”) in the Medicaid program expanding the scope of the federal False Claims Act and generally prohibiting physician-owned hospitals from adding new physician owners or increasing the number of beds and operating rooms for which they are licensed. The Affordable Care Act provides for additional enforcement tools, cooperation between agencies, and funding for enforcement. Since their enactment, the Affordable Care Act has been subject to a number of challenges to its constitutionality. On June 28, 2012, the United States Supreme Court upheld challenges to the constitutionality of the “individual mandate” provision, which generally requires all individuals to purchase healthcare insurance or pay a penalty, but struck down as unconstitutional the provision that would have allowed the federal government to revoke all federal Medicaid funding to any state that did not expand its Medicaid program. As a result, many states have refused to extend Medicaid eligibility to more individuals as envisioned by the law. Other legal challenges are pending.
In addition, several bills have been and will likely continue to be advanced in Congress that would defund, repeal or amend all or significant provisions of the Affordable Care Act, and a number of provisions of the Affordable Care Act that were supposed to become effective, have been delayed by the Obama administration. As a result, it is difficult to predict the impact the Affordable Care Act will have on our business given the threats to and uncertainty surrounding key provisions of the Affordable Care Act. However, depending on how the
33
Affordable Care Act is ultimately interpreted, amended and implemented, it could have an adverse effect on our business, financial condition and results of operations.
Moreover, other legislative changes have also been proposed and adopted since the Affordable Care Act was enacted. On August 2, 2011, the Budget Control Act of 2011, among other things, created measures for spending reductions by Congress. A Joint Select Committee on Deficit Reduction, tasked with recommending a targeted deficit reduction of at least $1.2 trillion for the years 2013 through 2021, was unable to reach required goals, thereby triggering the legislation’s automatic reduction to several government programs. This included aggregate reductions to Medicare payments to providers of 2% per fiscal year, which went into effect on April 1, 2013 and, due to subsequent legislative amendments, will remain in effect through 2025 unless additional Congressional action is taken. On January 2, 2013, President Obama signed into law the American Taxpayer Relief Act of 2012, which, among other things, further reduced Medicare payments to several providers, including hospitals, imaging centers and cancer treatment centers, and increased the statute of limitations period for the government to recover overpayments to providers from three to five years. These new laws may result in additional reductions in Medicare and other health care funding, which could have a material adverse effect on our financial operations.
If we fail to comply with or otherwise incur liabilities under the numerous federal and state laws and regulations relating to the operation of our facilities, we could incur significant penalties or other costs or be required to make significant changes to our operations.
The healthcare industry is heavily regulated and we are subject to many laws and regulations at the federal, state and local government levels in the markets in which we operate. These laws and regulations require that our facilities meet various licensing, accreditation, certification and other requirements, including, but not limited to, those relating to:
• | ownership and control of our facilities; |
• | operating policies and procedures; |
• | qualification, training and supervision of medical and support persons; |
• | pricing of, billing for and coding of services and properly handling overpayments, debt collection practices and the submission of false statements or claims; |
• | the necessity, appropriateness and adequacy of medical care, equipment, personnel, operating policies and procedures; maintenance and preservation of medical records; |
• | financial arrangements between referral sources and our facilities; |
• | the protection of privacy, including patient and credit card information; |
• | screening, stabilization and transfer of individuals who have emergency medical conditions and provision of emergency services; |
• | antitrust; |
• | building codes; |
• | workplace health and safety; |
• | licensure, certification and accreditation; |
• | fee-splitting and the corporate practice of medicine; |
• | handling of medication; |
• | confidentiality, data breach, identity theft and maintenance and protection of health-related and other personal information and medical records; and |
• | environmental protection, health and safety. |
If we fail or have failed to comply with applicable laws and regulations, we could subject ourselves to administrative, civil or criminal penalties, cease and desist orders, forfeiture of amounts owed and recoupment of amounts paid to us by governmental or commercial payors, loss of licenses necessary to operate and disqualification from Medicare, Medicaid and other government-sponsored healthcare programs.
Many of these laws and regulations have not been fully interpreted by regulatory authorities or the courts, and their provisions are sometimes open to a variety of interpretations. Different interpretations or enforcement of existing or new laws and regulations could subject our current practices to allegations of impropriety or illegality, or require us to make changes in our operations, facilities, equipment, personnel, services, capital expenditure programs or operating expenses to comply with the evolving rules. Any enforcement action against us, even if we successfully defend against it, could cause us to incur significant legal expenses and divert our management’s attention from the operation of our business.
In pursuing our growth strategy, we may seek to expand our presence into states in which we do not currently operate. In new geographic areas, we may encounter laws and regulations that differ from those applicable to our current operations. If we are unwilling or unable to comply with these legal requirements in a cost-effective manner, we may be unable to expand into new geographic markets.
A number of initiatives have been proposed during the past several years to reform various aspects of the healthcare system in the United States. In the future, different interpretations or enforcement of existing or new laws and regulations could subject our current practices to allegations of impropriety or illegality, or could require us to make changes in our facilities, equipment, personnel, services, capital expenditure programs and operating expenses. In addition, some of the governmental and regulatory bodies that regulate us are considering or may in the future consider enhanced or new regulatory requirements. These authorities may also seek to exercise their supervisory or enforcement authority in new or more robust ways. All of these possibilities, if they occurred, could detrimentally affect the
34
way we conduct our business and manage our capital, either of which, in turn, could have a material adverse effect on our business, prospects, results of operations and financial condition.
If laws governing the corporate practice of medicine or fee-splitting change, we may be required to restructure some of our relationships, which may result in a significant loss of revenue and divert other resources.
The laws of various states in which we operate or may operate in the future do not permit business corporations to practice medicine, to exercise control over or employ physicians who practice medicine or to engage in various business practices, such as fee-splitting with physicians (i.e., sharing in a percentage of professional fees). The interpretation and enforcement of these laws vary significantly from state to state. We provide management services to a physician network. If our arrangements with this network were deemed to violate state corporate practice of medicine, fee-splitting or similar laws, or if new laws are enacted rendering our arrangements illegal, we may be subject to civil and/or criminal penalties and could be required to restructure or terminate these arrangements, any of which may result in a significant loss of revenue and divert other resources.
If regulations change, we may be obligated to purchase some or all of the ownership of our physician partners or renegotiate some of our partnership and operating agreements with our physician partners and management agreements with surgical facilities.
Upon the occurrence of various fundamental regulatory changes or changes in the interpretation of existing regulations, we may be obligated to purchase all of the ownership of the physician investors in most of the partnerships or limited liability companies that own and operate our surgical facilities. The purchase price that we would be required to pay for the ownership is typically based on either a multiple of the surgical facility’s EBITDA, as defined in our partnership and operating agreements with these surgical facilities, or the fair market value of the ownership as determined by a third-party appraisal. The physician investors in some of our surgical facilities can require us to purchase their interests in exchange for cash or shares of our common stock if these regulatory changes occur. In addition, some of our partnership agreements with our physician partners and management agreements with surgical facilities require us to attempt to renegotiate the agreements upon the occurrence of various fundamental regulatory changes or changes in the interpretation of existing regulations and provide for termination of the agreements if renegotiations are not successful.
Regulatory changes that could create purchase or renegotiation obligations include changes that:
• | make illegal the referral of Medicare or other patients to our surgical facilities by physician investors; |
• | create a substantial likelihood that cash distributions to physician investors from the partnerships or limited liability companies through which we operate our surgical facilities would be illegal; |
• | make illegal the ownership by the physician investors of interests in the partnerships or limited liability companies through which we own and operate our surgical facilities; or |
• | require us to reduce the aggregate percentage of physician investor ownership in our hospitals. |
We do not control whether or when any of these regulatory events might occur. In the event we are required to purchase all of the physicians’ ownership, our existing capital resources would not be sufficient for us to meet this obligation. These obligations and the possible termination of our partnership and management agreements would have a material adverse effect on our financial condition and results of operations.
Our revenue will decline if federal or state programs reduce our Medicare or Medicaid payments or if managed care companies reduce reimbursement amounts. In addition, the financial condition of payors and healthcare cost containment initiatives may limit our revenue and profitability.
For the years ended December 31, 2015, 2014 and 2013, we derived 38.2%, 34.5% and 28.0% of our revenue, respectively, from government payors, including Medicare and Medicaid programs. The Medicare and Medicaid programs are subject to statutory and regulatory changes, administrative rulings, interpretations and determinations concerning patient eligibility requirements, funding levels and the method of calculating payments or reimbursements, among other things; requirements for utilization review; and federal and state funding restrictions, any of which could materially increase or decrease payments from these government programs in the future, as well as affect the timing of payments to our facilities.
Additionally, the Budget Control Act of 2011 requires that Medicare reimbursement rates be reduced by 2%, which went into effect in April 2013 and, due to subsequent legislative amendments to the statute, will remain in effect through 2025 unless additional Congressional action is taken.
We cannot predict whether these automatic spending reductions will be rescinded, extended or increased by future legislative action. If these automatic spending reductions are increased or extended, such action could adversely affect our business, results of operations and/or financial condition.
We are unable to predict the effect of future government healthcare funding policy changes on our operations. If the rates paid by governmental payors are reduced, if the scope of services covered by governmental payors is limited or if we, or one or more of our surgical facilities, are excluded from participation in the Medicare, Medicaid or other government-sponsored healthcare programs, there could be a material adverse effect on our business, financial condition, results of operations or cash flows.
During the past several years, healthcare payors, such as federal and state governments, insurance companies and employers, have undertaken initiatives to revise payment methodologies and monitor healthcare costs. As part of their efforts to contain healthcare costs, payors increasingly are demanding discounted fee structures or the assumption by healthcare providers of all or a portion of the financial risk relating to paying for care provided, often in exchange for exclusive or preferred participation in their benefit plans. We expect efforts to impose greater discounts and more stringent cost controls by government and other payors to continue, thereby reducing the payments we receive for our services.
35
By way of example, under the Medicare program, physician payments are updated on an annual basis according to a statutory formula. Because application of the statutory formula for the update factor would have resulted in a decrease in total physician payments for the past several years, Congress has intervened with interim legislation to prevent the reductions. In April 2015, however, the Medicare Access and CHIP Reauthorization Act of 2015, or MACRA, was signed into law, which repealed and replaced the statutory formula for Medicare payment adjustments to physicians. MACRA provides a permanent end to the annual interim legislative updates that had previously been necessary to delay or prevent significant reductions to payments under the Medicare Physician Fee Schedule. MACRA extended previous payment rates through June 30, 2015, with a 0.5% update for July 1, 2015 through December 31, 2015, and for each calendar year through 2019, after which there will be a 0% annual update each year through 2025. In addition, MACRA requires the establishment of the Merit-Based Incentive Payment System (“MIPS”), beginning in 2019, under which physicians may receive performance-based payment incentives or payment reductions based on their performance with respect to clinical quality, resource use, clinical improvement activities and meaningful use of electronic health records. MACRA also requires Centers for Medicare & Medicaid Services ("CMS"), beginning in 2019, to provide incentive payments for physicians and other eligible professionals that participate in alternative payment models, such as accountable care organizations, that emphasize quality and value over the traditional volume-based fee-for-service model. It is unclear what impact, if any, MACRA will have on our business and operating results, but any resulting decrease in payment may result in reduced demand for our services.
The amount of our provision for doubtful accounts is based on our assessments of historical collection trends, business and economic conditions, trends in federal and state governmental and private employer health coverage and other collection indicators. A continuation in trends that results in increasing the proportion of accounts receivable being comprised of uninsured accounts and deterioration in the collectability of these accounts could adversely affect our collections of accounts receivable, results of operations and cash flows. As enacted, the Affordable Care Act seeks to decrease, over time, the number of uninsured individuals. Specifically, the Affordable Care Act expands Medicaid eligibility and provides incentives to employers to offer and individuals to purchase health insurance. It is difficult to predict the full impact of the Affordable Care Act due to pending court challenges, legislative threats, implementation uncertainty, and its complexity.
Our surgical facilities do not satisfy the requirements for any of the safe harbors under the federal Anti-Kickback Statute. If a federal or state agency asserts a different position or enacts new laws in this regard, we could be subject to criminal and civil penalties, loss of licenses and exclusion from governmental programs, which may result in a substantial loss of revenue.
The statute commonly known as the federal Anti-Kickback statute (the “Anti-Kickback Statute”) prohibits the offer, payment, solicitation or receipt of any form of remuneration in return for referrals for items or services payable by Medicare, Medicaid, or any other federally funded healthcare program. Additionally, the Anti-Kickback Statute prohibits any form of remuneration in return for purchasing, leasing or ordering, or arranging for or recommending the purchasing, leasing or ordering of items or services payable by Medicare, Medicaid or any other federally funded healthcare program. The Anti-Kickback Statute is very broad in scope and many of its provisions have not been uniformly or definitively interpreted by existing case law or regulations. Moreover, several federal courts have held that the Anti-Kickback Statute can be violated if only one purpose (not necessarily the primary purpose) of a transaction is to induce or reward a referral of business, notwithstanding other legitimate purposes. In addition, a person or entity does not need to have actual knowledge of the statute or specific intent to violate it in order to have committed a violation. Moreover, the government may assert that a claim including items or services resulting from a violation of the federal Anti-Kickback Statute constitutes a false or fraudulent claim for purposes of the False Claims Act (discussed below). Violations of the Anti-Kickback Statute may result in substantial civil or criminal penalties, including up to five years imprisonment and criminal fines of up to $25,000 and civil penalties of up to $50,000 for each violation, plus three times the remuneration involved or the amount claimed and exclusion from participation in all federally funded healthcare programs. Our exclusion from participation in such programs would have a material adverse effect on our business, prospects, results of operations and financial condition. In addition, many of the states in which we operate have also adopted laws, similar to the Anti-Kickback Statute, that prohibit payments to physicians in exchange for referrals, some of which apply regardless of the source of payment for care. These statutes typically impose criminal and civil penalties, including the loss of a license to do business in the state.
In July 1991, the U.S. Department of Health and Human Services ("HHS"), issued final regulations defining various “safe harbors” under the Anti-Kickback Statute. Business arrangements that meet the requirements of the safe harbors are not treated as criminal violations under the Anti-Kickback Statute. Business arrangements that do not meet the safe harbor requirements do not necessarily violate the Anti-Kickback Statute, but may be subject to scrutiny by the federal government to determine compliance. Two of the original safe harbors issued in 1991 apply to business arrangements similar to those used in connection with our surgical facilities: the “investment interest” safe harbor and the “personal services and management contracts” safe harbor. However, the structure of the partnerships and limited liability companies operating our surgery centers and surgical hospitals, as well as our various business arrangements involving physician group practices, do not satisfy all of the requirements of either safe harbor.
On November 19, 1999, HHS promulgated final regulations creating additional safe harbor provisions, including a safe harbor that applies to physician ownership of or investment interests in surgery centers. The surgery center safe harbor protects four types of investment arrangements: (1) surgeon owned surgery centers; (2) single specialty surgery centers; (3) multi-specialty surgery centers; and (4) hospital/physician surgery centers. Each category has its own requirements with regard to what type of physician may be an investor in the surgery center. In addition to the physician investor, the categories permit an “unrelated” investor, who is a person or entity that is not in a position to provide items or services related to the surgery center or its investors. Our business arrangements with our surgical facilities typically consist of one of our subsidiaries being an investor in each partnership or limited liability company that owns the facility, in addition to providing management and other services to the facility. Therefore, our business arrangements with our surgery centers, surgical hospitals and physician groups do not qualify for “safe harbor” protection from government review or prosecution under the Anti-Kickback Statute, however, we attempt to otherwise structure our surgery centers to fit as closely as possible within the safe harbor. When a transaction or relationship does not fit within a safe harbor, it does not mean that an Anti-Kickback Statute violation has occurred; rather, it means that the
36
facts and circumstances as well as the intent of the parties related to a specific transaction or relationship must be examined to determine whether or not any illegal conduct has occurred.
We employ dedicated marketing personnel whose job functions include the recruitment of physicians to perform surgery at our centers. These employees are paid a base salary plus a productivity bonus. We believe our employment arrangements with these employees are consistent with a safe harbor provision designed to protect payments made to employees. However, a government agency or private party may assert a contrary position.
We also enter into lease agreements with physicians from time to time for the rental of space for our surgical facilities. We seek to structure these lease agreements so that they are in compliance with the Anti-Kickback Statute safe harbor provision regarding real estate leases. However, a government agency or private party may assert a contrary position.
If any of our business arrangements with physicians or sales and marketing personnel were alleged or deemed to violate the Anti-Kickback Statute or similar laws, or if new federal or state laws were enacted rendering these arrangements illegal, it could have a material adverse effect on our business, prospects, results of operations and financial condition.
If we fail to comply with physician self-referral laws as they are currently interpreted or may be interpreted in the future, or if other legislative restrictions are issued, we could incur substantial monetary penalties and a significant loss of revenue.
The federal physician self-referral law, commonly referred to as the Stark Law, prohibits a physician from making a Medicare or Medicaid reimbursed referral for a “designated health service” to an entity if the physician or a member of the physician’s immediate family has a “financial relationship” with the entity unless an exception applies. The list of “designated health services” under the Stark Law does not generally include ambulatory surgery services, but it does include services such as clinical laboratory services, and certain imaging services that may be provided and separately billed by an ASC. Under the current Stark Law and related regulations, services provided at an ASC are not covered by the statute, even if those services include imaging, laboratory services or other Stark designated health services, provided that (i) the ASC does not bill for these services separately, or (ii) if the center is permitted to bill separately for these services, they are specifically exempted from Stark Law prohibitions. These are generally radiology and other imaging services integral to performance of surgical procedures that meet certain requirements and certain outpatient prescription drugs. We believe that services provided at our facilities licensed as hospitals are covered by the Stark Law, but referrals for such services are exempt from the Stark Law under its “whole hospital exception,” which was significantly amended by the Affordable Care Act. We also believe that certain services provided by our managed physician network are covered by the Stark Law, but referrals for those services are exempt from the Stark Law under its “in-office ancillary services exception,” among others. Our diagnostic laboratory is also subject to the Stark Law, but we believe that we have structured our agreements with physicians so as to not violate the Stark Law and related regulations.
The Stark Law and similar state statutes are subject to different interpretations with respect to many important provisions. Violations of these self-referral laws may result in substantial civil or criminal penalties, including treble damages for amounts improperly claimed, civil monetary penalties of up to $15,000 per prohibited service billed, up to $100,000 per prohibited circumvention scheme and exclusion from participation in the Medicare and Medicaid and other federal and state healthcare programs. Violations of the Stark Law will also create liability under the federal False Claims Act. Exclusion of our ASCs or hospitals from these programs through judicial or agency interpretation of existing laws or additional legislative restrictions on physician ownership or investments in healthcare entities could result in a significant loss of reimbursement revenue. We cannot provide assurances that CMS will not undertake other rulemaking to address additional revisions to or interpretations of the Stark Law regulations. If future rules modify the provisions of the Stark Law regulations that are applicable to our business, our revenue and profitability could be materially adversely affected and could require us to modify our relationships with our physician and healthcare system partners.
Federal law restricts the ability of our surgical hospitals to expand surgical capacity.
The Stark Law includes an exception that permits physicians to refer Medicare and Medicaid patients to hospitals in which they have an ownership interest if certain requirements are met. However, the Affordable Care Act dramatically curtailed this exception and prohibits physician ownership in hospitals that did not have a Medicare provider agreement by December 31, 2010. This prohibition does not apply to any of our five surgical hospitals, each of which had a Medicare provider agreement in place prior to December 31, 2010 and are therefore able to continue operating with their pre-IPO Ownership structure. However, the Affordable Care Act prohibits “grandfathered” hospitals from increasing their percentage of physician ownership, and it limits to a certain extent their ability to grow, because it prohibits such hospitals from increasing the aggregate number of inpatient beds, operating rooms and procedure rooms.
Companies within the healthcare industry continue to be the subject of federal and state audits and investigations, and we may be subject to such audits and investigations, including actions for false and other improper claims.
Federal and state government agencies, as well as commercial payors, have increased their auditing and administrative, civil and criminal enforcement efforts as part of numerous ongoing investigations of healthcare organizations. These audits and investigations relate to a wide variety of topics, including the following: cost reporting and billing practices; quality of care; financial reporting; financial relationships with referral sources; and medical necessity of services provided. In addition, the Office of the Inspector General of the U.S. Department of Health and Human Services (the “OIG”) and the U.S. Department of Justice (“DOJ”) have, from time to time, undertaken national enforcement initiatives that focus on specific billing practices or other suspected areas of abuse. In its 2013 Work Plan, the OIG stated its intention to review the safety and quality of care for Medicare beneficiaries having surgeries and procedures in ambulatory surgery centers and hospital outpatient departments. We have not received any material related audit letters to date.
The federal government is authorized to impose criminal, civil and administrative penalties on any person or entity that files a false claim for payment from the Medicare or Medicaid programs and other federal and state healthcare programs. Claims filed with private insurers can also lead to criminal and civil penalties, including, but not limited to, penalties relating to violations of federal mail and wire fraud statutes, as well as penalties under the anti-fraud provisions of the HIPAA (as defined below). While the criminal statutes are generally
37
reserved for instances of fraudulent intent, the federal government is applying its criminal, civil and administrative penalty statutes in an ever-expanding range of circumstances, including claiming payment for unnecessary services if the claimant merely should have known the services were unnecessary and claiming payment for low-quality services if the claimant should have known that the care was substandard. In addition, a violation of the Stark Law or the Anti-Kickback Statute can result in liability under the False Claims Act ("FCA").
Over the past several years, the federal government has investigated an increasing number of healthcare providers for potential FCA violations, which, among other things, prohibits a person from knowingly presenting, or causing to be presented, a false or fraudulent claim to the federal government. The statute defines “knowingly” to include not only actual knowledge of a claim’s falsity, but also reckless disregard for or intentional ignorance of the truth or falsity of a claim. Violators of the FCA are subject to severe financial penalties, including treble damages and per claim penalties in excess of $10,000. Because our facilities perform hundreds or thousands of similar procedures each year for which they are paid by Medicare, and since the statute of limitations for such claims extends for six years under normal circumstances (and possibly as long as ten years in the event of failure to discover material facts), a repetitive billing error or cost reporting error could result in significant, material repayments and civil or criminal penalties.
Moreover, another trend impacting healthcare providers is the increased use of the FCA, particularly by individuals who bring actions under that law. Under the “qui tam,” or whistleblower, provisions of the FCA, private parties may bring actions on behalf of the federal government. If the government intervenes and prevails in the action, the defendant may be required to pay three times the actual damages sustained by the government, plus mandatory civil monetary penalties of between $5,500 and $11,000 for each false claim submitted to the government. These private parties, often referred to as relators, are entitled to share in any amounts recovered by the government through trial or settlement. These qui tam cases are sealed by the court at the time of filing. The only parties privy to the information contained in the complaint are the relator, the federal government and the presiding court. It is possible that qui tam lawsuits have been filed against us and that we are unaware of such filings. Both direct enforcement activity by the government and whistleblower lawsuits under the FCA have increased significantly in recent years; thus, the risk that we will have to defend a false claims action, pay significant fines or be excluded from the Medicare and Medicaid programs has increased.
In addition, the Fraud Enforcement and Recovery Act of 2009 (“FERA”) further expanded the scope of the FCA to create liability for knowingly and improperly avoiding or decreasing an obligation to pay money to the federal government and FERA, along with statutory provisions found in the Acts, created federal False Claims Act liability for the knowing failure to report and return an overpayment within 60 days of the identification of the overpayment or, in certain cases, the date by which a corresponding cost report is due, whichever is later. Governmental authorities may challenge or scrutinize our operations or we may be the subject of a whistleblower lawsuit at any time. A determination that we have violated these laws could have a material adverse effect on our business, prospects, results of operations and financial condition.
The Health Insurance Portability and Accountability Act of 1996, as amended by the Health Information Technology for Economic and Clinical Health Act of 2009 (the “HITECH Act”), and their implementing regulations (collectively referred to as “HIPAA”) also created new federal criminal statutes that prohibit among other actions, knowingly and willfully executing, or attempting to execute, a scheme to defraud any healthcare benefit program, including private third-party payors, knowingly and willfully embezzling or stealing from a healthcare benefit program, willfully obstructing a criminal investigation of a healthcare offense, and knowingly and willfully falsifying, concealing or covering up a material fact or making any materially false, fictitious or fraudulent statement in connection with the delivery of or payment for healthcare benefits, items or services. Similar to the federal Anti-Kickback Statute, a person or entity does not need to have actual knowledge of the statute or specific intent to violate it in order to have committed a violation.
In addition, a person who offers or transfers to a Medicare or Medicaid beneficiary any remuneration, including waivers of co-payments and deductible amounts (or any part thereof), that the person knows or should know is likely to influence the beneficiary’s selection of a particular provider, practitioner or supplier of Medicare or Medicaid payable items or services may be liable for civil monetary penalties of up to $10,000 for each wrongful act. Moreover, in certain cases, providers who routinely waive copayments and deductibles for Medicare and Medicaid beneficiaries can also be held liable under the Anti-Kickback Statute and civil False Claims Act, which can impose additional penalties associated with the wrongful act. Although this prohibition applies only to federal healthcare program beneficiaries, the routine waivers of copayments and deductibles offered to patients covered by commercial payors may implicate applicable state laws related to, among other things, unlawful schemes to defraud, excessive fees for services, tortious interference with patient contracts and statutory or common law fraud. To the extent our patient assistance programs or other discount policies are found to be inconsistent with applicable laws, we may be required to restructure or discontinue such programs, or be subject to other significant penalties.
To enforce compliance with the federal laws, the DOJ has recently increased its scrutiny of interactions between health care companies and health care providers, which has led to a number of investigations, prosecutions, convictions and settlements in the health care industry. Dealing with investigations can be time and resource consuming and can divert management’s attention from the business. In addition, settlements with the DOJ or other law enforcement agencies have forced healthcare providers to agree to additional compliance and reporting requirements as part of a consent decree or corporate integrity agreement. Any such investigation or settlement could increase our costs or otherwise have an adverse effect on our business.
We are also subject to various state laws and regulations, as well as contractual provisions with commercial payors that prohibit us from submitting inaccurate, incorrect or misleading claims. We cannot be sure that none of our surgical facilities’ claims will ever be challenged. If we were found to be in violation of a state’s laws or regulations, or of a commercial payor contract, we could be forced to discontinue the violative practice and be subject to recoupment actions, fines and criminal penalties, which could have a material adverse effect on our business, prospects, results of operations and financial condition.
All payors are increasingly conducting post-payment audits. For example, CMS has implemented the RAC program, involving Medicare claims audits nationwide. Under the program, CMS contracts with RACs on a contingency fee basis to conduct post-payment reviews to detect and correct improper payments in the fee-for-service Medicare program. The Affordable Care Act expanded the RAC
38
program’s scope to include managed Medicare plans and to include Medicaid claims. In addition, CMS employs Medicaid Integrity Contractors (“MICs”) to perform post-payment audits of Medicaid claims and identify overpayments. The Affordable Care Act increases federal funding for the MIC program. In addition to RACs and MICs, the state Medicaid agencies and other contractors have increased their review activities. We are regularly subject to these external audits and we also perform both internal and third-party audits and monitoring.
For instance, recently HMS Federal Solutions, a MIC, completed an audit of one of our surgical hospitals for the period July 1, 2009 through May 31, 2012 and determined an overpayment obligation in the amount of approximately $4.6 million based on its extrapolation of a statistical sampling of claims, as well as a civil monetary penalty in the amount of $162,000, for a total amount owed to Idaho’s Department of Health and Welfare, Medicaid Program Integrity Unit of approximately $4.7 million for failure to comply with Medicaid rules by billing for (i) non-covered services, (ii) services provided by non-eligible providers, (iii) services not provided and (iv) unauthorized services. We have appealed the audit and are currently awaiting the result.
Although all other repayments requested to date as a result of RAC, MIC and ZPIC audits have not been material to our Company, we are unable to quantify the aggregate financial impact of these audits on our facilities given the pending appeals and uncertainty about the extent of future audits and whether the underlying conduct could be considered systemic. As such, the resolution of these audits could have a material adverse effect on our business, prospects, results of operations and financial condition.
Failure to comply with Medicare’s conditions for coverage and conditions of participation may result in loss of program payment or other governmental sanctions.
To participate in and receive payment from the Medicare program, our facilities must comply with regulations promulgated by CMS. These regulations, known as “conditions for coverage” for ASCs and “conditions of participation” for hospitals, set forth specific requirements with respect to, among other things, the facility’s physical plant, equipment, personnel and standards of medical care. All of our surgery centers and surgical hospitals are certified to participate in the Medicare program. As such, these facilities are subject to on-site, unannounced surveys by state survey agencies working on behalf of CMS. Under the ASC survey process, the surveyors are becoming more familiar with expanded interpretive guidance and the updated ASC conditions for coverage, which may lead to an increased number of deficiency citations requiring remedy with appropriate action plans. Failure to comply with Medicare’s conditions for coverage or conditions of participation may result in loss of payment or other governmental sanctions, including termination from participation in the Medicare program. We have established ongoing quality assurance activities to monitor our facilities’ compliance with these conditions and respond to surveys, but we cannot be sure that our facilities are or will always remain in full compliance with the requirements.
Our use and disclosure of personally identifiable information, including health information, is subject to federal and state privacy and security regulations, and our failure to comply with those regulations or to adequately secure the information we hold could result in significant liability or reputational harm.
HIPAA as well as numerous other federal and state laws and regulations, govern the collection, dissemination, use, privacy, security, confidentiality, integrity and availability of personally identifiable information (“PII”), including protected health information (“PHI”). HIPAA applies national privacy and security standards for PHI to covered entities such as us. HIPAA requires covered entities to maintain policies and procedures governing PHI that is used or disclosed, and to implement administrative, physical and technical safeguards to protect PHI, including PHI maintained, used and disclosed in electronic form. These safeguards include teammate training, identifying “business associates” with whom we need to enter into HIPAA-compliant contractual arrangements and various other measures. Ongoing implementation and oversight of these measures involves significant time, effort and expense. While we undertake substantial efforts to secure the PHI we maintain, use and disclose in electronic form, a cyber-attack or other intrusion that bypasses our information security systems causing an information security breach, loss of protected health information or other data subject to privacy laws or a material disruption of our operational systems could result in a material adverse impact on our business, along with potentially substantial fines and penalties. Ongoing implementation and oversight of these security measures involves significant time, effort and expense.
HIPAA also requires our surgical facilities to use standard transaction code sets and identifiers for certain standardized healthcare transactions, including billing and other claim transactions. We have undertaken significant efforts involving substantial time and expense to implement these requirements, and we anticipate that continual time and expense will be required to submit standardized transactions and to ensure that any newly acquired facilities can submit HIPAA-compliant transactions.
HIPAA requires covered entities to report breaches of unsecured protected health information to affected individuals without unreasonable delay and in no case later than 60 days after the discovery of the breach by the covered entity or its agents. Notification must also be made to HHS and, in certain situations involving large breaches, to the media. The HIPAA rules created a presumption that all non-permitted uses or disclosures of unsecured protected health information are breaches unless the covered entity establishes that there is a low probability the information has been compromised. HIPAA imposes mandatory civil and criminal penalties for violations of its requirements ranging up to $50,000 per violation, with a maximum civil penalty of $1.5 million in a calendar year for violations of the same requirement. However, a single breach incident can result in violations of multiple requirements, resulting in possible penalties well in excess of $1.5 million. In addition, the HITECH Act authorized state attorneys general to bring civil actions seeking either an injunction or damages in response to violations of HIPAA privacy and security regulations that threaten the privacy of state residents.
HIPAA also authorizes state attorneys general to bring civil actions seeking either an injunction or damages in response to violations of HIPAA privacy and security regulations that threaten the privacy of state residents. While HIPAA does not create a private right of action allowing individuals to sue us in civil court for violations of HIPAA’s requirements, its standards have been used as a basis for the duty of care in state civil suits, such as those for negligence or recklessness in the handling of PHI. In addition, HIPAA mandates that the Secretary of HHS conduct periodic compliance audits of HIPAA covered entities such as us.
In addition, many states in which we operate may impose laws that are more protective of the privacy and security of PII than HIPAA. Where these state laws are more protective than HIPAA, we have to comply with their stricter provisions. Only some of these state laws impose fines and penalties upon violators, but some may afford private rights of action to individuals who believe their PII has been
39
misused. California’s patient privacy laws, for example, provide for penalties of up to $250,000 and permit injured parties to sue for damages. Both state and federal laws are subject to modification or enhancement of privacy protection at any time. Our facilities will continue to remain subject to any federal or state privacy-related laws that are more restrictive than the privacy regulations issued under HIPAA. These statutes vary and could impose additional requirements on us and more severe penalties for disclosures of confidential health information. New health information standards could have a significant effect on the manner in which we do business, and the cost of complying with new standards could be significant. We may not remain in compliance with the diverse privacy requirements in all of the jurisdictions in which we do business. If we fail to comply with HIPAA or similar state laws, we could incur substantial civil monetary or criminal penalties.
If we are unable to integrate and operate our information systems effectively or implement new systems and processes, our operations could be disrupted.
Our operations depend significantly on effective information systems, which require continual maintenance, upgrading and enhancement to meet our operational needs. Any system failure that causes an interruption in service or availability of our systems could adversely affect operations or delay the collection of revenue. Moreover, we use the development and implementation of sophisticated and specialized technology to improve our profitability, our growth and acquisition strategy will require frequent transitions and integration of various information systems. If we are unable to properly integrate other information systems or expand our current information systems it may have an adverse effect on our ability to obtain new business, retain existing business and maintain or increase our profit margins and we could suffer, among other things, operational disruptions, disruptions in cash flows and increases in administrative expenses.
Information security risks have generally increased in recent years because of threats from malicious persons and groups, new vulnerabilities, the proliferation of new technologies and the increased sophistication and activities of perpetrators of cyber-attacks. A failure in or breach of our operational or information security systems as a result of cyber-attacks or information security breaches could disrupt our business, result in the loss, disclosure or misuse of confidential or proprietary information, damage our reputation, increase our costs or lead to fines and financial losses. As a result, cyber security and the continued development and enhancement of the controls and processes designed to protect our systems, computers, software, data and networks from attack, damage or unauthorized access remain a priority for us. Although we believe that we have robust information security procedures and other safeguards in place, as cyber threats continue to evolve, we may be required to expend additional resources to continue to enhance our information security measures or to investigate and remediate any information security vulnerabilities.
Efforts to regulate the construction, acquisition or expansion of healthcare facilities could prevent us from acquiring additional surgical facilities, renovating our existing facilities or expanding the breadth of services we offer.
Some states require prior approval for the construction, acquisition or expansion of healthcare facilities or expansion of the services the facilities offer. In giving approval, these states consider the need for additional or expanded healthcare facilities or services, as well as the financial resources and operational experience of the potential new owners of existing healthcare facilities. In many of the states in which we currently operate, certificates of need must be obtained for capital expenditures exceeding a prescribed amount, changes in capacity or services offered and various other matters. The remaining states in which we now or may in the future operate may adopt similar legislation. Our costs of obtaining a certificate of need could be significant, and we cannot assure you that we will be able to obtain the certificates of need or other required approvals for additional or expanded surgical facilities or services in the future. In addition, at the time we acquire a surgical facility, we may agree to replace or expand the acquired facility. If we are unable to obtain required approvals, we may not be able to acquire additional surgical facilities, expand healthcare services we provide at these facilities or replace or expand acquired facilities.
If antitrust enforcement authorities conclude that our market share in any particular market is too concentrated, that our or our health system partners’ commercial payor contract negotiating practices are illegal, or that we other violate antitrust laws, we could be subject to enforcement actions that could have a material adverse effect on our business, prospects, results of operations and financial condition.
The federal government and most states have enacted antitrust laws that prohibit certain types of conduct deemed to be anti-competitive. These laws prohibit price fixing, concerted refusal to deal, market monopolization, price discrimination, tying arrangements, acquisitions of competitors and other practices that have, or may have, an adverse effect on competition. Violations of federal or state antitrust laws can result in various sanctions, including criminal and civil penalties. Antitrust enforcement in the healthcare industry is currently a priority of the Federal Trade Commission (the “FTC”). We believe we are in compliance with federal and state antitrust laws, but courts or regulatory authorities may reach a determination in the future that could have a material adverse effect on our business, prospects, results of operations and financial condition.
The healthcare laws and regulation to which we are subject is constantly evolving and may change significantly in the future.
The regulation applicable to our business and to the healthcare industry generally to which we are subject is constantly in a state of flux. While we believe that we have structured our agreements and operations in material compliance with applicable healthcare laws and regulations, there can be no assurance that we will be able to successfully address changes in the current regulatory environment. We believe that our business operations materially comply with applicable healthcare laws and regulations. However, some of the healthcare laws and regulations applicable to us are subject to limited or evolving interpretations, and a review of our business or operations by a court, law enforcement or a regulatory authority might result in a determination that could have a material adverse effect on us. Furthermore, the healthcare laws and regulations applicable to us may be amended or interpreted in a manner that could have a material adverse effect on our business, prospects, results of operations and financial condition.
Risks Related to Our Common Stock
40
We are a “controlled company” within the meaning of NASDAQ rules and, therefore, we qualify for, and currently rely on, exemptions from certain corporate governance requirements. Our stockholders do not have the same protections afforded to stockholders of companies that are subject to such requirements.
As of December 31, 2015, H.I.G. Surgery Centers, LLC, an affiliate of H.I.G. Capital, LLC (collectively, our “H.I.G.”) controlled a majority of the voting power of our outstanding common stock. As a result, we are a “controlled company” within the meaning of the corporate governance standards of NASDAQ. Under these rules, a company of which more than a majority of the voting power is held by an individual, group or another company is a “controlled company” and may elect not to comply with certain corporate governance requirements including:
• | the requirement that a majority of the board of directors consist of independent directors; |
• | the requirement that we have a nominating/corporate governance committee that is composed entirely of independent directors with a written charter addressing the committee’s purpose and responsibilities; and |
• | the requirement that we have a compensation committee that is composed entirely of independent directors with a written charter addressing the committee’s purpose and responsibilities. |
As of December 31, 2015, we have availed ourselves of certain of these exemptions. As a result, we do not have a majority of independent directors and we do not have a nominating and corporate governance committee. Accordingly, our stockholders will not have the same protections afforded to stockholders of companies that are subject to all of the corporate governance requirements of NASDAQ.
H.I.G., however, is not subject to any contractual obligation to retain its controlling interest, except that it has agreed, subject to certain exceptions, not to sell or otherwise dispose of any shares of our common stock or other capital stock or other securities exercisable or convertible therefor for a period of at least 180 days after the date of the IPO without the prior written consent of certain of the underwriters. Except for this period, there can be no assurance as to the period of time during which H.I.G. will maintain its ownership of our common stock.
H.I.G. has significant influence over us, including control over decisions that require the approval of stockholders, which could limit our stockholders’ ability to influence the outcome of key transactions, including a change of control.
As of December 31, 2015, we were controlled by H.I.G.. As of that time, H.I.G. beneficially owned 55% of our outstanding common stock. For as long as H.I.G. continues to beneficially own shares of common stock representing more than a majority of the voting power of our common stock, it will be able to direct the election of all of the members of our board of directors and could exercise a controlling influence over our business and affairs, including any determinations with respect to mergers or other business combinations, the acquisition or disposition of assets, the incurrence of indebtedness, the issuance of any additional common stock or other equity securities, the repurchase or redemption of common stock and the payment of dividends. Similarly, H.I.G. will have the power to determine matters submitted to a vote of our stockholders without the consent of our other stockholders, will have the power to prevent a change in our control and could take other actions that might be favorable to it. Even if H.I.G. ceases to beneficially own a majority of the voting power of our common stock, it will continue to be able to strongly influence or effectively control our decisions.
Additionally, H.I.G. is in the business of making investments in companies and may acquire and hold interests in businesses that compete directly or indirectly with us. H.I.G. may also pursue acquisition opportunities that may be complementary to our business, and, as a result, those acquisition opportunities may not be available to us.
We are an “emerging growth company,” as defined in the Securities Act, and we cannot be certain if the reduced disclosure requirements applicable to emerging growth companies will make our common stock less attractive to investors.
We are an “emerging growth company,” as defined in Section 2(a) of the Securities Act, as modified by the JOBS Act, and we may take advantage of certain exemptions from various reporting requirements that are applicable to other public companies that are not “emerging growth companies,” including not being required to comply with the auditor attestation requirements of Section 404 of the Sarbanes-Oxley Act, reduced disclosure obligations regarding executive compensation and exemptions from the requirements of holding a non-binding shareholder advisory vote on executive compensation and shareholder approval of any golden parachute payments not previously approved. As a result, our stockholders may not have access to certain information that they may deem important. We could be an emerging growth company for up to five years, although circumstances could cause us to lose that status earlier, including if our total annual gross revenues exceed $1.0 billion, if we issue more than $1.0 billion in non-convertible debt during any three-year period, or if the market value of our common stock held by non-affiliates exceeds $700.0 million as of any June 30. We cannot predict if investors will find our common stock less attractive because we may rely on these exemptions. If some investors find our common stock less attractive as a result, there may be a less active trading market for our common stock and our stock price may be more volatile.
Our stock price could be extremely volatile, and, as a result, our stockholders may not be able to resell their shares at or above the price paid for them.
The stock market in general has been highly volatile. As a result, the market price of our common stock is likely to be similarly volatile, and investors in our common stock may experience a decrease, which could be substantial, in the value of their stock, including decreases unrelated to our operating performance or prospects, and could lose part or all of their investment. The price of our common stock could be subject to wide fluctuations in response to a number of factors, including those described elsewhere in this report and others such as:
• | variations in our operating performance and the performance of our competitors; |
• | actual or anticipated fluctuations in our quarterly or annual operating results; |
• | publication of research reports by securities analysts about us or our competitors or our industry; |
41
• | announcements by us, our competitors or our vendors of significant contracts, acquisitions, joint marketing relationships, joint ventures or capital commitments; |
• | our failure or the failure of our competitors to meet analysts’ projections or guidance that we or our competitors may give to the market; |
• | additions and departures of key personnel; |
• | strategic decisions by us or our competitors, such as acquisitions, divestitures, spin-offs, joint ventures, strategic investments or changes in business strategy; |
• | the passage of legislation or other regulatory developments affecting us or our industry; |
• | speculation in the press or investment community; |
• | changes in accounting principles; |
• | terrorist acts, acts of war or periods of widespread civil unrest; |
• | natural disasters and other calamities; and |
• | changes in general market and economic conditions. |
In the past, securities class action litigation has often been initiated against companies following periods of volatility in their stock price. This type of litigation could result in substantial costs and divert our management’s attention and resources, and could also require us to make substantial payments to satisfy judgments or to settle litigation.
Future issuances of capital stock may dilute our stockholders’ percentage ownership in us, which could reduce their influence over matters on which stockholders vote.
Our board of directors has the authority, without action or vote of our stockholders, to issue all or any part of our authorized but unissued shares of common stock, including shares issuable upon the exercise of options, or shares of our authorized but unissued preferred stock. Issuances of common stock or voting preferred stock would reduce our current stockholders’ influence over matters on which our stockholders vote and, in the case of issuances of preferred stock, would likely result in common stockholders’ interest in us being subject to the prior rights of holders of that preferred stock.
Provisions in our charter documents and Delaware law may deter takeover efforts that could be beneficial to stockholder value.
Our certificate of incorporation and by-laws and Delaware law contain provisions that could make it harder for a third party to acquire us, even if doing so might be beneficial to our stockholders. These provisions include a classified board of directors and limitations on actions by our stockholders. In addition, our board of directors has the right to issue preferred stock without stockholder approval that could be used to dilute a potential hostile acquiror. Our certificate of incorporation also imposes some restrictions on mergers and other business combinations between us and any holder of 15.0% or more of our outstanding common stock other than affiliates of H.I.G.. As a result, our stockholders may lose their ability to sell their stock for a price in excess of the prevailing market price due to these protective measures, and efforts by stockholders to change the direction or management of the Company may be unsuccessful.
Our amended and restated certificate of incorporation designates courts in the State of Delaware as the sole and exclusive forum for certain types of actions and proceedings that may be initiated by our stockholders, which could limit our stockholders’ ability to obtain a favorable judicial forum for disputes with us or our directors, officers or employees.
Our amended and restated certificate of incorporation provides that, subject to limited exceptions, the Court of Chancery of the State of Delaware will be the sole and exclusive forum for (i) any derivative action or proceeding brought on our behalf, (ii) any action asserting a claim of breach of a fiduciary duty owed by any of our directors, officers or other employees to us or our stockholders, (iii) any action asserting a claim against us arising pursuant to any provision of the DGCL, our amended and restated certificate of incorporation or our amended and restated bylaws or (iv) any other action asserting a claim against us that is governed by the internal affairs doctrine (each, a “Covered Proceeding”). In addition, our amended and restated certificate of incorporation provides that if any action the subject matter of which is a Covered Proceeding is filed in a court other than the specified Delaware courts without the approval of our board of directors (each, a “Foreign Action”), the claiming party will be deemed to have consented to (i) the personal jurisdiction of the specified Delaware courts in connection with any action brought in any such courts to enforce the exclusive forum provision described above and (ii) having service of process made upon such claiming party in any such enforcement action by service upon such claiming party’s counsel in the Foreign Action as agent for such claiming party. Any person or entity purchasing or otherwise acquiring any interest in shares of our stock shall be deemed to have notice of and to have consented to these provisions. These provisions may limit a stockholder’s ability to bring a claim in a judicial forum that it finds favorable for disputes with us or our directors, officers or other employees, which may discourage such lawsuits against us and our directors, officers and employees. Alternatively, if a court were to find these provisions of our amended and restated certificate of incorporation inapplicable to, or unenforceable in respect of, one or more of the specified types of actions or proceedings, we may incur additional costs associated with resolving such matters in other jurisdictions, which could adversely affect our business and financial condition.
Because we have no current plans to pay cash dividends on our common stock for the foreseeable future, our stockholders may not receive any return on investment unless they sell their common stock for a price greater than that which they paid for it.
We may retain future earnings, if any, for future operations, expansion and debt repayment and have no current plans to pay any cash dividends for the foreseeable future. Any decision to declare and pay dividends in the future will be made at the discretion of our board of directors and will depend on, among other things, our results of operations, financial condition, cash requirements, contractual restrictions and other factors that our board of directors may deem relevant. In addition, our ability to pay dividends may be limited by covenants of any
42
existing and future outstanding indebtedness we or our subsidiaries incur, including our senior credit facility. As a result, our stockholders may not receive any return on an investment in our common stock unless they sell their common stock for a price greater than that which they paid for it.
As a result of becoming a public company, we are obligated to report on the effectiveness of our internal controls over financial reporting. These internal controls may not be effective and our independent registered public accounting firm may not be able to certify as to their effectiveness, which could have a significant and adverse effect on our business and reputation.
As a public company, we are required to evaluate our internal controls over financial reporting. Furthermore, at such time as we cease to be an “emerging growth company”, as more fully described in “-We are an “emerging growth company,” as defined in the Securities Act, and we cannot be certain if the reduced disclosure requirements applicable to emerging growth companies will make our common stock less attractive to investors,” we will also be required to comply with Section 404 of the Sarbanes-Oxley Act. At such time, we may identify material weaknesses that we may not be able to remediate in time to meet the applicable deadline imposed upon us for compliance with the requirements of Section 404 of the Sarbanes-Oxley Act. In addition, if we fail to achieve and maintain the adequacy of our internal controls, as such standards are modified, supplemented or amended from time to time, we may not be able to ensure that we can conclude on an ongoing basis that we have effective internal controls over financial reporting in accordance with Section 404 of the Sarbanes-Oxley Act. We cannot be certain as to the timing of completion of our evaluation, testing and any remediation actions or the impact of the same on our operations. If we are not able to implement the requirements of Section 404 of the Sarbanes-Oxley Act in a timely manner or with adequate compliance, our independent registered public accounting firm.
The requirements of being a public company may strain our resources and distract our management, which could make it difficult to manage our business, particularly after we are no longer an “emerging growth company” under the JOBS Act.
As a public company, we are subject to the reporting requirements of the Exchange Act, and requirements of the Sarbanes-Oxley Act. These requirements may place a strain on our systems and resources. The Exchange Act requires that we file annual, quarterly and current reports with respect to our business and financial condition. The Sarbanes-Oxley Act requires that we maintain effective disclosure controls and procedures and internal controls over financial reporting. To maintain and improve the effectiveness of our disclosure controls and procedures, we will need to commit significant resources, hire additional staff and provide additional management oversight. We have, and will continue to be, implementing additional procedures and processes for the purpose of addressing the standards and requirements applicable to public companies. Sustaining our growth also will require us to commit additional management, operational and financial resources to identify new professionals to join our firm and to maintain appropriate operational and financial systems to adequately support expansion. These activities may divert management’s attention from other business concerns, which could have a material adverse effect on our business, financial condition, results of operations and cash flows.
We also expect that operating as a public company will make it more expensive for us to obtain director and officer liability insurance, and we may be required to accept reduced coverage or incur substantially higher costs to obtain coverage. This could also make it more difficult for us to attract and retain qualified people to serve on our board of directors, our board committees, or as executive officers.
Furthermore, if we are unable to satisfy our obligations as a public company, we could be subject to delisting of our common stock, fines, sanctions, and other regulatory action and potentially civil litigation, which could have a material adverse effect on our financial condition and results of operations.
As an “emerging growth company” under the JOBS Act, we are permitted to, and intend to, take advantage of certain exemptions from various reporting requirements that are applicable to other public companies that are not “emerging growth companies,” including, but not limited to, not being required not being required to comply with the auditor attestation requirements of Section 404 of the Sarbanes-Oxley Act and reduced disclosure obligations regarding executive compensation in our periodic reports and proxy statements. When these exemptions cease to apply, we expect to incur additional expenses and devote increased management effort toward ensuring compliance with them. We will remain an “emerging growth company” for up to five years, although we may cease to be an emerging growth company earlier under certain circumstances. See “- We are an “emerging growth company,” as defined in the Securities Act, and we cannot be certain if the reduced disclosure requirements applicable to emerging growth companies will make our common stock less attractive to investors” for additional information on when we may cease to be an emerging growth company. We cannot predict or estimate the amount of additional costs we may incur as a result of becoming a public company or the timing of such costs.
If securities or industry analysts do not continue to publish research or publish inaccurate or unfavorable research about our business, our stock price and trading volume could decline.
The trading market for our common stock will depend in part on the research and reports that securities or industry analysts publish about us or our business. If securities or industry analysts ceases coverage of us or fails to publish reports on us regularly, demand for our common stock could decrease, which could cause our stock price and trading volume to decline . If one or more of the analysts who covers us downgrades our common stock or publishes inaccurate or unfavorable research about our business, our stock price would likely decline.
43
Item 1B. Unresolved Staff Comments
None.
Item 2. Properties
Our corporate headquarters is located in Nashville, Tennessee at 40 Burton Hills Boulevard, Suite 500, where we currently lease approximately 44,000 square feet of office space under a lease that extends through December 31, 2017. We have entered into a lease agreement to transfer our corporate headquarters to a location in Brentwood, Tennessee upon expiration of our current lease on December 31, 2017. The new space will be approximately 56,000 square feet. In addition, certain of our corporate operational functions are located in Tampa, Florida at 5426 Bay Center Drive, Suite 300, where we currently lease approximately 31,000 square feet of office space. This lease expires in April 2018. We believe these spaces are sufficient and adequate for our needs at this time.
Our surgical facilities typically are located on real estate leased by the partnership or limited liability company that operates the facility. These leases generally have initial terms of ten years, but range from two to 15 years. Most of the leases contain options to extend the lease period for up to ten additional years. The surgical facilities are generally responsible for property taxes, property and casualty insurance and routine maintenance expenses. One of our surgical facilities is located on real estate owned by the limited partnership or limited liability company that owns the surgical facility. We generally guarantee the lease obligations of the partnerships and limited liability companies that own our surgical facilities.
Additional information about our surgical facilities and our other properties can be found in Item 1 of this report under the caption, “Business—Surgical Facility Operations.”
Item 3. Legal Proceedings
We are, from time to time, subject to claims and suits arising in the ordinary course of business, including claims for damages for personal injuries, breach of management contracts and employment related claims. In certain of these actions, plaintiffs request payment for damages, including punitive damages, that may not be covered by insurance. In the opinion of management, we are not currently a party to any proceedings that would have a material adverse effect on our business, financial condition or results of operations.
Item 4. Mine Safety Disclosures
Not applicable.
44
PART II
Item 5. Market for Registrant’s Common Equity, Related Stockholder Matters and Issuer Purchases of Equity Securities
Our common stock trades under the symbol “SGRY” on the NASDAQ Global Select Market. The IPO of our common stock occurred on October 1, 2015. The high and low sales prices per share for the common stock from the date of the IPO through December 31, 2015, as reported on the NASDAQ Global Select Market, was $21.32 to $16.54, respectively. The last reported sales price of our common stock as reported on the NASDAQ Global Select Market on March 10, 2016 was $13.77.
Use of Proceeds from our Initial Public Offering
In October, 2015, we completed an IPO of our common stock in which we sold 14,285,000 shares of common stock and certain selling shareholders sold 1,569,465 shares of common stock pursuant to the partial exercise of the underwriter’ option to purchase additional shares. The shares sold in the offering were registered under the Securities Act pursuant to our Registration Statement on Form S‑1 (Registration No. 333-206439), which was declared effective by the SEC on September 30, 2015. The net proceeds to us, after deducting underwriting discounts and fees, were approximately $255.8 million. We did not receive any proceeds from shares sold by the selling shareholders. We used the net proceeds to repay a portion of the borrowings outstanding under our 2014 Second Lien Credit Agreement, and to pay fees associated with this offering (including fees associated with terminating a management agreement previously in place with an affiliate of H.I.G.).
Holders
As of March 10, 2016, there were 25 holders of record of our common stock. The actual number of common stockholders is greater than the number of record holders, and includes stockholders who are beneficial owners, but whose shares are held in street name by brokers and other nominees. This number of holders of record also does not include stockholders whose shares may be held in trust by other entities.
Dividends
We have never declared or paid a cash dividend on our common stock, and have no current plans to declare or pay any cash dividends for the foreseeable future. Any decision to declare and pay dividends in the future will be made at the discretion of our board of directors and will depend on, among other things, our results of operations, financial condition, cash requirements, contractual restrictions and other factors that our board of directors may deem relevant. In addition, our ability to pay dividends may be limited by covenants of any existing and future outstanding indebtedness we or our subsidiaries incur, including our credit facility. Additionally, because we are a holding company, we would depend on distributions from our subsidiaries to fund any potential dividends.
Equity Compensation Plans
See Item 12 for information with respect to the Company’s equity compensation plans.
Stock Performance Graph
The following graph compares the cumulative total shareholder return on our common stock from October 1, 2015 (using the closing price of our shares of common stock on October 1, 2015, the day they were initially sold to the public) to December 31, 2015 to that of the total return of the indices below, using the same date range. The comparison assumes $100 was invested in our common stock and in each of the indices on October 1, 2015 and assumes the reinvestment of dividends, if any.
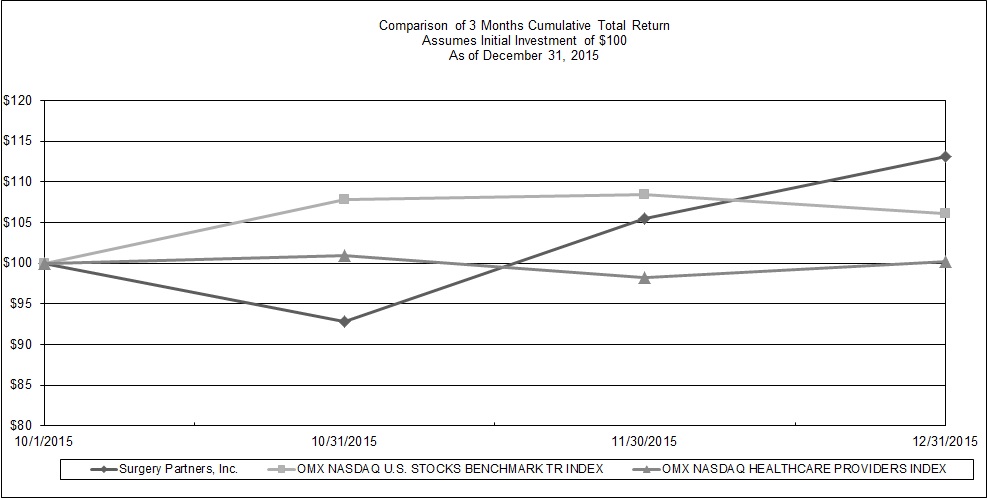
45
This graph is furnished and not filed with the SEC or soliciting material under the Exchange Act and shall not be incorporated by reference into any such filings, irrespective of any general incorporation contained in such filing. The stock performance shown on the graph represents historical stock performance and is not necessarily indicative of future stock price performance.
Item 6. Selected Financial Data
The following selected consolidated financial and other data should be read in conjunction with “Management’s Discussion and Analysis of Financial Condition and Results of Operations” in Item 7 and our audited consolidated financial statements and the related notes included elsewhere in this report. The selected consolidated statements of operations data and cash flow data set forth below for the years ended December 31, 2015, 2014, 2013 and 2012, and the selected consolidated balance sheets data set forth below as of December 31, 2015, 2014, and 2013 are derived from our audited consolidated financial statements.
The historical results presented below are not necessarily indicative of the results to be expected for any future period (dollars in thousands, except per share amounts):
46
Year Ended December 31, | ||||||||||||||||
2015 | 2014 | 2013 | 2012 | |||||||||||||
Consolidated Statements of Operations Data: | ||||||||||||||||
Revenues | $ | 959,891 | $ | 403,289 | $ | 284,599 | $ | 260,215 | ||||||||
Operating expenses: | ||||||||||||||||
Cost of revenues | 669,326 | 254,178 | 169,844 | 159,346 | ||||||||||||
General and administrative expenses | 55,992 | 31,452 | 26,339 | 25,263 | ||||||||||||
Depreciation and amortization | 34,545 | 15,061 | 11,663 | 11,208 | ||||||||||||
Provision for doubtful accounts | 23,578 | 9,509 | 5,885 | 3,073 | ||||||||||||
Income from equity investments | (3,777 | ) | (1,264 | ) | — | — | ||||||||||
(Gain) loss on disposal or impairment of long-lived assets, net | (2,097 | ) | 1,804 | 2,482 | 832 | |||||||||||
Loss on debt extinguishment | 16,102 | 23,414 | 9,863 | — | ||||||||||||
Merger transaction and integration costs | 17,920 | 21,690 | — | — | ||||||||||||
Termination of management agreement and IPO costs | 5,834 | — | — | — | ||||||||||||
Electronic health records incentive income | (1,761 | ) | (3,356 | ) | — | — | ||||||||||
Other (income) expenses | (525 | ) | (6 | ) | 297 | 40 | ||||||||||
Total operating expenses | 815,137 | 352,482 | 226,373 | 199,762 | ||||||||||||
Operating income | 144,754 | 50,807 | 58,226 | 60,453 | ||||||||||||
Tax receivable agreement expense | (119,911 | ) | — | — | — | |||||||||||
Interest expense, net | (100,980 | ) | (62,101 | ) | (32,929 | ) | (28,482 | ) | ||||||||
(Loss) income before income taxes | (76,137 | ) | (11,294 | ) | 25,297 | 31,971 | ||||||||||
Income tax (benefit) expense | (148,982 | ) | 15,758 | 7,570 | 6,110 | |||||||||||
Net income (loss) | 72,845 | (27,052 | ) | 17,727 | 25,861 | |||||||||||
Less: Net income attributable to non-controlling interests | (71,416 | ) | (38,845 | ) | (26,789 | ) | (23,945 | ) | ||||||||
Net income (loss) attributable to Surgery Partners, Inc. | $ | 1,429 | $ | (65,897 | ) | $ | (9,062 | ) | $ | 1,916 | ||||||
Net income (loss) per share attributable to common stockholders | ||||||||||||||||
Basic | 0.04 | (2.04 | ) | (0.28 | ) | 0.06 | ||||||||||
Diluted (1) | 0.04 | (2.04 | ) | (0.28 | ) | 0.06 | ||||||||||
Consolidated Statements of Cash Flow Data: | ||||||||||||||||
Net cash provided by operating activities | $ | 84,481 | $ | 21,949 | $ | 49,078 | $ | 46,377 | ||||||||
Net cash used in investing activities | (134,842 | ) | (271,016 | ) | (3,622 | ) | (3,468 | ) | ||||||||
Net cash provided by (used in) financing activities | 33,374 | 310,961 | (37,662 | ) | (43,061 | ) | ||||||||||
Other Data: | ||||||||||||||||
Adjusted EBITDA (2) | $ | 158,053 | $ | 77,034 | $ | 57,900 | $ | 50,959 | ||||||||
Adjusted EBITDA as a % of revenues | 16.5 | % | 19.1 | % | 20.3 | % | 19.6 | % | ||||||||
Number of surgical facilities as of the end of period (3) | 101 | 103 | 47 | 49 | ||||||||||||
Number of consolidated surgical facilities included as of the end of period | 90 | 91 | 47 | 49 | ||||||||||||
47
Year Ended December 31, | ||||||||||||
2015 | 2014 | 2013 | ||||||||||
Consolidated Balance Sheets Data: | ||||||||||||
Working capital | $ | 129,643 | $ | 127,258 | $ | 40,056 | ||||||
Total assets | 2,106,684 | 1,858,794 | 474,701 | |||||||||
Long-term debt, less current maturities | 1,230,328 | 1,339,266 | 418,559 | |||||||||
Total stockholders’ equity (deficit) | 297,927 | 29,536 | (14,375 | ) | ||||||||
(1) | The impact of potentially dilutive securities for the years ended December 31, 2014 and 2013 was not considered because the effect would be anti-dilutive in each of those periods. |
(2) | When we use the term “ Adjusted EBITDA,” we are referring to net income minus (a) net income attributable to non-controlling interests plus (b) income tax (benefit) expense, (c) interest expense, net, (d) depreciation and amortization, (e) management fee, (f) merger transaction, integration and practice acquisition costs, (g) termination of management agreement and IPO costs, (h) tax receivable agreement expense, (i) non-cash stock compensation expense, (j) loss on debt extinguishment and (k) (gain) loss on disposal of investments and long-lived assets. Non-controlling interests represent the interests of third parties, such as physicians, and in some cases, healthcare systems that own an interest in surgical facilities that we consolidate for financial reporting purposes. |
(3) | Includes surgical facilities that we manage but in which we have no ownership interest. |
We use "Adjusted EBITDA" to determine compliance with some of the covenants under the Credit Facility, as well as to determine the interest rate and commitment fee payable under our Credit Facility. See "Management's Discussion and Analysis of Financial Condition and Results of Operations - EBITDA and Adjusted EBITDA".
Adjusted EBITDA is not measurements of financial performance or liquidity under Generally Accepted Accounting Principles ("GAAP"). They should not be considered in isolation or as a substitute for net income, operating income, cash flows from operating, investing or financing activities, or any other measure calculated in accordance with generally accepted accounting principles. The items excluded from Adjusted EBITDA are significant components in understanding and evaluating financial performance and liquidity. Our calculation of Adjusted EBITDA may not be comparable to similarly titled measures reported by other companies.
48
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
Item 7. Management's Discussion and Analysis of Financial Condition and Results of Operations
The following discussion and analysis of our financial condition and results of operations should be read in conjunction with Item 6. “Selected Financial Data” and our audited consolidated financial statements and related notes included elsewhere in this report. This discussion contains forward-looking statements that involve risks and uncertainties. For additional information regarding some of the risks and uncertainties that affect our business and the industry in which we operate, please see Item 1A. “Risk Factors” found elsewhere in this report. Our actual results may differ materially from those estimated or projected in any of these forward-looking statements. Unless otherwise indicated or the context otherwise requires, references herein to the “Company”, “Surgery Partners”, “we”, “us” and “our” refer to, (i) Surgery Center Holdings, LLC and its consolidated subsidiaries, including Surgery Center Holdings, Inc., immediately prior to the Reorganization and (ii) Surgery Partners, Inc. and its consolidated subsidiaries, including Surgery Center Holdings, LLC and Surgery Center Holdings, Inc., immediately following the Reorganization. Unless the context implies otherwise, the term “affiliates” means direct and indirect subsidiaries of Surgery Center Holdings, LLC and Surgery Partners, Inc., as applicable, and partnerships and joint ventures in which such subsidiaries are partners. The terms “facilities” or “hospitals” refer to entities owned and operated by affiliates of Surgery Partners, and the term “employees” refers to employees of affiliates of Surgery Partners.
Cautionary Note Regarding Forward-Looking Statements
This report contains forward-looking statements, which are based on our current expectations, estimates and assumptions about future events. All statements other than statements of current or historical fact contained in this report, including statements regarding our future financial position, business strategy, budgets, effective tax rate, projected costs and plans and objectives of management for future operations, are forward-looking statements. The words “anticipate,” “believe,” “continue,” “estimate,” “expect,” “intend,” “may,” “plan,” “will,” and similar expressions are generally intended to identify forward-looking statements. These statements involve risks, uncertainties and other factors that may cause actual results to differ from the expectations expressed in the statements. Many of these factors are beyond our ability to control or predict. These factors include, without limitation: (i) reductions in payments from government healthcare programs and managed care organizations; (ii) inability to contract with private third-party payors; (iii) failure to fully integrate the operations of Surgery Partners and legacy Symbion; (iv) changes in our payor mix or surgical case mix; (v) failure to maintain relationships with our physicians; (vi) payor controls designed to reduce the number of surgical procedures; (vii) inability to integrate operations of acquired surgical facilities, attract new physician partners, or acquire additional surgical facilities; (viii) shortages or quality control issues with surgery-related products, equipment and medical supplies; (ix) competition for physicians, nurses, strategic relationships, acquisitions and managed care contracts; (x) inability to enforce non-compete restrictions against our physicians; (xi) material liabilities incurred as a result of acquiring surgical facilities; (xii) litigation or medical malpractice claims; (xiii) changes in the regulatory, economic and other conditions of the states where our surgical facilities are located; (xiv) substantial payments we expect to be required to make under the tax receivable agreement; and (xv) other risks and uncertainties described in this report.
In light of these risks, uncertainties and assumptions, the forward-looking events and circumstances discussed in this report may not occur, and actual results could differ materially from those anticipated or implied in the forward-looking statements. When you consider these forward-looking statements, you should keep in mind these risk factors and other cautionary statements in this report.
These forward-looking statements speak only as of the date made. Other than as required by law, we undertake no obligation to publicly update or revise any forward-looking statements, whether as a result of new information, future events or otherwise.
Executive Overview
As of March 11, 2016, we owned and operated a national network of surgical facilities, physician practices and a suite of ancillary services in 29 states. Our surgical facilities, which include ASCs and surgical hospitals, primarily provide non-emergency surgical procedures across many specialties, including, among others, otolaryngology ("ENT"), gastroenterology ("GI"), general surgery, ophthalmology, orthopedics, cardiology and pain management. Our surgical hospitals provide services, such as diagnostic imaging, laboratory, obstetrics, oncology, pharmacy, physical therapy and wound care. Our portfolio of outpatient surgical facilities is complemented by our suite of ancillary services, which support our physicians in providing high quality and cost-efficient patient care. These ancillary services are comprised of a diagnostic laboratory, multi-specialty physician practices, urgent care facilities, anesthesia services, optical services and specialty pharmacy services. As a result, we believe we are well positioned to benefit from rising consumerism and payors’ and patients’ focus on the delivery of high quality care and superior clinical outcomes in the lowest cost and care setting.
As of March 11, 2016, we owned or operated, primarily in partnership with physicians, a portfolio of 101 surgical facilities comprised of 96 ASCs and five surgical hospitals across 29 states. We owned a majority interest in 72 of the surgical facilities and consolidated 90 facilities for financial reporting purposes. In addition to surgical facilities, we owned or operated a network of 46 physician practices. For the year ended December 31, 2015, approximately 400,000 surgical procedures were performed in our surgical facilities, as compared to the year ended December 31, 2014, during which approximately 200,000 surgical procedures were performed.
We continue to focus on improving our same-facility performance, selectively acquiring established practices and developing new facilities. During the year ended December 31, 2015, we completed 13 in-market physician practice transactions through an aggregate investment of $40.4 million adding a total of 17 physicians to our network.
In addition, during the year ended December 31, 2015, we acquired a controlling interest in two surgical facilities located in new markets and three surgical facilities, four anesthesia practices and an urgent care in existing markets for an aggregate purchase price of
49
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
$84.2 million. Of the four anesthesia practices acquired, two are well established companies covering a total of ten hospitals and eleven ASCs in North Carolina and Georgia. Additionally, we acquired incremental ownership in two of our consolidated surgical facilities and in an existing anesthesia practice for an aggregate purchase price of $7.7 million.
On November 3, 2014, we completed the acquisition of Symbion Holdings Corporation ("Symbion") ("the Merger"), which added 55 surgical facilities, including 49 ASCs and six surgical hospitals, to our network of existing facilities. We acquired Symbion for a purchase price of $792.0 million pursuant to the terms of an Agreement and Plan of Merger dated as of June 13, 2014. The Symbion acquisition was financed through the issuance of approximately $1.4 billion under our Term Loans and Revolving Facility.
On October 1, 2015, we completed our initial public offering ("IPO") of 14,285,000 shares of common stock at an offering price of $19.00 per share. On October 6, 2015, we received net proceeds from the sale of common stock in this offering of $255.8 million, after deducting underwriting discounts and other fees of $15.6 million. These net proceeds were used to repay a portion of the borrowings outstanding under the 2014 Second Lien and to pay fees associated with this offering. The Company also incurred an additional $4.8 million in costs directly related to the IPO.
Revenues
Our revenues consist of patient service revenues and other service revenues. Patient service revenues consist of revenue from our surgical facility services and ancillary services segments. Specifically, patient service revenues include fees for surgical or diagnostic procedures performed at surgical facilities that we consolidate for financial reporting purposes, as well as for patient visits to our physician practices, anesthesia services, pharmacy services and diagnostic screens ordered by our physicians. Other service revenues consist of product sales from our optical laboratories, as well as the discounts and handling charges billed to the members of our optical products purchasing organization. Other service revenues also include management and administrative service fees derived from our non-consolidated facilities that we account for under the equity method, management of surgical facilities and physician practices in which we do not own an interest and management services we provide to physician practices for which we are not required to provide capital or additional assets.
The following table summarizes our revenues by service type as a percentage of total revenues for the periods indicated:
Year Ended December 31, | |||||||||
2015 | 2014 | 2013 | |||||||
Patient service revenues: | |||||||||
Surgical facilities revenues | 91.6 | % | 83.9 | % | 78.9 | % | |||
Ancillary services revenues | 6.4 | % | 12.3 | % | 15.5 | % | |||
98.0 | % | 96.2 | % | 94.4 | % | ||||
Other service revenues: | |||||||||
Optical services revenues | 1.5 | % | 3.5 | % | 5.6 | % | |||
Other | 0.5 | % | 0.3 | % | — | % | |||
2.0 | % | 3.8 | % | 5.6 | % | ||||
Total revenues | 100.0 | % | 100.0 | % | 100.0 | % | |||
Payor Mix
The following table sets forth by type of payor the percentage of our patient service revenues generated at the surgical facilities which we consolidate for financial reporting purposes in the periods indicated:
Year Ended December 31, | |||||||||
2015 | 2014 | 2013 | |||||||
Private insurance payors | 55.0 | % | 52.1 | % | 60.6 | % | |||
Government payors | 38.2 | % | 34.5 | % | 28.0 | % | |||
Self-pay payors | 1.7 | % | 3.5 | % | 2.8 | % | |||
Other payors(1) | 5.1 | % | 9.9 | % | 8.6 | % | |||
Total | 100.0 | % | 100.0 | % | 100.0 | % | |||
(1) Other is comprised of auto liability, letters of protection and other payor types.
50
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
The changes in payor mix are primarily related to the Symbion acquisition. On a pro forma basis, when effecting the 2014 and 2013 periods for Symbion, the payor mix percentages are consistent with the 2015 period.
Surgical Case Mix
We primarily operate multi-specialty surgical facilities where physicians perform a variety of procedures in various specialties, including ENT, GI, general surgery, ophthalmology, orthopedics, cardiology and pain management, among others. We believe this diversification helps to protect us from adverse pricing and utilization trends in any individual procedure type and results in greater consistency in our case volume.
The following table sets forth the percentage of cases in each specialty performed at the surgical facilities which we consolidate for financial reporting purposes for the periods indicated:
Year Ended December 31, | |||||||||
2015 | 2014 | 2013 | |||||||
Cardiology | 1.0 | % | 0.3 | % | — | % | |||
Otolaryngology | 4.1 | % | 2.8 | % | 2.5 | % | |||
Gastrointestinal | 22.2 | % | 15.0 | % | 10.7 | % | |||
General surgery | 2.9 | % | 2.9 | % | 2.4 | % | |||
Obstetrics/gynecology | 1.9 | % | 0.6 | % | — | % | |||
Ophthalmology | 30.0 | % | 40.7 | % | 47.6 | % | |||
Orthopedic | 12.1 | % | 11.6 | % | 10.8 | % | |||
Pain management | 17.6 | % | 21.5 | % | 22.2 | % | |||
Plastic surgery | 2.1 | % | 2.0 | % | 2.2 | % | |||
Other | 6.1 | % | 2.6 | % | 1.6 | % | |||
Total | 100.0 | % | 100.0 | % | 100.0 | % | |||
The changes in our surgical case mix are primarily attributable to the Symbion acquisition. On a pro forma basis, when effecting the 2014 and 2013 periods for Symbion, the surgical case mix is consistent with the 2015 period.
Same-facility Information
For the years ended December 31, 2015, 2014, and 2013, we define same facilities as those facilities that we have owned and operated since January 1, 2013. This includes facilities acquired in the Merger. We include the revenues from our surgical facilities, along with the revenues from our anesthesia services, diagnostic laboratory, physician practices, specialty pharmacy and optical services that complement our surgical facilities in our existing markets.
Year Ended December 31, | ||||||||
2015 | 2014 | |||||||
Cases | 400,230 | 380,623 | ||||||
Case growth | 5.2 | % | N/A | |||||
Revenue per case | $ | 2,484 | $ | 2,360 | ||||
Revenue per case growth | 5.3 | % | N/A | |||||
Number of facilities | 92 | N/A | ||||||
Operating Income Margin
Our operating income margin for the year ended December 31, 2015 increased to 15.1% from 12.6% during the year ended December 31, 2014. During the year ended December 31, 2015, we recorded $17.9 million of merger transaction and integration costs related to the Merger, a loss on debt extinguishment of $16.1 million, IPO equity-based compensation expense of $6.2 million, termination of management agreement and IPO costs of $5.8 million and a gain on disposal of long-lived assets of $2.1 million. Excluding the impact of these items, our operating income margin was 19.7% for the year ended December 31, 2015. Effecting the 2014 period for the Symbion acquisition, our operating income margin for the year ended December 31, 2014 was 21.5%.
Segment Information
A public company is required to report annual and interim financial and descriptive information about its reportable operating segments. Operating segments, as defined, are components of an enterprise about which separate financial information is available that is evaluated regularly by the chief operating decision maker, or “CODM,” in deciding how to allocate resources and in assessing
51
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
performance. Aggregation of similar operating segments into a single reportable operating segment is permitted if the businesses have similar economic characteristics and meet the criteria established by GAAP.
Our business is comprised of the following three reportable segments:
Surgical Facility Services Segment: Our surgical facility services segment consists of the operation of ASCs and surgical hospitals, and includes our anesthesia services. Our surgical facilities primarily provide non-emergency surgical procedures across many specialties, including, among others, ENT, GI, general surgery, ophthalmology, orthopedics, cardiology and pain management.
Ancillary Services Segment: Our ancillary services segment consists of a diagnostic laboratory, a specialty pharmacy and multi-specialty physician practices. These physician practices include our owned and operated physician practices pursuant to long-term management service agreements.
Optical Services Segment: Our optical services segment consists of an optical laboratory, an optical products group purchasing organization and a marketing business. Our optical laboratory manufactures eyewear, while our optical products purchasing organization negotiates volume buying discounts with optical product manufacturers.
Our financial information by reporting segment is prepared on an internal management reporting basis that the chief operating decision maker uses to allocate resources and assess the performance of the operating segments. Our operating segments have been defined based on the separate financial information that is regularly produced and reviewed by our CODM, which is our Chief Executive Officer.
During the three months ended June 30, 2015, we made changes to our internal reports issued to and reviewed by the CODM. The primary effect of these changes was to remove the allocation of general and administrative expense and assets to the reportable segments. We have revised the segment disclosures below to present corporate overhead and corporate assets as a reconciling item back to the reported consolidated financial information.
The following tables present financial information for each reportable segment (in thousands):
Year Ended December 31, | ||||||||||||
2015 | 2014 | 2013 | ||||||||||
Net Revenues: | ||||||||||||
Surgical facility services | $ | 884,144 | $ | 339,309 | $ | 224,578 | ||||||
Ancillary services | 61,175 | 49,787 | 44,103 | |||||||||
Optical services | 14,572 | 14,193 | 15,918 | |||||||||
Total revenues | $ | 959,891 | $ | 403,289 | $ | 284,599 | ||||||
Year Ended December 31, | ||||||||||||
2015 | 2014 | 2013 | ||||||||||
Segment Operating Income: | ||||||||||||
Surgical facility services | $ | 224,098 | $ | 112,237 | $ | 77,905 | ||||||
Ancillary services | 15,666 | 16,389 | 16,909 | |||||||||
Optical services | 2,283 | 2,238 | 3,032 | |||||||||
Total | $ | 242,047 | $ | 130,864 | $ | 97,846 | ||||||
General and administrative | $ | (59,534 | ) | $ | (33,149 | ) | $ | (27,275 | ) | |||
Gain (loss) on disposal or impairment of long-lived assets, net | 2,097 | (1,804 | ) | (2,482 | ) | |||||||
Loss on debt extinguishment | (16,102 | ) | (23,414 | ) | (9,863 | ) | ||||||
Merger transaction and integration costs | (17,920 | ) | (21,690 | ) | — | |||||||
Termination of management agreement and IPO costs | (5,834 | ) | — | — | ||||||||
Total operating income | $ | 144,754 | $ | 50,807 | $ | 58,226 | ||||||
52
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
Year Ended December 31, | ||||||||||||
2015 | 2014 | 2013 | ||||||||||
Supplemental Information: | ||||||||||||
Depreciation and amortization: | ||||||||||||
Surgical facility services | $ | 27,447 | $ | 9,911 | $ | 7,405 | ||||||
Ancillary services | 1,934 | 1,812 | 1,460 | |||||||||
Optical services | 1,622 | 1,641 | 1,862 | |||||||||
Total | $ | 31,003 | $ | 13,364 | $ | 10,727 | ||||||
General and administrative | $ | 3,542 | $ | 1,697 | $ | 936 | ||||||
Total depreciation and amortization | $ | 34,545 | $ | 15,061 | $ | 11,663 | ||||||
December 31, 2015 | December 31, 2014 | |||||||
Assets: | ||||||||
Surgical facility services | $ | 1,762,396 | $ | 1,638,874 | ||||
Ancillary services | 118,198 | 70,370 | ||||||
Optical services | 25,537 | 25,876 | ||||||
Total | $ | 1,906,131 | $ | 1,735,120 | ||||
General and administrative | $ | 200,553 | $ | 123,674 | ||||
Total assets | $ | 2,106,684 | $ | 1,858,794 | ||||
Year Ended December 31, | ||||||||||||
2015 | 2014 | 2013 | ||||||||||
Supplemental Information: | ||||||||||||
Cash purchases of property and equipment, net: | ||||||||||||
Surgical facility services | $ | 26,723 | $ | 5,158 | 2,301 | |||||||
Ancillary services | 1,051 | 1,034 | 562 | |||||||||
Optical services | 128 | 335 | 161 | |||||||||
Total | $ | 27,902 | $ | 6,527 | $ | 3,024 | ||||||
General and administrative | $ | 5,537 | $ | 1,209 | $ | 1,126 | ||||||
Total cash purchases of property and equipment, net | $ | 33,439 | $ | 7,736 | $ | 4,150 | ||||||
Critical Accounting Policies
Our significant accounting policies and practices are described in Note 2 of our consolidated financial statements included elsewhere in this report. In preparing our consolidated financial statements in conformity with Generally Accepted Accounting Principles ("GAAP"), our management must make estimates and assumptions that affect the reported amounts of assets and liabilities and related disclosures at the date of the financial statements and the reported amounts of revenue and expenses during the reporting period. Certain accounting estimates are particularly sensitive because of their complexity and the possibility that future events affecting them may differ materially from our current judgments and estimates. Our actual results could differ from those estimates. We believe that the following critical accounting policies are important to the portrayal of our financial condition and results of operations and require our management’s subjective or complex judgment because of the sensitivity of the methods, assumptions and estimates used. This listing of critical accounting policies is not intended to be a comprehensive list of all of our accounting policies. In many cases, the accounting treatment of a particular transaction is specifically dictated by GAAP, with no need for management’s judgment regarding accounting policy.
Consolidation and Control
Our consolidated financial statements include the accounts of our Company, wholly-owned or controlled subsidiaries and variable interest entities in which we are the primary beneficiary. Our controlled subsidiaries consist of wholly-owned subsidiaries and other subsidiaries that we control through our ownership of a majority voting interest or other rights granted to us by contract to function as the sole general partner or managing member of the surgical facility. The rights of limited partners or minority members at our controlled subsidiaries are generally limited to those that protect their ownership interests, including the right to approve the issuance of new
53
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
ownership interests, and those that protect their financial interests, including the right to approve the acquisition or divestiture of significant assets or the incurrence of debt that either physician limited partners or minority members are required to guarantee on a pro-rata basis based upon their respective ownership, or that exceeds 20.0% of the fair market value of the related surgical facility’s assets. All significant intercompany balances and transactions, including management fees from consolidated surgical facilities, are eliminated in consolidation.
We hold non-controlling interests in five surgical facilities, three anesthesia practices and one physician practice over which we exercise significant influence. Significant influence includes financial interests, duties, rights and responsibilities for the day-to-day management of the entity. We also consider the relevant sections of the Accounting Standard Codification ("ASC") 810, Consolidation, to determine if we have the power to direct the activities and are the primary beneficiary of (and therefore should consolidate) any entity whose operations we do not control with voting rights. As we were the primary beneficiary, we consolidated nine entities at December 31, 2015.
Revenue Recognition
Our patient service revenues are derived from surgical procedures performed at our ASCs, patient visits to physician practices, anesthesia services provided to patients, pharmacy services and diagnostic screens ordered by our physicians. The fees for such services are billed either to the patient or a third-party payor, including Medicare and Medicaid. We recognize patient service revenues, net of contractual allowances, which we estimate based on the historical trend of our cash collections and contractual write-offs.
Our optical products purchasing organization negotiates volume buying discounts with optical product manufacturers. The buying discounts and any handling charges billed to the members of the purchasing organization represent the revenues recognized for financial reporting purposes. Revenue is recognized as orders are shipped to members. Product sale revenues from our optical laboratories and marketing products and services businesses, net of an allowance for returns and discounts, is recognized when the product is shipped or service is provided to the customer. We base our estimates for sales returns and discounts on historical experience and have not experienced significant fluctuations between estimated and actual return activity and discounts given.
Other service revenues consist of management and administrative service fees derived from non-consolidated surgical facilities that we account for under the equity method, management of surgical facilities in which we do not own an interest and management services we provide to physician networks for which we are not required to provide capital or additional assets. The fees we derive from these management arrangements are based on a predetermined percentage of the revenues of each surgical facility and physician network. We recognize other service revenues in the period in which services are rendered.
Allowance for Contractual Adjustments and Doubtful Accounts
Our patient service revenues and other receivables from third-party payors are recorded net of estimated contractual adjustments and allowances from third-party payors, which we estimate based on the historical trend of our surgical facilities’ cash collections and contractual write-offs, accounts receivable agings, established fee schedules, relationships with payors and procedure statistics. While changes in estimated reimbursement from third-party payors remain a possibility, we expect that any such changes would be minimal and, therefore, would not have a material effect on our financial condition or results of operations.
We estimate our allowances for bad debts using similar information and analysis. While we believe that our allowances for contractual adjustments and bad debts are adequate, if the actual write-offs are significantly different from our estimates, it could have a material adverse effect on our financial condition and results of operations. Because in most cases we have the ability to verify a patient’s insurance coverage before services are rendered, and because we have entered into contracts with third-party payors which account for a majority of our total revenues, the out-of-period contractual adjustments have been minimal. Our net accounts receivable reflected allowances for doubtful accounts of $18.3 million and $5.3 million at December 31, 2015 and December 31, 2014, respectively.
Our collection policies and procedures are based on the type of payor, size of claim and estimated collection percentage for each patient account. The operating systems used to manage our patient accounts provide for an aging schedule in 30-day increments, by payor, physician and patient. We analyze accounts receivable at each of our surgical facilities to ensure the proper collection and aged category. The operating systems generate reports that assist in the collection efforts by prioritizing patient accounts. Collection efforts include direct contact with insurance carriers or patients, written correspondence and the use of legal or collection agency assistance, as required. Our days sales outstanding were 60 days for the year ended December 31, 2015 and 52 days for the year ended December 31, 2014.
At a consolidated level, we review the standard aging schedule, by facility, to determine the appropriate provision for doubtful accounts by monitoring changes in our consolidated accounts receivable by aged schedule, days sales outstanding and bad debt expense as a percentage of revenues. At a consolidated level, we do not review a consolidated aging by payor. Regional and local employees review each surgical facility’s aged accounts receivable by payor schedule. These employees have a closer relationship with the payors and have a more thorough understanding of the collection process for that particular surgical facility. Furthermore, this review is supported by an analysis of the actual revenues, contractual adjustments and cash collections received. If our internal collection efforts are unsuccessful, we further review patient accounts with balances of $25 or more. We then classify the accounts based on any external collection efforts we deem appropriate. An account is written-off only after we have pursued collection with legal or collection agency assistance or otherwise deemed an account to be uncollectible. Typically, accounts will be outstanding a minimum of 120 days before being written-off.
We recognize that final reimbursement of outstanding accounts receivable is subject to final approval by each third-party payor. However, because we have contracts with our third-party payors and we verify the insurance coverage of the patient before services
54
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
are rendered, the amounts that are pending approval from third-party payors are minimal. Amounts are classified outside of self-pay if we have an agreement with the third-party payor or we have verified a patient’s coverage prior to services rendered. It is our policy to collect co-payments and deductibles prior to providing services. It is also our policy to verify a patient’s insurance 72 hours prior to the patient’s procedure. Because our services are primarily non-emergency, our surgical facilities have the ability to control these procedures. Our patient service revenues from self-pay payors as a percentage of total revenues were approximately 1.7%, 3.5% and 2.8% for the years ended December 31, 2015, 2014 and 2013, respectively.
Income Taxes and Tax Receivable Agreement
We use the asset and liability method to account for income taxes. Under this method, deferred income tax assets and liabilities are recognized for the future tax consequences attributable to differences between the financial statement carrying amounts of existing assets and liabilities and their respective tax bases. Deferred tax assets and liabilities are measured using enacted tax rates expected to apply to taxable income in the years in which those temporary differences are expected to be recovered or settled. If a net operating loss carryforward exists, we make a determination as to whether that net operating loss carryforward will be utilized in the future. A valuation allowance will be established for certain net operating loss carryforwards and other deferred tax assets where their recoverability is deemed to be uncertain. The carrying value of the net deferred tax assets is based upon estimates and assumptions related to our ability to generate sufficient future taxable income in certain tax jurisdictions. If these estimates and related assumptions change in the future, we will be required to adjust our deferred tax valuation allowances.
As of December 31, 2015, we had unused federal net operating loss carryforwards (“NOLs”) of approximately $360.3 million. Such losses expire in various amounts at varying times beginning in 2025. Unless they expire, these NOLs may be used to offset future taxable income and thereby reduce our income taxes otherwise payable.
As a result of the successful IPO, reduction in interest expense, and continued growth and successful integration and synergies achieved from the Symbion acquisition, the Company released substantially all of the valuation allowance that was recorded against its deferred tax assets. Based on the Company's analysis of these and other items, it was determined that it is more likely than not that substantially all of the deferred tax assets will be realized. Therefore, the Company reduced its valuation allowance by approximately $136.0 million.
As a result of the reversal of the valuation allowance, we will need to continue to monitor results. If our expectations for future operating results on a consolidated basis or at the state jurisdiction level vary from actual results due to changes in healthcare regulations, general economic conditions, or other factors, we may need to adjust the valuation allowance, for all or a portion of our deferred tax assets. Our income tax expense in future periods will be reduced or increased to the extent of offsetting decreases or increases, respectively, in our valuation allowance in the period when the change in circumstances occurs. These changes could have a significant impact on our future earnings.
Section 382 (“Section 382”) of the Internal Revenue Code of 1986, as amended (the “Code”) imposes an annual limit on the ability of a corporation that undergoes an “ownership change” to use its NOLs to reduce its tax liability. An “ownership change” is generally defined as any change in ownership of more than 50.0% of a corporation’s “stock” by its “5-percent shareholders” (as defined in Section 382) over a rolling three-year period based upon each of those shareholder’s lowest percentage of stock owned during such period. As a result of the Symbion acquisition, approximately $179 million in NOL carryforwards are subject to an annual Section 382 base limitation of $4.9 million, and, as a result of the Novamed acquisition, approximately $17 million in NOL carryforwards are subject to an annual Section 382 base limitation of $4.9 million. It is possible that future transactions, not all of which would be within our control (including a possible sale by the investment funds affiliated with H.I.G. of some or all of their shares of our common stock), could cause us to undergo an ownership change as defined in Section 382. In that event, we would not be able to use our pre-ownership-change NOLs in excess of the limitation imposed by Section 382. At this time, we do not believe these limitations, when combined with amounts allowable due to net unrecognized built in gains, will affect our ability to use any NOLs before they expire. However, no such assurances can be provided. If our ability to utilize our NOLs to offset taxable income generated in the future is subject to this limitation, it could have an adverse effect on our business, prospects, results of operations and financial condition. We expect the payments we will be required to make under the TRA will be substantial.
As part of the Reorganization that was effective September 30, 2015, we entered into a Tax Receivable Agreement (“TRA”) under which generally we will be required to pay to our stockholders as of immediately prior to the IPO 85% of the cash savings, if any, in U.S. federal, state or local tax that we actually realize (or are deemed to realize in certain circumstances) as a result of (i) certain tax attributes, including NOLs, capital losses, charitable deductions, alternative minimum tax credit carryforwards and federal and state tax credits of Surgery Partners, Inc. and its affiliates relating to taxable years ending on or before the date of the Reorganization (calculated by assuming the taxable year of the relevant entity closes on the date of the Reorganization) that are or become available to us and our wholly-owned subsidiaries as a result of the Reorganization, and (ii) tax benefits attributable to payments made under the TRA, together with interest accrued at a rate of LIBOR plus 300 from the date the applicable tax return is due (without extension) until paid.
The amounts payable under the TRA will vary depending upon a number of factors, including the amount, character and timing of the taxable income of Surgery Partners, Inc. in the future. We estimate the total amounts payable under the TRA to be approximately $119.7 million, if the tax benefits of related deferred tax assets are ultimately realized. The amounts payable were recognized during the quarter ended December 31, 2015 in conjunction with the release of our valuation allowance recorded against the deferred tax assets.
55
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
Long-Lived Assets, Goodwill and Intangible Assets
We test our goodwill and indefinite-lived intangible assets for impairment annually, as of October 1, or more frequently if certain indicators arise. We review goodwill at the reporting unit level, which is defined as one level below an operating segment. We have determined that we has six reporting units, which include the following: 1) Surgical Facilities 2) Ancillary Services, 3) Midwest Labs, 4) The Alliance, including Optical Synergies, 5) Family Vision Care and 6) Patient Education Concepts, our marketing products and services business. When reviewing goodwill, we compare the carrying value of the net assets of the reporting unit to the net present value of the estimated discounted future cash flows of the reporting unit. If the carrying value exceeds the net present value of the estimated discounted future cash flows, an impairment indicator exists and an estimate of the impairment loss is calculated. The fair value calculation includes multiple assumptions and estimates, including the projected cash flows and discount rates applied.
During the quarter ended December 31, 2015, we voluntarily changed our annual goodwill and indefinite-lived intangible assets impairment testing date from December 31 to October 1. The change in the goodwill impairment test date better aligns the impairment testing procedures with the timing of our long-term planning process, which is a significant input to the testing. This change in testing date did not delay, accelerate, or avoid a goodwill impairment charge.
We performed our annual goodwill impairment assessment by developing a fair value estimate of the business enterprise as of October 1, 2015 using a discounted cash flows approach. The results of our fair value estimate were corroborated using a market-based approach. The result of our annual goodwill impairment test at October 1, 2015 indicated no impairment.
Off-Balance Sheet Arrangements
From time to time, we guarantee our pro-rata share of the third-party debts and other obligations of many of the non-consolidated partnerships and limited liability companies in which we own an interest. In most instances of these guarantees, the physicians and/or physician groups have also guaranteed their pro-rata share of the indebtedness to secure the financing. At December 31, 2015, we did not guarantee any debt of our non-consolidated surgical facilities.
JOBS Act Accounting Election
We are an “emerging growth company,” as defined in the Jumpstart Our Business Startups Act of 2012 ("the JOBS Act"). Under the JOBS Act, emerging growth companies can delay adopting new or revised accounting standards issued subsequent to the enactment of the JOBS Act until such time as those standards apply to private companies. We have irrevocably elected not to avail ourselves of this exemption from new or revised accounting standards and, therefore, will be subject to the same new or revised accounting standards as other public companies that are not emerging growth companies.
Equity-Based Compensation
We recognize in the financial statements the cost of employee services received in exchange for awards of equity instruments based on the fair value of those awards. Prior to the Reorganization, on the grant date, we employed a market approach to estimate the fair value of equity-based awards based on various considerations and assumptions, including implied earnings multiples and other metrics of relevant market participants, our operating results and forecasted cash flows and our capital structure. Such estimates require the input of highly subjective, complex assumptions. However, such assumptions are not required to determine fair value of shares of our common stock as our underlying shares are now publicly traded. The fair value of future stock options awarded will be based on the quoted market price of our common stock upon grant, as well as assumptions including expected stock price volatility, risk-free interest rate, expected dividends, and expected term.
Our policy is to recognize compensation expense using the straight line method over the relevant vesting period for units that vest based on time. Our equity-based compensation expense can vary in the future depending on many factors, including levels of forfeitures and whether performance targets are met and whether a liquidity event occurs. Prior to the Reorganization, employees held membership units in Surgery Center Holdings, LLC, and the associated expense was referred to as unit-based compensation; following the Reorganization, such expense is referred to as equity-based compensation.
56
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
Results of Operations
The following tables summarize certain results from the statements of operations for the years ended December 31, 2015, 2014 and 2013. The tables also show the percentage relationship to revenues for the periods indicated (dollars in thousands):
Year Ended December 31, | |||||||||||||||||||||
2015 | 2014 | 2013 | |||||||||||||||||||
Amount | % of Revenues | Amount | % of Revenues | Amount | % of Revenues | ||||||||||||||||
Revenues | $ | 959,891 | 100.0 | % | $ | 403,289 | 100.0 | % | $ | 284,599 | 100.0 | % | |||||||||
Operating expenses: | |||||||||||||||||||||
Cost of revenues | 669,326 | 69.7 | % | 254,178 | 63.0 | % | 169,844 | 59.7 | % | ||||||||||||
General and administrative expenses | 55,992 | 5.8 | % | 31,452 | 7.8 | % | 26,339 | 9.3 | % | ||||||||||||
Depreciation and amortization | 34,545 | 3.6 | % | 15,061 | 3.7 | % | 11,663 | 4.1 | % | ||||||||||||
Provision for doubtful accounts | 23,578 | 2.5 | % | 9,509 | 2.4 | % | 5,885 | 2.1 | % | ||||||||||||
Income from equity investments | (3,777 | ) | (0.4 | )% | (1,264 | ) | (0.3 | )% | — | — | % | ||||||||||
(Gain) loss on disposal or impairment of long-lived assets, net | (2,097 | ) | (0.2 | )% | 1,804 | 0.4 | % | 2,482 | 0.9 | % | |||||||||||
Loss on debt extinguishment | 16,102 | 1.7 | % | 23,414 | 5.8 | % | 9,863 | 3.5 | % | ||||||||||||
Merger transaction and integration costs | 17,920 | 1.9 | % | 21,690 | 5.4 | % | — | — | % | ||||||||||||
Termination of management agreement and IPO costs | 5,834 | 0.6 | % | — | — | % | — | — | % | ||||||||||||
Electronic health records incentive income | (1,761 | ) | (0.2 | )% | (3,356 | ) | (0.8 | )% | — | — | % | ||||||||||
Other (income) expenses | (525 | ) | (0.1 | )% | (6 | ) | — | % | 297 | 0.1 | % | ||||||||||
Total operating expenses | 815,137 | 84.9 | % | 352,482 | 87.4 | % | 226,373 | 79.5 | % | ||||||||||||
Operating income | 144,754 | 15.1 | % | 50,807 | 12.6 | % | 58,226 | 20.5 | % | ||||||||||||
Tax receivable agreement expense | (119,911 | ) | (12.5 | )% | — | — | % | — | — | % | |||||||||||
Interest expense, net | (100,980 | ) | (10.5 | )% | (62,101 | ) | (15.4 | )% | (32,929 | ) | (11.6 | )% | |||||||||
(Loss) income before income taxes | (76,137 | ) | (7.9 | )% | (11,294 | ) | (2.8 | )% | 25,297 | 8.9 | % | ||||||||||
Income tax (benefit) expense | (148,982 | ) | (15.5 | )% | 15,758 | 3.9 | % | 7,570 | 2.7 | % | |||||||||||
Net income (loss) | 72,845 | 7.6 | % | (27,052 | ) | (6.7 | )% | 17,727 | 6.2 | % | |||||||||||
Less: Net income attributable to non-controlling interests | (71,416 | ) | (7.4 | )% | (38,845 | ) | (9.6 | )% | (26,789 | ) | (9.4 | )% | |||||||||
Net income (loss) attributable to Surgery Partners, Inc. | $ | 1,429 | 0.1 | % | $ | (65,897 | ) | (16.3 | )% | $ | (9,062 | ) | (3.2 | )% | |||||||
Year Ended December 31, 2015 Compared to Year Ended December 31, 2014
Overview. During the year ended December 31, 2015, our revenues increased 138.0% to $959.9 million from $403.3 million for the year ended December 31, 2014. We incurred a net income attributable to Surgery Partners, Inc. for the 2015 period of $1.4 million, compared to a net loss attributable to Surgery Partners, Inc. of $65.9 million for the 2014 period.
Our financial results for the year ended December 31, 2015 compared to the year ended December 31, 2014 reflect the addition of the surgical facilities acquired in connection with our acquisition of Symbion on November 3, 2014.
Revenues. Revenues for the year ended December 31, 2015 compared to the year ended December 31, 2014 were as follows (dollars in thousands):
Year Ended December 31, | |||||||||||||||
2015 | 2014 | Dollar Variance | Percent Variance | ||||||||||||
Patient service revenues | $ | 940,711 | $ | 388,073 | $ | 552,638 | 142.4 | % | |||||||
Optical service revenues | 14,572 | 14,193 | 380 | 2.7 | % | ||||||||||
Other service revenues | 4,608 | 1,023 | 3,585 | 350.4 | % | ||||||||||
Total revenues | $ | 959,891 | $ | 403,289 | $ | 556,602 | 138.0 | % | |||||||
Patient service revenues increased 142.4% to $940.7 million for the year ended December 31, 2015 compared to $388.1 million for the year ended December 31, 2014. This increase in patient service revenues was primarily attributable to the acquisition of Symbion on November 3, 2014.
57
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
Cost of Revenues. Cost of revenues increased to $669.3 million for the year ended December 31, 2015 compared to $254.2 million for the year ended December 31, 2014 primarily due to the surgical facilities acquired in connection with the Symbion transaction on November 3, 2014. As a percentage of revenues, cost of revenues were 69.7% for the 2015 period and 63.0% for the 2014 period.
General and Administrative Expenses. General and administrative expenses increased to $56.0 million for the year ended December 31, 2015 compared to $31.5 million for the year ended December 31, 2014 primarily due to to the acquisition of Symbion on November 3, 2014 and the acceleration of stock compensation in connection with the IPO of $6.2 million. As a percentage of revenues, general and administrative expenses were 5.8% for the 2015 period compared to 7.8% for the 2014 period.
Depreciation and Amortization. Depreciation and amortization increased to $34.5 million for the year ended December 31, 2015 compared to $15.1 million for the year ended December 31, 2014 primarily due to the acquisition of Symbion on November 3, 2014. As a percentage of revenues, depreciation and amortization expenses were 3.6% for the 2015 period and 3.7% for the 2014 period.
Provision for Doubtful Accounts. The provision for doubtful accounts increased to $23.6 million for the year ended December 31, 2015 compared to $9.5 million for the year ended December 31, 2014 primarily due to the acquisition of Symbion on November 3, 2014. As a percentage of revenues, the provision for doubtful accounts was 2.5% for the 2015 period and 2.4% for the 2014 period.
Income from Equity Investments. Income from equity investments was $3.8 million for the year ended December 31, 2015 compared to $1.3 million for the year ended December 31, 2014 primarily due to the acquisition of Symbion on November 3, 2014 as we had no equity method investments prior to the Symbion acquisition.
(Gain) Loss on Disposal or Impairment of Long-Lived Assets, Net. The net gain on disposal of long-lived assets was $2.1 million for the year ended December 31, 2015 compared to a net loss of $1.8 million for the year ended December 31, 2014.
Loss on Debt Extinguishment. We incurred $16.1 million as a loss on debt extinguishment for the year ended December 31, 2015 compared to $23.4 million for the year ended December 31, 2014, related to the paydown of the Second Lien during 2015 and the refinancing in connection with the Merger during 2014.
Merger Transaction and Integration Costs. We incurred $17.9 million of merger transaction and integration costs for the year ended December 31, 2015 compared to $21.7 million for the year ended December 31, 2014, related to the Merger.
Termination of Management Agreement and IPO Costs. We incurred $5.8 million of costs related to the termination of our management agreement with Bayside Capital, Inc. and other related IPO costs for the year ended December 31, 2015.
Electronic Health Records Incentives. Income from electronic health records incentives was $1.8 million for the year ended December 31, 2015 compared to $3.4 million for the year ended December 31, 2014.
Operating Income. Our operating income was $144.8 million for the year ended December 31, 2015 compared to $50.8 million for the year ended December 31, 2014. The increase in the 2015 period from the 2014 period is primarily attributable to the surgical facilities acquired in connection with the Symbion transaction on November 3, 2014. As a percentage of revenues, operating income was 15.1% for the 2015 period and 12.6% for the 2014 period. During the year ended December 31, 2015, we recorded $17.9 million of merger transaction and integration costs related to the Merger, a loss on debt extinguishment of $16.1 million, IPO stock compensation expense of $6.2 million, termination of management agreement and IPO costs of $5.8 million and recorded a gain on the disposal of long-lived assets of $2.1 million. Excluding the impact of these items, our operating income margin was 19.7% for the year ended December 31, 2015. Effecting the 2014 period for the Symbion acquisition, our operating income margin for the year ended December 31, 2014 was 21.5%.
Tax Receivable Agreement Expense. We incurred tax receivable agreement expense of $119.9 million for the year ended December 31, 2015 due to the execution of the TRA on September 30, 2015 and the release of the valuation allowance previously recorded against our deferred tax assets.
Interest Expense, Net. Interest expense, net, increased to $101.0 million for the year ended December 31, 2015 compared to $62.1 million for the year ended December 31, 2014. The increase was primarily attributable to the new capital structure used to finance the acquisition of Symbion on November 3, 2014.
Income Tax (Benefit) Expense. The income tax (benefit) expense was $(149.0) million for the year ended December 31, 2015 compared to $15.8 million for the year ended December 31, 2014. The effective tax rate was 195.7% for the year ended December 31, 2015 compared to (139.5)% for the year ended December 31, 2014. The change in effective tax rate was primarily attributable to the tax-effect of the release of the valuation allowance during the year ended December 31, 2015.
Net Income Attributable to Non-Controlling Interests. Net income attributable to non-controlling interests increased to $71.4 million for the year ended December 31, 2015 compared to $38.8 million for the year ended December 31, 2014. The increase was primarily due to the surgical facilities acquired in connection with the Symbion transaction on November 3, 2014. As a percentage of revenues, net income attributable to non-controlling interests was 7.4% in the 2015 period and 9.6% for the 2014 period.
Year Ended December 31, 2014 Compared to Year Ended December 31, 2013
Overview. During the year ended December 31, 2014, our revenues increased 41.7% to $403.3 million from $284.6 million for the year ended December 31, 2013. We incurred a net loss attributable to Surgery Partners, Inc. for the year ended December 31, 2014 of $65.9 million, compared to $9.1 million for the year ended December 31, 2013.
58
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
Our financial results for the year ended December 31, 2014 compared to the year ended December 31, 2013 reflect the addition of 55 surgical facilities, including 49 ASCs and six hospitals, that were acquired in connection with our acquisition of Symbion on November 3, 2014.
Revenues. Revenues for the year ended December 31, 2014 compared to the year ended December 31, 2013 were as follows (dollars in thousands):
Year Ended December 31, | |||||||||||||||
2014 | 2013 | Dollar Variance | Percent Variance | ||||||||||||
Patient service revenues | $ | 388,073 | $ | 268,681 | $ | 119,392 | 44.4 | % | |||||||
Optical service revenues | 14,193 | 15,918 | (1,725 | ) | (10.8 | )% | |||||||||
Other service revenues | 1,023 | — | 1,023 | — | % | ||||||||||
Total revenues | $ | 403,289 | $ | 284,599 | $ | 118,690 | 41.7 | % | |||||||
Patient service revenues increased 44.4% to $388.1 million for the year ended December 31, 2014 compared to $268.7 million for the year ended December 31, 2013. This increase was primarily attributable to the surgical facilities we acquired in connection with the Symbion transaction on November 3, 2014.
Cost of Revenues. Cost of revenues increased to $254.2 million for the year ended December 31, 2014 compared to $169.8 million for the year ended December 31, 2013 primarily attributable to the surgical facilities we acquired in connection with the Symbion transaction on November 3, 2014. As a percentage of revenues, cost of revenues were 63.0% for the 2014 period and 59.7% for the 2013 period.
General and Administrative Expenses. General and administrative expenses were $31.5 million for the year ended December 31, 2014 compared to $26.3 million for the year ended December 31, 2013 primarily due to the acquisition of Symbion on November 3, 2014. As a percentage of revenues, general and administrative expenses were 7.8% for the 2014 period compared to 9.3% for the 2013 period.
Depreciation and Amortization. Depreciation and amortization expenses increased to $15.1 million for the year ended December 31, 2014 compared to $11.7 million for the year ended December 31, 2013 primarily due to the acquisition of Symbion on November 3, 2014. As a percentage of revenues, depreciation and amortization expenses were 3.7% for the 2014 period and 4.1% for the 2013 period.
Provision for Doubtful Accounts. The provision for doubtful accounts increased to $9.5 million for the year ended December 31, 2014 compared to $5.9 million for the year ended December 31, 2013 primarily due to the acquisition of Symbion on November 3, 2014. As a percentage of revenues, the provision for doubtful accounts was 2.4% for the 2014 period and 2.1% for the 2013 period.
Income from Equity Investments. Income from equity investments was $1.3 million in the year ended December 31, 2014. Prior to the acquisition of Symbion on November 3, 2014, we had no equity method investments.
Loss on Disposal or Impairment of Long-Lived Assets, Net. The net loss on disposal or impairment of long-lived assets was $1.8 million for the year ended December 31, 2014, and $2.5 million for the year ended December 31, 2013.
Merger Transaction and Integration Costs. We incurred $21.7 million of merger transaction and integration costs for the year ended December 31, 2014 related to the Merger.
Electronic Health Records Incentives. Income from electronic health records incentives was $3.4 million for the year ended December 31, 2014 compared to no income for the year ended December 31, 2013. This increase is attributable to the acquisition of Symbion, which included six surgical facilities licensed as hospitals that are eligible to receive incentive payments. In 2014, we met the meaningful use requirements and received incentive payments at three of our surgical hospitals.
Operating Income. Our operating income was $50.8 million for the year ended December 31, 2014 compared to $58.2 million for the year ended December 31, 2013. As a percentage of revenues, operating income was 12.6% for the 2014 period and 20.5% for the 2013 period. During the year ended December 31, 2014, we recorded $21.7 million of merger transaction and integration costs related to the Symbion acquisition, a loss on debt extinguishment of $23.4 million and recorded a gain of $1.8 million related to the sale of our ownership interest in a surgical facility. During the year ended December 31, 2013, we recorded a loss on debt extinguishment of $9.9 million and a loss on the disposal of $2.5 million. Excluding the impact of these items, our operating income margin was 24.2% for the year ended December 31, 2014 and 24.8% for the year ended December 31, 2013.
Interest Expense, Net. Interest expense, net, was $62.1 million for the year ended December 31, 2014 compared to $32.9 million for the year ended December 31, 2013. The increase was primarily attributable to the new capital structure used to finance the acquisition of Symbion on November 3, 2014.
Income Tax Expense. The provision for income taxes was $15.8 million for the year ended December 31, 2014 compared to $7.6 million for the year ended December 31, 2013. The effective tax rate was (139.5)% for the year ended December 31, 2014 compared to 29.9% for the year ended December 31, 2013. Income tax expense in each period was primarily attributable to non-cash deferred income tax expense related to our partnership investments.
59
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
Net Income Attributable to Non-Controlling Interests. Net income attributable to non-controlling interests increased to $38.8 million for the year ended December 31, 2014 compared to $26.8 million for the year ended December 31, 2013. This increase was primarily attributable to the surgical facilities we acquired in connection with the Symbion transaction on November 3, 2014. As a percentage of revenues, net income attributable to non-controlling interests was 9.6% for the 2014 period and 9.4% for the 2013 period.
Liquidity and Capital Resources
Operating Activities
The primary source of our operating cash flow is the collection of accounts receivable from federal and state agencies (under the Medicare and Medicaid programs), managed care health plans, commercial insurance companies and individuals. During the year ended December 31, 2015, our cash flow provided by operating activities increased to $84.5 million compared to $21.9 million in the year ended December 31, 2014. This increase was primarily attributable to the acquisition of Symbion. During the year ended December 31, 2015, we paid cash of $18.2 million in IPO and integration costs and $7.4 million related to third party settlements, net of cash received, related to prior years. Excluding the impact of these items, our cash flow provided by operating activities was $110.1 million for the year ended December 31, 2015. At December 31, 2015, we had working capital of $129.6 million compared to $127.3 million at December 31, 2014.
Investing Activities
Net cash used in investing activities during the year ended December 31, 2015 was $134.8 million, which included $33.4 million related to purchases of property and equipment. Additionally, we purchased five surgical facilities, thirteen physician practices, four anesthesia practices and an urgent care facility for an aggregate purchase price of $112.6 million (net of cash acquired). We received $11.2 million in aggregate proceeds for the sale of our interests in three surgical facilities.
Net cash used in investing activities during the year ended December 31, 2014 was $271.0 million, which included $7.7 million related to purchases of property and equipment. Additionally, we contributed cash of $300.1 million in connection with the acquisition of Symbion and contributed cash of $1.6 million to purchase three physician practices in the state of Florida.
Financing Activities
Net cash provided by financing activities during the year ended December 31, 2015 was $33.4 million. During this period, we received proceeds from our initial public offering, net of offering costs, of $251.0 million, made distributions to non-controlling interests holders of $69.7 million and payments related to ownership transactions with consolidated affiliates of $12.2 million. Further, we made repayments on our long-term debt of $328.3 million partially offset by borrowings of $196.4 million. Our repayments and borrowings include $104.5 million in draws and $14.5 million in repayments on our Revolver during the period.
Net cash provided by financing activities during the year ended December 31, 2014 was $311.0 million. During this period, we made distributions to owners of $93.0 million and to non-controlling interests holders of $35.2 million. We made repayments on our long-term debt of $1.0 billion and paid debt issuance costs of $7.5 million. These were offset by cash inflows from debt borrowings of $1.5 billion.
Long-Term Debt
A summary of long-term debt follows (in thousands):
December 31, 2015 | December 31, 2014 | December 31, 2013 | ||||||||||
2014 Revolver Loan | $ | 125,250 | $ | — | $ | — | ||||||
2014 First Lien Credit Agreement, dated November 3, 2014, maturing November 3, 2020, net of debt issuance and discount of $20,223 and $23,818 at December 31, 2015 and 2014, respectively | 841,078 | 846,183 | — | |||||||||
2014 Second Lien Credit Agreement, dated November 3, 2014, maturing November 3, 2021, net of debt issuance and discount of $8,159 and $18,184 at December 31, 2015 and 2014, respectively | 238,341 | 471,816 | — | |||||||||
2013 First Lien Credit Agreement, dated April 11, 2013, maturing April 11, 2019, net of debt issuance and discount of $6,385 at December 31, 2013 | — | — | 303,890 | |||||||||
2013 Second Lien Credit Agreement, dated April 11, 2013, maturing April 11, 2020, net of debt issuance and discount of $4,733 at December 31, 2013 | — | — | 115,267 | |||||||||
Subordinated Notes | 1,000 | 1,000 | 1,000 | |||||||||
Notes payable and secured loans | 40,615 | 31,600 | 3,590 | |||||||||
Capital lease obligations | 11,316 | 10,755 | 3,654 | |||||||||
Total debt | 1,257,600 | 1,361,354 | 427,401 | |||||||||
Less: Current maturities | 27,272 | 22,088 | 8,842 | |||||||||
Total long-term debt | $ | 1,230,328 | $ | 1,339,266 | $ | 418,559 | ||||||
The acquisition of Symbion on November 3, 2014 and payoff of the senior debt was financed through new $1.440 billion Senior Secured Credit Facilities (the "Facilities") consisting of the following:
• | $80.0 million revolving credit facility ("2014 Revolver Loan") |
• | $870.0 million 1st lien term loan facility ("2014 First Lien Credit Agreement") |
• | $490.0 million 2nd lien term loan facility ("2014 Second Lien Credit Agreement") |
On November 3, 2014, in connection with the consummation of the Symbion acquisition, we assumed and paid down approximately $440.0 million of outstanding indebtedness of Symbion, including accrued interest. Simultaneously, we paid off all of the debt outstanding under our 2013 First Lien Credit Agreement and 2013 Second Lien Credit Agreement ("2013 Credit Facilities") and revolver loan.
2014 Revolver Loan
The 2014 Revolver Loan (“Revolver”) will be used for working capital, acquisitions and development activities and general corporate purposes in an aggregate principal amount at any time outstanding not to exceed $80.0 million and matures on November 3, 2019. On October 7, 2015, we entered into an amendment to the 2014 First Lien Credit Agreement to increase certain lenders’ commitments under the Revolver from $80.0 million to an aggregate of $150.0 million. We have the option of classifying borrowings under the Revolver as either Alternate Base Rate ("ABR") loans or Eurodollar ("ED") loans. The interest base rate on an ABR loan is equal to the greatest of (a) the Prime Rate in effect on such day, (b) the Federal Funds Effective Rate in effect on such day plus 0.50% and (c) the adjusted LIBO Rate for a Eurodollar Borrowing with a one-month interest period plus 1.00%. In addition to the base rate, we are required to pay a 3.25% margin for ABR loans. The interest base rate on an ED loan is equal to (x) the LIBO Rate for such Eurodollar borrowing in effect for such Interest Period divided by (y) One minus the Statutory Reserves (if any) for such Eurodollar Borrowing for such interest period. In addition to the base rate, we are required to pay a 4.25% margin for ED loans. As of December 31, 2015, our availability on the Revolver was $21.6 million.
We paid $2.3 million in connection with obtaining the Revolver and recorded this amount as debt issuance costs, which is presented, net of accumulated amortization of approximately $530,000 and $76,000, in the accompanying consolidated balance sheets as of December 31, 2015 and December 31, 2014, respectively. We must also pay quarterly commitment fees of 0.50% per annum of the average daily unused amount of the Revolver.
The credit agreement that governs the Revolver contains various covenants that include limitations on our indebtedness, liens, acquisitions and investments. It additionally includes the requirement that we maintain a net leverage ratio within a specified range. At December 31, 2015, we were in compliance with the covenants contained in the credit agreement.
2014 First Lien Credit Agreement
The 2014 First Lien Credit Agreement (“2014 First Lien”) is a senior secured obligation of Surgery Center Holdings, Inc. and is guaranteed on a senior secured basis by us and certain of our subsidiaries. The 2014 First Lien matures on November 3, 2020. We have the option of classifying the 2014 First Lien as either an ABR loan or an ED loan. The interest base rate on an ABR loan is equal to the greatest of (a) the Prime Rate in effect on such day, (b) the Federal Funds Effective Rate in effect on such day plus 0.50%, and (c) the Adjusted LIBO Rate for a Eurodollar Borrowing with a one-month interest period plus 1.00%; provided that the base rate shall not be less than 2.00% per annum. In addition to the base rate, we are required to pay a 3.25% margin for ABR loans. The interest base rate on an ED loan is equal to (x) the LIBO Rate for such Eurodollar borrowing in effect for such Interest Period divided by (y) One minus the Statutory Reserves (if any) for such Eurodollar Borrowing for such interest period; provided that the rate shall not be less than 1.00% per annum. In addition to the base rate, we are required to pay a 4.25% margin for ED loans. In 2015, we classified the 2014 First Lien as an ED loan with an interest rate of 5.25% (1.00% base rate plus a 4.25% margin). Accrued interest is payable in arrears on a quarterly basis. Within five business days after the earlier of (i) 90 days after the end of each fiscal year or (ii) the date on which financial statements have been delivered, we are required to make mandatory prepayments in amounts calculated in accordance with the excess cash flow provisions of the 2014 First Lien Credit Agreement. There were no excess cash flow payments required as of December 31, 2015.
In 2014, we recorded $4.4 million and $20.0 million as a reduction of the carrying value of the 2014 First Lien as original issue discount and amounts paid to lender for debt related issuance costs, respectively, which are accreted to interest expense over the term of the loan. During the year ended December 31, 2015, approximately $3.6 million was accreted to interest expense. We also paid $1.9 million in connection with obtaining the 2014 First Lien and recorded this amount as debt issuance costs, which is presented as an asset, net of accumulated amortization of approximately $306,000 and $41,000, in the accompanying consolidated balance sheets as of December 31, 2015 and December 31, 2014, respectively.
The credit agreement that governs the 2014 First Lien contains various covenants that include limitations on our indebtedness, liens, acquisitions and investments. It additionally includes the requirement that we maintain a net leverage ratio within a specified range. At December 31, 2015, we were in compliance with the covenants contained in the credit agreement. The 2014 First Lien is collateralized by substantially all of our assets.
60
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
Scheduled amortization of the discount recorded in connection with the 2014 First Lien Credit Agreement follows (in thousands):
January 1, 2016 through December 31, 2016 | 3,767 | |||
January 1, 2017 through December 31, 2017 | 3,927 | |||
January 1, 2018 through December 31, 2018 | 4,107 | |||
January 1, 2019 through December 31, 2019 | 4,299 | |||
January 1, 2020 through November 3, 2020 | 4,123 | |||
Total discount on Senior Secured Notes | $ | 20,223 | ||
2014 Second Lien Credit Agreement
The 2014 Second Lien Credit Agreement (“2014 Second Lien”) is a senior secured obligation of Surgery Center Holdings, Inc. and is guaranteed on a senior secured basis by us and certain of our subsidiaries. The 2014 Second Lien matures on November 3, 2021. We have the option of classifying the 2014 Second Lien as either an ABR loan or an ED loan. The interest base rate on an ABR loan is equal to the greatest of (a) the Prime Rate in effect on such day, (b) the Federal Funds Effective Rate in effect on such day plus 0.50% and (c) the Adjusted LIBO Rate for a Eurodollar Borrowing with a one-month interest period plus 1.00%; provided that the base rate shall not be less than 2.00% per annum. In addition to the base rate, we are required to pay a 6.50% margin for ABR loans. The interest base rate on an ED loan is equal to (x) the LIBO Rate for such Eurodollar Borrowing in effect for such interest period divided by (y) One minus the Statutory Reserves (if any) for such Eurodollar Borrowing for such interest period; provided that the base rate shall not be less than 1.00% per annum. In addition to the base rate, we are required to pay a 7.50% margin for ED loans. During 2015, we classified the 2014 Second Lien as an ED loan with an interest rate of 8.50% (1.00% base rate plus a 7.50% margin). Accrued interest is payable in arrears on a quarterly basis. We are required to pay the remaining principal balance upon maturity of the 2014 Second Lien on November 3, 2021. We have the right at any time to prepay any borrowings, in whole or in part, provided that each partial prepayment shall be in an amount that is an integral multiple of $0.5 million and not less than $1.0 million. Within five business days after the earlier of (i) 90 days after the end of each fiscal year or (ii) the date on which financial statements have been delivered, we are required to make mandatory prepayments in amounts calculated in accordance with the excess cash flow provisions of the 2014 Second Lien. There were no excess cash flow payments required as of December 31, 2015.
We recorded $4.9 million and $13.6 million as a reduction of the carrying value of the 2014 Second Lien as original issue discount and amounts paid to lender for debt related issuance costs, respectively, which are accreted to interest expense over the term of the loan. During the year ended December 31, 2015, approximately $1.7 million was accreted to interest expense and $498,000 was written off to loss on debt extinguishment in connection with the prepayment discussed herein. We also paid $1.1 million in connection with obtaining the 2014 Second Lien and recorded this amount as debt issuance costs, which is presented as an asset, net of accumulated amortization of approximately $57,000 and $14,000, in the accompanying consolidated balance sheets as of December 31, 2015 and December 31, 2014, respectively.
On October 6, 2015, we prepaid $243.5 million in principal, net of the write-off of discounts and issuance costs totaling $8.3 million, and $65,000 of accrued interest on the 2014 Second Lien. Further, we incurred a prepayment penalty of 3% of the aggregate principal amount or $7.3 million. The write-off of the discounts and issuance costs, the prepayment penalty as well as certain other costs are presented as a loss on debt extinguishment of $16.1 million in the accompanying consolidated statement of operations as of December 31, 2015.
The credit agreement that governs the 2014 Second Lien contains various covenants that include limitations on our indebtedness, liens, acquisitions and investments. It additionally includes the requirement that we maintain a maximum net leverage ratio. At December 31, 2015, we were in compliance with the covenants contained in the credit agreement. The 2014 Second Lien is collateralized by substantially all of our assets.
Scheduled amortization of the discount recorded in connection with the Second Lien Term Loan follows (in thousands):
January 1, 2016 through December 31, 2016 | 1,102 | ||
January 1, 2017 through December 31, 2017 | 1,207 | ||
January 1, 2018 through December 31, 2018 | 1,325 | ||
January 1, 2019 through December 31, 2019 | 1,455 | ||
January 1, 2020 through November 30, 2020 | 1,602 | ||
January 1, 2021 through November 3, 2021 | 1,468 | ||
Total discount on Senior Secured Notes | $ | 8,159 | |
Other Debt Transactions
On April 11, 2013, we raised $465 million in Senior Secured Credit Facilities (“Credit Facilities”) to refinance a portion of its then existing debt and to return capital to its shareholders (“2013 Debt Refinancing”). These Credit Facilities were used to pay off the $233.7
61
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
million outstanding balance of the original $240.0 million term loan (“Term A Loan”), plus accrued interest and fees, and $52.8 million of the outstanding balance of the subordinated debt facility (“Subordinated Notes A”), plus accrued interest and fees. On the date of closing, we had no outstanding balance on the original $30.0 million Revolving Loan (“Revolving Loan”). As a result of these transactions, the Term A Loan and Revolving Loan were terminated. The Subordinated Notes A were amended with the outstanding principal balance reduced to $1.0 million.
On January 27, 2014, we obtained $90.0 million in additional borrowings on the 2013 Credit Facilities to return capital to shareholders. We recorded $1.4 million and $2.9 million as a reduction of the carrying value of the additional borrowings as original issue discount and amounts paid to lender for debt related issuance costs, respectively, which are accreted to interest expense over the term of the loan. During the year ended December 31, 2014, approximately $380,000 was accreted to interest expense. The $90.0 million in additional borrowings, including the related debt issuance costs, were included in the extinguishment of debt that was financed with the proceeds of the Facilities obtained in connection with the acquisition of Symbion on November 3, 2014.
Subordinated Notes
Effective April 11, 2013, we amended and reduced the size of our subordinated debt facility ("Subordinated Notes") to $1.0 million from $53.8 million. The prepayment premium of $1.6 million that we paid in connection with decreasing the size of the subordinated debt facility and the unamortized balance of debt issuance costs related to Subordinated Notes A of $1.1 million were recorded as loss on the extinguishment of debt in the accompanying consolidated statements of operations for the year ended December 31, 2013. Through a separate transaction in April 2013, H.I.G. Surgery Centers, LLC, our affiliate, LLC, purchased the Subordinated Notes from an independent third party. At December 31, 2015 and December 31, 2014, the debt is payable to H.I.G. Surgery Centers, LLC. and mature on August 4, 2017.
The outstanding balance of the Subordinated Notes A bore interest of 15.00% per annum through December 31, 2013, of which 12.00% per annum was payable quarterly in cash. We had the option to elect that the remaining 3.00% per annum be added to the unpaid principal amount as payment-in-kind ("PIK") or to pay the additional interest in cash. Beginning October 1, 2012, we elected to begin paying the additional 3.00% interest in cash on a quarterly basis. Effective January 1, 2014, the Subordinated Notes bear interest of 17.00% per annum.
Term Loan A
During 2011, we entered into a $240.0 million Term Loan A related to the acquisition of NovaMed. The Term Loan A was effective May 4, 2011, and was terminated on April 11, 2013 in connection with the 2013 Debt Transactions discussed above. We were required to pay quarterly principal payments of $600,000 on the last business day of each March, June, September and December during which the Term Loan A was outstanding. We had the option of classifying the Term Loan A as either an ABR loan or an ED loan. During 2013 (until termination of the Term Loan A), we classified the Term Loan A as an ED loan with an interest rate of 6.50%.
We recorded $1.2 million as a reduction of the carrying value of the Term Loan A as original issue discount which was accreted to interest expense over the term of the loan. During 2013, approximately $58,000 was accreted to interest expense, respectively. We also paid $8.7 million in connection with obtaining the Term Loan A and amortized approximately $417,000 of these costs during the years ended December 31, 2013, respectively.
2011 Revolving Loan
In 2011, we secured a 5-year, $20.0 million Revolving Loan (“2011 Revolving Loan”) to be used for working capital and general corporate purposes. The 2011 Revolving Loan was terminated on April 11, 2013 in connection with the 2013 Debt Refinancing. We recorded $100,000 as a reduction of the carrying value of the 2011 Revolving Loan as original issue discount, which was accreted to interest expense over the term of the loan. We also paid $681,000 in connection with obtaining the Revolving Loan and amortized $37,800 of these costs during the years ended December 31, 2013. We also paid quarterly commitment fees of 0.50% per annum on the average daily unused amount of the 2011 Revolving Loan.
Notes Payable and Secured Loans
Certain of our subsidiaries have outstanding bank indebtedness, which is collateralized by the real estate and equipment owned by the surgical facilities to which the loans were made. The various bank indebtedness agreements contain covenants to maintain certain financial ratios and also restrict encumbrance of assets, creation of indebtedness, investing activities and payment of distributions. At December 31, 2015, we were in compliance with the covenants contained in the credit agreement. The outstanding balance on notes payable to financial institutions was $40.6 million and $31.6 million as of December 31, 2015 and December 31, 2014, respectively.
Letters of Credit
As of December 31, 2014, we had two outstanding letters of credit at our optical purchasing group of $200,000 and $730,000. In May 2015, we increased one of these letters of credit from $200,000 to $500,000. We had two outstanding letters of credit issued to the landlords for two of its surgical facilities in Orlando, Florida in the amount of $100,000 and in Lubbock, Texas for $1.0 million. In addition, we had one outstanding letter of credit related to the Symbion, Inc. workers compensation self-insured plan for $835,000.
Capital Lease Obligations
We are liable to various vendors for several equipment leases. The carrying value of the leased assets was $12.3 million and $13.3 million as of December 31, 2015 and December 31, 2014, respectively.
62
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
Summary
We believe we have sufficient liquidity in the next 12 to 18 months as described above. Nevertheless, we continue to monitor the state of the financial and credit markets and our current and expected liquidity and capital resource needs, and intend to continue to explore various financing alternatives to improve capital structure, including reducing debt, extending maturities or relaxing financial covenants. These may include new equity or debt financings or exchange offers with existing security holders (including exchanges of debt for debt or equity) and other transactions involving our outstanding securities, given their secondary market trading prices. We cannot assure you, if we pursue any of these transactions, that we will be successful in completing a transaction on attractive terms, or at all.
EBITDA and Adjusted EBITDA
When we use the term “EBITDA,” we are referring to net income minus (a) net income attributable to non-controlling interests plus (b) income tax (benefit) expense, (c) interest expense, net, and (d) depreciation and amortization. Non-controlling interests represent the interests of third parties, such as physicians, and in some cases, healthcare systems that own an interest in surgical facilities that we consolidate for financial reporting purposes. Our operating strategy is to apply a market-based approach in structuring our partnerships with individual market dynamics driving the structure. We believe that it is helpful to investors to present EBITDA as defined above because it excludes the portion of net income attributable to these third-party interests and clarifies for investors our portion of EBITDA generated by our surgical facilities and other operations.
We use EBITDA as a measure of liquidity. We have included it because we believe that it provides investors with additional information about our ability to incur and service debt and make capital expenditures. We use "Adjusted EBITDA" to determine compliance with some of the covenants under the Credit Facility, as well as to determine the interest rate and commitment fee payable under our Credit Facility. When we use the term "Adjusted EBITDA", we are referring to EBITDA, as defined above, adjusted for (a) management fee, (b) merger transaction, integration and practice acquisition costs, (c) termination of management agreement and IPO costs, (d) tax receivable agreement expense, (e) non-cash stock compensation expense, (f) loss on debt extinguishment and (g) loss (gain) on disposal of investments and long-lived assets.
EBITDA and Adjusted EBITDA are not measurements of financial performance or liquidity under GAAP. They should not be considered in isolation or as a substitute for net income, operating income, cash flows from operating, investing or financing activities, or any other measure calculated in accordance with generally accepted accounting principles. The items excluded from EBITDA and Adjusted EBITDA are significant components in understanding and evaluating financial performance and liquidity. Our calculation of EBITDA and Adjusted EBITDA may not be comparable to similarly titled measures reported by other companies.
63
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
The following table reconciles Adjusted EBITDA to net income (in thousands):
Year Ended December 31, | ||||||||||||
2015 | 2014 | 2013 | ||||||||||
Consolidated Statements of Operations Data (in thousands): | ||||||||||||
Net income | $ | 72,845 | $ | (27,052 | ) | $ | 17,727 | |||||
(Minus): | ||||||||||||
Net income attributable to non-controlling interests | 71,416 | 38,845 | 26,789 | |||||||||
Plus (minus): | ||||||||||||
Income tax (benefit) expense | (148,982 | ) | 15,758 | 7,570 | ||||||||
Interest expense, net | 100,980 | 62,101 | 32,929 | |||||||||
Depreciation and amortization | 34,545 | 15,061 | 11,663 | |||||||||
EBITDA | (12,028 | ) | 27,023 | 43,100 | ||||||||
Plus: | ||||||||||||
Management fee (1) | 2,250 | 2,161 | 2,000 | |||||||||
Merger transaction, integration and practice acquisition costs | 20,579 | 21,690 | — | |||||||||
Termination of management agreement and IPO costs | 5,834 | — | — | |||||||||
Tax receivable agreement expense | 119,911 | — | — | |||||||||
Non-cash stock compensation expense | 7,502 | 942 | 455 | |||||||||
Loss on debt extinguishment | 16,102 | 23,414 | 9,863 | |||||||||
(Gain) loss on disposal of investments and long-lived assets, net | (2,097 | ) | 1,804 | 2,482 | ||||||||
Adjusted EBITDA | $ | 158,053 | $ | 77,034 | $ | 57,900 | ||||||
(1): Fee payable pursuant the Management and Investment Advisory Services Agreement between the Company and Bayside Capital, Inc.
Contractual Obligations and Commercial Commitments
The following table summarizes our contractual obligations by period as of December 31, 2015 (in thousands):
Payments Due by Period | ||||||||||||||||||||
Total | Less than 1 year | 1-3 years | 4-5 years | More than 5 years | ||||||||||||||||
Long-term debt, including current maturities | $ | 1,274,666 | $ | 23,102 | $ | 40,354 | $ | 963,226 | $ | 247,985 | ||||||||||
Cash interest obligations | 347,397 | 68,564 | 133,704 | 127,261 | 17,868 | |||||||||||||||
Capital lease obligations | 11,316 | 4,170 | 5,408 | 1,692 | 47 | |||||||||||||||
Operating lease obligations | 256,392 | 36,443 | 62,740 | 47,078 | 110,131 | |||||||||||||||
Other financing obligations(1) | 54,892 | 965 | 3,158 | 4,546 | 46,223 | |||||||||||||||
Total contractual obligations | $ | 1,944,663 | $ | 133,244 | $ | 245,364 | $ | 1,143,803 | $ | 422,254 | ||||||||||
(1) | Other financing obligations include a payable to the hospital facility lessor at our surgical hospital located in Idaho Falls, Idaho relating to the land, building and improvements at this facility and a payable to the facility lessor in Ocala, Florida relating to the building at this facility. |
Inflation
Inflation and changing prices have not significantly affected our operating results or the markets in which we operate.
Recent Accounting Pronouncements
In May 2014, the FASB issued ASU 2014-09, "Revenue from Contracts with Customers," which outlines a single comprehensive model for recognizing revenue and supersedes most existing revenue recognition guidance, including guidance specific to the healthcare industry. This ASU provides companies the option of applying a full or modified retrospective approach upon adoption. This ASU was originally set to be effective for fiscal years beginning after December 15, 2016, and early adoption was not permitted. In July 2015, the
64
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
FASB deferred the effective date for the standard to be effective for fiscal years beginning after December 15, 2017. The FASB will now permit companies to early adopt within one year of the new effective date. We will adopt this ASU on January 1, 2018 and is currently evaluating its plan for adoption and the impact on our revenue recognition policies, procedures and the resulting impact on our consolidated financial position, results of operations and cash flows.
In February 2015, the FASB issued ASU 2015-02, “Consolidation: Amendments to the Consolidation Analysis,” which amends the current consolidation guidance, including introducing a separate consolidation analysis specific to limited partnerships and other similar entities. Under this analysis, limited partnerships and other similar entities will be considered a variable-interest entity unless the limited partners hold substantive kick-out rights or participating rights. The provisions of ASU 2015-02 are effective for annual reporting periods beginning after December 15, 2015. Early adoption is permitted. We do not anticipate that the adoption of ASU 2015-02 will have a material impact on our financial position, results of operations, cash flows and financial disclosures.
In April 2015, the FASB issued ASU 2015-03, “Simplifying the Presentation of Debt Issuance Costs," which simplifies the presentation of debt issuance costs by requiring debt issuance costs related to a recognized debt liability be presented in the balance sheet as a direct deduction from the carrying amount of that debt liability, consistent with debt discounts. ASU 2015-03 is effective for fiscal years, and interim periods within those years, beginning after December 15, 2015. Early adoption is permitted, and the new guidance should be applied retrospectively. We plan to adopt this ASU on January 1, 2016, and do not anticipate that such adoption will have a material effect on our consolidated financial position, results of operations, or cash flows.
In August 2015, the FASB issued ASU 2015-15, "Presentation and Subsequent Measurement of Debt Issuance Costs Associated with Line-of-Credit Arrangements" which clarifies the SEC staff’s position on presenting and measuring debt issuance costs incurred in connection with line-of-credit arrangements given the lack of guidance on this topic in ASU 2015-03. The SEC staff has announced that it would “not object to an entity deferring and presenting debt issuance costs as an asset and subsequently amortizing the deferred debt issuance costs ratably over the term of the line-of-credit arrangement.” We plan to adopt this ASU on January 1, 2016, and do not anticipate that such adoption will have a material effect on our consolidated financial position, results of operations, or cash flows.
In September 2015, the FASB issued ASU 2015-16, “Business Combinations: Simplifying the Accounting for Measurement-Period Adjustments” which eliminates the requirement for an acquirer to retrospectively adjust its financial statements for changes to provisional amounts that are identified during the measurement-period following the consummation of a business combination. Instead, ASU 2015-16 requires these types of adjustments to be made during the reporting period in which they are identified and would require additional disclosure or separate presentation of the portion of the adjustment that would have been recorded in the previously reported periods as if the adjustment to the provisional amounts had been recognized as of the acquisition date. ASU 2015-16 is effective prospectively for fiscal years beginning after December 15, 2015, including interim periods within those years. We do not anticipate that the adoption of ASU 2015-16 will have a material impact on our financial position, results of operations, cash flows and financial disclosures.
In November 2015, the FASB issued ASU 2015-17, “Balance Sheet Classification of Deferred Taxes”, which simplifies the presentation of deferred income taxes. This ASU requires that deferred tax assets and liabilities be classified as non-current in a statement of financial position. We early adopted ASU 2015-17 effective December 31, 2015 on a prospective basis. Adoption of this ASU resulted in a reclassification of our net current deferred tax asset to the net non-current deferred tax asset in our consolidated balance sheet as of December 31, 2015. No prior periods were retrospectively adjusted.
In February 2016, the FASB issued ASU No. 2016-02, "Leases", which will require, among other items, lessees to recognize most leases as assets and liabilities on the balance sheet. Qualitative and quantitative disclosures will be enhanced to better understand the amount, timing and uncertainty of cash flows arising from leases. This guidance is effective for financial statements issued for fiscal years beginning after December 15, 2018, and interim periods within those fiscal years, with early adoption permitted. We are currently evaluating the impact this new guidance may have on the consolidated financial statements.
Sources of Revenue and Recent Regulatory Developments
General
The healthcare industry is highly regulated, and we cannot provide any assurance that the regulatory environment in which we operate will not significantly change in the future or that we will be able to successfully address any such changes.
Every state imposes licensing requirements on individual physicians and healthcare facilities. In addition, federal and state laws regulate HMOs and other managed care organizations. Many states require regulatory approval, including licensure and accreditation, and in some cases, certificates of need, before establishing certain types of healthcare facilities, including surgical hospitals and ASCs, offering certain services, including the services we offer, or making expenditures in excess of certain amounts for healthcare equipment, facilities or programs. Our ability to operate profitably will depend in part upon our surgical facilities obtaining and maintaining all necessary licenses, accreditation, certificates of need and other approvals and operating in compliance with applicable healthcare regulations. Failure to do so could have a material adverse effect on our business.
Our surgical facilities are subject to federal, state and local laws dealing with issues such as occupational safety, employment, medical leave, insurance regulations, civil rights, discrimination, building codes and medical waste and other environmental issues. Federal, state and local governments are expanding the regulatory requirements on businesses like ours. The imposition of these regulatory requirements may have the effect of increasing operating costs and reducing the profitability of our operations.
We believe that hospital, outpatient surgery, physician, laboratory and other diagnostic and healthcare services will continue to be subject to intense regulation at the federal and state levels. We are unable to predict what additional government regulations, if any, affecting our business may be enacted in the future or how existing or future laws and regulations might be interpreted. If we, or any of our surgical facilities, fail to comply with applicable laws, it might have a material adverse effect on our business.
Certificates of Need and Licensure
Capital expenditures for the construction of new healthcare facilities, the addition of beds or new healthcare services or the acquisition of existing healthcare facilities may be reviewable by state regulators under statutory schemes that are sometimes referred to as certificate of need laws. States with certificate of need laws place limits on the construction and acquisition of healthcare facilities and the expansion of existing facilities and services. In these states, approvals, generally known as certificates of need, are required for capital expenditures exceeding certain preset monetary thresholds for the development, acquisition and/or expansion of certain facilities or services, including surgical facilities. We have a concentration of surgical facilities in certificate of need states as we believe the regulations present a competitive advantage to existing operators.
Our healthcare facilities also are subject to state licensing requirements for medical providers. Our ASC facilities have licenses to operate in the states in which they operate and must meet all applicable requirements for ASCs. In addition, even though our surgical facilities that are licensed as hospitals primarily provide surgical services, they must meet all applicable requirements for general hospital licensure. To assure continued compliance with these regulations, governmental and other authorities periodically inspect our surgical facilities. The failure to comply with these regulations could result in the suspension or revocation of a facility’s license. In addition, based on the specific operations of our surgical facilities, some of these facilities maintain a pharmacy license, a controlled substance registration, a clinical laboratory certification waiver, and environmental protection permits for biohazards and/or radioactive materials, as required by applicable law.
Healthcare Reform
The Affordable Care Act has been subject to a number of challenges to its constitutionality. On June 28, 2012, the United States Supreme Court upheld challenges to the constitutionality of the “individual mandate” provision, which generally requires all individuals to purchase healthcare insurance or pay a penalty, but struck down as unconstitutional the provision that would have allowed the federal government to revoke all federal Medicaid funding to any state that did not expand its Medicaid program. As a result, many states have refused to extend Medicaid eligibility to more individuals as envisioned by the law.
On June 25, 2015, the United States Supreme Court upheld the legality of premium subsidies made available by the federal government to individuals residing in the 36 states that have federally-run health insurance exchanges. The subsidies are provided to low-income individuals to assist with the cost of purchasing health insurance through federally-run health insurance exchanges. Other legal challenges to the Affordable Care Act are pending.
In addition, several bills have been and will likely continue to be advanced in Congress that would defund, repeal or amend all or significant provisions of the Affordable Care Act, and a number of provisions of the Affordable Care Act that were supposed to become effective have been delayed by the Obama administration. As a result, it is difficult to predict the impact the Affordable Care Act will have on our business given the threats to and uncertainty surrounding key provisions of the Affordable Care Act. However, depending on how the Affordable Care Act is ultimately interpreted, amended and implemented, it could have an adverse effect on our business, financial condition and results of operations.
65
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
Moreover, other legislative changes have also been proposed and adopted since the Affordable Care Act was enacted. On August 2, 2011, the Budget Control Act of 2011, among other things, created measures for spending reductions by Congress. A Joint Select Committee on Deficit Reduction, tasked with recommending a targeted deficit reduction of at least $1.2 trillion for the years 2013 through 2021, was unable to reach required goals, thereby triggering the legislation’s automatic reduction to several government programs. This included aggregate reductions to Medicare payments to providers of 2% per fiscal year, which went into effect on April 1, 2013 and, due to subsequent legislative amendments, will remain in effect through 2025 unless additional Congressional action is taken. On January 2, 2013, President Obama signed into law the American Taxpayer Relief Act of 2012, which, among other things, further reduced Medicare payments to several providers, including hospitals, and increased the statute of limitations period for the government to recover overpayments to providers from three to five years. These and other similar new laws may result in additional reductions in Medicare and other health care funding, which could have a material adverse effect on our financial operations.
Medicare and Medicaid Private Contractor Audits
CMS has implemented a number of programs that use private contractors that contract with CMS to identify overpayments and underpayments and other potential sources of billing fraud. These contractors, known as Recovery Audit Contractors (“RACs”) and Zone Program Integrity Contractors (“ZPICs”) conduct both post-payment and pre-payment review of claims submitted by Medicare providers. In addition, CMS employs Medicaid Integrity Contractors (“MICs”) to perform post-payment audits of Medicaid claims and identify overpayments. Our facilities and providers continue to receive letters from auditors such as RACs and ZPICs requesting repayment of alleged overpayments for services and incur expenses associated with responding to and appealing these determinations, as well as the costs of repaying any overpayments. Moreover, in recent years, the increase in Medicare payment appeals has created a backlog such that resolving appeals often takes multiple years.
For instance, we recently received the results of a MIC audit that resulted in an overpayment obligation. HMS Federal Solutions, a MIC, completed the audit of one of our surgical hospitals for the period July 1, 2009 through May 31, 2012 and determined an overpayment obligation in the amount of approximately $4.6 million based on its extrapolation of a statistical sampling of claims, as well as a civil monetary penalty in the amount of $162,000, for a total amount owed to Idaho’s Department of Health and Welfare, Medicaid Program Integrity Unit of approximately $4.7 million for failure to comply with Medicaid rules by billing for (i) non-covered services, (ii) services provided by non-eligible providers, (iii) services not provided and (iv) unauthorized services. We have appealed the audit and are currently awaiting the result.
Although all other repayments requested to date as a result of RAC, MIC and ZPIC audits have not been material to our Company, we are unable to quantify the aggregate financial impact of these audits on our facilities given the pending appeals and uncertainty about the extent of future audits.
Quality Improvement
The Medicare program presently requires hospitals and ambulatory surgery centers to report performance data on a variety of quality metrics. Facilities that fail to report are penalized with reduced Medicare payments. Additionally, payments to hospitals are adjusted based on the hospital’s performance on these quality measures. A substantial portion of hospital payment is at risk depending on its individual performance relative to benchmarks and other hospitals’ performance. There is a substantial risk that our Medicare payments could be reduced if our hospitals fail to perform adequately on these measures. Additionally, there is a risk that Medicare payments could be reduced if our facilities-hospitals and ASCs-fail to adequate report data as required by CMS. Ambulatory surgery center payments are not yet adjusted based on performance against quality measures, but there is a substantial risk that Congress may soon link ASC Medicare payments to actual performance, in addition to reporting. The Obama administration in early 2015 announced its intent to subject even more Medicare fee-for-service payments to value-based payment program, and has proposed several specific changes that could increase the percentage of our payments at risk based on quality performance.
If the public performance data becomes a primary factor in determining where patients choose to receive care, and if competing hospitals and ASCs have better results than our facilities on those measures, we would expect that our patient volumes could decline.
Medicare and Medicaid Participation
The majority of our revenue is expected to continue to be received from third-party payors, including federal and state programs, such as Medicare and Medicaid, and commercial payors. To participate in the Medicare program and receive Medicare payment, our surgical facilities must comply with regulations promulgated by the Department of Health and Human Services (“HHS”). Among other things, these regulations, known as “conditions for coverage” or “conditions of participation,” impose numerous requirements on our facilities, their equipment, their personnel and their standards of medical care, as well as compliance with all applicable state and local laws and regulations. On April 26, 2007, CMS issued a policy memorandum that reaffirmed its prior interpretation of its conditions of participation that all hospitals (other than critical access hospitals) participating in the Medicare program are required to provide basic emergency care interventions regardless of whether or not the hospital maintains an emergency department. Our five facilities licensed as hospitals are required to meet this requirement to maintain their participating provider status in the Medicare program. As of December 31, 2015, two of our hospitals, which do not have an emergency room, maintain a protocol for the transfer of patients requiring emergency treatment, which protocol may be interpreted as inconsistent with the 2007 CMS policy memorandum. Our surgical facilities must also satisfy the conditions of participation to be eligible to participate in the various state Medicaid programs. The requirements for certification under Medicare and Medicaid are subject to change and, in order to remain qualified for these programs, we may have to make changes from time to time in our
66
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
facilities, equipment, personnel or services. Although we intend to continue to participate in these reimbursement programs, we cannot assure you that our surgical facilities will continue to qualify for participation.
The Affordable Care Act and its implementing regulations require a hospital to provide written disclosure of physician ownership interests to the hospital’s patients and on the hospital’s website and in any advertising, along with annual reports to the government detailing such interests. Additionally, hospitals that do not have 24/7 physician coverage are required to inform patients of this fact and receive signed acknowledgment from the patients of the disclosure. A hospital’s provider agreement may be terminated if it fails to provide the required notices. In 2010, CMS issued a “self-referral disclosure protocol” for hospitals and other providers that wish to self-disclose potential violations of the Stark Law to CMS and to attempt to resolve those potential violations and any related overpayment liabilities at levels below the maximum penalties and amounts set forth in the statute. The disclosure requirements set forth in the Affordable Care Act and the self-referral disclosure protocol reflect a move towards increasing government scrutiny of the financial relationships between hospitals and referring physicians and increasing disclosure of potential violations of the Stark Law to the government by hospitals and other healthcare providers. We intend for all of our facilities to meet their disclosure obligations.
Survey and Accreditation
Hospitals and healthcare facilities are subject to periodic inspection by federal, state and local authorities to determine their compliance with applicable regulations and requirements necessary for licensing, certification and accreditation. All of our hospitals and surgical facilities currently are licensed under appropriate state laws and are qualified to participate in the Medicare and Medicaid programs. Renewal and continuation of certain of these licenses, certifications and accreditations are based on inspections or other reviews generally conducted in the normal course of business of health facilities. Loss of, or limitations imposed on, licenses or accreditations could reduce a facility’s utilization or revenue, or its ability to operate all or a portion of its facilities.
Utilization Review
Federal law contains numerous provisions designed to ensure that services rendered by hospitals to Medicare and Medicaid patients meet professionally recognized standards and are medically necessary and that claims for reimbursement are properly filed. These provisions include a requirement that a sampling of admissions of Medicare and Medicaid patients must be reviewed by quality improvement organizations, which review the appropriateness of Medicare and Medicaid patient admissions and discharges, the quality of care provided, the validity of MS-DRG classifications and the appropriateness of cases of extraordinary length of stay or cost. Quality improvement organizations may deny payment for services provided or assess fines and also have the authority to recommend to HHS that a provider which is in substantial noncompliance with the standards of the quality improvement organization be excluded from participation in the Medicare program. Utilization review is also a requirement of most non-governmental managed care organizations.
Federal Anti-Kickback Statute and Medicare Fraud and Abuse Laws
The Social Security Act includes provisions addressing false statements, illegal remuneration and other instances of fraud and abuse in federal health care programs. These provisions include the statute commonly known as the federal Anti-Kickback statute (the “Anti-Kickback Statute”). The Anti-Kickback Statute prohibits providers and others from, among other things, soliciting, receiving, offering or paying, directly or indirectly, any remuneration in return for either making a referral for, or ordering or arranging for, or recommending the order of, any item or service covered by a federal healthcare program, including, but not limited to, the Medicare and Medicaid programs. Violations of the Anti-Kickback Statute are criminal offenses punishable by imprisonment and fines of up to $25,000 for each violation. Civil violations are punishable by fines of up to $50,000 for each violation, as well as damages of up to three times the total amount of remuneration received from the government for healthcare claims.
Because physician-investors in our surgical facilities are in a position to generate referrals to the facilities, the distribution of available cash to those investors could come under scrutiny under the Anti-Kickback Statute. Some courts have held that the Anti-Kickback Statute is violated if one purpose (as opposed to a primary or the sole purpose) of a payment to a provider is to induce referrals. Further, Section 6402(f)(2) of the Affordable Care Act amends the Anti-Kickback Statute by adding a provision to clarify that a person need not have actual knowledge of such section or specific intent to commit a violation of the Anti-Kickback Statute. Because none of these cases involved a joint venture such as those owning and operating our surgical facilities, it is not clear how a court would apply these holdings to our activities. It is clear, however, that a physician’s investment income from a surgical facility may not vary with the number of his or her referrals to the surgical facility, and we believe that we comply with this prohibition.
Under regulations issued by the OIG, certain categories of activities are deemed not to violate the Anti-Kickback Statute (commonly referred to as the safe harbors). According to the preamble to these safe harbor regulations, the failure of a particular business arrangement to comply with the regulations does not determine whether the arrangement violates the Anti-Kickback Statute. The safe harbor regulations do not make conduct illegal, but instead outline standards that, if complied with, protect conduct that might otherwise be deemed in violation of the Anti-Kickback Statute. Failure to meet a safe harbor does not indicate that the arrangement violates the Anti-Kickback Statute, although it may be subject to additional scrutiny.
67
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
We believe the ownership and operations of our surgery centers and hospitals do not fit wholly within any of the safe harbors, but we attempt to structure our ASCs to fit as closely as possible within the safe harbor designed to protect distributions to physician-investors in ambulatory surgery centers who directly refer patients to the ambulatory surgery center and personally perform the procedures at the center as an extension of their practice (the “ASC Safe Harbor”). The ASC Safe Harbor protects four categories of investors, including ASCs owned by (1) general surgeons, (2) single-specialty physicians, (3) multi-specialty physicians and (4) hospital/physician joint ventures, provided that certain requirements are satisfied. These requirements include the following:
• | The ASC must be an ASC certified to participate in the Medicare program, and its operating and recovery room space must be dedicated exclusively to the ASC and not a part of a hospital (although such space may be leased from a hospital if such lease meets the requirements of the safe harbor for space rental). |
• | Each investor must be either (a) a physician who derived at least one-third of his or her medical practice income for the previous fiscal year or 12-month period from performing procedures on the list of Medicare-covered procedures for ASCs, (b) a hospital, or (c) a person or entity not in a position to make or influence referrals to the center, nor to provide items or services to the ASC, nor employed by the ASC or any investor. |
• | Unless all physician-investors are members of a single specialty, each physician-investor must perform at least one-third of his or her procedures at the ASC each year. This requirement is in addition to the requirement that the physician-investor has derived at least one-third of his or her medical practice income for the past year from performing procedures. |
• | Physician-investors must have fully informed their referred patients of the physician’s investment. |
• | The terms on which an investment interest is offered to an investor are not related to the previous or expected volume of referrals, services furnished or the amount of business otherwise generated from that investor to the entity. |
• | Neither the ASC nor any other investor nor any person acting on their behalf may loan funds to or guarantee a loan for an investor if the investor uses any part of such loan to obtain the investment interest. |
• | The amount of payment to an investor in return for the investment interest is directly proportional to the amount of the capital investment (including the fair market value of any pre-operational services rendered) of that investor. |
• | All physician-investors, any hospital-investor and the center agree to treat patients receiving benefits or assistance under a federal healthcare program in a non-discriminatory manner. |
• | All ancillary services performed at the ASC for beneficiaries of federal healthcare programs must be directly and integrally related to primary procedures performed at the ASC and may not be billed separately. |
• | No hospital-investor may include on its cost report or any claim for payment from a federal healthcare program any costs associated with the ASC. |
• | The ASC may not use equipment owned by or services provided by a hospital-investor unless such equipment is leased in accordance with a lease that complies with the Anti-Kickback Statute equipment rental safe harbor and such services are provided in accordance with a contract that complies with the Anti-Kickback Statute personal services and management contract safe harbor. |
• | No hospital-investor may be in a position to make or influence referrals directly or indirectly to any other investor or the ASC. |
We believe that the ownership and operations of our surgical centers will not satisfy this ASC Safe Harbor for investment interests in ASCs because, among other things, we or one of our subsidiaries will generally be an investor in and provide management services to each ambulatory surgery center. We cannot assure you that the OIG would view our activities favorably even though we strive to achieve compliance with the remaining elements of this safe harbor.
In addition, although we expect each physician-investor to utilize the ASC as an extension of his or her practice and ask each physician-investor to certify this practice, we cannot assure you that all physician-investors will derive at least one-third of their medical practice income from performing Medicare-covered ASC procedures, perform one-third of their procedures at the ASC or inform their referred patients of their investment interests. Interests in our ASC joint ventures are purchased at what we believe to be fair market value. Investors who purchase at a later time generally pay more for a given percentage interest than founding investors. The result is that while all investors are paid distributions in accordance with their ownership interests, for ASCs where there are later purchases, we cannot meet the safe harbor requirement that return on investment is directly proportional to the amount of capital investment. The OIG has on several occasions reviewed investments relating to ASCs, and in Advisory Opinion No. 07-05, raised concerns that (a) purchases of interests from physicians might yield gains on investment rather than capital infusion to the ASCs, (b) such purchases could be meant to reward or influence the selling physicians’ referrals to the ASC or the hospital, and (c) such returns might not be directly proportional to the amount of capital invested. Nonetheless, we believe our fair market value purchase requirements and distribution policies comply with the Anti-Kickback Statute.
In OIG Advisory Opinion No. 09-09 (July 29, 2009), the OIG concluded that an arrangement involving an ASC joint venture between a hospital and physicians involving the combination of their two ASCs into a single, larger ASC presented minimal risk of fraud or abuse, despite the fact that it did not fit within any applicable Anti-Kickback safe harbors. Additionally, the OIG stated that fair market value should be determined based only on the tangible assets of each ASC since the physician investors are referral sources for the ASC. The OIG
68
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
stated that a cash flow-based valuation of the business contributed by the physician investors potentially would include the value of the physician investors’ referrals over the time that their ASC was in existence prior to the merger with the hospital’s ASC. The OIG went on to note that a valuation involving intangible assets would not necessarily result in a violation of the Anti-Kickback Statute, but would require a review of all the facts and circumstances. It is not clear whether the OIG is concerned about using a cash flow-based valuation in most healthcare transactions involving referral sources, or just transactions, similar to this one, where the parties’ contributions would be valued differently for contributing the same assets if only one party’s contribution is valued as a going concern based on cash flow. Also, the OIG appears to be focused on historical cash flow rather than a projected, discounted cash flow, which is a commonly used valuation methodology. What is clear is that for the first time, the OIG addressed valuation methodologies, which could lead to increased scrutiny of all transactions involving physicians.
Our hospital investments do not fit wholly within the safe harbor for investments in small entities because more than 40.0% of the investment interests are held by investors who are either in a position to refer to the hospital or who provide services to the hospital and more than 40.0% of the hospital’s gross revenue last year were derived from referrals generated by investors. However, we believe we comply with the remaining elements of the safe harbor.
In addition to the physician ownership in our surgical facilities, other financial relationships of ours with potential referral sources could potentially be scrutinized under the Anti-Kickback Statute. We have entered into management agreements to manage the majority of our surgical facilities. Most of these agreements call for our subsidiary to be paid a percentage-based management fee. Although there is a safe harbor for personal services and management contracts (the “Personal Services and Management Safe Harbor”), the Personal Services and Management Safe Harbor requires, among other things, that the amount of the aggregate compensation paid to the manager over the term of the agreement be set in advance. Because our management fees are generally based on a percentage of revenue, our management agreements do not typically meet this requirement. We do, however, believe that our management arrangements satisfy the other requirements of the Personal Services and Management Safe Harbor for personal services and management contracts. The OIG has taken the position in several advisory opinions that percentage-based management agreements are not protected by a safe harbor, and consequently, may violate the Anti-Kickback Statute. We have implemented formal compliance programs designed to safeguard against overbilling and believe that our management agreements comply with the requirements of the Anti-Kickback Statute. However, we cannot assure you that the OIG would find our compliance programs to be adequate or that our management agreements would be found to comply with the Anti-Kickback Statute.
Certain of our ASCs have entered into arrangements for professional services, including arrangements for anesthesia services. In a Special Advisory Bulletin issued in April 2003, the OIG focused on “questionable” contractual arrangements where a health care provider in one line of business (the “Owner”) expands into a related health care business by contracting with an existing provider of a related item or service (the “Manager/Supplier”) to provide the new item or service to the Owner’s existing patient population, including federal health care program patients (so called “suspect Contractual Joint Ventures”). The Manager/Supplier not only manages the new line of business, but may also supply it with inventory, employees, space, billing, and other services. In other words, the Owner contracts out substantially the entire operation of the related line of business to the Manager/Supplier-otherwise a potential competitor-receiving in return the profits of the business as remuneration for its referrals. Through an Advisory Opinion, the OIG extended this suspect contractual joint venture analysis to arrangements between anesthesiologists and physician owners of ASCs. In Advisory Opinion 12-06, the OIG concluded that certain proposed arrangements between anesthesia groups and physician-owned ASCs could result in prohibited remuneration under the federal Anti-Kickback Statute. We believe our arrangements for anesthesia services are distinguishable from those described in Advisory Opinion 12-06 (May 25, 2012) and are in compliance with the requirements of the federal Anti-Kickback Statute. However, we cannot assure you that regulatory authorities would agree with that position.
We also may guarantee a surgical facility’s third-party debt financing and certain lease obligations as part of our obligations under a management agreement. Physician investors are generally not required to enter into similar guarantees. The OIG might take the position that the failure of the physician investors to enter into similar guarantees represents a special benefit to the physician investors given to induce patient referrals and that such failure constitutes a violation of the Anti-Kickback Statute. We believe that the management fees (and in some cases guarantee fees) are adequate compensation to us for the credit risk associated with the guarantees and that the failure of the physician investors to enter into similar guarantees does not create a material risk of violating the Anti-Kickback Statute. However, the OIG has not issued any guidance in this regard.
The OIG is authorized to issue advisory opinions regarding the interpretation and applicability of the Anti-Kickback Statute, including whether an activity constitutes grounds for the imposition of civil or criminal sanctions. We have not, however, sought such an opinion regarding any of our arrangements. If it were determined that our activities, or those of our surgical facilities or hospitals, violate the Anti-Kickback Statute, we, our subsidiaries, our officers, our directors and each surgical facility and hospital investor could be subject, individually, to substantial monetary liability, prison sentences and/or exclusion from participation in any healthcare program funded in whole or in part by the U.S. government, including Medicare, Medicaid, TRICARE or state healthcare programs.
Evolving interpretations of current, or the adoption of new, federal or state laws or regulations could affect many of our arrangements. Law enforcement authorities, including the OIG, the courts and Congress, are increasing their scrutiny of arrangements between healthcare providers and potential referral sources to ensure that the arrangements are not designed as a mechanism to exchange remuneration for patient care referrals or opportunities. Investigators have also demonstrated a willingness to look behind the formalities of a business transaction to determine the underlying purposes of payments between healthcare providers and potential referral sources.
69
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
Federal Physician Self-Referral Law
Congress has enacted the federal physician self-referral law, or Stark Law, that prohibits certain self-referrals for healthcare services. As currently enacted, the Stark Law prohibits a practitioner, including a physician, dentist or podiatrist, from referring patients to an entity with which the practitioner or a member of his or her immediate family has a “financial relationship” for the provision of certain “designated health services” that are paid for in whole or in part by Medicare or Medicaid unless an exception applies. The term “financial relationship” is broadly defined and includes most types of ownership and compensation relationships. The Stark Law also prohibits the entity from seeking payment from Medicare or Medicaid for services that are rendered through a prohibited referral. If an entity is paid for services provided through a prohibited referral, it may be required to refund the payments. Violations of the Stark Law may also result in the imposition of damages equal to three times the amount improperly claimed and civil monetary penalties of up to $15,000 per prohibited claim and $100,000 per prohibited circumvention scheme and exclusion from participation in the Medicare and Medicaid programs. For the purposes of the Stark Law, the term “designated health services” is defined to include:
• | clinical laboratory services; |
• | physical therapy services; |
• | occupational therapy services; |
• | radiology services, including magnetic resonance imaging, computerized axial tomography scan and ultrasound services; |
• | radiation therapy services and supplies; |
• | durable medical equipment and supplies; |
• | parenteral and enteral nutrients, equipment and supplies; |
• | prosthetics, orthotics and prosthetic devices and supplies; |
• | home health services; |
• | outpatient prescription drugs; and |
• | inpatient and outpatient hospital services. |
The list of designated health services does not, however, include surgical services that are provided in an ASC. Furthermore, in final Stark Law regulations published by HHS on January 4, 2001, the term “designated health services” was specifically defined to not include services that are reimbursed by Medicare as part of a composite rate, such as services that are provided in an ASC. However, if designated health services are provided by an ASC and separately billed, referrals to the ASC by a physician-investor would be prohibited by the Stark Law. Because our facilities that are licensed as ASCs do not have independent laboratories and do not provide designated health services apart from surgical services, we do not believe referrals to these facilities by physician-investors are prohibited. If legislation or regulations are implemented that prohibit physicians from referring patients to surgical facilities in which the physician has a beneficial interest, our business and financial results would be materially adversely affected.
Five of our facilities are licensed as hospitals as of December 31, 2015. The Stark Law currently includes the Whole Hospital Exception, which applies to physician ownership of a hospital, provided such ownership is in the whole hospital and the physician is authorized to perform services at the hospital. We believe that physician investments in our facilities licensed as hospitals meet this requirement. However, changes to the Whole Hospital Exception have been the subject of recent regulatory action and legislation. Changes in the Affordable Care Act include:
• | a prohibition on hospitals from having any physician ownership unless the hospital already had physician ownership and a Medicare provider agreement in effect as of December 31, 2010; |
• | a limitation on the percentage of total physician ownership or investment interests in the hospital or entity whose assets include the hospital to the percentage of physician ownership or investment as of March 23, 2010; |
• | a prohibition from expanding the number of beds, operating rooms, and procedure rooms for which it is licensed after March 23, 2010, unless the hospital obtains an exception from the Secretary; |
• | a requirement that return on investment be proportionate to the investment by each investor; |
• | restrictions on preferential treatment of physician versus non-physician investors; |
• | a requirement for written disclosures of physician ownership interests to the hospital’s patients and on the hospital’s website and in any advertising, along with annual reports to the government detailing such interests; |
• | a prohibition on the hospital or other investors from providing financing to physician investors; |
• | a requirement that any hospital that does not have 24/7 physician coverage inform patients of this fact and receive signed acknowledgments from the patients of the disclosure; and |
• | a prohibition on “grandfathered” status for any physician owned hospital that converted from an ASC to a hospital on or after March 23, 2010. |
70
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
The Affordable Care Act also requires that each hospital with physician ownership submit an annual report of ownership and/or investment interest. Our hospitals have submitted their first reports. CMS has delayed the collection of the second report and publication of the first annual report. We cannot predict whether other proposed amendments to the Whole Hospital Exception will be included in any future legislation or if Congress will adopt any similar provisions that would prohibit or otherwise restrict physicians from holding ownership interests in hospitals. Any such changes could have an adverse effect on our financial condition and results of operations.
In addition to the physician ownership in our surgical facilities, we have other financial relationships with potential referral sources that potentially could be scrutinized under the Stark Law. We have entered into personal service agreements, such as medical director agreements, with physicians at our hospitals. We believe that our agreements with referral sources satisfy the requirements of the personal service arrangements exception to the Stark Law and have implemented formal compliance programs designed to ensure continued compliance. However, we cannot assure you that the OIG or CMS would find our compliance programs to be adequate or that our agreements with referral sources would be found to comply with the Stark Law.
False and Other Improper Claims
The U.S. government is authorized to impose criminal, civil and administrative penalties on any person or entity that files a false claim for payment from the Medicare or Medicaid programs or other federal and state healthcare programs. Claims filed with private insurers can also lead to criminal and civil penalties, including, but not limited to, penalties relating to violations of federal mail and wire fraud statutes, as well as penalties under the anti-fraud provisions of HIPAA. While the criminal statutes are generally reserved for instances of fraudulent intent, the U.S. government is applying its criminal, civil and administrative penalty statutes in an ever-expanding range of circumstances. For example, the U.S. government has taken the position that a pattern of claiming reimbursement for unnecessary services violates these statutes if the claimant merely should have known the services were unnecessary, even if the government cannot demonstrate actual knowledge. The U.S. government has also taken the position that claiming payment for low-quality services is a violation of these statutes if the claimant should have known that the care being provided was substandard.
Over the past several years, the U.S. government has investigated an increasing number of healthcare providers for potential violations of the federal False Claims Act. The federal False Claims Act prohibits a person from knowingly presenting, or causing to be presented, a false or fraudulent claim to the U.S. government. The statute defines “knowingly” to include not only actual knowledge of a claim’s falsity, but also reckless disregard for or intentional ignorance of the truth or falsity of a claim. The Fraud Enforcement and Recovery Act of 2009 further expanded the scope of the False Claims Act by, among other things, creating liability for knowingly and improperly avoiding or decreasing an obligation to pay money to the federal government. The Affordable Care Act also created federal False Claims Act liability for the knowing failure to report and return an overpayment within 60 days of the identification of the overpayment or the date by which a corresponding cost report is due, whichever is later. This requirement has led to an increasing use of the self-disclosure protocols that have been implemented by CMS, the OIG and other governmental agencies by the healthcare industry. The Affordable Care Act also provided that claims submitted in connection with patient referrals that result from violations of the Anti-Kickback Statute constitute false claims for the purposes of the federal False Claims Act, and some courts have held that a violation of the Stark Law can result in False Claims Act liability as well. Because our surgical facilities perform hundreds of similar procedures a year for which they are paid by Medicare and other government health care programs, and there is a relatively long statute of limitations, a billing error or cost reporting error could result in significant civil or criminal penalties.
Under the qui tam, or whistleblower, provisions of the False Claims Act, private parties may bring actions on behalf of the U.S. government. These private parties, often referred to as relators, are entitled to share in any amounts recovered by the government through trial or settlement. Both whistleblower lawsuits and direct enforcement activity by the government have increased significantly in recent years and have increased the risk that a healthcare company, like us, will have to defend a false claims action, pay fines or be excluded from the Medicare and Medicaid programs and other federal and state healthcare programs as a result of an investigation resulting from a whistleblower case. Although we believe that our operations materially comply with both federal and state laws, they may nevertheless be the subject of a whistleblower lawsuit or may otherwise be challenged or scrutinized by governmental authorities. Providers found liable for False Claims Act violations are subject to damages of up to three times the actual damage sustained by the government plus mandatory civil monetary penalties between $5,500 and $11,000 for each separate false claim. A determination that we have violated these laws could have a material adverse effect on us.
Other Fraud and Abuse Laws
The Medicare Patient and Program Protection Act of 1987, as amended by the Health Insurance Portability and Accountability Act of 1996, (“HIPAA”), and the Balanced Budget Act of 1997, impose civil monetary penalties and exclusion from state and federal healthcare programs on providers who commit violations of fraud and abuse laws. HIPAA authorizes the Secretary of the Department of Health & Human Services (“Secretary”), and in some cases requires the Secretary, to exclude individuals and entities that the Secretary determines have “committed an act” in violation of applicable fraud and abuse laws or improperly filed claims in violation of such laws from participating in any federal healthcare program. HIPAA also expanded the Secretary’s authority to exclude a person involved in fraudulent activity from participating in a program providing health benefits, whether directly or indirectly, in whole or in part, by the U.S. government. Additionally, under HIPAA, individuals who hold a direct or indirect ownership or controlling interest in an entity that is found to violate these laws may also be excluded from Medicare and Medicaid and other federal and state healthcare programs if the individual knew or should have known, or acted with deliberate ignorance or reckless disregard of, the truth or falsity of the information of the activity leading to the conviction or exclusion of the entity, or where the individual is an officer or managing employee of such
71
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
entity. This standard does not require that specific intent to defraud be proven by OIG. Under HIPAA it is also a crime to defraud any commercial healthcare benefit program.
Federal and State Privacy and Security Requirements
We are subject to HIPAA, including The HITECH Act, which was enacted as part of The American Recovery and Reinvestment Act of 2009. The HITECH Act strengthened the requirements and significantly increased the penalties for violations of the HIPAA privacy and security regulations. On January 25, 2013, HHS issued the HIPAA Omnibus Rule, which became effective on March 26, 2013. Prior to the HIPAA Omnibus Rule, the HITECH Act required us to notify patients of any unauthorized access, acquisition, or disclosure of their unsecured protected health information that poses significant risk of financial, reputational or other harm to a patient. The HIPAA Omnibus Rule eliminated this harm threshold standard and instead we are now required to notify patients of any unauthorized access, acquisition, or disclosure of their unsecured protected health information in all situations except those in which we can demonstrate that there is a low probability that the protected health information has been compromised. We now have the burden of demonstrating through a risk assessment that a breach of protected health information has not occurred. This new more objective standard may lead to an increased number of occurrences that require breach notifications. In addition, the HIPAA Omnibus Rule also modified the following aspects of the HIPAA privacy and security regulations:
• | makes our facilities’ business associates directly liable for compliance with certain of HIPAA’s requirements; |
• | makes our facilities liable for violations by their business associates if HHS determines an agency relationship exists between the facility and the business associate under federal agency law; |
• | adds limitations on the use and disclosure of health information for marketing and fund-raising purposes, and prohibits the sale of protected health information without individual authorization; |
• | expands our patients’ rights to receive electronic copies of their health information and to restrict disclosures to a health plan concerning treatment for which our patient has paid out of pocket in full; |
• | requires modifications to, and redistribution of, our facilities’ notice of privacy practices; |
• | requires modifications to existing agreements with business associates; |
• | adopts the additional HITECH Act provisions not previously adopted addressing enforcement of noncompliance with HIPAA due to willful neglect; |
• | incorporates the increased and tiered civil money penalty structure provided by the HITECH Act; and |
• | revises the HIPAA privacy rule to increase privacy protections for genetic information as required by the Genetic Information Nondiscrimination Act of 2008. |
The HIPAA privacy standards apply to individually identifiable information held or disclosed by a covered entity in any form, whether communicated electronically, on paper or orally. These standards impose extensive administrative requirements on us. These standards require our compliance with rules governing the use and disclosure of this health information. They create rights for patients in their health information, such as the right to amend their health information, and they require us to impose these rules, by contract, on any business associate to whom we disclose such information in order to perform functions on our behalf.
The HIPAA security standards require us to establish and maintain reasonable and appropriate administrative, technical and physical safeguards to ensure the integrity, confidentiality and the availability of electronic protected health and related financial information. Although the security standards do not reference or advocate a specific technology, and covered healthcare providers, plans and clearinghouses have the flexibility to choose their own technical solutions, the security standards have required us to implement significant new systems, business procedures and training programs.
Violations of the HIPAA privacy and security regulations may result in civil and criminal penalties. The HITECH Act strengthened the requirements of the HIPAA privacy and security regulations and significantly increased the penalties for violations by introducing a tiered penalty system, with penalties of up to $50,000 per violation with a maximum civil penalty of $1.5 million in a calendar year for violations of the same requirement. However, a single breach incident can result in violations of multiple requirements, resulting in possible penalties well in excess of $1.5 million. Under the HITECH Act, HHS is required to conduct periodic compliance audits of covered entities and their business associates. The HITECH Act and the HIPAA Omnibus Rule also extend the application of certain provisions of the security and privacy regulations to business associates and subjects business associates to civil and criminal penalties for violation of the regulations.
The HITECH Act authorizes State Attorneys General to bring civil actions seeking either an injunction or damages in response to violations of HIPAA privacy and security regulations or the new data breach law that affects the privacy of their state residents. We expect vigorous enforcement of the HITECH Act’s requirements by HHS and State Attorneys General. Additionally, HHS conducted a pilot audit program that concluded December 2012 in the first phase of HHS’ implementation of the HITECH Act’s requirements of periodic audits of covered entities and business associates to ensure their compliance with the HIPAA privacy and security regulations. HHS has allocated increased funding towards HIPAA enforcement activity and such enforcement activity has seen a marked increase over recent years. We cannot predict whether our surgical facilities will be able to comply with the final rules and the financial impact to our surgical facilities in implementing the requirements under the final rules when they take effect, or whether our hospitals will be selected for an audit, or the results of such an audit.
72
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
Our facilities also remain subject to any state laws that relate to privacy or the reporting of data breaches that are more restrictive than the regulations issued under HIPAA and the requirements of the HITECH Act. For example, various state laws and regulations may require us to notify affected individuals in the event of a data breach involving certain personal information, such as social security numbers, dates of birth and credit card information.
Adoption of Electronic Health Records
The HITECH Act includes provisions designed to increase the use of EHR by both physicians and hospitals. Beginning in 2011 and extending through 2016, eligible hospitals may receive incentive payments based upon successfully demonstrating meaningful use of its certified EHR technology. Beginning in 2015, those hospitals that do not successfully demonstrate meaningful use of EHR technology are subject to reduced payments from Medicare. EHR meaningful use objectives and measures that hospitals and physicians must meet in order to qualify for incentive payments will be implemented in three stages. Stage 1 has been in effect since 2011 and Stage 2 took effect for hospitals beginning in fiscal year 2014. On October 16, 2015, CMS published a final rule that consolidated Stage 1 and Stage 2 into a “Modified Stage 2” effective as of 2015 and set out requirements for Stage 3, which is set to take full effect in 2018. In connection with the acquisition of Symbion, we acquired six surgical facilities that are licensed as hospitals, five of which we own as of December 31, 2015. These hospitals began the implementation of EHR initiatives in 2012. We strive to comply with the EHR meaningful use requirements of the HITECH Act so as to qualify for incentive payments. Continued implementation of EHR and compliance with the HITECH Act will result in significant costs. We recorded incentive income of $1.8 million and $3.4 million which was recognized during the years ended December 31, 2015 and 2014, respectively. We incurred negligible costs for hardware, software and implementation expenses during the same periods. We do not currently know the extent of additional costs that will be associated with implementation of additional systems or the amount of future incentives that we will receive.
HIPAA Administrative Simplification Requirements
The HIPAA transaction regulations were issued to encourage electronic commerce in the healthcare industry. These regulations include standards that healthcare providers must follow when electronically transmitting certain healthcare transactions, such as healthcare claims.
Emergency Medical Treatment and Active Labor Act
Our hospitals are subject to the Emergency Medical Treatment and Active Labor Act (“EMTALA”). This federal law requires any hospital that participates in the Medicare program to conduct an appropriate medical screening examination of every person who presents to the hospital’s emergency department for treatment and, if the patient is suffering from an emergency medical condition, to either stabilize that condition or make an appropriate transfer of the patient to a facility that can handle the condition. The obligation to screen and stabilize emergency medical conditions or transfer exists regardless of a patient’s ability to pay for treatment. Off-campus facilities such as surgery centers that lack emergency departments or otherwise do not treat emergency medical conditions generally are not subject to EMTALA. They must, however, have policies in place that explain how the location should proceed in an emergency situation, such as transferring the patient to the closest hospital with an emergency department. There are severe penalties under EMTALA if a hospital fails to screen or appropriately stabilize or transfer a patient or if the hospital delays appropriate treatment in order to first inquire about the patient’s ability to pay, including civil monetary penalties and exclusion from participation in the government health care programs. In addition, an injured patient, the patient’s family or a medical facility that suffers a financial loss as a direct result of another hospital’s violation of the law can bring a civil suit against that other hospital. CMS has actively enforced EMTALA and has indicated that it will continue to do so in the future. Although we believe that our hospitals comply with EMTALA, we cannot predict whether CMS will implement new requirements in the future and, if so, whether our hospitals will comply with any new requirements.
State Regulation
Many of the states in which our surgical facilities operate have adopted statutes and/or regulations that prohibit the payment of kickbacks or any type of remuneration in exchange for patient referrals and that prohibit healthcare providers from, in certain circumstances, referring a patient to a healthcare facility in which the provider has an ownership or investment interest. While these statutes generally mirror the federal Anti-Kickback Statute and Stark Law, they vary widely in their scope and application. Some are specifically limited to healthcare services that are paid for in whole or in part by the Medicaid program; others apply to all healthcare services regardless of payor; and others apply only to state-defined designated services, which may differ from the designated health services under the Stark Law. In addition, many states have adopted statutes that mirror the False Claims Act and that prohibit the filing of a false or fraudulent claim with a state governmental agency. We intend to comply with all applicable state healthcare laws, rules and regulations. However, these laws, rules and regulations have typically been the subject of limited judicial and regulatory interpretation. As a result, we cannot assure you that our surgical facilities will not be investigated or scrutinized by the governmental authorities empowered to do so or, if challenged, that their activities would be found to be lawful. A determination of non-compliance with the applicable state healthcare laws, rules, and regulations could subject our surgical facilities to civil and criminal penalties and could have a material adverse effect on our operations.
We are also subject to various state insurance statutes and regulations that prohibit us from submitting inaccurate, incorrect or misleading claims. Many state insurance laws and regulations are broadly worded and could be implicated, for example, if our surgical facilities were to adjust an out-of-network co-payment or other patient responsibility amounts without fully disclosing the adjustment on the claim submitted to the payor. While some of our surgical facilities adjust the out-of-network costs of patient co-payment and deductible amounts to reflect in-network co-payment costs when providing services to patients whose health insurance is covered by a payor with
73
SURGERY PARTNERS, INC.
MANAGEMENT'S DISCUSSION AND ANALYSIS
which the surgical facilities are not contracted, our policy is to fully disclose adjustments in the claims submitted to the payors. We believe that our surgical facilities are in compliance with all applicable state insurance laws and regulations regarding the submission of claims. We cannot assure you, however, that none of our surgical facilities’ insurance claims will ever be challenged. If we were found to be in violation of a state’s insurance laws or regulations, we could be forced to discontinue the violative practice, which could have an adverse effect on our financial position and results of operations, and we could be subject to fines and criminal penalties.
Fee Splitting; Corporate Practice of Medicine
The laws of many states prohibit physicians from splitting fees with non-physicians (i.e., sharing in a percentage of professional fees), prohibit non-physician entities (such as us) from practicing medicine and exercising control over or employing physicians and prohibit referrals to facilities in which physicians have a financial interest. The existence, interpretation and enforcement of these laws vary significantly from state to state. In light of these restrictions, in certain states we facilitate the provision of physician services by maintaining long-term management services agreements through our subsidiaries with affiliated professional contractors, which employ or contract with physicians and other healthcare professionals to provide physician professional services. Under these arrangements, our subsidiaries perform only non-medical administrative services, do not represent that they offer medical services and do not exercise influence or control over the practice of medicine by the physicians employed by the affiliated professional contractors. Although we believe that the fees we receive from affiliated professional contractors have been structured in a manner that is compliant with applicable fee-splitting laws, it is possible that a government regulator could interpret such fee arrangements to be in violation of certain fee-splitting laws. Future interpretations of, or changes in, these laws might require structural and organizational modifications of our existing relationships, and we cannot assure you that we would be able to appropriately modify such relationships. In addition, statutes in some states could restrict our expansion into those states.
Clinical Laboratory Regulation
Our clinical laboratories are subject to federal oversight under the Clinical Laboratory Improvement Amendments of 1988 (“CLIA”) which extends federal oversight to virtually all clinical laboratories by requiring that they be certified by the federal government or by a federally-approved accreditation agency. CLIA requires that all clinical laboratories meet quality assurance, quality control and personnel standards. Laboratories also must undergo proficiency testing and are subject to inspections. Standards for testing under CLIA are based on the complexity of the tests performed by the laboratory, with tests classified as “high complexity,” “moderate complexity,” or “waived.” Laboratories performing high complexity testing are required to meet more stringent requirements than moderate complexity laboratories. Laboratories performing only waived tests, which are tests determined by the Food and Drug Administration to have a low potential for error and requiring little oversight, may apply for a certificate of waiver exempting them from most of the requirements of CLIA. Our operations also subject to state and local laboratory regulation. CLIA provides that a state may adopt laboratory regulations different from or more stringent than those under federal law, and a number of states have implemented their own laboratory regulatory requirements. State laws may require that laboratory personnel meet certain qualifications, specify certain quality controls, or require maintenance of certain records. We believe that we are in material compliance with all applicable laboratory requirements, but no assurances can be given that our laboratories will pass all future licensure or certification inspections.
Regulatory Compliance Program
It is our policy to conduct our business with integrity and in compliance with the law. We have in place and continue to enhance a company-wide compliance program that focuses on all areas of regulatory compliance including billing, reimbursement, cost reporting practices and contractual arrangements with referral sources.
This regulatory compliance program is intended to help ensure that high standards of conduct are maintained in the operation of our business and that policies and procedures are implemented so that employees act in full compliance with all applicable laws, regulations and company policies. Under the regulatory compliance program, every employee and certain contractors involved in patient care, and coding and billing, receive initial and periodic legal compliance and ethics training. In addition, we regularly monitor our ongoing compliance efforts and develop and implement policies and procedures designed to foster compliance with the law. The program also includes a mechanism for employees to report, without fear of retaliation, any suspected legal or ethical violations to their supervisors, designated compliance officers in our facilities, our compliance hotline or directly to our corporate compliance office. We believe our compliance program is consistent with standard industry practices. However, we cannot provide any assurances that our compliance program will detect all violations of law or protect against qui tam suits or government enforcement actions.
Item 7A. Quantitative and Qualitative Disclosures about Market Risk
We are subject to market risk primarily from exposure to changes in interest rates based on our financing, investing and cash management activities. We utilize a balanced mix of maturities along with both fixed rate and variable rate debt to manage our exposures to changes in interest rates, and do not hold or issue any derivative financial instruments for this purpose.
Our variable debt instruments are primarily indexed to the prime rate or LIBOR. Interest rate changes would result in gains or losses in the market value of our fixed rate debt portfolio due to differences in market interest rates and the rates at the inception of the debt agreements. At December 31, 2015, $48.5 million of our outstanding debt was in fixed rate instruments and the remaining $1.2 billion was in variable rate instruments. Assuming a hypothetical 100 basis points increase in LIBOR on our debt as of December 31, 2015, our annual interest expense would increase by approximately $6.6 million. Although there can be no assurances that interest rates will not change significantly, we do not expect changes in interest rates to have a material effect on our net earnings or cash flows in 2015.
74
Item 8. Financial Statements and Supplementary Data
Information with respect to this Item is contained in our consolidated financial statements beginning on Page F-1 of this report.
Item 9. Changes in and Disagreements With Accountants on Accounting and Financial Disclosure
None.
Item 9A. Controls and Procedures
Exemption from Management’s Report on Internal Control Over Financial Reporting
We are not currently required to comply with SEC rules that implement Sections 302 and 404 of the Sarbanes-Oxley Act, and therefore this annual report does not include a report of management’s assessment regarding internal control over financial reporting (as defined in Rule 13a-l5(f) of the Exchange Act) or an attestation report of our independent registered public accounting firm due to a transition period established by the rules of the SEC for newly public companies.
Disclosure Controls and Procedures and Limitations on the Effectiveness of Controls
Our management, with the participation of our chief executive officer and chief financial officer, evaluated the effectiveness of our disclosure controls and procedures, as such term is defined in Rules 13a-15(e) and 15d-15(e) under the Exchange Act of 1934, as amended, as of the end of the period covered by this report. Our management, including the chief executive officer and the chief financial officer, recognizes that any set of controls and procedures, no matter how well-designed and operated, can provide only reasonable, not absolute, assurance of achieving the desired control objectives. Further, the design of a control system must reflect the fact that there are resource constraints, and the benefits of controls must be considered relative to their costs. Because of the inherent limitations in all control systems, no evaluation of controls can provide absolute assurance that all control issues and instances of fraud, if any, with the Company have been detected. These inherent limitations include the realities that judgments in decision-making can be faulty and that breakdowns can occur because of simple error or mistake. Additionally, controls can be circumvented by the individual acts of some persons, by collusion of two or more people or by management override of controls. For these reasons, internal control over financial reporting may not prevent or detect misstatements. Also, projections of any evaluation of effectiveness to future periods are subject to the risk that controls may become inadequate because of changes in conditions, or that the degree of compliance with the policies or procedures may deteriorate. Based on the evaluation of our disclosure controls and procedures as of December 31, 2015, our chief executive officer and chief financial officer concluded that, as of such date, our disclosure controls and procedures were effective at the reasonable assurance level.
Changes in Internal Control over Financial Reporting
There have been no changes in our internal control over financial reporting that occurred during our most recent fiscal quarter that have materially affected, or are reasonably likely to materially affect, our internal control over financial reporting.
Item 9B. Other Information
None.
75
PART III
Item 10. Directors, Executive Officers and Corporate Governance
Information with respect to our directors, set forth in our Definitive Proxy Statement for the Annual Meeting of Shareholders to be held May 3, 2016, under the caption “Election of Directors,” is incorporated herein by reference. The information concerning our executive officers set forth in our Definitive Proxy Statement for the Annual Meeting of Shareholders to be held May 3, 2016, under the caption “Executive Officers of the Registrant,” is incorporated herein by reference.
Information with respect to compliance with Section 16(a) of the Securities Exchange Act of 1934, set forth in our Definitive Proxy Statement for the Annual Meeting of Shareholders to be held May 3, 2016, under the caption “Section 16(a) Beneficial Ownership Reporting Compliance,” is incorporated herein by reference.
Information with respect to our code of conduct, set forth in our Definitive Proxy Statement for the Annual Meeting of Shareholders to be held May 3, 2016, under the captions “Code of Conduct," is incorporated herein by reference.
Information with respect to our audit committee and audit committee financial experts, set forth in our Definitive Proxy Statement for the Annual Meeting of Shareholders to be held May 3, 2016, under the caption “Corporate Governance,” is incorporated herein by reference.
Item 11. Executive Compensation
Information required by this caption, set forth in our Definitive Proxy Statement for the Annual Meeting of Shareholders to be held May 3, 2016, under the caption “Executive Compensation,” is incorporated herein by reference.
Item 12. Security Ownership of Certain Beneficial Owners and Management and Related Stockholder Matters
Information with respect to security ownership of certain beneficial owners and management and related stockholder matters, set forth in our Definitive Proxy Statement for the Annual Meeting of Shareholders to be held May 3, 2016, under the caption “Stock Ownership” and information with respect to our equity compensation plans at December 31, 2015, set forth in our Definitive Proxy Statement for the Annual Meeting of Shareholders to be held May 3, 2016, under the caption “Equity Compensation Plan Information,” is incorporated herein by reference.
Item 13. Certain Relationships and Related Transactions, and Director Independence
Information with respect to certain relationships and related transactions, set forth in our Definitive Proxy Statement for the Annual Meeting of Shareholders to be held May 3, 2016, under the caption “Certain Relationships and Related Transactions,” is incorporated herein by reference.
Information with respect to the independence of our directors, set forth in our Definitive Proxy Statement for the Annual Meeting of Shareholders to be held May 3, 2016, under the caption “Corporate Governance,” is incorporated herein by reference.
Item 14. Principal Accounting Fees and Services
Information with respect to the fees paid to and services provided by our principal accountant, set forth in our Definitive Proxy Statement for the Annual Meeting of Shareholders to be held May 3, 2016, under the caption “Fees Billed to Us by Ernst & Young, LLP,” is incorporated herein by reference.
76
PART IV
Item 15. Exhibits and Financial Statement Schedules
(1) Financial Statements
Our Consolidated Financial Statements and Notes thereto are set forth starting on page F-1 of this Annual Report on Form 10-K.
(2) Financial Statement Schedules
All financial schedules have been omitted either because they are not applicable or because the required information is provided in our Consolidated Financial Statements and Notes thereto, starting on page F-1 of this Annual Report on Form 10-K.
(3) Exhibits
The Index to Exhibits, which appears immediately following the signature page and is incorporated herein by reference, is filed as part of this Annual Report on Form 10-K.
77
INDEX TO FINANCIAL STATEMENTS
Page | |
Report of Independent Registered Public Accounting Firm | |
Report of Independent Registered Public Accounting Firm | |
Consolidated Balance Sheets- December 31, 2015 and 2014 | |
Consolidated Statements of Operations- for the years ended December 31, 2015, 2014 and 2013 | |
Consolidated Statements of Comprehensive Income (Loss)- for the years ended December 31, 2015, 2014 and 2013 | |
Consolidated Statements of Stockholders' Equity (Deficit)- for the years ended December 31, 2015, 2014 and 2013 | |
Consolidated Statements of Cash Flows- for the years ended December 31, 2015, 2014 and 2013 | |
Notes to Consolidated Financial Statements | |
F-1
Report of Independent Registered Public Accounting Firm
The Board of Directors and Stockholders
Surgery Partners, Inc.
We have audited the accompanying consolidated balance sheets of Surgery Partners, Inc. (the “Company”) as of December 31, 2015 and 2014, and the related consolidated statements of operations, comprehensive income (loss), stockholders’ equity (deficit), and cash flows for each of the two years in the period ended December 31, 2015. These financial statements and schedule are the responsibility of the Company’s management. Our responsibility is to express an opinion on these consolidated financial statements based on our audits.
We conducted our audits in accordance with the standards of the Public Company Accounting Oversight Board (United States). Those standards require that we plan and perform the audit to obtain reasonable assurance about whether the financial statements are free of material misstatement. We were not engaged to perform an audit of the Company’s internal control over financial reporting. Our audits included consideration of internal control over financial reporting as a basis for designing audit procedures that are appropriate in the circumstances, but not for the purpose of expressing an opinion on the effectiveness of the Company’s internal control over financial reporting. Accordingly, we express no such opinion. An audit also includes examining, on a test basis, evidence supporting the amounts and disclosures in the financial statements, assessing the accounting principles used and significant estimates made by management, and evaluating the overall financial statement presentation. We believe that our audits provide a reasonable basis for our opinion.
In our opinion, the financial statements referred to above present fairly, in all material respects, the consolidated financial position of Surgery Partners, Inc. at December 31, 2015 and 2014, and the consolidated results of their operations and their cash flows for each of the two years in the period ended December 31, 2015, in conformity with U.S. generally accepted accounting principles.
As discussed in Note 2 to the consolidated financial statements, the Company changed the classification of all deferred tax assets and liabilities to noncurrent on the December 31, 2015 consolidated balance sheet as a result of the adoption of the amendments to the FASB Accounting Standards Codification resulting from Accounting Standards Update No. 2015-17, Balance Sheet Classification of Deferred Taxes.
/s/ Ernst & Young, LLP
Nashville, Tennessee
March 11, 2016
F-2
Report of Independent Registered Public Accounting Firm
Board of Directors
Surgery Partners, Inc.
Chicago, Illinois
We have audited the accompanying consolidated statements of operations and comprehensive income (loss), stockholders’ equity (deficit), and cash flows of Surgery Partners, Inc. for the year ended December 31, 2013. These financial statements are the responsibility of the Company’s management. Our responsibility is to express an opinion on these financial statements based on our audit.
We conducted our audit in accordance with the standards of the Public Company Accounting Oversight Board (United States). Those standards require that we plan and perform the audit to obtain reasonable assurance about whether the financial statements are free of material misstatement. The Company is not required to have, nor were we engaged to perform, an audit of its internal control over financial reporting. Our audit included consideration of internal control over financial reporting as a basis for designing audit procedures that are appropriate in the circumstances, but not for the purpose of expressing an opinion on the effectiveness of the Company’s internal control over financial reporting. Accordingly, we express no such opinion. An audit also includes examining, on a test basis, evidence supporting the amounts and disclosures in the financial statements, assessing the accounting principles used and significant estimates made by management, as well as evaluating the overall financial statement presentation. We believe that our audit provides a reasonable basis for our opinion.
In our opinion, the consolidated financial statements referred to above present fairly, in all material respects, the results of operations and cash flows of Surgery Partners, Inc. for the year ended December 31, 2013, in conformity with accounting principles generally accepted in the United States of America.
/s/ BDO USA, LLP
Chicago, Illinois
April 22, 2014, except for the effect of the reorganization, discussed in Note 1, on the 2013 financial statements, as to which the date is March 11, 2016 and except for 2013 segment reporting data disclosure within Note 15, as to which the date is August 17, 2015.
F-3
SURGERY PARTNERS, INC.
CONSOLIDATED BALANCE SHEETS
(In thousands, except shares and per share amounts)
December 31, 2015 | December 31, 2014 | |||||||
ASSETS | ||||||||
Current assets: | ||||||||
Cash and cash equivalents | $ | 57,933 | $ | 74,920 | ||||
Accounts receivable, less allowance for doubtful accounts of $18,322 and $5,329, respectively | 177,757 | 144,960 | ||||||
Inventories | 25,591 | 23,692 | ||||||
Prepaid expenses and other current assets | 34,620 | 24,005 | ||||||
Acquisition escrow deposit | 13,984 | — | ||||||
Indemnification receivable due from seller | 1,072 | 1,072 | ||||||
Total current assets | 310,957 | 268,649 | ||||||
Property and equipment, net | 184,550 | 175,006 | ||||||
Intangible assets, net | 53,568 | 54,888 | ||||||
Goodwill | 1,407,927 | 1,298,753 | ||||||
Investments in and advances to affiliates | 34,103 | 33,441 | ||||||
Restricted invested assets | 316 | 316 | ||||||
Long-term deferred tax assets | 94,105 | — | ||||||
Acquisition escrow deposit | 8,408 | 16,232 | ||||||
Debt issuance costs | 4,246 | 5,630 | ||||||
Other long-term assets | 8,504 | 5,879 | ||||||
Total assets | $ | 2,106,684 | $ | 1,858,794 | ||||
LIABILITIES AND STOCKHOLDERS' EQUITY | ||||||||
Current liabilities: | ||||||||
Accounts payable | $ | 45,341 | $ | 43,063 | ||||
Accrued payroll and benefits | 26,307 | 22,370 | ||||||
Acquisition escrow liability | 13,984 | — | ||||||
Other current liabilities | 68,410 | 53,870 | ||||||
Current maturities of long-term debt | 27,272 | 22,088 | ||||||
Total current liabilities | 181,314 | 141,391 | ||||||
Long-term debt, less current maturities | 1,230,328 | 1,339,266 | ||||||
Long-term tax receivable agreement liability | 119,655 | — | ||||||
Long-term deferred tax liabilities | — | 49,170 | ||||||
Acquisition escrow liability | 8,408 | 16,232 | ||||||
Other long-term liabilities | 85,613 | 90,610 | ||||||
Non-controlling interests—redeemable | 183,439 | 192,589 | ||||||
Stockholders' equity: | ||||||||
Preferred stock, $0.01 par value, 20,000,000 shares authorized, no shares issued at December 31, 2015; no shares authorized, issued or outstanding at December 31, 2014 (1) | — | — | ||||||
Common stock, $0.01 par value, 300,000,000 shares authorized, 48,156,990 shares issued and outstanding at December 31, 2015; 1,000 shares authorized, issued and outstanding at December 31, 2014 (1) | 482 | — | ||||||
Additional paid-in capital | 316,294 | 58,151 | ||||||
Retained deficit | (320,804 | ) | (322,233 | ) | ||||
Total Surgery Partners, Inc. stockholders' deficit | (4,028 | ) | (264,082 | ) | ||||
Non-controlling interests—non-redeemable | 301,955 | 293,618 | ||||||
Total stockholders' equity | 297,927 | 29,536 | ||||||
Total liabilities and stockholders' equity | $ | 2,106,684 | $ | 1,858,794 | ||||
(1) As described in Note 1 herein, the authorized, issued and outstanding shares of the Company are those of Surgery Partners, Inc. as of December 31, 2015, and those of Surgery Center Holdings, Inc. as of December 31, 2014.
See notes to consolidated financial statements.
F-4
SURGERY PARTNERS, INC.
CONSOLIDATED STATEMENTS OF OPERATIONS
(In thousands, except shares and per share amounts)
Year Ended December 31, | ||||||||||||
2015 | 2014 | 2013 | ||||||||||
Revenues | $ | 959,891 | $ | 403,289 | $ | 284,599 | ||||||
Operating expenses: | ||||||||||||
Salaries and benefits | 261,685 | 101,976 | 70,923 | |||||||||
Supplies | 242,083 | 94,224 | 63,726 | |||||||||
Professional and medical fees | 66,583 | 18,028 | 7,372 | |||||||||
Lease expense | 44,848 | 19,389 | 14,048 | |||||||||
Other operating expenses | 54,127 | 20,561 | 13,775 | |||||||||
Cost of revenues | 669,326 | 254,178 | 169,844 | |||||||||
General and administrative expenses | 55,992 | 31,452 | 26,339 | |||||||||
Depreciation and amortization | 34,545 | 15,061 | 11,663 | |||||||||
Provision for doubtful accounts | 23,578 | 9,509 | 5,885 | |||||||||
Income from equity investments | (3,777 | ) | (1,264 | ) | — | |||||||
(Gain) loss on disposal or impairment of long-lived assets, net | (2,097 | ) | 1,804 | 2,482 | ||||||||
Loss on debt extinguishment | 16,102 | 23,414 | 9,863 | |||||||||
Merger transaction and integration costs | 17,920 | 21,690 | — | |||||||||
Termination of management agreement and IPO costs | 5,834 | — | — | |||||||||
Electronic health records incentive income | (1,761 | ) | (3,356 | ) | — | |||||||
Other (income) expenses | (525 | ) | (6 | ) | 297 | |||||||
Total operating expenses | 815,137 | 352,482 | 226,373 | |||||||||
Operating income | 144,754 | 50,807 | 58,226 | |||||||||
Tax receivable agreement expense | (119,911 | ) | — | — | ||||||||
Interest expense, net | (100,980 | ) | (62,101 | ) | (32,929 | ) | ||||||
(Loss) income before income taxes | (76,137 | ) | (11,294 | ) | 25,297 | |||||||
Income tax (benefit) expense | (148,982 | ) | 15,758 | 7,570 | ||||||||
Net income (loss) | 72,845 | (27,052 | ) | 17,727 | ||||||||
Less: Net income attributable to non-controlling interests | (71,416 | ) | (38,845 | ) | (26,789 | ) | ||||||
Net income (loss) attributable to Surgery Partners, Inc. | $ | 1,429 | $ | (65,897 | ) | $ | (9,062 | ) | ||||
Net income (loss) per share attributable to common stockholders | ||||||||||||
Basic | $ | 0.04 | $ | (2.04 | ) | $ | (0.28 | ) | ||||
Diluted (1) | $ | 0.04 | $ | (2.04 | ) | $ | (0.28 | ) | ||||
Weighted average common shares outstanding (2) | ||||||||||||
Basic | 36,066,233 | 32,295,364 | 31,815,520 | |||||||||
Diluted (1) | 37,464,387 | 32,295,364 | 31,815,520 | |||||||||
(1) The impact of potentially dilutive securities for the years ended December 31, 2014 and 2013 was not considered because the effect would be anti-dilutive in each of those periods.
(2) Effect of the Reorganization, as defined in Note 1, has been retrospectively applied to all periods presented.
See notes to consolidated financial statements.
F-5
SURGERY PARTNERS, INC.
CONSOLIDATED STATEMENTS OF COMPREHENSIVE INCOME (LOSS)
(In thousands)
Year Ended December 31, | ||||||||||||
2015 | 2014 | 2013 | ||||||||||
Net income (loss) | $ | 72,845 | $ | (27,052 | ) | $ | 17,727 | |||||
Other comprehensive income | — | — | — | |||||||||
Comprehensive income (loss) | $ | 72,845 | $ | (27,052 | ) | $ | 17,727 | |||||
Less: Comprehensive income attributable to non-controlling interests | (71,416 | ) | (38,845 | ) | (26,789 | ) | ||||||
Comprehensive income (loss) attributable to Surgery Partners, Inc. | $ | 1,429 | $ | (65,897 | ) | $ | (9,062 | ) | ||||
See notes to consolidated financial statements.
F-6
SURGERY PARTNERS, INC.
CONSOLIDATED STATEMENTS OF STOCKHOLDERS' EQUITY (DEFICIT)
(In thousands, except shares)
Common Stock (1) | Additional Paid-in Capital | Retained Deficit | Non-Controlling Interests— Non-Redeemable | Total | ||||||||||||||||||
Shares | Amount | |||||||||||||||||||||
Balance as of December 31, 2012 | 1,000 | $ | — | $ | 59,061 | $ | (23,261 | ) | $ | 88,305 | $ | 124,105 | ||||||||||
Net (loss) income | — | — | — | (9,062 | ) | 26,789 | 17,727 | |||||||||||||||
Equity-based compensation | — | — | 455 | — | — | 455 | ||||||||||||||||
Acquisition and disposal of shares of non-controlling interests, net | — | — | 203 | — | (599 | ) | (396 | ) | ||||||||||||||
Distributions to owners | — | — | (131,013 | ) | — | (131,013 | ) | |||||||||||||||
Distributions to non-controlling interest—non-redeemable holders | — | — | — | — | (25,253 | ) | (25,253 | ) | ||||||||||||||
Balance as of December 31, 2013 | 1,000 | $ | — | $ | 59,719 | $ | (163,336 | ) | $ | 89,242 | $ | (14,375 | ) | |||||||||
Net (loss) income | — | — | — | (65,897 | ) | 34,766 | (31,131 | ) | ||||||||||||||
Equity-based compensation | — | — | 942 | — | — | 942 | ||||||||||||||||
Acquisition and disposal of shares of non-controlling interests, net | — | — | 633 | — | 202,024 | 202,657 | ||||||||||||||||
Distributions to owners | — | — | — | (93,000 | ) | — | (93,000 | ) | ||||||||||||||
Distributions to non-controlling interests—non-redeemable holders | — | — | — | — | (32,414 | ) | (32,414 | ) | ||||||||||||||
Repurchase of units | — | — | (3,143 | ) | — | — | (3,143 | ) | ||||||||||||||
Balance as of December 31, 2014 | 1,000 | $ | — | $ | 58,151 | $ | (322,233 | ) | $ | 293,618 | $ | 29,536 | ||||||||||
Net income | — | — | — | 1,429 | 53,800 | 55,229 | ||||||||||||||||
Equity-based compensation | — | — | 7,502 | — | — | 7,502 | ||||||||||||||||
Acquisition and disposal of shares of non-controlling interests, net | — | — | (835 | ) | — | 4,321 | 3,486 | |||||||||||||||
Distributions to non-controlling interests—non-redeemable holders | — | — | — | — | (49,784 | ) | (49,784 | ) | ||||||||||||||
Initial public offering | 14,285,000 | 143 | 250,836 | 250,979 | ||||||||||||||||||
Effect of Reorganization (2) | 33,870,990 | 339 | — | — | — | 339 | ||||||||||||||||
Other | 640 | 640 | ||||||||||||||||||||
Balance as of December 31, 2015 | 48,156,990 | $ | 482 | $ | 316,294 | $ | (320,804 | ) | $ | 301,955 | $ | 297,927 | ||||||||||
(1) As described in Note 1 herein, the common stock of the Company is that of Surgery Partners, Inc. as of December 31, 2015 and that of Surgery Center Holdings,
Inc. as of December 31, 2014 and 2013.
(2) As a result of the Reorganization that occurred on September 30, 2015 (as further described in Note 1), Surgery Center Holdings, Inc, became an indirect wholly
owned subsidiary of Surgery Partners, Inc. and the common stock of Surgery Center Holdings, Inc. is eliminated in consolidation.
See notes to consolidated financial statements.
F-7
SURGERY PARTNERS, INC.
CONSOLIDATED STATEMENTS OF CASH FLOWS
(In thousands)
Year Ended December 31, | ||||||||||||
2015 | 2014 | 2013 | ||||||||||
Cash flows from operating activities: | ||||||||||||
Net income | $ | 72,845 | $ | (27,052 | ) | $ | 17,727 | |||||
Adjustments to reconcile net income to net cash provided by operating activities: | ||||||||||||
Depreciation and amortization | 34,545 | 15,061 | 11,663 | |||||||||
Amortization of debt issuance costs and discounts | 6,263 | 3,746 | 2,430 | |||||||||
Goodwill impairment | — | — | 581 | |||||||||
Amortization of unfavorable lease liability | (431 | ) | (72 | ) | — | |||||||
Equity-based compensation | 7,502 | 942 | 455 | |||||||||
(Gain) loss on disposal or impairment of long-lived assets, net | (2,097 | ) | 1,804 | 2,482 | ||||||||
Loss on debt extinguishment | 16,102 | 23,414 | 9,863 | |||||||||
Tax receivable agreement expense | 119,911 | — | — | |||||||||
Deferred income taxes | (149,891 | ) | 14,089 | 7,136 | ||||||||
Interest on contingent consideration obligation | 1,041 | 964 | 892 | |||||||||
Provision for doubtful accounts | 23,578 | 9,509 | 5,885 | |||||||||
Income from equity investments, net of distributions received | (543 | ) | (713 | ) | — | |||||||
Changes in operating assets and liabilities, net of acquisitions and divestitures: | ||||||||||||
Accounts receivable | (48,783 | ) | (20,161 | ) | (9,722 | ) | ||||||
Other operating assets and liabilities | 4,439 | 418 | (314 | ) | ||||||||
Net cash provided by operating activities | 84,481 | 21,949 | 49,078 | |||||||||
Cash flows from investing activities: | ||||||||||||
Purchases of property and equipment, net | (33,439 | ) | (7,736 | ) | (4,150 | ) | ||||||
Payments for acquisitions, net of cash acquired | (112,596 | ) | (263,280 | ) | (486 | ) | ||||||
Proceeds from divestitures | 11,193 | — | 1,014 | |||||||||
Net cash used in investing activities | (134,842 | ) | (271,016 | ) | (3,622 | ) | ||||||
Cash flows from financing activities: | ||||||||||||
Proceeds from initial public offering, net of offering costs | 250,979 | — | — | |||||||||
Principal payments on long-term debt | (328,329 | ) | (1,009,874 | ) | (339,908 | ) | ||||||
Borrowings of long-term debt | 196,366 | 1,477,288 | 462,983 | |||||||||
Payments of debt issuance costs | — | (7,496 | ) | (4,974 | ) | |||||||
Penalty on prepayment of debt | (7,305 | ) | — | — | ||||||||
Payment of premium of debt extinguishment | — | (17,840 | ) | — | ||||||||
Distributions to non-controlling interest holders | (69,720 | ) | (35,182 | ) | (25,253 | ) | ||||||
Distribution to owners | — | (93,000 | ) | (131,013 | ) | |||||||
Payments related to ownership transactions with consolidated affiliates | (12,175 | ) | 278 | 503 | ||||||||
Repurchase of units | — | (3,143 | ) | — | ||||||||
Financing lease obligation | 3,558 | (70 | ) | — | ||||||||
Net cash provided by (used in) financing activities | 33,374 | 310,961 | (37,662 | ) | ||||||||
Net (decrease) increase in cash and cash equivalents | (16,987 | ) | 61,894 | 7,794 | ||||||||
Cash and cash equivalents at beginning of period | 74,920 | 13,026 | 5,232 | |||||||||
Cash and cash equivalents at end of period | $ | 57,933 | $ | 74,920 | $ | 13,026 | ||||||
Supplemental cash flow information: | ||||||||||||
Non-cash transactions: | ||||||||||||
Notes payable issued in connection with an acquisition | $ | 7,430 | $ | — | $ | — | ||||||
Increase in debt related to new capital lease obligations | 5,443 | 3,252 | 1,054 | |||||||||
Cash payments: | ||||||||||||
Interest paid, net of interest income received | 96,799 | 50,377 | 31,101 | |||||||||
Cash paid for income taxes | 1,093 | 676 | 538 | |||||||||
See notes to consolidated financial statements.
F-8
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
1. Organization
Surgery Partners, Inc., a Delaware corporation (together with its subsidiaries, the “Company”), was formed April 2, 2015, as a holding company for the purpose of facilitating an initial public offering (the “IPO”) of shares of common stock. Prior to September 30, 2015, the Company conducted business through Surgery Center Holdings, Inc. and its subsidiaries. Surgery Center Holdings, LLC was and is the sole direct owner of the equity interests of Surgery Center Holdings, Inc. and had no other material assets.
On September 30, 2015, Surgery Partners, Inc. became the direct parent and sole member of Surgery Center Holdings, LLC (the "Reorganization"). In the Reorganization, all of the equity interests held by the pre-IPO Owners of Surgery Center Holdings, LLC were contributed to Surgery Partners, Inc. in exchange for 33,871,990 shares of common stock of Surgery Partners, Inc. and certain rights to additional payments under a tax receivable agreement. After giving effect to the Reorganization, Surgery Partners, Inc. is a holding company, and its sole material asset is an equity interest in Surgery Center Holdings, LLC. The Company's consolidated financial statements for periods prior to the Reorganization represent the historical operating results and financial position of Surgery Center Holdings, Inc. and certain of its subsidiaries.
On October 1, 2015, the Company completed its IPO of 14,285,000 shares of common stock at an offering price of $19.00 per share. On October 6, 2015, the Company received net proceeds from the sale of common stock in this offering of $255.8 million, after deducting underwriting discounts and other fees of $15.6 million. These net proceeds were used to repay a portion of the borrowings outstanding under the 2014 Second Lien and to pay fees associated with this offering. The Company also incurred an additional $4.8 million in costs directly related to the IPO.
On November 3, 2014, the Company completed the acquisition of Symbion Holdings Corp. ("Symbion") ("the Merger"), which added 55 surgical facilities, including 49 ambulatory surgery centers ("ASCs") and six surgical hospitals, to its network of existing facilities. The Company acquired Symbion for a purchase price of $792.0 million pursuant to the terms of an Agreement and Plan of Merger dated as of June 13, 2014. The Symbion acquisition was financed through the issuance of approximately $1.4 billion under the Company's Term Loans and Revolving Facility.
As of December 31, 2015, the Company owned and operated a national network of surgical facilities and ancillary services in 29 states. The surgical facilities, which include ASCs and surgical hospitals, primarily provide non-emergency surgical procedures across many specialties, including, among others, otolaryngology ("ENT"), gastroenterology ("GI"), general surgery, ophthalmology, orthopedics, cardiology and pain management. The Company's surgical hospitals provide services such as diagnostic imaging, laboratory, obstetrics, oncology, pharmacy, physical therapy and wound care. Ancillary services are comprised of a diagnostic laboratory, multi-specialty physician practices, urgent care facilities, anesthesia services, optical services and specialty pharmacy services.
As of December 31, 2015, the Company owned or operated a portfolio of 101 surgical facilities, comprised of 96 ASCs and five surgical hospitals. The Company owns these facilities in partnership with physicians and, in some cases, healthcare systems in the markets and communities it serves. The Company owned a majority interest in 72 of the surgical facilities and consolidated 90 of these facilities for financial reporting purposes. In addition, the Company owned or operated a network of 46 physician practices.
2. Significant Accounting Policies
Principles of Consolidation
The consolidated financial statements include the accounts of the Company and its wholly-owned subsidiaries, as well as interests in partnerships and limited liability companies controlled by the Company through its ownership of a majority voting interest or other rights granted to the Company by contract to manage and control the affiliate's business. All significant intercompany balances and transactions are eliminated in consolidation.
Non-Controlling Interests
The physician limited partners and physician minority members of the entities that the Company controls are responsible for the supervision and delivery of medical services. The governance rights of limited partners and minority members are restricted to those that protect their financial interests. Under certain partnership and operating agreements governing these partnerships and limited liability companies, the Company could be removed as the sole general partner or managing member for certain events such as material breach of the partnership or operating agreement, gross negligence or bankruptcy. These protective rights do not preclude consolidation of the respective partnerships and limited liability companies.
Ownership interests in consolidated subsidiaries held by parties other than the Company are identified and generally presented in the consolidated financial statements within the equity section but separate from the Company's equity. However, in instances in which certain redemption features that are not solely within the control of the Company are present, classification of non-controlling interests outside of permanent equity is required. Consolidated net income attributable to the Company and to the non-controlling interests are identified and presented on the consolidated statements of operations; changes in ownership interests are accounted for as equity transactions assuming the Company continues to consolidate related entities. Certain transactions with non-controlling interests are classified within financing activities in the consolidated statements of cash flows.
F-9
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
The consolidated financial statements of the Company include all assets, liabilities, revenues and expenses of surgical facilities in which the Company has sufficient ownership and rights to allow the Company to consolidate the surgical facilities. Similar to its investments in non-consolidated affiliates, the Company regularly engages in the purchase and sale of ownership interests with respect to its consolidated subsidiaries that do not result in a change of control.
Non-Controlling Interests — Redeemable. Each of the partnerships and limited liability companies through which the Company owns and operates its surgical facilities is governed by a partnership or operating agreement. In certain circumstances, the partnership and operating agreements for the Company's surgical facilities provide that the facilities will purchase all of the physicians’ ownership if certain adverse regulatory events occur, such as it becoming illegal for the physicians to own an interest in a surgical facility, refer patients to a surgical facility or receive cash distributions from a surgical facility. The non-controlling interests - redeemable are reported outside of stockholders' equity in the consolidated balance sheets.
A summary of activity related to the non-controlling interests—redeemable follows (in thousands):
Balance at December 31, 2013 | $ | — | ||
Net income attributable to non-controlling interests—redeemable | 4,079 | |||
Acquisition and disposal of shares of non-controlling interests, net—redeemable | 191,278 | |||
Distributions to non-controlling interest —redeemable holders | (2,768 | ) | ||
Balance at December 31, 2014 | 192,589 | |||
Net income attributable to non-controlling interests—redeemable | 17,616 | |||
Acquisition and disposal of shares of non-controlling interests, net—redeemable | (6,830 | ) | ||
Distributions to non-controlling interest —redeemable holders | (19,936 | ) | ||
Balance at December 31, 2015 | $ | 183,439 | ||
Variable Interest Entities
The consolidated financial statements include the accounts of variable interest entities in which the Company is the primary beneficiary under the provisions of Accounting Standards Codification ("ASC") Topic 810, Consolidation. At December 31, 2015, the variable interest entities include five surgical facilities, three anesthesia practices and one physician practice. At December 31, 2014, the variable interest entities included an additional surgical facility which was disposed of during the three months ended March 31, 2015 and an additional anesthesia practice which no longer met variable interest entity classification in July 2015. There were an additional four acquisitions at December 31, 2015. The Company has the power to direct the activities that most significantly impact the variable interest entity's economic performance. Additionally, the Company would absorb the majority of the expected losses of these entities should they occur. As of December 31, 2015 and December 31, 2014, the consolidated balance sheets of the Company included total assets of $104.2 million and $24.7 million, respectively, and total liabilities of $13.2 million and $1.7 million, respectively, related to the Company's variable interest entities.
Equity Method Investments
The Company has non-consolidating investments in surgical facilities and management companies that own or manage surgical facilities. These investments are accounted for using the equity method of accounting. The total amount of these investments included in investments in and advances to affiliates in the consolidated balance sheets was $34.1 million and $33.4 million as of December 31, 2015 and December 31, 2014, respectively.
Use of Estimates
The consolidated financial statements have been prepared in accordance with U.S. generally accepted accounting principles ("GAAP"). The preparation of financial statements in conformity with GAAP requires management to make estimates and assumptions that affect the amounts reported in the consolidated financial statements and footnotes. Examples include, but are not limited to, estimates of accounts receivable allowances, professional and general liabilities and the estimate of deferred tax assets or liabilities. In the opinion of management, all adjustments considered necessary for a fair presentation have been included. All adjustments are of a normal, recurring nature. Actual results could differ from those estimates.
Reclassifications
Certain reclassifications have been made to the comparative periods' financial statements to conform to the current year presentation. The reclassifications primarily related to the presentation of certain expenses within costs of revenue and had no impact on the Company's consolidated financial position, results of operations or cash flows.
Fair Value of Financial Instruments
The fair value of a financial instrument is the amount at which the instrument could be exchanged in an orderly transaction between market participants to sell the asset or transfer the liability. The Company uses fair value measurements based on quoted prices in active
F-10
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
markets for identical assets or liabilities (Level 1), inputs other than quoted prices in active markets that are either directly or indirectly observable (Level 2), or unobservable inputs in which little or no market data exists, therefore requiring an entity to develop its own assumptions (Level 3), depending on the nature of the item being valued.
The carrying amounts reported in the consolidated balance sheets for cash and cash equivalents, accounts receivable, restricted invested assets and accounts payable approximate their fair values.
A summary of the carrying amounts and fair values of the Company's long-term debt follows (in thousands):
Carrying Amount | Fair Value | |||||||||||||||
December 31, 2015 | December 31, 2014 | December 31, 2015 | December 31, 2014 | |||||||||||||
2014 First Lien Credit Agreement, net of debt issuance and discount of $20,223 and $23,818 at December 31, 2015 and 2014, respectively | $ | 841,078 | $ | 846,183 | $ | 828,816 | $ | 820,798 | ||||||||
2014 Second Lien Credit Agreement, net of debt issuance and discount of $8,159 and $18,184 at December 31, 2015 and 2014, respectively | $ | 238,341 | $ | 471,816 | $ | 225,382 | $ | 452,943 | ||||||||
The fair values of the 2014 First Lien Credit Agreement and 2014 Second Lien Credit Agreement, as defined in Note 5 on Long-Term Debt, were based on a Level 2 computation using quoted prices for identical liabilities in inactive markets at December 31, 2015 and 2014, as applicable. The carrying amounts related to the Company's other long-term debt obligations approximate their fair values.
The Company maintains a supplemental executive retirement savings plan (the "SERP") for certain former Symbion executive officers. The SERP is a non-qualified deferred compensation plan for eligible executive officers and other key employees of the Company that allows participants to defer portions of their compensation. The fair value of the SERP asset and liability was based on a quoted market price, or a Level 1 computation. As of December 31, 2015 and 2014, the fair value of the assets in the SERP were $1.6 million and $1.4 million, respectively, and were included in other long-term assets in the consolidated balance sheets. The Company had a liability related to the SERP of $1.6 million and $1.4 million as of December 31, 2015 and 2014, respectively, which was included in other long-term liabilities in the consolidated balance sheets.
Revenues
The Company recognizes revenues in the period in which the services are performed. Patient service revenues and receivables from third-party payors are recorded net of estimated contractual adjustments and allowances, which the Company estimates based on the historical trend of its cash collections and contractual write-offs, accounts receivable agings, established fee schedules, contracts with payors and procedure statistics.
A summary of revenues by service type as a percentage of total revenues follows:
Year Ended December 31, | |||||||||
2015 | 2014 | 2013 | |||||||
Patient service revenues: | |||||||||
Surgical facilities revenues | 91.6 | % | 83.9 | % | 78.9 | % | |||
Ancillary services revenues | 6.4 | % | 12.3 | % | 15.5 | % | |||
98.0 | % | 96.2 | % | 94.4 | % | ||||
Other service revenues: | |||||||||
Optical services revenues | 1.5 | % | 3.5 | % | 5.6 | % | |||
Other | 0.5 | % | 0.3 | % | — | % | |||
2.0 | % | 3.8 | % | 5.6 | % | ||||
Total revenues | 100.0 | % | 100.0 | % | 100.0 | % | |||
Patient service revenues. The fee charged for healthcare procedures performed in surgical facilities varies depending on the type of service provided, but usually includes all charges for usage of an operating room, a recovery room, special equipment, medical supplies, nursing staff and medications. The fee does not normally include professional fees charged by the patient’s surgeon, anesthesiologist or other attending physician, which are billed directly by such physicians to the patient or third-party payor. However, in several surgical facilities, the Company charges for anesthesia services. Ancillary service revenues include fees for patient visits to the Company's physician practices, pharmacy services and diagnostic tests ordered by physicians. Patient service revenues are recognized on the date of service, net of estimated contractual adjustments and discounts from third-party payors, including Medicare and Medicaid. Changes in
F-11
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
estimated contractual adjustments and discounts are recorded in the period of change. During the year ended December 31, 2015, the Company recognized an increase to patient service revenues as a result of changes in estimates to third-party settlements related to prior years of approximately $2.3 million compared to a reduction to patient service revenues of $104,000 during the year ended December 31, 2014. These adjustments were related to two of the Company's surgical hospitals that were acquired in connection with the acquisition of Symbion on November 3, 2014.
The following table sets forth patient service revenues by type of payor and as a percentage of total patient service revenues for the Company's consolidated surgical facilities (dollars in thousands):
Year Ended December 31, | |||||||||||||||||||||
2015 | 2014 | 2013 | |||||||||||||||||||
Amount | % | Amount | % | Amount | % | ||||||||||||||||
Patient service revenues: | |||||||||||||||||||||
Private insurance | $ | 516,739 | 55.0 | % | $ | 202,172 | 52.1 | % | $ | 162,888 | 60.6 | % | |||||||||
Government | 359,471 | 38.2 | % | 134,041 | 34.5 | % | 75,125 | 28.0 | % | ||||||||||||
Self-pay | 16,190 | 1.7 | % | 13,645 | 3.5 | % | 7,587 | 2.8 | % | ||||||||||||
Other | 48,311 | 5.1 | % | 38,215 | 9.9 | % | 23,081 | 8.6 | % | ||||||||||||
Total patient service revenues | $ | 940,711 | 100.0 | % | $ | 388,073 | 100.0 | % | $ | 268,681 | 100.0 | % | |||||||||
Other service revenues: | |||||||||||||||||||||
Optical service revenues | $ | 14,572 | $ | 14,193 | $ | 15,918 | |||||||||||||||
Other revenues | 4,608 | 1,023 | — | ||||||||||||||||||
Total net revenues | $ | 959,891 | $ | 403,289 | $ | 284,599 | |||||||||||||||
Other service revenues. Optical service revenues consist of product sales from the Company's optical laboratories as well as handling charges billed to the members of the Company's optical products purchasing organization and sales from the Company's marketing products and services business. The Company's optical products purchasing organization negotiates volume buying discounts with optical products manufacturers. The buying discounts and any handling charges billed to the members of the buying group represent the revenue recognized for financial reporting purposes. Revenue is recognized as orders are shipped to members. The Company bases its estimates for sales returns and discounts on historical experience and has not experienced significant fluctuations between estimated and actual return activity and discounts given. The Company's optical laboratories manufacture and distribute corrective lenses and eyeglasses to ophthalmologists and optometrists. Revenue is recognized when product is shipped, net of allowance for discounts. The Company's marketing products and services businesses recognize revenue when product is shipped or services are rendered.
Other revenues include management and administrative service fees derived from the non-consolidated facilities that the Company accounts for under the equity method, management of surgical facilities in which it does not own an interest, and management services provided to physician practices for which the Company is not required to provide capital or additional assets. The fees derived from these management arrangements are based on a predetermined percentage of the revenues of each facility or practice and are recognized in the period in which services are rendered.
Cash and Cash Equivalents
The Company considers all highly liquid investments with a maturity of three months or less when purchased to be cash equivalents. The Company maintains its cash and cash equivalent balances at high credit quality financial institutions.
Accounts Receivable and Allowances for Contractual Adjustments and Doubtful Accounts
Accounts receivable are recorded net of contractual adjustments and allowances for doubtful accounts to reflect accounts receivable at net realizable value. Accounts receivable consists of receivables from federal and state agencies (under the Medicare and Medicaid programs), managed care health plans, commercial insurance companies, employers and patients. Management recognizes that revenues and receivables from government agencies are significant to the Company's operations, but it does not believe that there is significant credit risk associated with these government agencies. Concentration of credit risk with respect to other payors is limited because of the large number of such payors. As of December 31, 2015 and 2014, the Company had third-party Medicaid settlements of $5.2 million and $11.7 million, respectively, in other current liabilities in the consolidated balance sheets.
The Company recognizes that final reimbursement of accounts receivable is subject to final approval by each third-party payor. However, because the Company has contracts with its third-party payors and also verifies insurance coverage of the patient before medical services are rendered, the amounts that are pending approval from third-party payors are not significant. The Company's policy is to collect co-payments and deductibles prior to providing medical services. It is also the Company's policy to verify a patient’s insurance 72 hours prior to the patient’s procedure. Patient services of the Company are primarily non-emergency, which allows the surgical facilities to control the procedures for which third-party reimbursement is sought and obtained. The Company does not require collateral from self-pay patients.
F-12
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
The Company analyzes accounts receivable at each of its facilities to ensure the proper aged category and collection assessment. At a consolidated level, the Company's policy is to review accounts receivable aging, by facility, to determine the appropriate allowance for doubtful accounts. Patient account balances are reviewed for delinquency based on contractual terms. This review is supported by an analysis of the actual revenues, contractual adjustments and cash collections received. An account balance is written off only after the Company has pursued collection with legal or collection agency assistance or otherwise has deemed an account to be uncollectible.
A summary of the changes in the allowance for doubtful accounts receivable follows (in thousands):
Balance at December 31, 2012 | $ | 3,234 | ||
Provision for doubtful accounts | 5,885 | |||
Accounts written off, net of recoveries | (4,091 | ) | ||
Balance at December 31, 2013 | 5,028 | |||
Provision for doubtful accounts | 9,509 | |||
Accounts written off, net of recoveries | (9,208 | ) | ||
Balance at December 31, 2014 | 5,329 | |||
Provision for doubtful accounts | 23,578 | |||
Accounts written off, net of recoveries | (10,585 | ) | ||
Balance at December 31, 2015 | $ | 18,322 | ||
The Company records an estimate for doubtful accounts based on the aging category and historical collection experience of each product sales or other business included in other service revenues, as discussed in the note above.
The receivables related to the Company's optical products purchasing organization are recognized separately from patient accounts receivable, as discussed above, and are included in other current assets in the consolidated balance sheets. Such receivables were $8.4 million and $7.6 million at December 31, 2015 and 2014, respectively.
Inventories
Inventories, which consist primarily of medical and drug supplies, are stated at the lower of cost or market value. Cost is determined using the first-in, first-out method.
Prepaid Expenses and Other Current Assets
A summary of prepaid expenses and other current assets follows (in thousands):
December 31, | ||||||||
2015 | 2014 | |||||||
Prepaid expenses | $ | 7,409 | $ | 7,050 | ||||
Receivables - optical product purchasing organization | 8,434 | 7,556 | ||||||
Acquisition escrow receivable | 8,000 | — | ||||||
Other current assets | 10,777 | 9,399 | ||||||
Total | $ | 34,620 | $ | 24,005 | ||||
Property and Equipment
Property and equipment are stated at cost or, if obtained through acquisition, at fair value determined on the date of acquisition. Depreciation is recognized using the straight-line method over the estimated useful lives of the assets, generally three to five years for computers and software and five to seven years for furniture and equipment. Leasehold improvements are depreciated on a straight-line basis over the shorter of the lease term or the estimated useful life of the assets. Routine maintenance and repairs are expensed as incurred, while expenditures that increase capacities or extend useful lives are capitalized.
F-13
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
The Company also leases certain facilities and equipment under capital leases. Assets held under capital leases are stated at the present value of minimum lease payments at the inception of the related lease. Such assets are depreciated on a straight-line basis over the lesser of the lease term or the remaining useful life of the leased asset.
Goodwill and Intangible Assets
Goodwill represents the fair value of the consideration provided in an acquisition over the fair value of net assets acquired and is not amortized. The Company has indefinite-lived intangible assets related to the certificates of need held in jurisdictions where certain of its surgical facilities are located. The Company also has finite-lived intangible assets related to physician guarantee agreements, non-compete agreements, management agreements and customer relationships. Physician income guarantees are amortized into salaries and benefits costs in the consolidated statements of operations over the commitment period of the contract, generally three to four years. Non-compete agreements and management rights agreements are amortized into depreciation and amortization expense in the consolidated statements of operations over the service lives of the agreements, ranging from two years to 20 years for non-compete agreements and 15 years for the management rights agreements. Customer relationships are amortized into depreciation and amortization expense in the consolidated statements of operations over the estimated lives of the relationships, ranging from three to ten years.
Impairment of Long-Lived Assets, Goodwill and Intangible Assets
The Company evaluates the carrying value of long-lived assets when impairment indicators are present or when circumstances indicate that impairment may exist. The Company performs an impairment test by preparing an expected undiscounted cash flow projection. If the projection indicates that the recorded amount of the long-lived asset is not expected to be recovered, the carrying value is reduced to estimated fair value. The cash flow projection and fair value represents management’s best estimate, using appropriate and customary assumptions, projections and methodologies, at the date of evaluation. No impairment losses on long-lived assets were recognized during the years ended December 31, 2015, 2014 and 2013.
The Company tests its goodwill and indefinite-lived intangible assets for impairment annually, as of October 1, or more frequently if certain indicators arise. The Company performs its annual goodwill impairment assessment by developing a fair value estimate of the business enterprise as of October 1, 2015 using a discounted cash flows approach and comparing the fair value to the carrying value of the net assets of the individual reporting units as of October 1, or additionally if impairment indicators are present. The results of the Company's fair value estimate are then corroborated using a market-based approach. The result of the Company's annual goodwill impairment test at October 1, 2015 indicated no impairment. During the year ended December 31, 2013, the Company recorded an impairment charge of $581,000 related to its Patient Education Concepts reporting unit, which was the entire goodwill balance of this reporting unit. The impairment charge is included in the consolidated statement of operations as of December 31, 2013 as a component of other (income) expense. There was no impairment charges recorded during the year ended December 31, 2014.
During the quarter ended December 31, 2015, the Company voluntarily changed its annual goodwill and indefinite-lived intangible assets impairment testing date from December 31 to October 1 of each year. The change in the goodwill and indefinite-lived intangible assets impairment testing date better aligns the impairment testing procedures with the timing of the Company’s annual strategic planning and forecasting process, which is a significant input to the testing, and provides additional time for the completion of the annual analysis prior to the completion of the Company’s annual reporting period. Accordingly, the Company considers this accounting principle change to be preferable. The Company is unable to objectively determine, without the use of hindsight, the projected cash flows and related valuation estimates that would have been used in earlier periods. Therefore, the Company prospectively applied the change in the annual goodwill impairment and indefinite-lived intangible assets testing date beginning October 1, 2015 as retrospective application to prior periods is deemed impracticable. This change in testing date did not delay, accelerate, or avoid a goodwill impairment charge.
Restricted Invested Assets
Restricted invested assets of $316,000 at December 31, 2015 and 2014 were related to a requirement under the operating lease agreement at the Company's Chesterfield, Missouri facility. In accordance with the provisions of the lease agreement, the Company has a deposit with the landlord that shall be held as security for performance under the Company's covenants and obligations within the agreement through January 2024.
Other Long-Term Assets
A summary of other long-term assets follows (in thousands):
December 31, | ||||||||
2015 | 2014 | |||||||
Notes receivable | $ | 212 | $ | 182 | ||||
Deposits | 2,475 | 2,196 | ||||||
Assets of SERP | 1,606 | 1,402 | ||||||
Other | 4,211 | 2,099 | ||||||
Total | $ | 8,504 | $ | 5,879 | ||||
F-14
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
Other Current Liabilities
A summary of other current liabilities follows (in thousands):
December 31, | ||||||||
2015 | 2014 | |||||||
Interest payable | $ | 5,410 | $ | 7,027 | ||||
Current taxes payable | 1,977 | 3,189 | ||||||
Insurance liabilities | 5,476 | 5,552 | ||||||
Third-party settlements | 5,222 | 11,708 | ||||||
Acquisition consideration payable | 16,768 | — | ||||||
Amounts due to patients and payors | 11,424 | 9,476 | ||||||
Other accrued expenses | 22,133 | 16,918 | ||||||
Total | $ | 68,410 | $ | 53,870 | ||||
Other Long-Term Liabilities
A summary of other long-term liabilities follows (in thousands):
December 31, | ||||||||
2015 | 2014 | |||||||
Facility lease obligations | $ | 53,927 | $ | 50,749 | ||||
Medical malpractice liability | 6,339 | 4,253 | ||||||
Liability of SERP | 1,608 | 1,415 | ||||||
Contingent consideration obligation | 14,049 | 13,009 | ||||||
Acquisition consideration payable | — | 16,768 | ||||||
Unfavorable lease liability | 1,996 | 2,427 | ||||||
Other long-term liabilities | 7,694 | 1,989 | ||||||
Total | $ | 85,613 | $ | 90,610 | ||||
The Company has facility lease obligations in connection with the surgical hospital located in Idaho Falls, Idaho and with a radiation oncology building at this facility. The obligation is payable to the lessor of this facility for the land, building and improvements. The current portion of the lease obligation was $797,000 and $568,000 at December 31, 2015 and 2014, respectively, and was included in other current liabilities in the consolidated balance sheets. The total of the facility lease obligations related to the surgical hospital and radiation oncology building in Idaho Falls, Idaho was $50.8 million and $51.3 million at December 31, 2015 and 2014, respectively.
In August 2015, the Company sold real estate in Ocala, Florida for $4.2 million and subsequently leased the real estate from the new owner. As this transaction did not qualify for sale leaseback treatment under ASC 840, Leases, the Company recorded a financing lease obligation of $4.2 million. The obligation is payable to the lessor of this facility for the building. The current portion of the liability was $169,000 included in other current liabilities and $3.9 million included in other long-term liabilities at December 31, 2015.
Equity-Based Compensation
Transactions in which the Company receives employee and non-employee services in exchange for the Company’s equity instruments or liabilities that are based on the fair value of the Company’s equity securities or may be settled by the issuance of these securities are accounted for using a fair value method. Prior to the Reorganization, on the grant date, the Company employed a market approach to estimate the fair value of equity-based awards based on various considerations and assumptions, including implied earnings multiples and other metrics of relevant market participants, the Company’s operating results and forecasted cash flows and the Company’s capital structure. Such estimates require the input of highly subjective, complex assumptions. However, such assumptions are no longer required to determine fair value of shares of the Company’s common stock as its underlying shares began trading publicly during the fourth quarter of 2015. The Company applies the Black-Scholes-Merton method of valuation in determining share-based compensation expense for option awards.
The Company’s policy is to recognize compensation expense using the straight line method over the relevant vesting period for units that vest based on time. Prior to the Reorganization, employees held membership units in Surgery Center Holdings, LLC, and the associated expense was referred to as unit-based compensation; following the Reorganization, such expense is referred to as equity-based compensation.
F-15
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
Earnings Per Share
Basic and diluted earnings per share are calculated in accordance with ASC 260, Earnings Per Share, based on the weighted-average number of shares outstanding in each period and dilutive stock options, unvested shares and warrants, to the extent such securities exist and have a dilutive effect on earnings per share.
Professional, General and Workers' Compensation Insurance
The Company maintains general liability and professional liability insurance in excess of self-insured retentions through third party commercial insurance carriers in amounts that management believes is sufficient for the Company's operations, although, potentially, some claims may exceed the scope of coverage in effect. The professional and general insurance coverage is on a claims-made basis. Workers' compensation insurance is on an occurrence basis.
The Company expenses the costs under the self-insured retention exposure for general and professional liability and workers compensation claims which relate to (i) claims made during the policy period, which are offset by insurance recoveries and (ii) an estimate of claims incurred but not yet reported that are expected to be reported after the policy period expires. Reserves and provisions are based upon actuarially determined estimates using individual case-basis valuations and actuarial analysis. Reserves for professional, general and workers' compensation claim liabilities are determined with no regard for expected insurance recoveries and are presented gross on the consolidated balance sheets. Total professional, general and workers' compensation claim liabilities as of December 31, 2015 and 2014 are $9.5 million and $7.4 million, respectively. The balance includes expected insurance recoveries of $6.3 million and $5.0 million as of December 31, 2015 and 2014, respectively.
Electronic Health Record Incentives
The American Recovery and Reinvestment Act of 2009 provides for Medicare and Medicaid incentive payments beginning in calendar year 2011 for eligible hospitals and professionals that implement and achieve meaningful use of certified Electronic Health Records ("EHR") technology. Several of the Company's surgical hospitals, which were acquired in connection with the acquisition of Symbion, have implemented plans to comply with the EHR meaningful use requirements of the Health Information Technology for Economic and Clinical Health Act ("HITECH") in time to qualify for the maximum available incentive payments.
Compliance with the meaningful use requirements has and will continue to result in significant costs including business process changes, professional services focused on successfully designing and implementing the Company's EHR solutions, along with costs associated with the hardware and software components of the project. The Company currently estimates that total costs incurred to comply will be recovered through the total EHR incentive payments over the projected life cycle of this initiative. The Company incurs both capital expenditures and operating expenses in connection with the implementation of its various EHR initiatives. The amount and timing of these expenditures do not directly correlate with the timing of the Company's cash receipts or recognition of the EHR incentives as other income. The Company expects to receive incentive payments and recognize corresponding revenue upon the completion of the EHR meaningful use requirements. The Company recorded incentive income of $1.8 million and $3.4 million during the years ended December 31, 2015 and 2014, respectively.
Income Taxes
The Company uses the asset and liability method to account for income taxes. Under this method, deferred income tax assets and liabilities are recognized for the future tax consequences attributable to differences between the financial statement carrying amounts of existing assets and liabilities and their respective tax bases. Deferred tax assets and liabilities are measured using enacted tax rates expected to apply to taxable income in the years in which those temporary differences are expected to be recovered or settled. The effect on deferred tax assets and liabilities of a change in tax rates is recognized in income in the period that includes the enactment date. If a net operating loss carryforward exists, the Company makes a determination as to whether that net operating loss carryforward will be utilized in the future. A valuation allowance is established for certain net operating loss carryforwards when their recoverability is deemed to be uncertain. The carrying value of the net deferred tax assets assumes that the Company will be able to generate sufficient future taxable income in certain tax jurisdictions, based on estimates and assumptions. If these estimates and related assumptions change in the future, the Company may be required to adjust its deferred tax valuation allowances.
The Company, or one or more of its subsidiaries, files income tax returns in the U.S. federal jurisdiction and various state jurisdictions. With few exceptions, the Company is no longer subject to U.S. federal or state income tax examinations for years prior to 2010.
Recent Accounting Pronouncements
In May 2014, the Financial Accounting Standards Board ("FASB") issued Accounting Standards Update ("ASU") 2014-09, "Revenue from Contracts with Customers," which outlines a single comprehensive model for recognizing revenue and supersedes most existing revenue recognition guidance, including guidance specific to the healthcare industry. This ASU provides companies the option of applying a full or modified retrospective approach upon adoption. This ASU was originally set to be effective for fiscal years beginning after December 15, 2016, and early adoption was not permitted. In July 2015, the FASB deferred the effective date for the standard to be effective for fiscal years beginning after December 15, 2017. The FASB will now permit companies to early adopt within one year of the new effective date. The Company will adopt this ASU on January 1, 2018 and is currently evaluating its plan for adoption and the impact on the Company's revenue recognition policies, procedures and the resulting impact on the Company's consolidated financial position, results of operations and cash flows.
F-16
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
In February 2015, the FASB issued ASU 2015-02, “Consolidation: Amendments to the Consolidation Analysis,” which amends the current consolidation guidance, including introducing a separate consolidation analysis specific to limited partnerships and other similar entities. Under this analysis, limited partnerships and other similar entities will be considered a variable-interest entity unless the limited partners hold substantive kick-out rights or participating rights. The provisions of ASU 2015-02 are effective for annual reporting periods beginning after December 15, 2015. Early adoption is permitted. The Company does not anticipate that the adoption of ASU 2015-02 will have a material impact on its financial position, results of operations, cash flows and financial disclosures.
In April 2015, the FASB issued ASU 2015-03, “Simplifying the Presentation of Debt Issuance Costs," which simplifies the presentation of debt issuance costs by requiring debt issuance costs related to a recognized debt liability be presented in the balance sheet as a direct deduction from the carrying amount of that debt liability, consistent with debt discounts. ASU 2015-03 is effective for fiscal years, and interim periods within those years, beginning after December 15, 2015. Early adoption is permitted, and the new guidance should be applied retrospectively. The Company plans to adopt this ASU on January 1, 2016, and does not anticipate that such adoption will have a material effect on its consolidated financial position, results of operations, or cash flows.
In August 2015, the FASB issued ASU 2015-15, "Presentation and Subsequent Measurement of Debt Issuance Costs Associated with Line-of-Credit Arrangements" which clarifies the SEC staff’s position on presenting and measuring debt issuance costs incurred in connection with line-of-credit arrangements given the lack of guidance on this topic in ASU 2015-03. The SEC staff has announced that it would “not object to an entity deferring and presenting debt issuance costs as an asset and subsequently amortizing the deferred debt issuance costs ratably over the term of the line-of-credit arrangement.” The Company plans to adopt this ASU on January 1, 2016, and does not anticipate that such adoption will have a material effect on its consolidated financial position, results of operations, or cash flows.
In September 2015, the FASB issued ASU 2015-16, “Business Combinations: Simplifying the Accounting for Measurement-Period Adjustments” which eliminates the requirement for an acquirer to retrospectively adjust its financial statements for changes to provisional amounts that are identified during the measurement-period following the consummation of a business combination. Instead, ASU 2015-16 requires these types of adjustments to be made during the reporting period in which they are identified and would require additional disclosure or separate presentation of the portion of the adjustment that would have been recorded in the previously reported periods as if the adjustment to the provisional amounts had been recognized as of the acquisition date. ASU 2015-16 is effective prospectively for fiscal years beginning after December 15, 2015, including interim periods within those years. The Company does not anticipate that the adoption of ASU 2015-16 will have a material impact on its financial position, results of operations, cash flows and financial disclosures.
In November 2015, the FASB issued ASU 2015-17, “Balance Sheet Classification of Deferred Taxes”, which simplifies the presentation of deferred income taxes. This ASU requires that deferred tax assets and liabilities be classified as long-term in the statement of financial position. The Company early adopted ASU 2015-17 effective December 31, 2015 on a prospective basis. Adoption of this ASU resulted in a reclassification of the Company's net current deferred tax asset to a net long-term deferred tax asset in its consolidated balance sheet as of December 31, 2015. No prior periods were retrospectively adjusted.
In February 2016, the FASB issued ASU No. 2016-02, "Leases", which will require, among other items, lessees to recognize most leases as assets and liabilities on the balance sheet. Qualitative and quantitative disclosures will be enhanced to better understand the amount, timing and uncertainty of cash flows arising from leases. This guidance is effective for financial statements issued for fiscal years beginning after December 15, 2018, and interim periods within those fiscal years, with early adoption permitted. The Company is currently evaluating the impact this new guidance may have on the consolidated financial statements.
3. Acquisitions and Developments
The Company accounts for its business combinations in accordance with the fundamental requirements of the acquisition method of accounting and under the premise that an acquirer can be identified for each business combination. The acquirer is the entity that obtains control of one or more businesses in the business combination and the acquisition date is the date the acquirer achieves control. The assets acquired, liabilities assumed and any non-controlling interests in the acquired business at the acquisition date are recognized at their fair values as of that date, and the direct costs incurred in connection with the business combination are recorded and expensed separately from the business combination. Acquisitions in which the Company is able to exert significant influence but does not have control are accounted for using the equity method.
2015 Transactions
Surgical Facility Acquisitions
During the year ended December 31, 2015, the Company acquired a controlling interest in two surgical facilities located in new markets and three surgical facilities, four anesthesia practices and an urgent care facility in existing markets for an aggregate purchase price of $84.2 million. The Company consolidates these facilities for financial reporting purposes. These transactions were funded with a combination of cash from operations, facility ownership, and proceeds from the refinancing of the Company's credit facilities in connection with the Symbion acquisition.
Ancillary Services
During the year ended December 31, 2015, through its recruiting efforts and capital-efficient acquisitions, the Company completed thirteen in-market physician practice transactions through an aggregate investment of $40.4 million. These transactions added a total of 17 physicians to the Company’s physician network and were funded with a combination of cash from operations and revolver proceeds.
The aggregate amounts preliminarily recognized as of the acquisition date for each major class of assets and liabilities assumed in the acquisitions closed during the year ended December 31, 2015 as follows:
F-17
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
Cash consideration | $ | 122,470 | |
Fair value of non-controlling interests | 13,842 | ||
Aggregate fair value of acquisitions | 136,312 | ||
Net assets acquired: | |||
Cash and cash equivalents | 1,350 | ||
Accounts receivable | 8,448 | ||
Other current assets | 9,650 | ||
Property and equipment | 3,293 | ||
Intangible assets | 7,539 | ||
Long-term assets | 40 | ||
Accounts payable and other current assets | (5,391 | ) | |
Current maturities of long-term debt | (226 | ) | |
Long-term deferred tax liability | (1,836 | ) | |
Long-term debt | (367 | ) | |
Net assets acquired | 22,500 | ||
Excess of fair value over identifiable net assets acquired | $ | 113,812 | |
The fair values assigned to certain assets and liabilities assumed by the Company have been estimated on a preliminary basis and are subject to change as new facts and circumstances emerge that were present at the date of acquisition.
Acquisition of Symbion
On June 13, 2014, the Company, through its wholly-owned subsidiary, SCH Acquisition Corp. (“Merger Sub”), entered into an Agreement and Plan of Merger (the “Merger Agreement”) with Symbion Holdings Corporation ("Symbion"). Pursuant to the terms of the Merger Agreement, Merger Sub merged with and into Symbion, with Symbion being the surviving corporation in the merger (the “Merger”). At the closing of the Merger, each share of common stock of Symbion, other than those held by Symbion or by the Company, Merger Sub or their subsidiaries and other than those shares with respect to which appraisal rights are properly exercised in accordance with the General Corporation Law of the State of Delaware, were converted into the right to receive a cash payment per share equal to (x) $792.0 million, subject to certain adjustments for Symbion’s cash, debt, transaction expenses, working capital and other items at closing, plus the aggregate exercise price of all vested options, minus certain escrowed amounts relating to post-closing purchase price adjustment and indemnity obligations, divided by (y) the number of shares outstanding on a fully-diluted basis assuming full exercise of vested options and exercise of rights to receive shares upon the exchange of the 8.00% Senior PIK Exchangeable Notes due 2017 issued by Symbion (the “Merger Consideration”). In addition, each outstanding option to purchase shares of Symbion’s common stock were cancelled, and the holders of vested options were paid an amount equal to the excess, if any, of the Merger Consideration over the per-share exercise price of such vested options.
The Company obtained financing commitments for the transactions contemplated by the Merger Agreement, the aggregate proceeds of which were sufficient for the Company to pay the aggregate Merger Consideration and all related fees and expenses.
The Company completed the Merger effective November 3, 2014. At closing, the Company paid approximately $300.1 million in cash, including $16.2 million funded to an escrow account, and assumed approximately $472.4 million of outstanding indebtedness of Symbion, plus related accrued and unpaid interest. During the three months ended June 30, 2015, $2.1 million of the escrow account was distributed based on a working capital settlement reducing the total amount funded on the escrow account to $14.0 million as of December 31, 2015. The Company received $1.2 million of the escrow disbursement reducing the cash consideration to $298.9 million and adjusted the purchase price allocation to goodwill. The Company will fund an additional $16.8 million to the escrow account by May 3, 2016. The $30.8 million remaining escrow balance is payable to Symbion on May 3, 2016, pending the resolution of any adjustments and the settlement of any other indemnities.
The acquisition of Symbion enhances the growth profile of the Company by expanding its network of surgical facilities in attractive markets throughout the United States.
The Merger was financed through the issuance of $1.4 billion of Senior Secured Credit Facilities ("Facilities"), which includes an $870.0 million first lien term loan due November 3, 2020, a $490.0 million second lien term loan due November 3, 2021 and an $80.0 million revolving credit facility.
Fees associated with the Merger, which includes fees incurred related to the Company's debt financings, were approximately $93.3 million. Approximately $5.3 million was capitalized as deferred financing costs, $21.7 million related to legal and other transaction fees which were expensed as transaction costs, $42.9 million was recorded as a reduction of the carrying value of the Facilities and $23.4 million was recorded as debt extinguishment costs during the year ended December 31, 2014.
Acquired assets and assumed liabilities include, but are not limited to, fixed assets, intangible assets and professional liabilities. The valuations are based on appraisal reports, discounted cash flow analyses, actuarial analyses or other appropriate valuation techniques to determine the fair value of the assets acquired or liabilities assumed. A majority of the deferred income taxes recognized as a component of
F-18
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
the Company's purchase price allocation is a result of the difference between the book and tax basis of the amortizable intangible assets recognized.
The purchase price amount has been allocated to the related assets acquired and liabilities assumed based upon their respective fair values as follows:
Cash consideration | $ | 298,857 | |
Acquisition consideration payable | 16,768 | ||
Fair value of non-controlling interests | 395,663 | ||
Fair value of Symbion | 711,288 | ||
Net assets acquired: | |||
Cash | 40,374 | ||
Accounts receivable, net | 79,830 | ||
Inventories | 18,389 | ||
Prepaid expenses and other current assets | 9,876 | ||
Property and equipment | 153,179 | ||
Investments in and advances to affiliates | 32,728 | ||
Intangible assets | 31,534 | ||
Restricted invested assets | 316 | ||
Other long-term assets | 6,239 | ||
Accounts payable | (20,419 | ) | |
Accrued payroll and benefits | (14,600 | ) | |
Other current liabilities | (47,229 | ) | |
Current maturities of long-term debt | (83,805 | ) | |
Long-term debt, less current maturities | (376,395 | ) | |
Long-term deferred tax liabilities | (19,853 | ) | |
Other long-term liabilities | (60,500 | ) | |
Net assets acquired | (250,336 | ) | |
Excess of fair value over identifiable net assets acquired | $ | 961,624 | |
The entire amount of goodwill acquired in connection with the Merger was allocated to the Company's surgical facility services operating segment. The total amount of the goodwill related to the acquisition of Symbion that will be deductible for tax purposes is $142.5 million.
Fair value attributable to non-controlling interests was based on a Level 3 computation using significant inputs that are not observable in the market. Key inputs used to determine the fair value include financial multiples used in the purchase of non-controlling interests, primarily from acquisitions of surgical facilities. Such multiples, based on earnings, are used as a benchmark for the discount to be applied for the lack of control or marketability. Fair value attributable to the property and equipment acquired was based on Level 3 computations using key inputs such as cost trend data and comparable asset sales. Fair value attributable to the intangible assets acquired was based on Level 3 computations using key inputs such as the Company's internally-prepared financial projections. Fair values assigned to acquired working capital were based on carrying amounts reported by Symbion at the date of acquisition, which approximate their fair values.
F-19
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
The unaudited consolidated pro forma results for year ended ended December 31, 2014, assuming the Symbion acquisition had been consummated on January 1, 2013, are as follows (in thousands):
Year Ended December 31, | |||||||
2014 | 2013 | ||||||
Net revenues | $ | 873,683 | $ | 820,186 | |||
Net income | 31,557 | 42,714 | |||||
Less: net income attributable to non-controlling interests | (68,973 | ) | (64,396 | ) | |||
Net loss attributable to Surgery Partners, Inc. | $ | (37,416 | ) | $ | (21,682 | ) | |
These pro forma amounts for the year ended December 31, 2014, exclude expenses related to the Merger transaction of $21.7 million and the loss on debt extinguishment of $23.4 million. In addition, the year ended December 31, 2013 excludes $9.9 million of expense related to loss on debt extinguishment.
Other 2014 Transactions
Throughout 2014, the Company acquired three physician practices for an aggregate purchase price of $1.6 million. These transactions were funded with cash from continuing operations.
2013 Transactions
During 2013, the Company acquired 100% ownership interests in both a specialty pharmacy and a physician practice. The aggregate purchase price of these transactions was approximately $417,000.
4. Divestitures
2015 Transactions
During the year ended December 31, 2015, the Company sold its interest in three surgical facilities and received aggregate proceeds of $10.9 million resulting in a pre-tax gain of approximately $2.9 million in the consolidated statements of operations.
2013 Transactions
During the year ended December 31, 2013, the Company disposed of two surgical facilities and a physician practice and received aggregate proceeds of $1.0 million resulting in a pre-tax loss of approximately $2.6 million in the consolidated statements of operations.
5. Property and Equipment
A summary of property and equipment follows (in thousands):
December 31, | ||||||||
2015 | 2014 | |||||||
Land | $ | 6,790 | $ | 6,790 | ||||
Buildings and improvements | 104,971 | 100,574 | ||||||
Furniture and equipment | 14,520 | 13,662 | ||||||
Computer and software | 24,597 | 20,622 | ||||||
Medical equipment | 96,291 | 86,132 | ||||||
Construction in progress | 7,619 | 2,923 | ||||||
Property and equipment, at cost | 254,788 | 230,703 | ||||||
Less: Accumulated depreciation | (70,238 | ) | (55,697 | ) | ||||
Property and equipment, net | $ | 184,550 | $ | 175,006 | ||||
The carrying values of assets under capital lease were $12.3 million and $13.3 million as of December 31, 2015 and 2014, respectively, which included accumulated depreciation of $10.5 million and $6.8 million, respectively.
F-20
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
6. Goodwill and Intangible Assets
A summary of activity related to goodwill for the year ended December 31, 2015 follows (in thousands):
Balance at December 31, 2013 | $ | 339,521 | ||
Acquisitions | 959,232 | |||
Divestitures | — | |||
Purchase price adjustments | — | |||
Balance at December 31, 2014 | $ | 1,298,753 | ||
Acquisitions | 113,812 | |||
Divestitures | (8,399 | ) | ||
Purchase price adjustments | 3,761 | |||
Balance at December 31, 2015 | $ | 1,407,927 | ||
Additions to goodwill include new business combination acquisitions and incremental ownership acquired in the Company's subsidiaries. A summary of the Company's acquisitions for the years ended December 31, 2015 and 2014 is included in Note 3, Acquisitions and Developments.
The Company tests its goodwill and indefinite-lived intangible assets for impairment annually, as of October 1, or more frequently if certain indicators arise. The Company reviews goodwill at the reporting unit level, which is defined as one level below an operating segment. The Company has determined that it has six reporting units, which include the following: 1) Surgical Facilities 2) Ancillary Services, 3) Midwest Labs, 4) The Alliance, including Optical Synergies, 5) Family Vision Care and 6) Patient Education Concepts, the Company's marketing products and services business. When reviewing goodwill, the Company compares the carrying value of the net assets of the reporting unit to the estimated fair value of the reporting unit. If the carrying value exceeds the net present value of the estimated discounted future cash flows, an impairment indicator exists and an estimate of the possible impairment loss is calculated. The fair value calculation includes multiple assumptions and estimates, including the projected cash flows and discount rates applied.
The Company performed its annual goodwill impairment assessment by developing a fair value estimate of the business enterprise as of October 1, 2015 using a discounted cash flows approach. The results of the Company's fair value estimate were corroborated using a market-based approach. The result of the Company's annual goodwill impairment test at October 1, 2015 indicated no impairment. During the year ended December 31, 2013, the Company recorded an impairment charge of $581,000 related to its Patient Education Concepts reporting unit, which was the entire goodwill balance of this reporting unit. The impairment charge is included in the consolidated statement of operations as of December 31, 2013 as a component of other (income) expense. There was no impairment charges recorded during the years ended December 31, 2015 and 2014.
A summary of the activity related to intangible assets as of December 31, 2015 follows (in thousands):
Physician Income Guarantees | Management Rights | Non-Compete Agreements | Certificates of Need | Customer Relationships | Other | Total Intangible Assets | ||||||||||||||||||||||
Balance at December 31, 2013 | $ | — | $ | 377 | $ | 16,123 | $ | — | $ | 7,665 | $ | 2,811 | $ | 26,976 | ||||||||||||||
Additions | 1,081 | 24,700 | 3,500 | 3,711 | — | 242 | 33,234 | |||||||||||||||||||||
Recruitment expense | (108 | ) | — | — | — | — | — | (108 | ) | |||||||||||||||||||
Amortization | — | (320 | ) | (3,033 | ) | — | (1,391 | ) | (470 | ) | (5,214 | ) | ||||||||||||||||
Balance at December 31, 2014 | $ | 973 | $ | 24,757 | $ | 16,590 | $ | 3,711 | $ | 6,274 | $ | 2,583 | $ | 54,888 | ||||||||||||||
Additions | 1,052 | — | 7,532 | — | — | — | 8,584 | |||||||||||||||||||||
Recruitment expense | (813 | ) | — | — | — | — | — | (813 | ) | |||||||||||||||||||
Amortization | — | (1,731 | ) | (5,551 | ) | — | (1,338 | ) | (471 | ) | (9,091 | ) | ||||||||||||||||
Balance at December 31, 2015 | $ | 1,212 | $ | 23,026 | $ | 18,571 | $ | 3,711 | $ | 4,936 | $ | 2,112 | $ | 53,568 | ||||||||||||||
During the years ended December 31, 2015, 2014 and 2013, the Company had amortization expense of $9.1 million, $5.2 million and $4.9 million, respectively.
F-21
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
A summary of the scheduled amortization related to the Company's finite-lived intangible assets as of December 31, 2015 follows (in thousands):
Amortization of Finite-Lived Intangible Assets | ||||
2016 | $ | 9,707 | ||
2017 | 8,220 | |||
2018 | 6,316 | |||
2019 | 5,764 | |||
2020 | 2,616 | |||
Thereafter | 16,992 | |||
Total | $ | 49,615 | ||
7. Long-Term Debt
A summary of long-term debt follows (in thousands):
December 31, | ||||||||
2015 | 2014 | |||||||
2014 Revolver Loan | $ | 125,250 | $ | — | ||||
2014 First Lien Credit Agreement, dated November 3, 2014, maturing November 3, 2020, net of debt issuance and discount of $20,223 and $23,818 at December 31, 2015 and 2014, respectively | 841,078 | 846,183 | ||||||
2014 Second Lien Credit Agreement, dated November 3, 2014, maturing November 3, 2021, net of debt issuance and discount of $8,159 and $18,184 at December 31, 2015 and 2014, respectively | 238,341 | 471,816 | ||||||
Subordinated Notes | 1,000 | 1,000 | ||||||
Notes payable and secured loans | 40,615 | 31,600 | ||||||
Capital lease obligations | 11,316 | 10,755 | ||||||
Total debt | 1,257,600 | 1,361,354 | ||||||
Less: Current maturities | 27,272 | 22,088 | ||||||
Total long-term debt | $ | 1,230,328 | $ | 1,339,266 | ||||
The acquisition of Symbion on November 3, 2014 and payoff of the senior debt was financed through new $1.440 billion Senior Secured Credit Facilities (the "Facilities") consisting of the following:
• | $80.0 million revolving credit facility ( "2014 Revolver Loan") |
• | $870.0 million 1st lien term loan facility ("2014 First Lien Credit Agreement") |
• | $490.0 million 2nd lien term loan facility ("2014 Second Lien Credit Agreement") |
On November 3, 2014, in connection with the consummation of the Symbion acquisition, the Company assumed and paid down approximately $440.0 million of outstanding indebtedness of Symbion, including accrued interest. Simultaneously, the Company paid off all of the debt outstanding under its then-existing credit agreements ("Credit Facilities") and revolver loan.
2014 Revolver Loan
The 2014 Revolver Loan (“Revolver”) will be used for working capital, acquisitions and development activities and general corporate purposes in an aggregate principal amount at any time outstanding not to exceed $80.0 million and matures on November 3, 2019. On October 7, 2015, the Company entered into an amendment to the 2014 First Lien Credit Agreement to increase certain lenders’ commitments under the Revolver from $80.0 million to an aggregate of $150.0 million. The Company has the option of classifying borrowings under the Revolver as either Alternate Base Rate ("ABR") loans or Eurodollar ("ED") loans. The interest base rate on an ABR loan is equal to the greatest of (a) the Prime Rate in effect on such day, (b) the Federal Funds Effective Rate in effect on such day plus 0.50% and (c) the adjusted LIBO Rate for a Eurodollar Borrowing with a one-month interest period plus 1.00%. In addition to the base
F-22
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
rate, the Company is required to pay a 3.25% margin for ABR loans. The interest base rate on an ED loan is equal to (x) the LIBO Rate for such Eurodollar borrowing in effect for such Interest Period divided by (y) One minus the Statutory Reserves (if any) for such Eurodollar Borrowing for such interest period. In addition to the base rate, the Company is required to pay a 4.25% margin for ED loans.
The Company paid $2.3 million in connection with obtaining the Revolver and recorded this amount as debt issuance costs, which is presented, net of accumulated amortization of approximately $530,000 and $76,000, in the accompanying consolidated balance sheets as of December 31, 2015 and 2014, respectively.
The Company must also pay quarterly commitment fees of 0.50% per annum of the average daily unused amount of the Revolver. As of December 31, 2015, the Company's availability on the Revolver was $21.6 million.
The credit agreement that governs the Revolver contains various covenants that include limitations on the Company's indebtedness, liens, acquisitions and investments. It additionally includes the requirement that the Company maintain a net leverage ratio within a specified range. At December 31, 2015, the Company was in compliance with the covenants contained in the credit agreement.
2014 First Lien Credit Agreement
The 2014 First Lien Credit Agreement (“2014 First Lien”) is a senior secured obligation of Surgery Center Holdings, Inc. and is guaranteed on a senior secured basis by the Company and certain of its subsidiaries. The 2014 First Lien matures on November 3, 2020. The Company has the option of classifying the 2014 First Lien as either an ABR loan or an ED loan. The interest base rate on an ABR loan is equal to the greatest of (a) the Prime Rate in effect on such day, (b) the Federal Funds Effective Rate in effect on such day plus 0.50%, and (c) the Adjusted LIBO Rate for a Eurodollar Borrowing with a one-month interest period plus 1.00%; provided that the base rate shall not be less than 2.00% per annum. In addition to the base rate, the Company is required to pay a 3.25% margin for ABR loans. The interest base rate on an ED loan is equal to (x) the LIBO Rate for such Eurodollar borrowing in effect for such Interest Period divided by (y) One minus the Statutory Reserves (if any) for such Eurodollar Borrowing for such interest period; provided that the rate shall not be less than 1.00% per annum. In addition to the base rate, the Company is required to pay a 4.25% margin for ED loans. In 2015, the Company classified the 2014 First Lien as an ED loan with an interest rate of 5.25% (1.00% base rate plus a 4.25% margin). Accrued interest is payable in arrears on a quarterly basis. Within five business days after the earlier of (i) 90 days after the end of each fiscal year or (ii) the date on which financial statements have been delivered, the Company is required to make mandatory prepayments in amounts calculated in accordance with the excess cash flow provisions of the 2014 First Lien Credit Agreement. There were no excess cash flow payments required as of December 31, 2015.
In 2014, the Company recorded $4.4 million and $20.0 million as a reduction of the carrying value of the 2014 First Lien as original issue discount and amounts paid to lender for debt related issuance costs, respectively, which are accreted to interest expense over the term of the loan. During the year ended December 31, 2015, approximately $3.6 million was accreted to interest expense. The Company also paid $1.9 million in connection with obtaining the 2014 First Lien and recorded this amount as debt issuance costs, which is presented as an asset, net of accumulated amortization of approximately $306,000 and $41,000, in the accompanying consolidated balance sheets as of December 31, 2015 and 2014, respectively.
The credit agreement that governs the 2014 First Lien contains various covenants that include limitations on the Company's indebtedness, liens, acquisitions and investments. It additionally includes the requirement that the Company maintain a net leverage ratio within a specified range. At December 31, 2015, the Company was in compliance with the covenants contained in the credit agreement. The 2014 First Lien is collateralized by substantially all of the assets of the Company.
2014 Second Lien Credit Agreement
The 2014 Second Lien Credit Agreement (“2014 Second Lien”) is a senior secured obligation of Surgery Center Holdings, Inc. and is guaranteed on a senior secured basis by the Company and certain of its subsidiaries. The 2014 Second Lien matures on November 3, 2021. The Company has the option of classifying the 2014 Second Lien as either an ABR loan or an ED loan. The interest base rate on an ABR loan is equal to the greatest of (a) the Prime Rate in effect on such day, (b) the Federal Funds Effective Rate in effect on such day plus 0.50% and (c) the Adjusted LIBO Rate for a Eurodollar Borrowing with a one-month interest period plus 1.00%; provided that the base rate shall not be less than 2.00% per annum. In addition to the base rate, the Company is required to pay a 6.50% margin for ABR loans. The interest base rate on an ED loan is equal to (x) the LIBO Rate for such Eurodollar Borrowing in effect for such interest period divided by (y) One minus the Statutory Reserves (if any) for such Eurodollar Borrowing for such interest period; provided that the base rate shall not be less than 1.00% per annum. In addition to the base rate, the Company is required to pay a 7.50% margin for ED loans. During 2015, the Company classified the 2014 Second Lien as an ED loan with an interest rate of 8.50% (1.00% base rate plus a 7.50% margin). Accrued interest is payable in arrears on a quarterly basis. The Company is required to pay the remaining principal balance upon maturity of the 2014 Second Lien on November 3, 2021. The Company has the right at any time to prepay any borrowings, in whole or in part, provided that each partial prepayment shall be in an amount that is an integral multiple of $0.5 million and not less than $1.0 million. Within five business days after the earlier of (i) 90 days after the end of each fiscal year or (ii) the date on which financial statements have been delivered, the Company is required to make mandatory prepayments in amounts calculated in accordance with the excess cash flow provisions of the 2014 Second Lien. There were no excess cash flow payments required as of December 31, 2015.
The Company recorded $4.9 million and $13.6 million as a reduction of the carrying value of the 2014 Second Lien as original issue discount and amounts paid to lender for debt related issuance costs, respectively, which are accreted to interest expense over the term of the loan. During the year ended December 31, 2015, approximately $1.7 million was accreted to interest expense. The Company also paid $1.1 million in connection with obtaining the 2014 Second Lien and recorded this amount as debt issuance costs, which is presented as an
F-23
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
asset, net of accumulated amortization of approximately $57,000 and $14,000, in the accompanying consolidated balance sheets as of December 31, 2015 and 2014, respectively.
On October 6, 2015, the Company prepaid $243.5 million in principal, net of the write-off of discounts and issuance costs totaling $8.3 million, and $65,000 of accrued interest on the 2014 Second Lien. Further, the Company incurred a prepayment penalty of 3% of the aggregate principal amount or $7.3 million. The write-off of the discounts, issuance costs and the prepayment penalty as well as certain other costs are presented as a loss on debt extinguishment of $16.1 million in the accompanying consolidated statement of operations as of December 31, 2015.
The credit agreement that governs the 2014 Second Lien contains various covenants that include limitations on the Company's indebtedness, liens, acquisitions and investments. It additionally includes the requirement that the Company maintain a maximum net leverage ratio. At December 31, 2015, the Company was in compliance with the covenants contained in the credit agreement. The 2014 Second Lien is collateralized by substantially all of the assets of the Company.
Other Debt Transactions
On April 11, 2013, the Company raised $465 million in Senior Secured Credit Facilities (“Credit Facilities”) to refinance a portion of its then existing debt and to return capital to its shareholders (“2013 Debt Refinancing”). These Credit Facilities were used to pay off the $233.7 million outstanding balance of the original $240.0 million term loan (“Term A Loan”), plus accrued interest and fees, and $52.8 million of the outstanding balance of the subordinated debt facility (“Subordinated Notes A”), plus accrued interest and fees. On the date of closing, the Company had no outstanding balance on the original $30.0 million Revolving Loan (“Revolving Loan”). As a result of these transactions, the Term A Loan and Revolving Loan were terminated. The Subordinated Notes A were amended with the outstanding principal balance reduced to $1.0 million.
On January 27, 2014, the Company obtained $90.0 million in additional borrowings on the Credit Facilities to return capital to shareholders. The Company recorded $1.4 million and $2.9 million as a reduction of the carrying value of the additional borrowings as original issue discount and amounts paid to lender for debt related issuance costs, respectively, which are accreted to interest expense over the term of the loan. During the year ended December 31, 2014, approximately $380,000 was accreted to interest expense. The $90.0 million in additional borrowings, including the related debt issuance costs, were included in the extinguishment of debt that was financed with the proceeds of the Facilities obtained in connection with the acquisition of Symbion on November 3, 2014.
Subordinated Notes
Effective April 11, 2013, the Company amended and reduced the size of its subordinated debt facility ("Subordinated Notes") to $1.0 million from $53.8 million. The prepayment premium of $1.6 million that the Company paid in connection with decreasing the size of the subordinated debt facility and the unamortized balance of debt issuance costs related to Subordinated Notes A of $1.1 million were recorded as loss on the extinguishment of debt in the accompanying consolidated statements of operations for the year ended December 31, 2013. Through a separate transaction in April 2013, H.I.G. Surgery Centers, LLC, an affiliate of the Company, purchased the Subordinated Notes from an independent third party. At December 31, 2015 and 2014, the debt is payable to H.I.G. Surgery Centers, LLC. and mature on August 4, 2017.
The outstanding balance of the Subordinated Notes A bore interest of 15.00% per annum through December 31, 2013, of which 12.00% per annum was payable quarterly in cash. The Company had the option to elect that the remaining 3.00% per annum be added to the unpaid principal amount as payment-in-kind ("PIK") or to pay the additional interest in cash. Beginning October 1, 2012, the Company elected to begin paying the additional 3.00% interest in cash on a quarterly basis. Effective January 1, 2014, the Subordinated Notes bear interest of 17.00% per annum.
Term Loan A
During 2011, the Company entered into a $240.0 million Term Loan A related to the acquisition of NovaMed. The Term Loan A was effective May 4, 2011, and was terminated on April 11, 2013 in connection with the 2013 Debt Transactions discussed above. The Company was required to pay quarterly principal payments of $600,000 on the last business day of each March, June, September and December during which the Term Loan A was outstanding. The Company had the option of classifying the Term Loan A as either an ABR loan or an ED loan. During 2013 (until termination of the Term Loan A), the Company classified the Term Loan A as an ED loan with an interest rate of 6.50%.
The Company recorded $1.2 million as a reduction of the carrying value of the Term Loan A as original issue discount which was accreted to interest expense over the term of the loan. During 2013, approximately $58,000 was accreted to interest expense. The Company also paid $8.7 million in connection with obtaining the Term Loan A and amortized approximately $417,000 of these costs during the year ended December 31, 2013.
2011 Revolving Loan
In 2011, the Company secured a 5-year, $20.0 million Revolving Loan (“2011 Revolving Loan”) to be used for working capital and general corporate purposes. The 2011 Revolving Loan was terminated on April 11, 2013 in connection with the 2013 Debt Refinancing. The Company recorded $100,000 as a reduction of the carrying value of the 2011 Revolving Loan as original issue discount, which was accreted to interest expense over the term of the loan. The Company also paid $681,000 in connection with obtaining the Revolving Loan
F-24
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
and amortized $37,800 of these costs during the years ended December 31, 2013, respectively. The Company also paid quarterly commitment fees of 0.50% per annum on the average daily unused amount of the 2011 Revolving Loan.
Notes Payable and Secured Loans
Certain of the Company’s subsidiaries have outstanding bank indebtedness, which is collateralized by the real estate and equipment owned by the surgical facilities to which the loans were made. The various bank indebtedness agreements contain covenants to maintain certain financial ratios and also restrict encumbrance of assets, creation of indebtedness, investing activities and payment of distributions. At December 31, 2015, the Company was in compliance with its covenants contained in the credit agreement. The Company and its subsidiaries had notes payable to financial institutions of $40.6 million and $31.6 million as of December 31, 2015 and 2014, respectively.
Letters of Credit
As of December 31, 2014, the Company had two outstanding letters of credit at its optical purchasing group of $200,000 and $730,000. In May 2015, the Company increased one of these letters of credit from $200,000 to $500,000. The Company had two outstanding letters of credit issued to the landlords for two of its surgical facilities in Orlando, Florida in the amount of $100,000 and in Lubbock, Texas for $1.0 million. In addition, the Company had one outstanding letter of credit related to the Symbion, Inc. workers compensation self-insured plan for $835,000.
Capital Lease Obligations
The Company is liable to various vendors for several equipment leases classified as capital leases. The carrying value of the leased assets was $12.3 million and $13.3 million as of December 31, 2015 and 2014, respectively.
Maturities
A summary of the scheduled maturities of our debt obligations as of December 31, 2015 follows (in thousands):
Capital Lease Obligations | Other Long-Term Debt | Total | ||||||||||
2016 | $ | 4,170 | $ | 23,102 | $ | 27,272 | ||||||
2017 | 3,162 | 27,920 | 31,082 | |||||||||
2018 | 2,246 | 12,433 | 14,679 | |||||||||
2019 | 1,340 | 136,080 | 137,420 | |||||||||
2020 | 351 | 827,146 | 827,497 | |||||||||
Thereafter | 47 | 247,985 | 248,032 | |||||||||
Total debt | $ | 11,316 | $ | 1,274,666 | $ | 1,285,982 | ||||||
8. Operating Leases
The Company leases office space and equipment for its surgical facilities, including surgical facilities under development. The lease agreements generally require the lessee, or the Company, to pay all maintenance, property taxes, utilities and insurance costs. The Company accounts for operating lease obligations and sublease income on a straight-line basis. Contingent obligations of the Company, as defined by each lease agreement, are recognized when specific contractual measures have been met, typically the result of an increase in the Consumer Price Index. Lease obligations paid in advance are recorded as prepaid rent and included in prepaid expenses and other current assets on the consolidated balance sheets. The difference between actual lease payments and straight-line lease expense over the initial lease term, excluding optional renewal periods, is recorded as deferred rent and included in other current liabilities and other long-term liabilities on the consolidated balance sheets. As part of the Merger, the Company ceased use of four of their operating leases and accrued a liability of $4.6 million, net of discounting and sublease income, during the three months ended June 30, 2015. The Company expensed this through merger transaction and integration costs, as the leases related to offices shut down in connection with the Merger.
The future minimum lease payments under non-cancellable operating leases, net of sub-lease income, follows (in thousands):
2016 | $ | 36,443 | ||
2017 | 33,019 | |||
2018 | 29,721 | |||
2019 | 25,677 | |||
2020 | 21,401 | |||
Thereafter | 110,131 | |||
Total minimum operating lease payments | $ | 256,392 | ||
F-25
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
Total operating lease expense was $40.1 million, $18.8 million and $13.5 million for the years ended December 31, 2015, 2014 and 2013, respectively. Included in these amounts, the Company incurred lease expense of $12.9 million, $6.9 million and $5.8 million for years ended December 31, 2015, 2014 and 2013, respectively, under operating lease agreements with physician investors who are related parties.
The Company has various sub-lease arrangements and the future minimum lease payments to be received under these non-cancellable arrangements are as follows (in thousands):
2016 | $ | 1,043 | ||
2017 | 1,101 | |||
2018 | 1,137 | |||
2019 | 658 | |||
2020 | 468 | |||
Thereafter | 2,231 | |||
Total non-cancellable sub-lease income | $ | 6,638 | ||
9. Earnings Per Share
The following is a reconciliation of the numerator and denominator of basic and diluted earnings per share for the years ended December 31, 2015, 2014 and 2013 (in thousands except share and per share amounts):
Year Ended December 31, | ||||||||||||
2015 | 2014 | 2013 | ||||||||||
Numerator: | ||||||||||||
Net income (loss) attributable to Surgery Partners, Inc. | $ | 1,429 | $ | (65,897 | ) | $ | (9,062 | ) | ||||
Denominator: | ||||||||||||
Weighted average shares outstanding- basic (1) | 36,066,233 | 32,295,364 | 31,815,520 | |||||||||
Effect of dilutive securities (2) | 1,398,154 | — | — | |||||||||
Weighted average shares outstanding- diluted | 37,464,387 | 32,295,364 | 31,815,520 | |||||||||
Earnings (loss) per share: | ||||||||||||
Basic earnings (loss) per share | $ | 0.04 | $ | (2.04 | ) | $ | (0.28 | ) | ||||
Diluted earnings (loss) per share (2) | $ | 0.04 | $ | (2.04 | ) | $ | (0.28 | ) | ||||
(1) Effect of the Reorganization has been retrospectively applied to all periods presented.
(2) The impact of potentially dilutive securities for the years ended December 31, 2014 and 2013 was not considered because the effect would be anti-dilutive in each of those periods.
10. Income Taxes and Tax Receivable Agreement
As part of the Reorganization that was effective September 30, 2015, the Company entered into a Tax Receivable Agreement (“TRA”) under which generally the Company will be required to pay to its stockholders as of immediately prior to the IPO 85% of the cash savings, if any, in U.S. federal, state or local tax that the Company actually realizes (or is deemed to realize in certain circumstances) as a result of (i) certain tax attributes, including NOLs, capital losses, charitable deductions, alternative minimum tax credit carryforwards and federal and state tax credits of Surgery Partners, Inc. and its affiliates relating to taxable years ending on or before the date of the Reorganization (calculated by assuming the taxable year of the relevant entity closes on the date of the Reorganization) that are or become available to the Company and its wholly-owned subsidiaries as a result of the Reorganization, and (ii) tax benefits attributable to payments made under the TRA, together with interest accrued at a rate of LIBOR plus 300 basis points from the date the applicable tax return is due (without extension) until paid. The Company expects the payments it will be required to make under the TRA will be substantial.
The amounts payable under the TRA will vary depending upon a number of factors, including the amount, character and timing of the taxable income of Surgery Partners, Inc. in the future. The Company estimates the total amounts payable to be approximately $119.7 million, if the tax benefits of related deferred tax assets are ultimately realized. The amounts payable were recognized during the quarter ended December 31, 2015 in conjunction with the release of the Company's valuation allowance recorded against the deferred tax assets.
F-26
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
The Company and its subsidiaries file a consolidated federal income tax return. The partnerships, limited liability companies, and certain non-consolidated physician practice corporations file separate income tax returns. The Company's allocable portion of each partnership's and limited liability company's income or loss is included in taxable income of the Company. The remaining income or loss of each partnership and limited liability company is allocated to the other owners.
The Company made income tax payments of $1.1 million and $676,000 for the periods ended December 31, 2015 and 2014, respectively.
Income tax (benefit) expense is comprised of the following (in thousands):
Year Ended December 31, | ||||||||||||
2015 | 2014 | 2013 | ||||||||||
Current: | ||||||||||||
Federal | $ | — | $ | — | $ | — | ||||||
State | 909 | 1,669 | 469 | |||||||||
Deferred: | ||||||||||||
Federal | (132,311 | ) | 13,235 | 6,353 | ||||||||
State | (17,580 | ) | 854 | 748 | ||||||||
Total income tax (benefit) expense | $ | (148,982 | ) | $ | 15,758 | $ | 7,570 | |||||
A reconciliation of the provision for income taxes as reported in the consolidated statements of operations and the amount of income tax (benefit) expense computed by multiplying consolidated income (loss) in each year by the U.S. federal statutory rate of 35% follows (in thousands):
Year Ended December 31, | ||||||||||||
2015 | 2014 | 2013 | ||||||||||
Tax (benefit) expense at U.S.federal statutory rate | $ | (26,648 | ) | $ | (3,840 | ) | $ | 8,601 | ||||
State income tax, net of U.S. federal tax benefit | 1,059 | 1,402 | 408 | |||||||||
Change in valuation allowance | (137,721 | ) | 29,336 | 4,067 | ||||||||
Expiration of carryforwards and stock option forfeitures | — | 1,286 | 2,524 | |||||||||
Net income attributable to non-controlling interests | (24,996 | ) | (13,207 | ) | (9,108 | ) | ||||||
Changes in measurement of uncertain tax positions | (10 | ) | 589 | — | ||||||||
Nondeductible transaction costs | 3,442 | 4,230 | — | |||||||||
Tax return reconciling differences | (1,574 | ) | (4,419 | ) | 836 | |||||||
Change in effective tax rate | (2,143 | ) | ||||||||||
TRA liability | 39,428 | |||||||||||
Other | 181 | 381 | 242 | |||||||||
Total income tax (benefit) expense | $ | (148,982 | ) | $ | 15,758 | $ | 7,570 | |||||
F-27
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
The components of temporary differences and the approximate tax effects that give rise to the Company’s net deferred tax asset are as follows (in thousands):
December 31, | ||||||||
2015 | 2014 | |||||||
Deferred tax assets: | ||||||||
Medical malpractice liability | $ | 869 | $ | 526 | ||||
Accrued vacation and incentive compensation | 2,212 | 2,079 | ||||||
Net operating loss carryforwards | 146,663 | 123,709 | ||||||
Allowance for bad debts | 1,846 | 980 | ||||||
Basis differences of partnerships and joint ventures | — | 16,131 | ||||||
SERP liability | 685 | 527 | ||||||
Capital loss carryforwards | 2,052 | 3,513 | ||||||
Stock option compensation | 367 | 362 | ||||||
Deferred rent | 2,288 | — | ||||||
Deferred financing costs | 3,083 | 4,386 | ||||||
Audit and tax fee accruals | 242 | 760 | ||||||
FIN 48 liabilities | 244 | 440 | ||||||
TRA liability | 2,750 | — | ||||||
Other deferred assets | 1,748 | 1,597 | ||||||
Total gross deferred tax assets | 165,049 | 155,010 | ||||||
Less: Valuation allowance | (6,949 | ) | (142,909 | ) | ||||
Total deferred tax assets | 158,100 | 12,101 | ||||||
Deferred tax liabilities: | ||||||||
Depreciation on property and equipment | (806 | ) | (1,050 | ) | ||||
Amortization of intangible assets | (16,083 | ) | (16,159 | ) | ||||
Basis differences of partnerships and joint ventures | (46,494 | ) | (43,195 | ) | ||||
Deferred rent | — | (515 | ) | |||||
Other deferred liabilities | (612 | ) | (466 | ) | ||||
Total deferred tax liabilities | (63,995 | ) | (61,385 | ) | ||||
Net deferred tax assets (liabilities) | $ | 94,105 | $ | (49,284 | ) | |||
As of December 31, 2015 and 2014, the Company had net current deferred tax assets (liabilities) of zero and $(114,000), respectively, and net long-term deferred tax assets (liabilities) of $94.1 million and $(49.2) million, respectively. The Company had federal net operating loss carryforwards of $360.3 million as of December 31, 2015, which expire between 2025 and 2035 and state net operating loss carryforwards of $495.9 million as of December 31, 2015, which expire between 2016 and 2035. The Company had capital loss carryforwards of $5.5 million as of December 31, 2015, which expire between 2016 and 2019. The Company had federal and state credit carryforwards of $632,000 as of December 31, 2015. The federal credits do not expire, and the state credits expire between 2017 and 2028.
As a result of the successful IPO, reduction in interest expense, and continued growth and successful integration and synergies achieved from the Symbion acquisition, the Company released substantially all of the valuation allowance that was recorded against its deferred tax assets. Based on the Company's analysis of these and other items, it was determined that it is more likely than not that substantially all of the deferred tax assets will be realized. Therefore, the Company reduced its valuation allowance by approximately $136.0 million.
The Company has recorded a valuation allowance against its deferred tax assets at December 31, 2015 and 2014 totaling $6.9 million and $142.9 million, respectively. The valuation allowance continues to be provided for certain deferred tax assets for which the Company believes it is more likely than not that the tax benefits will not be realized, which are primarily certain state net operating losses and capital loss carryforwards.
Included in the decrease in the valuation allowance for the year ended December 31, 2015 was an increase of approximately $1.5 million that was recorded to additional-paid-in-capital as the result of the tax effect of the disposals of shares of noncontrolling interests. Finally, approximately $2.1 million of the valuation allowance as of December 31, 2015 is recorded against deferred tax assets that, if subsequently recognized, will be credited directly to contributed capital.
F-28
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
A reconciliation of the beginning and ending liability for gross unrecognized tax benefits for the years ended December 31, 2015 and 2014 is as follows (in thousands):
Year Ended December 31, | ||||||||
2015 | 2014 | |||||||
Unrecognized tax benefits at beginning of year | $ | 2,755 | $ | — | ||||
Additions for tax positions acquired from Symbion | — | 1,766 | ||||||
Additions based on tax provisions related to the current year | — | 66 | ||||||
Additions for tax positions of prior years | 136 | 923 | ||||||
Reductions for tax positions of prior year | (996 | ) | ||||||
Settlements | (492 | ) | ||||||
Unrecognized tax benefits at end of year | $ | 1,403 | $ | 2,755 | ||||
The Company recognizes interest and penalties related to uncertain tax positions in its provision for income taxes in the consolidated statements of operations. For the years ended December 31, 2015 and 2014, the Company had approximately $322,000 and $357,000, respectively, of accrued interest and penalties related to uncertain tax positions. The total amount of accrued liabilities related to uncertain tax positions that would affect the Company's effective tax rate, if recognized, is $548,000 as of December 31, 2015. The reserves are included in long-term taxes payable and long-term deferred tax assets in the consolidated balance sheet as of December 31, 2015.
In February 2015, the Company settled the IRS audit of the Company's federal income tax returns for the years ended December 31, 2010 and 2011. In March 2015, the Company settled the IRS audit of the Company's federal income tax returns for the year ended December 31, 2012. The Company's U.S. federal income tax returns for tax years 2012 and beyond remain subject to examination. The Company's state income tax returns for tax years 2011 and beyond remain subject to examination.
11. Equity-Based Compensation
Prior to the Reorganization, the Surgery Center Holdings, LLC’s ("Holdings LLC") Amended and Restated Limited Liability Company Agreement, dated December 24, 2009, provided, from time to time, as approved by the Holdings LLC's Board, for the issuance of a subordinate class of the Holdings LLC's nonvoting membership units to certain key persons, as defined, of the Company or its subsidiaries.
In April 2013, the Company modified the terms of the 2010 awards to allow for additional vesting in 2013 of its share-based awards with time-vesting conditions. In November 2014, the Holdings LLC issued to certain executives of Symbion, Inc. who became employees of the Company following the Company’s acquisition of Symbion an additional 1,300,000 unvested B-Units, which are subject to vesting conditions to occur through November 2019.
Prior to the Reorganization, in the event of employee termination, the B-Units were subject to a 90-day repurchase option. Upon termination, all unvested B-Units were effectively forfeited. If the employee was terminated for cause, as defined, or resigned prior to the expiration of certain tenure periods specified in such employee’s agreement, the repurchase price for each vested B-Unit was zero, and was deemed automatically repurchased by the Company. The repurchase price for vested B-Units, should the Company elect to exercise the repurchase option, was at fair market value, as defined. If the Company did not exercise the repurchase option, the employee owned the vested B-Units pursuant to the Holdings LLC's LLC Agreement, which included restrictions on transfer, among other provisions. The fair value of each Holdings LLC issued B-Unit was estimated on the date of grant.
In September 2015, the Company adopted the Surgery Partners, Inc. 2015 Omnibus Incentive Plan ("2015 Omnibus Incentive Plan") from which all equity-based awards will be granted. Under this plan, the Company can grant stock options, SARs, restricted stock, unrestricted stock, stock units, performance awards, cash awards and other awards convertible into or otherwise based on shares of its common stock. As of December 31, 2015, 4,815,700 shares were authorized to be granted under the 2015 Omnibus Incentive Plan and 4,807,212 were available for future equity grants.
Equity Valuation
In applying the Black-Scholes-Merton option pricing model, the Company used the following assumptions:
▪ Risk-free interest rate. The risk-free interest rate is used as a component of the fair value of stock options to take into account the time value of money. For the risk-free interest rate, the Company uses the implied yield on United States Treasury zero-coupon issues with a remaining term equal to the expected life, in years, of the options granted.
▪ Expected volatility. Volatility, for the purpose of share-based compensation, is a measurement of the amount that a share price has fluctuated. Expected volatility involves reviewing historical volatility and determining what, if any, change the share price will have in the future. The Company used historical stock price information of certain peer group companies for a period of time equal to the expected option life period to determine estimated volatility.
F-29
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
▪ Expected life, in years. A clear distinction is made between the expected life of an option and the contractual term of the option. The expected life of an option is considered the amount of time, in years, that an option is expected to be outstanding before it is exercised. Whereas, the contractual term of the stock option is the term an option is valid before it expires.
▪ Expected dividend yield. Since issuing dividends will affect the fair value of a stock option, GAAP requires companies to estimate future dividend yields or payments. The Company has not historically issued dividends and does not intend to issue dividends in the future. As a result, the Company does not apply a dividend yield component to its valuation.
The following table sets forth the assumptions used by the Company to estimate the fair value of options granted under the 2015 Omnibus Incentive Plan:
Expected volatility | 29% - 38% | |||
Risk-free interest rate | 0.90% - 1.36% | |||
Expected dividends | — | |||
Average expected term (years) | 3.00 | |||
Fair value of stock options granted | $ | 4.83 | ||
The estimated fair value of options is amortized to expense on a straight-line basis over the options’ vesting period.
Stock Option Activity
A summary of stock option activity during the year ended December 31, 2015 is as follows:
Units | Weighted Average Exercise Price | Weighted Average Remaining Contractual Term (years) | |||||||
Outstanding at December 31, 2014 | — | ||||||||
Granted | 8,488 | $ | 20.03 | 3.0 | |||||
Exercised | — | ||||||||
Forfeited | — | ||||||||
Outstanding at December 31, 2015 (1) | 8,488 | $ | 20.03 | 3.0 | |||||
(1) Of the outstanding options, none were exercisable as of December 31, 2015.
F-30
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
Restricted Share Activity
All units and per unit amounts in these consolidated financial statements and notes to the consolidated financial statements reflect the Reorganization that occurred in September 2015 (see Note 1). A summary of Holdings LLC issued restricted stock activity for the years ended December 31, 2015, 2014, and 2013 follows:
Total Shares | Vested Shares | Unvested Shares | Weighted-Average Grant Fair Value | ||||||||||
Outstanding at January 1, 2013 | 3,234,664 | 1,245,510 | 1,989,154 | $0.81 | |||||||||
Granted | — | — | — | — | |||||||||
Forfeited/Terminated | — | — | — | — | |||||||||
Purchased | — | — | — | — | |||||||||
Vested | — | 543,270 | (543,270 | ) | 0.83 | ||||||||
Outstanding at December 31, 2013 | 3,234,664 | 1,788,780 | 1,445,884 | $0.81 | |||||||||
Granted | 583,404 | — | 583,404 | 6.44 | |||||||||
Forfeited/Terminated | (127,582 | ) | — | (127,582 | ) | 1.27 | |||||||
Purchased | (803,336 | ) | (803,336 | ) | — | 3.64 | |||||||
Vested | — | 659,641 | (659,641 | ) | 1.43 | ||||||||
Outstanding at December 31, 2014 | 2,887,150 | 1,645,085 | 1,242,065 | $1.96 | |||||||||
Granted | 569,114 | — | 569,114 | 6.31 | |||||||||
Forfeited/Terminated | — | — | — | — | |||||||||
Purchased | (11,742 | ) | (11,742 | ) | — | 6.31 | |||||||
Vested | — | 1,643,525 | (1,643,525 | ) | 3.79 | ||||||||
Outstanding at December 31, 2015 | 3,444,522 | 3,276,868 | 167,654 | $2.53 | |||||||||
At December 31, 2015, unrecognized compensation cost related to unvested shares was approximately $1.1 million. Unrecognized compensation cost will be expensed annually based on the number of shares that vest during the year.
In 2015, 2014, and 2013, the Company terminated zero, 128,000 and zero unvested shares, respectively, related to the termination of employment of executives.
The Company recorded compensation expense of $7.5 million, $942,000, and $455,000 to recognize the fair value of the restricted shares that vested and stock options granted through December 31, 2015, 2014, and 2013, respectively. In connection with the IPO, 1,632,626 restricted shares immediately vested which resulted in accelerated vesting of $6.2 million which is included within the $7.5 million of equity-based compensation expense for the year ended December 31, 2015.
12. Employee Benefit Plans
Surgery Partners 401(k) Plan
The Surgery Partners 401(k) Plan is a defined contribution plan whereby certain employees who have completed at least one month of service, including at least one hour of service during that period of time, are eligible to participate. Employees may enroll in the plan immediately upon completion of the minimum service requirement. The Surgery Partners 401(k) Plan allows eligible employees to make contributions of varying percentages or flat dollar amounts of their annual compensation, up to the maximum allowable amounts by the Internal Revenue Service ("IRS"). Eligible employees may or may not receive a match by the Company of their contributions. Employee salary deferrals exceeding six percent of annual compensation are ineligible for a Company matching contribution. Employer contributions vest 20% after one year of service and continue vesting at 20% per year until fully vested.
Symbion, Inc. 401(k) Plan
In connection with the Symbion acquisition, the Company acquired and continues to maintain the Symbion, Inc. 401(k) Plan on behalf of certain former employees of Symbion. The Symbion, Inc. 401(k) Plan is a defined contribution plan whereby employees who have completed six months of service and are age 21 or older are eligible to participate. Employees may enroll in the plan on either January 1 or July 1 of each year. The 401(k) Plan allows eligible employees to make contributions of varying percentages of their annual compensation, up to the maximum allowable amounts by the IRS. Eligible employees may or may not receive a match by the Company of their contributions. The Company match varies depending on location and is determined prior to the start of each plan year. Generally, employer contributions vest 20% after two years of service and continue vesting at 20% per year until fully vested.
F-31
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
The Company's matching contribution expense for both the Surgery Partners 401(k) Plan and the Symbion, Inc. 401(k) Plan for the years ended December 31, 2015, 2014 and 2013 was $2.2 million, $754,000 and $516,000, respectively.
Supplemental Executive Retirement Savings Plan
In connection with the Symbion acquisition, the Company acquired and continues to maintain a supplemental executive retirement savings plan (the "SERP") for certain former Symbion executives. The SERP provides supplemental retirement savings alternatives to eligible officers and key employees of the Company by allowing participants to defer portions of their compensation. Under the SERP, eligible employees may enroll in the plan before December 31 to be entered in the plan the following year. Eligible employees may defer into the SERP up to 25% of their normal period payroll and up to 50% of their annual bonus. If the enrolled employee contributes a minimum of 2% of his or her base salary into the SERP, the Company will contribute 2% of the enrolled employee’s base salary to the plan and has the option of contributing additional amounts. Periodically, the enrolled employee’s deferred amounts are transferred to a plan administrator. The plan administrator maintains separate non-qualified accounts for each enrolled employee to track deferred amounts. On May 1 of each year, the Company is required to make its contribution to each enrolled employee’s account. See Note 2 on Significant Accounting Policies for information about the fair value of the assets and liabilities in the SERP.
13. Related Party Transactions
On December 24, 2009, the Company and Bayside Capital, Inc. (or "Bayside"), an affiliate of H.I.G. Capital, LLC (or "H.I.G."), entered into a Management and Investment Advisory Services Agreement ("Management Agreement") pursuant to which the Company will receive certain management, consulting and financial advisory services. Effective May 4, 2011, the Management Agreement was amended pursuant to the NovaMed merger and the management fee was increased to $2.0 million annually. The Company recognized $2.0 million for the year ended December 31, 2013 related to the Management Agreement. Effective November 3, 2014, the Management Agreement was amended pursuant to the Symbion acquisition and the management fee was increased to $3.0 million annually. Fees related to the Management Agreement for the years ended December 31, 2015, 2014 and 2013 are recognized as general and administrative expense in the accompanying consolidated statements of operations. Additionally, the Company incurred additional advisory fees related to refinancing transactions of $17.6 million and $2.7 million for the years ended December 31, 2014 and 2013 respectively. During the year ended December 31, 2015, Bayside was paid a transaction fee pursuant to the Management Agreement of $5.4 million as a result of the IPO and the Management Agreement was terminated upon the completion of the IPO.
14. Commitments and Contingencies
Lease and Debt Guarantees of Non-Consolidated Facilities
As of December 31, 2015 and 2014, the Company had guaranteed approximately $160,000 and $539,000, respectively, of operating lease payments for certain non-consolidated surgical facilities that were acquired in connection with the Symbion transaction. These operating leases typically have ten-year terms, with optional renewal periods.
Professional, General and Workers' Compensation Liability Risks
The Company is subject to claims and legal actions in the ordinary course of business, including claims relating to patient treatment, employment practices and personal injuries. To cover these claims, the Company maintains general liability and professional liability insurance in excess of self-insured retentions through third party commercial insurance carriers in amounts that management believes is sufficient for the Company's operations, although, potentially, some claims may exceed the scope of coverage in effect. The professional and general insurance coverage is on a claims-made basis. Workers' compensation insurance is on an occurrence basis. Plaintiffs in these matters may request punitive or other damages that may not be covered by insurance. The Company is not aware of any such proceedings that would have a material adverse effect on the Company's business, financial condition or results of operations.
Laws and Regulations
Laws and regulations governing the Company's business, including those relating to the Medicare and Medicaid programs, are complex and subject to interpretation. These laws and regulations govern every aspect of how the Company's surgical facilities conduct their operations, from licensing requirements to how and whether the Company's facilities may receive payments pursuant to the Medicare and Medicaid programs. Compliance with such laws and regulations can be subject to future government agency review and interpretation as well as legislative changes to such laws. Noncompliance with such laws and regulations may subject the Company to significant regulatory action including fines, penalties, and exclusion from the Medicare, Medicaid and other federal healthcare programs. From time to time, governmental regulatory agencies will conduct inquiries of the Company's practices, including, but not limited to, the Company's compliance with federal and state fraud and abuse laws, billing practices and relationships with physicians. It is the Company's current practice and future intent to cooperate fully with such inquiries. The Company is not aware of any such inquiry that would have a material adverse effect on the Company's business, financial condition, or results of operations.
F-32
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
Acquired Facilities
The Company, through its wholly-owned subsidiaries or controlled partnerships and limited liability companies, has acquired and will continue to acquire surgical facilities with prior operating histories. Such facilities may have unknown or contingent liabilities, including liabilities for failure to comply with healthcare laws and regulations, such as billing and reimbursement, fraud and abuse and similar anti-referral laws. Although the Company attempts to assure that no such liabilities exist, obtain indemnification from prospective sellers covering such matters and institute policies designed to conform centers to its standards following completion of acquisitions, there can be no assurance that the Company will not become liable for past activities that may later be asserted to be improper by private plaintiffs or government agencies. There can be no assurance that any such matter will be covered by indemnification or, if covered, that the liability sustained will not exceed contractual limits or the financial capacity of the indemnifying party.
The Company cannot predict whether federal or state statutory or regulatory provisions will be enacted that would prohibit or otherwise regulate relationships which the Company has established or may establish with other healthcare providers or have materially adverse effects on its business or revenues arising from such future actions. Management believes, however, that it will be able to adjust the Company's operations so as to be in compliance with any statutory or regulatory provision as may be applicable.
Potential Physician Investor Liability
A majority of the physician investors in the partnerships and limited liability companies which operate the Company's surgical facilities carry general and professional liability insurance on a claims-made basis. Each partnership or limited liability company may, however, be liable for damages to persons or property arising from occurrences at the surgical facilities. Although the various physician investors and other surgeons generally are required to obtain general and professional liability insurance with tail coverage that extends beyond the period of any claims-made policies, such individuals may not be able to obtain coverage in amounts sufficient to cover all potential liability. Since most insurance policies contain exclusions, the physician investors will not be insured against all possible occurrences. In the event of an uninsured or underinsured loss, the value of an investment in the partnership interests or limited liability company membership units and the amount of distributions could be adversely affected.
Contingent Consideration
Pursuant to a purchase agreement dated December 24, 2009 (“the Purchase Agreement”), the Company acquired controlling interests in thirty-six business entities in various Florida locations which operate freestanding ASCs and provided anesthesia and pain management services (“the 2009 Acquisition”). Non-controlling interests in the ASCs were owned by certain physicians that remained partners/members in the ASCs and other operating entities.
The Purchase Agreement provided for maximum potential contingent consideration of up to $10.0 million based on operating results subsequent to the acquisition for the period from January 1, 2010 to December 31, 2010. Pursuant to the Purchase Agreement, the contingent consideration is payable as principal under a Subordinated Promissory Note, the form of which was delivered concurrent with the Purchase Agreement. The balance is still outstanding due to ongoing litigation as a result of the civil claim discussed in detail below. The Subordinated Promissory Note bears interest at 8% and during the years ended December 31, 2015 and 2014, the Company recorded approximately $1.0 million of interest expense related to the note. As discussed below, the Company has made indemnification claims against the Seller exceeding the amount of the contingent consideration liability. The Company has a contractual right of offset against the contingent consideration. The fair value of the contingent consideration liability, including accrued interest, as of December 31, 2015 and 2014 was $14.0 million and $13.0 million, respectively.
In conjunction with the 2009 Acquisition, an escrow account in the amount of $2.9 million was created to cover any contingencies. With the formation of this escrow account, the Company was indemnified against certain indemnification obligations. In 2010, $589,000 was paid to the Company in settlement of the acquisition price adjustment noted above. In December 2010, the Company filed an indemnification claim against the Seller alleging breaches of and inaccuracies in representations and warranties included in the Purchase Agreement. Pursuant to the Purchase Agreement, the escrow agent has not paid the remaining escrow funds due to the unresolved claim associated with this acquisition.
Pursuant to the terms of the Purchase Agreement, in December 2010, the Company filed a claim for indemnification from the Seller for reimbursement of amounts to be repaid to payors for overpayment amounts received by the Seller prior to the date of acquisition, including other losses sustained, and submitted a withdrawal notice to the escrow agent in the amount of approximately $4.4 million. The indemnification claim asserts, among other allegations, that certain operating entities acquired from the Seller improperly recorded payments received from certain payors as income and that one acquired entity used improper billing, coding and collection practices for dates of service prior to acquisition date. The Seller submitted an objection to this claim and filed a civil claim requesting the court to dismiss the Company’s claim and release funds out of escrow.
The Company has included in the accompanying consolidated balance sheets a net indemnification receivable due from Seller of $1.1 million as of December 31, 2015 and 2014 pursuant to the terms of the Purchase Agreement. The amount due to the payors of approximately $1.8 million is included in accrued expenses in the accompanying consolidated balance sheets as of December 31, 2015 and 2014.
Subsequent to the acquisition date, the Company determined the acquired accounts receivable were not properly recorded at the net realizable value of the asset. The Company determined the fair value assigned in the initial acquisition accounting resulted in accounts receivable being recorded at an amount which was approximately $14.0 million in excess of the fair value. On June 10, 2013, the court issued a judgment in favor of the Company regarding its indemnification claim and its claim regarding the overstatement of accounts receivable. Specifically, the court ruled that the Company is entitled to recover approximately $454,000 for the indemnification claims which represents the amount
F-33
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
of the original claim less the application of deductibles. The court also ruled that the Company is entitled to receive approximately $10.8 million for the overstated net accounts receivable. The Purchase Agreement provides for any award of damages to the Company to be offset first by the money in the escrow account and then by an offset to the contingent consideration. Therefore, the court ordered that the funds in the escrow account be paid to the Company and the balance of approximately $8.3 million be offset against the $10.0 million contingent consideration. To date, no final judgment has been made regarding the award of attorneys’ fees and interest.
Following the judgment noted above, an appeal was filed by the Seller and the outcome of the appeal is still pending. The funds from the escrow account have not been released to the Company and the Company has retained the contingent consideration liability on its consolidated balance sheets at December 31, 2015 and 2014.
15. Segment Reporting
A public company is required to report annual and interim financial and descriptive information about its reportable operating segments. Operating segments, as defined, are components of an enterprise about which separate financial information is available that is evaluated regularly by the chief operating decision maker, or "CODM," in deciding how to allocate resources and in assessing performance.
The Company operates in three major lines of business that are also the Company's reportable operating segments - the operation of surgical facilities, the operation of optical services and the operation of ancillary services, which includes physician practices, a diagnostic laboratory and a specialty pharmacy.
During the three months ended June 30, 2015, the Company made changes to its internal reports issued to and reviewed by the CODM.
The primary effect of these changes was to remove the allocation of general and administrative expense and assets to the reportable operating segments. The Company has revised the segment disclosures below to present corporate overhead and corporate assets as a reconciling item back to the reported consolidated financial information.
The following tables present financial information for each reportable segment (in thousands):
Year Ended December 31, | ||||||||||||
2015 | 2014 | 2013 | ||||||||||
Net Revenues: | ||||||||||||
Surgical facility services | $ | 884,144 | $ | 339,309 | $ | 224,578 | ||||||
Ancillary services | 61,175 | 49,787 | 44,103 | |||||||||
Optical services | 14,572 | 14,193 | 15,918 | |||||||||
Total revenues | $ | 959,891 | $ | 403,289 | $ | 284,599 | ||||||
Year Ended December 31, | ||||||||||||
2015 | 2014 | 2013 | ||||||||||
Segment Operating Income: | ||||||||||||
Surgical facility services | $ | 224,098 | $ | 112,237 | $ | 77,905 | ||||||
Ancillary services | 15,666 | 16,389 | 16,909 | |||||||||
Optical services | 2,283 | 2,238 | 3,032 | |||||||||
Total | $ | 242,047 | $ | 130,864 | $ | 97,846 | ||||||
General and administrative | $ | (59,534 | ) | $ | (33,149 | ) | $ | (27,275 | ) | |||
Gain (loss) on disposal or impairment of long-lived assets, net | 2,097 | (1,804 | ) | (2,482 | ) | |||||||
Loss on debt extinguishment | (16,102 | ) | (23,414 | ) | (9,863 | ) | ||||||
Merger transaction and integration costs | (17,920 | ) | (21,690 | ) | — | |||||||
Termination of management agreement and IPO costs | (5,834 | ) | — | $ | — | |||||||
Total operating income | $ | 144,754 | $ | 50,807 | $ | 58,226 | ||||||
F-34
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
Year Ended December 31, | ||||||||||||
2015 | 2014 | 2013 | ||||||||||
Supplemental Information: | ||||||||||||
Depreciation and amortization: | ||||||||||||
Surgical facility services | $ | 27,447 | $ | 9,911 | $ | 7,405 | ||||||
Ancillary services | 1,934 | 1,812 | 1,460 | |||||||||
Optical services | 1,622 | 1,641 | 1,862 | |||||||||
Total | $ | 31,003 | $ | 13,364 | $ | 10,727 | ||||||
General and administrative | $ | 3,542 | $ | 1,697 | $ | 936 | ||||||
Total depreciation and amortization | $ | 34,545 | $ | 15,061 | $ | 11,663 | ||||||
December 31, | ||||||||
2015 | 2014 | |||||||
Assets: | ||||||||
Surgical facility services | $ | 1,762,396 | $ | 1,638,874 | ||||
Ancillary services | 118,198 | 70,370 | ||||||
Optical services | 25,537 | 25,876 | ||||||
Total | 1,906,131 | 1,735,120 | ||||||
General and administrative | $ | 200,553 | $ | 123,674 | ||||
Total assets | $ | 2,106,684 | $ | 1,858,794 | ||||
Year Ended December 31, | ||||||||||||
2015 | 2014 | 2013 | ||||||||||
Supplemental Information: | ||||||||||||
Cash purchases of property and equipment, net: | ||||||||||||
Surgical facility services | $ | 26,723 | $ | 5,158 | $ | 2,301 | ||||||
Ancillary services | 1,051 | 1,034 | 562 | |||||||||
Optical services | 128 | 335 | 161 | |||||||||
Total | $ | 27,902 | $ | 6,527 | $ | 3,024 | ||||||
General and administrative | $ | 5,537 | $ | 1,209 | $ | 1,126 | ||||||
Total cash purchases of property and equipment, net | $ | 33,439 | $ | 7,736 | $ | 4,150 | ||||||
16. Quarterly Financial Information (Unaudited)
The following tables include a summary of certain information related to the Company's quarterly consolidated results of operations for each of the four quarters in the years ended December 31, 2015 and 2014. The amounts are as follows (in thousands and unaudited):
Fiscal Quarter | |||||||||||
1Q15 | 2Q15 | 3Q15 | 4Q15 | ||||||||
Revenues | 224,143 | 232,827 | 239,599 | 263,322 | |||||||
Cost of revenues | 155,773 | 161,558 | 168,821 | 183,174 | |||||||
Net income | 10,488 | 12,479 | 13,784 | 36,094 | |||||||
Net income attributable to non-controlling interests | (17,250 | ) | (17,905 | ) | (16,906 | ) | (19,355 | ) | |||
Net income (loss) attributable to Surgery Partners, Inc. | (6,762 | ) | (5,426 | ) | (3,122 | ) | 16,739 | ||||
Basic net loss per share of common stock | (0.21 | ) | (0.17 | ) | (0.10 | ) | 0.35 | ||||
Diluted net loss per share common stock | (0.21 | ) | (0.17 | ) | (0.10 | ) | 0.35 | ||||
F-35
SURGERY PARTNERS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS – CONTINUED
Fiscal Quarter | |||||||||||
1Q14 | 2Q14 | 3Q14 | 4Q14 | ||||||||
Revenues | 70,480 | 76,815 | 76,303 | 179,691 | |||||||
Cost of revenues | 43,050 | 45,164 | 45,377 | 120,587 | |||||||
Net income (loss) | 2,258 | 7,025 | 430 | (36,765 | ) | ||||||
Net income attributable to non-controlling interests | (6,377 | ) | (7,631 | ) | (7,338 | ) | (17,499 | ) | |||
Net income (loss) attributable to Surgery Partners, Inc. | (4,119 | ) | (606 | ) | (6,908 | ) | (54,264 | ) | |||
Basic net loss per share of common stock | (0.13 | ) | (0.02 | ) | (0.22 | ) | (1.69 | ) | |||
Diluted net loss per share common stock | (0.13 | ) | (0.02 | ) | (0.22 | ) | (1.69 | ) | |||
17. Subsequent Events
A portion of the purchase price related to an acquisition in December 2015 was placed in escrow upon satisfaction of a contingency. The contingency was settled in February 2016 and as a result, the Company received $8.0 million. The $8.0 million is recorded on the accompanying balance sheet as of December 31, 2015 within prepaid expenses and other current assets and the purchase price allocation was adjusted to reflect this change.
Effective February 1, 2016, the Company acquired an ASC in Colorado Springs, Colorado for a purchase price of $3.9 million which was funded from proceeds from the Revolver. The operations of the ASC were merged into an existing in-market ASC.
F-36
SIGNATURES
Pursuant to the requirements of Section 13 or 15(d) of the Securities Exchange Act of 1934, the Registrant has duly caused this report to be signed on its behalf by the undersigned, thereunto duly authorized.
SURGERY PARTNERS, INC. | |
By: | /s/ Michael T. Doyle Michael T. Doyle Chief Executive Officer (Principal Executive Officer) |
Date: March 11, 2016
Pursuant to the requirements of the Securities Exchange Act of 1934, this report has been signed below by the following persons on behalf of the registrant and in the capacities and on the dates indicated.
SIGNATURES | TITLE | DATE |
Chief Executive Officer, Director (Principal Executive Officer) | March 11, 2016 | |
/s/ Michael T. Doyle | ||
Michael T. Doyle | ||
Executive Vice President, Chief Financial Officer (Principal Financial and Accounting Officer) | March 11, 2016 | |
/s/ Teresa F. Sparks | ||
Teresa F. Sparks | ||
Chairman | March 11, 2016 | |
/s/ Christopher Laitala | ||
Christopher Laitala | ||
Director | March 11, 2016 | |
/s/ Adam Feinstein | ||
Adam Feinstein | ||
Director | March 11, 2016 | |
/s/ Matthew I. Lozow | ||
Matthew I. Lozow | ||
Director | March 11, 2016 | |
/s/ Brent Turner | ||
Brent Turner | ||
F-37
EXHIBIT INDEX
No. | Description | |
3.1 | Amended and Restated Certificate of Incorporation (incorporated herein by reference to Exhibit 3.1 to the Company's Quarterly Report on Form 10-Q filed November 13, 2015). | |
3.2 | Amended and Restated By-Laws (incorporated herein by reference to Exhibit 3.2 to the Company's Quarterly Report on Form 10-Q filed November 13, 2015). | |
10.1 | Tax Receivable Agreement, dated as of September 30, 2015, among Surgery Partners, Inc., H.I.G. Surgery Centers, LLC and certain other Stockholders party thereto (incorporated herein by reference to Exhibit 10.1 to the Company's Quarterly Report on Form 10-Q filed November 13, 2015). | |
10.2 | Registration Rights Agreement, dated as of September 30, 2015, among Surgery Partners, Inc. and certain other Stockholders party thereto (incorporated herein by reference to Exhibit 10.2 to the Company's Quarterly Report on Form 10-Q filed November 13, 2015). | |
10.3 | Reorganization Agreement, dated as of September 30, 2015, among Surgery Partners, Inc., Surgery Center Holdings, LLC, H.I.G. Surgery Centers, LLC and certain other Members party thereto (incorporated herein by reference to Exhibit 10.3 to the Company's Quarterly Report on Form 10-Q filed November 13, 2015). | |
10.4 | Form of Indemnification Agreement (incorporated herein by reference to Exhibit 10.14 to the Company's Registration Statement on Form S-1, Amended, filed September 14, 2015). | |
10.5 | First Lien Credit Agreement, dated as of November 3, 2014, among SP Holdco I, Inc., Surgery Center Holdings, Inc., Jefferies Finance LLC and the other guarantors and lenders party thereto (incorporated herein by reference to Exhibit 10.5 to the Company's Registration Statement on Form S-1 filed August 17, 2015). | |
10.6 | First Lien Incremental Amendment to First Lien Credit Agreement, dated as of October 7, 2015, among SP Holdco I, Inc., Surgery Center Holdings, Inc., Jefferies Finance LLC and the other guarantors and lenders party thereto (incorporated herein by reference as Exhibit 10.1 to Surgery Partners, Inc.’s Current Report on Form 8-K filed October 9, 2015) | |
10.7 | Second Lien Credit Agreement, dated as of November 3, 2014, among SP Holdco I, Inc., Surgery Center Holdings, Inc., Jefferies Finance LLC and the other guarantors and lenders party thereto (incorporated herein by reference to Exhibit 10.6 to the Company's Registration Statement on Form S-1 filed August 17, 2015). | |
10.8 | Management and Investment Advisory Services Agreement, dated as of December 24, 2009, by and among Bayside Capital, Inc., Surgery Center Holdings, Inc. and certain of its subsidiaries (incorporated herein by reference to Exhibit 10.2 to the Company's Registration Statement on Form S-1 filed August 17, 2015). | |
10.9 | First Amendment to Management and Investment Advisory Services Agreement, dated as of May 4, 2011, by and among Bayside Capital, Inc., Surgery Center Holdings, Inc. and certain of its subsidiaries (incorporated herein by reference to Exhibit 10.3 to the Company's Registration Statement on Form S-1 filed August 17, 2015). | |
10.10 | Second Amendment to Management and Investment Advisory Services Agreement, dated as of November 3, 2014, by and among Bayside Capital, Inc., Surgery Center Holdings, Inc. and certain of its subsidiaries (incorporated herein by reference to Exhibit 10.4 to the Company's Registration Statement on Form S-1 filed August 17, 2015). | |
10.11 | Assignment and Acceptance Agreement, among H.I.G. Surgery Centers, LLC and THL Credit, Inc., for assignment effective April 11, 2013 (incorporated herein by reference to Exhibit 10.7 to the Company's Registration Statement on Form S-1 filed August 17, 2015). | |
10.12 (a) | Employment Agreement of Michael Doyle, as amended (incorporated herein by reference to Exhibit 10.10 to the Company's Registration Statement on Form S-1, Amended, filed September 21, 2015). | |
10.13 (a) | Employment Agreement of Teresa Sparks, as amended (incorporated herein by reference to Exhibit 10.11 to the Company's Registration Statement on Form S-1, Amended, filed September 21, 2015). | |
10.14 (a) | Employment Agreement of John Crysel, as amended (incorporated herein by reference to Exhibit 10.12 to the Company's Registration Statement on Form S-1, Amended, filed September 21, 2015). | |
10.15 (a) | 2015 Omnibus Incentive Plan (incorporated herein by reference as Exhibit 4.3 to the Company's Registration Statement on Form S-8 filed October 6, 2015). | |
10.16 (a) | Form of Reorganization Restricted Stock Award under the 2015 Omnibus Incentive Plan (incorporated herein by reference to Exhibit 10.5 to the Company's Quarterly Report on Form 10-Q filed November 13, 2015). | |
10.17 (a) | Form of Director Option Award under the 2015 Omnibus Incentive Plan (incorporated herein by reference to Exhibit 10.6 to the Company's Quarterly Report on Form 10-Q filed November 13, 2015). | |
10.18 (a) | Form of Restricted Stock Agreement under the 2015 Omnibus Incentive Plan (incorporated herein by reference to Exhibit 10.7 to the Company's Quarterly Report on Form 10-Q filed November 13, 2015). | |
10.19 (a) | Cash Incentive Plan (incorporated herein by reference to Exhibit 10.8 to the Company's Quarterly Report on Form 10-Q filed November 13, 2015). | |
10.20 (a) | Symbion, Inc. Supplemental Executive Retirement Plan, Effective May 1, 2005 (incorporated herein by reference to Exhibit 10.17 to the Company's Registration Statement on Form S-1, Amended, filed September 21, 2015). | |
F-38
10.21 | Office Lease Agreement dated November 17, 2015 between Highwoods Realty Limited Partnership and Surgery Partners, Inc. | |
21.1 | List of Subsidiaries of the Registrant | |
23.1 | Consent of Independent Registered Public Accounting Firm- Ernst & Young, LLP | |
23.2 | Consent of Independent Registered Public Accounting Firm- BDO USA, LLP | |
31.1 | Certification of Principal Executive Officer pursuant to Rule 13a-14(a) and Rule 15d-14(a) of the Securities Exchange Act, as amended as adopted pursuant to Section 302 of the Sarbanes-Oxley Act of 2002. | |
31.2 | Certification of Principal Financial Officer pursuant to Rule 13a-14(a) and Rule 15d-14(a) of the Securities Exchange Act, as amended as adopted pursuant to Section 302 of the Sarbanes-Oxley Act of 2002. | |
32.1 | Certification of Chief Executive Officer pursuant to 18 U.S.C. Section 1350, as adopted pursuant to Section 906 of the Sarbanes-Oxley Act of 2002. | |
32.2 | Certification of Chief Financial Officer pursuant to 18 U.S.C. Section 1350, as adopted pursuant to Section 906 of the Sarbanes-Oxley Act of 2002. | |
101.INS | XBRL Instance Document | |
101.SCH | XBRL Taxonomy Extension Schema Document | |
101.CAL | XBRL Taxonomy Extension Calculation Linkbase Document | |
101.DEF | XBRL Taxonomy Extension Definition Linkbase Document | |
101.LAB | XBRL Taxonomy Extension Label Linkbase Document | |
101.PRE | XBRL Taxonomy Extension Presentation Linkbase Document | |
(a) Management Contract or Compensatory Plan or Arrangement.
F-39
