Attached files
| file | filename |
|---|---|
| EX-31.1 - EXHIBIT 31.1 - U S PHYSICAL THERAPY INC /NV | h10034943x1_ex31-1.htm |
| EX-23.1 - EXHIBIT 23.1 - U S PHYSICAL THERAPY INC /NV | h10034943x1_ex23-1.htm |
| EX-31.3 - EXHIBIT 31.3 - U S PHYSICAL THERAPY INC /NV | h10034943x1_ex31-3.htm |
| EX-21.1 - EXHIBIT 21.1 - U S PHYSICAL THERAPY INC /NV | h10034943x1_ex21-1.htm |
| EX-32.1 - EXHIBIT 32.1 - U S PHYSICAL THERAPY INC /NV | h10034943x1_ex32-1.htm |
| EX-31.2 - EXHIBIT 31.2 - U S PHYSICAL THERAPY INC /NV | h10034943x1_ex31-2.htm |
UNITED STATES
SECURITIES AND EXCHANGE COMMISSION
Washington, D.C. 20549
Form 10-K
(Mark One)
| ☑ | ANNUAL REPORT PURSUANT TO SECTION 13 OR 15(d) OF THE SECURITIES EXCHANGE ACT OF 1934 |
FOR THE FISCAL YEAR ENDED DECEMBER 31, 2015
OR
| o | TRANSITION REPORT PURSUANT TO SECTION 13 OR 15(d) OF THE SECURITIES EXCHANGE ACT OF 1934 |
FOR THE TRANSITION PERIOD FROM TO
COMMISSION FILE NUMBER 1-11151
U.S. PHYSICAL THERAPY, INC.
(EXACT NAME OF REGISTRANT AS SPECIFIED IN ITS CHARTER)
|
NEVADA
|
76-0364866
|
|
(STATE OR OTHER JURISDICTION OF INCORPORATION
OR ORGANIZATION) |
(I.R.S. EMPLOYER IDENTIFICATION NO.)
|
|
|
|
|
1300 WEST SAM HOUSTON PARKWAY SOUTH,
SUITE 300, HOUSTON, TEXAS |
77042
|
|
(ADDRESS OF PRINCIPAL EXECUTIVE OFFICES)
|
(ZIP CODE)
|
|
|
|
|
REGISTRANT’S TELEPHONE NUMBER, INCLUDING AREA CODE: (713) 297-7000
SECURITIES REGISTERED PURSUANT TO SECTION 12(b) OF THE EXCHANGE ACT: |
|
|
|
|
|
Title of Each Class
|
Name of Each Exchange on Which Registered
|
|
Common Stock, $.01 par value
|
New York Stock Exchange
|
SECURITIES REGISTERED PURSUANT TO SECTION 12(g) OF THE EXCHANGE ACT: NONE
Indicate by check mark if the registrant is a well-known seasoned issuer, as defined in Rule 405 of the Securities Act. Yes o No ☑
Indicate by check mark if the registrant is not required to file reports pursuant to Section 13 or 15(d) of the Act. Yes o No ☑
Indicate by check mark whether the registrant (1) has filed all reports required to be filed by Section 13 or 15(d) of the Exchange Act during the preceding 12 months (or for such shorter period that the registrant was required to file such reports), and (2) has been subject to such filing requirements for the past 90 days. Yes ☑ No o
Indicate by check mark whether the registrant has submitted electronically and posted on its corporate Website, if any, every Interactive Data File required to be submitted and posted pursuant to Rule 405 of Regulation S-T during the preceding 12 months (or for such shorter period that the registrant was required to submit and post such files). Yes ☑ No o
Indicate by check mark if disclosure of delinquent filers pursuant to Item 405 of Regulation S-K is not contained herein, and will not be contained, to the best of registrant’s knowledge, in definitive proxy or information statements incorporated by reference in Part III of this Form 10-K or any amendment to this Form 10-K. ☑
Indicate by check mark whether the registrant is a large accelerated filer, an accelerated filer, a non-accelerated filer, or a smaller reporting company. See the definitions of “large accelerated filer,” “accelerated filer” and “smaller reporting company” in Rule 12b-2 of the Exchange Act.
|
Large accelerated filer
|
o
|
Accelerated filer
|
☑
|
|
Non-accelerated filer
|
o (Do not check if a smaller reporting company)
|
Smaller reporting company
|
o
|
Indicate by check mark whether the registrant is a shell company (as defined in Rule 12b-2 of the Exchange Act). Yes o No ☑
The aggregate market value of the shares of the registrant’s common stock held by non-affiliates of the registrant at June 30, 2015 was $467,032,000 based on the closing sale price reported on the NYSE for the registrant’s common stock on June 30, 2015, the last business day of the registrant’s most recently completed second fiscal quarter. For purposes of this computation, all executive officers, directors and 5% or greater beneficial owners of the registrant were deemed to be affiliates. Such determination should not be deemed an admission that such executive officers, directors and beneficial owners are, in fact, affiliates of the registrant.
As of March 4, 2016, the number of shares outstanding of the registrant’s common stock, par value $.01 per share, was: 12,498,126.
DOCUMENTS INCORPORATED BY REFERENCE
|
DOCUMENT
|
PART OF FORM 10-K
|
|
Portions of Definitive Proxy Statement for the 2016 Annual Meeting of Shareholders
|
PART III
|
FORWARD-LOOKING STATEMENTS
We make statements in this report that are considered to be forward-looking statements within the meaning given such term under Section 21E of the Securities Exchange Act of 1934, as amended (the “Exchange Act”). These statements contain forward-looking information relating to the financial condition, results of operations, plans, objectives, future performance and business of our Company. These statements (often using words such as “believes”, “expects”, “intends”, “plans”, “appear”, “should” and similar words) involve risks and uncertainties that could cause actual results to differ materially from those we project. Included among such statements are those relating to opening new clinics, availability of personnel and the reimbursement environment. The forward-looking statements are based on our current views and assumptions and actual results could differ materially from those anticipated in such forward-looking statements as a result of certain risks, uncertainties, and factors, which include, but are not limited to:
| • | changes as the result of government enacted national healthcare reform; |
| • | changes in Medicare rules and guidelines and reimbursement or failure of our clinics to maintain their Medicare certification status; |
| • | revenue we receive from Medicare and Medicaid being subject to potential retroactive reduction; |
| • | business and regulatory conditions including federal and state regulations; |
| • | governmental and other third party payor inspections, reviews, investigations and audits; |
| • | compliance with federal and state laws and regulations relating to the privacy of individually identifiable patient information, and associated fines and penalties for failure to comply; |
| • | possible legal actions; which could subject us to increased operating costs and uninsured liabilities; |
| • | changes in reimbursement rates or payment methods from third party payors including government agencies and deductibles and co-pays owed by patients; |
| • | revenue and earnings expectations; |
| • | general economic conditions; |
| • | availability and cost of qualified physical therapists; |
| • | personnel productivity and retaining key personnel; |
| • | competitive, economic or reimbursement conditions in our markets which may require us to reorganize or close certain clinics and thereby incur losses and/or closure costs including the possible write-down or write-off of goodwill and other intangible assets; |
| • | acquisitions, purchase of non-controlling interests (minority interests) and the successful integration of the operations of the acquired businesses; |
| • | maintaining adequate internal controls; |
| • | maintaining necessary insurance coverage; |
| • | availability, terms, and use of capital; and |
| • | weather and other seasonal factors. |
Many factors are beyond our control. Given these uncertainties, you should not place undue reliance on our forward-looking statements. Please see the other sections of this report and our other periodic reports filed with the Securities and Exchange Commission (the “SEC”) for more information on these factors. Our forward-looking statements represent our estimates and assumptions only as of the date of this report. Except as required by law, we are under no obligation to update any forward-looking statement, regardless of the reason the statement is no longer accurate.
1
PART I
GENERAL
Our company, U.S. Physical Therapy, Inc. (the “Company”), through its subsidiaries, operates outpatient physical therapy clinics that provide pre-and post-operative care and treatment for orthopedic-related disorders, sports-related injuries, preventative care, rehabilitation of injured workers and neurological-related injuries. We primarily operate through subsidiary clinic partnerships in which we generally own a 1% general partnership interest and a 49% through 94% limited partnership interest and the managing therapist(s) of the clinics owns the remaining limited partnership interest in the majority of the clinics (hereinafter referred to as “Clinic Partnerships”). To a lesser extent, we operate some clinics through wholly-owned subsidiaries under profit sharing arrangements with therapists (hereinafter referred to as “Wholly-Owned Facilities”). Unless the context otherwise requires, references in this Annual Report on Form 10-K to “we”, “our” or “us” includes the Company and all of its subsidiaries.
Our strategy is to develop outpatient physical therapy clinics and to acquire single and multi-clinic outpatient physical therapy practices on a national basis. At December 31, 2015, we operated 508 clinics in 42 states. The average age of the 508 clinics in operation at December 31, 2015 was 9.4 years. There were 359 clinics operated under Clinic Partnerships and the remaining clinics were operated as Wholly-Owned Facilities or through management arrangements. Of the 508 clinics, we developed 311 and acquired an interest in 197. Our highest concentration of clinics are in the following states: Tennessee, Texas, Michigan, Virginia, Washington, Maryland, Georgia, Pennsylvania and Wisconsin. In addition to our 508 clinics, at December 31, 2015, we also managed 21 physical therapy practices for unrelated physician groups and hospitals.
During the last three years, we completed the following multi-clinic acquisitions:
Acquisition |
Date |
% Interest Acquired |
Number of Clinics |
||||
2015 |
|||||||
January 2015 Acquisition |
January 31 |
60 | % |
9 | |||
April 2015 Acquisition |
April 30 |
70 | % |
3 | |||
June 2015 Acquisition |
June 30 |
70 | % |
4 | |||
December 2015 Acquisition |
December 31 |
59 | % |
4 | |||
2014 |
|||||||
April 2014 Acquisition |
April 30 |
70 | % |
13 | |||
August 2014 Acquisition |
August 1 |
100 | % |
3 | |||
2013 |
|||||||
February 2013 Acquisition |
February 28 |
72 | % |
9 | |||
April 2013 Acquisition |
April 30 |
50 | % |
5 | |||
May 2013 Acquistion |
May 24 |
80 | % |
5 | |||
December 9, 2013 Acquisition |
December 9 |
60 | % |
12 | |||
December 13, 2013 Acquisition |
December 13 |
90 | % |
11 | |||
In addition to the multi-clinic acquisitions detailed above, we acquired a 60% interest in an individual clinic practice during 2015, we acquired four individual clinics in separate transactions during 2014, and we acquired three individual clinics in separate transactions during 2013.
We continue to seek to attract physical therapists who have established relationships with physicians and other referral sources by offering therapists a competitive salary and a share of the profits or an ownership interest in the clinic operated by that therapist. In addition, we have developed satellite clinic facilities of existing clinics, with the result that a substantial number of Clinic Partnerships and Wholly-Owned facilities operate more than one clinic location. In 2016, we intend to continue to acquire clinic practices and continue to focus on developing new clinics and on opening satellite clinics where appropriate along with increasing our patient volume through marketing and new programs.
2
Therapists at our clinics initially perform a comprehensive evaluation of each patient, which is then followed by a treatment plan specific to the injury as prescribed by the patient’s physician. The treatment plan may include a number of procedures, including therapeutic exercise, manual therapy techniques, ultrasound, electrical stimulation, hot packs, iontophoresis, education on management of daily life skills and home exercise programs. A clinic’s business primarily comes from referrals by local physicians. The principal sources of payment for the clinics’ services are managed care programs, commercial health insurance, Medicare/Medicaid and workers’ compensation insurance.
We were re-incorporated in April 1992 under the laws of the State of Nevada and have operating subsidiaries organized in various states in the form of limited partnerships, limited liability companies and wholly-owned corporations. This description of our business should be read in conjunction with our financial statements and the related notes contained in Item 8 in this Annual Report on Form 10-K. Our principal executive offices are located at 1300 West Sam Houston Parkway South, Suite 300, Houston, Texas 77042. Our telephone number is (713) 297-7000. Our website is www.usph.com.
OUR CLINICS
Most of our clinics are operated by Clinic Partnerships in which we own the general partnership interest and a majority of the limited partnership interests. The managing healthcare practitioner of the clinics usually owns a portion of the limited partnership interests. Generally, the therapist partners have no interest in the net losses of Clinic Partnerships, except to the extent of their capital accounts. Since we also develop satellite clinic facilities of existing clinics, most Clinic Partnerships consist of more than one clinic location. As of December 31, 2015, through wholly-owned subsidiaries, we owned a 1% general partnership interest in all the Clinic Partnerships, except for one partnership in which we own a 6% general partnership interest. Our limited partnership interests range from 49% to 99% in the Clinic Partnerships, but with respect to the majority of our Clinic Partnerships, we own a limited partnership interest of 64%. For the vast majority of the Clinic Partnerships, the managing healthcare practitioner is a physical therapist who owns the remaining limited partnership interest in the Clinic Partnership.
For our Clinic Partnership agreements related to those that we acquired a majority interest, generally, the prior management continues to own a 10% to 50% interest. For our Clinic Partnership agreements related to our developed clinics, the therapist partner typically begins with a 20% interest in their Clinic Partnership earnings which increases by 3% at the end of each year thereafter up to a maximum interest of 35%.
Typically, each therapist partner or director, including those employed by Clinic Partnerships in which we acquired a majority interest, enters into an employment agreement for a term of up to five years with their Clinic Partnership. Each agreement typically provides for a covenant not to compete during the period of his or her employment and for up to two years thereafter. Under each employment agreement, the therapist partner receives a base salary and may receive a bonus based on the net revenues or profits generated by their Clinic Partnership or specific clinic. In the case of Clinic Partnerships, the therapist partner receives earnings distributions based upon their ownership interest. Upon termination of employment, we typically have the right, but not the obligation, to purchase the therapist’s partnership interest in Clinic Partnerships. In connection with most of our acquired clinics, in the event that a limited minority partner’s employment ceases at any time after three or four years from the acquisition date, as applicable, we have agreed to repurchase that individual’s non-controlling interest at a predetermined multiple of earnings before interest and taxes.
Each Clinic Partnership maintains an independent local identity, while at the same time enjoying the benefits of national purchasing, negotiated third-party payor contracts, centralized support services and management practices. Under a management agreement, one of our subsidiaries provides a variety of support services to each clinic, including supervision of site selection, construction, clinic design and equipment selection, establishment of accounting systems and billing procedures and training of office support personnel, processing of accounts payable, operational direction, auditing of regulatory compliance, payroll, benefits administration, accounting services, legal services, quality assurance and marketing support.
Our typical clinic occupies approximately 1,500 to 3,000 square feet of leased space in an office building or shopping center. We attempt to lease ground level space for patient ease of access to our clinics. We also attempt to make the decor in our clinics less institutional and more aesthetically pleasing than traditional hospital clinics.
3
Typical minimum staff at a clinic consists of a licensed physical therapist and an office manager. As patient visits grow, staffing may also include additional physical therapists, occupational therapists, therapy assistants, aides, exercise physiologists, athletic trainers and office personnel. Therapy services are performed under the supervision of a licensed therapist.
We provide services at our clinics on an outpatient basis. Patients are usually treated for approximately one hour per day, two to three times a week, typically for two to six weeks. We generally charge for treatment on a per procedure basis. Medicare patients are charged based on prescribed time increments and Medicare billing standards. In addition, our clinics will develop, when appropriate, individual maintenance and self-management exercise programs to be continued after treatment. We continually assess the potential for developing new services and expanding the methods of providing our existing services in the most efficient manner while providing high quality patient care.
FACTORS INFLUENCING DEMAND FOR THERAPY SERVICES
We believe that the following factors, among others, influence the growth of outpatient physical therapy services:
Economic Benefits of Therapy Services. Purchasers and providers of healthcare services, such as insurance companies, health maintenance organizations, businesses and industries, continuously seek cost savings for traditional healthcare services. We believe that our therapy services provide a cost-effective way to prevent short-term disabilities from becoming chronic conditions and to speed recovery from surgery and musculoskeletal injuries.
Earlier Hospital Discharge. Changes in health insurance reimbursement, both public and private, have encouraged the earlier discharge of patients to reduce costs. We believe that early hospital discharge practices foster greater demand for outpatient physical therapy services.
Aging Population. In general, the elderly population has a greater incidence of disability compared to the population as a whole. As this segment of the population continues to grow, we believe that demand for rehabilitation services will expand.
MARKETING
We focus our marketing efforts primarily on physicians, including orthopedic surgeons, neurosurgeons, physiatrists, internal medicine physicians, podiatrists, occupational medicine physicians and general practitioners. In marketing to the physician community, we emphasize our commitment to quality patient care and regular communication with physicians regarding patient progress. We employ personnel to assist clinic directors in developing and implementing marketing plans for the physician community and to assist in establishing relationships with health maintenance organizations, preferred provider organizations, industry, case managers and insurance companies.
SOURCES OF REVENUE
Payor sources for clinic services are primarily managed care programs, commercial health insurance, Medicare/Medicaid and workers’ compensation insurance. Commercial health insurance, Medicare and managed care programs generally provide coverage to patients utilizing our clinics after payment by the patients of normal deductibles and co-insurance payments. Workers’ compensation laws generally require employers to provide, directly or indirectly through insurance, costs of medical rehabilitation for their employees from work-related injuries and disabilities and, in some jurisdictions, mandatory vocational rehabilitation, usually without any deductibles, co-payments or cost sharing. Treatments for patients who are parties to personal injury cases are generally paid from the proceeds of settlements with insurance companies or from favorable judgments. If an unfavorable judgment is received, collection efforts are generally not pursued against the patient and the patient’s account is written-off against established reserves. Bad debt reserves relating to all receivable types are regularly reviewed and adjusted as appropriate.
4
The following table shows our payor mix for the years ended:
December 31, 2015 |
December 31, 2014 |
December 31, 2013 |
||||||||||||||||
Payor |
Net Patient Revenue |
Percentage |
Net Patient Revenue |
Percentage |
Net Patient Revenue |
Percentage |
||||||||||||
(Net Patient Revenues in Thousands) |
||||||||||||||||||
Managed Care Program |
$ | 73,554 | 22.7 | % |
$ | 67,139 | 22.5 | % |
$ | 58,680 | 22.8 | % |
||||||
Commercial Health Insurance |
91,845 | 28.3 | % |
87,890 | 29.4 | % |
79,148 | 30.6 | % |
|||||||||
Medicare/Medicaid |
79,321 | 24.5 | % |
69,857 | 23.4 | % |
60,697 | 23.5 | % |
|||||||||
Workers’ Compensation Insurance |
60,087 | 18.5 | % |
57,643 | 19.3 | % |
45,221 | 17.5 | % |
|||||||||
Other |
19,485 | 6.0 | % |
16,480 | 5.4 | % |
14,537 | 5.6 | % |
|||||||||
Total |
$ | 324,292 | 100.0 | % |
$ | 299,009 | 100.0 | % |
$ | 258,283 | 100.0 | % |
||||||
Our business depends to a significant extent on our relationships with commercial health insurers, health maintenance organizations, preferred provider organizations and workers’ compensation insurers. In some geographical areas, our clinics must be approved as providers by key health maintenance organizations and preferred provider plans to obtain payments. Failure to obtain or maintain these approvals would adversely affect financial results.
During the year ended December 31, 2015, approximately 26.6% of our visits and 22.6% of our net patient revenues were from patients with Medicare program coverage. To receive Medicare reimbursement, a facility (Medicare Certified Rehabilitation Agency) or the individual therapist (Physical/Occupational Therapist in Private Practice) must meet applicable participation conditions set by the Department of Health and Human Services (“HHS”) relating to the type of facility, equipment, recordkeeping, personnel and standards of medical care, and also must comply with all state and local laws. HHS, through Centers for Medicare & Medicaid Services (“CMS”) and designated agencies, periodically inspects or surveys clinics/providers for approval and/or compliance. We anticipate that our newly developed and acquired clinics will become certified as Medicare providers or will be enrolled as a group of physical/occupation therapists in a private practice. Failure to obtain or maintain this certification would adversely affect financial results.
The Medicare program reimburses outpatient rehabilitation providers based on the Medicare Physician Fee Schedule (“MPFS”). The MPFS rates have historically been subject to an automatic annual update based on a formula, called the sustainable growth rate (“SGR”) formula. The use of the SGR formula would have resulted in calculated automatic reductions in rates in every year since 2002; however, for each year through September 30, 2015, Centers for Medicare & Medicaid Services (“CMS”) or Congress has taken action to prevent the implementation of SGR formula reductions. On April 16, 2015, the Medicare Access and CHIP Reauthorization Act of 2015 (“MACRA”) was signed into law, eliminating the SGR formula and the associated annual automatic rate reductions. For services provided between January 1, 2015 and June 30, 2015 a 0% payment update was applied to the Medicare physician fee schedule payment rates; for services provided between July 1, 2015 and December 31, 2015 a 0.5% increase was applied to the fee schedule payment rates; for services provided in 2016 a 0.3% decrease is being applied to the fee schedule payment rates, and for 2017 through 2019, a 0.5% increase will be applied each year to the fee schedule payment rates, unless further adjusted by CMS. In addition, the MACRA promotes the development of new payment models that focus on quality and outcomes.
The Budget Control Act of 2011 increased the federal debt ceiling in connection with deficit reductions over the next ten years, and requires automatic reductions in federal spending by approximately $1.2 trillion. Payments to Medicare providers are subject to these automatic spending reductions, subject to a 2% cap. On April 1, 2013, a 2% reduction to Medicare payments was implemented.
As a result of the Balanced Budget Act of 1997, the formula for determining the total amount paid by Medicare in any one year for outpatient physical therapy, occupational therapy, and/or speech-language pathology services provided to any Medicare beneficiary (i.e., the “Therapy Cap” or “Limit”) was established. Based on the statutory definitions which constrained how the Therapy Cap would be applied, there is one Limit for Physical Therapy and Speech Language Pathology Services combined, and one Limit for Occupational Therapy. For 2015, the annual Limit on outpatient therapy services was $1,940 for Physical and Speech Language Pathology Services combined and $1,940 for Occupational Therapy Services. For 2016, the annual Limit on
5
outpatient therapy services is $1,960 for Physical and Speech Language Pathology Services combined and $1,960 for Occupational Therapy Services. Historically, these Therapy Caps applied to outpatient therapy services provided in all settings, except for services provided in departments of hospitals. However, the Protecting Access to Medicare Act of 2014, and prior legislation, extended the Therapy Caps to services furnished in hospital outpatient department settings. The application of these annual limits to hospital outpatient department settings will sunset on December 31, 2017 unless Congress extends it.
In the Deficit Reduction Act of 2005, Congress implemented an exceptions process to the annual Limit for therapy expenses for therapy services above the annual Limit. Therapy services above the annual Limit that are medically necessary satisfy an exception to the annual Limit and such claims are payable by the Medicare program. The Protecting Access to Medicare Act of 2014 extended the exceptions process for outpatient therapy caps through March 31, 2015. The MACRA further extended the exceptions process for outpatient therapy caps through December 31, 2017. Unless Congress extends the exceptions process further, the therapy caps will apply to all outpatient therapy services beginning January 1, 2018, except those services furnished and billed by outpatient hospital departments. For any claim above the annual Limit, the claim must contain a modifier indicating that the services are medically necessary and justified by appropriate documentation in the medical record.
Furthermore, under the Middle Class Tax Relief and Job Creation Act of 2012 (“MCTRA”), since October 1, 2012, patients who met or exceeded $3,700 in therapy expenditures during a calendar year have been subject to a manual medical review to determine whether applicable payment criteria are satisfied. The $3,700 threshold is applied to Physical Therapy and Speech Language Pathology Services; a separate $3,700 threshold is applied to the Occupational Therapy. The MACRA directed CMS to modify the manual medical review process such that those reviews will no longer apply to all claims exceeding the $3,700 threshold and instead will be determined on a targeted basis based on a variety of factors that CMS considers appropriate. The new factors have applied to exception requests for which CMS did not conduct a medical review by July 15, 2015.
CMS adopted a multiple procedure payment reduction (“MPPR”) for therapy services in the final update to the MPFS for calendar year 2011. The MPPR applies to all outpatient therapy services paid under Medicare Part B — occupational therapy, physical therapy and speech-language pathology. Under the policy, the Medicare program pays 100% of the practice expense component of the Relative Value Unit (“RVU”) for the therapy procedure with the highest practice expense RVU, then reduces the payment for the practice expense component for the second and subsequent therapy procedures or units of service furnished during the same day for the same patient, regardless of whether those therapy services are furnished in separate sessions. Since 2013, the practice expense component for the second and subsequent therapy service furnished during the same day for the same patient was reduced by 50%. In addition, the MCTRA directed CMS to implement a claims-based data collection program to gather additional data on patient function during the course of therapy in order to better understand patient conditions and outcomes. All practice settings that provide outpatient therapy services are required to include this data on the claim form. Since 2013, therapists have been required to report new codes and modifiers on the claim form that reflect a patient’s functional limitations and goals at initial evaluation, periodically throughout care, and at discharge; CMS has rejected claims if the required data is not included in the claim.
The Physician Quality Reporting System, or “PQRS,” is a CMS reporting program that uses a combination of incentive payments and payment reductions to promote reporting of quality information by “eligible professionals.” Although physical therapists, occupational therapists and qualified speech-language therapists are generally able to participate in the PQRS program, therapy professionals for whose services we bill through our certified rehabilitation agencies cannot participate because the Medicare claims processing systems currently cannot accommodate institutional providers such as certified rehabilitation agencies. Eligible professionals, such as those of our therapy professionals for whose services we bill using their individual Medicare provider numbers, who do not satisfactorily report data on quality measures will be subject to a 2% reduction in their Medicare payment in 2016 and 2017.
Statutes, regulations, and payment rules governing the delivery of therapy services to Medicare beneficiaries are complex and subject to interpretation. We believe we are in compliance in all material respects with all applicable laws and regulations and are not aware of any pending or threatened investigations involving
6
allegations of potential wrongdoing that would have a material effect on our financial statements as of December 31, 2015. Compliance with such laws and regulations can be subject to future government review and interpretation, as well as significant regulatory action including fines, penalties, and exclusion from the Medicare program.
REGULATION AND HEALTHCARE REFORM
Numerous federal, state and local regulations regulate healthcare services and those who provide them. Some states into which we may expand have laws requiring facilities employing health professionals and providing health-related services to be licensed and, in some cases, to obtain a certificate of need (that is, demonstrating to a state regulatory authority the need for, and financial feasibility of, new facilities or the commencement of new healthcare services). Only one of the states in which we currently operate requires a certificate of need for the operation of our physical therapy business functions. Our therapists and/or clinics, however, are required to be licensed, as determined by the state in which they provide services. Failure to obtain or maintain any required certificates, approvals or licenses could have a material adverse effect on our business, financial condition and results of operations.
Regulations Controlling Fraud and Abuse. Various federal and state laws regulate financial relationships involving providers of healthcare services. These laws include Section 1128B(b) of the Social Security Act (42 U.S. C. § 1320a-7b[b]) (the “Fraud and Abuse Law”), under which civil and criminal penalties can be imposed upon persons who, among other things, offer, solicit, pay or receive remuneration in return for (i) the referral of patients for the rendering of any item or service for which payment may be made, in whole or in part, by a Federal health care program (including Medicare and Medicaid); or (ii) purchasing, leasing, ordering, or arranging for or recommending purchasing, leasing, ordering any good, facility, service, or item for which payment may be made, in whole or in part, by a Federal health care program (including Medicare and Medicaid). We believe that our business procedures and business arrangements are in compliance with these provisions. However, the provisions are broadly written and the full extent of their specific application to specific facts and arrangements to which we are a party is uncertain and difficult to predict. In addition, several states have enacted state laws similar to the Fraud and Abuse Law, which may be more restrictive than the federal Fraud and Abuse Law.
The Office of the Inspector General (“OIG”) of HHS has issued regulations describing compensation financial arrangements that fall within a “Safe Harbor” and, therefore, are not viewed as illegal remuneration under the Fraud and Abuse Law. Failure to fall within a Safe Harbor does not mean that the Fraud and Abuse Law has been violated; however, the OIG has indicated that failure to fall within a Safe Harbor may subject an arrangement to increased scrutiny under a “facts and circumstances” test.
The OIG also has issued special fraud alerts and special advisory bulletins to remind the provider community of the importance and application of certain aspects of the Fraud and Abuse Law. One of the OIG special fraud alerts related to the rental of space in physician offices by persons or entities to which the physicians refer patients. The OIG’s stated concern in these arrangements is that rental payments may be disguised kickbacks to the physician-landlords to induce referrals. We rent clinic space for a few of our clinics from referring physicians and have taken the steps that we believe are necessary to ensure that all leases comply to the extent possible and applicable with the space rental Safe Harbor to the Fraud and Abuse Law.
One of the OIG’s special advisory bulletins addressed certain complex contractual arrangements for the provision of items and services. This special advisory bulletin identified several characteristics commonly exhibited by suspect arrangements, the existence of one or more of which could indicate a prohibited arrangement to the OIG. Generally, the indicia of a suspect contractual joint venture as identified by the special advisory bulletin and an associated OIG advisory opinion include the following:
| • | New Line of Business. A provider in one line of business (“Owner”) expands into a new line of business that can be provided to the Owner’s existing patients, with another party who currently provides the same or similar item or service as the new business (“Manager/Supplier”). |
| • | Captive Referral Base. The arrangement predominantly or exclusively serves the Owner’s existing patient base (or patients under the control or influence of the Owner). |
7
| • | Little or No Bona Fide Business Risk. The Owner’s primary contribution to the venture is referrals; it makes little or no financial or other investment in the business, delegating the entire operation to the Manager/Supplier, while retaining profits generated from its captive referral base. |
| • | Status of the Manager/Supplier. The Manager/Supplier is a would-be competitor of the Owner’s new line of business and would normally compete for the captive referrals. It has the capacity to provide virtually identical services in its own right and bill insurers and patients for them in its own name. |
| • | Scope of Services Provided by the Manager/Supplier. The Manager/Supplier provides all, or many, of the new business’ key services. |
| • | Remuneration. The practical effect of the arrangement, viewed in its entirety, is to provide the Owner the opportunity to bill insurers and patients for business otherwise provided by the Manager/Supplier. The remuneration from the venture to the Owner (i.e., the profits of the venture) takes into account the value and volume of business the Owner generates. |
| • | Exclusivity. The arrangement bars the Owner from providing items or services to any patients other than those coming from Owner and/or bars the Manager/Supplier from providing services in its own right to the Owner’s patients. |
Due to the nature of our business operations, many of our management service arrangements exhibit one or more of these characteristics. However, the we believe we have taken steps regarding the structure of such arrangements as necessary to sufficiently distinguish them from these suspect ventures, and to comply with the requirements of the Fraud and Abuse Law. However, if the OIG believes we have entered into a prohibited contractual joint venture, it could have an adverse effect on our business, financial condition and results of operations.
Although the business of managing physician-owned physical therapy facilities is regulated by the Fraud and Abuse Law, the manner in which we contract with such facilities often falls outside the complete scope of available Safe Harbors. We believe our arrangements comply with the Fraud and Abuse Law, even though federal courts provide limited guidance as to the application of the Fraud and Abuse Law to these arrangements. If our management contracts are held to violate the Fraud and Abuse Law, it could have an adverse effect on our business, financial condition and results of operations.
Stark Law. Provisions of the Omnibus Budget Reconciliation Act of 1993 (42 U.S.C. § 1395nn) (the “Stark Law”) prohibit referrals by a physician of “designated health services” which are payable, in whole or in part, by Medicare or Medicaid, to an entity in which the physician or the physician’s immediate family member has an investment interest or other financial relationship, subject to several exceptions. Unlike the Fraud and Abuse Law, the Stark Law is a strict liability statute. Proof of intent to violate the Stark Law is not required. Physical therapy services are among the “designated health services”. Further, the Stark Law has application to our management contracts with individual physicians and physician groups, as well as, any other financial relationship between us and referring physicians, including medical advisor arrangements and any financial transaction resulting from a clinic acquisition. The Stark Law also prohibits billing for services rendered pursuant to a prohibited referral. Several states have enacted laws similar to the Stark Law. These state laws may cover all (not just Medicare and Medicaid) patients. As with the Fraud and Abuse Law, we consider the Stark Law in planning our clinics, establishing contractual and other arrangements with physicians, marketing and other activities, and believe that our operations are in substantial compliance with the Stark Law. If we violate the Stark Law or any similar state laws, our financial results and operations could be adversely affected. Penalties for violations include denial of payment for the services, significant civil monetary penalties, and exclusion from the Medicare and Medicaid programs.
HIPAA. In an effort to further combat healthcare fraud and protect patient confidentially, Congress included several anti-fraud measures in the Health Insurance Portability and Accountability Act of 1996 (“HIPAA”). HIPAA created a source of funding for fraud control to coordinate federal, state and local healthcare law enforcement programs, conduct investigations, provide guidance to the healthcare industry concerning fraudulent healthcare practices, and establish a national data bank to receive and report final adverse actions. HIPAA also criminalized certain forms of health fraud against all public and private payors. Additionally, HIPAA mandates the adoption of standards regarding the exchange of healthcare information in an effort to ensure the privacy and electronic security of patient information and standards relating to the privacy of health information. Sanctions
8
for failing to comply with HIPAA include criminal penalties and civil sanctions. In February of 2009, the American Recovery and Reinvestment Act of 2009 (“ARRA”) was signed into law. Title XIII of ARRA, the Health Information Technology for Economic and Clinical Health Act (“HITECH”), provided for substantial Medicare and Medicaid incentives for providers to adopt electronic health records (“EHRs”) and grants for the development of health information exchange (“HIE”). Recognizing that HIE and EHR systems will not be implemented unless the public can be assured that the privacy and security of patient information in such systems is protected, HITECH also significantly expanded the scope of the privacy and security requirements under HIPAA. Most notable are the mandatory breach notification requirements and a heightened enforcement scheme that includes increased penalties, and which now apply to business associates as well as to covered entities. In addition to HIPAA, a number of states have adopted laws and/or regulations applicable in the use and disclosure of individually identifiable health information that can be more stringent than comparable provisions under HIPAA.
We believe that our operations comply with applicable standards for privacy and security of protected healthcare information. We cannot predict what negative effect, if any, HIPAA/HITECH or any applicable state law or regulation will have on our business.
Other Regulatory Factors. Political, economic and regulatory influences are fundamentally changing the healthcare industry in the United States. Congress, state legislatures and the private sector continue to review and assess alternative healthcare delivery and payment systems. Potential alternative approaches could include mandated basic healthcare benefits, controls on healthcare spending through limitations on the growth of private health insurance premiums and Medicare and Medicaid spending, the creation of large insurance purchasing groups, and price controls. Legislative debate is expected to continue in the future and market forces are expected to demand only modest increases or reduced costs. For instance, managed care entities are demanding lower reimbursement rates from healthcare providers and, in some cases, are requiring or encouraging providers to accept capitated payments that may not allow providers to cover their full costs or realize traditional levels of profitability. We cannot reasonably predict what impact the adoption of federal or state healthcare reform measures or future private sector reform may have on our business.
COMPETITION
The healthcare industry, including the physical therapy business, is highly competitive. The physical therapy business is highly fragmented with no company having a significant market share nationally. We believe that we are currently the fourth largest national outpatient rehabilitation provider.
Competitive factors affecting our business include quality of care, cost, treatment outcomes, convenience of location, and relationships with, and ability to meet the needs of, referral and payor sources. Our clinics compete, directly or indirectly, with many types of healthcare providers including the physical therapy departments of hospitals, private therapy clinics, physician-owned therapy clinics, and chiropractors. We may face more intense competition if consolidation of the therapy industry continues.
We believe that our strategy of providing key therapists in a community with an opportunity to participate in ownership or clinic profitability provides us with a competitive advantage by helping to ensure the commitment of local management to the success of the clinic.
We also believe that our competitive position is enhanced by our strategy of locating our clinics, when possible, on the ground floor of buildings and shopping centers with nearby parking, thereby making the clinics more easily accessible to patients. We offer convenient hours. We also attempt to make the decor in our clinics less institutional and more aesthetically pleasing than traditional hospital clinics.
ENFORCEMENT ENVIRONMENT
In recent years, federal and state governments have launched several initiatives aimed at uncovering behavior that violates the federal civil and criminal laws regarding false claims and fraudulent billing and coding practices. Such laws require providers to adhere to complex reimbursement requirements regarding proper billing and coding in order to be compensated for their services by government payors. Our compliance program requires adherence to applicable law and promotes reimbursement education and training; however, a determination that our clinics’ billing and coding practices are false or fraudulent could have a material adverse effect on us.
9
As a result of our participation in the Medicare and Medicaid programs, we are subject to various governmental inspections, reviews, audits and investigations to verify our compliance with these programs and applicable laws and regulations. In addition, our Corporate Integrity Agreement requires annual audits to be performed by an independent review organization on a small sample of our clinics, the results of which are reported to the federal government. See “-Compliance Program – Corporate Integrity Agreement”. Managed care payors may also reserve the right to conduct audits. An adverse inspection, review, audit or investigation could result in: refunding amounts we have been paid; fines penalties and/or revocation of billing privileges for the affected clinics; expansion of the scope of our Corporate Integrity Agreement; exclusion from participation in the Medicare or Medicaid programs or one or more managed care payor network; or damage to our reputation.
We and our clinics are subject to federal and state laws prohibiting entities and individuals from knowingly and willfully making claims to Medicare, Medicaid and other governmental programs and third party payors that contain false or fraudulent information. The federal False Claims Act encourages private individuals to file suits on behalf of the government against healthcare providers such as us. As such suits are generally filed under seal with a court to allow the government adequate time to investigate and determine whether it will intervene in the action, the implicated healthcare providers often are unaware of the suit until the government has made its determination and the seal is lifted. Violations or alleged violations of such laws, and any related lawsuits, could result in (i) exclusion from participation in Medicare, Medicaid and other federal healthcare programs, or (ii) significant financial or criminal sanctions, resulting in the possibility of substantial financial penalties for small billing errors that are replicated in a large number of claims, as each individual claim could be deemed a separate violation. In addition, many states also have enacted similar statutes, which may include criminal penalties, substantial fines, and treble damages.
COMPLIANCE PROGRAM
Our Compliance Program. Our ongoing success depends upon our reputation for quality service and ethical business practices. We operate in a highly regulated environment with many federal, state and local laws and regulations. We take a proactive interest in understanding and complying with the laws and regulations that apply to our business.
Our Board of Directors (the “Board”) has adopted a Code of Business Conduct and Ethics and a set of Corporate Governance Guidelines to clarify the ethical standards under which the Board and management carry out their duties. In addition, the Board has created a Compliance Committee of the Board (“Compliance Committee”) whose purpose is to assist the Board in discharging their oversight responsibilities with respect to compliance with federal and state laws and regulations relating to healthcare.
We have issued an Ethics and Compliance Manual and created compliance training materials, hand-outs and an on-line testing program. These tools were prepared to ensure that every employee of our Company and subsidiaries has a clear understanding of our mutual commitment to high standards of professionalism, honesty, fairness and compliance with the law in conducting business. These standards are administered by our Chief Compliance Officer (“CO”), who has the responsibility for the day-to-day oversight, administration and development of our compliance program. The CO, internal and external counsel, management and the Compliance Committee review our policies and procedures for our compliance program from time to time in an effort to improve operations and to ensure compliance with requirements of standards, laws and regulations and to reflect the on-going compliance focus areas which have been identified by management, counsel or the Compliance Committee. We also have established systems for reporting potential violations, educating our employees, monitoring and auditing compliance and handling enforcement and discipline.
Committees. Our Compliance Committee, appointed by the Board, consists of five independent directors. The Compliance Committee has general oversight of our Company’s compliance with the legal and regulatory requirements regarding healthcare operations. The Compliance Committee relies on the expertise and knowledge of management, the CO and other compliance and legal personnel. The CO regularly communicates with the Chairman of the Compliance Committee. The Compliance Committee meets at least four times a year or more frequently as necessary to carry out its responsibilities and reports regularly to the Board regarding its actions and recommendations.
We also have an Internal Compliance Committee, which is comprised of Company leaders in the areas of operations, clinical services, finance, human resources, legal, information technology and credentialing. The Internal Compliance Committee has the responsibility for evaluating and assessing Company areas of risk
10
relating to compliance with federal and state healthcare laws, and generally to assist the CO. The Internal Compliance Committee meets at least four times a year or more frequently as necessary to carry out its responsibilities. In addition, management has appointed a team to address our Company’s compliance with HIPAA. The HIPAA team consists of a security officer and employees from our legal, information systems, finance, operations, compliance, business services and human resources departments. The team prepares assessments and makes recommendations regarding operational changes and/or new systems, if needed, to comply with HIPAA.
Each clinic certified as a Medicare Rehabilitation Agency has a formally appointed governing body composed of a member of our management and the director/administrator of the clinic. The governing body retains legal responsibility for the overall conduct of the clinic. The members confer regularly and discuss, among other issues, clinic compliance with applicable laws and regulations. In addition, there are Professional Advisory Committees which serve as Infection Control Committees. These committees meet in the facilities and function as advisors.
We have in place a Risk Management Committee consisting of, among others, the CO, our General Counsel. other legal and compliance department personnel and the Corporate Vice President of Administration. This committee reviews and monitors all employee and patient incident reports and provides clinic personnel with actions to be taken in response to the reports.
Reporting Violations. In order to facilitate our employees’ ability to report in confidence, anonymously and without retaliation any perceived improper work-related activities, accounting irregularities and other violations of our compliance program, we have set up an independent national compliance hotline. The compliance hotline is available to receive confidential reports of wrongdoing Monday through Friday (excluding holidays), 24 hours a day. The compliance hotline is staffed by experienced third party professionals trained to utilize utmost care and discretion in handling sensitive issues and confidential information. The information received is documented and forwarded timely to the CO, who, together with the Compliance Committee, has the power and resources to investigate and resolve matters of improper conduct.
Educating Our Employees. We utilize numerous methods to train our employees in compliance related issues. The directors/administrators of each clinic are responsible for conducting the initial training sessions on compliance with existing employees. Training is based on our Ethics and Compliance Manual, inclusive of HIPAA information, and our compliance training materials. The directors/administrators also provide periodic “refresher” training for existing employees and one-on-one comprehensive training with new hires. The corporate compliance group responds to questions from clinic personnel and conducts frequent teleconference meetings, webinars and training sessions on a variety of compliance related topics.
When a clinic opens, the Company provides a package of compliance materials containing manuals and detailed instructions for meeting Medicare Conditions of Participation Standards and other compliance requirements. During follow up training with the director/administrator of the clinic, compliance department staff explain various details regarding requirements and compliance standards. Compliance staff will remain in contact with the director/administrator while the clinic is implementing compliance standards and will provide any assistance required. All new office managers receive training (including Medicare, regulatory and corporate compliance, insurance billing, charge entry and transaction posting and coding, daily, weekly and monthly accounting reports) from the training staff at the corporate office. The corporate compliance group will assist in continued compliance, including guidance to the clinic staff with regard to Medicare certifications, state survey requirements and responses to any inquiries from regulatory agencies.
Monitoring and Auditing Clinic Operational Compliance. We have in place audit programs and other procedures to monitor and audit clinic operational compliance with applicable policies and procedures. We employ internal auditors who, as part of their job responsibilities, conduct periodic audits of each clinic. Most clinics are audited at least once every 24 months and additional focused audits are performed as deemed necessary. During these audits, particular attention is given to compliance with Medicare and internal policies, Federal and state laws and regulations, third party payor requirements, and patient chart documentation, billing, reporting, record keeping, collections and contract procedures. The audits typically are conducted on site and include interviews with the employees involved in management, operations, billing and accounts receivable.
11
Formal audit reports are prepared and reviewed with corporate management and the Compliance Committee. Each clinic director/administrator receives a letter instructing them of any corrective measures required. Each clinic director/administrator then works with the compliance team and operations to ensure such corrective measures are achieved.
Handling Enforcement and Discipline. It is our policy that any employee who fails to comply with compliance program requirements or who negligently or deliberately fails to comply with known laws or regulations specifically addressed in our compliance program should be subject to disciplinary action up to and including discharge from employment. The Compliance Committee, compliance staff, human resources staff and management investigate violations of our compliance program and impose disciplinary action as considered appropriate.
Corporate Integrity Agreement. The Company also performs certain additional compliance related functions pursuant to the Corporate Integrity Agreement (“Corporate Integrity Agreement” or “CIA”) that the Company entered into with the OIG. The CIA, which became effective as of December 21, 2015, outlines certain specific requirements relating to compliance oversight and program implementation, as well as periodic reporting. In addition, pursuant to the CIA, an independent review organization annually will perform a Medicare billing and coding audit on a small group of randomly selected Company clinics. The Company’s Compliance Program has been modified so as to comply with the requirements of the CIA. The term of the CIA is five years.
The CIA was entered into as part of the settlement by one of the Company’s Subsidiaries with the U. S. Department of Justice related to certain Medicare billings that occurred between 2007 and 2009 at a single outpatient physical therapy clinic. The settlement resolved claims relating to whether certain physical therapy services provided to a limited number of Medicare patients at the clinic satisfied all of the criteria for payment by the Medicare program, including proper supervision of physical therapist assistants. The Subsidiary paid $718,000 to resolve the matter, and the Subsidiary and the Company entered into the CIA.
EMPLOYEES
At December 31, 2015, we employed approximately 3,400 people, of which 2,400 were full-time employees. At that date, no Company employees were governed by collective bargaining agreements or were members of a union. We consider our relations with our employees to be good.
In the states in which our current clinics are located, persons performing designated physical therapy services are required to be licensed by the state. Based on standard employee screening systems in place, all persons currently employed by us who are required to be licensed are licensed. We are not aware of any federal licensing requirements applicable to our employees.
AVAILABLE INFORMATION
Our annual reports on Form 10-K, quarterly reports on Form 10-Q, current reports on Form 8-K and amendments to those reports filed or furnished pursuant to Section 13(a) or 15(d) of the Exchange Act are made available free of charge on our internet website at www.usph.com as soon as reasonably practicable after we electronically file such material with, or furnish it to, the SEC.
Our business, operations and financial condition are subject to various risks. Some of these risks are described below, and readers of this Annual Report on Form 10-K should take such risks into account in evaluating our Company or making any decision to invest in us. This section does not describe all risks applicable to our Company, our industry or our business, and it is intended only as a summary of material factors affecting our business.
Risks related to our business and operations
Healthcare reform legislation may affect our business.
In recent years, many legislative proposals have been introduced or proposed in Congress and in some state legislatures that would affect major changes in the healthcare system, either nationally or at the state level. At the federal level, Congress has continued to propose or consider healthcare budgets that substantially reduce
12
payments under the Medicare programs. See “Business- Sources of Revenue” in Item 1 for more information. The ultimate content, timing or effect of any healthcare reform legislation and the impact of potential legislation on us is uncertain and difficult, if not impossible, to predict. That impact may be material to our business, financial condition or results of operations.
Our operations are subject to extensive regulation.
The healthcare industry is subject to extensive federal, state and local laws and regulations relating to:
| • | facility and professional licensure/permits, including certificates of need; |
| • | conduct of operations, including financial relationships among healthcare providers, Medicare fraud and abuse, and physician self-referral; |
| • | addition of facilities and services; and |
| • | billing and payment for services. |
In recent years, there have been heightened coordinated civil and criminal enforcement efforts by both federal and state government agencies relating to the healthcare industry. We believe we are in substantial compliance with all laws, but differing interpretations or enforcement of these laws and regulations could subject our current practices to allegations of impropriety or illegality or could require us to make changes in our methods of operations, facilities, equipment, personnel, services and capital expenditure programs and increase our operating expenses. If we fail to comply with these extensive laws and government regulations, we could become ineligible to receive government program reimbursement, suffer civil or criminal penalties or be required to make significant changes to our operations. In addition, we could be forced to expend considerable resources responding to an investigation or other enforcement action under these laws or regulations. For a more complete description of certain of these laws and regulations, see “Business—Regulation and Healthcare Reform” in Item 1.
The healthcare industry is subject to extensive federal, state and local laws and regulations relating to (1) facility and professional licensure, including certificates of need, (2) conduct of operations, including financial relationships among healthcare providers, Medicare fraud and abuse and physician self-referral, (3) addition of facilities and services and enrollment of newly developed facilities in the Medicare program, (4) payment for services and (5) safeguarding protected health information.
Both federal and state regulatory agencies inspect, survey and audit our facilities to review our compliance with these laws and regulations. While our facilities intend to comply with the existing licensing, Medicare certification requirements and accreditation standards, there can be no assurance that these regulatory authorities will determine that all applicable requirements are fully met at any given time. A determination by any of these regulatory authorities that a facility is not in compliance with these requirements could lead to the imposition of requirements that the facility takes corrective action, assessment of fines and penalties, or loss of licensure or Medicare certification of accreditation. These consequences could have an adverse effect on our Company.
The Company’s CIA imposes certain compliance related functions and reporting obligations on the Company. In addition, the CIA requires the Company to engage an independent review organization to conduct annual audits of randomly selected Company clinics in order to review compliance with federal requirements relating to the proper billing and coding for claims. While our facilities intend to comply with the federal requirements for properly coding and billing claims for reimbursement, there can be no assurance that these audits will determine that all applicable requirements are fully met at the clinics that are reviewed. In addition, a failure to fully comply with the requirements of the CIA may subject the Company to the assessment of fines and penalties, or exclusion from participation in the Medicare program. These consequences could have an adverse effect on our Company.
Decreases in Medicare reimbursement rates, implementation of annual caps, and payment reductions applied to the second and subsequent therapy services will adversely affect our financial results.
The Medicare program reimburses outpatient rehabilitation providers based on the Medicare Physician Fee Schedule (“MPFS”). The MPFS rates have historically been subject to an automatic annual update based on a formula, called the sustainable growth rate (“SGR”) formula. The use of the SGR formula would have resulted in calculated automatic reductions in rates in every year since 2002; however, for each year through
13
September 30, 2015, Centers for Medicare & Medicaid Services (“CMS”) or Congress has taken action to prevent the implementation of SGR formula reductions. On April 16, 2015, the Medicare Access and CHIP Reauthorization Act of 2015 (“MACRA”) was signed into law, eliminating the SGR formula and the associated annual automatic rate reductions. For services provided between January 1, 2015 and June 30, 2015 a 0% payment update was applied to the Medicare physician fee schedule payment rates; for services provided between July 1, 2015 and December 31, 2015 a 0.5% increase was applied to the fee schedule payment rates; for services provided in 2016 a 0.3% decrease is being applied to the fee schedule payment rates, and for 2017 through 2019, a 0.5% increase will be applied each year to the fee schedule payment rates, unless further adjusted by CMS. In addition, the MACRA promotes the development of new payment models that focus on quality and outcomes.
The Budget Control Act of 2011 increased the federal debt ceiling in connection with deficit reductions over the next ten years, and requires automatic reductions in federal spending by approximately $1.2 trillion. Payments to Medicare providers are subject to these automatic spending reductions, subject to a 2% cap. On April 1, 2013, a 2% reduction to Medicare payments was implemented.
As a result of the Balanced Budget Act of 1997, the formula for determining the total amount paid by Medicare in any one year for outpatient physical therapy, occupational therapy, and/or speech-language pathology services provided to any Medicare beneficiary (i.e., the “Therapy Cap” or “Limit”) was established. Based on the statutory definitions which constrained how the Therapy Cap would be applied, there is one Limit for Physical Therapy and Speech Language Pathology Services combined, and one Limit for Occupational Therapy. For 2015, the annual Limit on outpatient therapy services was $1,940 for Physical and Speech Language Pathology Services combined and $1,940 for Occupational Therapy Services. For 2016, the annual Limit on outpatient therapy services is $1,960 for Physical and Speech Language Pathology Services combined and $1,960 for Occupational Therapy Services. Historically, these Therapy Caps applied to outpatient therapy services provided in all settings, except for services provided in departments of hospitals. However, the Protecting Access to Medicare Act of 2014, and prior legislation, extended the Therapy Caps to services furnished in hospital outpatient department settings. The application of these annual limits to hospital outpatient department settings will sunset on December 31, 2017 unless Congress extends it.
In the Deficit Reduction Act of 2005, Congress implemented an exceptions process to the annual Limit for therapy expenses for therapy services above the annual Limit. Therapy services above the annual Limit that are medically necessary satisfy an exception to the annual Limit and such claims are payable by the Medicare program. The Protecting Access to Medicare Act of 2014 extended the exceptions process for outpatient therapy caps through March 31, 2015. The MACRA further extended the exceptions process for outpatient therapy caps through December 31, 2017. Unless Congress extends the exceptions process further, the therapy caps will apply to all outpatient therapy services beginning January 1, 2018, except those services furnished and billed by outpatient hospital departments. For any claim above the annual Limit, the claim must contain a modifier indicating that the services are medically necessary and justified by appropriate documentation in the medical record.
Furthermore, under the Middle Class Tax Relief and Job Creation Act of 2012 (“MCTRA”), since October 1, 2012, patients who met or exceeded $3,700 in therapy expenditures during a calendar year have been subject to a manual medical review to determine whether applicable payment criteria are satisfied. The $3,700 threshold is applied to Physical Therapy and Speech Language Pathology Services; a separate $3,700 threshold is applied to the Occupational Therapy. The MACRA directed CMS to modify the manual medical review process such that those reviews will no longer apply to all claims exceeding the $3,700 threshold and instead will be determined on a targeted basis based on a variety of factors that CMS considers appropriate. The new factors have applied to exception requests for which CMS did not conduct a medical review by July 15, 2015.
CMS adopted a multiple procedure payment reduction (“MPPR”) for therapy services in the final update to the MPFS for calendar year 2011. The MPPR applied to all outpatient therapy services paid under Medicare Part B — occupational therapy, physical therapy and speech-language pathology. Under the policy, the Medicare program pays 100% of the practice expense component of the Relative Value Unit (“RVU”) for the therapy procedure with the highest practice expense RVU, then reduces the payment for the practice expense component for the second and subsequent therapy procedures or units of service furnished during the same day for the same patient, regardless of whether those therapy services are furnished in separate sessions. Since 2013, the practice expense component for the second and subsequent therapy service furnished during the same day for the same
14
patient was reduced by 50%. In addition, the MCTRA directed CMS to implement a claims-based data collection program to gather additional data on patient function during the course of therapy in order to better understand patient conditions and outcomes. All practice settings that provide outpatient therapy services are required to include this data on the claim form. Since 2013, therapists have been required to report new codes and modifiers on the claim form that reflect a patient’s functional limitations and goals at initial evaluation, periodically throughout care, and at discharge; CMS has rejected claims if the required data is not included in the claim.
The Physician Quality Reporting System, or “PQRS,” is a CMS reporting program that uses a combination of incentive payments and payment reductions to promote reporting of quality information by “eligible professionals.” Although physical therapists, occupational therapists and qualified speech-language therapists are generally able to participate in the PQRS program, therapy professionals for whose services we bill through our certified rehabilitation agencies cannot participate because the Medicare claims processing systems currently cannot accommodate institutional providers such as certified rehabilitation agencies. Eligible professionals, such as those of our therapy professionals for whose services we bill using their individual Medicare provider numbers, who do not satisfactorily report data on quality measures will be subject to a 2% reduction in their Medicare payment in 2016 and 2017.
Statutes, regulations, and payment rules governing the delivery of therapy services to Medicare beneficiaries are complex and subject to interpretation. We believe we are in compliance in all material respects with all applicable laws and regulations and are not aware of any pending or threatened investigations involving allegations of potential wrongdoing that would have a material effect on our financial statements as of December 31, 2015. Compliance with such laws and regulations can be subject to future government review and interpretation, as well as significant regulatory action including fines, penalties, and exclusion from the Medicare program.
Given the history of frequent revisions to the Medicare program and its reimbursement rates and rules, we may not continue to receive reimbursement rates from Medicare that sufficiently compensate us for our services or, in some instances, cover our operating costs. Limits on reimbursement rates or the scope of services being reimbursed could have a material adverse effect on our revenue, financial condition and results of operations. Additionally, any delay or default by the federal or state governments in making Medicare and/or Medicaid reimbursement payments could materially and, adversely, affect our business, financial condition and results of operations.
Revenue we receive from Medicare and Medicaid is subject to potential retroactive reduction.
Payments we receive from Medicare and Medicaid can be retroactively adjusted after examination during the claims settlement process or as a result of post-payment audits. Payors may disallow our requests for reimbursement, or recoup amounts previously reimbursed, based on determinations by the payors or their third-party audit contractors that certain costs are not reimbursable because either adequate or additional documentation was not provided or because certain services were not covered or deemed to not be medically necessary. Significant adjustments, recoupments or repayments of our Medicare or Medicaid revenue, and the costs associated with complying with investigative audits by regulatory and governmental authorities, could adversely affect our financial condition and results of operations.
Additionally, from time to time we become aware, either based on information provided by third parties and/or the results of internal audits, of payments from payor sources that were either wholly or partially in excess of the amount that we should have been paid for the service provided. Overpayments may result from a variety of factors, including insufficient documentation supporting the services rendered or medical necessity of the services or other failures to document the satisfaction of the necessary conditions of payment. We are required by law in most instances to refund the full amount of the overpayment after becoming aware of it, and failure to do so within requisite time limits imposed by the law could lead to significant fines and penalties being imposed on us. Furthermore, our initial billing of and payments for services that are unsupported by the requisite documentation and satisfaction of any other conditions of payment, regardless of our awareness of the failure at the time of the billing or payment, could expose us to significant fines and penalties. We, and/or certain of our operating companies, could also be subject to exclusion from participation in the Medicare or Medicaid programs in some circumstances as well, in addition to any monetary or other fines, penalties or sanctions that we may incur under applicable federal and/or state law. Our repayment of any such amounts, as well as any fines, penalties or other sanctions that we may incur, could be significant and could have a material and adverse effect on our results of operations and financial condition.
15
From time to time we are also involved in various external governmental investigations, audits and reviews. Reviews, audits and investigations of this sort can lead to government actions, which can result in the assessment of damages, civil or criminal fines or penalties, or other sanctions, including restrictions or changes in the way we conduct business, loss of licensure or exclusion from participation in government programs. Failure to comply with applicable laws, regulations and rules could have a material and adverse effect on our results of operations and financial condition. Furthermore, becoming subject to these governmental investigations, audits and reviews can also require us to incur significant legal and document production expenses as we cooperate with the government authorities, regardless of whether the particular investigation, audit or review leads to the identification of underlying issues.
As a result of increased post-payment reviews of claims we submit to Medicare for our services, we may incur additional costs and may be required to repay amounts already paid to us.
We are subject to regular post-payment inquiries, investigations and audits of the claims we submit to Medicare for payment for our services. These post-payment reviews have increased as a result of government cost-containment initiatives. These additional post-payment reviews may require us to incur additional costs to respond to requests for records and to pursue the reversal of payment denials, and ultimately may require us to refund amounts paid to us by Medicare that are determined to have been overpaid.
For a further description of this and other laws and regulations involving governmental reimbursements, see “Business—Sources of Revenue” and “—Regulation and Healthcare Reform” in Item 1.
If we fail to accurately report using the new ICD-10 coding system, our operations could be adversely affected.
Since October 1, 2015, Health plans and providers are required to report billing codes for third party claims using the new ICD-10 coding system, which greatly expanded the number and detail of billing codes used for third-party claims. It is possible that we could experience disruption or delays in payment due to technical or coding errors or other implementation issues involving our systems or the systems and implementation efforts of health plans and their business partners.
An economic downturn, state budget pressures, sustained unemployment and continued deficit spending by the federal government may result in a reduction in reimbursement and covered services.
An economic downturn could have a detrimental effect on our revenues. Historically, state budget pressures have translated into reductions in state spending. Given that Medicaid outlays are a significant component of state budgets, we can expect continuing cost containment pressures on Medicaid outlays for our services in the states in which we operate. In addition, an economic downturn, coupled with sustained unemployment, may also impact the number of enrollees in managed care programs as well as the profitability of managed care companies, which could result in reduced reimbursement rates.
The existing federal deficit, as well as deficit spending by federal and state governments as the result of adverse developments in the economy or other reasons, can lead to continuing pressure to reduce governmental expenditures for other purposes, including government-funded programs in which we participate, such as Medicare and Medicaid. Such actions in turn may adversely affect our results of operations.
We depend upon reimbursement by third-party payors.
Substantially all of our revenues are derived from private and governmental third-party payors. In 2015, approximately 75.5% of our revenues were derived collectively from managed care plans, commercial health insurers, workers’ compensation payors, and other private pay revenue sources while approximately 24.5% of our revenues were derived from Medicare and Medicaid. Initiatives undertaken by industry and government to contain healthcare costs affect the profitability of our clinics. These payors attempt to control healthcare costs by contracting with healthcare providers to obtain services on a discounted basis. We believe that this trend will continue and may limit reimbursement for healthcare services. If insurers or managed care companies from whom we receive substantial payments were to reduce the amounts they pay for services, our profit margins may decline, or we may lose patients if we choose not to renew our contracts with these insurers at lower rates. In addition, in certain geographical areas, our clinics must be approved as providers by key health maintenance organizations and preferred provider plans. Failure to obtain or maintain these approvals would adversely affect our financial results.
16
In recent years, through legislative and regulatory actions, the federal government has made substantial changes to various payment systems under the Medicare program. See “Business—Sources of Revenue” in Item 1 for more information. President Obama signed into law comprehensive reforms to the healthcare system, including changes to Medicare reimbursement. Additional reforms or other changes to these payment systems may be proposed or adopted, either by the U.S. Congress or by CMS, including bundled payments, outcomes-based payment methodologies and a shift away from traditional fee-for-service reimbursement. If revised regulations are adopted, the availability, methods and rates of Medicare reimbursements for services of the type furnished at our facilities could change. Some of these changes and proposed changes could adversely affect our business strategy, operations and financial results.
We face inspections, reviews, audits and investigations under federal and state government programs and contracts. These audits could have adverse findings that may negatively affect our business.
As a result of our participation in the Medicare and Medicaid programs, we are subject to various governmental inspections, reviews, audits and investigations to verify our compliance with these programs and applicable laws and regulations. Managed care payors may also reserve the right to conduct audits. An adverse inspection, review, audit or investigation could result in:
| • | refunding amounts we have been paid pursuant to the Medicare or Medicaid programs or from managed care payors; |
| • | state or federal agencies imposing fines, penalties and other sanctions on us; |
| • | temporary suspension of payment for new patients to the facility or agency; |
| • | decertification or exclusion from participation in the Medicare or Medicaid programs or one or more managed care payor networks; |
| • | expansion of the scope of our Corporate Integrity Agreement; |
| • | damage to our reputation; |
| • | the revocation of a facility’s or agency’s license; and |
| • | loss of certain rights under, or termination of, our contracts with managed care payors. |
If adverse inspections, reviews, audits or investigations occur and any of the results noted above occur, it could have a material adverse effect on our business and operating results.
Our facilities are subject to extensive federal and state laws and regulations relating to the privacy of individually identifiable information.
HIPAA required the HHS to adopt standards to protect the privacy and security of individually identifiable health-related information. The department released final regulations containing privacy standards in 2000 and published revisions to the final regulations in 2002. The privacy regulations extensively regulate the use and disclosure of individually identifiable health-related information. The regulations also provide patients with significant rights related to understanding and controlling how their health information is used or disclosed. The security regulations require healthcare providers to implement administrative, physical and technical practices to protect the security of individually identifiable health information that is maintained or transmitted electronically. HITECH, which was signed into law in 2009, enhanced the privacy, security and enforcement provisions of HIPAA by, among other things establishing security breach notification requirements, allowing enforcement of HIPAA by state attorneys general, and increasing penalties for HIPAA violations. Violations of HIPAA or HITECH could result in civil or criminal penalties.
In addition to HIPAA, there are numerous federal and state laws and regulations addressing patient and consumer privacy concerns, including unauthorized access or theft of personal information. State statutes and regulations vary from state to state. Lawsuits, including class actions and action by state attorneys general, directed at companies that have experienced a privacy or security breach also can occur.
The Company and its clinics have established policies and procedures in an effort to ensure compliance with these privacy related requirements. However, if there is a breach, we may be subject to various penalties and damages and may be required to incur costs to mitigate the impact of the breach on affected individuals.
17
We may be adversely affected by a cyber attack that could compromise our information technologies, which may cause a violation of HIPAA or HITECH.
In the normal course of business, our information technology systems hold sensitive patient information including patient demographic data, eligibility for various medical plans including Medicare and Medicaid and protected health information, which is subject to HIPAA and HITECH. We maintain our information technology systems with safeguards protecting against cyber-attacks, including passive intrusion protection, firewalls and virus detection software. However, these safeguards do not ensure that a significant cyber attack could not occur. A cyber attack that bypasses our information technology security systems could cause the loss of protected health information, or other data subject to privacy laws, the loss of proprietary business information, or a material disruption to our information technology business systems resulting in a material adverse effect on our business, financial condition, and results of operations or cash flows. In addition, our future results could be adversely affected due to the theft, destruction, loss, misappropriation or release of protected health information, other confidential data or proprietary business information, operational or business delays resulting from the disruption of information technology systems and subsequent clean-up and mitigation activities, negative publicity resulting in reputation or brand damage with clients, members, or industry peers, or regulatory action taken as a result of such incident.
We depend upon the cultivation and maintenance of relationships with the physicians in our markets.
Our success is dependent upon referrals from physicians in the communities our clinics serve and our ability to maintain good relations with these physicians and other referral sources. Physicians referring patients to our clinics are free to refer their patients to other therapy providers or to their own physician owned therapy practice. If we are unable to successfully cultivate and maintain strong relationships with physicians and other referral sources, our business may decrease and our net operating revenues may decline.
We depend upon our ability to recruit and retain experienced physical therapists.
Our revenue generation is dependent upon referrals from physicians in the communities our clinics serve, and our ability to maintain good relations with these physicians. Our therapists are the front line for generating these referrals and we are dependent on their talents and skills to successfully cultivate and maintain strong relationships with these physicians. If we cannot recruit and retain our base of experienced and clinically skilled therapists, our business may decrease and our net operating revenues may decline. Periodically, we have clinics in isolated communities that are temporarily unable to operate due to the unavailability of a therapist who satisfies our standards.
Our revenues may fluctuate due to weather.
We have a significant number of clinics in states that normally experience snow and ice during the winter months. Also, a significant number of our clinics are located in states along the Gulf Coast and Atlantic Coast which are subject to periodic winter storms, hurricanes and other severe storm systems. Periods of severe weather may cause physical damage to our facilities or prevent our staff or patients from traveling to our clinics, which may cause a decrease in our net operating revenues.
We operate in a highly competitive industry.
We encounter competition from local, regional or national entities, some of which have superior resources or other competitive advantages. Intense competition may adversely affect our business, financial condition or results of operations. For a more complete description of this competitive environment, see “Business—Competition” in Item 1. An adverse effect on our business, financial condition or results of operations may require us to write-down goodwill.
We may incur closure costs and losses.
The competitive, economic or reimbursement conditions in our markets in which we operate may require us to reorganize or to close certain clinics. In the event a clinic is reorganized or closed, we may incur losses and closure costs. The closure costs and losses may include, but are not limited to, lease obligations, severance, and write-down or write-off of goodwill and other intangible assets.
18
Future acquisitions may use significant resources, may be unsuccessful and could expose us to unforeseen liabilities.
As part of our growth strategy, we intend to continue pursuing acquisitions of outpatient physical therapy clinics. Acquisitions may involve significant cash expenditures, potential debt incurrence and operational losses, dilutive issuances of equity securities and expenses that could have an adverse effect on our financial condition and results of operations. Acquisitions involve numerous risks, including:
| • | the difficulty and expense of integrating acquired personnel into our business; |
| • | the diversion of management’s time from existing operations; |
| • | the potential loss of key employees of acquired companies; |
| • | the difficulty of assignment and/or procurement of managed care contractual arrangements; and |
| • | the assumption of the liabilities and exposure to unforeseen liabilities of acquired companies, including liabilities for failure to comply with healthcare regulations. |
Failure to maintain effective internal control over our financial reporting could have an adverse effect on our ability to report our financial results on a timely and accurate basis.
We produce our consolidated financial statements in accordance with the requirements of accounting principles generally accepted in the United States of America. Effective internal control over financial reporting is necessary for us to provide reliable financial reports, to help mitigate the risk of fraud and to operate successfully. We are required by federal securities laws to document and test our internal control procedures in order to satisfy the requirements of the Sarbanes-Oxley Act of 2002, which requires annual management assessments of the effectiveness of our internal control over financial reporting.
Testing and maintaining our internal control over financial reporting can be expensive and divert our management’s attention from other matters that are important to our business. We may not be able to conclude on an ongoing basis that we have effective internal control over financial reporting in accordance with applicable law, or our independent registered public accounting firm may not be able or willing to issue an unqualified attestation report if we conclude that our internal control over financial reporting is not effective. If we fail to maintain effective internal control over financial reporting, or our independent registered public accounting firm is unable to provide us with an unqualified attestation report on our internal control, we could be required to take costly and time-consuming corrective measures, be required to restate the affected historical financial statements, be subjected to investigations and/or sanctions by federal and state securities regulators, and be subjected to civil lawsuits by security holders. Any of the foregoing could also cause investors to lose confidence in our reported financial information and in our company and would likely result in a decline in the market price of our stock and in our ability to raise additional financing if needed in the future.
Issuance of shares in connection with financing transactions or under stock incentive plans will dilute current stockholders.
Pursuant to our stock incentive plans, our Compensation Committee of the Board, consisting solely of independent directors, is authorized to grant stock awards to our employees, directors and consultants. Shareholders will incur dilution upon the exercise of any outstanding stock awards or the grant of any restricted stock. In addition, if we raise additional funds by issuing additional common stock, or securities convertible into or exchangeable or exercisable for common stock, further dilution to our existing stockholders will result, and new investors could have rights superior to existing stockholders.
The number of shares of our common stock eligible for future sale could adversely affect the market price of our stock.
At December 31, 2015, we had reserved approximately 349,000 shares for future equity grants. These shares of common stock are registered for sale or resale on currently effective registration statements and have been approved by stockholders. We may issue additional restricted securities or register additional shares of common stock under the Securities Act of 1933, as amended (the “Securities Act”), in the future. The issuance of a significant number of shares of common stock upon the exercise of stock options or the availability for sale, or sale, of a substantial number of the shares of common stock eligible for future sale under effective registration statements, under Rule 144 or otherwise, could adversely affect the market price of the common stock.
19
Provisions in our articles of incorporation and bylaws could delay or prevent a change in control of our company, even if that change would be beneficial to our stockholders.
Certain provisions of our articles of incorporation and bylaws may delay, discourage, prevent or render more difficult an attempt to obtain control of our company, whether through a tender offer, business combination, proxy contest or otherwise. These provisions include the charter authorization of “blank check” preferred stock and a restriction on the ability of stockholders to call a special meeting.
ITEM 1B. UNRESOLVED STAFF COMMENTS.
Not Applicable.
We lease the properties used for our clinics under non-cancelable operating leases with terms ranging from one to five years, with the exception of the property for one clinic which we own. We intend to lease the premises for any new clinic locations except in rare instances where leasing is not a cost-effective alternative. Our typical clinic occupies 1,500 to 3,000 square feet.
We also lease our executive offices located in Houston, Texas, under a non-cancelable operating lease expiring in April 2022. We currently occupy approximately 39,452 square feet of space (including allocations for common areas) at our executive offices.
We are involved in litigation and other proceedings arising in the ordinary course of business. While the ultimate outcome of lawsuits or other proceedings cannot be predicted with certainty, we do not believe the impact of existing lawsuits or other proceedings will have a material impact on our business, financial condition or results of operations.
ITEM 4. MINE SAFETY DISCLOSURES.
Not Applicable.
20
PART II
ITEM 5. MARKET FOR REGISTRANT’S COMMON EQUITY, RELATED STOCKHOLDER MATTERS AND ISSUER PURCHASES OF EQUITY SECURITIES.
PRICE QUOTATIONS
Our common stock has traded on the New York Stock Exchange (“NYSE”) since August 14, 2012 under the symbol “USPH.” Prior to that, our common stock was traded on the Nasdaq Global Select Market under the symbol “USPH”. As of March 4, 2016, there were __ holders of record of our outstanding common stock. The table below indicates the high and low sales prices of our common stock reported for the periods presented.
2015 |
2014 |
|||||||||||
Quarter |
High |
Low |
High |
Low |
||||||||
First |
$ | 50.79 | $ | 38.17 | $ | 37.25 | $ | 30.16 | ||||
Second |
55.22 | 43.13 | 35.23 | 29.56 | ||||||||
Third |
56.37 | 42.59 | 37.19 | 33.21 | ||||||||
Fourth |
55.75 | 43.18 | 44.00 | 34.00 | ||||||||
During 2015, we paid a regular quarterly dividend of $0.15 per share totaling $0.60 per share, which amounted to a total of aggregate cash payments of dividends to holders of our common stock in 2015 of approximately $7.4 million. During 2014, we paid a quarterly dividend of $0.12 per share totaling $0.48 per share for 2014, which amounted to a total of aggregate cash payments of dividends to holders of our common stock in 2014 of approximately $5.9 million. In 2016, our Board of Directors declared a quarterly dividend of $.17 per share payable to shareholders of record on March 18, 2016 to be paid on April 1, 2016. We are currently restricted from paying dividends in excess of $10,000,000 in any fiscal year on our common stock under the Credit Agreement.
FIVE YEAR PERFORMANCE GRAPH
The performance graph and related description shall not be deemed incorporated by reference into any filing under the Securities Act or under the Exchange Act, except to the extent that the Company specifically incorporates this information by reference. In addition, the performance graph and the related description shall not be deemed “soliciting material” or “filed” with the SEC or subject to Regulation 14A or 14C.
Prior to August 14, 2012, our common stock traded on the Nasdaq Global Select Market. On August 14, 2012, our common stock began trading on NYSE. The following performance graph compares the cumulative total stockholder return of our common stock to The NYSE Composite Index and the NYSE Health Care Index for the period from December 31, 2010 through December 31, 2015. The graph assumes that $100 was invested in our common stock and the common stock of each of the companies listed on The NYSE Composite Index and The NYSE Health Care Index on December 31, 2010 and that any dividends were reinvested.
21
Comparison of Five Years Cumulative Total Return for the Year Ended December 31, 2015
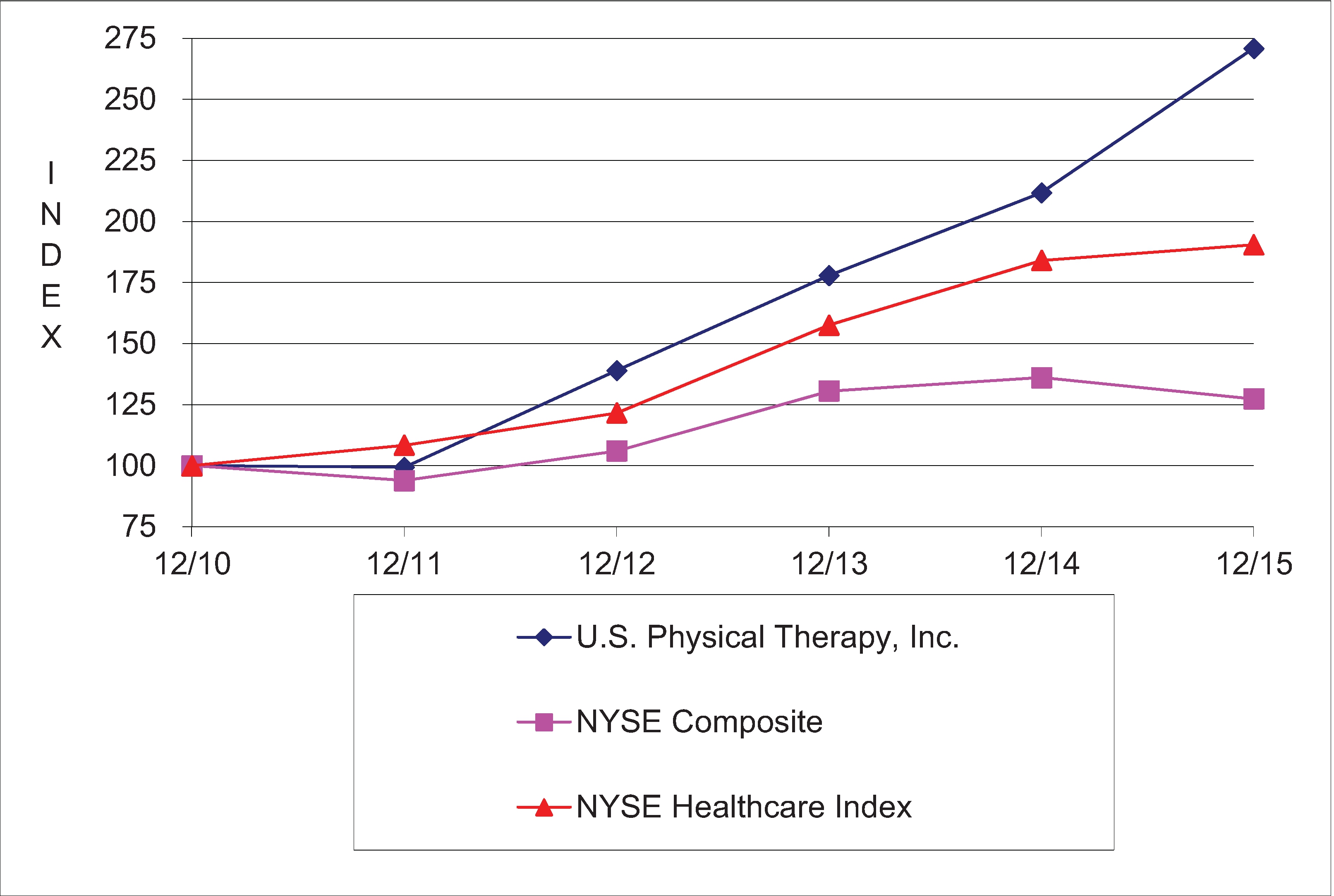
12/10 |
12/11 |
12/12 |
12/13 |
12/14 |
12/15 |
|||||||||||||
U. S. Physical Therapy, Inc. |
100 | 99 | 139 | 178 | 212 | 271 | ||||||||||||
NYSE Composite |
100 | 94 | 106 | 131 | 136 | 127 | ||||||||||||
NYSE Healthcare Index |
100 | 108 | 122 | 158 | 184 | 190 | ||||||||||||
ITEM 6. SELECTED FINANCIAL DATA.
The following selected financial data from continuing operations should be read in conjunction with the description of our critical accounting policies set forth in “Management’s Discussion and Analysis of Results of Operations and Financial Condition” and the Consolidated Financial Statements and Notes included herein.
For the Years Ended December 31, |
||||||||||||||||
2015 |
2014 |
2013 |
2012 |
2011 |
||||||||||||
($ in thousands, except per share data) |
||||||||||||||||
Net revenues |
$ | 331,302 | $ | 305,074 | $ | 264,058 | $ | 249,651 | $ | 231,523 | ||||||
Income from continuing operations including non-controlling interests, net of tax |
$ | 31,691 | $ | 30,424 | $ | 26,003 | $ | 26,640 | $ | 26,679 | ||||||
Net income including non-controlling interests |
$ | 31,691 | $ | 30,424 | $ | 20,996 | $ | 26,217 | $ | 29,783 | ||||||
Net income attributable to common shareholders |
$ | 22,279 | $ | 20,853 | $ | 17,492 | $ | 18,212 | $ | 18,812 | ||||||
Basic earnings per share attributable to common shareholders: |
$ | 1.80 | $ | 1.71 | $ | 1.45 | $ | 1.54 | $ | 1.60 | ||||||
Diluted earnings per share attributable to common shareholders: |
$ | 1.80 | $ | 1.71 | $ | 1.45 | $ | 1.53 | $ | 1.57 | ||||||
Dividends declared and paid per common share |
$ | 0.60 | $ | 0.48 | $ | 0.40 | $ | 0.76 | $ | 0.32 | ||||||
22
On December 31, |
||||||||||||||||
2015 |
2014 |
2013 |
2012 |
2011 |
||||||||||||
($ in thousands) |
||||||||||||||||
Total assets. |
$ | 279,913 | $ | 244,551 | $ | 224,135 | $ | 171,714 | $ | 163,252 | ||||||
Long-term debt, less current portion |
$ | 48,335 | $ | 34,734 | $ | 40,650 | $ | 17,575 | $ | 23,784 | ||||||
Working capital |
$ | 41,175 | $ | 29,347 | $ | 26,488 | $ | 29,015 | $ | 29,343 | ||||||
Current ratio |
3.17 | 2.15 | 2.14 | 2.78 | 2.80 | |||||||||||
Total long-term debt to total capitalization |
0.25 | 0.21 | 0.27 | 0.13 | 0.20 | |||||||||||
ITEM 7. MANAGEMENT’S DISCUSSION AND ANALYSIS OF FINANCIAL CONDITION AND RESULTS OF OPERATIONS.
EXECUTIVE SUMMARY
Our Business. We operate outpatient physical therapy clinics that provide pre- and post-operative care and treatment for a variety of orthopedic-related disorders and sports-related injuries, neurologically-related injuries and rehabilitation of injured workers. At December 31, 2015, we operated 508 clinics in 42 states. The average age of our clinics at December 31, 2015 was 9.4 years.
During 2015, 2014 and 2013, we completed the following multi-clinic acquisitions:
Acquisition |
Date |
% Interest Acquired |
Number of Clinics |
||||
2015 |
|||||||
January 2015 Acquisition |
January 31 |
60 | % |
9 | |||
April 2015 Acquisition |
April 30 |
70 | % |
3 | |||
June 2015 Acquisition |
June 30 |
70 | % |
4 | |||
December 2015 Acquisition |
December 31 |
59 | % |
4 | |||
2014 |
|||||||
April 2014 Acquisition |
April 30, 2014 |
70 | % |
13 | |||
August 2014 Acquisition |
August 1, 2014 |
100 | % |
3 | |||
2013 |
|||||||
February 2013 Acquisition |
February 28, 2013 |
72 | % |
9 | |||
April 2013 Acquisition |
April 30, 2013 |
50 | % |
5 | |||
May 2013 Acquistion |
May 24, 2013 |
80 | % |
5 | |||
December 9, 2013 Acquisition |
December 9, 2013 |
60 | % |
12 | |||
December 13, 2013 Acquisition |
December 13, 2013 |
90 | % |
11 | |||
In addition to the multi-clinic acquisitions, we acquired a 60% interest in a single clinic practice during 2015. We acquired four individual clinics in separate transactions during 2014, and we acquired three individual clinics in separate transactions during 2013.
The results of operations of the acquired clinics have been included in our consolidated financial statements since the date of their acquisition.
On September 30, 2013, we sold the remainder of our physician services business. Previously, the Company closed its two physician services facilities – one in August 2013 and the other in December 2012. As previously disclosed in the Company’s public filings, the physician services business incurred negative gross margins in 2012 and through the first nine months of 2013. Revenues from physician services were generated by patient visits, franchise arrangements and fees from third parties. The results of operations and the loss on the sale of the physician services business have been reclassified to discontinued operations for all periods presented.
23
The following table details the losses from discontinued operations reported for the physician services business (in thousands):
Year Ended December 31, 2013 |
|||
Net revenues |
$ | 864 | |
Operating cost |
1,537 | ||
Gross margin |
(673 | ) |
|
Direct general and administrative expenses less proceeds |
1,176 | ||
Write off goodwill and other intangible assets |
6,338 | ||
Loss from discontinued operations, before tax |
(8,187 | ) |
|
Tax benefit (provision) |
3,180 | ||
(Loss) income from discontinued operations |
$ | (5,007 | ) |
In addition to our owned clinics, we also manage physical therapy facilities for third parties. As of December 31, 2015, we had 21 physician or hospital owned facilities under management.
CRITICAL ACCOUNTING POLICIES
Critical accounting policies are those that have a significant impact on our results of operations and financial position involving significant estimates requiring our judgment. Our critical accounting policies are:
Revenue Recognition. Revenues are recognized in the period in which services are rendered. Net patient revenues (patient revenues less estimated contractual adjustments) are reported at the estimated net realizable amounts from insurance companies, third-party payors, patients and others for services rendered. The Company has agreements with third-party payors that provide for payments to the Company at contracted amounts different from its established rates. The allowance for estimated contractual adjustments is based on terms of payor contracts and historical collection and write-off experience.
Contractual Allowances. Contractual allowances result from the differences between the rates charged for services performed and expected reimbursements by both insurance companies and government sponsored healthcare programs for such services. Medicare regulations and the various third party payors and managed care contracts are often complex and may include multiple reimbursement mechanisms payable for the services provided in our clinics. We estimate contractual allowances based on our interpretation of the applicable regulations, payor contracts and historical calculations. Each month the Company estimates its contractual allowance for each clinic based on payor contracts and the historical collection experience of the clinic and applies an appropriate contractual allowance reserve percentage to the gross accounts receivable balances for each payor of the clinic. Based on our historical experience, calculating the contractual allowance reserve percentage at the payor level is sufficient to allow us to provide the necessary detail and accuracy with our collectibility estimates. However, the services authorized and provided and related reimbursement are subject to interpretation that could result in payments that differ from our estimates. Payor terms are periodically revised necessitating continual review and assessment of the estimates made by management. Our billing system may not capture the exact change in our contractual allowance reserve estimate from period to period. Therefore, in order to assess the accuracy of our revenues and hence our contractual allowance reserves, our management regularly compares its cash collections to corresponding net revenues measured both in the aggregate and on a clinic-by-clinic basis. In the aggregate, the historical difference between net revenues and corresponding cash collections has generally reflected a difference within approximately 1% of net revenues. Additionally, analysis of subsequent period’s contractual write-offs on a payor basis reflects a difference within approximately 1% between the actual aggregate contractual reserve percentage as compared to the estimated contractual allowance reserve percentage associated with the same period end balance. As a result, we believe that a reasonable likely change in the contractual allowance reserve estimate would not be more than 1% at December 31, 2015. For purposes of demonstrating the sensitivity of this estimate on the Company’s financial condition, a one percent increase or decrease in our aggregate contractual allowance reserve percentage would decrease or increase, respectively, net patient revenue by approximately $845,000 for the year ended December 31, 2015. Management believes the changes in the estimate of the contractual allowance reserve for the periods ended December 31, 2015, 2014 and 2013 have not been material to the statement of operations.
24
The following table sets forth information regarding our patient accounts receivable as of the dates indicated (in thousands):
December 31, |
||||||
2015 |
2014 |
|||||
Gross patient accounts receivable |
$ | 84,584 | $ | 79,721 | ||
Less contractual allowances |
46,909 | 45,161 | ||||
Subtotal - accounts receivable |
37,675 | 34,560 | ||||
Less allowance for doubtful accounts |
1,444 | 1,669 | ||||
Net patient accounts receivable |
$ | 36,231 | $ | 32,891 | ||
The following table presents our patient accounts receivable aging by payor class as of the dates indicated (in thousands):
December 31, 2015 |
December 31, 2014 |
|||||||||||||||||
Payor |
Current to 120 Days |
120+ Days |
Total |
Current to 120 Days |
120+ Days |
Total |
||||||||||||
Managed Care/Commercial Plans |
$ | 12,936 | $ | 1,381 | $ | 14,317 | $ | 11,906 | $ | 1,418 | $ | 13,324 | ||||||
Medicare/Medicaid |
7,380 | 1,107 | 8,487 | 7,121 | 1,391 | 8,512 | ||||||||||||
Workers Compensation* |
7,945 | 1,144 | 9,089 | 7,160 | 1,136 | 8,296 | ||||||||||||
Self-pay |
2,296 | 1,504 | 3,800 | 1,250 | 1,461 | 2,711 | ||||||||||||
Other** |
1,165 | 817 | 1,982 | 1,171 | 546 | 1,717 | ||||||||||||
Totals |
$ | 31,722 | $ | 5,953 | $ | 37,675 | $ | 28,608 | $ | 5,952 | $ | 34,560 | ||||||
| * | Workers compensation is paid by state administrators or their designated agents. |
| ** | Other includes primarily litigation claims and, to a lesser extent, vehicular insurance claims. |
Reimbursement for Medicare beneficiaries is based upon a fee schedule published by HHS. For a more complete description of our third party revenue sources, see “Business—Sources of Revenue” in Item 1.
Provision for Doubtful Accounts. We determine our provision for doubtful accounts based on the specific agings and payor classifications at each clinic. We review the accounts receivable aging and rely on prior experience with particular payors to determine an appropriate reserve for doubtful accounts. Historically, clinics that have a large number of aged accounts generally have less favorable collection experience, and thus, require a higher allowance. Accounts that are ultimately determined to be uncollectible are written off against our bad debt provision. The amount of our aggregate provision for doubtful accounts is regularly reviewed for adequacy in light of current and historical experience.
Accounting for Income Taxes. We account for income taxes under the asset and liability method. Deferred tax assets and liabilities are recognized for the future tax consequences attributable to differences between the financial statement carrying amounts of existing assets and liabilities and their respective tax bases and operating loss and tax credit carryforwards. Deferred tax assets and liabilities are measured using enacted tax rates expected to apply to taxable income in the years in which those temporary differences are expected to be recovered or settled. The effect on deferred tax assets and liabilities of a change in tax rates is recognized in income in the period that includes the enactment date. The Company recognizes the financial statement benefit of a tax position only after determining that the relevant tax authority would more likely than not sustain the position following an audit. For tax positions meeting the more-likely-than-not threshold, the amount to be recognized in the financial statements is the largest benefit that has a greater than 50 percent likelihood of being realized upon ultimate settlement with the relevant tax authority.
We do not believe that we have any significant uncertain tax positions at December 31, 2015, nor is this expected to change within the next twelve months due to the settlement and expiration of statutes of limitation.
We did not have any accrued interest or penalties associated with any unrecognized tax benefits nor was any interest expense recognized during the twelve months ended December 31, 2015 and 2014.
25
Carrying Value of Long-Lived Assets. Our property and equipment, intangible assets and goodwill (collectively, our “long-lived assets”) comprise a significant portion of our total assets. The accounting standards require that we periodically, and upon the occurrence of certain events, assess the recoverability of our long-lived assets. If the carrying value of our property and equipment exceeds their undiscounted cash flows, we are required to write the carrying value down to estimated fair value.
Goodwill. The fair value of goodwill and other intangible assets with indefinite lives are tested for impairment annually and upon the occurrence of certain events, and are written down to fair value if considered impaired. We evaluate goodwill for impairment on at least an annual basis (in the third quarter) by comparing the fair value of its reporting units to the carrying value of each reporting unit including related goodwill. We operate a one segment business which is made up of various clinics within partnerships. The partnerships are components of regions and are aggregated to that operating segment level for the purpose of determining reporting units when performing the annual goodwill impairment test. In 2015 and 2014, we had six regions.
An impairment loss generally would be recognized when the carrying amount of the net assets of a reporting unit, inclusive of goodwill and other intangible assets, exceeds the estimated fair value of the reporting unit. The estimated fair value of a reporting unit is determined using two factors: (i) earnings prior to taxes, depreciation and amortization for the reporting unit multiplied by a price/earnings ratio used in the industry and (ii) a discounted cash flow analysis. A weight is assigned to each factor and the sum of each weight times the factor is considered the estimated fair value. For 2015, the factors (i.e., price/earnings ratio, discount rate and residual capitalization rate) were updated to reflect current market conditions. The evaluation of goodwill in 2015, 2014 and 2013 did not result in any goodwill amounts that were deemed impaired.
SELECTED OPERATING AND FINANCIAL DATA
The following table and discussion relates to continuing operations unless otherwise noted. The defined terms with their respective description used in the following discussion are listed below:
|
2015
|
Year ended December 31, 2015
|
|
2014
|
Year ended December 31, 2014
|
|
2013
|
Year ended December 31, 2013
|
|
New Clinics
|
Clinics opened or acquired during the year ended December 31, 2015
|
|
Mature Clinics
|
Clinics opened or acquired prior to January 1, 2015
|
|
2014 New Clinics
|
Clinics opened or acquired during the year ended December 31, 2014
|
|
2014 Mature Clinics
|
Clinics opened or acquired prior to January 1, 2014
|
|
2013 New Clinics
|
Clinics opened or acquired during the year ended December 31, 2013
|
|
2013 Mature Clinics
|
Clinics opened or acquired prior to January 1, 2013
|
The following table presents selected operating and financial data, used by management as key indicators of our operating performance:
For the Years Ended December 31, |
|||||||||
2015 |
2014 |
2013 |
|||||||
Number of clinics, at the end of period |
508 | 489 | 472 | ||||||
Working days |
255 | 255 | 255 | ||||||
Average visits per day per clinic |
24.1 | 22.9 | 21.5 | ||||||
Total patient visits |
3,080,166 | 2,818,815 | 2,440,590 | ||||||
Net patient revenue per visit |
$ | 105.28 | $ | 106.08 | $ | 105.83 | |||
26
RESULTS OF OPERATIONS
FISCAL YEAR 2015 COMPARED TO FISCAL 2014
| • | Net revenues rose 8.6 % to $331.3 million for 2015 from $305.1 million for 2014 primarily due to increases in net patient revenues which are discussed in detail below. |
| • | Net income attributable to common shareholders prior to the revaluation of non-controlling interests, increased 6.8% to $22.3 million, or $1.80 per diluted share, from $20.9 million, or $1.71 per diluted share. |
Net Patient Revenues
| • | Net patient revenues increased to $324.3 million for 2015 from $299.0 million for 2014, an increase of $25.3 million, or 8.5%. The increase in net patient revenues of $25.3 million consisted of an increase of $15.2 million from New Clinics and $10.1 million from Mature Clinics of which $10.3 million was related to 2014 New Clinics offset by a small decrease of $0.2 million related to 2014 Mature Clinics. During 2015, we acquired four multi-clinic groups for a total of 20 clinics. The net patient revenues from these multi-clinic groups are included in our results of operations since the respective date of their acquisition. See above table under “—Executive Summary” detailing our multi-clinic acquisitions. |
| • | Total patient visits increased to 3,080,200 for 2015 from 2,818,800 for 2014. The growth in patient visits was attributable to 150,200 visits in New Clinics primarily due to the acquisitions in 2015 and an increase of 111,200 visits for Mature Clinics primarily due to 2014 New Clinics. |
| • | The average net patient revenue per visit decreased to $105.28 in 2015 from $106.08 in 2014. |
Net patient revenues are based on established billing rates less allowances and discounts for patients covered by contractual programs and workers’ compensation. Net patient revenues reflect contractual and other adjustments, which we evaluate monthly, relating to patient discounts from certain payors. Payments received under these programs are based on predetermined rates and are generally less than the established billing rates of the clinics.
Other Revenues
Other revenues, consisting primarily of management fees, increased by $0.9 million, from $6.1 million in 2014 to $7.0 million in 2015. On December 31, 2015, we managed 21 third-party physical therapy facilities versus 16 on December 31, 2014.
Clinic Operating Costs
Clinic operating costs were $252.9 million, or 76.3% of net revenues, for 2015 and $228.9 million, or 75.0% of net revenues, for 2014. The increase was attributable to $13.9 million in operating costs for New Clinics, an increase in operating costs of $8.1 million for 2014 New Clinics and an increase of $2.0 million for 2014 Mature Clinics primarily resulting from 2013 New Clinics. Each component of clinic operating costs is discussed below:
Clinic Operating Costs—Salaries and Related Costs
Salaries and related costs increased to $180.5 million for 2015 from $163.4 million for 2014, an increase of $17.1 million, or 10.5%. Approximately $9.9 million of the increase was attributable to New Clinics and $5.6 million of the increase was due to a higher costs at various 2014 New Clinics due to a full year of activity (see table detailing acquisition dates above under “-Executive Summary”) and higher costs of $1.6 million at 2014 Mature Clinics. Salaries and related costs as a percentage of net revenues was 54.5% for 2015 and 53.6% for 2014.
Clinic Operating Costs—Rent, Clinic Supplies, Contract Labor and Other
Rent, clinic supplies, contract labor and other costs increased to $68.0 million for 2015 from $61.2 million for 2014, an increase of $6.8 million, or 11.2%. For 2015, New Clinics accounted for approximately $3.8 million of the increase and 2014 New Clinics accounted for approximately $2.5 million of the increase due to a full year of activity. Rent, clinic supplies, contract labor and other costs for 2014 Mature Clinics increased $0.5 million in 2015 as compared to 2014. Rent, clinic supplies, contract labor and other costs as a percent of net revenues was 20.5% for 2015 and 20.1% for 2014.
27
Clinic Operating Costs—Provision for Doubtful Accounts
The provision for doubtful accounts for net patient receivables was $4.2 million for 2015 and $4.1 million for 2014. As a percentage of net patient revenues, the provision for doubtful accounts was 1.3% for 2015 and 1.4% for 2014.
Our provision for doubtful accounts as a percentage of total patient accounts receivable was 3.8% at December 31, 2015 and 4.8% at December 31, 2014. The provision for doubtful accounts at the end of each period is based on a detailed, clinic-by-clinic review of overdue accounts and is regularly reviewed in the aggregate in light of historical experience.
The average accounts receivable days outstanding were 36 days for December 31, 2015 and 39 days for December 31, 2014. Net patient receivables in the amount of $4.4 million and $3.9 million were written-off in 2015 and 2014, respectively.
Closure Costs
For 2015 and 2014, closure costs amounted to $211,000 and $169,000, respectively.
Gross Margin
In 2015, the gross margin (net revenues less total clinic operating costs) increased by 2.9% to $78.4 million from $76.2 million in 2014. The gross margin percentage for 2015 was 23.7% as compared to 25.0% for 2014.
Corporate Office Costs
Corporate office costs, consisting primarily of salaries, benefits and equity based compensation of corporate office personnel and directors, rent, insurance costs, depreciation and amortization, travel, legal, compliance, professional, marketing and recruiting fees, were $31.1 million for 2015 and $30.4 million for 2014. The dollar increase is primarily due to increases in salaries, benefits and equity based compensation. Corporate office costs as a percentage of net revenues were 9.4% for 2015 and 10.0% in 2014.
Interest Expense
Interest expense remained relatively the same in 2015 and 2014. Interest expense was $1.0 million for 2015 and $1.1 million for 2014. At December 31, 2015, $44.0 million was outstanding under our Credit Agreement. See “—Liquidity and Capital Resources” below for a discussion of the terms of our Amended Credit Agreement (as defined below under “—Liquidity and Capital Resources”).
Provision for Income Taxes
The provision for income taxes was $14.7 million for 2015 and $14.3 million for 2014. We accrued state and federal income taxes at an effective tax rate (provision for taxes divided by the difference between income from operations and net income attributable to non-controlling interest) of 39.7% for 2015 and 40.6% for 2014. The 2015 provision for taxes includes an additional $147,000 due to reconciliation of the 2014 federal and state returns to our book provision and an additional $223,000 in 2014 for the 2013 reconciliation.
Net Income Attributable to Non-controlling Interests
Net income attributable to non-controlling interests was $9.4 million in 2015 and $9.6 million in 2014. As a percentage of operating income before corporate office costs, net income attributable to non-controlling interests was 12.0% in 2015 compared to 12.6% in 2014. The reduction is attributable to the Company’s increased ownership interest in certain physical therapy partnerships.
FISCAL YEAR 2014 COMPARED TO FISCAL 2013
| • | Net revenues rose 15.5 % to $305.1 million for 2014 from $264.1 million for 2013 primarily due to increases in net patient revenues which are discussed in detail below. |
| • | Net income from continuing operations prior to the revaluation of non-controlling interests, net of tax for 2014 increased 19.2% to $20.8 million, or $1.71 per diluted share, from $17.5 million, or $1.45 per diluted share. |
28
Net Patient Revenues
| • | Net patient revenues increased to $299.0 million for 2014 from $258.3 million for 2013, an increase of $40.7 million, or 15.8%. The increase in net patient revenues of $40.7 million consisted of an increase of $11.4 million from 2014 New Clinics and $29.3 million from 2014 Mature Clinics of which $17.9 million related to the two clinic groups acquired in December 2013. During 2014, we acquired two multi-clinic groups for a total of 16 clinics. The net patient revenues from these multi-clinic groups are included in our results of operations since the respective date of their acquisition. See above table under “—Executive Summary” detailing our multi-clinic acquisitions. |
| • | Total patient visits increased to 2,819,000 for 2014 from 2,441,000 for 2013. The growth in patient visits was attributable to 108,000 visits in 2014 New Clinics primarily due to the acquisitions in 2014 and an increase of 270,000 visits for 2014 Mature Clinics primarily due to the two clinic groups acquired in December 2013. |
| • | The average net patient revenue per visit increased to $106.08 in 2014 from $105.83 in 2013. |
Net patient revenues are based on established billing rates less allowances and discounts for patients covered by contractual programs and workers’ compensation. Net patient revenues reflect contractual and other adjustments, which we evaluate monthly, relating to patient discounts from certain payors. Payments received under these programs are based on predetermined rates and are generally less than the established billing rates of the clinics.
Other Revenues
Other revenues, consisting primarily of management fees, increased by $290,000, from $5.8 million in 2013 to $6.1 million in 2014. On December 31, 2014, we managed 16 third-party physical therapy facilities versus 18 on December 31, 2013, however our average number of management contracts was higher in 2014 versus 2013.
Clinic Operating Costs
Clinic operating costs were $228.9 million, or 75.0% of net revenues, for 2014 and $199.4 million, or 75.5% of net revenues, for 2013. The increase was attributable to $10.2 million in operating costs for 2014 New Clinics, an increase in operating costs of $18.5 million for 2013 New Clinics due to a full year of activity and an increase of $0.8 million 2013 Mature Clinics. Each component of clinic operating costs is discussed below:
Clinic Operating Costs—Salaries and Related Costs
Salaries and related costs increased to $163.4 million for 2014 from $141.8 million for 2013, an increase of $21.6 million, or 15.2%. Approximately $7.3 million of the increase was attributable to 2014 New Clinics. The remaining $14.3 million of the increase was due to $12.5 million in higher costs at various 2013 New Clinics due to a full year of activity (see table detailing acquisition dates above under “—Executive Summary”) and higher costs of $1.8 million in costs at 2013 Mature Clinics. Salaries and related costs as a percentage of net revenues was 53.6% for 2014 and 53.7% for 2013.
Clinic Operating Costs—Rent, Clinic Supplies, Contract Labor and Other
Rent, clinic supplies, contract labor and other costs increased to $61.2 million for 2014 from $52.9 million for 2013, an increase of $8.3 million, or 15.7%. The 2014 New Clinics accounted for approximately $2.8 million of the increase and 2013 New Clinics accounted for approximately $6.0 million of the increase due to a full year of activity. Rent, clinic supplies, contract labor and other costs for 2012 Mature Clinics decreased $0.5 million in 2014 as compared to 2013. For 2013, included in the rent, clinic supplies and other costs for 2012 Mature Clinics is a pre-tax charge of $850,000 related to an estimated refund due to a payor for overpayments to a partnership clinic group over several years. Rent, clinic supplies, contract labor and other costs as a percent of net revenues was 20.1% for 2014 and 20.0% for 2013.
Clinic Operating Costs—Provision for Doubtful Accounts
The provision for doubtful accounts for net patient receivables of $4.1 million as a percentage of net patient revenues was 1.3% for 2014. The provision for doubtful accounts for net patient receivables of $4.4 million as a percentage of net patient revenues was 1.7% for 2013. During 2013, we recorded a reserve for a receivable from a management contract of $0.1 million.
29
Our provision for doubtful accounts as a percentage of total patient accounts receivable was 4.8% at December 31, 2014 and 4.4% at December 31, 2013. The provision for doubtful accounts at the end of each period is based on a detailed, clinic-by-clinic review of overdue accounts and is regularly reviewed in the aggregate in light of historical experience.
The average accounts receivable days outstanding were 39 days for both December 31, 2014 and December 31, 2013. Net patient receivables in the amount of $3.9 million and $4.4 million were written-off in 2014 and 2013, respectively.
Closure Costs
For 2014, closure costs amounted to $169,000 which included a write-off of goodwill of $135,000. In 2013, closure costs amounted to $246,000.
Gross Margin
In 2014, the gross margin increased by $11.5 million, or 17.7%, as compared to 2013. The gross margin percentage for 2014 was 25.0% as compared to 24.5% for 2013.
Corporate Office Costs
Corporate office costs, consisting primarily of salaries, benefits and equity based compensation of corporate office personnel and directors, rent, insurance costs, depreciation and amortization, travel, legal, compliance, professional, marketing and recruiting fees, were $30.4 million for 2014 and $25.9 million for 2013. Corporate office costs as a percentage of net revenues were 10.0% for 2014 and 9.8% in 2013. The increase is primarily due to increases in salaries, benefits and equity based compensation
Interest Expense
Interest expense increased to $1.1 million for 2014 from $538,000 for 2013 primarily due to higher average borrowings throughout the year as result of acquisitions. At December 31, 2014, $34.5 million was outstanding under our Credit Agreement. See “—Liquidity and Capital Resources” below for a discussion of the terms of our Credit Agreement.
Provision for Income Taxes
The provision for income taxes was $14.3 million for 2014 and $12.2 million for 2013. We accrued state and federal income taxes at an effective tax rate (provision for taxes divided by the difference between income from operations and net income attributable to non-controlling interest) of 40.6% for 2014 and 41.1% for 2013. The provision for income taxes for 2014 includes an additional provision of $223,000 related to the true-up of our 2013 tax provision, and for 2013, $393,000, based on a detailed reconciliation of our federal and state taxes payable and receivable accounts along with our federal and state deferred tax asset and liability accounts.
Net Income Attributable to Non-controlling Interests
Net income attributable to non-controlling interests was $9.6 million in 2014 and $8.5 million in 2013. As a percentage of operating income before corporate office costs, net income attributable to non-controlling interests was 12.6% in 2014 compared to 13.2% in 2013. The reduction is attributable to the Company’s increased ownership interest in certain physical therapy partnerships.
LIQUIDITY AND CAPITAL RESOURCES
We believe that our business is generating sufficient cash flow from operating activities to allow us to meet our short-term and long-term cash requirements, other than those with respect to future significant acquisitions. At December 31, 2015, we had $15.8 million in cash and cash equivalents compared to $14.3 million at December 31, 2014. Although the start-up costs associated with opening new clinics and our planned capital expenditures are significant, we believe that our cash and cash equivalents and availability under our Amended Credit Agreement are sufficient to fund the working capital needs of our operating subsidiaries, future clinic development and acquisitions and investments through at least December 2016. Significant acquisitions would likely require financing under our Amended Credit Agreement.
30
Effective December 5, 2013, we entered into an Amended and Restated Credit Agreement with a commitment for a $125.0 million revolving credit facility with a maturity date of November 30, 2018. This agreement was amended in August 2015 and January 2016 (hereafter referred to as “Amended Credit Agreement”). The Amended Credit Agreement is unsecured and has loan covenants, including requirements that the Company comply with a consolidated fixed charge coverage ratio and consolidated leverage ratio. Proceeds from the Amended Credit Agreement may be used for working capital, acquisitions, purchases of the Company’s common stock, dividend payments to the Company’s common stockholders, capital expenditures and other corporate purposes. The pricing grid which is based on the Company’s consolidated leverage ratio with the applicable spread over LIBOR ranging from 1.5% to 2.5% or the applicable spread over the Base Rate ranging from 0.1% to 1%. Fees under the Amended Credit Agreement include an unused commitment fee ranging from 0.1% to 0.25% depending on the Company’s consolidated leverage ratio and the amount of funds outstanding under the Amended Credit Agreement. On December 31, 2015, $44.0 million was outstanding under our Amended Credit Agreement resulting in $81.0 million of availability, and we were in compliance with all of the covenants thereunder.
The increase in cash and cash equivalents of $1.5 million from December 31, 2014 to December 31, 2015 was due primarily to $41.2 million provided by operations and $9.5 million net proceeds from our Amended Credit Agreement. The major uses of cash for investing and financing activities included: purchase of businesses ($19.0 million), distributions to non-controlling interests ($9.6 million), payments of cash dividends to our shareholders ($7.4 million), acquisitions of non-controlling interests ($7.1 million), purchases of fixed assets ($6.3 million), and payments on notes payable ($0.9 million).
On December 31, 2015, we acquired a 59% interest in a four-clinic practice for $4.6 million in cash and $400,000 in seller notes that are payable in two principal installments of an aggregate of $200,000 each, plus accrued interest, in December 2016 and 2017. On June 30, 2015, we acquired a 70% interest in a four-clinic physical therapy practice. The purchase price was $3.6 million in cash and $0.7 million in seller notes that are payable plus accrued interest, in June 2018. On April 30, 2015, we acquired a 70% interest in a three-clinic physical therapy practice. The purchase price was $4.7 million in cash and $150,000 in a seller note that is payable in two principal installments of $75,000 each, plus accrued interest, in April 2016 and 2017. On January 31, 2015, we acquired a 60% interest in a nine-clinic physical therapy practice. The purchase price for the 60% interest was $6.7 million in cash and $0.5 million in a seller note that is payable in two principal installments of $250,000 each, plus accrued interest, in January 2016 and 2017. In addition to the multi-clinic acquisitions, on August 31, 2015, we acquired a 60% interest in a single physical therapy clinic for $150,000 in cash and $50,000 in a seller note that is payable plus accrued interest in August 2016.
The purchase price for the 70% interest in the April 2014 Acquisition was $10.6 million in cash and a $400,000 seller note, that is payable in two principal installments totaling $200,000 each, plus accrued interest, in April 2015 and 2016. The purchase price for the August 2014 Acquisition was $1.0 million in cash. In addition, during 2014, we acquired three individual clinic practices for an aggregate of $595,000. The purchase price for the 72% interest in the February 2013 Acquisition was $4.3 million in cash and $400,000 in a seller note, that is payable in two principal installments totaling $200,000 each, plus accrued interest, in February 2014 and 2015, which has been paid in full. The purchase price for the 50% interest in the April 2013 Acquisition was $2.4 million in cash and $200,000 in a seller note, that is payable in two principal installments totaling $100,000 each, plus accrued interest, in April of 2014 and 2015, which has been paid in full. The purchase price for the 80% interest in the May 2013 Acquisition was $3.6 million in cash and $200,000 in a seller note, that is payable in two principal installments totaling $100,000 each, plus accrued interest, in May of 2014 and 2015, which has been paid in full. The purchase price for the 60% interest in the December 9, 2013 Acquisition was $1.7 million in cash. The purchase price for the 90% interest in the December 13, 2013 Acquisition was $35.5 million in cash and $500,000 in a seller note, that is payable in two principal installments totaling $250,000 each, plus accrued interest, in December 2014 and 2015, which has been paid in full. The aggregate purchase price for the three individual clinics acquired in 2013 was $238,000. In four separate transactions during 2014, we purchased interests in two partnerships which were previously classified as redeemable, non-controlling interest. The interests in the partnerships purchased ranged from 10.0% to 35.0%, The aggregate of the purchase prices paid was $4.9 million, which included $3.0 million of net book value. The remaining purchase price of $1.9 million, less future tax benefits of $0.8 million, was recognized as an adjustment to additional paid-in capital. Also, in four separate transactions during 2014, we purchased partnership interests in four partnerships. The interests in the partnerships purchased and sold ranged from less than 1% to 35%. The aggregate of the purchase prices paid
31
was $0.6 million. The purchase prices paid included a net of $0.1 million of undistributed earnings. The remaining $0.5 million, less future tax benefits of $0.2 million, was recognized as an adjustment to additional paid-in capital. Through 15 separate transactions during 2013, the Company purchased partnership interests in 10 partnerships and sold interests in five partnerships. The interests in the partnerships purchased and sold ranged from less than 1% to 35%. The aggregate of the purchase prices paid was $1.9 million and the proceeds for the sales were $0.8 million, which included cash of $0.2 million and notes receivable of $0.6 million.
Historically, we have generated sufficient cash from operations to fund our development activities and to cover operational needs. We plan to continue developing new clinics and making additional acquisitions in selected markets. We have from time to time purchased the non-controlling interests of limited partners in our Clinic Partnerships. We may purchase additional non-controlling interests in the future. Generally, any acquisition or purchase of non-controlling interests is expected to be accomplished using a combination of cash and financing. Any large acquisition would likely require financing.
We make reasonable and appropriate efforts to collect accounts receivable, including applicable deductible and co-payment amounts. Claims are submitted to payors daily, weekly or monthly in accordance with our policy or payor’s requirements. When possible, we submit our claims electronically. The collection process is time consuming and typically involves the submission of claims to multiple payors whose payment of claims may be dependent upon the payment of another payor. Claims under litigation and vehicular incidents can take a year or longer to collect. Medicare and other payor claims relating to new clinics awaiting CMS approval initially may not be submitted for six months or more. When all reasonable internal collection efforts have been exhausted, accounts are written off prior to sending them to outside collection firms. With managed care, commercial health plans and self-pay payor type receivables, the write-off generally occurs after the account receivable has been outstanding for 120 days or longer.
We have future obligations for debt repayments, employment agreements and future minimum rentals under operating leases. The obligations as of December 31, 2015 are summarized as follows (in thousands):
Contractual Obligation |
Total |
2016 |
2017 |
2018 |
2019 |
2020 |
Thereafter |
||||||||||||||
Credit Agreement |
$ | 44,000 | $ | — | $ | — | $ | 44,000 | $ | — | $ | — | $ | — | |||||||
Notes Payable |
$ | 5,110 | $ | 775 | $ | 559 | $ | 1,930 | $ | 1,846 | $ | — | $ | — | |||||||
Interest Payable |
$ | 399 | 152 | 131 | 111 | 5 | — | — | |||||||||||||
Employee Agreements |
$ | 41,874 | 27,125 | 12,205 | 1,546 | 998 | — | — | |||||||||||||
Operating Leases |
$ | 84,229 | 26,799 | 20,896 | 14,872 | 9,216 | 9,329 | 3,117 | |||||||||||||
$ | 175,612 | $ | 54,851 | $ | 33,791 | $ | 62,459 | $ | 12,065 | $ | 9,329 | $ | 3,117 | ||||||||
We generally enter into various notes payable as a means of financing our acquisitions. Our present outstanding notes payable relate only to certain of the acquisitions of businesses and non-controlling interests that occurred in 2015 and 2014. For those acquisitions, we entered into several notes payable aggregating $5.3 million. Generally, the notes are payable in equal annual installments of principal over two years plus any accrued and unpaid interest. See above table for a detail of future principal payments. Interest accrues at various interest rates ranging from 3.25% to 4.0% per annum, subject to adjustment. In addition, we assumed leases with remaining terms of 1 month to 6 years for the operating facilities. At December 31, 2015, the balance on these outstanding notes was $5.1 million.
In conjunction with the above mentioned acquisitions, in the event that a limited minority partner’s employment ceases at any time after three or four years from the acquisition date, as applicable, we have agreed to repurchase that individual’s non-controlling interest at a predetermined multiple of earnings before interest, taxes, depreciation and amortization.
As of December 31, 2015, we have accrued $1.5 million related to credit balances and overpayments due to patients and payors. This amount is expected to be paid in 2016.
As previously disclosed in public filings, on December 22, 2015, a limited partnership, in which we own a majority interest, finalized and entered into a settlement with the U. S. Department of Justice related to certain Medicare billings that occurred between 2007 and 2009 at a single outpatient physical therapy clinic. The limited partnership paid $718,000 to resolve the matter. The settlement expense was estimated and accrued for in 2012. We, along with the limited partnership, cooperated fully in the government review and we conducted our own
32
internal audit of all of the Medicare claims submitted by that clinic during the relevant period in order to assist the government in determining the appropriate dollar amount that should be refunded. As is customary at the conclusion of such government investigations, the limited partnership and the Company have entered into a Corporate Integrity Agreement (“CIA”) that will be incorporated into our existing comprehensive compliance program. See Item 1. Business – Compliance Program.
From September 2001 through December 31, 2008, the Board authorized us to purchase, in the open market or in privately negotiated transactions, up to 2,250,000 shares of our common stock. In March 2009, the Board authorized the repurchase of up to 10% or approximately 1,200,000 shares of our common stock (“March 2009 Authorization”). In connection with the March 2009 Authorization, we amended our prior credit agreement to permit share repurchases of up to $15,000,000. We are required to retire shares purchased under the March 2009 Authorization. Under the March 2009 Authorization, we have purchased a total of 859,499 shares. There is no expiration date for the share repurchase program. The Amended Credit Agreement permits the Company to purchase, commencing on October 24, 2012 and at all times thereafter, up to $15,000,000 of its common stock subject to compliance with covenants. There are currently an additional estimated 279,433 shares (based on a closing price of $53.68 on December 31, 2015) that may be purchased shares that may be purchased from time to time in the open market or private transactions depending on price, availability and our cash position. We did not purchase any shares of our common stock during 2015 or 2014.
Off Balance Sheet Arrangements
With the exception of operating leases for our executive offices and clinic facilities discussed in Note 16 to our consolidated financial statements included in Item 8, we have no off-balance sheet debt or other off-balance sheet financing arrangements.
FACTORS AFFECTING FUTURE RESULTS
The risks related to our business and operations include:
| • | changes as the result of government enacted national healthcare reform; |
| • | changes in Medicare rules and guidelines and reimbursement or failure of our clinics to maintain their Medicare certification or enrollment status; |
| • | revenue we receive from Medicare and Medicaid being subject to potential retroactive reduction; |
| • | business and regulatory conditions including federal and state regulations; |
| • | governmental and other third party payor inspections, reviews, investigations and audits; |
| • | compliance with federal and state laws and regulations relating to the privacy of individually identifiable patient information, and associated fines and penalties for failure to comply; |
| • | possible legal actions, which could subject us to increased operating costs and uninsured liabilities; |
| • | changes in reimbursement rates or payment methods from third party payors including government agencies and deductibles and co-pays owed by patients; |
| • | revenue and earnings expectations; |
| • | general economic conditions; |
| • | availability and cost of qualified physical therapists; |
| • | personnel productivity and retaining key personnel; |
| • | competitive, economic or reimbursement conditions in our markets which may require us to reorganize or close certain clinics and thereby incur losses and/or closure costs including the possible write-down or write-off of goodwill and other intangible assets; |
| • | acquisitions, purchase of non-controlling interests (minority interests) and the successful integration of the operations of the acquired businesses; |
| • | maintaining adequate internal controls; |
| • | maintaining necessary insurance coverage; |
33
| • | availability, terms, and use of capital; and |
| • | weather and other seasonal factors. |
See also Risk Factors in Item 1A of this Annual Report on Form 10-K.
ITEM 7A. QUANTITATIVE AND QUALITATIVE DISCLOSURES ABOUT MARKET RISK.
We do not maintain any derivative instruments such as interest rate swap arrangements, hedging contracts, futures contracts or the like. Our only indebtedness as of December 31, 2015 was the outstanding balance of seller notes of $5.1 million and an outstanding balance on our Amended Credit Agreement of $44.0 million. The outstanding balance under our Amended Credit Agreement is subject to fluctuating interest rates. A 1% change in the interest rate would yield an additional $440,000 of interest expense. See Note 10 to our consolidated financial statements included in Item 8.
34
ITEM 8. FINANCIAL STATEMENTS AND SUPPLEMENTARY DATA.
U.S. PHYSICAL THERAPY, INC. AND SUBSIDIARIES
INDEX TO CONSOLIDATED FINANCIAL STATEMENTS AND RELATED INFORMATION
35
REPORT OF INDEPENDENT REGISTERED PUBLIC ACCOUNTING FIRM
Board of Directors and Shareholders
U.S. Physical Therapy, Inc.
We have audited the accompanying consolidated balance sheets of U.S. Physical Therapy, Inc. (a Nevada corporation) and subsidiaries (the “Company”) as of December 31, 2015 and 2014, and the related consolidated statements of net income, equity, and cash flows for each of the three years in the period ended December 31, 2015. Our audits of the basic consolidated financial statements included the financial statement schedule listed in the index appearing under Item 15(a)(2). These financial statements and financial statement schedule are the responsibility of the Company’s management. These financial statements are the responsibility of the Company’s management. Our responsibility is to express an opinion on these financial statements based on our audits.
We conducted our audits in accordance with the standards of the Public Company Accounting Oversight Board (United States). Those standards require that we plan and perform the audit to obtain reasonable assurance about whether the financial statements are free of material misstatement. An audit includes examining, on a test basis, evidence supporting the amounts and disclosures in the financial statements. An audit also includes assessing the accounting principles used and significant estimates made by management, as well as evaluating the overall financial statement presentation. We believe that our audits provide a reasonable basis for our opinion.
In our opinion, the consolidated financial statements referred to above present fairly, in all material respects, the financial position of U.S. Physical Therapy, Inc. and subsidiaries as of December 31, 2015 and 2014, and the results of their operations and their cash flows for each of the three years in the period ended December 31, 2015 in conformity with accounting principles generally accepted in the United States of America. Also in our opinion, the related financial statement schedule, when considered in relation to the basic consolidated financial statements taken as a whole, present fairly, in all material respects, the information set forth therein.
We also have audited, in accordance with the standards of the Public Company Accounting Oversight Board (United States), the Company’s internal control over financial reporting as of December 31, 2015, based on criteria established in the 2013 Internal Control—Integrated Framework issued by the Committee of Sponsoring Organizations of the Treadway Commission (COSO), and our report dated March 4, 2016 expressed unqualified opinion.
/s/ GRANT THORNTON LLP
Houston, Texas
March 4, 2016
36
REPORT OF INDEPENDENT REGISTERED PUBLIC ACCOUNTING FIRM
Board of Directors and Shareholders
U.S. Physical Therapy, Inc.
We have audited the internal control over financial reporting of U.S. Physical Therapy, Inc. (a Nevada corporation) and subsidiaries (the “Company”) as of December 31, 2015, based on criteria established in the 2013 Internal Control—Integrated Framework issued by the Committee of Sponsoring Organizations of the Treadway Commission (COSO). The Company’s management is responsible for maintaining effective internal control over financial reporting and for its assessment of the effectiveness of internal control over financial reporting, included in the accompanying Management’s Report on Internal Control over Financial Reporting. Our responsibility is to express an opinion on the Company’s internal control over financial reporting based on our audit.
We conducted our audit in accordance with the standards of the Public Company Accounting Oversight Board (United States). Those standards require that we plan and perform the audit to obtain reasonable assurance about whether effective internal control over financial reporting was maintained in all material respects. Our audit included obtaining an understanding of internal control over financial reporting, assessing the risk that a material weakness exists, testing and evaluating the design and operating effectiveness of internal control based on the assessed risk, and performing such other procedures as we considered necessary in the circumstances. We believe that our audit provides a reasonable basis for our opinion.
A company’s internal control over financial reporting is a process designed to provide reasonable assurance regarding the reliability of financial reporting and the preparation of financial statements for external purposes in accordance with generally accepted accounting principles. A company’s internal control over financial reporting includes those policies and procedures that (1) pertain to the maintenance of records that, in reasonable detail, accurately and fairly reflect the transactions and dispositions of the assets of the company; (2) provide reasonable assurance that transactions are recorded as necessary to permit preparation of financial statements in accordance with generally accepted accounting principles, and that receipts and expenditures of the company are being made only in accordance with authorizations of management and directors of the company; and (3) provide reasonable assurance regarding prevention or timely detection of unauthorized acquisition, use, or disposition of the company’s assets that could have a material effect on the financial statements.
Because of its inherent limitations, internal control over financial reporting may not prevent or detect misstatements. Also, projections of any evaluation of effectiveness to future periods are subject to the risk that controls may become inadequate because of changes in conditions, or that the degree of compliance with the policies or procedures may deteriorate.
In our opinion, the Company maintained, in all material respects, effective internal control over financial reporting as of December 31, 2015, based on criteria established in the 2013 Internal Control—Integrated Framework issued by COSO.
We also have audited, in accordance with the standards of the Public Company Accounting Oversight Board (United States), the consolidated financial statements of the Company as of and for the year ended December 31, 2015, and our report dated March 4, 2016 expressed an unqualified opinion on those financial statements.
/s/ GRANT THORNTON LLP
Houston, Texas
March 4, 2016
37
U.S. PHYSICAL THERAPY, INC. AND SUBSIDIARIES
CONSOLIDATED BALANCE SHEETS
(In thousands, except per share data)
December 31, 2015 |
December 31, 2014 |
|||||
ASSETS |
||||||
Current assets: |
||||||
Cash and cash equivalents |
$ | 15,778 | $ | 14,271 | ||
Patient accounts receivable, less allowance for doubtful accounts of $1,444 and $1,669, respectively |
36,231 | 32,891 | ||||
Accounts receivable - other, less allowance for doubtful accounts of $198 and $198, respectively |
2,388 | 1,503 | ||||
Other current assets |
5,785 | 6,186 | ||||
Total current assets |
60,182 | 54,851 | ||||
Fixed assets: |
||||||
Furniture and equipment |
44,749 | 42,003 | ||||
Leasehold improvements |
25,160 | 22,806 | ||||
Fixed assets, gross |
69,909 | 64,809 | ||||
Less accumulated depreciation and amortization |
53,255 | 49,045 | ||||
Fixed assets, net |
16,654 | 15,764 | ||||
Goodwill |
171,547 | 147,914 | ||||
Other identifiable intangible assets, net |
30,296 | 24,907 | ||||
Other assets |
1,234 | 1,115 | ||||
Total assets |
$ | 279,913 | $ | 244,551 | ||
LIABILITIES AND SHAREHOLDERS’ EQUITY |
||||||
Current liabilities: |
||||||
Accounts payable - trade |
$ | 1,636 | $ | 1,782 | ||
Accrued expenses |
16,596 | 22,839 | ||||
Current portion of notes payable |
775 | 883 | ||||
Total current liabilities |
19,007 | 25,504 | ||||
Notes payable |
4,335 | 234 | ||||
Revolving line of credit |
44,000 | 34,500 | ||||
Deferred rent |
1,395 | 991 | ||||
Deferred taxes and other long-term liabilities |
9,223 | 8,732 | ||||
Total liabilities |
77,960 | 69,961 | ||||
Commitments and contingencies |
||||||
Redeemable non-controlling interests |
8,843 | 7,376 | ||||
Equity: |
||||||
U. S. Physical Therapy, Inc. shareholders’ equity: |
||||||
Preferred stock, $.01 par value, 500,000 shares authorized, no shares issued and outstanding |
— | — | ||||
Common stock, $.01 par value, 20,000,000 shares authorized, 14,635,874 and 14,487,346 shares issued, respectively |
146 | 145 | ||||
Additional paid-in capital |
45,251 | 43,577 | ||||
Retained earnings |
149,016 | 134,186 | ||||
Treasury stock at cost, 2,214,737 shares |
(31,628 | ) |
(31,628 | ) |
||
Total U. S. Physical Therapy, Inc. shareholders’ equity |
162,785 | 146,280 | ||||
Non-controlling interests |
30,325 | 20,934 | ||||
Total equity |
193,110 | 167,214 | ||||
Total liabilities and equity |
$ | 279,913 | $ | 244,551 | ||
See notes to consolidated financial statements.
38
U.S. PHYSICAL THERAPY, INC. AND SUBSIDIARIES
CONSOLIDATED STATEMENTS OF NET INCOME
(In thousands, except per share data)
Year Ended December 31, 2015 |
Year Ended December 31, 2014 |
Year Ended December 31, 2013 |
|||||||
Net patient revenues |
$ | 324,293 | $ | 299,009 | $ | 258,283 | |||
Other revenues |
7,009 | 6,065 | 5,775 | ||||||
Net revenues |
331,302 | 305,074 | 264,058 | ||||||
Clinic operating costs: |
|||||||||
Salaries and related costs |
180,514 | 163,417 | 141,840 | ||||||
Rent, clinic supplies, contract labor and other |
68,046 | 61,209 | 52,887 | ||||||
Provision for doubtful accounts |
4,170 | 4,112 | 4,384 | ||||||
Closure costs |
211 | 169 | 246 | ||||||
Total clinic operating costs |
252,941 | 228,907 | 199,357 | ||||||
Gross margin |
78,361 | 76,167 | 64,701 | ||||||
Corporate office costs |
31,067 | 30,399 | 25,931 | ||||||
Operating income from continuing operations |
47,294 | 45,768 | 38,770 | ||||||
Interest and other income, net |
81 | 18 | 7 | ||||||
Interest expense |
(1,031 | ) |
(1,088 | ) |
(538 | ) |
|||
Income before taxes from continuing operations |
46,344 | 44,698 | 38,239 | ||||||
Provision for income taxes |
14,653 | 14,274 | 12,236 | ||||||
Net income from continuing operations including non-controlling interests |
31,691 | 30,424 | 26,003 | ||||||
Discontinued operations, net of tax benefit of $-0-, $-0- and $3,180. |
— | — | (5,007 | ) |
|||||
Net income including non-controlling interests |
31,691 | 30,424 | 20,996 | ||||||
Less: net income attributable to non-controlling interests |
(9,412 | ) |
(9,571 | ) |
(8,273 | ) |
|||
Net income attributable to common shareholders |
$ | 22,279 | $ | 20,853 | $ | 12,723 | |||
Basic earnings per share attributable to common shareholders: |
|||||||||
Prior to revaluation of redeemable non-controlling interests, net of tax |
$ | 1.80 | $ | 1.71 | $ | 1.45 | |||
Charges to additional-paid-in-capital - revaluation of non-controlling interests, net of tax |
(0.03 | ) |
(0.09 | ) |
— | ||||
From continuing operations, net of tax |
1.77 | 1.62 | 1.45 | ||||||
From discontinued operations, net of tax |
— | — | (0.40 | ) |
|||||
Basic |
$ | 1.77 | $ | 1.62 | $ | 1.05 | |||
Diluted earnings per share attributable to common shareholders: |
|||||||||
Prior to revaluation of redeemable non-controlling interests, net of tax |
$ | 1.80 | $ | 1.71 | $ | 1.45 | |||
Charges to additional-paid-in-capital - revaluation of non-controlling interests, net of tax |
(0.03 | ) |
(0.09 | ) |
— | ||||
From continuing operations, net of tax |
1.77 | 1.62 | 1.45 | ||||||
From discontinued operations, net of tax |
— | — | (0.40 | ) |
|||||
Diluted |
$ | 1.77 | $ | 1.62 | $ | 1.05 | |||
Shares used in computation: |
|||||||||
Basic |
12,392 | 12,217 | 12,063 | ||||||
Diluted |
12,392 | 12,221 | 12,082 | ||||||
Dividends declared per common share |
$ | 0.60 | $ | 0.48 | $ | 0.40 | |||
Earnings attributable to common shareholders: |
|||||||||
From continuing operations |
$ | 22,279 | $ | 20,853 | $ | 17,492 | |||
From discontinued operations |
— | — | (4,769 | ) |
|||||
Net income attributable to common shareholders |
$ | 22,279 | $ | 20,853 | $ | 12,723 | |||
See notes to consolidated financial statements.
39
U.S. PHYSICAL THERAPY, INC. AND SUBSIDIARIES
CONSOLIDATED STATEMENTS OF EQUITY
(In thousands)
U.S. Physical Therapy, Inc. |
|||||||||||||||||||||||||||
Common Stock |
Additional Paid-In Capital |
Retained Earnings |
Treasury Stock |
Total Shareholders’ Equity |
Non- controlling Interests |
Total |
|||||||||||||||||||||
Shares |
Amount |
Shares |
Amount |
||||||||||||||||||||||||
(In thousands) |
|||||||||||||||||||||||||||
Balance December 31, 2012 |
14,130 | $ | 141 | $ | 37,489 | $ | 111,321 | (2,215 | ) |
$ | (31,628 | ) |
$ | 117,323 | $ | 17,336 | $ | 134,659 | |||||||||
Proceeds from exercise of stock options |
17 | 2 | 45 | — | — | — | 47 | — | 47 | ||||||||||||||||||
Net tax benefit from equity-based awards |
— | — | 695 | — | — | — | 695 | — | 695 | ||||||||||||||||||
Issuance of restricted stock |
175 | — | — | — | — | — | — | — | — | ||||||||||||||||||
Cancellation of restricted stock |
(6 | ) |
— | — | — | — | — | — | — | — | |||||||||||||||||
Compensation expense - restricted stock |
— | — | 2,743 | — | — | — | 2,743 | — | 2,743 | ||||||||||||||||||
Transfer of compensation liability for certain stock issued pursuant to long-term incentive plans |
— | — | 248 | — | — | — | 248 | — | 248 | ||||||||||||||||||
Purchase of businesses |
— | — | — | — | — | — | — | 10,541 | 10,541 | ||||||||||||||||||
Acquisitions and sales of non-controlling interests, net |
— | — | (651 | ) |
— | — | — | (651 | ) |
(155 | ) |
(806 | ) |
||||||||||||||
Reclass to redeemable non-controlling interests |
— | — | — | — | — | — | — | (4,104 | ) |
(4,104 | ) |
||||||||||||||||
Distributions to non-controlling interest partners |
— | — | — | — | — | — | — | (9,164 | ) |
(9,164 | ) |
||||||||||||||||
Cash dividends to shareholders |
— | — | — | (4,838 | ) |
— | — | (4,838 | ) |
— | (4,838 | ) |
|||||||||||||||
Net income |
— | — | — | 12,723 | — | — | 12,723 | 8,273 | 20,996 | ||||||||||||||||||
Balance December 31, 2013 |
14,316 | $ | 143 | $ | 40,569 | $ | 119,206 | (2,215 | ) |
$ | (31,628 | ) |
$ | 128,290 | $ | 22,727 | $ | 151,017 | |||||||||
Proceeds from exercise of stock options |
21 | 1 | 43 | — | — | — | 44 | — | 44 | ||||||||||||||||||
Net tax benefit from equity-based awards |
— | — | 948 | — | — | — | 948 | — | 948 | ||||||||||||||||||
Issuance of restricted stock |
150 | 1 | — | — | — | — | 1 | — | 1 | ||||||||||||||||||
Cancellation of restricted stock |
— | — | — | — | — | — | — | — | |||||||||||||||||||
Compensation expense - restricted stock |
— | — | 3,363 | — | — | — | 3,363 | — | 3,363 | ||||||||||||||||||
Purchase of business |
— | — | — | — | — | — | — | 4,725 | 4,725 | ||||||||||||||||||
Revaluation of redeemable non controlling interets |
— | (1,086 | ) |
— | — | — | (1,086 | ) |
— | (1,086 | ) |
||||||||||||||||
Reclass to redeemable non-controlling interests |
— | — | — | — | — | — | — | (6,375 | ) |
(6,375 | ) |
||||||||||||||||
Acquisitions and sales of non-controlling interests, net |
— | — | (260 | ) |
— | — | — | (260 | ) |
(63 | ) |
(323 | ) |
||||||||||||||
Cash dividends to shareholders |
— | — | (5,873 | ) |
— | (5,873 | ) |
— | (5,873 | ) |
|||||||||||||||||
Contribution of non-controlling interest partners |
— | — | — | — | — | — | — | 177 | 177 | ||||||||||||||||||
Distributions to non-controlling interest partners |
— | — | — | — | — | — | — | (9,432 | ) |
(9,432 | ) |
||||||||||||||||
Net income |
— | — | — | 20,853 | — | — | 20,853 | 9,175 | 30,028 | ||||||||||||||||||
Balance December 31, 2014 |
14,487 | $ | 145 | $ | 43,577 | $ | 134,186 | (2,215 | ) |
$ | (31,628 | ) |
$ | 146,280 | $ | 20,934 | $ | 167,214 | |||||||||
Proceeds from exercise of stock options |
1 | 1 | 4 | — | — | — | 5 | — | 5 | ||||||||||||||||||
Net tax benefit from equity-based awards |
— | — | 947 | — | — | — | 947 | — | 947 | ||||||||||||||||||
Issuance of restricted stock |
148 | — | — | — | — | — | — | — | — | ||||||||||||||||||
Compensation expense - restricted stock |
— | — | 4,491 | — | — | — | 4,491 | — | 4,491 | ||||||||||||||||||
Transfer of compensation liability for certain stock issued pursuant to long-term incentive plans |
— | — | 446 | — | — | — | 446 | — | 446 | ||||||||||||||||||
Purchase of businesses |
— | — | — | — | — | — | — | 12,292 | 12,292 | ||||||||||||||||||
Revaluation of redeemable non-controlling interets |
— | (319 | ) |
— | — | — | (319 | ) |
— | (319 | ) |
||||||||||||||||
Reclass to redeemable non-controlling interests |
— | — | — | — | — | — | — | (2,681 | ) |
(2,681 | ) |
||||||||||||||||
Acquisitions and sales of non-controlling interests, net |
— | — | (3,895 | ) |
— | — | — | (3,895 | ) |
(260 | ) |
(4,155 | ) |
||||||||||||||
Cash dividends to shareholders |
— | — | (7,449 | ) |
— | (7,449 | ) |
— | (7,449 | ) |
|||||||||||||||||
Contribution of non-controlling interest partners |
— | — | — | — | — | — | — | 17 | 17 | ||||||||||||||||||
Distributions to non-controlling interest partners |
— | — | — | — | — | — | — | (8,723 | ) |
(8,723 | ) |
||||||||||||||||
Net income |
— | — | — | 22,279 | — | — | 22,279 | 8,746 | 31,025 | ||||||||||||||||||
Balance December 31, 2015 |
14,636 | $ | 146 | $ | 45,251 | $ | 149,016 | (2,215 | ) |
$ | (31,628 | ) |
$ | 162,785 | $ | 30,325 | $ | 193,110 | |||||||||
See notes to consolidated financial statements.
40
U.S. PHYSICAL THERAPY, INC. AND SUBSIDIARIES
CONSOLIDATED STATEMENTS OF CASH FLOWS
(In thousands)
Year Ended December 31, 2015 |
Year Ended December 31, 2014 |
Year Ended December 31, 2013 |
|||||||
(In thousands) |
|||||||||
OPERATING ACTIVITIES |
|||||||||
Net income including non-controlling interests |
$ | 31,691 | $ | 30,424 | $ | 20,996 | |||
Adjustments to reconcile net income including non-controlling interests to net cash provided by operating activities: |
|||||||||
Depreciation and amortization |
7,952 | 6,740 | 5,562 | ||||||
Provision for doubtful accounts |
4,170 | 4,112 | 4,384 | ||||||
Equity-based awards compensation expense |
4,491 | 3,363 | 2,743 | ||||||
Loss (gain) on sale of business and fixed assets |
84 | 35 | 7,335 | ||||||
Excess tax benefit from equity-based awards |
(947 | ) |
(948 | ) |
(695 | ) |
|||
Deferred income tax |
7,001 | 6,275 | 2,369 | ||||||
Write-off of goodwill - closed clinics |
180 | 135 | — | ||||||
Changes in operating assets and liabilities: |
|||||||||
Increase in patient accounts receivable |
(5,519 | ) |
(5,388 | ) |
(5,389 | ) |
|||
Increase in accounts receivable - other |
(852 | ) |
341 | (5 | ) |
||||
(Increase) decrease in other assets |
(1,477 | ) |
(2,493 | ) |
1,803 | ||||
(Decrease) increase in accounts payable and accrued expenses |
(7,013 | ) |
1,868 | 4,833 | |||||
(Decrease) increase in other liabilities |
1,482 | 730 | 859 | ||||||
Net cash provided by operating activities |
41,243 | 45,194 | 44,795 | ||||||
INVESTING ACTIVITIES |
|||||||||
Purchase of fixed assets |
(6,263 | ) |
(5,167 | ) |
(4,637 | ) |
|||
Purchase of businesses, net of cash acquired |
(18,965 | ) |
(12,270 | ) |
(46,628 | ) |
|||
Acquisitions of non-controlling interests |
(7,083 | ) |
(5,490 | ) |
(1,876 | ) |
|||
Sale of non-controlling interests |
— | — | 233 | ||||||
Proceeds on sale of business and fixed assets, net |
71 | 47 | 459 | ||||||
Net cash used in investing activities |
(32,240 | ) |
(22,880 | ) |
(52,449 | ) |
|||
FINANCING ACTIVITIES |
|||||||||
Distributions to non-controlling interests (including redeemable non-controlling interests) |
(9,632 | ) |
(9,913 | ) |
(9,164 | ) |
|||
Cash dividends to shareholders |
(7,449 | ) |
(5,873 | ) |
(4,838 | ) |
|||
Proceeds from revolving line of credit |
103,000 | 134,300 | 150,800 | ||||||
Payments on revolving line of credit |
(93,500 | ) |
(139,800 | ) |
(128,200 | ) |
|||
Principal payments on notes payable |
(884 | ) |
(825 | ) |
(459 | ) |
|||
Tax benefit from stock based awards |
947 | 948 | 695 | ||||||
Other |
22 | 222 | 47 | ||||||
Net cash (used in) provided by financing activities |
(7,496 | ) |
(20,941 | ) |
8,881 | ||||
Net increase in cash and cash equivalents |
1,507 | 1,373 | 1,227 | ||||||
Cash and cash equivalents - beginning of period |
14,271 | 12,898 | 11,671 | ||||||
Cash and cash equivalents - end of period |
$ | 15,778 | $ | 14,271 | $ | 12,898 | |||
SUPPLEMENTAL DISCLOSURES OF CASH FLOW INFORMATION |
|||||||||
Cash paid during the period for: |
|||||||||
Income taxes |
$ | 7,779 | $ | 9,253 | $ | 4,111 | |||
Interest |
$ | 884 | $ | 1,103 | $ | 352 | |||
Non-cash investing and financing transactions during the period: |
|||||||||
Purchase of business - seller financing portion |
$ | 1,800 | $ | 400 | $ | 1,300 | |||
Acquisition of non-controlling interest - seller financing portion |
$ | 3,077 | $ | 67 | $ | — | |||
Revaluation of redeembale non-controlling interests |
$ | 529 | $ | 1,841 | $ | — | |||
See notes to consolidated financial statements.
41
U.S. PHYSICAL THERAPY, INC. AND SUBSIDIARIES
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
DECEMBER 31, 2015
1. Organization, Nature of Operations and Basis of Presentation
U.S. Physical Therapy, Inc. and its subsidiaries (together, the “Company”) operate outpatient physical therapy clinics that provide pre-and post-operative care and treatment for orthopedic-related disorders, sports-related injuries, preventative care, rehabilitation of injured workers and neurological-related injuries. As of December 31, 2015 the Company owned and/or operated 508 clinics in 42 states. The clinics’ business primarily originates from physician referrals. The principal sources of payment for the clinics’ services are managed care programs, commercial health insurance, Medicare/Medicaid, workers’ compensation insurance and proceeds from personal injury cases. In addition to the Company’s ownership and operation of outpatient physical therapy clinics, it also manages physical therapy facilities for third parties, such as physicians and hospitals, with 21 such third-party facilities under management as of December 31, 2015.
The consolidated financial statements include the accounts of U.S. Physical Therapy, Inc. and its subsidiaries. All significant intercompany transactions and balances have been eliminated. The Company primarily operates through subsidiary clinic partnerships, in which the Company generally owns a 1% general partnership interest and a 49% through 94% limited partnership interest. The managing therapist of each clinic owns the remaining limited partnership interest in the majority of the clinics (hereinafter referred to as “Clinic Partnership”). To a lesser extent, the Company operates some clinics through wholly-owned subsidiaries under profit sharing arrangements with therapists (hereinafter referred to as “Wholly-Owned Facilities”).
During the last three years, the Company completed the following multi-clinic acquisitions:
Acquisition |
Date |
% Interest Acquired |
Number of Clinics |
||||
2015 |
|||||||
January 2015 Acquisition |
January 31 |
60 | % |
9 | |||
April 2015 Acquisition |
April 30 |
70 | % |
3 | |||
June 2015 Acquisition |
June 30 |
70 | % |
4 | |||
December 2015 Acquisition |
December 31 |
59 | % |
4 | |||
2014 |
|||||||
April 2014 Acquisition |
April 30, 2014 |
70 | % |
13 | |||
August 2014 Acquisition |
August 1, 2014 |
100 | % |
3 | |||
2013 |
|||||||
February 2013 Acquisition |
February 28, 2013 |
72 | % |
9 | |||
April 2013 Acquisition |
April 30, 2013 |
50 | % |
5 | |||
May 2013 Acquisition |
May 24, 2013 |
80 | % |
5 | |||
December 9, 2013 Acquisition |
December 9, 2013 |
60 | % |
12 | |||
December 13, 2013 Acquisition |
December 13, 2013 |
90 | % |
11 | |||
In addition to the multi-clinic acquisitions, the Company acquired a 60% interest in a single clinic practice during 2015,the Company acquired four individual clinics in separate transactions during 2014, and the Company acquired three individual clinics in separate transactions during 2013.
Clinic Partnerships
For Clinic Partnerships, the earnings and liabilities attributable to the non-controlling interest, typically owned by the managing therapist, directly or indirectly, are recorded within the statements of net income and balance sheets as non-controlling interests.
42
Wholly-Owned Facilities
For Wholly-Owned Facilities with profit sharing arrangements, an appropriate accrual is recorded for the amount of profit sharing due the clinic partners/directors. The amount is expensed as compensation and included in clinic operating costs—salaries and related costs. The respective liability is included in current liabilities—accrued expenses on the balance sheets.
2. Significant Accounting Policies
Cash Equivalents
The Company maintains its cash and cash equivalents at financial institutions. The combined account balances at several institutions typically exceed Federal Deposit Insurance Corporation (“FDIC”) insurance coverage and, as a result, there is a concentration of credit risk related to amounts on deposit in excess of FDIC insurance coverage. Management believes that this risk is not significant.
Long-Lived Assets
Fixed assets are stated at cost. Depreciation is computed on the straight-line method over the estimated useful lives of the related assets. Estimated useful lives for furniture and equipment range from three to eight years and for software purchased from three to seven years. Leasehold improvements are amortized over the shorter of the related lease term or estimated useful lives of the assets, which is generally three to five years.
Impairment of Long-Lived Assets and Long-Lived Assets to Be Disposed Of
The Company reviews property and equipment and intangible assets with finite lives for impairment upon the occurrence of certain events or circumstances that indicate the related amounts may be impaired. Assets to be disposed of are reported at the lower of the carrying amount or fair value less costs to sell.
Goodwill
Goodwill represents the excess of the amount paid and fair value of the non-controlling interests over the fair value of the acquired business assets, which include certain identifiable intangible assets. Historically, goodwill has been derived from acquisitions and, prior to 2009, from the purchase of some or all of a particular local management’s equity interest in an existing clinic. Effective January 1, 2009, if the purchase price of a non-controlling interest by the Company exceeds or is less than the book value at the time of purchase, any excess or shortfall is recognized as an adjustment to additional paid-in capital.
The fair value of goodwill and other identifiable intangible assets with indefinite lives are tested for impairment annually and upon the occurrence of certain events, and are written down to fair value if considered impaired. The Company evaluates goodwill for impairment on at least an annual basis (in its third quarter) by comparing the fair value of its reporting units to the carrying value of each reporting unit including related goodwill. The Company operates a one segment business which is made up of various clinics within partnerships. The partnerships are components of regions and are aggregated to the operating segment level for the purpose of determining the Company’s reporting units when performing its annual goodwill impairment test. In 2015, 2014 and 2013, there were six regions.
An impairment loss generally would be recognized when the carrying amount of the net assets of a reporting unit, inclusive of goodwill and other identifiable intangible assets, exceeds the estimated fair value of the reporting unit. The estimated fair value of a reporting unit is determined using two factors: (i) earnings prior to taxes, depreciation and amortization for the reporting unit multiplied by a price/earnings ratio used in the industry and (ii) a discounted cash flow analysis. A weight is assigned to each factor and the sum of each weight times the factor is considered the estimated fair value. For 2015, the factors (i.e., price/earnings ratio, discount rate and residual capitalization rate) were updated to reflect current market conditions. The evaluation of goodwill in 2015, 2014 and 2013 did not result in any goodwill amounts that were deemed impaired.
43
The Company has not identified any triggering events occurring after the testing date that would impact the impairment testing results obtained. Factors which could result in future impairment charges include but are not limited to:
| • | changes as the result of government enacted national healthcare reform; |
| • | changes in Medicare rules and guidelines and reimbursement or failure of our clinics to maintain their Medicare certification or enrollment status; |
| • | revenue we receive from Medicare and Medicaid being subject to potential retroactive reduction; |
| • | business and regulatory conditions including federal and state regulation; |
| • | governmental and other third party payor inspections, reviews, investigations and audits; |
| • | compliance with federal and state laws and regulations relating to the privacy of individually identifiable patient information and associated fines and penalties for failure to comply; |
| • | possible legal actions, which could subject us to increased operating costs and uninsured liabilities; |
| • | changes in reimbursement rates or payment methods from third party payors including government agencies and deductibles and co-pays owed by patients; |
| • | revenue and earnings expectations; |
| • | general economic conditions; |
| • | availability and cost of qualified physical and occupational therapists; |
| • | personnel productivity and retaining key personnel; |
| • | competitive, economic or reimbursement conditions in our markets which may require us to reorganize or close certain operations and thereby incur losses and/or closure costs including the possible write-down or write-off of goodwill and other intangible assets; |
| • | acquisitions, purchases of non-controlling interests (minority interests) and the successful integration of the operations of the acquired business; |
| • | maintaining adequate internal controls; |
| • | maintaining necessary insurance coverage; |
| • | availability, terms, and use of capital; and |
| • | weather and other seasonal factors. |
The Company will continue to monitor for any triggering events or other indicators of impairment.
Non-controlling Interests
The Company recognizes non-controlling interests as equity in the consolidated financial statements separate from the parent entity’s equity. The amount of net income attributable to non-controlling interests is included in consolidated net income on the face of the statements of net income. Changes in a parent entity’s ownership interest in a subsidiary that do not result in deconsolidation are treated as equity transactions if the parent entity retains its controlling financial interest. The Company recognizes a gain or loss in net income when a subsidiary is deconsolidated. Such gain or loss is measured using the fair value of the non-controlling equity investment on the deconsolidation date.
When the purchase price of a non-controlling interest by the Company exceeds the book value at the time of purchase, any excess or shortfall is recognized as an adjustment to additional paid-in capital. Additionally, operating losses are allocated to non-controlling interests even when such allocation creates a deficit balance for the non-controlling interest partner.
The non-controlling interests that are reflected as redeemable non-controlling interests in the consolidated financial statements consist of those outside owners that have certain redemption rights that are currently exercisable, and that, if exercised, require that the Company purchases the non-controlling interest of the particular limited partner. At December 31, 2015, the redeemable non-controlling interests reflect the book value
44
of the non-controlling interests for those not deemed probable that the limited partner will assert the redemption rights and the fair value of the non-controlling interest for those deemed probable. The redeemable non-controlling interests was adjusted to the fair value in the reporting period in which the Company deems it probable that the limited partner will assert the redemption rights and will be adjusted each reporting period thereafter. The adjustments are charged to additional paid-in capital and are not reflected in the statements of net income. Although, the adjustments are not reflected in the statements of net income, current accounting rules require that the Company reflects the charge in the earning per share calculation.
Typically, for acquisitions, the Company agrees to purchase the individual’s non-controlling interest at a predetermined multiple of earnings before interest, taxes, depreciation and amortization.
Revenue Recognition
Revenues are recognized in the period in which services are rendered. Net patient revenues (patient revenues less estimated contractual adjustments) are reported at the estimated net realizable amounts from third-party payors, patients and others for services rendered. The Company has agreements with third-party payors that provide for payments to the Company at amounts different from its established rates. The allowance for estimated contractual adjustments is based on terms of payor contracts and historical collection and write-off experience.
The Company determines allowances for doubtful accounts based on the specific agings and payor classifications at each clinic. The provision for doubtful accounts is included in clinic operating costs in the statements of net income. Patient accounts receivable, which are stated at the historical carrying amount net of contractual allowances, write-offs and allowance for doubtful accounts, includes only those amounts the Company estimates to be collectible.
Medicare Reimbursement
The Medicare program reimburses outpatient rehabilitation providers based on the Medicare Physician Fee Schedule (“MPFS”). The MPFS rates have historically been subject to an automatic annual update based on a formula, called the sustainable growth rate (“SGR”) formula. The use of the SGR formula would have resulted in calculated automatic reductions in rates in every year since 2002; however, for each year through September 30, 2015, Centers for Medicare & Medicaid Services (“CMS”) or Congress has taken action to prevent the implementation of SGR formula reductions. On April 16, 2015, the Medicare Access and CHIP Reauthorization Act of 2015 (“MACRA”) was signed into law, eliminating the SGR formula and the associated annual automatic rate reductions. For services provided between January 1, 2015 and June 30, 2015 a 0% payment update was applied to the Medicare physician fee schedule payment rates; for services provided between July 1, 2015 and December 31, 2015 a 0.5% increase was applied to the fee schedule payment rates; for services provided in 2016 a 0.3% decrease is being applied to the fee schedule payment rates, and for 2017 through 2019, a 0.5% increase will be applied each year to the fee schedule payment rates, unless further adjusted by CMS. In addition, the MACRA promotes the development of new payment models that focus on quality and outcomes.
The Budget Control Act of 2011 increased the federal debt ceiling in connection with deficit reductions over the next ten years, and requires automatic reductions in federal spending by approximately $1.2 trillion. Payments to Medicare providers are subject to these automatic spending reductions, subject to a 2% cap. On April 1, 2013, a 2% reduction to Medicare payments was implemented.
As a result of the Balanced Budget Act of 1997, the formula for determining the total amount paid by Medicare in any one year for outpatient physical therapy, occupational therapy, and/or speech-language pathology services provided to any Medicare beneficiary (i.e., the “Therapy Cap” or “Limit”) was established. Based on the statutory definitions which constrained how the Therapy Cap would be applied, there is one Limit for Physical Therapy and Speech Language Pathology Services combined, and one Limit for Occupational Therapy. For 2015, the annual Limit on outpatient therapy services was $1,940 for Physical and Speech Language Pathology Services combined and $1,940 for Occupational Therapy Services. For 2016, the annual Limit on outpatient therapy services is $1,960 for Physical and Speech Language Pathology Services combined and $1,960 for Occupational Therapy Services. Historically, these Therapy Caps applied to outpatient therapy services provided in all settings, except for services provided in departments of hospitals. However, the Protecting Access to Medicare Act of 2014, and prior legislation, extended the Therapy Caps to services furnished in hospital
45
outpatient department settings. The application of these annual limits to hospital outpatient department settings will sunset on December 31, 2017 unless Congress extends it.
In the Deficit Reduction Act of 2005, Congress implemented an exceptions process to the annual Limit for therapy expenses for therapy services above the annual Limit. Therapy services above the annual Limit that are medically necessary satisfy an exception to the annual Limit and such claims are payable by the Medicare program. The Protecting Access to Medicare Act of 2014 extended the exceptions process for outpatient therapy caps through March 31, 2015. The MACRA further extended the exceptions process for outpatient therapy caps through December 31, 2017. Unless Congress extends the exceptions process further, the therapy caps will apply to all outpatient therapy services beginning January 1, 2018, except those services furnished and billed by outpatient hospital departments. For any claim above the annual Limit, the claim must contain a modifier indicating that the services are medically necessary and justified by appropriate documentation in the medical record.
Furthermore, under the Middle Class Tax Relief and Job Creation Act of 2012 (“MCTRA”), since October 1, 2012, patients who met or exceeded $3,700 in therapy expenditures during a calendar year have been subject to a manual medical review to determine whether applicable payment criteria are satisfied. The $3,700 threshold is applied to Physical Therapy and Speech Language Pathology Services; a separate $3,700 threshold is applied to the Occupational Therapy. The MACRA directed CMS to modify the manual medical review process such that those reviews will no longer apply to all claims exceeding the $3,700 threshold and instead will be determined on a targeted basis based on a variety of factors that CMS considers appropriate. The new factors have applied to exception requests for which CMS did not conduct a medical review by July 15, 2015.
CMS adopted a multiple procedure payment reduction (“MPPR”) for therapy services in the final update to the MPFS for calendar year 2011. The MPPR applied to all outpatient therapy services paid under Medicare Part B — occupational therapy, physical therapy and speech-language pathology. Under the policy, the Medicare program pays 100% of the practice expense component of the Relative Value Unit (“RVU”) for the therapy procedure with the highest practice expense RVU, then reduces the payment for the practice expense component for the second and subsequent therapy procedures or units of service furnished during the same day for the same patient, regardless of whether those therapy services are furnished in separate sessions. Since 2013, the practice expense component for the second and subsequent therapy service furnished during the same day for the same patient was reduced by 50%. In addition, the MCTRA directed CMS to implement a claims-based data collection program to gather additional data on patient function during the course of therapy in order to better understand patient conditions and outcomes. All practice settings that provide outpatient therapy services are required to include this data on the claim form. Since 2013, therapists have been required to report new codes and modifiers on the claim form that reflect a patient’s functional limitations and goals at initial evaluation, periodically throughout care, and at discharge: CMS has rejected claims if the required data is not included in the claim.
The Physician Quality Reporting System, or “PQRS,” is a CMS reporting program that uses a combination of incentive payments and payment reductions to promote reporting of quality information by “eligible professionals.” Although physical therapists, occupational therapists and qualified speech-language therapists are generally able to participate in the PQRS program, therapy professionals for whose services we bill through our certified rehabilitation agencies cannot participate because the Medicare claims processing systems currently cannot accommodate institutional providers such as certified rehabilitation agencies. Eligible professionals, such as those of our therapy professionals for whose services we bill using their individual Medicare provider numbers, who do not satisfactorily report data on quality measures will be subject to a 2% reduction in their Medicare payment in 2016 and 2017.
Statutes, regulations, and payment rules governing the delivery of therapy services to Medicare beneficiaries are complex and subject to interpretation. The Company believes that it is in compliance in all material respects with all applicable laws and regulations and is not aware of any pending or threatened investigations involving allegations of potential wrongdoing that would have a material effect on the Company’s financial statements as of December 31, 2015. Compliance with such laws and regulations can be subject to future government review and interpretation, as well as significant regulatory action including fines, penalties, and exclusion from the Medicare program. For 2015, net revenue from Medicare accounts for $73.2 million.
46
Management Contract Revenues
Management contract revenues are derived from contractual arrangements whereby the Company manages a clinic for third party owners. The Company does not have any ownership interest in these clinics. Typically, revenues are determined based on the number of visits conducted at the clinic and recognized when services are performed. Costs, typically salaries for the Company’s employees, are recorded when incurred. Management contract revenues are included in “other revenues” in the accompanying Consolidated Statements of Net Income.
Contractual Allowances
Contractual allowances result from the differences between the rates charged for services performed and expected reimbursements by both insurance companies and government sponsored healthcare programs for such services. Medicare regulations and the various third party payors and managed care contracts are often complex and may include multiple reimbursement mechanisms payable for the services provided in Company clinics. The Company estimates contractual allowances based on its interpretation of the applicable regulations, payor contracts and historical calculations. Each month the Company estimates its contractual allowance for each clinic based on payor contracts and the historical collection experience of the clinic and applies an appropriate contractual allowance reserve percentage to the gross accounts receivable balances for each payor of the clinic. Based on the Company’s historical experience, calculating the contractual allowance reserve percentage at the payor level is sufficient to allow the Company to provide the necessary detail and accuracy with its collectibility estimates. However, the services authorized and provided and related reimbursement are subject to interpretation that could result in payments that differ from the Company’s estimates. Payor terms are periodically revised necessitating continual review and assessment of the estimates made by management. The Company’s billing system does not capture the exact change in its contractual allowance reserve estimate from period to period in order to assess the accuracy of its revenues and hence its contractual allowance reserves. Management regularly compares its cash collections to corresponding net revenues measured both in the aggregate and on a clinic-by-clinic basis. In the aggregate, historically the difference between net revenues and corresponding cash collections has generally reflected a difference within approximately 1% of net revenues. Additionally, analysis of subsequent period’s contractual write-offs on a payor basis reflects a difference within approximately 1% between the actual aggregate contractual reserve percentage as compared to the estimated contractual allowance reserve percentage associated with the same period end balance. As a result, the Company believes that a change in the contractual allowance reserve estimate would not likely be more than 1% at December 31, 2015.
Income Taxes
Income taxes are accounted for under the asset and liability method. Deferred tax assets and liabilities are recognized for the future tax consequences attributable to differences between the financial statement carrying amounts of existing assets and liabilities and their respective tax bases and operating loss and tax credit carryforwards. Deferred tax assets and liabilities are measured using enacted tax rates expected to apply to taxable income in the years in which those temporary differences are expected to be recovered or settled. The effect on deferred tax assets and liabilities of a change in tax rates is recognized in income in the period that includes the enactment date.
The Company recognizes the financial statement benefit of a tax position only after determining that the relevant tax authority would more likely than not sustain the position following an audit. For tax positions meeting the more-likely-than-not threshold, the amount to be recognized in the financial statements is the largest benefit that has a greater than 50 percent likelihood of being realized upon ultimate settlement with the relevant tax authority.
The Company did not have any accrued interest or penalties associated with any unrecognized tax benefits nor was any interest expense recognized during the twelve months ended December 31, 2015 and 2014. The Company will book any interest or penalties, if required, in interest and/or other income/expense as appropriate.
On September 13, 2013, the U.S. Treasury Department and the I.R.S. issued final regulations that address costs incurred in acquiring, producing, or improving tangible property (the “Tangible Property Regulations”). The Tangible Property Regulations are generally effective for tax years beginning on or after January 1, 2014, and may be adopted in earlier years. The Company adopted the tax treatment of expenditures to improve tangible property and the capitalization of inherently facilitative costs to acquire tangible property as of January 1, 2014. Historically, the Company has treated the expenditures to improve tangible property and the capitalization of
47
inherently facilitative costs to acquire tangible property similar for tax and book. The impact of these changes were not material to the Company's consolidated financial statements.
Fair Values of Financial Instruments
The carrying amounts reported in the balance sheets for cash and cash equivalents, accounts receivable, accounts payable and notes payable approximate their fair values due to the short-term maturity of these financial instruments. The carrying amount under the Amended Credit Agreement (as defined in Note 10) approximates its fair value. The interest rate on the Credit Agreement, which is tied to the Eurodollar Rate, is set at various short-term intervals, as detailed in the Credit Agreement.
Segment Reporting
Operating segments are components of an enterprise for which separate financial information is available that is evaluated regularly by chief operating decision makers in deciding how to allocate resources and in assessing performance. The Company identifies operating segments based on management responsibility and believes it meets the criteria for aggregating its operating segments into a single reporting segment.
Use of Estimates
In preparing the Company’s consolidated financial statements, management makes certain estimates and assumptions, especially in relation to, but not limited to, goodwill impairment, allowance for receivables, tax provision and contractual allowances, that affect the amounts reported in the consolidated financial statements and related disclosures. Actual results may differ from these estimates.
Self-Insurance Program
The Company utilizes a self-insurance plan for its employee group health insurance coverage administered by a third party. Predetermined loss limits have been arranged with the insurance company to minimize the Company’s maximum liability and cash outlay. Accrued expenses include the estimated incurred but unreported costs to settle unpaid claims and estimated future claims. Management believes that the current accrued amounts are sufficient to pay claims arising from self-insurance claims incurred through December 31, 2015.
Restricted Stock
Restricted stock issued to employees and directors is subject to continued employment or continued service on the board, respectively. Generally, restrictions on the stock granted to employees lapse in equal annual installments on the following four anniversaries of the date of grant. For those shares granted to directors, the restrictions will lapse in equal quarterly installments during the first year after the date of grant. For those granted to executive officers, the restriction will lapse in equal quarterly installments during the four years following the date of grant. Compensation expense for grants of restricted stock is recognized based on the fair value per share on the date of grant amortized over the vesting period. The restricted stock issued is included in basic and diluted shares for the earnings per share computation.
Recently Adopted Accounting Guidance
In April 2014, the Financial Accounting Standards Board (“FASB”) issued changes to reporting discontinued operations and disclosures of disposals of components of an entity. These changes require a disposal of a component to meet a higher threshold in order to be reported as a discontinued operation in an entity’s financial statements. The threshold is defined as a strategic shift that has, or will have, a major effect on an entity’s operations and financial results such as a disposal of a major geographical area or a major line of business. Additionally, the following two criteria have been removed from consideration of whether a component meets the requirements for discontinued operations presentation: (i) the operations and cash flows of a disposal component have been or will be eliminated from the ongoing operations of an entity as a result of the disposal transaction, and (ii) an entity will not have any significant continuing involvement in the operations of the disposal component after the disposal transaction. Furthermore, equity method investments now may qualify for discontinued operations presentation. These changes also require expanded disclosures for all disposals of
48
components of an entity, whether or not the threshold for reporting as a discontinued operation is met, related to profit or loss information and/or asset and liability information of the component. These changes became effective for the Company on January 1, 2015. The adoption of these changes did not have an immediate impact on the Consolidated Financial Statements.
In November 2015, the FASB issued changes to the balance sheet classification of deferred taxes, which the Company early adopted, on a prospective basis in 2015. These changes simplify the presentation of deferred income taxes by requiring all deferred income tax assets and liabilities to be classified as noncurrent in a classified balance sheet. The current requirement that deferred tax assets and liabilities of a tax-paying component of an entity be offset and presented as a single amount is not affected by these changes. As such, all deferred income tax liabilities were classified in Other long-term liabilities line item on the December 31, 2015 Consolidated Balance Sheet.
Recently Issued Accounting Guidance
In September 2015, the FASB issued changes to the accounting for measurement-period adjustments related to business combinations. Currently, an acquiring entity is required to retrospectively adjust the balance sheet amounts of the acquiree recognized at the acquisition date with a corresponding adjustment to goodwill during the measurement period, as well as revise comparative information for prior periods presented within financial statements as needed, including revising income effects, such as depreciation and amortization, as a result of changes made to the balance sheet amounts of the acquiree. Such adjustments are required when new information is obtained about facts and circumstances that existed as of the acquisition date that, if known, would have affected the measurement of the amounts initially recognized or would have resulted in the recognition of additional assets or liabilities. The measurement period is the period after the acquisition date during which the acquirer may adjust the balance sheet amounts recognized for a business combination (generally up to one year from the date of acquisition). The changes eliminate the requirement to make such retrospective adjustments, and, instead require the acquiring entity to record these adjustments in the reporting period they are determined. Additionally, the changes require the acquiring entity to present separately on the face of the income statement or disclose in the notes to the financial statements the portion of the amount recorded in current-period income by line item that would have been recorded in previous reporting periods if the adjustment to the balance sheet amounts had been recognized as of the acquisition date. These changes become effective for the Company on January 1, 2016; however, early adoption is permitted. The Company is currently evaluating the standard to determine the impact it will have on its consolidated financial statements.
Subsequent Event
The Company has evaluated events occurring after the balance sheet date for possible disclosure as a subsequent event through the date that these consolidated financial statements were issued. No disclosure was required.
49
3. Acquisitions of Businesses
During 2015, 2014 and 2013, the Company completed the following multi-clinic acquisitions of physical therapy practices:
Acquisition |
Date |
% Interest Acquired |
Number of Clinics |
||||
2015 |
|||||||
January 2015 Acquisition |
January 31 |
60 | % |
9 | |||
April 2015 Acquisition |
April 30 |
70 | % |
3 | |||
June 2015 Acquisition |
June 30 |
70 | % |
4 | |||
December 2015 Acquisition |
December 31 |
59 | % |
4 | |||
2014 |
|||||||
April 2014 Acquisition |
April 30, 2014 |
70 | % |
13 | |||
August 2014 Acquisition |
August 1, 2014 |
100 | % |
3 | |||
2013 |
|||||||
February 2013 Acquisition |
February 28, 2013 |
72 | % |
9 | |||
April 2013 Acquisition |
April 30, 2013 |
50 | % |
5 | |||
May 2013 Acquisition |
May 24, 2013 |
80 | % |
5 | |||
December 9, 2013 Acquisition |
December 9, 2013 |
60 | % |
12 | |||
December 13, 2013 Acquisition |
December 13, 2013 |
90 | % |
11 | |||
In addition to the multi-clinic acquisitions detailed above, the Company acquired a 60% interest in an individual clinic practice during 2015, the Company acquired four individual clinics in separate transactions during 2014 and the Company acquired three individual clinics in separate transactions during 2013.
On December 31, 2015, the Company acquired a 59% interest in a four-clinic physical therapy practice. The purchase price was $4.6 million in cash and $400,000 in seller notes payable that are payable in two principal installments of an aggregate of $200,000 each, plus accrued interest, in December 2016 and 2017. On June 30, 2015, the Company acquired a 70% interest in a four-clinic physical therapy practice. The purchase price was $3.6 million in cash and $0.7 million in seller notes that are payable plus accrued interest, in June 2018. On April 30, 2015, the Company acquired a 70% interest in a three-clinic physical therapy practice. The purchase price was $4.7 million in cash and $150,000 in a seller note that is payable in two principal installments of $75,000 each, plus accrued interest, in April 2016 and 2017. On January 31, 2015, the Company acquired a 60% interest in a nine-clinic physical therapy practice. The purchase price for the 60% interest was $6.7 million in cash and $0.5 million in a seller note that is payable in two principal installments of $250,000 each, plus accrued interest, in January 2016 and 2017. In addition to the multi-clinic acquisitions, on August 31, 2015, the Company acquired a 60% interest in a single physical therapy clinic for $150,000 in cash and $50,000 in a seller note payable that is payable plus accrued interest in August 2016.
The purchase prices for the 2015 acquisitions have been preliminarily allocated as follows (in thousands):
Cash paid, net of cash acquired |
$ | 18,965 | |
Seller notes |
1,800 | ||
Total consideration |
$ | 20,765 | |
Estimated fair value of net tangible assets acquired: |
|||
Total current assets |
$ | 2,146 | |
Total non-current assets |
1,404 | ||
Total liabilities |
(1,036 | ) |
|
Net tangible assets acquired |
$ | 2,514 | |
Referral relationships |
3,069 | ||
Non-compete |
731 | ||
Tradename |
3,315 | ||
Goodwill |
23,428 | ||
Fair value of non-controlling interest |
(12,292 | ) |
|
$ | 20,765 |
50
The purchase price for the 70% interest in the April 2014 Acquisition was $10.6 million in cash and a $400,000 seller note, that is payable in two principal installments totaling $200,000 each, plus accrued interest, in April 2015 and 2016. The purchase price for the August 2014 Acquisition was $1.0 million in cash. In addition, during 2014, the Company acquired three individual clinic practices for an aggregate of $595,000.
The purchase prices for the 2014 acquisitions have been allocated as follows:
Cash paid, net of cash acquired |
$ | 12,270 | |
Seller notes |
400 | ||
Total consideration |
$ | 12,670 | |
Estimated fair value of net tangible assets acquired: |
|||
Total current assets |
$ | 1,213 | |
Total non-current assets |
1,051 | ||
Total liabilities |
(406 | ) |
|
Net tangible assets acquired |
$ | 1,858 | |
Referral relationships |
280 | ||
Non-compete |
330 | ||
Tradename |
1,600 | ||
Goodwill |
13,327 | ||
Fair value of non-controlling interest |
(4,725 | ) |
|
$ | 12,670 |
The purchase price for the 72% interest in the February 2013 Acquisition was $4.3 million in cash and $400,000 in a seller note, that was payable in two principal installments totaling $200,000 each, plus accrued interest, in February 2014 and 2015, which has been paid in full. The purchase price for the 50% interest in the April 2013 Acquisition was $2.4 million in cash and $200,000 in a seller note, that was payable in two principal installments totaling $100,000 each, plus accrued interest, in April of 2014 and 2015, which has been paid in full. The purchase price for the 80% interest in the May 2013 Acquisition was $3.6 million in cash and $200,000 in a seller note, that was payable in two principal installments totaling $100,000 each, plus accrued interest, in May of 2014 and 2015, which has been paid in full. The purchase price for the 60% interest in the December 9, 2013 Acquisition was $1.7 million in cash. The purchase price for the 90% interest in the December 13, 2013 Acquisition was $35.5 million in cash and $500,000 in a seller note, that was payable in two principal installments totaling $250,000 each, plus accrued interest, in December 2014 and 2015, which has been paid in full. The aggregate purchase price for the three individual clinic practices acquired in 2013 was $238,000.
The purchase prices for the acquisitions in 2013 were allocated as follows (in thousands):
Cash paid, net of cash acquired |
$ | 46,628 | |
Seller notes |
1,300 | ||
Total consideration |
$ | 47,928 | |
Estimated fair value of net tangible assets acquired: |
|||
Total current assets |
$ | 3,177 | |
Total non-current assets |
1,541 | ||
Total liabilities |
(538 | ) |
|
Net tangible assets acquired |
$ | 4,180 | |
Referral relationships |
6,140 | ||
Non-compete |
1,080 | ||
Tradename |
3,700 | ||
Goodwill |
43,369 | ||
Fair value of non-controlling interest |
(10,541 | ) |
|
$ | 47,928 |
The purchase prices plus the fair value of the non-controlling interests for the acquisitions in January 2015 and in 2014 and 2013 were allocated to the fair value of the assets acquired, inclusive of identifiable intangible assets, i.e. trade names, referral relationships and non-compete agreements, and liabilities assumed based on the
51
fair values at the acquisition date, with the amount exceeding the fair values being recorded as goodwill. For the other acquisitions in 2015, the Company is in the process of completing its formal valuation analysis to identify and determine the fair value of tangible and identifiable intangible assets acquired and the liabilities assumed. Thus, the final allocation of the purchase price may differ from the preliminary estimates used at December 31, 2015 based on additional information obtained and completion of the valuation of the identifiable intangible assets. Changes in the estimated valuation of the tangible assets acquired, the completion of the valuation of identifiable intangible assets and the completion by the Company of the identification of any unrecorded pre-acquisition contingencies, where the liability is probable and the amount can be reasonably estimated, will likely result in adjustments to goodwill.
For the acquisitions in January 2015 and in 2014 and 2013, the values assigned to the referral relationships and non-compete agreements are being amortized to expense equally over the respective estimated lives. For referral relationships, the range of the estimated lives was 4½ to 13 years, and for non-compete agreements the estimated lives was six years. Generally, the values assigned to tradenames are tested annually for impairment, however with regards to one acquisition in 2013, the tradename is being amortized over the term of the six year agreement in which the Company has acquired the rights to use the specific tradename. The values assigned to goodwill are tested annually for impairment.
For the 2015, 2014 and 2013 acquisitions, total current assets primarily represent primarily patient accounts receivable. Total non-current assets are fixed assets, primarily equipment, used in the practices.
The consideration paid for each of the acquisitions was derived through arm’s length negotiations. Funding for the cash portions was derived from proceeds from the Company’s revolving credit facility. The results of operations of the acquisitions have been included in the Company’s consolidated financial statements since their respective date of acquisition. Unaudited proforma consolidated financial information for the acquisitions in 2015, 2014, with the exception of the December 13, 2013 Acquisition (previously disclosed), and 2013 acquisitions have not been included as the results, individually and in the aggregate, were not material to current operations.
4. Acquisitions of Non-Controlling Interests
In 2015, the Company purchased additional interests in eight partnerships. The interests in the partnerships purchased ranged from 5% to 35%. The aggregate purchase price paid was $8.7 million of which $5.6 million was paid in cash and the Company entered into several notes payable of $3.1 million. The notes are payable in two installments plus accrued interest (interest accrues at 3.25%). The first principal installments in an aggregate of $1.2 million are due on December 31, 2018 and the second principal installments in an aggregate of $1.9 million are due on January 31, 2019. The purchase prices included an aggregate of $260,000 of undistributed earnings. The remaining $8.4 million, less future tax benefits of $3.3 million, was recognized as an adjustment to additional paid-in capital.
5. Redeemable Non-Controlling Interest
In 2015, the Company purchased additional interests in a partnership which was classified as redeemable non-controlling interest. The purchase price was $1.5 million in cash.
Also, in four separate transactions during 2014, the Company purchased partnership interests in four partnerships. The interests in the partnerships purchased and sold ranged from less than 1% to 35%. The aggregate of the purchase prices paid was $0.6 million. The purchase prices paid included a net of $0.1 million of undistributed earnings. The remaining $0.5 million, less future tax benefits of $0.2 million, was recognized as an adjustment to additional paid-in capital.
52
The following table details the changes in the carrying amount of redeemable non-controlling interest:
Year Ended December 31, 2015 |
Year Ended December 31, 2014 |
|||||
Beginning balance |
$ | 7,376 | $ | 4,104 | ||
Operating results allocated to redeemable non-controlling interest partners |
666 | 396 | ||||
Distributions to redeemable non-controlling interest partners |
(909 | ) |
(453 | ) |
||
Reclass of non-controlling interests |
2,681 | 6,375 | ||||
Increase due to revaluation fair value of redeemable non-controlling interest |
529 | 1,841 | ||||
Payments for purchase of redeemable non-controlling interests |
(1,500 | ) |
(4,887 | ) |
||
Ending balance |
$ | 8,843 | $ | 7,376 | ||
The non-controlling interests that are reflected as redeemable non-controlling interests in the consolidated financial statements consist of those owners who have certain redemption rights that are currently exercisable, and that, if exercised, require that the Company purchase the non-controlling interest of those owners. The redeemable non-controlling interests are adjusted to the fair value in the reporting period in which the Company deems it probable that the limited partner will assert the redemption rights and it will be adjusted each reporting period thereafter. The after tax adjustments are charged to additional paid-in capital and are not reflected in the statements of net income. Although the adjustments are not reflected in the statements of net income, current accounting rules require that the Company reflects the charge in the earnings per share calculation.
The results of operations of the acquired non-controlling interests are included in the accompanying financial statements from the dates of purchase in the net income attributable to common shareholders.
6. Divestiture of Business
On September 30, 2013, the Company sold the remainder of its physician services business. Previously, the Company closed its two physician services facilities – one in August 2013 and the other in December 2012. As previously disclosed in the Company’s public filings, the physician services business incurred negative gross margins in 2012 and through the first nine months of 2013. Revenues from physician services were generated by patient visits, franchise arrangements and fees from third parties. The results of operations and the loss on the sale of the physician services business have been reclassified to discontinued operations for all periods presented.
The Company received $400,000 cash and a note receivable of $500,000. The sale less the write-off of assets, primarily of goodwill and other intangible assets, and recording of appropriate accruals resulted in an after-tax loss of $4.4 million.
The following table details the losses from discontinued operations reported for the physician services business (in thousands):
Year Ended December 31, 2013 |
|||
Net revenues |
$ | 864 | |
Operating cost |
1,537 | ||
Gross margin |
(673 | ) |
|
Direct general and administrative expenses less proceeds |
1,176 | ||
Write off goodwill and other intangible assets |
6,338 | ||
Loss from discontinued operations, before tax |
(8,187 | ) |
|
Tax benefit (provision) |
3,180 | ||
(Loss) income from discontinued operations |
$ | (5,007 | ) |
The cash flow impact of the sale and closures is deemed immaterial for the consolidated statements of cash flows.
53
7. Goodwill
The changes in the carrying amount of goodwill as of December 31, 2015 and 2014 consisted of the following (in thousands):
Year Ended December 31, 2015 |
Year Ended December 31, 2014 |
|||||
Beginning balance |
$ | 147,914 | $ | 143,955 | ||
Goodwill acquired during the year |
23,428 | 12,974 | ||||
Goodwill allocated to specific assets for businesses acquired in 2013 |
— | (9,760 | ) |
|||
Goodwill adjustments for purchase price allocation of businesses acquired |
385 | 880 | ||||
Goodwill written-off - closed clinics |
(180 | ) |
(135 | ) |
||
Ending balance |
$ | 171,547 | $ | 147,914 | ||
8. Intangible Assets, net
Intangible assets, net as of December 31, 2015 and 2014 consisted of the following (in thousands):
December 31, 2015 |
December 31, 2014 |
|||||
Tradenames, net of accumulated amortization of $170 and $86, respectively |
$ | 17,660 | $ | 14,427 | ||
Referral relationships, net of accumulated amortization of $3,763 and $2,610, respectively |
10,866 | 8,951 | ||||
Non-compete agreements, net of accumulated amortization of $2,855 and $2,377, respectively |
1,770 | 1,529 | ||||
$ | 30,296 | $ | 24,907 | |||
Tradenames, referral relationships and non-compete agreements are related to the businesses acquired. Typically, the value assigned to tradenames has an indefinite life and is tested at least annually for impairment using the relief from royalty method in conjunction with the Company’s annual goodwill impairment test. However, for one acquisition, the value assigned to tradename is being amortized over the term of the six year agreement in which the Company has acquired the right to use the specific tradename. The value assigned to referral relationships is being amortized over their respective estimated useful lives which range from six to 16 years. Non-compete agreements are amortized over the respective term of the agreements which range from five to six years.
The following table details the amount of amortization expense recorded for intangible assets for the years ended December 31, 2015, 2014 and 2013 (in thousands):
Year Ended December 31, 2015 |
Year Ended December 31, 2014 |
Year Ended December 31, 2013 |
|||||||
Tradenames |
$ | 84 | $ | 86 | $ | — | |||
Referral relationships |
1,153 | 1,028 | 521 | ||||||
Non-compete agreements |
478 | 427 | 372 | ||||||
$ | 1,715 | $ | 1,541 | $ | 893 | ||||
During 2013, in conjunction with the sale of the physician services business, the Company wrote-off the referral relationships and non-compete agreements related to this business which included accumulated amortization of $156,000 and $270,000, respectively.
54
The remaining balances of the tradename, referral relationships and non-compete agreements is expected to be amortized as follows (in thousands):
Tradename |
Referral Relationships |
Non-Compete Agreements |
|||||||||||||
Years |
Annual Amount |
Years |
Annual Amount |
Years |
Annual Amount |
||||||||||
2016 |
83 | 2016 | 1,234 | 2016 | 485 | ||||||||||
2017 |
84 | 2017 | 1,234 | 2017 | 441 | ||||||||||
2018 |
83 | 2018 | 1,188 | 2018 | 384 | ||||||||||
2019 |
80 | 2019 | 1,099 | 2019 | 312 | ||||||||||
2020 | 1,099 | 2020 | 99 | ||||||||||||
2021 | 1,099 | 2021 | 49 | ||||||||||||
2022 | 1,050 | ||||||||||||||
2023 | 942 | ||||||||||||||
2024 | 824 | ||||||||||||||
2025 | 716 | ||||||||||||||
2026 | 255 | ||||||||||||||
2027 | 107 | ||||||||||||||
2028 | 19 | ||||||||||||||
9. Accrued Expenses
Accrued expenses as of December 31, 2015 and 2014 consisted of the following (in thousands):
December 31, 2015 |
December 31, 2014 |
|||||
Salaries and related costs |
$ | 9,414 | $ | 15,400 | ||
Group health insurance claims |
2,276 | 2,116 | ||||
Credit balances and overpayments due to patients and payors |
1,472 | 1,834 | ||||
Other |
3,434 | 3,489 | ||||
Total |
$ | 16,596 | $ | 22,839 | ||
10. Notes Payable
Notes payable as of December 31, 2015 and 2014 consisted of the following (dollars in thousands):
December 31, 2015 |
December 31, 2014 |
|||||
Credit Agreement average effective interest rate of 2.5% inclusive of unused fee |
$ | 44,000 | $ | 34,500 | ||
Various notes payable with $775 plus accrued interest due in the next year interest accrues in the range of 3.25% through 3.5% per annum |
5,110 | 1,117 | ||||
49,110 | 35,617 | |||||
Less current portion |
(775 | ) |
(883 | ) |
||
Long term portion |
$ | 48,335 | $ | 34,734 | ||
Effective December 5, 2013, we entered into an Amended and Restated Credit Agreement with a commitment for a $125.0 million revolving credit facility with a maturity date of November 30, 2018. This agreement was amended in August 2015 and January 2016 (hereafter referred to as “Amended Credit Agreement”). The Amended Credit Agreement is unsecured and has loan covenants, including requirements that the Company comply with a consolidated fixed charge coverage ratio and consolidated leverage ratio. Proceeds from the Amended Credit Agreement may be used for working capital, acquisitions, purchases of the Company’s common stock, dividend payments to the Company’s common stockholders, capital expenditures and other corporate purposes. The pricing grid which is based on the Company’s consolidated leverage ratio with the applicable spread over LIBOR ranging from 1.5% to 2.5% or the applicable spread over the Base Rate ranging from 0.1% to 1%. Fees under the Amended Credit Agreement include an unused commitment fee ranging from 0.1% to 0.25% depending on the Company’s consolidated leverage ratio and the amount of funds outstanding under the Amended Credit Agreement.
55
Effective January 11, 2016, the Company entered into an amendment to the Credit Agreement to increase the cash and noncash consideration that the Company could pay with respect to acquisitions permitted under the Amended Credit Agreement to $50,000,000 for any fiscal year from $25,000,000 and increased the amount the Company may pay in cash dividends to its shareholders in an aggregate amount not to exceed $10,000,000 in any fiscal year from $7,500,000.
On December 31, 2015, $44.0 million was outstanding on the Credit Agreement resulting in $81.0 million of availability. As of December 31, 2015, the Company was in compliance with all of the covenants thereunder.
The Company generally enters into various notes payable as a means of financing a portion of its acquisitions and purchases of non-controlling interests. In conjunction with the acquisitions in 2015 and the purchases of a non-controlling interest, the Company entered into notes payable in the aggregate amount of $4.9 million of which an aggregate principal payment of $575,000 in due in 2016; $525,000 in 2017; $1.9 million in 2018; and $1.9 million in 2019. Interest accrues in the range of 3.25% to 3.5% per annum and is payable with each principal installment. In conjunction with the 13 clinic-practice acquisition in 2014 and the purchase of a non-controlling interest, the Company entered into notes payable in the aggregate amount of $0.5 million, each note payable in two equal annual installments totaling $233,000 plus any accrued and unpaid interest. Interest accrues at 3.25% per annum, subjective to adjustment. In conjunction with the acquisitions in 2013, the Company entered into notes payable in the aggregate amount of $1.3 million, each payable in two equal annual installments totaling $650,000 plus any accrued and unpaid interest. Interest accrues at 3.25% per annum, subjective to adjustment.
Aggregate annual payments of principal required pursuant to the Credit Agreement and the above notes payable subsequent to December 31, 2015 are as follows (in thousands):
December 31, 2015 |
|||
During the twelve months ended December 30, 2016 |
$ | 775 | |
During the twelve months ended December 30, 2017 |
559 | ||
During the twelve months ended December 30, 2018 |
45,930 | ||
During the twelve months ended December 30, 2019 |
1,846 | ||
$ | 49,110 | ||
11. Income Taxes
Significant components of deferred tax assets included in the consolidated balance sheets at December 31, 2015 and 2014 were as follows (in thousands):
December 31, 2015 |
December 31, 2014 |
|||||
Deferred tax assets: |
||||||
Compensation |
$ | 1,830 | $ | 1,447 | ||
Allowance for doubtful accounts |
472 | 538 | ||||
Lease obligations - closed clinics |
50 | 32 | ||||
Deferred tax assets |
$ | 2,352 | $ | 2,017 | ||
Deferred tax liabilities: |
||||||
Depreciation and amortization |
$ | (8,989 | ) |
$ | (8,843 | ) |
Other |
(1,718 | ) |
(1,083 | ) |
||
Deferred tax liabilities |
(10,707 | ) |
(9,926 | ) |
||
Net deferred tax liabilities |
$ | (8,355 | ) |
$ | (7,909 | ) |
Amount included in: |
||||||
Other current assets |
$ | — | $ | 86 | ||
Deferred taxes and other long-term liabilities |
$ | (8,355 | ) |
$ | (7,995 | ) |
During 2015 and 2014, the Company recorded deferred tax assets of $3.5 million and $1.0 million, respectively, related to acquisitions of non-controlling interests. During 2015, the Company recorded an adjustment to the deferred tax assets of $3.0 million related to acquisitions of non-controlling interests in 2014 based on a detailed reconciliation of its federal and state taxes payable and receivable accounts along with its
56
federal and state deferred tax asset and liability accounts. The offset to this adjustment was a reduction in the previously reported tax receivable of approximately $1.8 million and a credit to additional-paid-in-capital of $1.2 million. At December 31, 2015 and 2014, the Company had a tax receivable of $3.4 million and $4.3 million (prior to adjustment of $3.0 million), respectively, included in other current assets on the accompanying consolidated balance sheets.
The differences between the federal tax rate and the Company’s effective tax rate for results of continuing operations for the years ended December 31, 2015, 2014 and 2013 were as follows (in thousands):
December 31, 2015 |
December 31, 2014 |
December 31, 2013 |
||||||||||||||||
U.S. tax at statutory rate |
$ | 12,926 | 35.0 | % |
$ | 12,294 | 35.0 | % |
$ | 10,415 | 35.0 | % |
||||||
State income taxes, net of federal benefit |
1,408 | 3.8 | % |
1,688 | 4.8 | % |
1,814 | 6.1 | % |
|||||||||
Deductible losses |
— | 0.0 | % |
— | 0.0 | % |
(98 | ) |
-0.3 | % |
||||||||
Non-deductible expenses |
319 | 0.9 | % |
292 | 0.8 | % |
105 | 0.3 | % |
|||||||||
$ | 14,653 | 39.7 | % |
$ | 14,274 | 40.6 | % |
$ | 12,236 | 41.1 | % |
|||||||
Significant components of the provision for income taxes for continuing operations for the years ended December 31, 2015, 2014 and 2013 were as follows (in thousands):
December 31, 2015 |
December 31, 2014 |
December 31, 2013 |
|||||||
Current: |
|||||||||
Federal |
$ | 6,460 | $ | 7,059 | $ | 8,445 | |||
State |
1,192 | 940 | 1,422 | ||||||
Total current |
7,652 | 7,999 | 9,867 | ||||||
Deferred: |
|||||||||
Federal |
6,237 | 5,266 | 1,970 | ||||||
State |
764 | 1,009 | 399 | ||||||
Total deferred |
7,001 | 6,275 | 2,369 | ||||||
Total income tax provision for continuing operations |
$ | 14,653 | $ | 14,274 | $ | 12,236 | |||
For 2015, 2014 and 2013, the Company performed a detailed reconciliation of its federal and state taxes payable and receivable accounts along with its federal and state deferred tax asset and liability accounts. As a result of this detailed analysis, the Company recorded an increase in the income tax provision of $147,000, $223,000 and $393,000 for 2015, 2014, and 2013, respectively. The Company considers this reconciliation process to be an annual control.
The Company is required to establish a valuation allowance for deferred tax assets if, based on the weight of available evidence, it is more likely than not that some portion or all of the deferred tax assets will not be realized. The ultimate realization of deferred tax assets is dependent upon the generation of future taxable income during the periods in which those temporary differences become deductible. Management considers the projected future taxable income and tax planning strategies in making this assessment. Based upon the level of historical taxable income and projections for future taxable income in the periods which the deferred tax assets are deductible, management believes that a valuation allowance is not required, as it is more likely than not that the results of future operations will generate sufficient taxable income to realize the deferred tax assets.
The Company’s U.S. federal returns remain open to examination for 2012 through 2014 and U.S. state jurisdictions are open for periods ranging from 2011 through 2014.
The Company does not believe that it has any significant uncertain tax positions at December 31, 2015, nor is this expected to change within the next twelve months due to the settlement and expiration of statutes of limitation.
The Company did not have any accrued interest or penalties associated with any unrecognized tax benefits nor was any interest expense recognized during the years ended December 31, 2015, 2014 and 2013.
57
12. Equity Based Plans
The Company has the following equity based plans with outstanding equity grants:
The Amended and Restated 1999 Employee Stock Option Plan (the “Amended 1999 Plan”) permits the Company to grant to non-employee directors and employees of the Company up to 600,000 non-qualified options to purchase shares of common stock and restricted stock (subject to proportionate adjustments in the event of stock dividends, splits, and similar corporate transactions). The exercise prices of options granted under the Amended 1999 Plan are determined by the Compensation Committee. The period within which each option will be exercisable is determined by the Compensation Committee. The Amended 1999 Plan was approved by the shareholders of the Company at the 2008 Shareholders Meeting on May 20, 2008.
The Amended and Restated 2003 Stock Option Plan (the “Amended 2003 Plan”) permits the Company to grant to key employees and outside directors of the Company incentive and non-qualified options and shares of restricted stock covering up to 1,750,000 shares of common stock (subject to proportionate adjustments in the event of stock dividends, splits, and similar corporate transactions). The material terms of the Amended 2003 Plan was reapproved by the shareholders of the Company at the 2015 Shareholders Meeting on May 19, 2015.
A cumulative summary of equity plans as of December 31, 2015 follows:
Authorized |
Restricted Stock Issued |
Outstanding Stock Options |
Stock Options Exercised |
Stock Options Exercisable |
Shares Available for Grant |
|||||||||||||
Equity Plans |
||||||||||||||||||
Amended 1999 Plan |
600,000 | 377,552 | — | 139,791 | — | 82,657 | ||||||||||||
Amended 2003 Plan |
1,750,000 | 705,382 | — | 778,300 | — | 266,318 | ||||||||||||
2,350,000 | 1,082,934 | — | 918,091 | — | 348,975 | |||||||||||||
During 2015, 2014 and 2013, the Company granted the following shares (net of those shares cancelled in their respective grant year due to employee terminations prior to restrictions lapsing) of restricted stock to directors, officers and employees pursuant to its equity plans as follows:
Year Granted |
Number of Shares |
Weighted Average Fair Value Per Share |
||||
2013 |
174,938 | $ | 23.52 | |||
2014 |
159,443 | $ | 33.29 | |||
2015 |
147,928 | $ | 41.66 | |||
Generally, restrictions on the stock granted to employees lapse in equal annual installments on the following four or five anniversaries of the date of grant. For those shares granted to directors, the restrictions will lapse in equal quarterly installments during the first year after the date of grant. For those granted to executive officers, the restriction will lapse in equal quarterly installments during the four years following the date of grant.
As of December 31, 2015, there were 265,718 shares outstanding for which restrictions had not lapsed. The restrictions will lapse in 2016 through 2019.
Compensation expense for grants of restricted stock is recognized based on the fair value on the date of grant. Compensation expense for restricted stock grants was $4,491,000, $3,363,000 and $2,743,000, respectively, for 2015, 2014 and 2013. As of December 31, 2015, the remaining $6.8 million of compensation expense will be recognized from 2016 through 2019.
13. Preferred Stock
The Board is empowered, without approval of the shareholders, to cause shares of preferred stock to be issued in one or more series and to establish the number of shares to be included in each such series and the rights, powers, preferences and limitations of each series. There are no provisions in the Company’s Articles of Incorporation specifying the vote required by the holders of preferred stock to take action. All such provisions would be set out in the designation of any series of preferred stock established by the Board. The bylaws of the Company specify that, when a quorum is present at any meeting, the vote of the holders of at least a majority of the outstanding shares entitled to vote who are present, in person or by proxy, shall decide any question brought before the meeting, unless a different vote is required by law or the Company’s Articles of Incorporation.
58
Because the Board has the power to establish the preferences and rights of each series, it may afford the holders of any series of preferred stock, preferences, powers, and rights, voting or otherwise, senior to the right of holders of common stock. The issuance of the preferred stock could have the effect of delaying or preventing a change in control of the Company.
14. Common Stock
From September 2001 through December 31, 2008, the Board authorized the Company to purchase, in the open market or in privately negotiated transactions, up to 2,250,000 shares of the Company’s common stock. In March 2009, the Board authorized the repurchase of up to 10% or approximately 1,200,000 shares of its common stock (the “March 2009 Authorization”). In connection with the March 2009 Authorization, the Company amended its prior credit agreement to permit share repurchases of up to $15,000,000. The Company is required to retire shares purchased under the March 2009 Authorization.
Under the March 2009 Authorization, the Company has purchased a total of 859,499 shares. There is no expiration date for the share repurchase program. The Credit Agreement was further amended to permit the Company to purchase, commencing on October 24, 2012 and at all times thereafter, up to $15,000,000 of its common stock subject to compliance with covenants. There are an additional estimated 279,433 shares (based on a closing price of $53.68 on December 31, 2015) that may be purchased from time to time in the open market or private transactions depending on price, availability and the Company’s cash position. The Company did not purchase any shares of its common stock during 2015 or 2014.
15. Defined Contribution Plan
The Company has several 401(k) profit sharing plans covering all employees with three months of service. For certain plans, the Company makes matching contributions. The Company may also make discretionary contributions of up to 50% of employee contributions. The Company did not make any discretionary contributions for the years ended December 31, 2015, 2014 and 2013. The Company matching contributions totaled $0.9 million, $0.7 million and $0.5 million, respectively, for the years ended December 31, 2015, 2014 and 2013.
16. Commitments and Contingencies
Operating Leases
The Company has entered into operating leases for its executive offices and clinic facilities. In connection with these agreements, the Company incurred rent expense of $28.3 million, $25.6 million and $22.0 million for the years ended December 31, 2015, 2014 and 2013, respectively. Several of the leases provide for an annual increase in the rental payment based upon the Consumer Price Index. The majority of the leases provide for renewal periods ranging from one to five years. The agreements to extend the leases specify that rental rates would be adjusted to market rates as of each renewal date.
The future minimum operating lease commitments for each of the next five years and thereafter and in the aggregate as of December 31, 2015 are as follows (in thousands):
December 31, 2015 |
|||
2016 |
$ | 26,799 | |
2017 |
20,896 | ||
2018 |
14,872 | ||
2019 |
9,216 | ||
2020 |
9,329 | ||
Thereafter |
3,117 | ||
Total |
$ | 84,229 | |
Employment Agreements
At December 31, 2015, the Company had outstanding employment agreements with three of its executive officers. These agreements, which presently expire on December 31, 2018, provide for automatic two year renewals at the conclusion of each expiring term or renewal term. All of the agreements contain a provision for annual adjustment of salaries.
59
In addition, the Company has outstanding employment agreements with most of the managing physical therapist partners of the Company’s physical therapy clinics and with certain other clinic employees which obligate subsidiaries of the Company to pay compensation of $25.7 million in 2016 and $13.3 million in the aggregate from 2017 through 2020. In addition, most of the employment agreements with the managing physical therapists provide for monthly bonus payments calculated as a percentage of each clinic’s net revenues (not in excess of operating profits) or operating profits.
17. Earnings Per Share
The computations of basic and diluted earnings per share for the years ended December 31, 2015, 2014 and 2013 are as follows (in thousands, except per share data):
Year Ended December 31, 2015 |
Year Ended December 31, 2014 |
Year Ended December 31, 2013 |
|||||||
Earnings per share attributable to common shareholders: |
|||||||||
Prior to revaluation of redeemable non-controlling interests, net of tax |
$ | 22,279 | $ | 20,853 | $ | 17,492 | |||
Charges to additional-paid-in-capital - revaluation of non-controlling interests, net of tax |
(314 | ) |
(1,086 | ) |
— | ||||
From continuing operations, net of tax |
21,965 | 19,767 | 17,492 | ||||||
From discontinued operations, net of tax |
— | — | (4,769 | ) |
|||||
$ | 21,965 | $ | 19,767 | $ | 12,723 | ||||
Basic earnings per share attributable to common shareholders: |
|||||||||
Prior to revaluation of redeemable non-controlling interests, net of tax |
$ | 1.80 | $ | 1.71 | $ | 1.45 | |||
Charges to additional-paid-in-capital - revaluation of non-controlling interests, net of tax |
(0.03 | ) |
(0.09 | ) |
— | ||||
From continuing operations, net of tax |
1.77 | 1.62 | 1.45 | ||||||
From discontinued operations, net of tax |
— | — | (0.40 | ) |
|||||
Basic |
$ | 1.77 | $ | 1.62 | $ | 1.05 | |||
Diluted earnings per share attributable to common shareholders: |
|||||||||
Prior to revaluation of redeemable non-controlling interests, net of tax |
$ | 1.80 | $ | 1.71 | $ | 1.45 | |||
Charges to additional-paid-in-capital - revaluation of non-controlling interests, net of tax |
(0.03 | ) |
(0.09 | ) |
— | ||||
From continuing operations, net of tax |
1.77 | 1.62 | 1.45 | ||||||
From discontinued operations, net of tax |
— | — | (0.40 | ) |
|||||
Diluted |
$ | 1.77 | $ | 1.62 | $ | 1.05 | |||
Shares used in computation: |
|||||||||
Basic earnings per share - weighted-average shares |
12,392 | 12,217 | 12,063 | ||||||
Effect of dilutive securities - stock options |
— | 4 | 19 | ||||||
Denominator for diluted earnings per share - adjusted weighted-average shares |
12,392 | 12,221 | 12,082 | ||||||
All options to purchase shares for the year ended December 31, 2015, 2014 and 2013 were included in the diluted earnings per share calculation as the average market price for those years exceeded the options’ exercise price.
60
18. Selected Quarterly Financial Data (Unaudited)
2015 Q1 |
2015 Q2 |
2015 Q3 |
2015 Q4 |
|||||||||
Net patient revenues |
$ | 75,807 | $ | 81,451 | $ | 82,154 | $ | 84,881 | ||||
Net revenues |
$ | 77,241 | $ | 83,288 | $ | 84,049 | $ | 86,724 | ||||
Operating income |
$ | 9,185 | $ | 13,549 | $ | 11,949 | $ | 12,611 | ||||
Net income including non-controlling interests |
$ | 6,151 | $ | 9,117 | $ | 8,064 | $ | 8,359 | ||||
Net income attributable to common shareholders |
$ | 4,166 | $ | 6,304 | $ | 5,818 | $ | 5,991 | ||||
Basic earnings per share attributable to common shareholders: |
||||||||||||
Prior to revaluation of redeemable non-controlling interests, net of tax |
$ | 0.34 | $ | 0.51 | $ | 0.47 | $ | 0.48 | ||||
Charges to additional-paid-in-capital - revaluation of redeemable non-controlling interests, net of tax |
— | (0.03 | ) |
— | — | |||||||
$ | 0.34 | $ | 0.48 | $ | 0.47 | $ | 0.48 | |||||
Diluted earnings per share attributable to common shareholders: |
||||||||||||
Prior to revaluation of redeemable non-controlling interests, net of tax |
$ | 0.34 | $ | 0.51 | $ | 0.47 | $ | 0.48 | ||||
Charges to additional-paid-in-capital - revaluation of redeemable non-controlling interests, net of tax |
— | (0.03 | ) |
— | — | |||||||
$ | 0.34 | $ | 0.48 | $ | 0.47 | $ | 0.48 | |||||
Shares used in computation: |
||||||||||||
Basic |
12,313 | 12,409 | 12,421 | 12,421 | ||||||||
Diluted |
12,313 | 12,409 | 12,421 | 12,421 | ||||||||
2014 Q1 |
2014 Q2 |
2014 Q3 |
2014 Q4 |
|||||||||
Net patient revenues |
$ | 68,397 | $ | 76,470 | $ | 76,184 | $ | 77,958 | ||||
Net revenues |
$ | 69,767 | $ | 78,201 | $ | 77,716 | $ | 79,390 | ||||
Operating income |
$ | 9,514 | $ | 14,221 | $ | 11,278 | $ | 10,755 | ||||
Net income including non-controlling interests |
$ | 6,323 | $ | 9,420 | $ | 7,418 | $ | 7,263 | ||||
Net income attributable to common shareholders |
$ | 4,228 | $ | 6,432 | $ | 5,216 | $ | 4,977 | ||||
Basic earnings per share attributable to common shareholders: |
||||||||||||
Prior to revaluation of redeemable non-controlling interests, net of tax |
$ | 0.35 | $ | 0.53 | $ | 0.43 | $ | 0.41 | ||||
Charges to additional-paid-in-capital - revaluation of redeemable non-controlling interests, net of tax |
(0.08 | ) |
(0.01 | ) |
— | — | ||||||
$ | 0.27 | $ | 0.52 | $ | 0.43 | $ | 0.41 | |||||
Diluted earnings per share attributable to common shareholders: |
||||||||||||
Prior to revaluation of redeemable non-controlling interests, net of tax |
$ | 0.35 | $ | 0.53 | $ | 0.43 | $ | 0.41 | ||||
Charges to additional-paid-in-capital - revaluation of redeemable non-controlling interests, net of tax |
(0.08 | ) |
(0.01 | ) |
— | — | ||||||
$ | 0.27 | $ | 0.52 | $ | 0.43 | $ | 0.41 | |||||
Shares used in computation: |
||||||||||||
Basic |
12,129 | 12,224 | 12,244 | 12,267 | ||||||||
Diluted |
12,144 | 12,226 | 12,247 | 12,271 | ||||||||
61
ITEM 9. CHANGES IN AND DISAGREEMENTS WITH ACCOUNTANTS ON ACCOUNTING AND FINANCIAL DISCLOSURE.
Not applicable.
ITEM 9A. CONTROLS AND PROCEDURES.
Evaluation of Disclosure Controls and Procedures
Our management, including our Chief Executive Officer and Chief Financial Officer, has conducted an evaluation of the effectiveness of our disclosure controls and procedures (as defined in Rule 13a-15(e) promulgated under the Exchange Act) as of the end of the fiscal period covered by this report. Based upon that evaluation, our Chief Executive Officer and Chief Financial Officer have concluded that our disclosure controls and procedures are effective in ensuring that the information required to be disclosed in the reports we file or submit under the Exchange Act is recorded, processed, summarized and reported, within the time periods specified in the rules and forms of the SEC and that such information is accumulated and communicated to our management, including our Chief Executive Officer and Chief Financial Officer, as appropriate to allow timely decisions regarding disclosure.
Changes in Internal Control Over Financial Reporting
There have been no changes in our internal control over financial reporting during the quarter ended December 31, 2015 that have materially affected, or are reasonably likely to materially affect, our internal control over financial reporting.
MANAGEMENT’S REPORT ON INTERNAL CONTROL OVER FINANCIAL REPORTING
Management is responsible for establishing and maintaining adequate internal control over financial reporting, as such term is defined in Rule 13a-15(f) under Exchange Act. U.S. Physical Therapy, Inc. and subsidiaries’ (the “Company”) internal control over financial reporting is designed to provide reasonable assurance regarding the reliability of financial reporting and the preparation of financial statements for external purposes in accordance with generally accepted accounting principles.
Internal control over financial reporting includes those policies and procedures that:
| • | Pertain to the maintenance of records that, in reasonable detail, accurately and fairly reflect the transactions and dispositions of the assets of the Company; |
| • | Provide reasonable assurance that transactions are recorded as necessary to permit preparation of financial statements in accordance with generally accepted accounting principles, and that our receipts and expenditures are being made only in accordance with authorizations of the Company’s management and directors; and |
| • | Provide reasonable assurance regarding prevention or timely detection of unauthorized acquisition, use or disposition of the Company’s assets that could have a material effect on the financial statements. |
Internal control over financial reporting cannot provide absolute assurance of achieving financial reporting objectives because of its inherent limitations. Internal control over financial reporting is a process that involves human diligence and compliance and is subject to lapses in judgment and breakdowns resulting from human failures. Internal control over financial reporting can also be circumvented by collusion or improper management override. Because of such limitations, there is a risk that material misstatements may not be prevented or detected on a timely basis by internal control over financial reporting. Also, projections of any evaluation of effectiveness to future periods are subject to the risk that controls may become inadequate because of changes in conditions, or that the degree of compliance with the policies or procedures may deteriorate. However, these inherent limitations are known features of the financial reporting process. Therefore, it is possible to design into the process safeguards to reduce, though not eliminate, the risk.
Management conducted an assessment of the effectiveness of our internal control over financial reporting as of December 31, 2015. In making this assessment, management used the criteria described in Internal Control — Integrated Framework (2013) issued by the Committee of Sponsoring Organizations of the Treadway Commission. Based on this assessment, management concluded that our internal control over financial reporting was effective as of December 31, 2015.
62
The Company’s internal control over financial reporting has been audited by Grant Thornton LLP, an independent registered public accounting firm, as stated in their report included on page 37.
Not applicable.
PART III
ITEM 10. DIRECTORS, EXECUTIVE OFFICERS AND CORPORATE GOVERNANCE.
The information required in response to this Item 10 is incorporated herein by reference to our definitive proxy statement relating to our 2016 Annual Meeting of Stockholders to be filed with the SEC pursuant to Regulation 14A, not later than 120 days after the end of our fiscal year covered by this report.
ITEM 11. EXECUTIVE COMPENSATION.
The information required in response to this Item 11 is incorporated herein by reference to our definitive proxy statement relating to our 2016 Annual Meeting of Stockholders to be filed with the SEC pursuant to Regulation 14A, not later than 120 days after the end of our fiscal year covered by this report.
ITEM 12. SECURITY OWNERSHIP OF CERTAIN BENEFICIAL OWNERS AND MANAGEMENT AND RELATED STOCKHOLDER MATTERS.
The information required in response to this Item 12 is incorporated herein by reference to our definitive proxy statement relating to our 2016 Annual Meeting of Stockholders to be filed with the SEC pursuant to Regulation 14A, not later than 120 days after the end of our fiscal year covered by this report.
ITEM 13. CERTAIN RELATIONSHIPS AND RELATED TRANSACTIONS, AND DIRECTOR INDEPENDENCE.
The information required in response to this Item 13 is incorporated herein by reference to our definitive proxy statement relating to our 2016 Annual Meeting of Stockholders to be filed with the SEC pursuant to Regulation 14A, not later than 120 days after the end of our fiscal year covered by this report.
ITEM 14. PRINCIPAL ACCOUNTANT FEES AND SERVICES.
The information required in response to this Item 14 is incorporated herein by reference to our definitive proxy statement relating to our 2016 Annual Meeting of Stockholders to be filed with the SEC pursuant to Regulation 14A, not later than 120 days after the end of our fiscal year covered by this report.
PART IV
ITEM 15. EXHIBITS AND FINANCIAL STATEMENT SCHEDULES.
(a) Documents filed as a part of this report:
1. Financial Statements. Reference is made to the Index to Financial Statements and Related Information under Item 8 in Part II hereof, where these documents are listed.
2. Financial Statement Schedules. See page 67 for Schedule II — Valuation and Qualifying Accounts. All other schedules are omitted because of the absence of conditions under which they are required or because the required information is shown in the financial statements or notes thereto.
3. Exhibits. The exhibits listed in List of Exhibits on the next page are filed or incorporated by reference as part of this report.
63
EXHIBIT INDEX
LIST OF EXHIBITS
|
Number
|
Description
|
|
|
|
|
3.1
|
Articles of Incorporation of the Company [filed as an exhibit to the Company’s Form 10-Q for the quarterly period ended June 30, 2001 and incorporated herein by reference].
|
|
|
|
|
3.2
|
Amendment to the Articles of Incorporation of the Company [filed as an exhibit to the Company’s Form 10-Q for the quarterly period ended June 30, 2001 and incorporated herein by reference].
|
|
|
|
|
3.3
|
Bylaws of the Company, as amended [filed as an exhibit to the Company’s Form 10-KSB for the year ended December 31, 1993 and incorporated herein by reference—Commission File Number—1-11151].
|
|
|
|
|
10.1+
|
1999 Employee Stock Option Plan (as amended and restated May 20, 2008) [incorporated by reference to Appendix A to the Company’s Definitive Proxy Statement on Schedule 14A, filed with the SEC on April 17, 2008].
|
|
|
|
|
10.2+
|
U. S. Physical Therapy, Inc. 2003 Stock Incentive Plan, as amended and restated March 26, 2010 [incorporated by reference to Appendix A to the Company’s proxy statement on Schedule 14A filed with the SEC on April 9, 2010].
|
|
|
|
|
10.3+
|
Consulting agreement between the Company and J. Livingston Kosberg [filed as an exhibit to the Company’s Form 10-Q for the quarterly period ended June 30, 2001 and incorporated herein by reference].
|
|
|
|
|
10.4+
|
First Amendment to the Consulting Agreement between the Company and J. Livingston—Kosberg [filed as an exhibit to the Company’s Form 10-K for the year ended December 31, 2002 and incorporated herein by reference.]
|
|
|
|
|
10.5+
|
Amended and Restated Employment Agreement dated May 24, 2007, between U.S. Physical Therapy, Inc. and Christopher J. Reading [incorporated by reference to Exhibit 10.3 to the Company’s Current Report on Form 8-K filed with the SEC on May 25, 2007].
|
|
|
|
|
10.6+
|
Amendment to Amended and Restated Employment Agreement dated December 2, 2008 between U.S. Physical Therapy, Inc. and Christopher J. Reading [incorporated by reference to Exhibit 10.1 to the Company’s Current Report on Form 8-K, filed with the SEC on December 5, 2008].
|
|
|
|
|
10.7+
|
Amended and Restated Employment Agreement dated May 24, 2007, between U.S. Physical Therapy, Inc. and Lawrance W. McAfee [incorporated by reference to Exhibit 10.4 to the Company’s Current Report on Form 8-K filed with the SEC on May 25, 2007].
|
|
|
|
|
10.8+
|
Amendment to Amended and Restated Employment Agreement dated December 2, 2008 between U.S. Physical Therapy, Inc. and Lawrance W. McAfee [incorporated by reference to Exhibit 10.2 to the Company’s Current Report on Form 8-K, filed with the SEC on December 5, 2008].
|
|
|
|
|
10.9+
|
Form of Restricted Stock Agreement [incorporated by reference to Exhibit 10.17 to the Company’s Annual Report on Form 10-K filed with the SEC on March 12, 2013.]
|
|
|
|
|
10.10+
|
Employment Agreement dated May 24, 2007, between U. S. Physical Therapy, Inc. and Glenn D. McDowell [incorporated by reference to Exhibit 10.2 to the Company’s Current Report on Form 8-K filed with the SEC on May 25, 2007].
|
|
|
|
|
10.11+
|
U. S. Physical Therapy, Inc. Long-Term Incentive Plan for Senior Management for 2013, effective March 27, 2013 [incorporated by reference to Exhibit 99.1 to the Company Current Report on Form 8-K filed with the SEC on April 1, 2013].
|
|
|
|
|
10.12+
|
U. S. Physical Therapy, Inc. Objective Cash Bonus Plan for 2013, effective March 27, 2013 [incorporated by reference to Exhibit 99.2 to the Company Current Report on Form 8-K filed with the SEC on April 1, 2013].
|
64
|
Number
|
Description
|
|
|
|
|
10.13+
|
U. S. Physical Therapy, Inc. Discretionary Cash Bonus Plan for 2013, effective March 27, 2013 [incorporated by reference to Exhibit 99.3 to the Company Current Report on Form 8-K filed with the SEC on April 1, 2013].
|
|
|
|
|
10.14+
|
U. S. Physical Therapy, Inc. Long-Term Incentive Plan for Senior Management for 2014, effective March 21, 2014 [incorporated by reference to Exhibit 99.1 to the Company Current Report on Form 8-K filed with the SEC on March 27, 2014].
|
|
|
|
|
10.15+
|
U. S. Physical Therapy, Inc. Discretionary Long-Term Incentive Plan for Senior Management for 2014, effective March 21, 2014 [incorporated by reference to Exhibit 99.2 to the Company Current Report on Form 8-K filed with the SEC on March 27, 2014].
|
|
|
|
|
10.16+
|
U. S. Physical Therapy, Inc. Objective Cash Bonus Plan for Senior Management for 2014, effective March 21, 2014 [incorporated by reference to Exhibit 99.3 to the Company Current Report on Form 8-K filed with the SEC on March 27, 2014].
|
|
|
|
|
10.17+
|
U. S. Physical Therapy, Inc. Discretionary Cash Bonus Plan for Senior Management for 2014, effective March 21, 2014 [incorporated by reference to Exhibit 99.4 to the Company Current Report on Form 8-K filed with the SEC on March 27, 2014].
|
|
|
|
|
10.18+
|
U. S. Physical Therapy, Inc. Long Term Incentive Plan for Senior Management for 2015, effective March 23, 2015 [incorporated by reference to Exhibit 99.1 to the Company’s Current Report on Form 8-K filed with the SEC on March 27, 2015.]
|
|
|
|
|
10.19+
|
U. S. Physical Therapy, Inc. Discretionary Long Term Incentive Plan for Senior Management for 2015, effective March 23, 2015 [incorporated by reference to Exhibit 99.2 to the Company’s Current Report on Form 8-K filed with the SEC on March 27, 2015.]
|
|
|
|
|
10.20+
|
U. S. Physical Therapy, Inc. Objective Cash Bonus Plan for Senior Management for 2015, effective March 23, 2015 [incorporated by reference to Exhibit 99.3 to the Company’s Current Report on Form 8-K filed with the SEC on March 27, 2015.]
|
|
|
|
|
10.21+
|
U. S. Physical Therapy, Inc. Discretionary Cash Bonus Plan for Senior Management for 2015, effective March 23, 2015 [incorporated by reference to Exhibit 99.4 to the Company’s Current Report on Form 8-K filed with the SEC on March 27, 2015.]
|
|
|
|
|
10.22
|
Amended and Restated Credit Agreement dated as of December 5, 2013, among the Company, as the borrower, and Bank of America, N.A., as Administrative Agent and other lenders party hereto [incorporated by reference to Exhibit 99.2 to the Company’s Current Report on Form 8-K filed with the SEC on December 9, 2013].
|
|
|
|
|
10.23
|
First Amendment to Amended and Restated Credit Agreement by and among the Company and the Lenders party hereto, and Bank of America, N.A., as Administrative Agent [incorporated by reference to Exhibit 99.1 to the Company’s Current Report on Form 8-K, filed with the SEC on September 4, 2015].
|
|
|
|
|
10.24
|
Second Amendment to Amended and Restated Credit Agreement by and among the Company and the Lenders party hereto, and Bank of America, N.A., as Administrative Agent [incorporated by reference to Exhibit 99.1 to the Company’s Current Report on Form 8-K, filed with the SEC on January 13, 2016].
|
|
|
|
|
10.25+
|
Amendment to employment agreement effective March 8, 2013 between U. S. Physical Therapy, Inc. and Christopher J. Reading [incorporated by reference to Exhibit 10.37 to the Company’s Annual Report on Form 10-K filed with the SEC on March 12, 2013].
|
|
|
|
|
10.26+
|
Amendment to employment agreement effective March 8, 2013 between U. S. Physical Therapy, Inc. and Lawrance M. McAfee [incorporated by reference to Exhibit 10.38 to the Company’s Annual Report on Form 10-K filed with the SEC on March 12, 2013].
|
65
|
Number
|
Description
|
|
|
|
|
10.27+
|
Second Amended and Restated Employment Agreement by and between the Company and Christopher J. Reading dated effective February 9, 2016 [incorporated by reference to Exhibit 10.1 to the Company’s Current Report on Form 8-K, filed with the SEC on February 12, 2016].
|
|
|
|
|
10.28+
|
Second Amended and Restated Employment Agreement by and between the Company and Lawrance W. McAfee dated effective February 9, 2016 [incorporated by reference to Exhibit 10.2 to the Company’s Current Report on Form 8-K, filed with the SEC on February 12, 2016].
|
|
|
|
|
10.29+
|
Amended and Restated Employment Agreement by and between the Company and Glenn D. McDowell dated effective February 9, 2016 [incorporated by reference to Exhibit 10.3 to the Company’s Current Report on Form 8-K, filed with the SEC on February 12, 2016].
|
|
|
|
|
10.30
|
Reorganization and Purchase Agreement dated as of December 13, 2013 between ARC Rehabilitation Services, LLC, Athletic & Rehabilitation Center, LLC, Matthew J. Condon and Kevin O’Rourke (as Sellers) and U.S. Physical Therapy, LTD (Purchaser). (Schedules pursuant to the Reorganization and Purchase Agreement have not been filed by the Registrant, who hereby undertakes to file such schedules upon the request of the Commission.) [incorporated by reference to Exhibit 10.1 to the Company’s Current Report on Form 8-K filed with the SEC on December 18, 2013].
|
|
|
|
|
21.1*
|
Subsidiaries of the Registrant
|
|
|
|
|
23.1*
|
Consent of Independent Registered Public Accounting Firm—Grant Thornton LLP
|
|
|
|
|
31.1*
|
Certification of Chief Executive Officer pursuant to Rule 13a-14(a) of the Securities Exchange Act of 1934, as amended
|
|
|
|
|
31.2*
|
Certification of Chief Financial Officer pursuant to Rule 13a-14(a) of the Securities Exchange Act of 1934, as amended
|
|
|
|
|
31.3*
|
Certification of Controller pursuant to Rule 13a-14(a) of the Securities Exchange Act of 1934, as amended
|
|
|
|
|
32.1*
|
Certification of Periodic Report of the Chief Executive Officer, Chief Financial Officer and Controller pursuant to Rule 13a-14(b) of the Securities Exchange Act of 1934, as amended, and 18 U.S.C. Section 1350, as adopted pursuant to Section 906 of the Sarbanes-Oxley Act of 2002
|
|
|
|
|
101.INS*
|
XBRL Instance Document
|
|
|
|
|
101.SCH*
|
XBRL Taxonomy Extension Schema Document
|
|
|
|
|
101.CAL*
|
XBRL Taxonomy Extension Calculation Linkbase Document
|
|
|
|
|
101.DEF*
|
XBRL Taxonomy Extension Definition Linkbase Document
|
|
|
|
|
101.LAB*
|
XBRL Taxonomy Extension Label Linkbase Document
|
|
|
|
|
101.PRE*
|
XBRL Taxonomy Extension Presentation Linkbase Document
|
| * | Filed herewith |
| + | Management contract or compensatory plan or arrangement. |
66
FINANCIAL STATEMENT SCHEDULE*
SCHEDULE II — VALUATION AND QUALIFYING ACCOUNTS
U.S. PHYSICAL THERAPY, INC. AND SUBSIDIARIES
COL. A |
COL B |
COL C |
COL D |
COL E |
|||||||||||
Additions |
|||||||||||||||
Description |
Balance at Beginning of Period |
Charged to Costs and Expenses |
Charged to Other Accounts |
Deductions |
Balance at End of Period |
||||||||||
(Amounts in Thousands) |
|||||||||||||||
YEAR ENDED DECEMBER 31, 2015: |
|||||||||||||||
Reserves and allowances deducted from asset accounts: |
|||||||||||||||
Allowance for doubtful accounts(1) |
$ | 1,867 | $ | 4,170 | — | $ | 4,395(2 | ) |
$ | 1,642 | |||||
YEAR ENDED DECEMBER 31, 2014: |
|||||||||||||||
Reserves and allowances deducted from asset accounts: |
|||||||||||||||
Allowance for doubtful accounts |
$ | 1,628 | $ | 4,112 | — | $ | 3,873(2 | ) |
$ | 1,867 | |||||
YEAR ENDED DECEMBER 31, 2013: |
|||||||||||||||
Reserves and allowances deducted from asset accounts: |
|||||||||||||||
Allowance for doubtful accounts |
$ | 2,109 | $ | 4,370 | — | $ | 4,851(2 | ) |
$ | 1,628 | |||||
| (1) | Related to patient accounts receivable and accounts receivable—other. |
| (2) | Uncollectible accounts written off, net of recoveries. |
| * | All other schedules are omitted because of the absence of conditions under which they are required or because the required information is shown in the financial statements or notes thereto. |
67
Pursuant to the requirements of Section 13 or 15(d) of the Securities Exchange Act of 1934, the registrant has duly caused this report to be signed on its behalf by the undersigned, thereunto duly authorized.
|
|
U.S. PHYSICAL THERAPY, INC.
|
|
|
|
(Registrant)
|
|
|
|
|
|
|
|
By:
|
/S/ LAWRANCE W. MCAFEE
|
|
|
|
Lawrance W. McAfee
|
|
|
|
Chief Financial Officer
|
|
|
|
|
|
|
By:
|
/S/ JON C. BATES
|
|
|
|
Jon C. Bates
|
|
|
|
Vice President/Controller
|
Date: March 4, 2016
Pursuant to the requirements of the Securities Exchange Act of 1934, this report has been signed below by the following persons on behalf of the registrant and in the capacities indicated as of the date indicated above.
|
By:
|
/S/ CHRISTOPHER J. READING
|
President, Chief Executive Officer and Director
(principal executive officer) |
|
|
Christopher J. Reading
|
|
|
|
|
|
|
By:
|
/S/ LAWRANCE W. MCAFEE
|
Executive Vice President, Chief Financial Officer and Director (principal financial and accounting officer)
|
|
|
Lawrance W. McAfee
|
|
|
|
|
|
|
By:
|
/S/ JERALD PULLINS
|
Chairman of the Board
|
|
|
Jerald Pullins
|
|
|
|
|
|
|
By:
|
/S/ DANIEL C. ARNOLD
|
Vice Chairman of the Board
|
|
|
Daniel C. Arnold
|
|
|
|
|
|
|
By:
|
/S/ MARK J. BROOKNER
|
Director
|
|
|
Mark J. Brookner
|
|
|
|
|
|
|
By:
|
/S/ HARRY S. CHAPMAN
|
Director
|
|
|
Harry S. Chapman
|
|
|
|
|
|
|
By:
|
/S/ BERNARD A. HARRIS, JR.
|
Director
|
|
|
Bernard A. Harris, Jr.
|
|
|
|
|
|
|
By:
|
/S/ MARLIN W. JOHNSTON
|
Director
|
|
|
Marlin W. Johnston
|
|
|
|
|
|
|
By:
|
/S/ EDWARD L. KUNTZ
|
Director
|
|
|
Edward L. Kuntz
|
|
|
|
|
|
|
By:
|
/S/ REGG SWANSON
|
Director
|
|
|
Regg Swanson
|
|
|
|
|
|
|
By:
|
/S/ CLAYTON TRIER
|
Director
|
|
|
Clayton Trier
|
|
68
EXHIBIT INDEX
LIST OF EXHIBITS
|
Number
|
Description
|
|
|
|
|
3.1
|
Articles of Incorporation of the Company [filed as an exhibit to the Company’s Form 10-Q for the quarterly period ended June 30, 2001 and incorporated herein by reference].
|
|
|
|
|
3.2
|
Amendment to the Articles of Incorporation of the Company [filed as an exhibit to the Company’s Form 10-Q for the quarterly period ended June 30, 2001 and incorporated herein by reference].
|
|
|
|
|
3.3
|
Bylaws of the Company, as amended [filed as an exhibit to the Company’s Form 10-KSB for the year ended December 31, 1993 and incorporated herein by reference—Commission File Number—1-11151].
|
|
|
|
|
10.1+
|
1999 Employee Stock Option Plan (as amended and restated May 20, 2008) [incorporated by reference to Appendix A to the Company’s Definitive Proxy Statement on Schedule 14A, filed with the SEC on April 17, 2008].
|
|
|
|
|
10.2+
|
U. S. Physical Therapy, Inc. 2003 Stock Incentive Plan, as amended and restated March 26, 2010 [incorporated by reference to Appendix A to the Company’s proxy statement on Schedule 14A filed with the SEC on April 9, 2010].
|
|
|
|
|
10.3+
|
Consulting agreement between the Company and J. Livingston Kosberg [filed as an exhibit to the Company’s Form 10-Q for the quarterly period ended June 30, 2001 and incorporated herein by reference].
|
|
|
|
|
10.4+
|
First Amendment to the Consulting Agreement between the Company and J. Livingston—Kosberg [filed as an exhibit to the Company’s Form 10-K for the year ended December 31, 2002 and incorporated herein by reference.]
|
|
|
|
|
10.5+
|
Amended and Restated Employment Agreement dated May 24, 2007, between U.S. Physical Therapy, Inc. and Christopher J. Reading [incorporated by reference to Exhibit 10.3 to the Company’s Current Report on Form 8-K filed with the SEC on May 25, 2007].
|
|
|
|
|
10.6+
|
Amendment to Amended and Restated Employment Agreement dated December 2, 2008 between U.S. Physical Therapy, Inc. and Christopher J. Reading [incorporated by reference to Exhibit 10.1 to the Company’s Current Report on Form 8-K, filed with the SEC on December 5, 2008].
|
|
|
|
|
10.7+
|
Amended and Restated Employment Agreement dated May 24, 2007, between U.S. Physical Therapy, Inc. and Lawrance W. McAfee [incorporated by reference to Exhibit 10.4 to the Company’s Current Report on Form 8-K filed with the SEC on May 25, 2007].
|
|
|
|
|
10.8+
|
Amendment to Amended and Restated Employment Agreement dated December 2, 2008 between U.S. Physical Therapy, Inc. and Lawrance W. McAfee [incorporated by reference to Exhibit 10.2 to the Company’s Current Report on Form 8-K, filed with the SEC on December 5, 2008].
|
|
|
|
|
10.9+
|
Form of Restricted Stock Agreement [incorporated by reference to Exhibit 10.17 to the Company's Annual Report on Form 10-K filed with the SEC on March 12, 2013.]
|
|
|
|
|
10.10+
|
Employment Agreement dated May 24, 2007, between U. S. Physical Therapy, Inc. and Glenn D. McDowell [incorporated by reference to Exhibit 10.2 to the Company’s Current Report on Form 8-K filed with the SEC on May 25, 2007].
|
|
|
|
|
10.11+
|
U. S. Physical Therapy, Inc. Long-Term Incentive Plan for Senior Management for 2013, effective March 27, 2013 [incorporated by reference to Exhibit 99.1 to the Company Current Report on Form 8-K filed with the SEC on April 1, 2013].
|
|
|
|
|
10.12+
|
U. S. Physical Therapy, Inc. Objective Cash Bonus Plan for 2013, effective March 27, 2013 [incorporated by reference to Exhibit 99.2 to the Company Current Report on Form 8-K filed with the SEC on April 1, 2013].
|
69
|
Number
|
Description
|
|
|
|
|
10.13+
|
U. S. Physical Therapy, Inc. Discretionary Cash Bonus Plan for 2013, effective March 27, 2013 [incorporated by reference to Exhibit 99.3 to the Company Current Report on Form 8-K filed with the SEC on April 1, 2013].
|
|
|
|
|
10.14+
|
U. S. Physical Therapy, Inc. Long-Term Incentive Plan for Senior Management for 2014, effective March 21, 2014 [incorporated by reference to Exhibit 99.1 to the Company Current Report on Form 8-K filed with the SEC on March 27, 2014].
|
|
|
|
|
10.15+
|
U. S. Physical Therapy, Inc. Discretionary Long-Term Incentive Plan for Senior Management for 2014, effective March 21, 2014 [incorporated by reference to Exhibit 99.2 to the Company Current Report on Form 8-K filed with the SEC on March 27, 2014].
|
|
|
|
|
10.16+
|
U. S. Physical Therapy, Inc. Objective Cash Bonus Plan for Senior Management for 2014, effective March 21, 2014 [incorporated by reference to Exhibit 99.3 to the Company Current Report on Form 8-K filed with the SEC on March 27, 2014].
|
|
|
|
|
10.17+
|
U. S. Physical Therapy, Inc. Discretionary Cash Bonus Plan for Senior Management for 2014, effective March 21, 2014 [incorporated by reference to Exhibit 99.4 to the Company Current Report on Form 8-K filed with the SEC on March 27, 2014].
|
|
|
|
|
10.18+
|
U. S. Physical Therapy, Inc. Long Term Incentive Plan for Senior Management for 2015, effective March 23, 2015 [incorporated by reference to Exhibit 99.1 to the Company’s Current Report on Form 8-K filed with the SEC on March 27, 2015.]
|
|
|
|
|
10.19+
|
U. S. Physical Therapy, Inc. Discretionary Long Term Incentive Plan for Senior Management for 2015, effective March 23, 2015 [incorporated by reference to Exhibit 99.2 to the Company’s Current Report on Form 8-K filed with the SEC on March 27, 2015.]
|
|
|
|
|
10.20+
|
U. S. Physical Therapy, Inc. Objective Cash Bonus Plan for Senior Management for 2015, effective March 23, 2015 [incorporated by reference to Exhibit 99.3 to the Company’s Current Report on Form 8-K filed with the SEC on March 27, 2015.]
|
|
|
|
|
10.21+
|
U. S. Physical Therapy, Inc. Discretionary Cash Bonus Plan for Senior Management for 2015, effective March 23, 2015 [incorporated by reference to Exhibit 99.4 to the Company’s Current Report on Form 8-K filed with the SEC on March 27, 2015.]
|
|
|
|
|
10.22
|
Amended and Restated Credit Agreement dated as of December 5, 2013, among the Company, as the borrower, and Bank of America, N.A., as Administrative Agent and other lenders party hereto [incorporated by reference to Exhibit 99.2 to the Company's Current Report on Form 8-K filed with the SEC on December 9, 2013].
|
|
|
|
|
10.23
|
First Amendment to Amended and Restated Credit Agreement by and among the Company and the Lenders party hereto, and Bank of America, N.A., as Administrative Agent [incorporated by reference to Exhibit 99.1 to the Company’s Current Report on Form 8-K, filed with the SEC on September 4, 2015].
|
|
|
|
|
10.24
|
Second Amendment to Amended and Restated Credit Agreement by and among the Company and the Lenders party hereto, and Bank of America, N.A., as Administrative Agent [incorporated by reference to Exhibit 99.1 to the Company’s Current Report on Form 8-K, filed with the SEC on January 13, 2016].
|
|
|
|
|
10.25+
|
Amendment to employment agreement effective March 8, 2013 between U. S. Physical Therapy, Inc. and Christopher J. Reading [incorporated by reference to Exhibit 10.37 to the Company's Annual Report on Form 10-K filed with the SEC on March 12, 2013].
|
|
|
|
|
10.26+
|
Amendment to employment agreement effective March 8, 2013 between U. S. Physical Therapy, Inc. and Lawrance M. McAfee [incorporated by reference to Exhibit 10.38 to the Company's Annual Report on Form 10-K filed with the SEC on March 12, 2013].
|
70
|
Number
|
Description
|
|
|
|
|
10.27+
|
Second Amended and Restated Employment Agreement by and between the Company and Christopher J. Reading dated effective February 9, 2016 [incorporated by reference to Exhibit 10.1 to the Company’s Current Report on Form 8-K, filed with the SEC on February 12, 2016].
|
|
|
|
|
10.28+
|
Second Amended and Restated Employment Agreement by and between the Company and Lawrance W. McAfee dated effective February 9, 2016 [incorporated by reference to Exhibit 10.2 to the Company’s Current Report on Form 8-K, filed with the SEC on February 12, 2016].
|
|
|
|
|
10.29+
|
Amended and Restated Employment Agreement by and between the Company and Glenn D. McDowell dated effective February 9, 2016 [incorporated by reference to Exhibit 10.3 to the Company’s Current Report on Form 8-K, filed with the SEC on February 12, 2016].
|
|
|
|
|
10.30
|
Reorganization and Purchase Agreement dated as of December 13, 2013 between ARC Rehabilitation Services, LLC, Athletic & Rehabilitation Center, LLC, Matthew J. Condon and Kevin O'Rourke (as Sellers) and U.S. Physical Therapy, LTD (Purchaser). (Schedules pursuant to the Reorganization and Purchase Agreement have not been filed by the Registrant, who hereby undertakes to file such schedules upon the request of the Commission.) [incorporated by reference to Exhibit 10.1 to the Company's Current Report on Form 8-K filed with the SEC on December 18, 2013].
|
|
|
|
|
21.1*
|
Subsidiaries of the Registrant
|
|
|
|
|
23.1*
|
Consent of Independent Registered Public Accounting Firm—Grant Thornton LLP
|
|
|
|
|
31.1*
|
Certification of Chief Executive Officer pursuant to Rule 13a-14(a) of the Securities Exchange Act of 1934, as amended
|
|
|
|
|
31.2*
|
Certification of Chief Financial Officer pursuant to Rule 13a-14(a) of the Securities Exchange Act of 1934, as amended
|
|
|
|
|
31.3*
|
Certification of Controller pursuant to Rule 13a-14(a) of the Securities Exchange Act of 1934, as amended
|
|
|
|
|
32.1*
|
Certification of Periodic Report of the Chief Executive Officer, Chief Financial Officer and Controller pursuant to Rule 13a-14(b) of the Securities Exchange Act of 1934, as amended, and 18 U.S.C. Section 1350, as adopted pursuant to Section 906 of the Sarbanes-Oxley Act of 2002
|
|
|
|
|
101.INS*
|
XBRL Instance Document
|
|
|
|
|
101.SCH*
|
XBRL Taxonomy Extension Schema Document
|
|
|
|
|
101.CAL*
|
XBRL Taxonomy Extension Calculation Linkbase Document
|
|
|
|
|
101.DEF*
|
XBRL Taxonomy Extension Definition Linkbase Document
|
|
|
|
|
101.LAB*
|
XBRL Taxonomy Extension Label Linkbase Document
|
|
|
|
|
101.PRE*
|
XBRL Taxonomy Extension Presentation Linkbase Document
|
| * | Filed herewith |
| + | Management contract or compensatory plan or arrangement. |
71
