Attached files
| file | filename |
|---|---|
| 8-K - 8-K - REVA Medical, Inc. | a15-21188_18k.htm |
Exhibit 99.1

Fantom Presentation at Next-Generation Session
San Diego, California and Sydney, Australia (Thursday, 15 October 2015, AEST) — REVA Medical, Inc. (ASX: RVA) (“REVA” or the “Company”) is pleased to announce that Dr. J. Ribamar Costa, from Dante Pazzanese of Cardiology, in Sao Paulo, Brazil, is presenting performance data on REVA’s Fantom® sirolimus-eluting bioresorbable scaffold at the Transcatheter Cardiovascular Therapeutics (“TCT”) Conference, which is being held October 11th through 15th in San Francisco, California.
Dr. Costa’s presentation is during the Next-Generation DES Technology: Let the Future Begin session this evening. His presentation highlights the imaging advantages physicians can expect when using the Fantom scaffold to treat coronary artery disease. These advantages are made possible by Fantom’s complete visibility under x-ray, an attribute that is unique among bioresorbable scaffolds. This feature enhances both x-ray and optical coherence tomography (“OCT”) imaging to help ensure precise scaffold placement and accurate lesion coverage, especially when implanting in challenging anatomy.
Dr. Costa is also presenting angiographic results from the Company’s FANTOM I pilot study, which enrolled seven patients between December 2014 and February 2015. The data demonstrates sustained vessel patency through the four-month follow-up time point. Additional data from the FANTOM I pilot study and preliminary data from the FANTOM II CE Mark trial will be presented at TCT’s Bioresorbable Vascular Scaffolds, Part 2 session, which is being held on Thursday, October 15th.
The presentation materials delivered at the Next Generation Session are attached hereto. The presentation materials are also available in the Investor Relations section of REVA’s website at www.revamedical.com and are being filed with the U.S. Securities and Exchange Commission.
About REVA
REVA is a clinical stage medical device company located in San Diego, California, USA, that is working to commercialize its proprietary bioresorbable stents, which are called “scaffolds” because of their temporary nature. The Company’s scaffolds have been developed as an alternative to metal stents, which are small tube-like devices permanently implanted into an artery to treat coronary artery disease. Scaffolds provide restoration of blood flow, support the artery through the healing process, then disappear (or “resorb”) from the body over a period of time. This resorption allows the return of natural movement and function of the artery, a result not attainable with permanent metal stents. The Company’s initial product, the Fantom® scaffold, has been designed to offer an ideal balance of thinness and strength and distinct ease-of-use features including complete scaffold visibility under x-ray, expansion with one continuous inflation, and no procedural time limitations. REVA will require successful clinical trial results and regulatory approval before it can commercialize Fantom or any other products.
HEAD OFFICE: 5751 Copley Drive, San Diego, CA 92111 · +1 (858) 966-3000 · +1 (858) 966-3099 (FAX) · www.revamedical.com
AUSTRALIAN OFFICE: Suite 4, Level 14, 6 O’Connell Street, Sydney NSW 2000 · +61 2 9237 2800
ARBN 146 505 777 · REVA Medical, Inc., is a foreign company incorporated in Delaware, USA, whose stockholders have limited liability
Forward-Looking Statements
This announcement contains or may contain forward-looking statements that are based on management’s beliefs, assumptions and expectations and on information currently available to management. All statements that are not statements of historical fact, including those statements that address future operating performance and events or developments that we expect or anticipate will occur in the future, are forward-looking statements, such as those statements regarding our ability to obtain regulatory approvals, timely and successfully complete our clinical trials, protect our intellectual property position, commercialize our products if and when approved, develop and commercialize new products, recruit and retain our key personnel, and estimates regarding our capital requirements and financial performance. You should not place undue reliance on forward-looking statements. Although management believes forward-looking statements are reasonable as and when made, forward-looking statements are subject to a number of risks and uncertainties that may cause our actual results to vary materially from those expressed in forward-looking statements, including the risks and uncertainties that are described in the “Risk Factors” section of our Annual Report on Form 10-K filed with the US Securities and Exchange Commission (the “SEC”) on March 30, 2015, and as may be updated in our periodic reports thereafter. Any forward-looking statements in this announcement speak only as of the date when made. REVA does not assume any obligation to publicly update or revise any forward-looking statements, whether as a result of new information, future events, or otherwise.
|
United States |
|
Australia |
|
Australia |
|
Investor & Media Enquiries: |
|
Investor Enquiries: |
|
Media Enquiries: |
|
REVA Medical, Inc. |
|
Inteq Limited |
|
Buchan Consulting |
|
Cheryl Liberatore |
|
Kim Jacobs |
|
Rebecca Wilson |
|
Director, Communications |
|
+61 2 9229 2700 |
|
+61 3 9866 4722 |
|
+1 858-966-3045 |
|
|
|
Annabel Murphy |
|
|
|
|
|
+61 2 9237 2800 |
FantomTM Radiopacity & Imaging Differences Jose de Ribamar Costa Jr, MD, PhD, FACC Instituto Dante Pazzanese de Cardiologia HCOR São Paulo - Brazil

Disclosure Statement of Financial Interest I, Jose de Ribamar Costa, DO NOT have a financial interest/arrangement or affiliation with one or more organizations that could be perceived as a real or apparent conflict of interest in the context of the subject of this presentation.

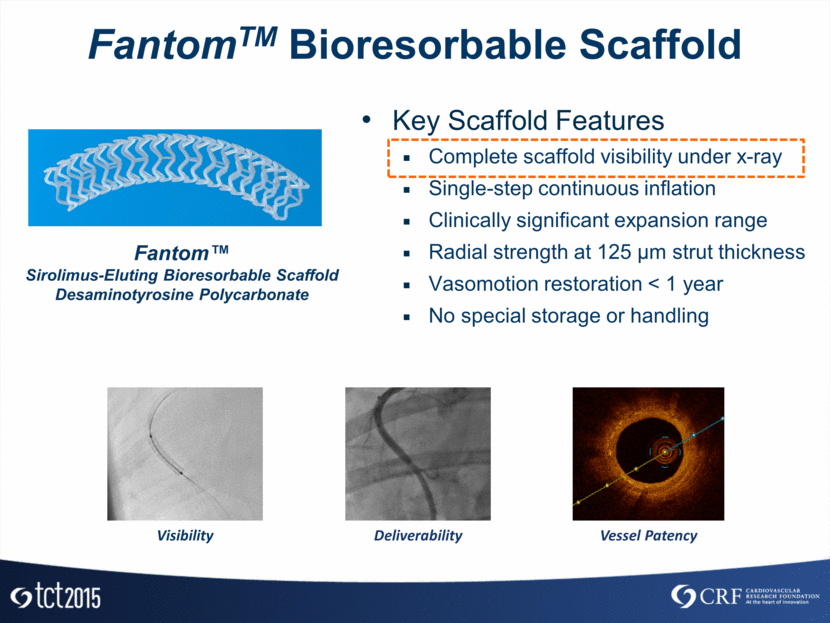
FantomTM Bioresorbable Scaffold Fantom™ Sirolimus-Eluting Bioresorbable Scaffold Desaminotyrosine Polycarbonate Key Scaffold Features Complete scaffold visibility under x-ray Single-step continuous inflation Clinically significant expansion range Radial strength at 125 µm strut thickness Vasomotion restoration < 1 year No special storage or handling Deliverability Vessel Patency Visibility
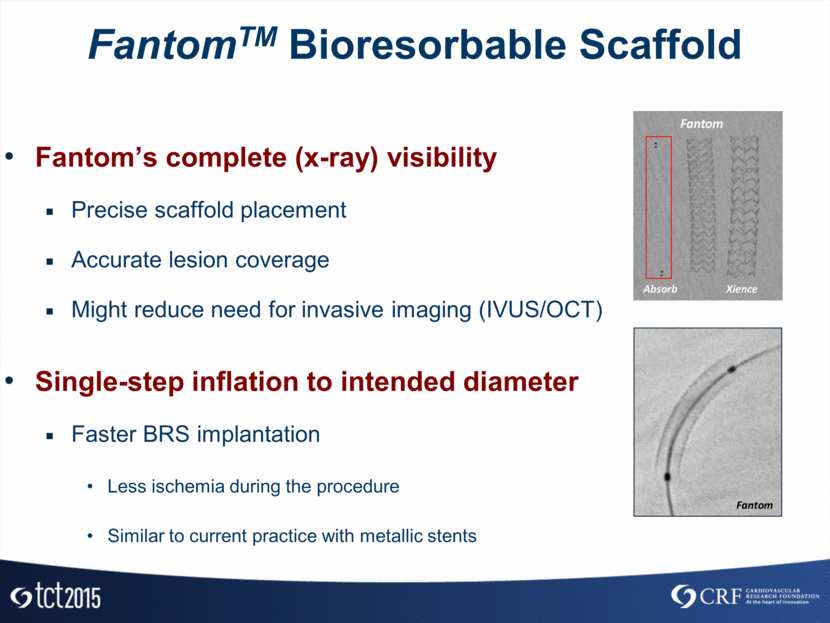
FantomTM Bioresorbable Scaffold Fantom’s complete (x-ray) visibility Precise scaffold placement Accurate lesion coverage Might reduce need for invasive imaging (IVUS/OCT) Single-step inflation to intended diameter Faster BRS implantation Less ischemia during the procedure Similar to current practice with metallic stents Absorb Fantom Xience Fantom
FantomTM How Radiopacity is Achieved Fantom is constructed of a unique proprietary polymer Desaminotyrosine (DAT) based polymer DAT is a derivative of the naturally occurring amino acid Tyrosine Iodine atoms are covalently bound to the polymer backbone providing radiopacity at implant and through degradation Iodine content is < 3% of what is contained in 1 ml of contrast R H O I I

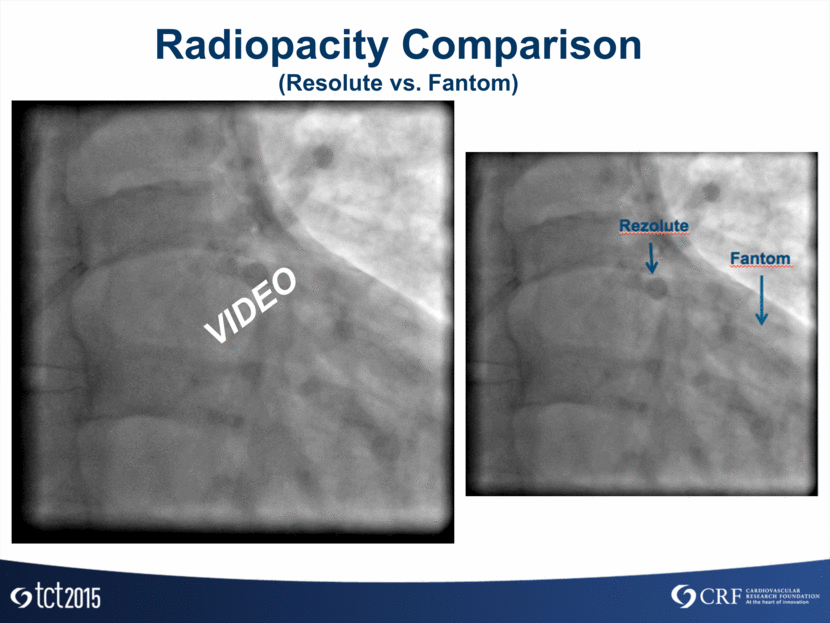
Radiopacity Comparison (Resolute vs. Fantom) VIDEO
FantomTM Radiopacity Changes Fantom Degradation Primarily degrades through a hydrolysis process Polymer is first separated into monomer components Monomer containing bound iodine is safely excreted from the body Results in a reduction in radiopacity over time Non-invasive imaging such as CT can track degradation. Fantom™ Polymer Degradation I2DAT I2DAT PLx Radiolabel ADME study shows I2DAT is safely excreted Safely Metabolized Results in a reduction of radiopacity over time

However, there are other features to look at in a BRS! Efficacy Safety Deliverability Conformability

However, there are other feature to look at in a BRS! Efficacy Safety Deliverability Conformability

Fantom Bioresorbable Scaffold Clinical Program Overview FANTOM I (Pilot Trial) 7 patients; 2 clinical sites Goal: verification of acute performance FANTOM II 220 patients; up to 30 clinical sites Cohort A - 110 patients for CE Mark application data set Cohort B - 110 patients for additional data to support product use Goal: safety & performance evaluation to support CE Mark

FANTOM I Study Design and Baseline Characteristics Patient Characteristics Patient Age (average years) 55.9±7.7 Male 100% Diabetes 42.9% Current/Former Smoker 100% Hypertension (requiring medication) 85.7% Hyperlipidemia (requiring medication) 71.4% Prior PCI 57.1% Prior CABG 0% Prior MI 57.1% LVEF 50.7±12.2% (n=6) Study Population N= 7 Patients 2 Clinical Centers (Brazil & Poland) 4 Month Follow-up Clinical & Imaging 6 Month Follow-up Clinical Angiographic N=7 OCT N=5 IVUS N=5 Long Term Follow-up Clinical (annual through 5 years)

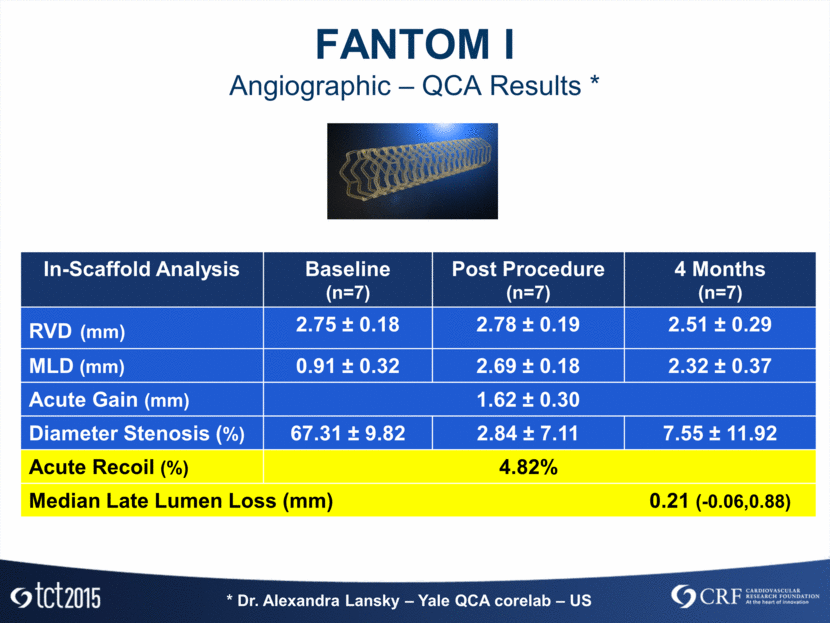
FANTOM I Angiographic – QCA Results * In-Scaffold Analysis Baseline (n=7) Post Procedure (n=7) 4 Months (n=7) RVD (mm) 2.75 ± 0.18 2.78 ± 0.19 2.51 ± 0.29 MLD (mm) 0.91 ± 0.32 2.69 ± 0.18 2.32 ± 0.37 Acute Gain (mm) 1.62 ± 0.30 Diameter Stenosis (%) 67.31 ± 9.82 2.84 ± 7.11 7.55 ± 11.92 Acute Recoil (%) 4.82% Median Late Lumen Loss (mm) 0.21 (-0.06,0.88) * Dr. Alexandra Lansky – Yale QCA corelab – US
Absorb ABBOTT Fantom REVA MEDICAL DESolve NX ELIXIR Differences and Similarities Poly-L-lactic acid Poly-L-lactic acid poly(I2DAT-co-lactic acid) 157µm 125 µm 150µm Crossing profile ~1.5mm Crossing profile ~1.5mm Crossing profile ~1.3mm Fantom Optical Properties Comparison
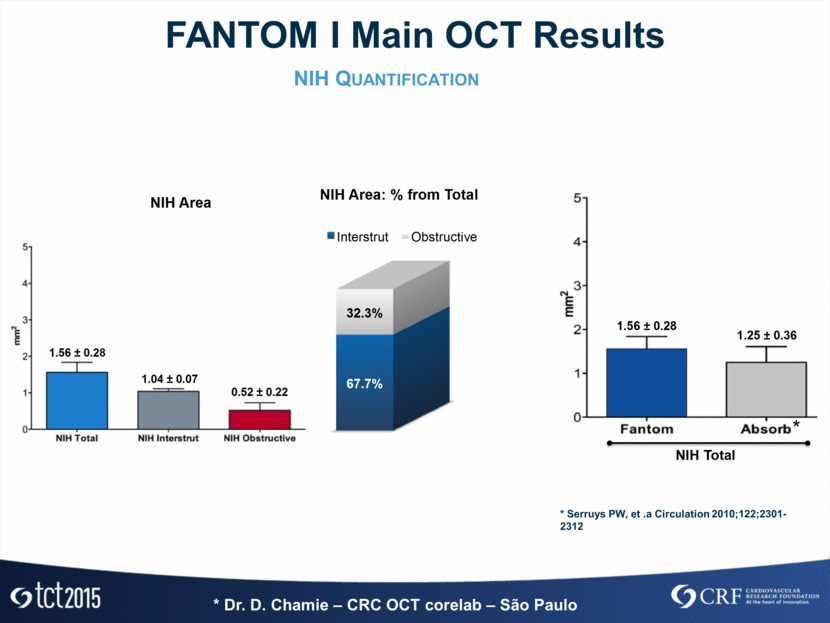
* Dr. D. Chamie – CRC OCT corelab – São Paulo NIH Quantification FANTOM I Main OCT Results * Serruys PW, et .a Circulation 2010;122;2301-2312 N I H T o ta l 1.56 ± 0.28 1.25 ± 0.36 * * Se rru ys PW , e t . a C i rcu l a t i o n 2 0 1 0 ; 1 2 2 ; 2 3 0 1 -2 3 1 2 67.7% 32.3% I n t e rst ru t O b st ru ct i ve 1.56 ± 0.28 1.04 ± 0.07 0.52 ± 0.22 NIH Area N I H A r e a : % fr o m T o ta l 67.7% 32.3% I n t e rst ru t O b st ru ct i ve 1.56 ± 0.28 1.04 ± 0.07 0.52 ± 0.22 NIH Area N I H A r e a : % fr o m T o ta l
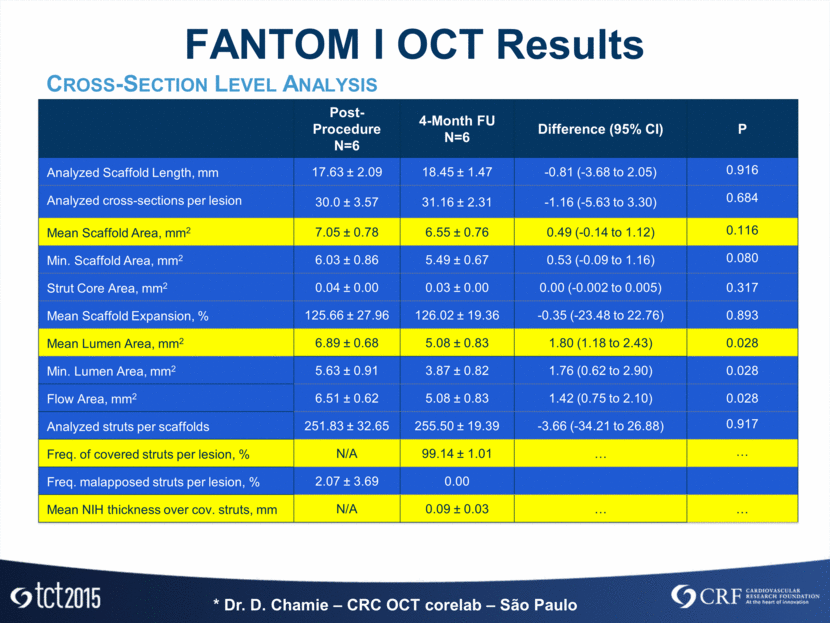
FANTOM I OCT Results Cross-Section Level Analysis Post-Procedure N=6 4-Month FU N=6 Difference (95% CI) P Analyzed Scaffold Length, mm 17.63 ± 2.09 18.45 ± 1.47 -0.81 (-3.68 to 2.05) 0.916 Analyzed cross-sections per lesion 30.0 ± 3.57 31.16 ± 2.31 -1.16 (-5.63 to 3.30) 0.684 Mean Scaffold Area, mm2 7.05 ± 0.78 6.55 ± 0.76 0.49 (-0.14 to 1.12) 0.116 Min. Scaffold Area, mm2 6.03 ± 0.86 5.49 ± 0.67 0.53 (-0.09 to 1.16) 0.080 Strut Core Area, mm2 0.04 ± 0.00 0.03 ± 0.00 0.00 (-0.002 to 0.005) 0.317 Mean Scaffold Expansion, % 125.66 ± 27.96 126.02 ± 19.36 -0.35 (-23.48 to 22.76) 0.893 Mean Lumen Area, mm2 6.89 ± 0.68 5.08 ± 0.83 1.80 (1.18 to 2.43) 0.028 Min. Lumen Area, mm2 5.63 ± 0.91 3.87 ± 0.82 1.76 (0.62 to 2.90) 0.028 Flow Area, mm2 6.51 ± 0.62 5.08 ± 0.83 1.42 (0.75 to 2.10) 0.028 Analyzed struts per scaffolds 251.83 ± 32.65 255.50 ± 19.39 -3.66 (-34.21 to 26.88) 0.917 Freq. of covered struts per lesion, % N/A 99.14 ± 1.01 Freq. malapposed struts per lesion, % 2.07 ± 3.69 0.00 Mean NIH thickness over cov. struts, mm N/A 0.09 ± 0.03 * Dr. D. Chamie – CRC OCT corelab – São Paulo
However, there are other feature to look at in a BRS! Efficacy Safety Deliverability Conformability

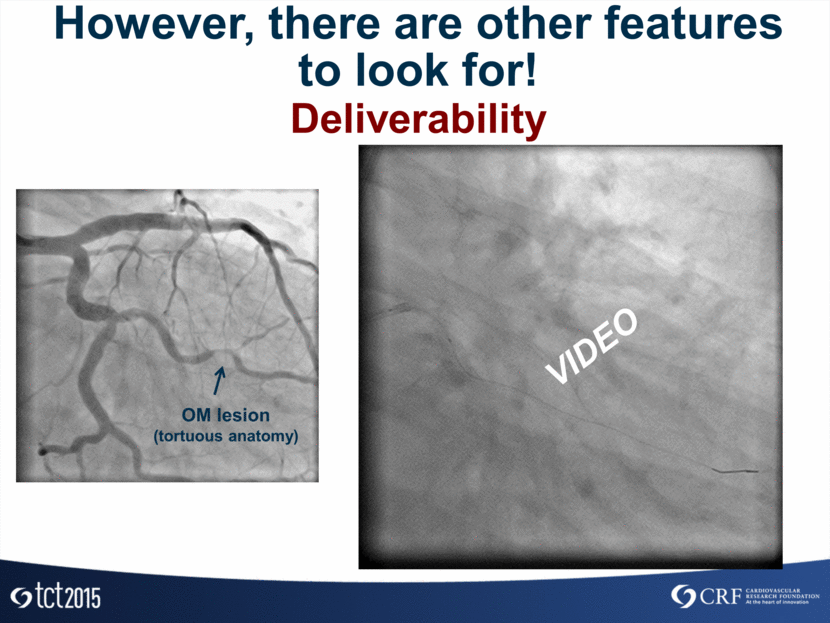
However, there are other features to look for! Deliverability OM lesion (tortuous anatomy) VIDEO
However, there are other feature to look at in a BRS! Efficacy Safety Deliverability Conformability

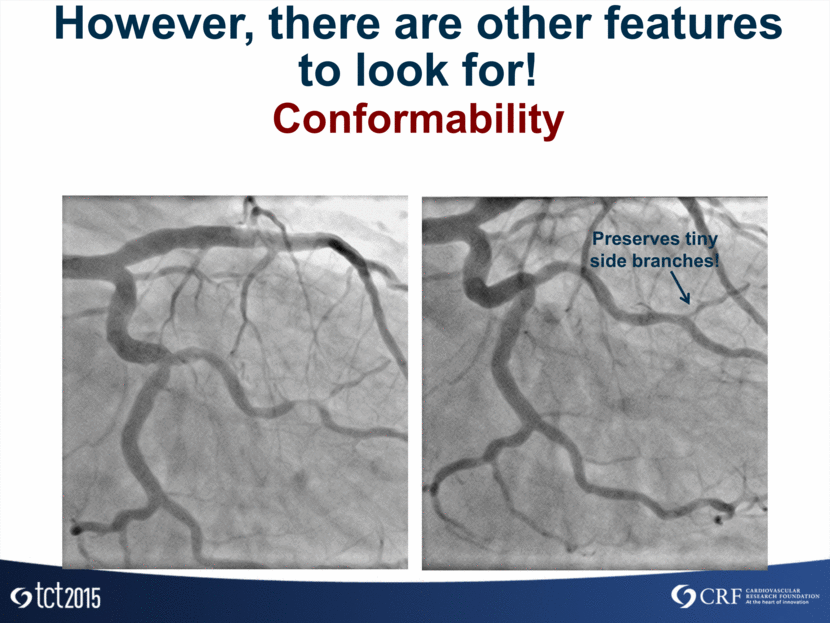
However, there are other features to look for! Conformability Preserves tiny side branches!
Conclusions Fantom’s proprietary polymer: Enhances both X-Ray and OCT visualization Provides for complete scaffold visualization Increases precision of device placement Confirmation of lesion coverage Precise alignment of secondary devices when needed Additionally, in the initial in human evaluation Fantom has shown: Good acute performance High rate of device deliverability Minimal residual stenosis Encouraging imaging performance at 4 months (minimal NIH formation, all struts covered and apposed) Low MACE rate

